What Exactly Happens When Someone Starts Hospice Care?
When a person chooses hospice care, they are shifting their focus. It's a move away from treatments meant to cure an illness. Instead, it's about a new kind of care centered on comfort, dignity, and quality of life.
The word "hospice" can feel final and frightening. People worry it means care will stop. But hospice is about making the most of the time a person has, comfortably and with dignity.
Understanding the Shift to Hospice Care
Thinking about hospice can feel overwhelming. It’s easy to believe it means giving up, but it is actually the opposite. It’s about taking control and living as well as possible for as long as possible.
The process begins when a doctor certifies that a patient’s illness is life-limiting. The goal of treatment then pivots from finding a cure to ensuring comfort. This shift is not just about medical care; it’s about adding a new layer of support.
As a nonprofit that has served the Central Coast of California for over 74 years, Central Coast VNA & Hospice guides families through this first step. We provide care in Monterey County, San Benito County, Santa Cruz County, and South Santa Clara County.
A Look at Hospice Care Today
Hospice isn't a rare choice anymore. It has become a trusted and beneficial path for end-of-life care. Research shows it helps patients live more peacefully and reduces unnecessary hospital visits.
In fact, this approach is now widely accepted. Over half of all Medicare patients who passed away in 2020 used hospice services. This shows how many families are choosing comfort and dignity at the end of life.
Here’s a simple breakdown of how the goals of care change when moving to hospice.
Hospice Care Focus vs. Curative Care Focus
| Aspect of Care | Curative Care Goal | Hospice Care Goal |
|---|---|---|
| Primary Objective | To cure the disease or prolong life. | To maximize comfort and quality of life. |
| Treatment Approach | Aggressive treatments (e.g., surgery, chemotherapy). | Managing pain and symptoms to relieve suffering. |
| Patient Focus | Primarily on the disease itself. | On the whole person—physical, emotional, and spiritual needs. |
| Family Involvement | The family provides support but is not the focus of care. | The family is part of the unit of care and receives support. |
| Location of Care | Often in a hospital or clinical setting. | Wherever the patient calls home. |
As you can see, hospice isn't about stopping care. It’s about changing the kind of care to align with the patient’s wishes.
What to Expect When You Start
Upon admission, an interdisciplinary team gets to work. This team includes a Registered Nurse, physicians, social workers, Chaplains, Hospice Aides, and volunteers. They create a plan to manage pain and address emotional needs from home.
This coordinated approach reduces stress and prevents last-minute trips to the hospital. It allows patients to live peacefully in a familiar place.
Making an Informed Decision
A common misstep is waiting too long to start hospice. Many families think it’s only for the last few days of life. This delay can lead to unmanaged pain, stress, and missed opportunities for meaningful time together.
It is better to consider hospice earlier when curative treatments are no longer helping. It is helpful to understand when to call hospice so you can make the most of the support available. Taking time to understand tools like a Texas Durable Power of Attorney for Health Care can also clarify decision-making.
If you're in Monterey, Salinas, Hollister, or Santa Cruz and are unsure if it's time for hospice, talk to a Central Coast VNA & Hospice team member. We can guide you with compassion—no pressure, just answers. Call 831-372-6668 or visit ccvna.com.
Your Initial Hospice Admission Visit
So, you’ve made a referral and are ready to explore hospice care. What happens next? The first step is a gentle visit from one of our Registered Nurses.
We come to you, whether that's a home in Salinas or a facility in Santa Cruz. This meeting is a compassionate conversation designed to put your family at ease. The nurse will explain our services, listen to your worries, and answer your questions.
What to Expect During the Visit
During this first meeting, the Registered Nurse will walk you through the necessary paperwork. They explain every form in simple, easy-to-understand terms. We want you to feel confident and informed.
This meeting is about putting you and your loved one back in control. The goal is to build a personalized plan of care that honors the patient's wishes. We will talk about everything from symptom management to spiritual support.
This simple graphic shows how the process begins.
Starting hospice is a structured journey. It begins with open communication and leads to a personalized assessment.
Creating Your Personalized Care Plan
Everything we gather during the admission visit becomes the foundation for the care plan. This is a living guide that we can adjust as needs change.
Your care plan will outline things like:
- Medical Care: How we will manage pain, schedule medications, and deliver medical supplies.
- Personal Care: A schedule for visits from a Hospice Aide to help with tasks like bathing.
- Emotional and Spiritual Support: Plans for visits from a Medical Social Worker and Chaplain.
- Coordination with Your Doctor: How our team will work with the patient's primary physician.
A well-crafted plan acts as a roadmap for our entire team. It ensures everyone understands the patient's goals and is working together. You can learn more about how we develop a hospice care plan that fits your family's needs.
At Central Coast VNA & Hospice, our mission is to make this transition smooth. Our team in Monterey County, San Benito County, Santa Cruz County, and South Santa Clara County is ready to help.
Meeting Your Dedicated Hospice Support Team
When starting hospice care, you are no longer walking this path alone. You gain a team of compassionate professionals dedicated to your well-being. This team provides comfort and guidance every step of the way.
At Central Coast VNA & Hospice, this team approach is at the heart of our mission. With over 74 years of service, we've built a care model that honors the whole person.

Who Is on Your Hospice Team?
Your hospice team is a group of specialists from different fields. They work together to carry out a personalized care plan.
Your team will typically include:
- Registered Nurse (RN) Case Manager: Your main contact for clinical care.
- Hospice Aide: Provides hands-on personal care like bathing and dressing.
- Medical Social Worker: Offers emotional support to the patient and family.
- Chaplain: Provides spiritual support tailored to your personal beliefs.
- Hospice Physician: Works with your doctor to provide expertise in pain and symptom management.
- Volunteers: Offer companionship, respite, pet therapy, and music therapy.
Starting hospice isn't just about managing an illness. It's about surrounding a person with a complete circle of support.
How Your Team Works Together
Our Central Coast VNA & Hospice team gets right to work. Our Registered Nurses and other team members are available 24/7 to deliver expert pain management and emotional support.
The RN Case Manager leads regular team meetings to discuss the patient's needs. This constant communication ensures your care plan remains effective.
The Role of the Hospice Aide
The Hospice Aide plays an important role in daily comfort. They provide personal care with a gentle touch. This helps patients maintain their hygiene and dignity.
Their presence brings relief to the patient and peace of mind to the family. You can learn more about their specific duties by reading about Hospice Aide responsibilities on our website.
How We Manage Pain and Symptoms
The core promise of hospice care is making patients as comfortable as possible. This is our first focus when someone begins care. It’s a shift from curing an illness to maximizing the quality of every day.
Comfort is more than just managing pain. Patients may also deal with shortness of breath, anxiety, or nausea. Our Registered Nurses and Hospice Physicians are experts at navigating these challenges.
A Comprehensive Approach to Comfort
Getting symptoms under control is a team effort. Your hospice team will oversee all medications related to the illness. This careful management helps patients stay alert and engaged with loved ones.
We also provide all necessary medical equipment to make the home safer. This often includes items like:
- A hospital bed to make resting easier.
- An oxygen concentrator to help with breathing.
- A bedside commode or walker to assist with mobility.
- Wound care supplies and other essential items.
This equipment is typically covered by the Medicare Hospice Benefit. Our team handles everything from ordering to setup, so you don’t have to worry.
We relieve the physical stresses of an illness so a patient can save their energy for what matters. When symptoms are controlled, that energy can go toward creating memories with family.
Around-the-Clock Support and Peace of Mind
One of the most reassuring parts of hospice is knowing that help is always there. Symptoms don’t follow a 9-to-5 schedule. For families in our four-county service area, our 24/7 on-call support is a vital lifeline.
A Central Coast VNA & Hospice Registered Nurse is always just a phone call away. This immediate access provides peace of mind and cuts down on stressful trips to the emergency room. You can learn more about our expert pain and symptom management on our website.
By taking on symptom control, hospice gives families freedom. You can concentrate on being present with your loved one. This is the compassionate care at the heart of our mission.
What Does a Typical Week in Hospice Care Actually Look Like?
When families first hear "hospice," it's natural to wonder how daily life will change. Hospice is not a constant medical presence in the home. It is a flexible schedule of supportive visits designed to fit into your life.
The point is to create a peaceful home environment built around the patient’s wishes. At Central Coast VNA & Hospice, our team works with your family to establish a routine.
The Rhythm of Scheduled Visits
A typical week in hospice is structured around visits from your care team. The frequency of these visits is tailored to the patient's individual needs.
A weekly schedule might look something like this:
- Registered Nurse Visits: A nurse will likely visit two to three times a week to manage symptoms and educate the family.
- Hospice Aide Visits: A Hospice Aide might come two or three times a week to help with personal care like bathing.
- Social Worker and Chaplain Check-ins: These team members schedule regular check-ins, often weekly or bi-weekly.
This structure ensures that professional support is always part of the weekly routine.
It’s So Much More Than Just Medical Support
Beyond clinical care, hospice is about enhancing quality of life. The nonprofit mission of Central Coast VNA & Hospice truly shines here. We offer services that bring joy and comfort to our patients.
To enrich a patient's week, we can arrange for:
- Volunteer Companionship: A trained volunteer can visit, giving family members a break.
- Pet Therapy: Certified therapy animals can bring moments of happiness and calm.
- Music Therapy: A music therapist can use music to help patients find peace.
These are integral parts of the care plan. We weave them into the schedule to help make each day as meaningful as possible.
The 24/7 On-Call Safety Net
While scheduled visits form the backbone of a typical week, a key benefit is access to 24/7 on-call support. Your family is never alone on this journey.
A sudden change in symptoms can be stressful. With hospice, you don't have to wait or rush to an emergency room. A Registered Nurse is always just a phone call away.
This constant availability is a vital safety net. Families in Salinas, Hollister, and throughout our service area can rest easier. This immediate access to care is what makes the hospice experience so supportive.
How Hospice Supports the Entire Family
Hospice care isn’t just for the patient. It’s a circle of support that wraps around the entire family. A life-limiting illness creates stress and uncertainty for everyone.
This comprehensive support is a core part of what happens when someone starts hospice. It transforms a lonely struggle into a shared journey.

Emotional and Spiritual Guidance
Navigating this chapter brings up complex emotions. Our Medical Social Workers are here to help families cope with stress. They can also connect you with helpful community resources.
At the same time, our Chaplains offer spiritual guidance to people of all backgrounds. They are gifted listeners who provide a calming presence. This support is tailored to your unique values.
Support That Continues After Loss
The support from Central Coast VNA & Hospice doesn’t end when a loved one passes away. We know the grieving process is a difficult road.
Our bereavement services are available to families for up to 13 months following a loss. This support includes:
- Individual Grief Counseling
- Support Groups
- Memorial Services
This continuing care ensures that families are never left to navigate loss alone. We also offer programs like respite care for family caregivers to provide them with needed breaks. You can also find other valuable guidance on navigating grief online.
Frequently Asked Questions About Starting Hospice Care
It’s completely normal to have questions when you’re thinking about hospice. Getting clear answers can help replace fear with facts. This empowers you to make the best decision for your loved one.
1. Does starting hospice mean giving up hope?
Not at all. It shifts the definition of hope. Instead of hoping for a cure, the focus turns to hope for comfort, peace, and meaningful moments. Choosing hospice is a decision to put dignity and comfort first.
2. Can a patient leave hospice care?
Yes, absolutely. A patient's condition may improve, or they may decide to try a new treatment. The choice always belongs to the patient and their family. You can stop hospice services at any time and can always return if needed.
3. How is hospice care paid for?
Hospice is a comprehensive benefit covered by Medicare Part A, Medi-Cal, the VA, and most private insurance plans. This coverage is all-inclusive and typically covers team visits, medications, and medical equipment. As a nonprofit, Central Coast VNA & Hospice is committed to providing care to all who are eligible, regardless of ability to pay.
4. Where is hospice care provided?
Hospice care is provided wherever the patient calls home. This could be a private residence, an assisted living facility, or a nursing home. Central Coast VNA & Hospice brings this care directly to patients throughout Monterey, San Benito, Santa Cruz, and South Santa Clara counties.
5. How soon can hospice care start?
Once a referral is made and the patient is certified as eligible, care can begin very quickly. At Central Coast VNA & Hospice, our team can often start care within 24 to 48 hours. Our goal is to provide relief and support to patients and families as soon as possible.
If you still have questions or are wondering if it's the right time to consider hospice, the compassionate team at Central Coast VNA & Hospice is here to help. Contact us today for a pressure-free conversation to get the answers and support your family needs.
Is Palliative Care Only for People Who Are Dying?
Many people ask, “Is palliative care only for people who are dying?” The short answer is no. This common myth comes from confusing palliative care with hospice care.
They are not the same. Palliative care is a specialized form of support that helps people live better while managing a serious illness. It is not about giving up on treatment.
What Is Palliative Care?
Palliative care is designed for anyone living with a serious illness. Its main goal is to provide relief from symptoms and stress. This care works alongside your regular medical treatments.
Think of it as an extra layer of support. It helps you manage the physical and emotional challenges of your illness. It does not replace curative treatments like chemotherapy or surgery.
An Extra Layer of Support, Not a Replacement
The goal of palliative care is to improve your quality of life. Your doctors focus on treating the disease. The palliative team focuses on you as a whole person.
This diagram shows how palliative care and curative treatment work together. They support you during a serious illness.
As you can see, these two types of care are not mutually exclusive. They are pillars of support that help you feel your best.
Why You Should Start Palliative Care Early
Waiting to start palliative care is a common misstep. People often delay because they think it means death is near. This delay can lead to unnecessary suffering and fewer care options.
Starting palliative care early gives you an advantage. It helps you get relief from symptoms like pain, fatigue, and anxiety. It also offers emotional and spiritual support.
This support can help you:
- Manage difficult symptoms like pain, nausea, and shortness of breath.
- Reduce stress and anxiety for you and your family.
- Improve communication with your entire healthcare team.
- Feel more in control of your treatment and health choices.
At Central Coast Vna & Hospice, we bring this support to families in Monterey, San Benito, Santa Cruz, and South Santa Clara counties. We believe everyone deserves the comfort and dignity that palliative care provides. You can learn more about the significant benefits of palliative care on our website.
Who Can Benefit from Palliative Care?
Palliative care is for anyone with a serious illness, regardless of their age or life expectancy. The primary goal is to improve your quality of life while you manage your condition.
It is an added resource that complements the care you already receive. You can start palliative support at any time, even while pursuing aggressive treatments.

A Wide Range of Conditions
Palliative care helps people with many long-term illnesses. It is not limited to a specific diagnosis.
Common conditions include:
- Cancer
- Heart disease (like congestive heart failure)
- Lung disease (like COPD)
- Kidney failure
- Dementia or Alzheimer's disease
- Parkinson's disease
- Amyotrophic Lateral Sclerosis (ALS)
The number of people who could benefit from this care is large. Data shows that 95% of people over 60 have at least one chronic illness. Nearly 80% have two or more. Palliative care helps manage these conditions to improve quality of life. For more information, you can review the extensive benefits of palliative care for cancer patients.
The Goals of a Palliative Care Team
A palliative care team works with you, your family, and your doctors. The team may include a Nurse Practitioner, a Registered Nurse, a Medical Social Worker, and a Chaplain.
Their mission is to treat the person, not just the disease. They work to ensure you can live each day to the fullest.
Key goals of the team include:
- Relieving Symptoms: The team provides expert management of pain, shortness of breath, fatigue, nausea, and anxiety.
- Improving Communication: They help you, your family, and your healthcare providers stay on the same page.
- Providing Emotional and Spiritual Support: A Medical Social Worker and Chaplain help you cope with the emotional and spiritual challenges of your illness.
- Coordinating Care: The team helps you navigate the healthcare system and make informed decisions.
At Central Coast Vna & Hospice, our team brings this compassionate care to your home in Monterey County and surrounding communities. We provide support that honors your wishes.
Why Waiting for Palliative Care Is a Mistake
One of the biggest missteps is waiting too long to start palliative care. This delay often comes from the myth that it signals the end of life. Waiting can lead to unnecessary suffering.
When symptoms are not managed early, they can become overwhelming. Pain, fatigue, and anxiety take a physical and emotional toll. Waiting until a crisis hits means you are always reacting instead of being proactive.
This hesitation is rooted in fear. The confusion between palliative care and hospice leads many to believe that starting this support is a step toward dying. It is actually a step toward living better with an illness.
The High Cost of Delayed Comfort
Delaying palliative care means losing valuable time. This is time that could be spent with better symptom control and more meaningful moments. Getting support early gives you the tools to manage your illness on your own terms.
Waiting to start palliative care is like waiting for a storm to pass without an umbrella. The support is designed to shield you, but it works best when you use it from the start.
Unfortunately, this delay is a global problem. An estimated 56.8 million people need palliative care each year. However, the World Health Organization reports that only about 14% of them receive it. You can discover key insights from the WHO's research to learn more.
Don't Miss the Opportunity for a Better Life
When families wait too long, they miss the chance to improve quality of life. By the time many patients get a referral, their symptoms may be severe. This creates a stressful cycle of crisis instead of steady support.
It is important to understand that palliative support is not the same as hospice. While Central Coast Vna & Hospice provides expert hospice services, palliative support is available much earlier. Our guide can help you understand when to consider hospice care.
Starting palliative care early gives you:
- More Control: You have a greater say in your treatment and comfort measures.
- Fewer Hospitalizations: Proactive symptom management at home can prevent emergency situations.
- Better Emotional Support: It gives your family resources to cope from the beginning.
The goal is not to shorten life but to improve the quality of the life you are living. Embracing palliative care early gives you an essential ally in your healthcare journey.
What In-Home Palliative Care Includes
So what does palliative care look like when our team from Central Coast Vna & Hospice arrives at your home? We bring a team-based approach directly to you, whether you live in Salinas, Santa Cruz, or Hollister. Our in-home services are built around caring for you as a whole person.
Expert Symptom Management
Living with a serious illness often means battling difficult symptoms. Our skilled Registered Nurses are experts at managing these challenges.
Our symptom management focuses on:
- Pain Relief: We work with your doctor to control your pain effectively.
- Controlling Nausea and Fatigue: We help manage side effects from treatments, giving you back your energy.
- Easing Shortness of Breath: Our nurses teach strategies to help you breathe more comfortably.
Getting symptoms under control can help you feel stronger. This proactive care often reduces the need for emergency room visits.
Emotional and Spiritual Support
A serious diagnosis affects your mind and spirit. It is normal to feel anxious or overwhelmed. Our team includes professionals trained to help you navigate these emotions.
Palliative care isn’t just about treating physical symptoms. It’s about caring for the whole person—mind, body, and spirit—to bring peace and comfort.
Our Medical Social Workers and Chaplains offer a safe space to talk. This support is shaped by your unique beliefs and values.
This support includes:
- Coping Strategies: Our Medical Social Worker can connect you with resources and provide counseling.
- Spiritual Guidance: Our Chaplains offer support that respects your personal beliefs.
- Family Support: We are here for your whole family, giving them the emotional tools they need.
Care Coordination and Advocacy
The healthcare system can be complicated. A big part of our job is making sure everyone on your medical team is on the same page. We act as your advocate and coordinator.
We ensure communication flows between your primary doctor and specialists. This helps your treatment plan align with your personal goals.
At Central Coast Vna & Hospice, our mission for over 74 years has been to provide this compassionate support. To learn more, explore our guide on palliative home care services.
Palliative Care on the Central Coast
At Central Coast Vna & Hospice, we bring expert palliative care to your front door. For over 74 years, we have been a nonprofit, mission-driven organization. We serve Monterey County, San Benito County, Santa Cruz County, and South Santa Clara County.
We are your neighbors, deeply rooted in the Central Coast. Our process is clear, compassionate, and simple.

Your Local Team of Experts
When you choose Central Coast Vna & Hospice, you gain a dedicated team. Our palliative care team collaborates with you, your family, and your doctors.
This team includes:
- A Nurse Practitioner specializing in symptom management.
- A Registered Nurse for ongoing assessment and care.
- A Medical Social Worker for emotional support and resources.
- A Chaplain for spiritual care that honors your beliefs.
This team approach ensures we see you as a whole person. We focus on your physical, emotional, and spiritual needs.
How to Get Started with In-Home Care
Getting started is simple. It all begins with a conversation about your needs.
We bring care to you, allowing you to remain in the comfort and familiarity of your own home. This focus on in-home support is a cornerstone of our compassionate care model.
Here’s what you can expect:
- Initial Contact: You, a family member, or your physician can call us to learn more.
- In-Home Assessment: One of our clinicians will visit you at home to listen to your concerns.
- Personalized Care Plan: We work with you and your doctors to create a care plan focused on your goals.
- Ongoing Support: Our team provides regular visits and is always available to support you.
If you are in Monterey, Hollister, Salinas, or Santa Cruz, our local team can help. We can guide you on whether palliative care is the right next step. You can learn more about why Central Coast VNA is the best choice for palliative care on the Central Coast.
Take the Next Step Toward Comfort and Control
Palliative care is not just for the end of life. This specialized support is about living better, not giving up. It is an extra layer of care that works alongside your regular treatments.
If you or a loved one is worn down by a chronic condition, you don’t have to go through it alone. The right support can improve your quality of life. It allows you to focus on what matters most.
Connect With Your Local Experts
For families on the Central Coast, expert support is available in your community. As a local nonprofit with over 74 years of service, Central Coast Vna & Hospice is dedicated to bringing this vital care to you at home.
Palliative care is a choice for hope—hope for better symptom control, for more good days, and for a stronger support system. Asking for help is a sign of strength.
If you live in Monterey, Salinas, Hollister, or Santa Cruz, our skilled team is ready to help. We work with your doctors to create a care plan that respects your goals.
Don’t wait for a crisis. Reach out to Central Coast Vna & Hospice today. Let us help you find out if in-home palliative care is right for you.
Let's start the conversation:
- Call us: 831‑372‑6668
- Visit our website: Learn more about our palliative care services
Frequently Asked Questions About Palliative Care
Many families have questions when they explore palliative care. Here are clear answers to some common questions we hear.

Will my insurance cover palliative care?
Yes, in most cases. Palliative care is a medical specialty covered by Medicare Part B, Medicaid, and most private insurance plans. Our team at Central Coast Vna & Hospice can help you understand your specific coverage.
Can I keep my own doctor?
Absolutely. Our palliative team works alongside your current doctors and specialists. We do not replace them. We act as an extension of your existing medical team.
How is palliative care different from home health care?
Home health care is usually short-term and focuses on recovery after an event like surgery. Palliative care is long-term support for managing a chronic, serious illness. It focuses on ongoing symptom management and improving quality of life.
Does starting palliative care mean I have to stop my treatments?
No, not at all. You can receive palliative care while you are undergoing curative treatments like chemotherapy. Our support can help you manage treatment side effects, making it easier to continue your care plan.
Who is on the palliative care team?
Our in-home palliative care team is a group of professionals who work together to support you. The team usually includes a Registered Nurse, a Medical Social Worker, and a Chaplain. This group works with your doctors to make sure all your needs are met. For more answers, please visit our palliative care FAQs page.
How Do I Get Help Caring for My Aging Parent at Home? A Practical Guide
Feeling stretched thin while caring for an aging parent is an incredibly common experience. Acknowledging you need support is the first and most important step.
You're not just looking for buzzwords; you're asking, "What do I do next?" This guide provides clear, practical steps to find the right help.
Recognizing When It Is Time to Ask for Help
Caring for an aging loved one often starts small. It might be helping with groceries or offering rides to appointments.
Over time, these tasks can grow until you're managing medications and worrying about safety. You might feel overwhelmed and isolated, unsure of what to do.

If this sounds familiar, you are not alone. This guide will walk you through building a support system so you no longer have to do everything yourself.
The Growing Need for Support
Nearly half of adults expect to care for an aging relative at some point. Many find themselves overwhelmed when insurance-covered services don't meet the full need.
The number of family caregivers for older adults has grown significantly. Learn more about the trends in family care for older Americans. This shows the pressure families face today.
Professional in-home support isn't a luxury. It's often a necessity for maintaining both your parent's well-being and your own.
Moving Past Common Missteps
A common misstep is waiting for a crisis to ask for help. Families often assume they must piece together care on their own.
Many don't know what services can come to the home beyond basic nursing. The key is to be proactive and plan ahead.
Planning can reduce burnout, prevent accidents, and improve your parent’s comfort. It empowers you to make thoughtful decisions instead of reacting to emergencies.
Look into full-spectrum services that combine skilled nursing, therapy, and palliative support. As a nonprofit serving the Central Coast for over 74 years, Central Coast VNA & Hospice offers this coordinated approach.
Our services bring expertise right to your parent's home in Monterey County, San Benito County, Santa Cruz County, and South Santa Clara County:
- Skilled Nursing: A Registered Nurse helps manage complex medical needs.
- Therapies: Physical, occupational, and speech therapists improve strength and safety.
- Palliative Consults: We help manage symptoms and stress from serious illness.
- Social Work Support: Our team connects you with resources and provides emotional support.
If you see changes in your loved one's health, it helps to know what to look for. You can learn more about the 5 warning signs that elderly parents need home health care.
Your Quick Guide to Getting Started
Taking the first step can feel daunting. This table breaks down the immediate actions you can take.
| Action Item | Why It Matters | Real-World Example |
|---|---|---|
| Have an open conversation. | This builds trust and ensures your parent feels involved in decisions. | "Mom, I've noticed you're having a harder time with the stairs. I want to talk about how we can make things easier for you." |
| Assess daily needs. | You can't find the right help if you don't know what you're solving for. | Does Dad need help with meals? Medication reminders? Bathing? Make a list of what he struggles with daily. |
| Contact a local expert. | A professional can explain options, navigate insurance, and save you guesswork. | Call a trusted local agency like CCVNA. A quick call can clarify if home health or another service is the right fit. |
These simple actions move you from worry to proactive planning.
Creating a Clear Picture of Your Parent's Needs
Moving from general concern to an action plan can feel overwhelming. The first step is to get a realistic look at your parent's day-to-day life.
This isn't about being critical. It’s about creating a map of where support is needed most.
This clarity helps you talk to doctors and find services that will make a difference.
A Practical Checklist for Assessing Needs
Think through a typical day for your loved one. Being specific and honest here will guide your decisions.
This assessment helps you figure out if you need a Registered Nurse for medical tasks or a Hospice Aide for personal support.
Here are four key areas to evaluate:
- Medical Tasks: Is your parent keeping up with medications correctly? Can they manage multiple doctor's appointments?
- Personal Care: Does your loved one need help with daily routines like bathing or dressing? This is often where hands-on support becomes essential.
- Household Responsibilities: Who is handling groceries and cooking? Is the house clean? These chores are important for nutrition and safety.
- Safety and Mobility: Can your parent move around their home without risk of falling?
A thorough assessment turns a broad concern into an actionable problem. It gives you something concrete to work with.
This detailed picture is your most powerful tool. It lets you have productive conversations with your parent’s doctor and providers like our team at Central Coast VNA & Hospice.
From Observation to Action
Once you have a list of challenges, you can match them to the right solutions. For medication worries, skilled nursing visits can ensure proper management.
Our guide on effective medication management for the elderly offers more details.
If mobility is the main issue, in-home Physical Therapy can improve strength and reduce fall risk. A Medical Social Worker can connect you with local programs for meal prep and other needs.
You don't have to piece this together on your own. A Registered Nurse from Central Coast VNA & Hospice can perform an in-home assessment and build a professional care plan.
This plan can include services tailored to every need you identified. This proactive approach enhances your parent's comfort and safety at home in communities like Salinas or Santa Cruz.
Understanding Your In-Home Care Options
Once you know your parent's needs, the next step is finding the right professional help. Many families feel lost, thinking their only option is basic nursing care.
There is a whole spectrum of expert support that can be delivered at home. Getting familiar with these services is key.
For families on the Central Coast, Central Coast VNA & Hospice provides a full Continuum of Care. This ensures consistent, coordinated support through home health, palliative care, and hospice.
Identifying a specific challenge helps narrow down the kind of professional support needed.
Home Health Care for Recovery and Rehabilitation
Home Health Care is skilled, short-term medical support prescribed by a doctor. It helps patients recover after an illness, injury, or surgery.
This care is for a parent recently discharged from the hospital or managing a new condition. For example, a Physical Therapist can help regain strength after a hip replacement.
A Registered Nurse might visit to change a dressing or manage IV medications.
The main goals are to:
- Restore independence through therapy and skilled nursing.
- Prevent a return trip to the hospital.
- Empower patients and families with knowledge.
Palliative Care for Comfort and Quality of Life
A common misconception is that Palliative Care is only for the end of life. It's specialized medical support focused on relief from symptoms and stress of a serious illness.
It can be provided at any age and stage, alongside curative treatments. For example, a palliative care team can help a father manage chemotherapy side effects.
The goal isn't to replace treatment but to improve his quality of life. Palliative care adds an extra layer of support for the whole person.
Hospice Care for Peace and Dignity
When a doctor determines an illness is no longer curable, Hospice Care becomes an option. The focus shifts from curing the disease to providing comfort and dignity.
This is comprehensive support from a dedicated team, including a physician, Registered Nurse, and Hospice Aide. They work together to manage symptoms and offer spiritual and emotional support.
Hospice care at home means a parent can stay in a familiar place, surrounded by loved ones.
Comparing Home Health, Palliative, and Hospice Care
This table breaks down the key differences between these core in-home services.
| Service Type | Primary Goal | Ideal Candidate | Medicare Coverage |
|---|---|---|---|
| Home Health | Recover from illness, injury, or surgery. Restore independence. | Someone needing short-term, skilled care post-hospitalization. | Typically covered for eligible patients who are homebound. |
| Palliative Care | Relieve symptoms and stress of a serious illness; improve quality of life. | Anyone with a serious illness, still receiving curative treatment. | Often covered under Medicare Part B and private insurance. |
| Hospice Care | Provide comfort, dignity, and peace at the end of life. | Someone with a terminal illness and a life expectancy of 6 months or less. | Fully covered under the Medicare Hospice Benefit. |
Each service plays a unique role depending on your parent's health journey. According to the National Hospice and Palliative Care Organization (NHPCO), over 1.72 million Medicare beneficiaries received hospice services in 2020 (NHPCO, 2021).
At Central Coast VNA & Hospice, our mission for over 74 years has been to provide this continuum of support. We help families in Monterey, Salinas, and Hollister find the right in-home care for seniors.
Navigating Insurance to Pay for In-Home Care
The fear of cost often stops families from seeking help. The good news is that expert in-home medical care is often accessible.
Most in-home medical services are covered through Medicare, Medi-Cal, and private insurance. You don’t have to become an expert overnight.
Organizations like Central Coast VNA & Hospice help families navigate these financial questions daily.
How Medicare Covers In-Home Medical Care
For many older adults, Medicare is the first place to turn for home health coverage. There are specific criteria that must be met.
To qualify for Medicare-covered home health care, a patient must:
- Be under the care of a doctor with a plan of care.
- Require intermittent skilled services, like nursing or therapy.
- Be certified by a doctor as "homebound."
"Homebound" doesn't mean your parent has to be bedridden. They can still go to medical appointments and qualify.
You can learn more about the specifics of Medicare home care eligibility on our site. A common misconception is that families must figure out insurance details alone.
Trusted providers like CCVNA will verify benefits and handle the insurance side for you.
The Role of Medi-Cal and Private Insurance
Medicare doesn't cover everything. This is where other plans like Medi-Cal and private insurance are essential.
Medi-Cal (California's Medicaid program) provides critical support beyond Medicare. It is a lifeline for many families facing financial hardship.
Private insurance plans can also cover home health, palliative, and hospice services. Long-term care insurance is specifically designed for these needs.
Planning ahead by understanding the real long term care insurance cost is critical.
You Don't Have to Navigate This Alone
Coordinating benefits can feel like a full-time job. Choosing a local, mission-driven provider makes a difference.
For over 74 years, Central Coast VNA & Hospice has helped families in our region secure the care they need. Our team handles the complexities for you.
We work directly with doctors and insurance providers to confirm eligibility. Our goal is to make the process smooth and stress-free.
How to Arrange Services and What to Expect
You've figured out what your parent needs and the types of care available. The next question is: how do you get started?
Getting professional help at home is often more straightforward than you might realize.
For skilled services like Home Health, the journey begins with your parent's doctor. A physician's referral is the first step, confirming medical necessity.
Making the First Call
With a doctor's referral, your next move is to contact a trusted local provider. When you call Central Coast VNA & Hospice at 831-372-6668, you're building a real support system.
That first conversation is simple and reassuring. Our care managers will ask about your parent’s situation, their doctor, and insurance details.
This is the starting point for our team to begin verifying benefits and scheduling the in-home assessment.
The In-Home Assessment and Care Plan
Within a day or two, a Registered Nurse will visit your parent’s home. This is a comprehensive evaluation of your parent’s health and living environment.
It’s a collaborative process where the nurse listens to your concerns and answers questions.
This in-home visit is foundational. It’s where a personalized plan of care is created. This plan outlines goals, services needed, and visit frequency.
The plan is a living document that we adjust as your parent's needs change.
Meeting Your Interdisciplinary Care Team
One of the greatest benefits of working with an agency like Central Coast VNA & Hospice is the team. You get a whole team of specialists who coordinate holistic care.
Each member brings a unique skill set:
- Registered Nurse (RN): The clinical leader who manages the care plan and communicates with the doctor.
- Medical Social Worker (MSW): Provides emotional and practical support, connecting you to community resources.
- Hospice Aide: Assists with personal care like bathing and dressing, preserving dignity.
- Chaplain: Offers non-denominational spiritual support, respecting all beliefs.
From the first call, you and your parent are guided by compassionate experts. Our team helps you build a plan that works, right at home.
Finding Support for Yourself Before Burnout Sets In
You can only give your best care when you're also taking care of yourself. The day-to-day reality of caregiving is emotionally and physically draining.
Pushing yourself to the limit leads to burnout. Recognizing you need a hand is a smart strategy for the long haul.

Many families feel overwhelmed, especially when insurance-covered services don't cover everything. This is where planning ahead makes a difference.
Building Your Own Support System
Access to education and emotional support is a powerful tool. This help is often woven into professional home-based services.
A Medical Social Worker from Central Coast VNA & Hospice is there for the whole family. They provide counseling and connect you with community resources.
Asking for help is the most powerful thing you can do for your parent and yourself. It prevents burnout and ensures consistent care.
Exploring options like respite care for family caregivers can give you a needed break. It's a critical piece of a sustainable care plan.
If you're in Monterey, Hollister, Santa Cruz, or Salinas, you don't have to figure this out alone. Central Coast VNA & Hospice has spent over 74 years helping families like yours.
Call 831-372-6668 or visit ccvna.com to learn more about how our team can help you build a plan that works—before burnout sets in.
Frequently Asked Questions About In-Home Care
Exploring care options for a loved one brings up many questions. Below are answers to some of the most common things families ask.
How do I start the conversation about needing help with my parent?
Start with love and concern. Frame it as a way to support their independence, not take it away. Say something like, "I want to make sure you're safe and comfortable here at home. Let's talk about some options to make things easier."
Does my parent have to be completely bedridden to get home health care?
Not at all. Under Medicare, a person is 'homebound' if it takes a major effort to leave the house. They can still go to doctor’s appointments or infrequent outings and qualify for skilled nursing and therapy at home.
Can my parent receive palliative care while still trying to cure their illness?
Yes, absolutely. Palliative care is an extra layer of support alongside curative treatments. Its purpose is to help manage symptoms and improve day-to-day quality of life during a serious illness.
What if my parent refuses to accept help from strangers?
This is a common concern. Start small, perhaps with just one type of service. Often, when a parent meets our compassionate clinicians, like a friendly Registered Nurse or therapist, they become much more comfortable with the idea.
How quickly can we start getting care from Central Coast VNA & Hospice?
Once we receive a referral from your parent’s doctor, our team moves quickly. We can typically schedule the first in-home assessment within 24 to 48 hours to get a personalized care plan started.
Trying to figure out in-home care can feel overwhelming, but you don’t have to do it alone. The compassionate team at Central Coast VNA & Hospice has been the trusted guide for families in our community for over 74 years.
Give us a call at 831-372-6668 or visit us online to learn more about how we can help.
Can Home Health Care Really Help My Parent Stay Out of the Hospital?
Can home health care truly help your parent stay out of the hospital? The answer is a strong yes. It acts as a bridge, bringing skilled medical care into the comfort of home. This ensures recovery stays on track and helps prevent return trips to the ER.
The Overwhelming Journey from Hospital to Home
Bringing a parent home after a hospital stay can feel confusing. You often get a stack of papers, a long list of new medications, and are told to set up follow-up appointments. This is a common and stressful experience for families across Monterey County. It leaves them wondering, "Am I doing this right?"
The good news is that you don't have to figure it all out alone. When facing a sudden illness or a hospital discharge, many families are told to “get home health care.” But they often don't know what it includes, who provides it, or how to qualify.
Understanding Your Options
Many people think home health is just a quick nurse visit or only for someone who is bedbound. Others hire expensive private help without realizing Medicare may cover what their parent needs to recover safely. Getting the right care early is key to avoiding ER visits and hospital readmissions.
Home health care helps over 12 million Americans a year recover from illness, manage chronic conditions, and live independently at home. It’s not just basic help—it’s skilled care, including nursing and rehabilitation therapy, prescribed by a doctor.
The first step is to ask your parent's doctor or the hospital discharge planner for a referral to a Medicare-certified home health agency. This professional support often includes:
- Wound Care: To prevent serious infections that could send your parent back to the hospital.
- Medication Management: Teaching you and your parent how to safely manage new prescriptions.
- Fall Prevention: Physical and occupational therapy to rebuild strength and make the home safer.
- Disease-Specific Education: Hands-on training for managing conditions like heart failure or diabetes.
To help you understand the different types of in-home support, here's a quick comparison:
Home Health Care vs Private-Duty Care
| Service Provided | Medicare-Certified Home Health (e.g., CCVNA) | Private-Duty Care (Hired Help) |
|---|---|---|
| Type of Care | Skilled medical care (nursing, PT, OT, speech therapy) ordered by a doctor. | Non-medical assistance with daily living (bathing, meals, errands). |
| Goal | To help a patient recover from an illness, injury, or surgery. | To provide long-term support for daily activities and personal care. |
| Payment | Typically covered 100% by Medicare and most private insurance plans. | Paid for out-of-pocket by the individual or family. |
| Duration | For a specific, doctor-ordered period until recovery goals are met. | Can be arranged for as many hours as needed, for an indefinite period. |
The main takeaway is that Medicare-certified home health focuses on skilled clinical care for recovery. Private-duty care is about ongoing personal assistance.
As a nonprofit organization serving our community for over 74 years, Central Coast VNA & Hospice provides this critical link between the hospital and home. Our skilled clinicians offer personalized, expert care that supports a safe recovery. You can learn more in our guide to discharge planning from the hospital.
How Skilled Care Keeps Your Parent Out of the Hospital
When a parent comes home from the hospital, the biggest fear is a return trip to the ER. This is where skilled home health care makes a real difference. It creates a safety net of clinical support right in their living room.
This isn't just having someone check in. It’s a strategic plan designed by licensed clinicians—like Registered Nurses and therapists—who work with your parent's doctor. The goal is to target specific risks that could send your loved one back to the hospital.
The journey from a hospital stay to a safe recovery at home is a critical transition. Home health care acts as the bridge, ensuring a smoother healing process.
This coordinated, proactive approach is what Central Coast VNA & Hospice provides. We are a mission-driven nonprofit serving Monterey, San Benito, Santa Cruz, and South Santa Clara counties.
The Power of Proactive Care at Home
The true value of home health care is catching problems before they become crises. Our clinicians are trained to spot subtle changes in a patient's condition. This consistent oversight is a game-changer.
Research shows that home health care can dramatically cut the risk of returning to the hospital within 30 days. One key study found that patients receiving home health services had a 60% lower risk of readmission compared to those without that support.
This professional oversight gives families incredible peace of mind. Knowing a skilled clinician is keeping a close watch allows you to focus on your parent's well-being.
A Coordinated Team Approach to Recovery
With home health care, you get a whole team of specialists. It’s a holistic approach that ensures all of your parent's needs are met.
This team often includes:
- Registered Nurses (RNs): They manage the overall care plan, handle medications, and treat wounds.
- Physical Therapists (PTs): PTs are essential for regaining strength and mobility after an illness or surgery.
- Occupational Therapists (OTs): OTs help patients relearn how to safely perform daily activities like bathing and dressing.
- Speech-Language Pathologists: They work with patients who have trouble speaking or swallowing.
This team-based therapy and support is vital. For example, they can guide patients through safe and effective cardiac rehab exercises at home to build strength safely.
This coordinated effort makes all the difference. To see how we put these strategies into action, read our article on how Central Coast VNA reduces hospital readmissions. Our expert team helps your parent thrive safely at home.
Managing Chronic Conditions to Avoid a Crisis
Most hospital stays don't happen because of a sudden injury. They often occur when a chronic condition—like heart failure (CHF) or diabetes—spirals out of control. Skilled home health care acts as an early warning system to stop a crisis before it begins.
This proactive approach is one of the most powerful ways home health keeps a loved one out of the hospital. A Registered Nurse becomes a health coach, providing hands-on education in your parent's home.
For families in Monterey, Salinas, or Hollister, this personalized guidance from Central Coast VNA & Hospice can be a game-changer. Our clinicians teach you how to recognize early warning signs. This one-on-one attention helps turn anxiety into informed action.

Empowering Patients Through Education
Effective management of any chronic illness is built on understanding. When a parent knows why they need to take a pill, they are more likely to stick with their care plan. A home health nurse from CCVNA provides this education in a comfortable setting.
This isn’t about just handing over a pamphlet. It’s about demonstrating skills and answering questions in real-time.
Key areas where our nurses educate families include:
- Symptom Recognition: We teach the difference between a normal fluctuation and a red flag that requires a call to the doctor.
- Medication Adherence: It’s vital to understand what each medication does and how to create a simple system so doses aren't missed.
- Dietary Guidance: Our team helps your parent understand and follow special diets, like low-sodium for heart conditions.
- Equipment Use: We provide clear instructions for using medical equipment like blood pressure cuffs or glucose meters.
This expert guidance transforms the home into a safe environment for healing.
The Role of Medication Management
One of the biggest risks for a patient just home from the hospital is medication mismanagement. New prescriptions and changed dosages can lead to errors. Home health nurses are experts at untangling this complexity.
Our nurses perform medication reconciliation to catch dangerous discrepancies. They can set up pill organizers and create easy-to-follow schedules. You can learn more in our guide to medication management for the elderly.
A home health nurse doesn't just manage medications; they build a system of safety and understanding. This skill is fundamental to preventing hospital readmissions.
This careful oversight ensures your parent receives the full benefit of their prescribed treatments. It is a foundational piece of helping your parent stay safely at home.
For over 74 years, Central Coast VNA & Hospice has been dedicated to this mission. If you have questions about managing a chronic condition at home, call us at 831-372-6668.
Signs Your Parent Is Ready for Home Health Care
How do you know when it’s the right time for home health care? A recent hospital stay is an obvious trigger, but many subtle signs can tell you that skilled support is needed. Catching these cues early is one of the best ways to help your parent stay out of the hospital.
It often starts with small changes. Maybe your parent is less steady on their feet or seems confused about their new medications. These are signals that professional support could prevent a future crisis.
For families in Monterey County and San Benito County, this can be a tough conversation. But waiting until after a fall is far more stressful. The goal is to be proactive.

Common Warning Signs to Watch For
If you notice one or more of these situations, it might be time to talk with your parent's doctor. Each sign points to a skilled service that can make a huge difference.
- A Recent Fall or Growing Fear of Falling: A Physical Therapist can build an exercise plan to improve strength, while an Occupational Therapist can remove hazards at home.
- Confusion Over Medications: Are there multiple pill bottles on the counter? A Registered Nurse from Central Coast VNA & Hospice can organize their medications and create an easy-to-follow schedule.
- More Frequent ER Visits or Hospital Stays: This pattern often means a chronic condition isn't being managed effectively. Skilled nursing provides the monitoring needed to stabilize their health.
- Difficulty with Daily Tasks: If bathing or dressing has become a struggle, an Occupational Therapist can teach safer, easier ways to handle these tasks.
The Link Between Health Risks and Hospital Readmissions
Certain health issues significantly raise the odds of a patient ending up back in the hospital. The good news is these are the exact risk factors our home health clinicians are trained to manage.
Broader data on patients transitioning from the hospital to home health showed a 14.7% 30-day readmission rate. Key predictors for readmission included longer hospital stays, having multiple chronic conditions, the presence of urinary catheters, and pressure ulcers.
Home health care directly confronts these risks. Our nurses and therapists create customized care plans to manage wounds, provide therapy, and monitor for trouble.
Taking the Next Step
Recognizing the signs is the first step. The next is reaching out for help. A simple conversation with your parent's doctor about a home health evaluation can open the door to the support they need.
For a more in-depth look, check out our guide on the 5 warning signs that elderly parents need home health care.
Navigating the Referral Process and Medicare Coverage
One of the first questions families ask is, "How will we pay for this?" For most eligible seniors, Medicare covers 100% of the cost of skilled home health care. This knowledge often brings a huge sense of relief.
Let's break down how the process works so you can feel confident taking the next step.
Getting the Referral
It all starts with a doctor's referral. This can happen during a hospital discharge in Salinas or a routine check-up in Santa Cruz. That one step connects your parent with the professional care they need.
You don't have to wait for a crisis to ask for help. If you've noticed your parent is struggling, bring it up with their doctor.
Hospital discharge planners are also your allies. They want to make sure patients have a solid recovery plan to avoid penalties for high readmission rates.
Understanding Medicare Eligibility
For Medicare to cover home health care, your parent needs to meet a few basic requirements. Our team at Central Coast VNA & Hospice is always here to help you navigate it.
The main criteria are straightforward:
- A Doctor's Order: A physician must certify that your parent needs skilled medical services at home.
- Needing Skilled Care: Your parent must require intermittent skilled nursing or therapy services.
- Being "Homebound": This doesn't mean your parent is stuck in bed. It simply means leaving home requires a considerable effort.
The most important thing for families to know is that you have a choice. You can request a Medicare-certified agency, like Central Coast VNA & Hospice, to ensure your parent receives care from a trusted, local, nonprofit provider.
You can get a more detailed breakdown by reviewing our guide on Medicare home care eligibility. Families often have questions about other equipment, too; knowing about things like Medicare coverage for electric wheelchairs can be a big part of successful home care planning.
Once the referral is made, one of our skilled clinicians will visit your parent's home. They will work with your family to create a personalized plan of care.
Your Partner in Health on the Central Coast
Choosing a home health provider is about inviting someone you trust into your home. At Central Coast VNA & Hospice, we have always understood that. We are a local, nonprofit organization that’s been part of this community for over 74 years.
Our roots run deep here. We proudly serve our neighbors across Monterey County, San Benito County, Santa Cruz County, and South Santa Clara County. From Salinas to Santa Cruz, we are here because this is our home, too.
A True Continuum of Care
What sets us apart is our seamless continuum of care. Health needs can shift. If your parent’s situation changes, they can transition smoothly from our home health services to palliative or hospice care without stress.
They will be supported by a team they already know and trust. It’s a level of stability that makes a world of difference.
Our skilled team—including Registered Nurses, Physical Therapists, and Occupational Therapists—partners with your parent's doctor. We work together to build strength, manage symptoms, and restore independence.
We believe that expert medical care, delivered with warmth and respect, is the key to avoiding unnecessary hospital trips. If you think your parent could use that support, the first step is a simple conversation.
If you’re in Salinas, Monterey, Hollister, or Santa Cruz, contact Central Coast VNA & Hospice today. Call us at 831‑372‑6668 or visit us at ccvna.com to request a nurse consultation.
Frequently Asked Questions About Home Health Care
When you're looking into care options, many questions come up. Families want to feel sure they're making the right choice.
Here are some of the most common questions we hear from families across the Central Coast.
What happens during a typical home health visit?
A home health visit is a focused medical appointment in your living room. It is led by a licensed clinician like a Registered Nurse or a Physical Therapist. The visit is built around the health goals in your parent’s care plan.
During a visit, the clinician might check vital signs, provide wound care, or guide your parent through therapy exercises. They also review medications and teach you about symptoms to watch for. It's active, skilled care designed to move your parent toward independence.
How is home health different from private-duty care?
This is an important distinction. Home health care is skilled medical care prescribed by a doctor and often covered by Medicare. It is delivered by licensed clinicians to help someone recover from an illness or surgery.
Private-duty home care is non-medical assistance with daily activities like bathing or meals. These services are paid for out-of-pocket and are for long-term support.
How long will my parent receive home health services?
The length of time is tied to medical needs and recovery goals. It is not a permanent arrangement.
Services continue as long as there is a medical reason and your parent is showing progress. Once the goals in the care plan are met, the services are completed.
Who is part of the home health care team?
Your parent’s care is a coordinated team effort. The professionals involved depend on the doctor's orders. This team-based approach looks at the whole picture of their recovery.
A typical team is led by a Registered Nurse case manager. It can also include Physical Therapists, Occupational Therapists, Speech-Language Pathologists, Medical Social Workers, and Home Health Aides. At Central Coast VNA & Hospice, this team works with your parent's primary doctor.
How do we get started if my parent is already home?
You do not need a hospital stay to start home health care. If you notice your parent is struggling, you can be proactive.
The first step is a call to their primary care physician. Explain what you've seen and ask for a home health evaluation. The doctor can then order services from a Medicare-certified agency like Central Coast VNA & Hospice.
If you're in Monterey, San Benito, Santa Cruz, or South Santa Clara County, the team at Central Coast VNA & Hospice is ready to help.
Give us a call today at 831-372-6668 or visit us online at ccvna.com to request a conversation.
Why Home Health Isn’t 24-Hour Care and What to Do Instead
When a doctor prescribes home health care for a loved one, many families feel a sense of relief. They often assume it means a skilled professional will be in the home around the clock.
However, the reality is quite different. Home health provides intermittent, skilled medical care, not 24-hour supervision. Understanding this difference is the first step to building a safe and complete support system at home.
The Misconception of Around-The-Clock Home Health Care
 home health nurse arrives to visit an elderly man sitting on a sofa with medication." />
home health nurse arrives to visit an elderly man sitting on a sofa with medication." />Many families assume that once home health care starts, a nurse or aide will be in the home for daily help. They might expect support with things like bathing, cleaning, and cooking every day.
But this is a common misunderstanding. Home health is designed to deliver targeted medical treatments and therapies. It helps a patient recover from an illness, injury, or surgery.
Think of a home health clinician—like a Registered Nurse or Physical Therapist—as a specialist making a focused house call. Their visit has a clear medical goal. This could be changing a surgical dressing, giving a complex injection, or guiding a patient through therapy exercises.
Scheduled Visits, Not Constant Presence
Home health visits are scheduled for specific times and are not continuous. They typically last from 30 minutes to a couple of hours, depending on the patient's care plan.
The goal is to provide expert medical support and teach the patient and family how to manage care. This model is about empowering patients to regain independence, not providing constant supervision.
The structure of home health is also defined by insurance rules. Medicare, which covers most home health services, sets clear limits. Recent insights show that home health under Medicare includes only intermittent skilled services like wound care, injections, therapy, and condition monitoring.
According to Medicare, skilled nursing is strictly limited to up to 8 hours per day or 28 hours per week. In rare cases, a doctor may request up to 35 hours, but this is for short-term recovery for homebound patients. You can learn more by exploring these home health statistics and regulations.
A Local Partner in Care Navigation
For over 74 years, Central Coast VNA & Hospice has helped families navigate these challenges. We serve communities across Monterey County, San Benito County, Santa Cruz County, and South Santa Clara County.
As a local nonprofit, our mission is to provide compassionate guidance. We help families understand that while our clinicians provide essential medical care, you may need to add other support to keep your loved one safe and comfortable.
What a Typical Home Health Plan Actually Provides

So, what does a home health plan look like day-to-day? Think of it as a team of medical specialists making house calls, not a constant companion.
A typical plan includes a series of visits from clinicians. Each visit has a specific goal to help a patient recover and regain independence at home.
This model is built on intermittent skilled care. This means clinicians visit for scheduled periods to perform tasks requiring their professional expertise. The goal is to provide medical help, track progress, and teach the family how to manage care between visits.
Meet Your Clinical Team
At Central Coast VNA & Hospice, our team works together to create a seamless care experience. Your loved one’s doctor-prescribed plan might include several specialists:
- Registered Nurse (RN): The RN often leads the team, overseeing the care plan. They handle tasks like wound care, managing IVs, and teaching you about a chronic condition.
- Physical Therapist (PT): A PT helps patients rebuild strength, improve balance, and move safely after a surgery, fall, or stroke.
- Occupational Therapist (OT): An OT helps patients regain the ability to do daily tasks like getting dressed, cooking a meal, or bathing.
- Speech-Language Pathologist (SLP): An SLP provides therapy to improve swallowing or communication after a stroke or illness.
- Home Health Aide (HHA): Working under an RN's supervision, an HHA may help with personal tasks like bathing as part of a skilled nursing care plan.
Each professional plays a vital role in recovery. To learn more about what our nurses do, you can read about what skilled nursing care entails on our website.
Focused on Recovery, Not Replacement
The purpose of home health is to prevent rehospitalization and improve health. It is not meant to replace the role of a family member.
Our clinicians teach, treat, and monitor. They do not stay to cook meals, do laundry, or provide companionship around the clock.
This table clarifies what is included in home health versus personal care.
| Service Category | Included in Home Health (Skilled Care) | Not Included in Home Health (Personal/Custodial Care) |
|---|---|---|
| Medical Tasks | Wound dressing, medication administration, IV therapy, disease management education. | Reminding to take medication, organizing pillboxes. |
| Therapy | Physical, occupational, and speech therapy sessions to restore function. | General exercise or walking assistance. |
| Personal Care | Bathing assistance if part of the skilled plan and supervised by a nurse. | Daily bathing, dressing, and grooming support. |
| Household Tasks | Not included. | Meal preparation, light housekeeping, laundry, running errands. |
| Companionship | Not included. | Social interaction, accompanying to appointments, supervision. |
Home health is strictly medical and therapeutic. For other daily needs, a different type of care is required.
What this actually means is that home health is medical care, not daily caregiving. Families may still need to coordinate transportation, meal prep, or private duty care on their own—especially for seniors living alone.
By coordinating expert visits, the Central Coast VNA & Hospice team helps patients in Monterey, Salinas, Hollister, and Santa Cruz achieve the best results. Our approach ensures every medical need is addressed, creating a strong foundation for recovery.
Understanding the Financial Reality of 24 Hour Care
Beyond the clinical reasons, the cost of continuous professional care is a major barrier. For most families, paying for 24-hour care is not realistic.
When you receive skilled home health from a Medicare-certified provider like Central Coast VNA & Hospice, the cost is often $0 out-of-pocket. This is because Medicare and other insurance plans cover these intermittent medical visits.
But the financial picture changes for continuous, non-medical support.
The True Cost of 24/7 Support
Hiring professional aides to be present 24 hours a day means covering multiple shifts. The costs add up quickly.
The numbers can be surprising. The U.S. median cost for 24/7 home care is about $30 per hour. Let's break that down:
- Daily: $720
- Weekly: $5,040
- Monthly: Over $21,000
As you can see from these insights on 24-hour care costs, this amount is often much higher than a nursing home.
For most families, paying over $260,000 annually for at-home care is not a realistic option. This is why the healthcare system separates intermittent medical care from continuous custodial support.
This highlights a key economic challenge. Skilled home health is a covered medical need, while 24-hour supervision is considered a long-term custodial need that insurance typically does not pay for.
Navigating Your Financial Options
Seeing these numbers can feel overwhelming, but it’s the first step toward a realistic care plan. The goal is to find a balance between what is medically necessary and financially possible.
Often, the solution involves blending different types of support. Families can use Medicare-covered home health for skilled needs while finding other resources for daily assistance.
At Central Coast VNA & Hospice, we understand these financial questions. As a nonprofit serving our community for over 74 years, we are committed to helping families in Monterey, San Benito, Santa Cruz, and South Santa Clara counties find practical solutions.
For a deeper look at managing these expenses, our guide on how to fund home health care costs offers more detail.
Finding Practical Alternatives for Continuous Support

Once you realize home health is not 24-hour care, the next step is building a complete safety net. You need a solution that blends skilled medical care with hands-on daily support.
Fortunately, many excellent options can be layered on top of visits from your Central Coast VNA & Hospice clinical team. This approach ensures every need is met without gaps.
Building Your Support System
Crafting a comprehensive care plan often means combining different services. This layered approach allows you to address specific needs safely and affordably.
Here are some effective ways to fill the gaps:
- Private-Duty Aides: These aides are hired to help with non-medical tasks, or Activities of Daily Living (ADLs). They can assist with bathing, meals, light housekeeping, and companionship.
- Adult Day Programs: These centers offer a safe, supervised place for seniors during the day. They provide social activities, meals, and some health services.
- Respite Care: Family caregiving is a demanding role. Respite care provides short-term relief, allowing you to rest and recharge.
For families here in Monterey County and surrounding areas, knowing your options is key. You can learn more about respite care for family caregivers and see how it can support your well-being.
Considering Live-In and 24/7 Care
For those who need round-the-clock supervision, it's important to understand the difference between live-in and 24/7 care.
A live-in aide lives in the home and has dedicated periods for sleep and personal time. In contrast, true 24/7 care involves multiple aides working in shifts to ensure someone is always awake and available.
The cost difference is significant. While a live-in aide is a major expense, 24/7 shift care is often far more costly.
For many families, the most effective strategy is to combine skilled home health for medical needs with non-medical private aides for daily activities like meals, personal care, and companionship. This integrated approach ensures comprehensive support without the extreme costs of 24/7 skilled nursing.
For example, a live-in aide usually gets 8-12 hours off daily plus a few days off per week. On the other hand, 24/7 shift care can cost up to $24,090 per month. Blending skilled visits with private aides creates a safer and more affordable plan.
Adding Another Layer of Support with Palliative Care
When a loved one has a serious illness, managing symptoms like pain or anxiety can be challenging. This is where palliative care can make a profound difference.
Palliative care is specialized medical care focused on relief from the symptoms and stress of a serious illness. It can be provided alongside home health and curative treatments.
The goal is to improve the quality of life for both the patient and the family. At Central Coast VNA & Hospice, our palliative care team works with your primary doctor to add an extra layer of expert support. Central Coast VNA & Hospice can help you explore if palliative care is the right choice for your family.
When Hospice Is the Right Choice for 24/7 Support
For families seeking true around-the-clock support, hospice is often the answer. While routine hospice care involves intermittent visits, it includes a crucial safety net. This includes having a clinical team on call 24 hours a day, 7 days a week.
The most significant difference appears during a crisis. Hospice provides specialized care to manage intense symptoms at home, offering an alternative to a stressful hospital trip.
Continuous Home Care for Acute Symptoms
This unique service is called Continuous Home Care (CHC). It is one of the four levels of care required by Medicare for all hospice providers.
When a patient has a medical crisis—like severe pain or breathing difficulties—the hospice team can provide short-term, round-the-clock nursing care at home.
A Registered Nurse or Licensed Vocational Nurse will stay at the bedside for extended periods. They deliver skilled care until the symptoms are under control.
Continuous Home Care isn't a long-term 24/7 solution. It is a short-term, intensive intervention to stabilize a patient in their familiar surroundings, avoiding rehospitalization and bringing rapid relief.
This responsive, in-home support is a key part of hospice care and is not available through traditional home health. It is essential to know when hospice is the most appropriate choice. To help, you can learn more about end-of-life services.
More Than Just Medical Support
Beyond physical symptoms, hospice provides a complete support system for the whole person. At Central Coast VNA & Hospice, our interdisciplinary team brings this support to families across Monterey, San Benito, Santa Cruz, and South Santa Clara counties.
Our hospice services include:
- Expert Medical Care: Our physicians and nurses specialize in pain and symptom management.
- Emotional and Spiritual Support: Chaplains and Medical Social Workers help patients and families navigate complex emotions.
- Practical Assistance: Hospice Aides can assist with personal care, while volunteers provide companionship and respite.
This holistic approach brings peace of mind. Knowing when to make this decision can be tough, and our guide on when to call hospice offers clear advice.
Building a Comprehensive and Realistic Care Plan
Creating a care plan that works starts with seeing the whole picture of your loved one’s needs. Proactive planning and clear communication are your best tools.
When you start with a home health provider, ask direct questions. Good communication prevents surprises and makes sure everyone is on the same page.
Key Questions for Your Provider
To build a solid foundation, ask your home health agency these crucial questions. This is an actionable step to help you plan effectively.
- What exactly will your clinicians do? Get a specific list of what the nurse, therapist, and aide will and won't do.
- What’s the real visit schedule? Ask for the frequency and length of visits to help you plan.
- How do we handle after-hours issues? Understand the process for reaching a clinician for urgent needs.
- What should we be watching for? Ask what symptoms or changes might require a call to the team.
Facing home health's limitations is the first step. The next is building a comprehensive family care plan that covers everything.
This decision tree helps visualize the two main paths for at-home support.
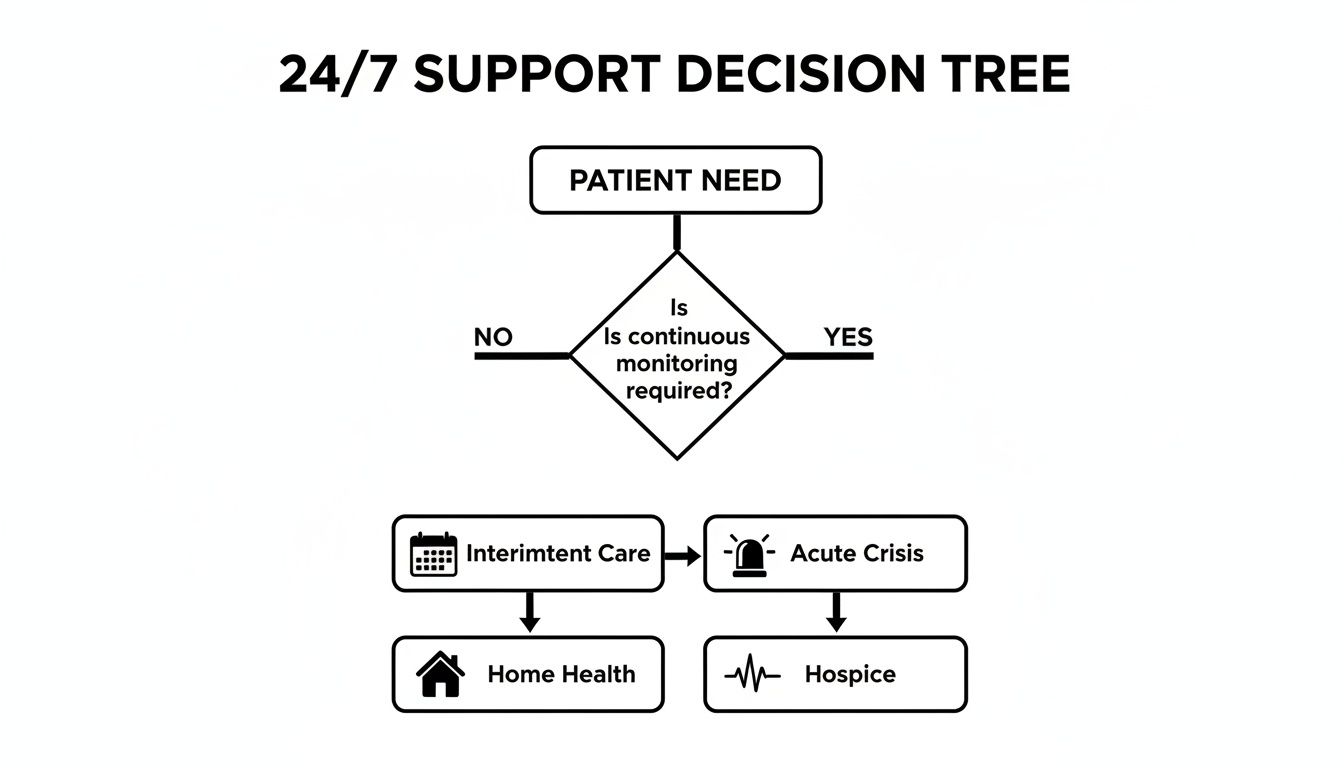
Home health is the answer for scheduled, intermittent medical needs. But for acute symptoms or an end-of-life crisis, hospice is the more appropriate choice.
Creating a Holistic Plan
True peace of mind comes from a plan that supports the whole person. Look beyond the diagnosis to your loved one’s emotional and social well-being.
At Central Coast VNA & Hospice, our role is to help families in Monterey, Salinas, Hollister, and Santa Cruz navigate this journey. With over 74 years of local service, we know great care is more than medicine. We also offer guidance on end-of-life care planning.
Ask your provider early on what's covered, how often clinicians will visit, and whether other services like palliative care are available. Planning ahead prevents gaps in care.
FAQs: Your Home Care Questions, Answered
Arranging medical support at home for a loved one can bring up many questions. Getting clear answers is the first step toward making confident decisions.
1. Does Medicare pay for 24-hour care at home?
No, Medicare generally does not cover 24-hour personal care at home. The Medicare home health benefit is designed for intermittent, skilled medical needs, like a nurse visiting for wound care. It is not set up for continuous supervision.
2. What is the difference between a Home Health Aide and a private aide?
A Home Health Aide from a certified agency like CCVNA works under a Registered Nurse's supervision. They assist with personal tasks as part of a medical care plan. A private aide is hired by you to help with daily living activities like meals, companionship, and errands.
3. How do I know if my loved one needs palliative care?
If your loved one has a serious illness and struggles with symptoms like chronic pain, fatigue, or anxiety, palliative care can help. It focuses on improving quality of life and can be provided alongside home health and other treatments.
4. Can we receive CCVNA services in an assisted living facility?
Yes, absolutely. Our teams provide home health, palliative, and hospice care wherever our patients call home. This includes private homes, assisted living communities, and skilled nursing facilities throughout Monterey, San Benito, Santa Cruz, and South Santa Clara counties.
5. What is our first step if we need more support?
Your best first step is to have an open conversation with your current home health provider. Ask for a clear breakdown of the visit schedule and covered services. This will help you identify gaps and figure out what additional support you need to arrange.
If you’re managing a loved one’s care in Monterey, Salinas, Hollister, or Santa Cruz and need help understanding what home health includes, Central Coast VNA & Hospice can guide you. Visit ccvna.com or call 831‑372‑6668 to talk to a nurse today.
Using Telehealth in Hospice and Palliative Care: Comfort and Connection at Home
Using telehealth in hospice and palliative care adds an extra layer of support for patients and families. It uses technology like video calls and remote monitoring to supplement, but never replace, in-person care.
This approach gives families timely symptom management and connects loved ones who are far away. It also reduces stress by ensuring compassionate support from a Registered Nurse or Hospice Aide is always just a click away.
What Telehealth for Hospice Really Looks Like

When families first hear "telehealth," they might picture complicated, impersonal gadgets. The reality is much simpler and warmer. Think of it as a way to extend the compassionate reach of our care team.
For families here on the Central Coast, telehealth blends seamlessly with our traditional, hands-on care. It’s not about replacing the human touch of a Hospice Aide or the clinical expertise of a Registered Nurse. It’s about adding crucial moments of connection between those essential home visits.
Extending Compassionate Care Virtually
Telehealth in hospice can take many forms, each designed to make life easier. This virtual support is built around familiar technology, so it feels accessible and not intimidating.
Here’s what this kind of support often includes:
- Virtual Check-Ins: A quick video call with a nurse can help manage a new symptom or answer a question. This immediate access can prevent discomfort from worsening and may even help avoid a stressful ER trip.
- Family Care Conferences: Telehealth allows family members—whether they’re in Monterey County or across the country—to join important care discussions. Everyone can stay connected and involved in decision-making.
- Emotional and Spiritual Support: A video chat with a Medical Social Worker or Chaplain creates a private space for comfort. This support is available from the familiarity of home.
- Digital Symptom Tracking: Simple tools allow a patient or family member to report symptoms like pain or anxiety. This helps our care team adjust the care plan to keep your loved one comfortable.
This approach has proven its value. In fact, 43% of adults 65 and older have used telehealth since the pandemic. This shows that seniors are often more comfortable with digital tools than many assume.
How Technology Supports the Human Connection
A key part of making telehealth work is using the right tools. At Central Coast VNA & Hospice, we ensure this technology is straightforward. Its main purpose is to strengthen the bond between our team, our patients, and their families.
We are dedicated to making our hospice-at-home services as supportive as possible. You can learn more about our approach here: https://ccvna.com/hospice-at-home/.
By integrating telehealth, we honor our 74-year legacy of providing compassionate, local care. We serve Monterey County, San Benito County, Santa Cruz County, and South Santa Clara County. We're committed to ensuring every family feels connected, whether we’re with them in person or online.
Enhancing Quality of Life with Virtual Support
For many families, a top priority is ensuring their loved one is comfortable and at peace. Telehealth brings expert hospice and palliative support right into the home. This helps preserve a patient's energy and gives them a greater sense of control.
Think about a patient in Monterey County with an advanced illness. Instead of tiring trips to a clinic, they can have regular video check-ins with their Nurse Practitioner. These calls allow the care team to fine-tune medications and manage symptoms before they become a crisis.
This proactive care helps patients feel more comfortable and empowered. It also saves precious energy that’s better spent on creating memories with loved ones.
Providing Consistent Emotional and Spiritual Comfort
A serious illness affects a person's emotional and spiritual health. It's normal for patients and families to feel anxiety, fear, and uncertainty. Telehealth provides a direct line to the compassionate support needed to navigate these feelings.
A video call with a Chaplain or a Medical Social Worker can feel just as personal as a face-to-face meeting. It creates a safe, private space to talk through worries from the comfort of home. For so many, getting this support without leaving their favorite armchair makes a huge difference.
This isn’t just a feeling; it’s backed by research. A study found that video consultations for patients with advanced lung cancer provided nearly identical quality-of-life benefits as in-person care. You can learn more about these powerful findings on cancertodaymag.org.
Fostering Shared Decision-Making for Families
Telehealth also acts as a crucial bridge for families spread across different locations. It ensures everyone can be part of important conversations. This builds a strong sense of connection and shared decision-making.
A daughter in another state can join a video call with her father and his palliative care nurse. This inclusive approach has real advantages. It leads to clearer communication and gives everyone a chance to ask questions and decide on the best path forward.
For families in Santa Cruz County or San Benito County, the first step is understanding how these services can help. Our team is here to explain how our palliative home care uses technology to improve comfort. By blending hands-on visits with virtual check-ins, we offer a more responsive and personalized experience.
How We Make Telehealth Simple and Accessible
We know that bringing new technology into your home can feel overwhelming. That’s why we’ve made our telehealth process simple and supportive. Our goal is to make care in Monterey County and surrounding areas more accessible, not more complicated.
Many families worry about setting up strange devices or learning confusing software. Our team ensures that using telehealth feels as natural as a phone call with a trusted friend.
Getting Started with Virtual Care
For families trying telehealth for the first time, the setup couldn't be easier. We provide everything needed to get started with total confidence. Our approach is hands-on and tailored to your loved one’s comfort.
Here’s how we make the process worry-free:
- We Provide the Tech: If you need it, we’ll deliver a pre-configured tablet to your home. Everything is set up and ready to use.
- Personalized Guidance: A member of our team will personally walk you through the first virtual call. We’ll show you exactly how it works and answer every question.
- Ongoing Support: Should any technical issues pop up, our team is just a phone call away. You’ll never have to troubleshoot a connection problem on your own.
This whole process is designed to bring comfort and support right into your home.
A Look at Our Virtual Services
Once you’re set up, you’ll have an added layer of compassionate care. These virtual services complement the essential in-person visits from our Registered Nurses and Hospice Aides. It's a powerful way we use telehealth in hospice and palliative care.
Our virtual support includes several key services:
- Routine "Tuck-In" Calls: These are brief video check-ins from a nurse to see how your loved one is feeling. They provide regular reassurance between our scheduled home visits.
- Video Consultations for Adjustments: If a new symptom appears, a quick video call with a Nurse Practitioner can provide a timely assessment. This allows us to make immediate changes to the care plan.
- Simple Symptom Tracking: We also offer easy-to-use digital tools for tracking things like pain. This gives our clinical team real-time data to better manage your loved one’s comfort.
Central Coast VNA & Hospice has been a pillar of this community for over 74 years. Adopting telehealth is another way we fulfill our nonprofit mission. You can learn more about our technology by exploring our user-friendly VNA&CS tablets.
Keeping Long-Distance Families Connected

When a loved one is seriously ill, it's hard not to be there in person. For adult children living outside of Monterey County or Santa Cruz County, that distance can cause stress. Telehealth is a bridge across that gap, turning long-distance relatives into active members of the care team.
Our approach uses technology to make sure families feel connected and heard. It helps lift the emotional weight that comes with managing care from afar.
Bridging the Miles with Virtual Presence
Imagine your mother is receiving palliative care in her Salinas home, but you live hundreds of miles away. Telehealth lets you join a video conference with her and her Central Coast VNA & Hospice Registered Nurse.
You get to see her face and hear the nurse’s insights firsthand. This face-to-face connection brings a level of clarity and reassurance that a simple phone call can’t match.
Staying Informed with Secure Updates
Telehealth also offers other ways to stay connected without interrupting your loved one's day. We use secure messaging platforms and family portals to send quick notes. This might be an update about a medication change or a short message to let you know your parent had a comfortable day.
These small, consistent updates provide immense peace of mind. They keep you in the loop and reduce the anxiety of the unknown.
A Real-Life Scenario in Action
Here’s a common situation:
- The Patient: An 82-year-old man in Hollister is on our hospice service.
- The Family: His son lives in another state, and his daughter lives an hour away with a demanding job.
- The Solution: The family joins a weekly video call with our Medical Social Worker to discuss emotional support. Between calls, the son uses a secure portal to ask non-urgent questions, and the daughter gets quick text updates.
This integrated system keeps everyone on the same page. It supports collaboration and strengthens family bonds during a tough time.
We know that navigating elderly care from a distance is a challenge. Sometimes, families also want to show support through symbolic gestures. Resources like A Thoughtful Guide to Choosing Flowers for a Funeral can be helpful.
At Central Coast VNA & Hospice, our mission has always been to care for the whole family. By using technology to bring loved ones closer, we extend our compassionate care beyond the physical walls of a home.
Knowing When Virtual and Hands-On Care are Needed
It’s important to see telehealth as a tool that adds to, but never replaces, hands-on clinical care. While virtual visits offer flexibility, they work hand-in-hand with the in-person expertise of our local team. This balanced approach is at the heart of our 74+ years of service.
Our team, including your Registered Nurse and Hospice Aide, carefully decides when a face-to-face visit is best. Certain needs will always be met in person to ensure your loved one’s safety, comfort, and dignity.
When In-Person Care Is Essential
A video call is perfect for a quick check-in, but some situations require a physical presence. Our deep local roots in Monterey County, San Benito County, and Santa Cruz County make a difference. Our clinicians are your neighbors, ready to provide direct, hands-on support.
Here are examples of care that will always be provided in person:
- Hands-On Wound Care: A skilled clinician needs to be physically present to clean, dress, and monitor wounds properly.
- Assistance with Personal Hygiene: Our compassionate Hospice Aides provide essential help with bathing and dressing to preserve comfort and dignity.
- Complex Symptom Assessments: Evaluating complex symptoms often requires a physical examination by one of our Registered Nurses.
- Support During a Crisis: Having a Chaplain physically present during intense emotional or spiritual moments offers support that technology cannot replicate.
This hybrid model blends the efficiency of virtual check-ins with the irreplaceable value of human touch.
A Proven Approach to Better Outcomes
Bringing telehealth into palliative care isn't just about convenience. It leads to real improvements for patients and families. Studies have shown this blended approach can lead to fewer hospitalizations and lower psychological distress.
Globally, telehealth is an essential tool for filling critical gaps in care. You can read more about these telehealth findings in a comprehensive review.
This is especially true for families in the rural parts of the Central Coast. For them, virtual visits can mean less travel and reduced risk of infection. At Central Coast VNA & Hospice, our dedicated local team is available 24/7 for any urgent needs.
Frequently Asked Questions About Telehealth in Hospice Care
1. Is telehealth secure and private for hospice patients?
Yes. We use secure, HIPAA-compliant platforms for all virtual communications. Your loved one's personal health information is always encrypted and protected, ensuring every conversation remains confidential.
2. What if my parent isn’t comfortable with technology?
We understand this concern. Our approach is built around simplicity and support. If needed, we provide a pre-configured tablet and a team member will visit to walk your loved one through their first call.
3. Does using telehealth mean we’ll see nurses less often?
Not at all. Telehealth adds more support; it doesn't replace it. Your loved one will continue to receive all necessary in-person visits from our Registered Nurses and Hospice Aides for hands-on care.
4. Can family from different locations join a call?
Yes, this is one of the greatest benefits. We can schedule virtual family meetings that allow relatives from anywhere to join a single video call with your loved one and our clinical team.
5. How do I know if telehealth is a good option for my family?
The best way to know is to have a conversation with our team. We will work with you to develop a personalized care plan that blends in-person visits with virtual support, based on what will best enhance your loved one’s comfort and quality of life.
At Central Coast VNA & Hospice, we are dedicated to providing compassionate care that supports the whole family. If you're supporting a loved one on the Central Coast, our team can explain how telehealth works alongside our essential hands-on care. Contact us today to explore what’s possible—virtual, in-person, or both. Learn more at https://ccvna.com.
What’s the Difference Between Home Care and Senior Care Services?
When a loved one needs more help, families often search for "senior care." But what does that term really mean? It can feel overwhelming to sort through options like home care, nursing homes, and therapy.
Getting the terms right is the first step to finding the support you need. Home care is skilled medical care from licensed professionals, ordered by a doctor. Senior care is a broad term for non-medical help, like companionship or assistance with daily tasks.
Understanding the Core Differences in Senior Support

Trying to figure out care options for a family member can be confusing. Many families in Monterey County and surrounding areas search for “senior care” without realizing it covers everything from a few hours of help to 24/7 medical support. Let’s clear things up.
Home care, often called “home health care,” is a specific type of medical service. It helps someone recover from an illness, injury, or surgery at home. A team of licensed clinicians provides this care.
In contrast, "senior care" includes almost any service that helps older adults live safely. This could be non-medical help with cooking and cleaning or even moving to a residential facility. It’s all about assistance with daily life, not clinical treatment.
Home Care vs. Senior Care at a Glance
One option isn’t better than the other; they just serve different purposes. The right choice depends entirely on your loved one’s health needs. Making an informed decision starts with knowing the difference.
This table breaks down the key distinctions.
| Key Aspect | Home Care (Clinical Focus) | Senior Care (Broad Category) |
|---|---|---|
| Primary Goal | To treat a medical condition, aid in recovery, or manage a chronic illness. | To provide support for daily living, ensure safety, and offer companionship. |
| Service Provider | Licensed medical professionals (e.g., Registered Nurses, Physical Therapists). | Non-medical aides, companions, or staff at residential facilities. |
| Common Services | Wound care, medication administration, physical therapy, skilled nursing. | Meal preparation, light housekeeping, transportation, assistance with bathing. |
| Who Prescribes It | A physician's order is required to initiate services. | Typically arranged directly by the family or individual based on need. |
| Payment Source | Often covered by Medicare, Medi-Cal, and private insurance. | Usually paid for privately or with long-term care insurance. |
Think of it this way: if a doctor orders it and a licensed clinician provides it, it’s home health care. If it's about making daily life easier and safer, it falls under the senior care umbrella.
As a nonprofit serving the Central Coast for over 74 years, Central Coast VNA & Hospice specializes in clinical care. Our continuum of home health and hospice services helps families build a care plan that fits their medical needs, so no one feels unprepared.
A Deeper Look at Clinical Home Care Services

Clinical home care, or home health, is a specific medical service prescribed by a physician. It is not about companionship or errands. It’s about licensed healthcare professionals delivering skilled medical care in a patient's home.
These services are part of a formal care plan, often after a hospital stay or surgery. The goal is recovery, rehabilitation, and helping patients regain independence. For over 74 years, Central Coast VNA & Hospice has provided this expert care to our community.
Who Provides Clinical Home Care
The qualifications of the professionals involved is a major difference between home care and senior care. A team of licensed clinicians delivers home health care. Each person plays a specific role in the patient's recovery.
This team often includes:
- Registered Nurses (RNs) who manage complex needs like wound care, IV therapy, and patient education.
- Physical Therapists (PTs) who guide patients through exercises to rebuild strength and balance after an injury.
- Occupational Therapists (OTs) who help individuals relearn daily activities like dressing or cooking safely at home.
- Speech Therapists (STs) who work on communication or swallowing difficulties, often after a stroke.
- Medical Social Workers who connect families with community resources and provide emotional support.
Real-World Scenarios for Home Care
Let’s look at a few common situations to see how home care works. Imagine a patient in Salinas recovering from joint replacement surgery. A Physical Therapist would help them regain strength and learn to navigate stairs at home.
Here’s another example: a patient in Hollister is newly diagnosed with heart failure. A Registered Nurse from Central Coast VNA & Hospice would visit to monitor vital signs and manage medications. To learn more about this role, see what is skilled nursing care.
According to the Alliance for Home Health Quality and Innovation, patients receiving home health care show significant improvement in their ability to perform daily activities. This highlights its powerful role in rehabilitation.
Nearly 12 million Americans receive home health care services annually. As a mission-driven, nonprofit provider, Central Coast VNA & Hospice ensures this essential care remains accessible in Monterey County, San Benito County, and our other service areas. You can get more insight into these roles by learning about working in home health care as a CNA.
Digging Into the World of Senior Care
While home care focuses on medical needs, "senior care" covers a wide range of non-medical services. It’s designed to support an older adult's safety, comfort, and quality of life. Think of it as help with practical, everyday challenges.
This is often the first place families on the Central Coast look when a loved one starts to struggle. These services are arranged privately and are not prescribed by a doctor. The goal is to provide a helping hand and peace of mind.
What Does Non-Medical Senior Care Actually Look Like?
Non-medical senior care is a flexible spectrum of support. It can be customized to fit a person’s unique needs and preferences. This allows families to build a support system that truly works.
These services generally fall into two categories:
- Companion Care: This focuses on social interaction and help with household tasks. It’s ideal for seniors who are independent but could use company to prevent loneliness or help with errands.
- Personal Care: This involves more hands-on help with Activities of Daily Living (ADLs). A personal care aide can assist with bathing, dressing, and moving around safely.
Many families start by exploring in-home care for seniors to help their loved one stay safely at home.
How Clinical and Non-Medical Care Work Together
It is common for someone to need both skilled medical care and non-medical support. This is where a team approach becomes essential. For instance, a patient in Monterey recovering from a stroke might get physical therapy from a Central Coast VNA & Hospice clinician while a non-medical aide helps them with meals.
By combining services, families can create a complete safety net. The clinical team addresses medical recovery, while a non-medical aide ensures daily life continues smoothly.
As a nonprofit provider with deep roots on the Central Coast, we see how vital this collaboration is. Our clinical teams coordinate with non-medical providers across Salinas, Santa Cruz, and Hollister. We work together to ensure a patient’s care plan covers every need.
How to Choose the Right Level of Care
Choosing the right support for a loved one is a big decision. The best approach is to focus on what they need right now. A clear, step-by-step process helps you make a proactive choice instead of waiting for a crisis.
Start with a simple needs assessment: is the primary need medical or non-medical? If your loved one is recovering from surgery or managing a chronic illness, the answer is medical. In this case, home health care, prescribed by a doctor, is the right path.
If they are medically stable but struggling with daily tasks, their needs are non-medical. These issues are a good fit for senior care services like companion or personal care.
Matching Services to Specific Scenarios
Seeing how these services work in real life makes the choice clearer. Let's look at a few common situations we see with families on the Central Coast.
-
Scenario 1: Post-Surgery Rehabilitation
A Santa Cruz resident is home after a hip replacement. They need help managing pain and learning to use a walker safely.- Correct Choice: Clinical Home Care. A Registered Nurse from Central Coast VNA & Hospice can manage wound care, while a Physical Therapist provides in-home rehab.
-
Scenario 2: Managing a Chronic Condition
An older adult in Salinas with congestive heart failure needs help to stay out of the hospital. They have a complicated medication schedule.- Correct Choice: Clinical Home Care. A skilled nurse can teach them about their condition, monitor vital signs, and work with their doctor.
-
Scenario 3: Early-Stage Dementia Support
Someone in Hollister is physically healthy but showing signs of memory loss. They sometimes forget to eat and can no longer drive safely.- Correct Choice: Non-Medical Senior Care. A companion can offer supervision, prepare meals, and provide transportation to keep them safe and socially connected.
This decision tree helps show the difference between companionship and personal care needs when choosing non-medical senior care.
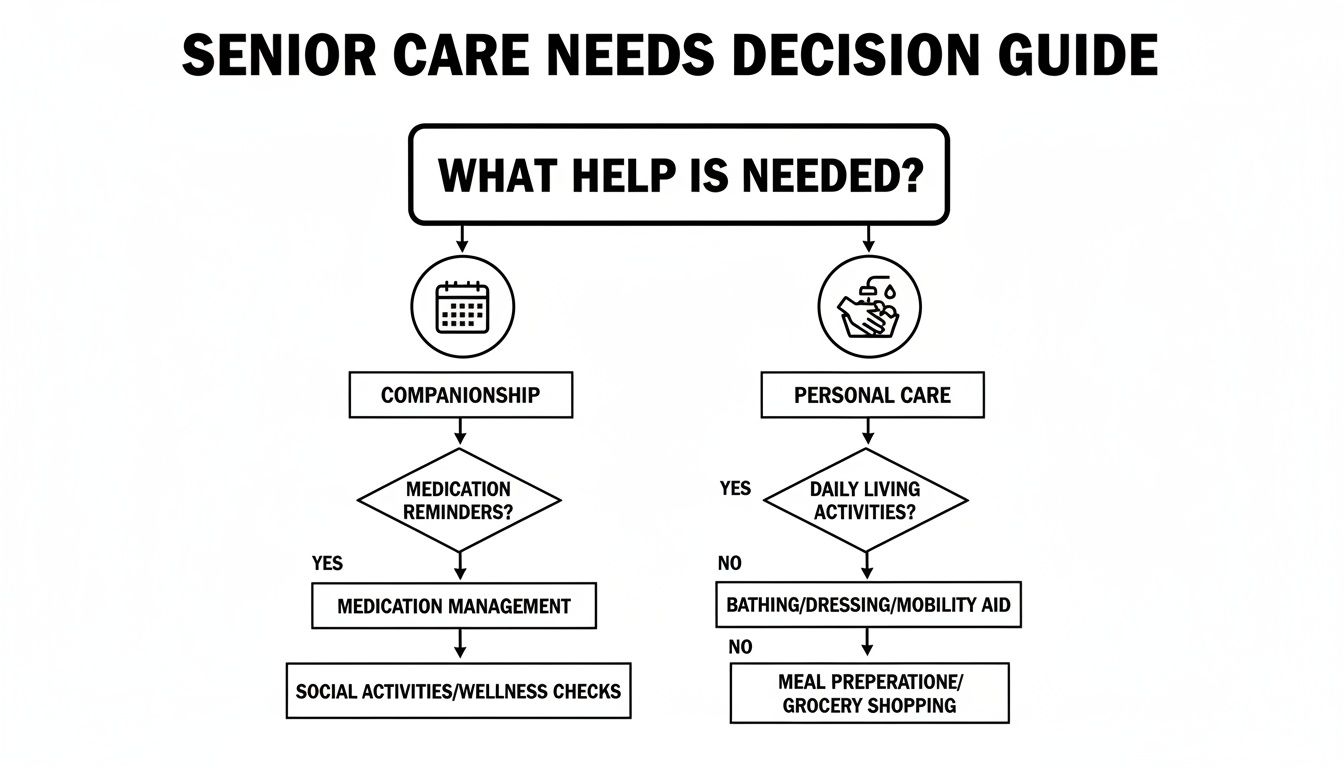
As the flowchart shows, the first step is to figure out the specific type of daily help required. This will determine if social engagement or hands-on assistance is needed.
When Both Types of Care Are Needed
Life is rarely simple, and a person's needs often require a blend of support. A layered approach is important in these cases. The most effective care plans often combine both clinical and non-medical services.
The most successful support systems are built by layering services. A patient can receive skilled nursing from Central Coast VNA & Hospice while also having a non-medical aide assist with meals.
This combination ensures all bases are covered. A licensed clinician handles medical needs, while a non-medical aide supports daily living. This strategy prevents family burnout and creates a complete safety net.
Figuring out the financial side is also a big piece of the puzzle. Exploring resources on topics like Understanding Grants for Senior Citizens can provide valuable insights.
Integrating Services for a Complete Support System

A person’s care needs change over time. The key to effective support is a flexible system that layers services together. This creates a complete safety net at home.
Many families think they must choose between medical and non-medical care. In reality, the best plans often blend both. This ensures clinical needs are managed by professionals while daily needs are also supported.
As the only nonprofit on the Central Coast providing a full continuum of care, Central Coast VNA & Hospice guides families through this journey. Our teams in Monterey, San Benito, Santa Cruz, and South Santa Clara counties create personalized, adaptable care plans.
Building a Personalized Continuum of Care
The path of care is different for everyone. At Central Coast VNA & Hospice, our teams build a pathway of support that evolves with the patient. This ensures the right care is always available without the stress of finding new providers.
Our integrated model might look like this:
- Starting with Home Health: A patient in Salinas might begin with skilled nursing and physical therapy to focus on recovery.
- Transitioning to Palliative Care: If a serious illness progresses, they could move to our specialized palliative home care. This service focuses on managing symptoms and improving quality of life.
- Receiving Hospice Support: Later, if their illness is terminal, they can seamlessly transition to our compassionate hospice care. The focus shifts to comfort and dignity.
This entire journey is managed under one roof by a team that knows your family. This continuity provides great comfort and eliminates confusion.
The Advantage of a Single, Trusted Provider
Figuring out the difference between home care and senior care services is hard enough. Working with a single, mission-driven organization like Central Coast VNA & Hospice offers clear advantages. Our clinicians communicate with each other, ensuring the care plan is perfectly aligned.
With over 74 years of dedicated service, our nonprofit model allows us to focus entirely on the patient. We help families build a comprehensive plan so no one feels alone or unprepared.
Our Registered Nurses might identify when a patient could benefit from palliative support for pain. In the same way, our hospice team can bring in volunteers and bereavement specialists to support the entire family. This cohesive approach ensures nothing is missed.
Your Trusted Partner for Care on the Central Coast
Figuring out senior care options can feel overwhelming, but you don't have to do it alone. For over 74 years, Central Coast VNA & Hospice has been a dedicated nonprofit partner for families across Monterey, San Benito, Santa Cruz, and South Santa Clara counties. We are your neighbors, committed to helping you find the right support.
Our mission is to bring compassionate, high-quality healthcare to your doorstep. Whether you’re in Salinas, Monterey, Hollister, or Santa Cruz, our skilled clinicians are part of this community. Our focus is entirely on our patients' well-being.
Your Local Guide to Senior Care
Understanding the difference between home care and senior care is a huge first step. Our team is here to give you clear, no-obligation guidance. We help families build a care plan that fits their unique situation.
We are the only organization on the Central Coast offering a full continuum of home health, palliative care, and hospice care under one roof. This means we provide seamless support as your loved one's needs change.
Having one integrated team means you have a single, trusted partner. There are no gaps in care, just consistent support from clinicians who know your family. They work together to adjust the plan as needed, giving you peace of mind.
We invite you to learn how Central Coast VNA & Hospice impacts lives across the Central Coast. When you’re ready to explore your options, our team is here to help you move forward with confidence. Contact us today.
Frequently Asked Questions About Home and Senior Care
Figuring out senior support services can be confusing. Here are answers to some common questions we hear from families.
Is Home Care Covered by Medicare?
Yes, but only a specific kind. Skilled home health care—clinical services from a nurse or therapist—is typically covered by Medicare. A doctor must order these services as medically necessary for a patient who is "homebound."
Non-medical senior care, like companionship or meal prep, is usually not covered by Medicare. This type of care is most often paid for out-of-pocket.
Can My Loved One Receive Home Care in an Assisted Living Facility?
Absolutely. A person’s “home” is wherever they live. Our skilled clinicians from Central Coast VNA & Hospice regularly provide home health, palliative, and hospice care to patients in assisted living communities throughout Monterey, San Benito, Santa Cruz, and South Santa Clara counties.
What Is the First Step to Getting Care for My Parent?
Start by talking with your parent's doctor about their health and safety. If they need medical care at home, the doctor can send a referral to a home health agency like ours. You can also call our team directly for guidance.
How Is Palliative Care Different from Home Health or Hospice?
These services represent different points along our continuum of care. Each one has a distinct goal:
- Home Health is doctor-ordered care focused on helping a patient recover from an illness or injury.
- Palliative Care is specialized support focused on relief from the symptoms and stress of a serious illness.
- Hospice Care is for individuals with a terminal illness when comfort and quality of life become the primary goals.
Does Central Coast VNA & Hospice Provide Non-Medical Senior Care?
Central Coast VNA & Hospice is a licensed medical provider specializing in skilled clinical services: home health, palliative care, and hospice care. We do not offer standalone non-medical companion services. However, our Medical Social Workers can connect you with trusted local agencies that provide these services.
At Central Coast VNA & Hospice, our nonprofit mission is to provide compassionate, high-quality healthcare right where you are. If you have more questions or need help building a care plan for your loved one, contact us today. Learn more at https://ccvna.com.
5 Ways to Spot Quality Hospice Care in 2026
Choosing a hospice provider is one of the most important decisions a family can make. It is a choice that shapes the final chapter of a loved one's life. It focuses on comfort, dignity, and peace. As we look toward 2026, the standards for quality hospice care are clearer than ever.
It’s no longer just about medical services. It's about delivering compassionate and holistic support that honors a person's journey. Families across the Central Coast of California need reliable information. This guide will help you spot quality care.
This article focuses on five key areas. We will cover the importance of a coordinated care team, transparent quality data, and 24/7 support. We'll also discuss personalized care plans and official accreditations. With these tools, you can make an informed choice.
1. Look for Transparent Quality Metrics and Patient Satisfaction Scores
When choosing a provider in 2026, quality metrics matter more than ever. Trustworthy providers are open about their performance. They share data from patient and family satisfaction surveys.
Families can review Medicare star ratings and CAHPS (Consumer Assessment of Healthcare Providers and Systems) scores. These scores show how other families rated their experience. Providers with transparent quality data, like Central Coast VNA & Hospice, build trust by showing these results.
According to the National Hospice and Palliative Care Organization (NHPCO), over 1.72 million Medicare beneficiaries received hospice services in 2020 (NHPCO, 2021). This highlights how many families rely on these services and the importance of verified quality. You can learn more about how an interdisciplinary team works in hospice care to deliver this quality care.
What to Look For in Quality Data
High-quality providers don't just collect feedback; they use it. They make real changes based on what families say. This shows a commitment to getting better.
Here are signs of a quality-focused provider:
- Publicly Shared Scores: They share their CAHPS scores and Medicare star ratings on their website or upon request.
- High Satisfaction Rates: Their scores are consistently high, showing that patients and families feel well-supported.
- Clear Improvement Plans: They can explain how they use feedback to improve their services, such as staff training or new communication tools.
Why Verified Metrics are a Non-Negotiable
Verified data gives you an unbiased look at a hospice’s performance. It helps you compare providers on key areas. These areas include pain management, emotional support, and communication.
A hospice confident in its care will share its scores proudly. They see family feedback as a gift, not a critique. This transparency is a key sign of quality.
Actionable Questions to Ask
When evaluating a hospice provider, dig deeper. Use these specific questions:
- Can you share your most recent CAHPS Hospice Survey results with me?
- How do your scores compare to state and national averages?
- Can you give me an example of a change you made based on family feedback?
- What is your process for handling a complaint or concern?
2. Choose a Provider with Local Roots and Community Ties
Where your hospice provider comes from matters. In 2026, the difference between a local nonprofit and a national chain is clear. Local providers often have a stronger connection to the community they serve.

Unlike national chains with rotating staff, a local agency’s clinicians live and work in the same community. For over 74 years, Central Coast VNA & Hospice has served Monterey County, San Benito County, Santa Cruz County, and South Santa Clara County. This local connection builds trust and ensures better continuity of care. You can learn more about compassionate hospice pain management delivered by a local team.
What Local Roots Look Like
A provider with deep community ties is more than just a business. It is a dedicated partner in the local healthcare system. They are invested in the well-being of their neighbors.
A locally grounded provider often has:
- A Stable, Local Team: The Registered Nurses, Hospice Aides, and Chaplains are from the area and are committed to serving their community long-term.
- Strong Local Relationships: They have established partnerships with local doctors, hospitals, and community organizations.
- Nonprofit, Mission-Driven Focus: Many local providers are nonprofits. They reinvest their resources into patient care and community programs, not shareholder profits.
- Community Board of Directors: Their leadership is often made up of local community members who ensure the organization stays true to its mission.
Why Local Matters for Your Care
Choosing a local provider means you are more likely to receive personalized care. The team understands the local culture and resources. This leads to a more seamless and supportive experience.
A local, nonprofit provider like Central Coast VNA & Hospice puts patients first. Their mission is to provide comfort and dignity, not to generate profit. This focus is a core part of their identity.
Actionable Questions to Ask
Understand a provider’s connection to your community. Use these questions to learn more:
- How long has your organization been serving our community?
- Are your clinical team members employees, or are they contractors?
- Is your agency a nonprofit or a for-profit company?
- Who serves on your board of directors? Are they from our local area?
3. Confirm They Offer True 24/7 Clinical Support
A terminal illness does not follow a 9-to-5 schedule. A crisis like unmanaged pain or breathing difficulties can happen at any time. Quality hospice care in 2026 means having access to real clinical support, 24/7.

True 24/7 support means you can reach an experienced hospice Registered Nurse by phone at 3 a.m. It is not an answering service that takes a message. It is an active clinical safety net for patients and families. You can learn how trust, transparency, and testimonials help in choosing the right hospice for your loved one.
What 24/7 Support Looks Like
Round-the-clock availability provides great peace of mind. It prevents late-night trips to the emergency room. It also empowers families to manage symptoms at home with confidence.
High-quality 24/7 support includes:
- After-Hours Triage by a Registered Nurse: When you call, you speak directly with a nurse who can provide immediate guidance.
- On-Call Staff for Home Visits: The provider has nurses and other staff available to make urgent visits at night or on weekends.
- Fully Staffed Hospice Shifts: For patients with complex needs, some providers offer continuous care with staff present in the home.
- A Clear Emergency Plan: The team gives you clear instructions on who to call and what to do if a crisis occurs.
Why Constant Availability is Non-Negotiable
Waiting for help when your loved one is in distress is stressful. A quality hospice understands this. They build their services to be responsive whenever a need arises.
Central Coast VNA & Hospice offers fully staffed hospice shifts and on-call support 24/7. This ensures that expert help is always just a phone call away. This commitment is a hallmark of excellent care.
Actionable Questions to Ask
Get specific about after-hours support. Use these questions to understand what a provider truly offers:
- If I call after hours, who will answer the phone? Will it be a Registered Nurse?
- What is your average response time for a nurse to arrive at our home for an urgent need?
- Do you offer continuous care in the home if symptoms become severe?
- What kind of support is available on weekends and holidays?
4. Ensure Care Plans are Tailored to the Individual
Every patient is different. Their journey, values, and goals are unique. Quality hospice providers in 2026 recognize this and create care plans that are tailored to each person.

One-size-fits-all care is not quality care. The best providers use an interdisciplinary team. This team includes a physician, Registered Nurse, Hospice Aide, Medical Social Worker, and Chaplain. They collaborate with the family to shape care with them, not for them. To learn about how hospice care is funded, this link provides helpful information.
What a Personalized Care Plan Looks Like
A tailored care plan goes beyond medical orders. It reflects the patient's personal goals, culture, and preferences. It is a living document that changes as the patient's needs change.
A personalized plan should include:
- Patient-Centered Goals: The plan is built around what is most important to the patient, whether that's being pain-free or being able to enjoy a final family gathering.
- Cultural and Spiritual Respect: It honors the patient’s background, beliefs, and traditions.
- Family Involvement: The hospice team actively listens to the family and includes their insights and concerns in the plan.
- Regular Team Meetings: The full care team meets often to discuss the patient’s progress and adjust the plan as needed.
Why Personalization is a Sign of Quality
Personalized care shows that a provider sees the patient as a whole person, not just a diagnosis. It ensures that the care provided is meaningful and respectful. This approach helps maintain the patient’s dignity and sense of control.
At Central Coast VNA & Hospice, our interdisciplinary teams work closely with families. We listen to their stories and honor their wishes. This collaboration is at the heart of our compassionate care model. You can find more information here: guidance for culturally inclusive hospice care.
Actionable Questions to Ask
Find out how a provider tailors their care. Use these questions to see if they are a good fit:
- How will my loved one and our family be involved in creating the care plan?
- How often does the care team meet to review and update the plan?
- Can you give an example of how you have adapted a care plan to meet a patient's unique cultural or personal wishes?
- Who is our main point of contact on the care team?
5. Verify Accreditation and Awards
Not all hospice providers are held to the same standards. Official accreditations and awards are important signs of quality. They show that a provider has met rigorous national standards for patient safety and care.

Look for accreditations from organizations like The Joint Commission. These are not just logos on a website. They reflect a provider's commitment to consistent, measurable excellence in care. Awards like "Hospice Honors" also show that a provider is recognized as a national leader.
What Accreditations and Awards Mean
Achieving these honors is a difficult process. It requires a hospice to undergo a thorough review of its policies, procedures, and patient outcomes. It is proof of a deep commitment to high-quality care. A crucial aspect of personalized care, especially in end-of-life settings, involves understanding how staff are trained to provide specialized care tips for dementia patients or others with unique needs.
Indicators of excellence include:
- The Joint Commission Accreditation: This is considered the gold standard in healthcare accreditation.
- Community Health Accreditation Partner (CHAP) Accreditation: Another highly respected accrediting body for home and community-based care.
- Hospice Honors Recognition: An award given to hospices that score above the national average on patient and family satisfaction surveys.
- We Honor Veterans Program: Shows a commitment to meeting the unique needs of veterans at the end of life.
Why This Verification Matters
These credentials provide an extra layer of assurance. They confirm that an independent organization has reviewed the hospice and found it to meet high standards. This can give you confidence in your decision.
Central Coast VNA & Hospice is proud to be accredited by The Joint Commission. This reflects our long-standing dedication to providing the best possible care to the communities we serve. It is a key part of our promise to our patients and their families.
Actionable Questions to Ask
Ask providers about their credentials. Their answers will tell you a lot about their commitment to quality.
- Is your hospice accredited by The Joint Commission or another national body?
- Have you received any recent awards or recognition for patient care?
- How do you use the accreditation process to improve your services?
- Are your clinicians certified in hospice and palliative care?
Your Local Partner in Compassionate, Quality-First Care
Choosing a hospice provider is a deeply personal decision. By using these five ways to spot quality care, you can make an informed choice. Look for transparent quality data and a provider with local roots. Ensure they offer true 24/7 support and personalized care plans. Finally, verify their accreditations.
These steps empower you to find a partner who will honor your loved one with dignity. The right hospice provides a full support system for the entire family. It lifts burdens and offers peace of mind.
For families in Monterey, Santa Cruz, Salinas, or Hollister, Central Coast VNA & Hospice is here to help. For over 74 years, our nonprofit mission has guided our work. Our local team is dedicated to providing compassionate, quality-first care.
Choosing a hospice is an act of love. Let it also be an act of informed confidence. Contact Central Coast VNA & Hospice to learn how our quality-first, locally grounded approach can support your family in 2026.
When you're ready to find a partner who exemplifies the highest standards of care, Central Coast VNA & Hospice is here to help. Our local, nonprofit team has been providing compassionate, quality-first care on the Central Coast for over 74 years. Contact us today to learn more about our services and let us support your family on this journey. Learn more about our services.
Frequently Asked Questions (FAQs)
1. What is the difference between palliative care and hospice care?
Palliative care can be provided at any stage of a serious illness and can be given alongside curative treatments. Hospice care is for patients with a terminal illness who are no longer seeking curative treatment and focuses on comfort and quality of life. Central Coast VNA & Hospice provides both as part of our Continuum of Care.
2. How is hospice care paid for?
Hospice care is covered by Medicare, Medicaid, and most private insurance plans. As a nonprofit, Central Coast VNA & Hospice provides care to everyone who needs it, regardless of their ability to pay.
3. Can hospice care be provided at home?
Yes, most hospice care is provided in the patient's home. It can also be provided in nursing homes, assisted living facilities, or a hospital. Our team at Central Coast VNA & Hospice specializes in providing expert hospice care at home.
4. What does the hospice interdisciplinary team do?
The team works together to meet all of the patient's needs—physical, emotional, and spiritual. The team includes a physician, Registered Nurse, Hospice Aide, Medical Social Worker, Chaplain, and volunteers who create and manage a personalized care plan.
5. How quickly can hospice services begin?
Once a referral is made and the patient is determined to be eligible, services can often begin within 24 to 48 hours. Contact Central Coast VNA & Hospice to learn more about starting hospice care in Monterey County or our other service areas.
Caring for a Loved One? Support for Family Caregivers
When you step into the role of a family caregiver, you become a lifeline for someone you love. It's a journey of deep dedication, but it also has unique challenges. Reaching out for support for family caregivers is a sign of strength that helps both you and the person you care for.
The Reality of Being a Family Caregiver
Becoming a caregiver often happens slowly. It might start with small tasks like picking up groceries or driving to a doctor's appointment. Soon, these tasks can become a big part of your daily life. It’s a role born from love, but it can feel demanding and isolating.
This guide is here to help. We'll share practical advice and real solutions to help you find balance and avoid burnout. For over 74 years, Central Coast VNA & Hospice has been a nonprofit partner to families across Monterey County, San Benito County, Santa Cruz County, and South Santa Clara County. We support patients and the incredible families who care for them.
Understanding the Scope of Caregiving
The role of a family caregiver is more common than you might think. Many spouses, children, and friends provide essential support behind the scenes. Millions of Americans juggle their own lives with the needs of a loved one.
The numbers are staggering. About 63 million Americans will be family caregivers by 2025. That's nearly one in four adults providing unpaid support. This number has grown by almost 50% since 2015 due to our aging population. You can learn more at AARP.org.
The image below shows the scale of this commitment.
These statistics show that caregiving is a huge, often unpaid job. It touches a large part of our communities.
The Emotional and Physical Toll
Caregiving has rewarding moments, but it also carries a heavy weight. The constant worry and physical demands can lead to serious stress. Research shows family caregivers face higher risks of anxiety, depression, and other health problems.
Nearly 88% of family caregivers report feeling increased anxiety directly related to their duties. Almost three out of four experience significant financial or emotional strain while providing long-term care.
Recognizing your own needs isn’t selfish; it’s essential. To give the best care to your loved one, you must first care for yourself. Acknowledging the emotional toll is the first step toward building a sustainable routine.
How to Recognize Caregiver Burnout Early

Caregiver burnout isn’t a sign of weakness. It’s a natural response to long-term stress. It’s a signal from your body and mind that you’re carrying too much without enough rest.
Spotting the early signs is key to getting relief. Burnout often starts quietly. You might feel a deep exhaustion that sleep doesn't fix.
Emotional and Mental Signs of Burnout
One of the first places burnout shows up is in your emotions. You may feel more irritable or withdrawn than usual. Conversations that were once easy might feel draining.
Losing interest in hobbies is another major red flag. If you’ve stopped making time for things you enjoy, your caregiving duties may be consuming all your energy.
Feeling hopeless or easily overwhelmed can also signal burnout. It means your emotional reserves are low, making it hard to cope with daily pressures.
Understanding when you're nearing your limit is vital. You can learn to recognize the 10 key signs of emotional burnout before they take hold.
Physical Symptoms to Watch For
Burnout isn’t just in your head; it has real physical effects. Chronic stress can show up in your body. It's important to listen to these signals.
Here are some common physical signs to look out for:
- Changes in Sleep: This could be trouble falling asleep, waking up often, or sleeping more but still feeling tired.
- Frequent Aches: Unexplained muscle tension, back pain, or headaches are often tied to stress.
- Lowered Immunity: If you get sick more often, it may be because stress is weakening your immune system.
It's easy to dismiss these symptoms. But when they form a pattern, they point to a deeper issue. For a closer look, read our guide on the five signs it's time to ask for help as a family caregiver.
At Central Coast VNA & Hospice, we know that providing support for family caregivers is as important as patient care. Our teams in Monterey County and Santa Cruz County are here with resources to help. If you see these signs in yourself, remember that help is available.
Finding Practical Support Systems for Relief
Admitting you need help is a huge step. But figuring out where to turn can feel overwhelming. The good news is you’re not alone, and you don’t have to figure it all out yourself.
Real support systems exist right here on the Central Coast. Think of these resources as essential tools in your caregiving toolbox. They are designed to meet different needs.
Central Coast VNA & Hospice provides a range of these services. This ensures you always have a local, nonprofit partner to lean on. Let's look at key options that can make a real difference.
Respite Care for Essential Breaks
One of the best tools for preventing burnout is respite care. This service provides a short-term break for you, the family caregiver. It allows you to rest and recharge.
Even a few hours away can reduce stress. Central Coast VNA & Hospice can arrange for a compassionate Hospice Aide or another trained professional to stay with your loved one. This gives you peace of mind while you take time for yourself.
Emotional and Spiritual Support
The emotional weight of caregiving is immense. It's important to have a safe space to work through your feelings. This is where dedicated emotional and spiritual support can be a lifeline.
Central Coast VNA & Hospice offers services to support your emotional health:
- Medical Social Workers: These professionals are your advocates. They provide counseling and connect you with community resources.
- Chaplains: Our non-denominational chaplains offer spiritual support that respects your family’s beliefs.
Taking care of your mental health is critical. If you're feeling overwhelmed, our guide on how to get real support as a family caregiver offers more strategies.
Professional Care Coordination
Managing a loved one’s illness often feels like a full-time job. You track medications, appointments, and symptoms. Professional care coordination can lift this burden from your shoulders.
Our interdisciplinary teams include Registered Nurses, Hospice Aides, and Medical Social Workers. They work together to manage your loved one's entire care plan. This team-based approach means you have a network of specialists backing you up.
Unpaid family caregivers provide an astonishing $873.5 billion to $1.1 trillion in services annually. This immense contribution often comes at a steep personal cost.
One in five caregivers reports going into debt to manage their duties. This highlights the urgent need for support systems. You can discover more about the economic impact of caregiving and see why asking for help is crucial.
Whether you need respite in Monterey County or skilled nursing in San Benito County, practical help is here. Central Coast VNA & Hospice provides comprehensive support for family caregivers.
Proven Strategies for Managing Daily Challenges
Caring for a loved one involves many daily tasks that can feel overwhelming. Creating a simple, structured routine can help. Having a few strategies can make your duties feel more manageable.
A clear system helps you stay on top of medical needs. It also frees up mental energy. Let's walk through some practical approaches.
Organizing Medical Information and Schedules
Juggling medications and appointments is a big daily hurdle. Disorganization can lead to mistakes and more stress. The key is to create one central hub for everything.
Start with a simple medication schedule. You can use a pill organizer, a whiteboard, or a digital calendar. This visual reminder helps prevent errors. For more tips, check out these expert tips to prevent medication errors at home.
Here are a few other organizational tips:
- Create a Care Binder: Keep all vital documents here, like insurance info, doctor contacts, and medication lists.
- Use a Shared Calendar: A tool like Google Calendar helps coordinate appointments so family can help.
- Prepare for Doctor Visits: Before an appointment, write down your questions to make the most of your time.
Improving Communication and Connection
Clear and compassionate communication is vital when a loved one is seriously ill. It reduces frustration and strengthens your bond. Listen patiently and validate their feelings to build trust.
Sometimes, difficult behaviors arise from pain or fear. Try to respond with empathy. Simple things, like making eye contact and speaking in a calm tone, can help. Communication is especially key when caring for someone at the end of life, and these 5 tips for talking with a loved one that’s terminally ill offer valuable insights.
Your role goes beyond managing tasks. You are providing comfort and presence. Often, these small moments of connection are the most meaningful.
Daily Caregiving Strategy Checklist
| Strategy | Why It Helps | Pro Tip |
|---|---|---|
| Morning Check-In | Sets a positive tone and helps you assess immediate needs. | Keep it light. "How did you sleep?" or "What's on your mind today?" |
| Medication Routine | Prevents errors and creates a predictable structure. | Use a pill organizer and set daily alarms on your phone. |
| Schedule Review | Keeps everyone aware of appointments for the day. | Post a large-print calendar or whiteboard in the kitchen. |
| Plan One Small Joy | Fights monotony and provides something to look forward to. | Watch a favorite show, listen to music, or sit outside for 10 minutes. |
| "Take Five" Breaks | Gives you short moments to step away and recharge. | Even five minutes of quiet time can make a huge difference. |
| Evening Wind-Down | Helps ensure a calm transition to bedtime for better sleep. | Create a simple routine like dimming the lights or reading aloud. |
Putting just a few of these strategies in place can bring calm back into your day. Our teams across Monterey County and San Benito County are here to offer practical support for family caregivers.
How to Ask for Help and Build a Support Network

If you're a family caregiver, asking for help can feel hard. You might worry about being a burden. But reaching out is one of the strongest steps you can take.
Building a support network helps you provide care without burning out. It lets you share the physical and emotional load. This network can be family, friends, and professional services working together.
Starting the Conversation
The secret to getting help is how you ask. A vague "I need help" is hard for people to act on. A better approach is to make clear, direct requests.
Think about specific tasks that would lift a weight off your shoulders. Breaking down your needs into smaller asks feels more manageable for others.
Here are a few ways to frame it:
- "Could you sit with Mom for two hours on Tuesday so I can go to my doctor's appointment?"
- "Would you be able to pick up groceries for us this week?"
- "I'm feeling drained. Could we talk on the phone tonight?"
Being specific takes the guesswork out of it. It empowers people to offer support that makes a difference.
Connecting with Formal Support Systems
Formal support systems offer professional assistance. For families in Monterey County, San Benito County, Santa Cruz County, and South Santa Clara County, Central Coast VNA & Hospice is a key local resource.
Reaching out for professional help is a sign of proactive care planning. It shows your commitment to providing the best support for your loved one.
Services like respite care are built to give you a break. A trained professional, like one of our Hospice Aides, can step in. This gives you peace of mind while you rest. You can learn more about how respite care for family caregivers works.
Building a support network means accepting you can't do this alone. Every bit of help strengthens your ability to provide loving care.
Your Local Partner in Care on the Central Coast
The path of a caregiver is demanding, but you do not have to walk it alone. Here in Monterey, San Benito, Santa Cruz, and South Santa Clara Counties, Central Coast VNA & Hospice is your local, nonprofit partner. We are committed to providing support where you need it most—at home.
For over 74 years, our work has been guided by one belief: to support the entire family. We understand the challenges families face on the Central Coast because we are your neighbors. Our services—from home health and palliative care to hospice—are designed to grow with your family’s needs.
A Legacy of Local, Nonprofit Care
Unlike large, for-profit agencies, our focus is on our community. Our mission is to serve, making sure your family receives high-quality, heartfelt care. We are your trusted local guide for navigating serious illness.
The screenshot below is the first thing you'll see on our website. It's a clear starting point for families looking for help.
We designed our site to be a simple resource when you need it most. The need for this support is growing. This highlights the urgent need for reliable, local help.
Take the First Step Today
We know making that first call can feel overwhelming. That’s why our team is here to listen without judgment. We offer clear, simple guidance. For a deeper look at your options, read our guide on where to turn when a loved one is seriously ill.
Your strength as a caregiver is remarkable. Allowing us to support you is a powerful way to sustain that strength for the road ahead.
If you are caring for someone at home and feeling stretched thin, please don’t wait. Reach out to Central Coast VNA & Hospice today. Learn how our dedicated team can walk alongside you, every step of the way.
Frequently Asked Questions About Caregiver Support
What is respite care?
Respite care provides a short break for family caregivers. A trained professional, like a Hospice Aide from Central Coast VNA & Hospice, steps in to provide care. This allows you to rest, run errands, or attend to your own needs without worry. It is a vital service for preventing burnout.
How can I get help with medical tasks at home?
Managing complex medical needs can be stressful. Our home health and palliative care services can help. A Registered Nurse can visit your home to handle skilled tasks, like wound care, and teach you how to manage them safely. We coordinate directly with your loved one’s doctor.
What kind of emotional support is available for caregivers?
The emotional toll of caregiving is significant. Central Coast VNA & Hospice offers access to Medical Social Workers and non-denominational Chaplains. They provide a safe space to process difficult emotions, learn coping strategies, and connect with community resources.
Who do I talk to about my loved one’s care plan?
We provide a dedicated team, including a Registered Nurse case manager, as your main point of contact. This team approach ensures you always know who to call with questions. Everyone works together to coordinate care and keep communication clear.
How much do these support services cost?
Services like home health, palliative care, and hospice care in Monterey County are often covered by Medicare, Medi-Cal, and most private insurance plans. As a nonprofit, our mission is to provide care to everyone who needs it. Our team will help you understand your benefits and explore all available coverage options.
If you're caring for a loved one and looking for support, Central Coast VNA & Hospice is here for you. Our teams across the Central Coast are ready to provide the compassionate, expert care your family deserves. Contact us today to learn more about our services.
Starting Hospice Sooner: What Families Should Know
Many families think of hospice as something for the last few days of life. This common misunderstanding often means missing out on weeks or even months of incredible support. Choosing to start hospice sooner isn't about giving up.
It's about making a choice to prioritize comfort, dignity, and quality of life. This shift in focus gives the entire family a support system—physically, emotionally, and spiritually—right when it's needed most.
Why Starting Hospice Sooner Makes a Difference
Thinking about hospice can feel overwhelming. Too often, families put off the conversation until a crisis strikes. This can mean losing the chance to manage symptoms and reduce stress.
By looking into hospice care earlier, you give your loved one and your family the gift of time. This means time for expert pain management, emotional support, and meaningful moments together. This guide is here to reframe the conversation around starting hospice sooner: what families should know.
Maximizing Comfort and Quality of Life
When hospice begins early, the care team has more time to know the patient. This allows them to create a personalized care plan that keeps pain and symptoms under control. The result is fewer trips to the emergency room and fewer stressful hospital stays.
Instead of reacting to one crisis after another, the focus shifts to creating a calm environment at home. This approach helps patients stay in a familiar space, surrounded by people they love. It builds a support system that honors their wishes for peace and dignity.
This infographic captures the core benefits of enrolling in hospice sooner.

Starting sooner lets the care team build a trusting relationship with the patient and family. A longer period of care also opens the door for important conversations. Families can also explore the legal aspects of planning for a longer hospice journey.
Recognizing the Signs It Might Be Time
Knowing when to consider hospice can feel hard. It’s a decision loaded with emotion. But recognizing the signs early isn’t about giving up—it’s about shifting the focus to comfort and quality of life.
The conversation usually starts when the goal of treatment moves from finding a cure to making the most of the time left. This is the heart of the care we provide at Central Coast VNA & Hospice. It's about helping your loved one live as fully and comfortably as possible.

Key Clinical Indicators to Watch For
While every person's journey is different, there are common physical signs that it might be time to explore hospice. Watching for these trends can help your family make an informed decision. Clear signs include frequent hospitalizations, unmanaged pain, and exhaustion for both the patient and family.
One of the most obvious signs is repeat hospitalizations or trips to the emergency room. If your loved one is constantly in and out of the hospital, their condition may be too difficult to manage with their current treatment.
Other important signs include:
- Unmanaged Symptoms: Pain, shortness of breath, or nausea that won't go away, even with medication.
- Significant Weight Loss: A noticeable drop in weight, often paired with a poor appetite.
- Decline in Function: A clear downturn in their ability to handle daily activities like getting dressed or bathing.
- Increased Fatigue: A growing weakness that forces them to spend most of the day in a chair or bed.
It’s tough to see these changes, but they are important signals. For a deeper look, you can read our guide on when to call hospice.
Quality of Life and Emotional Signs
Just as important as physical signs are changes in emotional state and quality of life. Sometimes, the most telling clues aren't on a medical chart. These shifts affect both the person who is ill and the family members caring for them.
You might notice your loved one withdrawing from hobbies or showing less interest in seeing friends. This isn't a choice; it's often the result of physical and emotional exhaustion. All their energy is being used just to cope.
For families, caregiver burnout is also a key sign. If you feel overwhelmed by managing medications and daily needs, that's a signal that more support is needed. This is where the interdisciplinary team at Central Coast VNA & Hospice can step in, offering relief to families across Monterey and Santa Cruz counties.
The Real Benefits of Earlier Hospice Enrollment
Choosing hospice earlier isn't about giving up. It's about getting more—more time, more comfort, and more support. When families start hospice services sooner, they give their loved one the gift of a better quality of life.
This extra time lets our team build a strong relationship and create a personal care plan. It leads to a more stable environment. Instead of reacting to one crisis after another, our team can proactively manage symptoms and provide consistent support.
Superior Symptom Management and Comfort
More time with the hospice team means better control over pain and other symptoms. It gives our Registered Nurses the chance to adjust medications and teach the family how to manage symptoms. The result is a higher quality of life, allowing your loved one to stay engaged with the people they care about.
With a good plan in place, the focus shifts from just getting through each day to truly living it. At Central Coast VNA & Hospice, we ensure every medical step aligns with the patient's comfort. This helps people remain in the one place they want to be—at home.
Earlier hospice enrollment is associated with measurable improvements in symptom management and caregiver outcomes. Patients who enter hospice with longer lengths of stay receive more visits per week and more continuous symptom-management resources, while their families report lower rates of unmet needs. Read more about these findings on hospice monitoring reports.
Financial and Emotional Relief for Families
The relief that early hospice brings to families is huge, and it’s not just emotional. One of the biggest benefits is financial. The Medicare Hospice Benefit, which covers most of our patients, includes:
- Medications related to the terminal illness.
- Medical equipment like hospital beds and oxygen.
- Medical supplies such as bandages and catheters.
This coverage lifts a huge financial weight off the family’s shoulders. The support also extends to emotional needs. The Central Coast VNA & Hospice team includes a Medical Social Worker and a Chaplain to ensure the entire family feels supported.
The quality of care is boosted by how efficiently our teams work. Understanding the benefits of medical voice charting shows how healthcare providers can spend more time on patient care.
A Structured Support System at Home
The power of starting hospice sooner is having a team in your corner. This team includes a Registered Nurse, a Hospice Aide, a Medical Social Worker, a Chaplain, and trained volunteers. They all work together to create a network of support at home.
This structure prevents the chaotic experience of navigating a late-stage illness alone. You have a professional team on call 24/7 to answer questions and provide hands-on care. For families across Monterey County, San Benito County, Santa Cruz County, and South Santa Clara County, this means you are never alone.
This approach is at the heart of our hospice at home services. By enrolling sooner, you empower your loved one to live their final months with dignity.
How to Start the Hospice Conversation With Your Family
Bringing up the topic of hospice is one of the most difficult talks a family can have. It feels heavy. But it doesn't have to.
The key is to frame the discussion around comfort, dignity, and quality of life—not about giving up. It's about honoring your loved one’s wishes. The best approach is to lead with love and listen more than you talk.
Gentle Ways to Begin the Discussion
Finding the right words can feel impossible. Try easing into the conversation with open-ended questions. This gives your loved one space to share their thoughts without feeling pressured.
Using "I" statements can also soften the talk. For example, saying, "I've been worried about your pain, and I want to be sure we're doing everything to keep you comfortable," places the focus on their well-being.
Here are a few gentle conversation starters:
- "I've been thinking about what you're going through. What are your biggest worries?"
- "If things were to get more difficult, what's most important for you?"
- "I want to make sure we respect your wishes. Have you thought about what you would want if your health changed?"
For more advice, our guide on how to talk to your parents about hospice care is a great resource.
Involving the Medical Team
You don't have to do this alone. Your loved one’s doctor is an essential partner. A doctor can offer a clinical view that helps ground the conversation in facts.
When you talk to the doctor, frame your questions around exploring all available options. This opens the door for the medical team to discuss the full spectrum of care. This can include the benefits of starting hospice sooner.
An informational consultation is not a commitment to begin services. It is an opportunity for families to ask questions, understand the support available, and make a plan that feels right for everyone, without any pressure.
How a No-Obligation Consultation Works
Many people worry that calling a hospice provider locks them in. That isn't true. At Central Coast VNA & Hospice, we offer no-obligation consultations for families across Monterey County, San Benito County, and Santa Cruz County.
Here’s what to expect when one of our Registered Nurses visits you:
- Listen: First, we listen. We want to hear about your family’s needs and health concerns.
- Explain: We'll walk you through how hospice works and what services are included.
- Answer: You'll have the chance to ask anything about our interdisciplinary team.
- Provide: We'll leave you with resources, whether you decide to enroll now or later.
This meeting is about empowering you with knowledge. It’s a conversation about the possibilities for comfort and peace.
Getting Started: Hospice Eligibility and How It's Paid For
The logistics of starting hospice care can feel overwhelming. But many families are surprised to find the requirements are straightforward. Understanding eligibility and payment can clear away major hurdles.
At Central Coast VNA & Hospice, our job is to bring clarity to this journey. We want to demystify the process for families across Monterey, San Benito, and Santa Cruz counties.
The Main Eligibility Guideline
What does it take to qualify for hospice? The main requirement is a clinical one. A person is eligible when two physicians—their doctor and our hospice medical director—agree.
They certify that the person has a life-limiting illness with a life expectancy of six months or less if the illness runs its natural course. It's important to remember this is a guideline, not an exact timeline.
Patients can, and often do, receive hospice support for longer than six months. This is possible as long as they still meet the medical criteria.
How Is Hospice Paid For?
For most families, the cost of healthcare is a worry. The good news is that hospice is designed to lift that financial burden. This ensures compassionate support is available to everyone who needs it.
The main payment source is the Medicare Hospice Benefit. This covers nearly everything related to the terminal diagnosis, including:
- Visits from the Registered Nurse and other care team members.
- Medications for pain and symptom management.
- Medical equipment, like a hospital bed or oxygen.
- Supplies needed for care, such as bandages.
This all-in-one coverage means you can focus on your loved one, not medical bills. It’s a huge part of what makes starting hospice sooner a practical choice for families.
The Medicare Hospice Benefit is designed as a complete package of care. Families aren't billed separately for nursing visits, medications, or equipment related to the hospice diagnosis. This alone removes a massive source of stress.
Besides Medicare, hospice is also covered by Medi-Cal and most private insurance plans. As a nonprofit, Central Coast VNA & Hospice is committed to making sure cost is never a barrier to care. Our team is here to help you understand your specific coverage.
For a more detailed breakdown, learn more about how to pay for hospice care on our website.
Your Local Partner in Compassionate Care on the Central Coast
For families navigating a serious illness across Monterey, San Benito, Santa Cruz, and South Santa Clara counties, the journey can feel isolating. For over 74 years, Central Coast VNA & Hospice has been a dedicated, nonprofit partner in the community. We are your neighbors, here to walk alongside you.
Our care is designed as a seamless continuum. This means your loved one can move from home health to palliative care, and then to hospice, all within one trusted organization. Having a familiar team that understands your family’s history makes all the difference.
A Team That Honors Your Wishes
What sets our care apart is our dedicated, interdisciplinary team. This group of Registered Nurses, Hospice Aides, Medical Social Workers, and Chaplains works together to honor each patient's goals. Our mission is to provide personalized care that centers on comfort and dignity.
Our philosophy is simple: we empower families with education and support, not just services. We believe that when you have clear information, you can make the best decisions for your loved one with confidence and peace of mind.
Having access to this kind of structured support is vital. Globally, the ability to start hospice sooner often depends on established programs. You can read more about the global landscape of hospice access to understand why this matters.
If you are caring for a loved one and wondering when to ask about hospice, start with a conversation. Central Coast VNA & Hospice is here for families across the Central Coast—offering guidance, not pressure, and compassionate care when it’s needed most. You can learn more about why Central Coast VNA & Hospice is the best choice for your family.
Frequently Asked Questions About Starting Hospice Sooner
Does starting hospice mean we’re giving up on our loved one?
Not at all. Starting hospice is about shifting the focus from trying to cure an illness to providing comfort and quality of life. It is a proactive choice to ensure your loved one's final months are lived with dignity and support, rather than in a cycle of hospital visits.
Can a patient leave hospice care after they start?
Yes. A person can stop hospice care at any time if their health improves or they decide to seek other treatments. The Medicare Hospice Benefit is flexible, allowing patients to re-enroll later if their condition changes again.
What professionals are on a hospice care team?
The hospice team provides complete support for the patient and family. At Central Coast VNA & Hospice, our interdisciplinary team includes a Registered Nurse, Hospice Physician, Hospice Aide, Medical Social Worker, Chaplain, and trained volunteers who all work together.
Where is hospice care usually provided?
Hospice care is typically provided wherever the patient calls home. This could be a private residence, an assisted living facility, or a nursing home. Our team serves patients across Monterey County, San Benito County, Santa Cruz County, and South Santa Clara County, bringing care directly to them.
When is the right time to contact a hospice provider for information?
It is never too early to learn about your options. We encourage families to contact us for a no-obligation conversation as soon as a life-limiting illness is diagnosed. This allows you to gather information and make an informed decision without pressure when the time is right.
If you have more questions or want to talk about your family’s specific needs, Central Coast VNA & Hospice is here to listen. Contact us today for a compassionate, no-obligation conversation about how we can support you.










