When a loved one is nearing the end of their life, their comfort becomes the single most important thing. This is the heart of hospice pain management.
It’s a specialized philosophy of care that shifts the focus away from curing a disease and toward providing a compassionate shield from distress. The goal is simple: to allow them to spend their remaining time with dignity, surrounded by family, and as free from pain as possible. Hospice pain management is about treating the whole person, not just the illness.
Understanding Compassionate Pain Management in Hospice
At Central Coast VNA & Hospice, our approach is built on more than 74 years of local, nonprofit service. We know firsthand that pain isn’t just a physical sensation.
It's a complex experience that can deeply affect a person’s spirit, emotions, and relationships. Because of this, our mission as a mission-driven healthcare provider is to address every part of a person's well-being.
The core philosophy is simple: every person deserves to live their final chapter with grace and comfort. Our job is to make that a reality for families in Monterey County, San Benito County, Santa Cruz County, and South Santa Clara County.
A Focus on Quality of Life
The primary goal of hospice isn't to extend life, but to maximize the quality of the life that remains. This means we build a care plan centered entirely around the patient's personal wishes and goals.
For one person, that might mean being alert and present enough to share stories with grandchildren. For another, it could simply be resting peacefully and without anxiety in the familiar comfort of their own home.
Effective pain relief is a fundamental human need. According to the World Health Organization (WHO), an estimated 56.8 million people, including 25.7 million in their last year of life, need palliative care each year (WHO, 2020). This global reality underscores just how critical dedicated hospice services are.
It's also important to know that while both palliative care and hospice care focus on comfort, they serve different needs. We've put together a guide that walks you through the key differences between palliative and hospice care to help you make informed decisions.
Before we go deeper, it helps to understand the foundational principles that guide our work. This isn't just a checklist; it's a commitment to ensuring every patient feels seen, heard, and cared for with the utmost respect.
Core Principles of Hospice Pain Management
| Principle | Description |
|---|---|
| Patient-Centered Care | The patient's personal goals, values, and preferences are the driving force behind all decisions. |
| Holistic Approach | Pain is treated as a multidimensional experience, addressing physical, emotional, social, and spiritual needs. |
| Proactive Management | We anticipate and treat pain before it becomes severe, rather than just reacting to it. |
| Continuous Assessment | Pain is regularly monitored and the care plan is adjusted in real-time to ensure ongoing comfort. |
| Interdisciplinary Teamwork | A team of experts collaborates to provide comprehensive, layered support for the patient and their family. |
These principles aren't just words on a page—they are the pillars of the compassionate care we provide every single day. They ensure that our focus remains squarely on the patient's comfort and dignity.
Building a Personalized Comfort Plan
There is no one-size-fits-all solution in hospice. Every person’s journey with their illness is unique, and so is their experience of pain.
That’s why our dedicated teams work side-by-side with patients and their families to craft a comfort plan that is as individual as they are. This plan always involves:
- Listening Carefully: We start by truly hearing the patient. We want to understand their specific symptoms, their fears, and most importantly, their wishes.
- Continuous Assessment: Pain isn't static; it can change from day to day, or even hour to hour. Our Registered Nurses continually monitor comfort levels and adjust the care plan as needed.
- A Team Approach: We bring together a compassionate team of experts—including a physician, Registered Nurse, and Hospice Aide—to provide layered, comprehensive support.
For families across the Central Coast, from Santa Cruz County to South Santa Clara County, our promise is to deliver expert, compassionate care when it matters most. By focusing on total comfort, we help ensure your loved one's final days are defined by peace, not by pain. Contact us today to learn how our team can support your family through this journey.
Your Expert Hospice Care Team

Effective hospice pain management isn't a one-person job. It takes a dedicated group of professionals working in harmony, each bringing their unique skills to the table. This creates a complete, layered system of support for both the patient and their family.
Think of it as a specialized support system where every single member plays a crucial part in ensuring total comfort. This team approach is the bedrock of our philosophy at Central Coast VNA & Hospice, something we've been refining for over 74 years.
It’s our way of making sure no aspect of a person’s well-being is overlooked—from physical symptoms to their emotional and spiritual needs. When you choose our services, you aren’t just getting a provider; you’re gaining an entire team of compassionate experts.
The Core Members of Your Care Team
Each professional on your hospice team has a specific focus, but they all communicate constantly. They share insights and adjust their approach together to meet your loved one’s changing needs.
This tight-knit coordination is what provides consistent and reliable comfort right at home. Here’s who is on your side:
- The Registered Nurse (RN): The RN is usually the team coordinator. They are true experts in assessing pain and other symptoms, managing medications, and, just as importantly, teaching the family how to provide day-to-day care.
- The Hospice Aide: These are the compassionate professionals who provide gentle, hands-on personal care. Their work, like helping with bathing and dressing, is absolutely essential for maintaining comfort and dignity.
- The Medical Social Worker: A serious illness brings more than just physical challenges. The Medical Social Worker is there to provide emotional support and help families navigate practical stressors, like financial concerns or finding community resources.
- The Chaplain: For many people, spiritual comfort is a vital part of finding peace. Our chaplains offer non-denominational spiritual support that respects every family's unique beliefs and traditions, helping address deep questions of meaning and legacy.
This team works together seamlessly to wrap your loved one in a blanket of comprehensive care.
How Your Team Works Together
What does this collaboration look like in practice? Imagine the Registered Nurse notices that a patient seems more restless than yesterday.
The RN immediately shares this observation with the team. The Hospice Aide might then suggest a new, more comfortable position in bed, while the Medical Social Worker could check in with the family to see if any new emotional stressors are contributing.
This constant, fluid communication ensures the care plan is always responsive. To keep everyone connected securely, your hospice team uses HIPAA-compliant video conferencing platforms for virtual consultations, protecting your loved one’s sensitive health information.
At Central Coast VNA & Hospice, our interdisciplinary team meets regularly to discuss every single patient. This ensures everyone is aligned on the care goals, creating a unified and powerful support network for families across Monterey, San Benito, Santa Cruz, and South Santa Clara counties.
This collaborative spirit means you always have multiple advocates working on your family’s behalf. To learn more about how our teams provide comfort and dignity, you can explore our detailed guide to Central Coast VNA & Hospice care.
How We Understand and Measure Pain

You can't manage pain effectively if you don't first understand what a person is truly feeling. This isn't about running through a simple checklist.
It's an ongoing, compassionate conversation between our team, the patient, and their family. At Central Coast VNA & Hospice, we believe every expression of discomfort—spoken or unspoken—deserves to be heard, validated, and addressed.
Our entire approach is built on continuous assessment. Pain isn't a static condition; it can shift in intensity, location, and nature. Our Registered Nurses and Hospice Aides are constantly observing, listening, and asking questions to stay ahead of it.
The Art and Science of Pain Assessment
Measuring something as subjective as pain takes a blend of proven clinical tools and deep empathy. We tailor our methods to each individual.
This ensures we can get an accurate picture of their comfort level, whether they can speak for themselves or not. Our assessment methods include:
- Verbal Pain Scales: For patients who can communicate, we often use a simple 0-10 scale. Zero means no pain, and 10 represents the worst pain imaginable. This gives us a clear baseline.
- Descriptive Language: We also encourage patients to use their own words. Is the pain "sharp," "dull," "aching," or "burning"? These details help our clinicians pinpoint the source and choose the most effective treatment.
- Observing Non-Verbal Cues: Many of our patients can't articulate their feelings. In these situations, our team is expertly trained to recognize the non-verbal signs of distress.
These subtle but critical cues are often the clearest language a patient has. Recognizing them is a true cornerstone of compassionate care.
Listening to What Is Not Being Said
For patients who can't verbalize their needs, our hospice professionals become detectives of discomfort. We carefully watch for physical and behavioral shifts that signal pain.
We operate on a core belief: a person's inability to speak does not mean they have nothing to say about their pain. Our job is to listen with our eyes and our hearts, translating subtle cues into meaningful relief.
This focus on observation is vital for anyone in hospice, especially those with advanced dementia or who are non-responsive. The signs we look for include:
- Facial Expressions: Subtle grimacing, a furrowed brow, or frequent wincing can all point to pain.
- Restlessness: Increased agitation, constant fidgeting, or an inability to get comfortable are common signs.
- Changes in Breathing: Holding one's breath, taking shallow breaths, or a sudden spike in respiratory rate can be an involuntary reaction to discomfort.
- Body Language: Guarding a specific part of the body or pulling away when touched often signals the source of pain.
Family members are invaluable partners in this process. You know your loved one better than anyone and can often spot subtle changes that might otherwise be missed.
Your insights help us build a complete picture of your loved one’s comfort. You can learn more by reading our guide on how doctors determine hospice eligibility.
This detailed, ongoing assessment is what allows us to provide truly effective hospice pain management across Monterey County, San Benito County, and our neighboring communities. It ensures our care plan is always aligned with one simple goal: total comfort.
Tailoring Treatments for Total Comfort
Once we have a clear picture of what a person is feeling, our focus shifts entirely to bringing them relief. Think of it like opening a comprehensive comfort toolkit.
This kit isn’t limited to just one or two options. It’s filled with a wide range of tools, from proven medications to gentle, hands-on therapies. This allows us to build a hospice pain management plan that’s a perfect fit for the individual.
At Central Coast VNA & Hospice, our care philosophy isn't about choosing one method over another. It's about blending different approaches to create a layered, supportive effect for patients across Monterey County and our neighboring communities.
Pharmacological Treatments: The Role of Medication
Medication is often a cornerstone of effective pain management in hospice. Our expert medical team, led by a physician and closely managed by a Registered Nurse, uses medications with incredible precision.
The absolute priority is always to maximize comfort while keeping any unwanted side effects to a minimum. One of the most common concerns we hear from families is about the use of strong pain relievers, especially opioids.
They understandably worry about the risk of addiction. In the context of end-of-life care, however, the clinical focus shifts completely. The goal is to relieve the very real, physical suffering caused by a terminal illness, which means addiction is no longer a primary medical concern. Our team's expertise is in finding the lowest possible dose that still keeps your loved one comfortable.
Research into serious health-related suffering (SHS) from 1990 to 2021 revealed a growing need for hospice pain management worldwide. This was due to chronic conditions like cancer and dementia. This analysis highlights that pain management gaps disproportionately impact women, children, and the elderly. You can read the full research findings on global palliative care needs.
This careful, proactive management is what truly sets hospice care apart. It’s an approach designed to stay ahead of the pain.
Non-Pharmacological Methods: Comfort Beyond Medication
While medications are vital, they are only one piece of the puzzle. We know that true comfort comes from a holistic approach that nurtures the body, mind, and spirit.
This is where non-pharmacological—or non-medication—therapies play a crucial role. These gentle, supportive methods can be incredibly powerful, both on their own and when used alongside medication.
These comfort-focused therapies often include:
- Therapeutic Repositioning: Sometimes, a simple change in position is all it takes to relieve pressure and reduce stiffness. Our Hospice Aides are skilled in gently repositioning patients.
- Massage and Touch Therapy: A gentle hand or foot massage can do wonders for easing muscle tension, improving circulation, and providing a deep sense of human connection and calm.
- Music Therapy: Listening to favorite songs can lower anxiety, bring back positive memories, and offer a powerful, welcome distraction from physical discomfort.
- Creating a Peaceful Environment: Lowering the lights, reducing noise, and adding a pleasant scent to the room can transform a space into a tranquil sanctuary.
These techniques work in harmony to soothe the nervous system and promote deep relaxation. This integrated model shares many core principles with palliative care, which also focuses on improving quality of life. You can learn more about the wide-ranging benefits of palliative care in our detailed guide.
Pharmacological vs. Non-Pharmacological Pain Treatments
| Treatment Category | Examples | Best Used For |
|---|---|---|
| Pharmacological | Opioids (morphine, fentanyl), NSAIDs (ibuprofen), Nerve pain medications (gabapentin), Anti-anxiety medications | Managing moderate to severe persistent or breakthrough pain from the illness itself. |
| Non-Pharmacological | Massage, Therapeutic Repositioning, Music Therapy, Aromatherapy, Creating a calm environment | Easing anxiety, reducing muscle tension, promoting relaxation, and providing emotional and spiritual comfort. Often used with medications. |
It's not a matter of "either/or." The best, most comprehensive pain management plans use both approaches to address all facets of a person's discomfort.
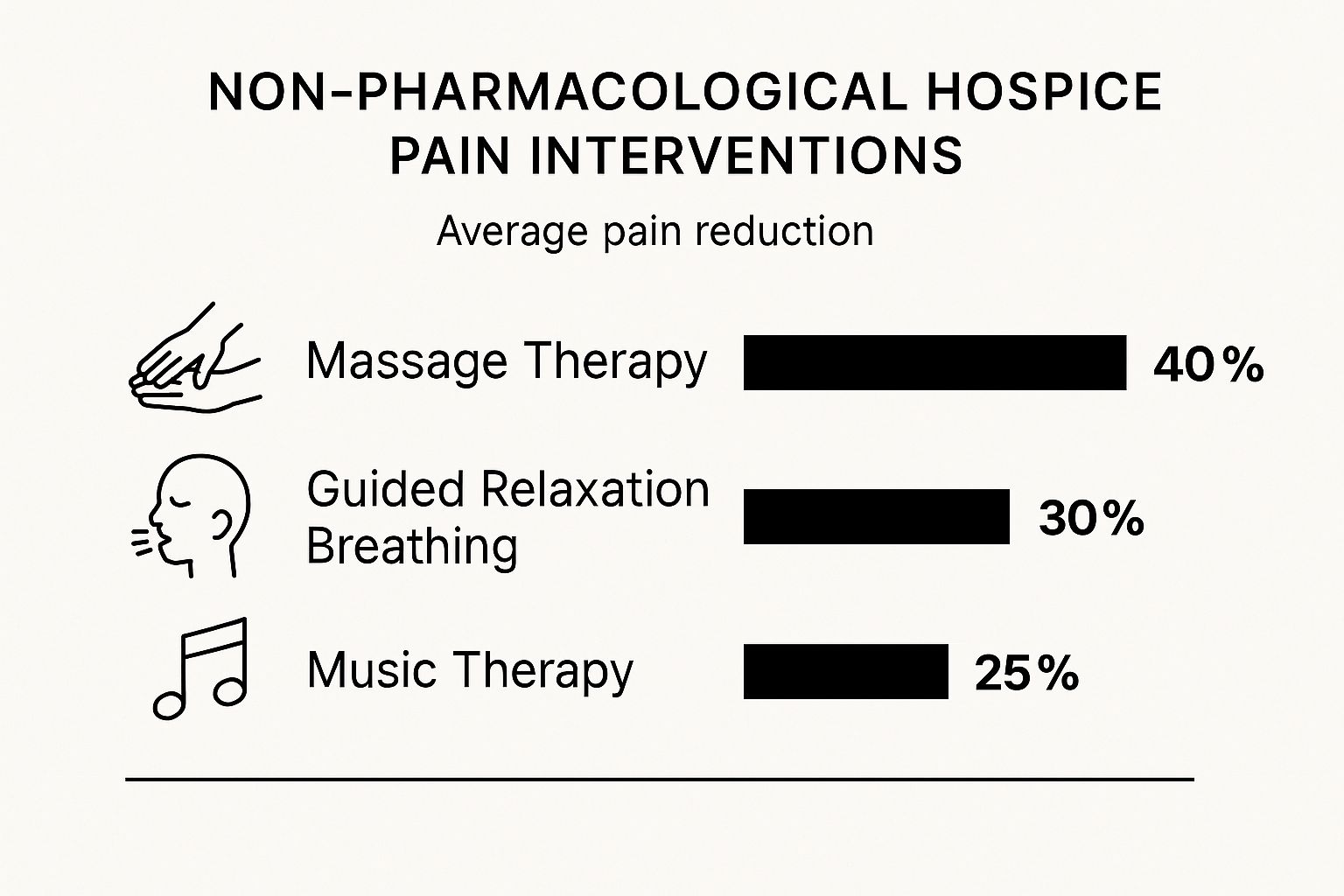
The data in this infographic really drives home the point. Gentle therapies like massage and guided relaxation can provide a significant reduction in pain, reinforcing the immense value of a multi-faceted comfort plan.
By blending the best of both worlds—expert medication management and compassionate comfort therapies—we create a truly personalized care experience. This is the promise of Central Coast VNA & Hospice.
How Families Can Partner in Providing Comfort
When a loved one receives hospice care at home, family members become essential partners in their comfort. You're not just a bystander; you're a vital part of the care team.
At Central Coast VNA & Hospice, our goal is to give families the knowledge and confidence to step into this active role. This partnership between our clinical team and your family is a cornerstone of effective hospice pain management.
Becoming an Effective Comfort Advocate
As a family member, your observations are invaluable. You know your loved one's normal moods, behaviors, and subtle cues better than anyone.
Being an effective advocate means knowing what to watch for and feeling confident when you communicate with your hospice team. Think of yourself as the team's eyes and ears between our visits.
Noticing small changes—and reporting them right away—allows our Registered Nurses to make timely adjustments to the care plan. Simple yet powerful ways you can be an advocate include:
- Observing and Reporting: Keep a simple log of when your loved one seems comfortable versus when they appear distressed. Note the time and the symptoms you see.
- Maintaining a Consistent Schedule: Giving pain medication on the schedule prescribed by the Registered Nurse is critical. This prevents the cycle of pain from returning.
- Communicating Openly: Never hesitate to call your hospice team with a question or concern. There's no such thing as an insignificant detail when it comes to your loved one’s comfort.
Creating a Soothing Home Environment
Beyond medication and direct care, the atmosphere of the home itself plays a huge role in providing comfort. You have the power to create a peaceful sanctuary.
Small, thoughtful actions can make a world of difference. These acts of care contribute directly to your loved one's sense of well-being and security.
Your presence and touch are powerful non-pharmacological tools. Simply holding a hand, reading aloud, or being quietly present can lower stress and provide a profound sense of connection and peace.
Consider these simple ways to foster tranquility:
- Reduce Sensory Overload: Dim the lights, lower the volume on the television, and minimize loud or sudden noises to create a calm space.
- Engage the Senses Gently: Play favorite, calming music from their past. Use a diffuser with a familiar, pleasant scent like lavender. Offer a soft blanket.
- Encourage Peaceful Moments: If you can, position their bed near a window with a pleasant view. Your own calm and reassuring presence is one of the most comforting things you can offer.
Partnering with Central Coast VNA & Hospice means you are never alone on this journey. We are here to support your entire family with education and reassurance across Monterey, San Benito, Santa Cruz, and South Santa Clara counties.
Taking the Next Steps With Confidence

We've walked through how hospice pain management really works. It’s a combination of a dedicated team, personalized assessments, and a mix of treatments all working together.
This isn't just a service; it's a fundamental right for every person as they near the end of life. The goal is to make sure your loved one feels peace, dignity, and comfort.
The road to end-of-life care can feel uncertain, but you don’t have to wait for a crisis to start getting answers. Looking into hospice is a positive, loving step you can take right now to honor your loved one's wishes.
A Legacy of Trusted, Nonprofit Care
For more than 74 years, Central Coast VNA & Hospice has been a steadfast, mission-driven partner for families in our community. As a local nonprofit, our focus is on people, not profits.
We've had the honor of serving generations of residents across Monterey, San Benito, Santa Cruz, and South Santa Clara Counties. The need for this kind of dedicated support has never been greater.
Starting the conversation about hospice early is one of the most empowering things you can do for your family. It puts the focus back on quality of life. If you're wondering how to begin, we offer guidance on how to prepare your loved one for hospice care.
Choosing hospice isn't about giving up. It's about choosing comfort, embracing peace, and giving your loved one the gentle, dignified care they deserve in the familiar surroundings of home.
Our team is here to walk alongside you on this journey. You are not alone, and we have the expertise to help you navigate this path with confidence.
Take the First Step Toward Peace of Mind
If you think a loved one could benefit from our compassionate hospice services, please reach out. Our team is ready to provide a consultation, answer your questions, and help you understand all of your options.
Contact Central Coast VNA & Hospice today to learn more about how we can bring comfort and dignity to your family when it matters most.
Frequently Asked Questions About Hospice Pain Management
Of all the topics surrounding hospice, pain management is often the one families have the most questions about. It’s completely understandable.
At Central Coast VNA & Hospice, we believe in being open and honest, giving you clear answers so you can feel confident. Here are some of the most common questions we hear.
Will my loved one become addicted to pain medication?
This is a worry we hear all the time, and it comes from a place of deep care. But in hospice, our goals shift completely.
Our primary mission is to provide comfort and ensure the best possible quality of life. The clinical definitions of addiction simply do not apply when treating pain from a terminal illness. Our expert team, led by a physician and a Registered Nurse, manages medications to relieve suffering so your loved one can be comfortable.
What if my family member cannot say they are in pain?
This is where the expertise of a hospice team shines. Our Registered Nurses and Hospice Aides are specially trained to recognize the non-verbal signs of discomfort.
We look for subtle cues like new restlessness, a slight grimace, or a change in breathing patterns. We also see you—the family—as our most essential partners. Your insights help us create a pain management plan that truly meets their needs.
One of our core beliefs is that every person has a right to be free from pain. An inability to speak doesn't change that right one bit. Our team is committed to listening with our eyes and our expertise to provide comfort.
Does pain medication in hospice speed up the end of life?
This is a persistent myth that causes unnecessary fear. The truth is, the goal of pain medication in hospice is to improve the quality of life, not shorten it.
When a person's body is no longer fighting against constant, exhausting pain, they can finally rest more peacefully. The medications prescribed are carefully dosed to provide relief and comfort, not to hasten death.
Are there non-medication options for pain relief?
Yes, absolutely. We believe in a holistic approach because pain isn't just physical. That's why we combine medication with other powerful, comfort-focused therapies.
Some of these non-medication options include:
- Gentle massage to ease tense muscles.
- Therapeutic repositioning to relieve pressure.
- Music therapy to soothe anxiety.
- Emotional and spiritual support from our Medical Social Workers and Chaplains.
Who pays for hospice pain management and medications?
For the vast majority of families, there is no out-of-pocket cost. Hospice care, which includes all team visits, medical equipment, supplies, and medications related to the terminal diagnosis, is covered 100% by the Medicare Hospice Benefit.
This coverage is also provided by Medi-Cal and most private insurance plans. As a nonprofit provider serving the Central Coast for over 74 years, Central Coast VNA & Hospice is committed to ensuring everyone can access this care.
Understanding your options is the first step toward finding peace of mind. To learn more about how our expert team can support your family with compassionate, personalized care, contact Central Coast VNA & Hospice today. Visit us at https://ccvna.com to start the conversation.
