Top Guide: Is Home Nursing Care Better Than a Nursing Facility?
When families ask, "is home nursing care better than a nursing facility?" the answer depends on your loved one. Many find that skilled medical care at home offers a safer and more personal choice. It helps them keep their independence with true one-on-one attention.
Deciding Between Home Nursing Care and a Facility
Choosing the right care for a loved one is a major decision. You want high-level medical support but also want them to feel comfortable. The good news is that you have options and don't have to trade quality for comfort.
Many people believe skilled nursing only happens in a facility. This is a common misstep. In reality, Registered Nurses and therapists can provide these exact services at home.
These services are often covered by Medicare after a hospital stay or during a chronic illness. This makes professional care accessible right where your loved one feels most secure.
Core Differences at a Glance
Home nursing care supports a loved one's wish for Aging In Place Staying Independent. This approach honors their personal routines. It also keeps them connected to their community.
Central Coast VNA & Hospice has served the Central Coast for over 74 years. As a local nonprofit, we help families in Monterey County, San Benito County, Santa Cruz County, and South Santa Clara County navigate these choices every day.
This table shows the key differences between skilled care at home versus in a nursing facility. It helps you see the primary trade-offs at a glance.
At a Glance Comparison: Home Nursing vs. Nursing Facility
| Factor | Home Nursing Care | Nursing Facility |
|---|---|---|
| Environment | The patient's own comfortable and familiar home. | A clinical, institutional setting with multiple residents. |
| Personalization | One-on-one care from a dedicated team of clinicians. | Staff care for multiple residents simultaneously. |
| Independence | Promotes autonomy and allows for personal routines. | Structured schedules for meals, activities, and care. |
| Family Involvement | Easy and frequent access for family visits and participation. | Restricted visiting hours and less direct involvement. |
| Social Interaction | Maintained connections with neighbors and community. | Primarily with other residents and facility staff. |
The choice often comes down to what matters most. Is it the personalized, independent environment of home care? Or is it the structured setting of a facility?
This chart helps show the benefits of each setting. It highlights how home care focuses on comfort and safety. A facility focuses more on clinical structure.

The image shows that home care provides a personal touch. Facilities offer a structured environment with 24/7 on-site staff. You can learn more about how we provide in-home support to avoid a nursing home on the Central Coast.
A Nuanced Look at Clinical Outcomes and Patient Safety
When comparing home nursing to a facility, safety is a top concern. While facilities offer constant supervision, home nursing provides dedicated, one-on-one attention. This personalized focus often leads to better health outcomes.
When a skilled Registered Nurse from Central Coast VNA & Hospice works with a patient, the care plan is very responsive. Any change in health is noticed and addressed quickly. This can stop a small problem from becoming a crisis.

Reducing Risks in a Familiar Environment
A clear advantage of home care is the lower risk of infection. Infections can spread quickly in hospitals and nursing facilities. Receiving care at home reduces this exposure, which is vital for patients with a weakened immune system.
Falls and poor communication are also common concerns in facilities. Skilled care at home offers a safer, more personalized alternative.
Medication management is another area where home nursing shines. A home health Registered Nurse oversees medications, reducing the risk of errors. The nurse also teaches the patient and family about the regimen.
The Healing Power of Comfort
The benefits of being home are mental as well as physical. Familiar surroundings provide a deep sense of comfort, especially for those with dementia. This stability can reduce stress and confusion.
This emotional well-being is tied to better physical health. When a patient feels safe, they tend to rest and eat better. You can read our guide that asks, is it safer to age at home instead of a nursing home?
Data backs this up. A study of Medicare beneficiaries showed a clear survival advantage for those who received skilled care at home.
After one year, 77.7% of home health patients were still alive, compared to just 76.2% of nursing home patients. Even more telling, for patients eligible for both Medicare and Medicaid, long-term care costs were $4,582 higher for nursing home residents.
You can read more in the full study on long-term care outcomes. This research shows that home nursing is a powerful and effective model for managing health. It blends clinical expertise with the comfort of being home.
Breaking Down the Costs of Care
Cost is a major concern when deciding on care. Many families assume a facility is the only option for serious medical needs. However, skilled nursing at home can be more affordable and effective.
The biggest factor is overhead. Nursing facilities have high costs for their buildings, utilities, and round-the-clock staff. These expenses are bundled into their daily rate.
Home nursing care is different. You pay only for the specific, skilled services your loved one needs from a Registered Nurse or therapist. This model cuts out the high overhead costs of a facility.
How Medicare Supports Care at Home
Many families do not realize how home nursing gets paid for. For those recovering from a hospital stay, Medicare often covers the full cost of skilled home health services.
To qualify for Medicare-covered home health, a patient needs to meet a few criteria:
- Be under a doctor's care. A physician must create and review a plan of care.
- Need skilled services. This includes skilled nursing, physical therapy, or speech therapy.
- Be certified as homebound. This means leaving the house requires a lot of effort.
When these conditions are met, Medicare can cover care from an agency like Central Coast VNA & Hospice. You can learn more in our guide on how families afford in-home care long-term.
Comparing the Numbers
Home care's financial edge is clear when looking at national averages. The data shows that receiving care at home is much less expensive than a nursing facility.
Cost comparisons show full-time home care has a national median of $6,292 per month. In contrast, a semi-private room in a nursing home averages $9,277 per month, representing potential savings of up to 32%.
These numbers show how home care helps you avoid paying for a facility's bundled costs.
For families in Monterey County and surrounding areas, this means you can get professional support without the financial strain. Learning about long-term care insurance costs is another key step.
As a nonprofit, Central Coast VNA & Hospice is mission-driven. Our focus is on delivering the highest quality of care. This gives families on the Central Coast peace of mind.
Evaluating Quality of Life and Emotional Well-Being
The care environment has a huge impact on a person’s emotional health. This human element is often the tiebreaker when families decide between home and a facility. The comfort of a familiar home can be very powerful.
Receiving care at home means being surrounded by personal memories and even the family pet. This reinforces a person’s dignity. It is about honoring a life well-lived, not just medical treatment.

Fostering Independence and Connection
Good home nursing care is designed to support independence. Patients keep their own routines and sleep in their own beds. This control helps maintain a sense of purpose.
Staying at home also makes it easier to stay connected with friends and neighbors. Social isolation is a major risk for older adults. Home-based care allows for natural social interactions that support mental health.
Home care prioritizes personal dignity by allowing individuals to receive expert medical care without sacrificing the familiarity and warmth of their own home. It shifts the focus from simply managing a condition to supporting a whole person.
This model helps the whole family. Loved ones can visit freely and take part in care decisions. Read our guide on how to get real support as a family caregiver on the Central Coast.
The Link Between Comfort and Thriving
A person’s environment affects their ability to heal. A calm setting can reduce stress, which has a real effect on physical health. It can lead to better sleep and appetite.
This is especially true for people with cognitive conditions like dementia. A familiar environment can decrease confusion and agitation. The comfort of home provides a stable anchor.
At Central Coast VNA & Hospice, our teams in Monterey County, San Benito County, Santa Cruz County, and South Santa Clara County see this daily. Our Registered Nurses and therapists know that healing is more than medicine. It's about creating an environment where patients feel safe and respected.
How to Choose the Right Care for Your Loved One
Deciding between home nursing and a facility is a personal choice. There is no one-size-fits-all answer, but there is a right answer for your family. This guide gives you a framework to feel confident in your choice.
The best first step is to look at your loved one’s needs. This includes their medical, social, and emotional needs. The right path often becomes clear when you consider the whole person.

Considering Different Health Scenarios
A health condition often points to the best care environment. Here are a few common examples.
- Post-Surgery Recovery: After a surgery like a hip replacement, home nursing is often ideal. A skilled Registered Nurse or Physical Therapist can provide one-on-one care at home to manage pain and guide recovery.
- Chronic Illness Management: For conditions like COPD or diabetes, home health offers consistent medical oversight. A Registered Nurse can help manage medications, monitor symptoms, and teach the patient how to stay healthy.
- Advanced Cognitive Decline: In this case, a facility might be safer. If a loved one with advanced dementia needs 24/7 supervision, a specialized memory care unit is often the best option.
These are general guidelines. The best choice depends on the individual’s needs and support system.
Essential Questions to Ask Yourself
Take a moment to think about your loved one’s needs and what your family can provide. Answering these questions can bring clarity.
- Medical Needs: What specific medical tasks are required, like wound care or IV therapy? How often are they needed?
- Safety and Mobility: Is the home safe and accessible? Can your loved one move around without risk of falling?
- Social and Emotional Needs: How important is their social network? Do they thrive on the comfort of home, or would they enjoy the activities a facility offers?
- Family Support: What level of support can the family truly provide? Be honest about who will be the main point of contact and their limitations.
A growing national trend shows a strong preference for aging in place. Data from 2009 to 2020 reveal that home care workforces expanded while nursing home staffs contracted. This reflects both patient preference and the effectiveness of care at home. You can learn more about this shift toward home care.
How We Can Help on the Central Coast
Navigating these decisions is tough, but you don’t have to do it alone. At Central Coast VNA & Hospice, we help families in Monterey, San Benito, Santa Cruz, and South Santa Clara counties find the right care. Our experienced clinicians can come to the home for an assessment.
We help determine the most appropriate care along our continuum. This may be home health, palliative care, or hospice care. We work with you and your doctor to create a plan that honors your loved one’s wishes. Contact us today to start the conversation.
Your Partner in Home-Based Care on the Central Coast
Figuring out the right care for a loved one is a personal journey. For over 74 years, Central Coast VNA & Hospice has been a nonprofit partner for families like yours. Our mission is to provide expert care right where you want to be—at home.
We understand. Choosing home nursing is about holding onto comfort, dignity, and independence. Our teams of Registered Nurses, therapists, and Hospice Aides are committed to that vision.
Care at Every Stage of Life
A local, community-focused provider can offer continuous support as needs change. Central Coast VNA & Hospice provides a seamless experience for patients and families.
Our continuum of care includes:
- Home Health: Skilled nursing and therapy to help you recover after surgery or manage an illness.
- Palliative Care: Support that focuses on relieving symptoms and stress of a serious illness.
- Hospice Care: Compassionate end-of-life care that puts comfort, dignity, and quality of life first.
This integrated approach means your loved one gets the right support at the right time. They get it all from a single team they know and trust.
Because we’re a nonprofit, mission-driven organization, every decision is guided by what’s best for our patients, not the bottom line. We reinvest our resources into providing exceptional care for our neighbors across Monterey, San Benito, Santa Cruz, and South Santa Clara counties.
If you're in Monterey County or South Santa Clara County and need help, we are here. Our team can come to you for an in-home assessment and answer your questions. Learning why Central Coast VNA is the best choice for home health care can give you peace of mind.
Contact us today to learn how we can support your family with compassionate, professional care at home.
Frequently Asked Questions (FAQs)
Can my loved one get the same level of medical care at home?
Yes. Home health agencies like Central Coast VNA & Hospice bring skilled nursing and therapy right to your door. Our licensed clinicians, including Registered Nurses and therapists, are experts at managing complex needs like wound care and IV therapy under a doctor’s supervision.
Does Medicare cover home nursing care?
Yes, it often does. Medicare will cover skilled home health care if a doctor certifies it is medically necessary and the patient is "homebound." To be homebound means leaving the house requires a major effort.
What happens if their health needs become too complex for home care?
Our team at Central Coast VNA & Hospice continuously assesses a patient’s condition. If needs change, we talk with the family and doctor to decide on the next steps. We help make any transition smooth, whether that means adding palliative services or coordinating with a facility.
Is home care a good option for someone with dementia?
For many, it is an excellent choice in the early-to-moderate stages. The familiar sights of home can reduce confusion and anxiety. For advanced stages that require 24/7 supervision, a specialized memory care facility might be a safer alternative.
What should I do to get started with home nursing care?
The first step is to ask about Medicare-covered in-home nursing. Talk to your doctor, especially after a hospital discharge or during chronic illness, as their order is required. You can also contact Central Coast VNA & Hospice directly if you live in Monterey County, San Benito County, Santa Cruz County, or South Santa Clara County.
Smart Steps: What’s the Best Way to Help My Parents Age in Place?
When you ask, "what’s the best way to help my parents age in place?" the answer is simple. Create a coordinated, proactive plan. It starts with open talks and professional support long before a crisis happens.
This approach means you look at their needs honestly. You make their home as safe as possible and know when to bring in medical help.
Your Proactive Plan for Aging in Place
Many adult children want to support their parents living at home. But they often don't know where to begin. The process can feel overwhelming.
This often leads families to wait until a fall or health emergency. Then, they are forced to make rushed, stressful decisions. But creating a plan now is the most compassionate way to honor your parents’ wishes.
And most seniors want to stay home. Research shows older adults prefer to age in their own homes. According to the World Health Organization, by 2030, one in six people globally will be 60 or older. This makes aging in place more important than ever.
A good aging-in-place plan is not just one action. It is built on a few core pillars that create a strong support system.
The Four Pillars of a Successful Plan
Thinking about the future can feel hard. The key is to break the challenge into smaller parts. A proactive plan focuses on four areas.
These areas are assessing needs, making the home safe, coordinating care, and planning for the future. This framework helps you handle the most critical parts of aging at home.
This visual guide breaks down the 4-step process for building a plan that works.

As the infographic shows, each step builds on the last. This creates a full support structure for your parents.
The table below explains these four pillars. It lists key actions for each and why they are so important.
Four Pillars of a Successful Aging-in-Place Plan
| Pillar | Key Actions | Why It Matters |
|---|---|---|
| 1. Honest Assessment | Talk openly about health, finances, and what they want. Involve doctors to get a clear picture of their needs. | This avoids guesswork and makes sure the plan is based on reality. It gives your parents a voice. |
| 2. A Safe Home | Install grab bars, improve lighting, remove trip hazards, and consider things like walk-in showers. | This prevents falls, which often trigger a health crisis. It allows for independence in a secure home. |
| 3. Coordinated Care | Arrange for home health services from a Registered Nurse or Physical Therapist if needed. Use a shared calendar to track appointments. | A strong support network ensures all medical and daily needs are met. It also prevents family burnout. |
| 4. Future-Proofing | Complete legal documents like a Power of Attorney. Discuss long-term financial plans and know the signs when more help is needed. | This prepares you for unexpected changes. It removes legal stress during an emergency so you can focus on care. |
This structured approach turns a vague hope into a real plan. It gives everyone a clear roadmap to follow.
The most common mistake families make is waiting for a crisis to start planning. Being proactive is the best way to protect your parents' independence and reduce stress.
For families in Monterey County, San Benito County, and nearby areas, you don't have to do this alone. For over 74 years, Central Coast VNA & Hospice has been a trusted local nonprofit partner. We help families navigate these challenges.
Our expertise is providing compassionate care at every stage, from home health to palliative and hospice care. To learn more, read our guide on what aging in place really means for families.
Adapting the Home for Safety and Independence
A safe home is the foundation of aging in place. Our homes are our comfort zones. But as parents' mobility changes, familiar spaces can hide new risks.
The goal is to proactively shape their environment. This supports their independence and keeps them safe. It is more than just a checklist.
It's about looking at their home through their eyes. Small changes can make a huge difference in their safety and confidence. This is true whether they live in Monterey or Salinas.

A Room-by-Room Approach to Safety
Start by walking through the house with your parents. Look at each space with a "safety first" mindset. When you do it together, they feel like part of the solution.
Focus on the high-impact changes first. These are often simple and cheap tweaks that can lower the risk of an accident.
Key Areas for Immediate Attention:
- Pathways and Floors: Clear walkways of clutter and cords. Area rugs are a major trip hazard, so secure them with tape or remove them.
- Lighting: Make sure every room, hallway, and staircase is bright. Add nightlights to bedrooms, bathrooms, and hallways for safer navigation at night.
- Stairs: Check that all handrails are sturdy. If possible, install them on both sides of the staircase and add non-slip treads to each step.
Once you’ve handled these basics, you can focus on specific rooms.
Focusing on Critical Zones: The Bathroom and Kitchen
The bathroom and kitchen are the two most critical areas to address. Bathrooms are risky because of wet surfaces. Kitchens involve reaching, bending, and handling hot items.
In the bathroom, the top priority is preventing slips and falls. This is where you can make life-saving adjustments.
Bathroom Safety Must-Haves:
- Grab Bars: Install sturdy grab bars next to the toilet and in the shower. Never rely on suction-cup bars as they are not a safe substitute.
- Non-Slip Surfaces: Use non-slip mats or decals inside the tub and on the floor.
- Accessible Seating: A shower chair can reduce fatigue. A raised toilet seat can make a big difference for stiff joints.
If your parents' needs are greater, a full aging in place bathroom remodel might be a good long-term solution. For more tips, check our guide on preventing falls in the home.
In the kitchen, it's all about easy access. You want to reduce the need for your parents to bend or stretch.
Rearrange cabinets so that frequently used items are on lower, easy-to-reach shelves. This simple change reduces the need for a step stool, a common cause of falls.
Knowing When to Bring in Professional Help
Many of these changes are simple DIY projects. But some things need a professional, like installing grab bars or stairlifts.
If you’re not sure where to start, a professional home safety assessment can help. At Central Coast VNA & Hospice, our skilled Physical Therapists and Occupational Therapists can provide an expert evaluation as part of our home health care services. We serve families across Monterey, Santa Cruz, and South Santa Clara Counties.
Integrating Professional Home Health Services

Making the house safe is a key first step. But what happens when your parent needs more than grab bars? Managing chronic conditions like diabetes or heart failure can feel like a full-time job.
This is where professional home health services become essential. These skilled services bring clinical experts right into your parent’s home. They create a bridge between their doctor's office and daily life.
The goal is to manage health issues proactively. This helps prevent hospital visits that can disrupt an older adult’s life. For many families on the Central Coast, this support is the key to aging in place with dignity.
What Home Health Care Actually Involves
Home health care is different from non-medical help. This is skilled medical care prescribed by a doctor. It is often covered by Medicare after a hospital stay or a change in health.
A dedicated home health team from a trusted local nonprofit like Central Coast VNA & Hospice can help. This team works under a doctor's orders to create a personalized care plan.
A typical home health team might include:
- Registered Nurses: They manage medications, provide wound care, and teach you how to manage an illness at home.
- Physical Therapists: They focus on rebuilding strength and improving balance after a fall or surgery.
- Occupational Therapists: They help your parent regain the ability to handle daily tasks like bathing and dressing.
- Speech-Language Pathologists: These specialists help with communication or swallowing problems after a stroke.
This team approach means every part of your parent's health is addressed. All of this happens in the comfort of their home.
The Benefits of Clinical Oversight at Home
Home health is valuable because it is proactive. A skilled clinician can spot warning signs early. A Registered Nurse might notice subtle changes in your mom’s condition before it becomes a crisis.
This professional oversight leads to better health outcomes. It also gives families peace of mind. You can learn more by exploring our home health care services.
By managing symptoms and providing education at home, skilled home health care reduces the chance of re-hospitalization. This stability is key to helping your parents age in place successfully.
For families in Monterey County, San Benito County, Santa Cruz County, and South Santa Clara County, having a reliable partner is vital. As a nonprofit home health provider with over 74 years of local service, Central Coast VNA & Hospice is committed to our community. Our mission is to provide a seamless continuum of care, from home health to palliative or hospice care.
If your parent is struggling to manage their health, don't wait. Contact us today to learn how our compassionate, expert team can help.
Planning for the Future

Helping your parents stay safe at home means more than just physical support. It also means preparing for the future. You need to have crucial talks about their legal, financial, and healthcare wishes.
These talks can feel hard. But starting them early is a gift of clarity for everyone. It ensures their future is guided by their values. This is called advance care planning.
Starting the Conversation
Starting these talks requires a soft touch. The goal is to understand their wishes, not to take control. Frame the conversation around empowerment, so their voice is heard.
Try starting with gentle questions like:
- "Mom, if you ever got sick and couldn't speak for yourself, who would you want to make medical decisions for you?"
- "Dad, have you thought about what kind of medical care you would want in certain situations?"
- "It would give me peace of mind to know we have a plan in place that respects your wishes."
These questions open the door for a real dialogue. Remember to listen more than you talk.
The most loving thing you can do is ensure your parents' values guide their future care. These conversations honor their independence.
Essential Legal Documents
Once you’ve started talking, make their wishes official with legal documents. These papers give authority to the people your parents choose to act for them.
Key Advance Care Planning Documents:
- Durable Power of Attorney for Healthcare: This names a "healthcare agent" to make medical decisions if your parent is unable.
- Living Will (Advance Directive): This outlines specific wishes for end-of-life medical treatments.
- Durable Power of Attorney for Finances: This appoints someone to manage financial matters like paying bills.
For help, you can look at guides on Power of Attorney for aging parents. Having these documents prepared by a legal professional is always a good idea.
For families in Monterey, Santa Cruz, or San Benito County, we can help. As a local nonprofit with over 74 years of experience, Central Coast VNA & Hospice offers compassionate guidance. Our palliative care team can help facilitate these talks.
When to Consider Palliative and Hospice Care
As your parents age, comfort may become the main priority. Palliative or hospice care is not about giving up. It is about wrapping your loved one in expert support when they need it most.
Palliative care can start at any stage of a serious illness. It focuses on relief from symptoms like pain and stress. It works alongside other medical treatments.
Hospice care is for when life expectancy is six months or less. It focuses on quality of life instead of curative treatments. For a deeper look, see our guide on the Difference Between Hospice and Palliative Care.
Central Coast VNA & Hospice offers a seamless continuum of care. Our team ensures that if needs change, the transition from home health to palliative or hospice care is handled with expertise. We have supported families in Salinas, Santa Cruz, and across the Central Coast for over 74 years.
Frequently Asked Questions (FAQs)
1. How early should we start planning for aging in place?
The best time to start is now, before a crisis happens. Planning early gives your parents a voice in their future. It allows you to explore options without pressure.
2. What if my parents are resistant to getting help?
This is normal and often comes from a fear of losing independence. Frame conversations around preserving their freedom. For example, explain that grab bars can help them stay independent at home longer.
3. What are the first steps to making my parents' home safer?
Start with a walk-through to identify risks. Focus on improving lighting, removing trip hazards like rugs, and installing grab bars in the bathroom.
4. What is the difference between home health and palliative care?
Home health provides skilled medical care, like nursing or physical therapy, to help someone recover from an illness or injury. Palliative care focuses on relieving symptoms and stress from a serious illness and can be provided at any time, even alongside curative treatment.
5. How can Central Coast VNA & Hospice help my family?
As a local nonprofit with over 74 years of experience, we provide a full continuum of care in Monterey, San Benito, Santa Cruz, and South Santa Clara counties. We offer home health, palliative care, and hospice services to support your parents at every stage of their health journey.
If you're asking, “What’s the best way to help my parents age in place?” the first step is to talk to a trusted partner. At Central Coast VNA & Hospice, we are a mission-driven nonprofit here to provide care at every stage. Contact us today to learn how we can support your family.
Can Someone with Dementia Go on Hospice? An Essential Guide
Yes, a person with dementia can absolutely go on hospice. It’s a question that weighs heavily on families, and the answer brings both relief and a path forward.
Many families delay this crucial support because dementia’s progression is unpredictable. It’s often a slow decline, not a sudden event. This uncertainty can leave families feeling lost and leads to missed opportunities for comfort and peace.
Choosing hospice isn't about giving up. It's a decision to shift the focus from trying to cure an incurable disease to ensuring the highest possible quality of life.
Understanding When Hospice Is the Right Choice for Dementia
Navigating a dementia diagnosis is a tough journey for any family. As the disease advances, priorities shift from aggressive treatments to making sure your loved one is comfortable and free from pain. Answering the question, “Can someone with dementia go on hospice?” is the first step toward compassionate care.
Hospice is designed for the final phase of a terminal illness. For a person with dementia, this means focusing on them as a whole person, not just the disease. It's about managing symptoms like agitation while providing emotional and spiritual support for everyone involved.
The Importance of Early Conversations
A common misstep is waiting for a doctor to bring up hospice. Families might also wait for a major health crisis to force the conversation. It's easy to overlook the subtle signs of decline that signal eligibility for this care.
Some of these indicators can include:
- Frequent infections, like recurring pneumonia or urinary tract infections (UTIs).
- A noticeable decline in mobility, needing more help to walk or stand.
- Significant, unintentional weight loss over the last six months.
- Increasing difficulty with speaking, often using just a few words or becoming non-verbal.
Recognizing these changes early allows for a calmer transition to comfort-focused care. At Central Coast VNA & Hospice, a nonprofit provider with over 74 years of service, we encourage families in Monterey and Santa Cruz Counties to talk sooner. You can learn about specific hospice eligibility requirements.
To help families identify these signs, here is a quick reference table.
Key Indicators for Hospice Eligibility in Dementia
| Indicator Category | Specific Signs to Watch For |
|---|---|
| Functional Decline | Needing help with most daily activities like dressing, bathing, and eating. |
| Communication | Speaking only a few words a day or becoming non-verbal. |
| Mobility | Unable to walk without assistance; often chair-bound or bed-bound. |
| Swallowing Issues | Frequent coughing or choking during meals; difficulty swallowing food or liquids. |
| Recurrent Infections | Frequent UTIs, pneumonia, or sepsis. |
| Weight Loss | Significant, unintentional weight loss (typically 10% or more) in the past six months. |
Watching for a combination of these indicators provides a clearer picture of when your loved one might be ready for hospice.
Hospice shifts the focus from curative treatment to compassionate care. It’s a decision to prioritize comfort, manage pain, and provide emotional support, ensuring a loved one’s final chapter is lived with dignity and peace in the familiar surroundings of home.
Choosing hospice brings a dedicated team of professionals—including a Registered Nurse, a Hospice Aide, and a Medical Social Worker—directly into your home. This support system helps manage symptoms around the clock. This reduces stressful hospital visits and allows your family to focus on making memories together.
Understanding the Hospice Criteria for Dementia
When caring for a loved one with dementia, figuring out if it’s time for hospice can feel overwhelming. The decision is based on specific medical guidelines that help identify when the focus should shift toward comfort.
Knowing these criteria can empower families in Monterey County and surrounding areas to have clearer conversations with doctors. The main tool used to measure dementia's progression is the Functional Assessment Staging (FAST) scale.
It also helps to start with a big-picture view, like understanding the different kinds of dementia. This context helps explain why the disease can look so different from one person to the next.
The Role of the FAST Scale
The FAST scale lays out seven distinct stages of dementia. For hospice eligibility, clinicians look closely at Stage 7. This stage signals a severe decline in a person's ability to function.
Stage 7 is marked by a few key signs:
- Loss of Mobility: The person can no longer walk without help and might be confined to a bed or chair.
- Impaired Speech: Communication is extremely limited, often six intelligible words or fewer per day.
- Dependence on Others: They need help with all activities of daily living, from dressing and bathing to eating.
A person doesn't have to show every single one of these signs. Reaching this advanced stage is the first major indicator for hospice.
Beyond the FAST Scale: Other Important Factors
Clinicians always look at the whole person. Along with the FAST scale, they consider other medical complications that have popped up within the last year. These secondary conditions are a sign that the body is weakening.
The flowchart below shows how the journey from a dementia diagnosis can lead toward a focus on comfort care.

As the disease moves forward and daily abilities decline, the focus naturally shifts to providing compassionate, comfort-oriented care.
Here are some of the crucial secondary factors doctors look for:
- Recurrent Infections: This might mean repeated bouts of pneumonia, sepsis, or frequent urinary tract infections (UTIs).
- Significant Weight Loss: An unintentional loss of 10% or more of their body weight in the last six months is a key indicator.
- Trouble Swallowing (Dysphagia): This can cause choking, lead to aspiration pneumonia, and make it difficult to get enough food and fluids.
When a person in Stage 7 dementia also has one or more of these secondary conditions, they will likely meet the medical criteria for hospice. We cover this topic in more detail here: How Doctors Determine Hospice Eligibility.
The Challenge of a Six-Month Prognosis
One of the biggest hurdles for families is Medicare's rule that a doctor must certify a life expectancy of six months or less. With dementia, predicting that timeline is incredibly difficult. Dementia often progresses slowly and unpredictably.
According to the National Hospice and Palliative Care Organization (NHPCO), over 1.72 million Medicare beneficiaries received hospice services in 2020 (NHPCO, 2021). Still, many with dementia are referred late. This data shows just how important it is for families to understand all the eligibility criteria.
If your loved one lives in Santa Cruz, San Benito, or South Santa Clara County, our team at Central Coast VNA & Hospice is here to help. We can offer a no-obligation consultation to talk through your loved one’s situation.
Why Earlier Hospice Enrollment Makes a Difference
Many families see choosing hospice as giving up. But it’s exactly the opposite. It's about choosing a better quality of life for the time that’s left.
Starting hospice care sooner allows an expert team to get ahead of distressing symptoms like pain and anxiety. This specialized care can prevent late-night trips to the emergency room. It empowers your loved one to spend their final months where they are most comfortable—at home.

A Focus on Whole-Person Comfort
Hospice care isn’t just about managing physical symptoms. At Central Coast VNA & Hospice, our team works together to address the complex needs that come with late-stage dementia.
Our goal is to improve day-to-day life by creating a calm and dignified environment. This comprehensive approach helps ensure your loved one’s final chapter is lived with grace.
The benefits of this early support are backed by research. A UCSF study of 2,059 Medicare seniors found that 59% of those with dementia who enrolled in hospice received excellent end-of-life care. That rate surpassed those who didn't use hospice. You can discover more insights about these findings on UCSF.edu.
Enrolling in hospice sooner means more time for symptom control, more opportunities for meaningful connection, and more support for the entire family. It shifts the focus from crisis management to quality of life.
Support for the Entire Family
A dementia diagnosis impacts everyone in the family. The emotional and logistical challenges can feel overwhelming. Hospice provides an essential layer of support for family, helping you navigate this journey with less stress.
Our team at Central Coast VNA & Hospice supports the whole family. We provide guidance and resources in our communities, from Salinas to Santa Cruz.
- Medical Social Workers help families navigate complex dynamics and connect with community resources.
- Chaplains offer non-denominational spiritual support, providing comfort that aligns with your family's beliefs.
- Hospice Aides provide practical, hands-on assistance with personal care.
- Registered Nurses are on call 24/7, giving you peace of mind that expert help is just a phone call away.
This team-based approach means you never have to walk this path alone. You can learn more about starting hospice sooner in our guide for families.
As a nonprofit provider serving Monterey County, San Benito County, Santa Cruz County, and South Santa Clara County for over 74 years, our mission is to bring compassionate care to every family who needs it.
How to Start the Hospice Conversation
Talking about hospice can feel like an impossible weight. It’s a conversation that comes from a place of love, yet finding the right words is often the hardest part. The best approach is a gentle one, involving your family and your loved one's doctor.
Starting this dialogue isn’t about giving up. It's about changing the focus to what truly matters now: making sure your loved one’s final chapter is lived with dignity.
When you discuss end-of-life wishes, you may encounter legal documents. Tools like a Texas durable power of attorney for health care can empower family members to be strong advocates for their loved one's choices.

Talking to Your Family and the Doctor
The first step is getting key family members together. Find a quiet time to talk. You can open the conversation by sharing what you’ve noticed about your loved one's health.
Try using "I" statements to share your feelings. For instance, "I've been worried about Mom's comfort lately, and I want to be sure we're doing everything possible to support her."
Next, schedule an appointment with your loved one’s doctor. Go in with a list of the specific changes you’ve seen. This gives the physician a fuller picture.
Don't be afraid to ask direct questions:
- "We've noticed these changes... Do you think it’s time we focus more on comfort care?"
- "What are your thoughts on hospice at this stage?"
- "Could you help us understand the benefits hospice might offer right now?"
Our guide on how to talk to your parents about hospice care has more practical tips for these sensitive talks.
Understanding the Admission Process
Once your family decides to explore hospice, the process is straightforward. For families in Salinas, Santa Cruz, and nearby areas, Central Coast VNA & Hospice provides a clear and supportive path.
Here’s what you can generally expect:
- The Initial Call: It starts with a simple phone call. You can ask questions and learn about our services with no commitment.
- A No-Obligation Visit: A Registered Nurse will schedule a visit to your loved one’s home. This is an assessment to understand their needs and confirm eligibility.
- Creating the Care Plan: If you move forward, our team works with you and the doctor. Together, we create a personalized care plan.
The hospice admission process isn't about losing control; it's about gaining a dedicated team of experts. This team comes to you, providing comprehensive, compassionate care right in the comfort of home, 24/7.
As soon as someone is admitted, the support begins. You'll get regular visits, hands-on help with personal care, and 24/7 on-call support. This brings an incredible sense of peace, allowing families to spend quality time together.
Specialized Dementia Care on the Central Coast
When navigating advanced dementia, choosing the right care partner is a profound decision. It's about finding a local team in Monterey or Santa Cruz County that understands our community.
Central Coast VNA & Hospice is that partner. For over 74 years, we’ve served our neighbors as a nonprofit home healthcare provider. Our mission is simple: we are guided by people, not profits.
The Continuum of Care: A Seamless Approach
Dementia is a journey, and your loved one's needs will change over time. That’s why we offer a seamless continuum of care that adapts with them. This approach prevents the stress of changing agencies when consistency matters most.
Our services flow together to meet you where you are:
- Home Health: In the earlier stages, our home health nursing and therapy teams can help manage health conditions at home.
- Palliative Care: As symptoms become more challenging, palliative care at home can be added for expert symptom management.
- Hospice Care: When the focus shifts to comfort, the transition to our hospice service is smooth.
This continuum ensures your loved one gets the right support at the right time. It all comes from one trusted organization rooted on the Central Coast.
Your Dedicated In-Home Hospice Team
When your family chooses Central Coast VNA & Hospice, you welcome an entire team of compassionate experts into your home. Each person plays a vital role, creating a circle of support around your loved one and your family.
Your dedicated team includes:
- Registered Nurse: Manages the care plan and provides expert pain and symptom control.
- Hospice Aide: Offers gentle, hands-on help with personal care like bathing and dressing.
- Medical Social Worker: Provides emotional support and practical guidance for families.
- Chaplain: Offers non-denominational spiritual comfort for patients and families of all beliefs.
At Central Coast VNA & Hospice, our team-based model means you are never alone. We provide 24/7 on-call support, so peace of mind is always just a phone call away.
Families across Monterey County, San Benito County, Santa Cruz County, and South Santa Clara County have trusted us for generations. As you explore your options, you might find our guide on who offers the best hospice care for parents near Monterey helpful.
Contact us today. Families in Santa Cruz, Salinas, and nearby areas can call VNA for a no-obligation hospice consultation today.
Frequently Asked Questions About Hospice for Dementia
1. What is the main goal of hospice care for someone with dementia?
The main goal is to maximize comfort and quality of life. Hospice care focuses on managing symptoms like pain, anxiety, and agitation. It also provides emotional and spiritual support for both the patient and their family.
2. Can a person with dementia refuse hospice care?
Yes, if they still have the capacity to make their own healthcare decisions. If they can no longer do so, the decision falls to their legally appointed healthcare agent. This person is expected to make choices based on the patient's known wishes.
3. Does choosing hospice for dementia mean we are giving up?
Not at all. Choosing hospice is a shift in focus. Instead of seeking a cure, the hope is for comfort, peace, and dignity. It is a proactive choice to ensure the best possible quality of life during the final months.
4. What happens if my loved one lives longer than six months on hospice?
The six-month prognosis is a guideline for admission, not a time limit. A person can continue to receive hospice care as long as their doctor recertifies that they have a life-limiting illness. Hospice support continues for as long as it is needed.
5. Who pays for hospice care for a person with dementia?
Hospice care is typically covered 100% by Medicare Part A. Medicaid and most private insurance plans also offer comprehensive coverage. This includes the care team's services, medications for symptom control, medical equipment, and supplies.
At Central Coast VNA & Hospice, our nonprofit mission is to provide compassionate, expert care that supports patients and families at every stage. If you have more questions, we are here to help. Contact us today for a no-obligation consultation to learn more about our home health, palliative, and hospice care in Monterey County. Learn more at ccvna.com.
Beyond the Basics: How Skilled Nursing Fits into Whole-Person Care
Skilled nursing is often seen as short-term medical care after a hospital stay. But it is much more. It can be the start of whole-person care.
This approach uses one team to manage a patient's physical, emotional, and social needs. It prevents scattered care and builds long-term stability at home. It creates a roadmap for the entire care journey.
Rethinking Skilled Nursing in Modern Healthcare
When a loved one comes home from the hospital, families focus on immediate tasks. This can include managing medicines or helping with therapy. Many providers view skilled nursing as a temporary service with a clear start and end.
This limited view often creates a gap in care.
After short-term recovery ends, families are often left alone. This happens in communities from Salinas to Santa Cruz. They must find new providers and manage complex needs without a clear path, adding to their stress.
The Problem with Fragmented Care
Fragmented care happens when healthcare providers do not communicate. Families must repeat medical histories and manage transitions on their own. This lack of coordination can lead to serious problems.
Without a unified team, small health issues can be missed. They can become emergencies. This often results in hospital readmissions that could have been prevented.
A Seamless Approach to Health at Home
At Central Coast VNA & Hospice, we offer a different path. For over 74 years, our nonprofit mission has been to provide a full continuum of care. We ensure patients in Monterey County and San Benito County get seamless support.
Our interdisciplinary teams include Registered Nurses, therapists, and Medical Social Workers. They work together from day one. This model ensures care plans are built around the whole person, not just one health issue.
Skilled Nursing: Traditional View vs. Whole-Person Care
| Care Aspect | The Traditional View | The Whole-Person Approach |
|---|---|---|
| Focus | Treats a specific medical issue, like a wound or post-op recovery. | Addresses the patient's complete physical, emotional, and social needs. |
| Timeline | Short-term service that ends when the immediate issue is resolved. | A continuous journey that adapts as the patient's needs change. |
| Team Structure | Separate providers who work independently and may not communicate. | An integrated team that works together on a single care plan. |
| Goal | Fix the immediate problem and discharge the patient from service. | Achieve long-term stability, prevent future crises, and improve quality of life. |
| Family Role | Often left to coordinate services and fill care gaps on their own. | Supported as an essential part of the care team. |
This table shows a shift in thinking. Instead of restarting the care process with each new challenge, your family gets a single, trusted team. This continuity improves patient safety and reduces family stress.
Deciding on the right environment is also key. Many families wonder if skilled nursing care at home is better than a facility for their loved one's needs.
Understanding the Power of Whole-Person Care
What is “whole-person care”? It is like a dedicated pit crew for a race car. Each person has a specific job, but they all work together toward one goal.
This approach focuses on a person’s complete well-being. This includes their emotional, social, and spiritual health. Our team creates a care plan that supports every part of a person's life.
More Than Just Medical Tasks
In traditional healthcare, different providers often work alone. A nurse might handle medicines while a therapist focuses on movement. Whole-person care brings everyone to the same table.
This teamwork is critical for managing chronic illness. A staggering 95% of adults over 60 live with at least one chronic condition, and 80% have two or more. An integrated team is the best defense against fragmented services that can lead to confusion and unnecessary hospital trips.
The Team Behind the Care
Our whole-person care is brought to life by a team of professionals. Each member contributes their unique skills to support your family.
- Registered Nurses manage complex medical needs, from medication to wound care.
- Physical, Occupational, and Speech Therapists work to restore function, improve safety, and help patients regain independence.
- Medical Social Workers offer emotional support and connect families with community resources.
- Chaplains provide spiritual guidance and comfort to patients and their loved ones.
This infographic captures the shift from a confusing system to the seamless approach of whole-person care.

As you can see, a coordinated care model leads to fewer crises and better health. It also brings peace of mind for families.
Why This Coordinated Approach Matters Now
The need for coordinated, whole-person care is more urgent than ever. Staffing shortages continue to challenge the healthcare system. Today, nursing facility residents get an average of just 3.85 hours of nursing care per day.
This is a 7% decline from a decade ago. It is driven by a 19% drop in registered nurse hours.
By bringing a full team into a patient’s home, we bridge the gaps left by a strained system. This ensures every patient receives consistent, high-quality attention.
Embracing whole-person care means considering every aspect of well-being. This can include proactive steps like getting at-home health testing insights. Our model is designed to improve quality of life, which is why it is important to know that palliative care isn't just for the end of life.
How Skilled Nursing Anchors the Care Continuum
For many families on the Central Coast, their journey with us starts with skilled nursing. It often begins after a hospital stay or a new diagnosis. But this service is more than a temporary fix—it’s the anchor for our continuum of care.
Our Registered Nurses are highly trained professionals. They do more than manage medicines. They become our eyes and ears in your home, seeing the complete picture of your loved one’s well-being.

Having this consistent presence in the home is what makes our model work. It allows our team to spot a family’s changing needs before they become a crisis.
The Nurse as a Central Coordinator
Picture this: a skilled nurse is visiting a patient recovering from pneumonia. The nurse checks vitals and gives medicine. They also notice the patient seems withdrawn and is in pain.
In a disconnected system, these details might be missed. But at Central Coast VNA & Hospice, our nurse acts as a central coordinator. They know that health is about more than just physical symptoms.
Connecting the Dots for Better Care
Our skilled nurses are trained to see when more support is needed. They act as the link between different levels of care.
Here’s how they connect the dots:
- Identifying Palliative Care Needs: If a patient has ongoing pain or other symptoms, the nurse can bring in our palliative care team to improve comfort.
- Engaging Social Work Support: When a family is stressed by financial worries or caregiving, a nurse will bring in a Medical Social Worker for guidance.
- Integrating Therapy Services: If a patient is at risk for falls, the nurse will coordinate with our therapists to build strength and make the home safer.
This integrated approach means you have one team looking out for your loved one. It prevents the frustration of starting over with new providers. You can explore our guide on how VNA is reducing hospital readmissions on the Central Coast.
Building a Foundation for Long-Term Stability
By anchoring the care continuum, skilled nursing sets the stage for future success. It ensures the care plan is a living roadmap that adapts to your family’s needs. It is a proactive model designed to prevent emergencies and reduce hospital visits.
Physical comfort also plays a huge role in well-being. For example, things like adjustable beds for seniors can make a big difference in comfort. Our nurses look at the entire home to make recommendations that improve daily life.
At Central Coast VNA & Hospice, skilled nursing is not just a service—it’s the beginning of a partnership. Our goal is to build a foundation of trust and stability that supports your family.
Why Integrated Care Reduces Family Stress and Prevents Crises
Navigating healthcare can feel like solving a puzzle with missing pieces. Families often repeat medical histories and make stressful trips to the emergency room. This reactive cycle leaves everyone exhausted.
The stability of a single, trusted team makes all the difference. When care is coordinated, worry is replaced by confidence and peace of mind. The benefits create a supportive journey instead of a chaotic one.

From Chaos to Coordination
Imagine an elderly man is discharged from the hospital after a fall. He has new prescriptions and follow-up appointments with different specialists. His daughter is left to coordinate everything.
This creates constant stress. Every new symptom feels like a crisis. It is emotionally draining and can lead to poor health outcomes.
Now, imagine the alternative with Central Coast VNA & Hospice. Our skilled nurse visits the same man at his home in Salinas. The nurse manages his medications and also listens to the family’s concerns.
With a single point of contact, the family knows who to call. The nurse becomes their partner, proactively addressing issues before they get worse.
The Tangible Benefits of a Single Team
Having one team from a nonprofit provider like CCVNA transforms the care experience. Instead of starting over with each new service, families gain continuity and trust. This is true for people in Hollister, Monterey, and Santa Cruz County.
The benefits are clear:
- Reduced Family Stress: Loved ones no longer have to manage a complex healthcare puzzle. We handle the coordination.
- Improved Patient Safety: With a team that communicates constantly, there's less risk of medication errors or missed symptoms.
- Fewer Hospitalizations: Our proactive approach helps manage chronic conditions at home, preventing crises that lead to ER visits.
Workforce challenges in nursing facilities are reshaping care. You can learn more by reading these insights on nursing facility challenges. This reality reinforces the value of home-based services, where patients get coordinated care.
We also offer resources for the challenges of being a family member providing care. You can find help in our article on support for family caregivers.
Navigating Your Journey with Central Coast VNA & Hospice
Taking the first step to get support for a loved one can feel overwhelming. We understand. We have made accessing our care as simple as possible.
You do not need a doctor's referral to contact us. If you're in Monterey County, San Benito County, Santa Cruz County, or South Santa Clara County, you can call us. We are here to listen and help you review your options for home health, palliative, and hospice care.
How to Get Started
The process starts with a simple conversation. Our team will ask about your loved one's health and what your family hopes to achieve. From there, we can see if they are eligible for services.
As a nonprofit organization for over 74 years, our decisions are guided by your needs. Our mission-driven focus means we are committed to delivering the right care at the right time.
Understanding Your Coverage
Insurance can be confusing, but we are here to help. Our services are covered by a wide variety of plans.
Coverage typically includes:
- Medicare: Most of our home health and hospice patients find their care is 100% covered by Medicare.
- Medi-Cal: We work with Medi-Cal to provide essential services for those who are eligible.
- Private Insurance: We accept many private insurance plans and can help you verify your coverage.
The financial weight of healthcare is a big worry for families. Home-based services from a nonprofit like ours offer a clear advantage. We help reduce healthcare costs while allowing your loved one to stay independent at home. You can read more about these cost trends in senior care.
Our commitment as a nonprofit is to ensure that care decisions are based on what is best for your family. We help you explore all coverage options.
This focus on accessible, high-quality care at home is critical. We help families avoid the high costs and strain of repeat hospitalizations. For a deeper dive, check out our guide on whether you can get skilled nursing care without moving your parent.
Your Partner on the Central Coast
If you are managing complex care in Monterey, Hollister, Salinas, or Santa Cruz, you are not alone. A single call can connect you with a team that has been a trusted partner for generations.
Let us show you how an integrated care plan can bring stability and peace of mind. Contact us today to learn more about our services.
Frequently Asked Questions
1. What is whole-person care?
Whole-person care is an approach that addresses a patient's complete needs. This includes their physical, emotional, social, and spiritual well-being. A single, coordinated team works together to create a unified care plan.
2. How is skilled nursing different from other home care?
Skilled nursing care is provided by a licensed medical professional, like a Registered Nurse. It involves clinical tasks such as wound care, medication management, and patient education. Other types of home care may focus on non-medical support like daily chores or personal hygiene.
3. Will my loved one lose their primary doctor?
No. Our team works closely with your loved one’s primary care physician and specialists. We act as an extension of their medical team, providing regular updates from the home. This collaboration ensures everyone is on the same page.
4. How do we know when it's time to consider palliative or hospice care?
Our team helps guide these decisions. If a skilled nurse notices that symptoms are becoming harder to manage, they will start a gentle conversation with your family. We explain the options clearly, so you can make an informed choice that is right for your loved one.
5. How are your services paid for?
Our services are covered by Medicare, Medi-Cal, and most private insurance plans. For eligible patients, Medicare often covers 100% of the cost for home health and hospice. As a nonprofit, our goal is to provide the best care regardless of a family's financial situation.
At Central Coast VNA & Hospice, our mission is to provide compassionate, high-quality care that supports the whole person. If you are managing complex care at home in Monterey, Hollister, Salinas, or Santa Cruz, you don’t have to do it alone. Contact us today to learn how our integrated team can bring peace of mind to your family. https://ccvna.com
What’s the Difference Between Hospice and Palliative Care?
The main difference between hospice and palliative care comes down to timing and goals. Both types of care focus on comfort and improving quality of life for people with serious illnesses.
Palliative care can start at any time during a serious illness. You can receive it while you are also getting treatments to cure your illness. Hospice care is for someone with a life expectancy of six months or less who is no longer seeking a cure.
Understanding the Core Differences in Supportive Care
People often use the terms “hospice” and “palliative care” to mean the same thing, especially in moments of crisis. While both provide comfort and dignity, they are not the same. Knowing the difference can help you and your family get the right support sooner.
A common mistake is waiting too long to request palliative care. Many people think it means “giving up,” but that is not true. Research shows that palliative care, when started earlier, improves quality of life and symptom control.
Palliative care is not about stopping treatment. It’s about adding a layer of expert support to help you live better while you continue your treatments.
Understanding these differences is the first step toward making informed decisions. At Central Coast VNA & Hospice, our mission is to offer compassionate guidance. Learn about our services, from home health to palliative and hospice care, to see how we support local families.

Hospice vs. Palliative Care: A Quick Comparison
This table offers a simple, side-by-side look at what makes each type of care unique. It breaks down who qualifies, the main goals, and when each service is best.
| Feature | Palliative Care | Hospice Care |
|---|---|---|
| When It Starts | At any stage of a serious illness, often at diagnosis. | When life expectancy is six months or less. |
| Treatment Goal | To relieve symptoms and stress alongside curative treatments. | To provide comfort and quality of life when curative treatment ends. |
| Curative Care | Provided at the same time as treatments like chemotherapy. | Not provided; the focus is on comfort and symptom management. |
| Who Qualifies | Anyone with a serious illness, regardless of prognosis. | Anyone with a terminal diagnosis certified by a physician. |
| Location | Typically provided at home, in clinics, or during hospital stays. | Provided wherever the patient calls home, including facilities. |
This table helps clarify the main purpose of each service. Both are valuable, but they serve different needs at different times.
A Deeper Look Into Palliative Care Support
When facing a serious illness, medical care often focuses on treating the disease. But what about the person living with it? Palliative care is designed to relieve the symptoms and stress that come with a serious diagnosis.
Its main goal is to improve the quality of life for both the patient and their family. This type of care addresses physical pain as well as emotional, social, and spiritual challenges.

Unlike hospice, palliative care can begin at any age and stage of an illness. It works alongside curative treatments. For example, a person getting chemotherapy can also receive palliative care to manage side effects like nausea and fatigue.
Who Delivers Palliative Care at Home
Central Coast VNA & Hospice brings palliative care services directly to you in the comfort of your home. Our nonprofit, mission-driven team provides compassionate care in Monterey County, San Benito County, Santa Cruz County, and South Santa Clara County.
Our interdisciplinary team includes:
- Registered Nurses who are experts in managing complex symptoms.
- Medical Social Workers to provide emotional support and connect you to community resources.
- Chaplains who offer spiritual guidance for patients and families of all backgrounds.
- Therapists to help with daily activities, mobility, and communication.
This team works with your existing doctors to add a layer of support. We focus on managing difficult symptoms like pain, shortness of breath, and anxiety.
The Right Time to Ask for Support
A common misstep is waiting until symptoms are unbearable to ask for help. Many people put off seeking palliative care because they think it’s only for the end of life. However, research shows that starting palliative care earlier leads to better symptom control and a higher quality of life.
You should ask about palliative care as soon as a serious illness starts affecting daily life. It’s not about stopping treatment; it’s about adding a layer of support.
The need for this care is huge. According to the National Hospice and Palliative Care Organization (NHPCO), over 1.72 million Medicare beneficiaries received hospice services in 2020 (NHPCO, 2021). Yet many more could benefit from palliative support much earlier in their illness.
Palliative Care in Your Community
For over 74 years, Central Coast VNA & Hospice has served our local communities. As a nonprofit, we ensure residents in Monterey, Salinas, Hollister, and Santa Cruz have access to expert care at home.
If you are struggling with the symptoms of a serious illness, don’t wait to get support. You can call (831) 375-9882 to ask questions or schedule an in-home evaluation. You do not need a referral from a doctor to start the conversation.
Understanding Hospice Care For Comfort and Dignity
Hospice care is for someone with a terminal illness. It is chosen when treatments to cure the illness are no longer working or wanted. A doctor must certify that the person's life expectancy is likely six months or less.
The focus of hospice shifts from curing the disease to ensuring comfort, dignity, and peace. It is not about giving up. Choosing hospice means choosing to live the rest of your life as fully and comfortably as possible.

A Team Approach to Whole-Person Care
At Central Coast VNA & Hospice, our care is delivered by an interdisciplinary team. This team looks at the needs of both the patient and their family. They create a personalized care plan that honors the patient’s wishes.
Each team member brings a unique skill:
- Physicians and Registered Nurses are experts in managing pain and other symptoms.
- Hospice Aides offer hands-on help with personal care like bathing and dressing.
- Medical Social Workers provide emotional support and help families with practical issues.
- Chaplains offer non-denominational spiritual guidance to help find peace.
- Trained Volunteers provide companionship for the patient and a break for family members.
This team approach ensures that a person’s physical, emotional, and spiritual needs are met. We bring this care to wherever a patient calls home in Monterey County or our other service areas. You can learn more in our guide on what is hospice care.
Support That Extends to the Entire Family
A serious illness affects the whole family. That’s why our support goes beyond the patient's medical needs. We provide guidance, education, and emotional support to family members.
Hospice provides support for the entire family. This includes bereavement counseling and grief support for up to 13 months after a loved one has passed.
This ongoing support helps families work through their loss and begin to heal. For some, finding comfort can involve documenting significant events in life. This can be a way to celebrate a life well-lived.
Choosing Comfort and Dignity on the Central Coast
For over 74 years, Central Coast VNA & Hospice has been the trusted nonprofit provider of end-of-life care in our community. Our local roots in Monterey, Salinas, Hollister, and Santa Cruz mean we understand our neighbors' needs.
We believe everyone deserves to experience their final days with grace and peace. Choosing hospice is a decision to prioritize comfort with a team that will honor your wishes.
How to Qualify For Palliative or Hospice Services
Understanding how to qualify for care is a big source of confusion for families. The paths to palliative care and hospice are very different. Knowing the criteria can help you have better talks with doctors.
For palliative care, the main requirement is a diagnosis of a serious, life-limiting illness. This could be cancer, heart failure, COPD, or dementia. The key is that the illness is affecting your quality of life.
Palliative care is not tied to a timeline. You can receive this support from the moment of diagnosis and continue it for as long as it helps. It is designed to work alongside treatments like chemotherapy or physical therapy.
Palliative Care Eligibility at a Glance
A person is a good candidate for palliative care if their illness is causing major challenges, such as:
- Uncontrolled Symptoms: Lasting pain, shortness of breath, fatigue, or nausea that are hard to manage.
- Frequent Hospital Visits: Too many trips to the ER or hospital for the same condition.
- A Decline in Daily Functioning: The illness makes it harder to do everyday activities.
- Emotional or Spiritual Distress: The diagnosis is taking a heavy toll on the patient or family.
At Central Coast VNA & Hospice, our palliative team comes to your home in Monterey, Salinas, or Hollister to help. We add a layer of support, not take anything away.
Understanding Hospice Care Requirements
Qualifying for hospice is more specific because it signals a shift in care goals. The focus moves from finding a cure to maximizing comfort. The requirements are clearly defined by Medicare.
The main criteria for hospice are:
- A Terminal Diagnosis: Two physicians must certify that the illness is terminal.
- A Prognosis of Six Months or Less: A doctor estimates that life expectancy is six months or less if the illness runs its natural course.
- The Choice for Comfort Care: The patient decides to stop treatments aimed at curing the illness and focus on quality of life.
This is a personal decision and is never about "giving up." It’s about choosing to live your remaining time with dignity and peace. You can read more in our guide on hospice eligibility requirements.
How Insurance and Medicare Cover These Services
How these services are paid for is another key difference. Understanding this can relieve a lot of stress for families.
Palliative care is usually paid for by:
- Medicare Part B
- Medi-Cal
- Most private insurance plans
You may have co-pays or deductibles, just like with other specialist doctors.
Hospice care is covered by the Medicare Hospice Benefit. This is an all-inclusive benefit that covers nearly everything related to the terminal diagnosis, often with no out-of-pocket costs.
This coverage includes the hospice team, medications, and medical equipment related to the illness. This allows families to focus on their time together.
When You Should Consider Palliative Care or Hospice
Knowing the difference between these types of care is a great start. But when is it time to ask for help? Too often, families wait until a crisis before reaching out.
The biggest mistake is waiting too long. People delay asking about palliative care because they think it means giving up. Or they wait to talk about hospice until symptoms are overwhelming.
Signs It Might Be Time for Palliative Care
Think of palliative care as an extra layer of support. The right time to ask about it is when a serious illness starts to get in the way of daily life. You don't have to stop your treatments; you're just getting more help to live better.
It might be time for palliative care if you are dealing with:
- Stubborn Symptoms: Pain, fatigue, or anxiety that won’t quit, even with regular treatments.
- Too Many Hospital Visits: Ending up in the ER or hospital multiple times for the same issue.
- Trouble with Daily Tasks: Noticing it’s harder to do simple things like walk or get dressed.
- Emotional Wear-and-Tear: Feeling overwhelmed, stressed, or uncertain about the future.
At Central Coast VNA & Hospice, our palliative care team helps you manage symptoms at home in Monterey, Salinas, or Hollister.
Knowing When to Transition to Hospice
The conversation about hospice usually starts when the focus of care changes. This is when treatments for a cure are no longer working or are causing more harm than good. The goal shifts completely to comfort.
This is a deeply personal decision. It's about choosing to live your remaining time with dignity and peace. To qualify, a doctor needs to certify a life expectancy of about six months or less.
This decision tree gives a simple visual guide for understanding which type of care might be the right fit.

As the graphic shows, palliative care is an option for anyone with a serious illness. Hospice is for when the prognosis becomes limited.
The need for this type of care is huge, but access is unequal. Local organizations like Central Coast VNA & Hospice are essential for our communities. We serve Monterey, San Benito, Santa Cruz, and South Santa Clara counties.
If you or someone in your family lives in Monterey, Salinas, Hollister, or Santa Cruz, our team is ready to talk. Call us at (831) 375-9882 to ask questions or set up an evaluation.
How Our Local Team Can Support Your Family
Making decisions about care during a serious illness is tough. You don’t have to do it alone. For over 74 years, Central Coast VNA & Hospice has provided expert, compassionate support right here at home.
We are the only local nonprofit offering a full continuum of care. This means we provide a seamless transition from home health to palliative care, and then to hospice. Our team understands your journey, values, and goals every step of the way.
A Mission-Driven Local Provider
Having a local team you can trust makes all the difference. As a nonprofit, our focus is on patients and their families, not profits. Our team of Registered Nurses, Hospice Aides, Chaplains, and Medical Social Workers are your neighbors.
Our team lives and works in the same communities we serve, from Salinas to Santa Cruz. That local connection is at the heart of what we do.
When you choose Central Coast VNA & Hospice, you are choosing a team that has been a pillar of this community for generations. We are here to provide the compassionate guidance and expert medical care your family deserves.
Start the Conversation Today
Understanding the difference between hospice and palliative care is the first step. The next is reaching out. Call us for a no-obligation consultation to talk through your situation.
You do not need a doctor's referral to have a conversation with our team. We believe every family deserves the best possible care. You can learn more about why Central Coast VNA is the best choice for palliative care on the Central Coast.
Call us today at (831) 375-9882 to find out how we can support your family.
Frequently Asked Questions About Care Options
It's natural to have questions when exploring healthcare options. We have been helping families on the Central Coast for over 74 years. Here are some of the most common questions we answer.
Can I keep my own doctor if I start palliative or hospice care?
Yes, absolutely. Your doctor remains a central part of your care team. The Central Coast VNA & Hospice team works closely with your primary physician to coordinate your care plan.
Does choosing palliative care mean I am giving up hope?
Not at all. This is a common myth. Palliative care is extra support you receive at the same time as treatments to cure your illness. Its goal is to improve your quality of life while you continue to fight your illness.
Where are palliative and hospice services provided?
Central Coast VNA & Hospice provides both types of care wherever you call home. This includes private residences, assisted living facilities, and nursing homes across Monterey County, San Benito County, Santa Cruz County, and South Santa Clara County.
Who pays for palliative and hospice care?
Palliative care is typically covered by Medicare Part B, Medi-Cal, and most private insurance plans, similar to a specialist visit. Hospice care is fully covered by the Medicare Hospice Benefit, as well as by Medi-Cal and many private insurance policies, often with no out-of-pocket costs for services related to the terminal illness.
Can my loved one receive care if they have dementia?
Yes. Both palliative care and hospice are available for patients with dementia. Palliative care can help manage symptoms and improve quality of life at any stage of the disease. Hospice care is an option in the advanced stages when a doctor certifies a life expectancy of six months or less.
What is the first step to get started?
The first step is to call us. You do not need a referral from a doctor to ask questions or request an informational visit. Our team is here to listen and help you understand your options.
The compassionate team at Central Coast VNA & Hospice has proudly served the Central Coast for over 74 years. If you have more questions about palliative or hospice care, please contact us today to learn how we can support your family.
Who Provides In-Home Care for Aging Parents Near Me? A Guide for Central Coast Families
Juggling a career and family while caring for an aging parent is a heavy load. Many adult children ask, “Can I get help at home, or do I have to put Mom in a facility?” This question often leads to burnout and stress.
You might assume it's an "either/or" choice: do it all yourself or move your parent. But there is a compassionate, effective third option. Professional in-home care can bridge the gap between independence and safety.
Most seniors want to stay in their homes. In fact, 75% of adults over 50 say this is their goal. With the right support, aging in place is possible. This guide will help you find that support in Monterey, San Benito, Santa Cruz, and South Santa Clara counties.
1. Central Coast VNA & Hospice
For families on the Central Coast, Central Coast VNA & Hospice (CCVNA) is a trusted, nonprofit choice. With over 74 years of local service, CCVNA offers a full continuum of in-home clinical care. Their mission is to help seniors age safely and comfortably at home.
Unlike many agencies, CCVNA provides integrated medical services. This means your loved one can move between different levels of care without changing providers. This continuity helps avoid the stress of finding new teams as health needs change.
Why It Stands Out: A Full-Spectrum, Team-Based Approach
CCVNA’s model is built on an interdisciplinary team approach covering home health, palliative, and hospice care. This structure ensures care is coordinated and holistic. Their team addresses physical, emotional, and spiritual needs.
Key Features and Services:
- Integrated Continuum of Care: CCVNA offers home health, palliative care, and hospice services. This ensures a smooth transition from post-surgery recovery to long-term symptom management or end-of-life support.
- Interdisciplinary Care Teams: Care is managed by a team of professionals. This includes Registered Nurses, Physical Therapists, Medical Social Workers, Chaplains, and Hospice Aides.
- Specialized Clinical Programs: CCVNA offers tailored support for patients with cardiac, diabetic, and orthopedic conditions. These focused care plans lead to better outcomes.
- Nonprofit Mission: As a nonprofit, CCVNA enriches care with volunteer programs. These include pet therapy and veteran-to-veteran companionship, adding comfort and connection.
- 24/7 Hospice Availability: Families with a loved one in hospice receive around-the-clock clinical support. This provides peace of mind during challenging times.
CCVNA bridges the gap between family care and facility placement. They deliver professional medical support that allows seniors to remain at home. You can learn more about how VNA helps seniors live safely at home in Monterey.
Practical Information for Families
CCVNA makes accessing care simpler by accepting many payment options. These include Medicare, Medi-Cal, Central California Alliance for Health, and most private insurance plans. This reduces financial barriers to high-quality care.
The best first step is to contact their team to discuss your parent’s needs. With local offices in Monterey, Salinas, and Hollister, they offer accessible, community-based support.
Bottom Line: For skilled nursing, therapy, or compassionate support for a serious illness on the Central Coast, CCVNA is a trusted, local, and clinically excellent solution.
- Pros:
- Comprehensive care (home health, palliative, hospice) ensures continuity.
- Deep local roots, serving the community for over 74 years.
- Interdisciplinary teams provide holistic, person-centered support.
- Accepts major payers, including Medicare, Medi-Cal, and private plans.
- Offers unique volunteer programs like pet therapy and veteran support.
- Cons:
- Services are limited to Monterey, San Benito, Santa Cruz, and South Santa Clara counties.
- Pricing depends on insurance and clinical need and is not listed online.
Website: https://ccvna.com
2. Medicare Care Compare
When skilled medical care is needed, the official Medicare Care Compare website is a vital resource. This government tool helps you find and evaluate Medicare-certified home health agencies. It is an authoritative source for anyone asking, "who provides in-home care for aging parents near me?".
Unlike a simple internet search, Care Compare provides standardized, trustworthy data. It allows you to search for providers by ZIP code and compare them on key quality metrics.
Key Features and How to Use Them
The platform’s strength is its transparency. You can see how local agencies in Salinas or Santa Cruz perform on important measures.
- Side-by-Side Comparisons: View agencies' performance on health outcomes. See how often patients improve at walking or how well their pain is managed.
- Patient Experience Surveys: The site includes HHCAHPS survey results. These ratings show how patients scored an agency on communication, professionalism, and care.
- Service Filters: Narrow your search to find providers offering specific clinical services. These include skilled nursing, physical therapy, occupational therapy, and medical social work.
Pro Tip: Pay close attention to the "Quality of patient care" star rating. This rating summarizes an agency’s performance on key measures, giving you a quick snapshot of their quality.
Pros and Cons of Using Medicare Care Compare
While Care Compare is an excellent tool, it's important to understand its scope.
| Pros | Cons |
|---|---|
| Official & Trustworthy: Data comes directly from Medicare, ensuring accuracy and objectivity. | Limited Scope: Only lists Medicare-certified agencies. It excludes private-pay, non-medical home care companies that provide companion or personal care. |
| Focus on Quality: Provides concrete data on clinical outcomes and patient satisfaction, helping you make an evidence-based decision. | Technical Barriers: The website requires JavaScript and its interface may be challenging for some users to navigate effectively. |
| Cost & Coverage Info: Helps you understand what Medicare covers for home health services. You can learn more about Medicare eligibility for home care here. | Not a Complete Picture: Quality scores are important, but they don’t capture an agency’s culture, responsiveness, or full range of supportive services. |
Medicare Care Compare is the best first step for families needing skilled medical care covered by Medicare. It helps you create a shortlist of high-quality, certified providers in your community.
Website: https://www.medicare.gov/care-compare/
3. Eldercare Locator
The Eldercare Locator is an invaluable public service for families navigating senior care. This free resource from the U.S. government connects you with your local Area Agency on Aging (AAA). It is a trusted guide to community-based programs.
Unlike private online directories, the Eldercare Locator is a curated starting point. It directs you to local experts who can provide information on in-home help, meal services, and transportation. This is especially helpful for understanding publicly funded options.
Key Features and How to Use Them
The platform’s greatest strength is its localized, human-assisted guidance. It connects you with real people who know the resources available in Monterey, San Benito, and Santa Cruz counties.
- ZIP Code Search: Enter a ZIP code to find the contact information for the Area Agency on Aging that serves that location. These agencies are local hubs for senior services.
- Live Assistance: You can call their toll-free number (1-800-677-1116) or use the online chat. A specialist will help you identify relevant programs and next steps.
- Comprehensive Referrals: The service provides referrals to a wide range of supports. This includes publicly funded programs and private service providers.
- Funding & Eligibility Info: Specialists can explain local funding sources and eligibility rules for programs like Meals on Wheels or in-home support services.
Pro Tip: When you contact your local Area Agency on Aging, be prepared to discuss your parent's needs, financial situation, and location. This will help them provide the most relevant referrals.
Pros and Cons of Using Eldercare Locator
While Eldercare Locator is a powerful tool, it’s important to know its function and limitations.
| Pros | Cons |
|---|---|
| Free & Government-Run: It provides unbiased, trustworthy information with deep local knowledge. | Referral Hub, Not a Direct Provider: It connects you to other organizations that provide hands-on services. You cannot hire anyone through the website. |
| Focus on Subsidized Support: It is useful for families seeking publicly funded or low-cost care options. | Varies by Location: The quality and range of available resources can differ significantly from one county to another. |
| Personalized Guidance: Live support offers a human touch, which is invaluable when you feel overwhelmed. It helps you find the right aging in place care services near you. | No Quality Ratings: It does not provide star ratings or quality comparisons between the providers it refers you to. |
Eldercare Locator is the best starting point for understanding all the senior support in your community. It provides a roadmap to local agencies that can help a loved one live safely at home.
Website: https://eldercare.acl.gov/
4. Care.com
For families who want direct control over hiring non-medical help, Care.com is a large online marketplace. It connects individuals with providers of companion and personal care. This makes it a popular choice for finding one-on-one assistance.
This platform empowers you to browse profiles, post a job, and interview candidates yourself. It is geared toward finding help with daily living activities rather than skilled medical services.
Key Features and How to Use Them
Care.com puts the hiring process in your hands. It gives you access to a large pool of local candidates from Salinas to Santa Cruz.
- Local Search: Enter your ZIP code to find profiles of individuals in your area. You can filter results by skills, experience, and availability.
- Detailed Profiles: Each profile lists self-reported experience, qualifications, hourly rates, and reviews from previous families.
- Safety Options: The platform offers optional background checks for an added layer of security.
- Job Posting: You can create a detailed job post outlining your parent's needs and desired schedule to attract suitable applicants.
Pro Tip: You must purchase a paid membership to contact providers. Before subscribing, use the free search to confirm there is a good selection of candidates in your area.
Pros and Cons of Using Care.com
This direct-hire model offers flexibility but also comes with significant responsibilities.
| Pros | Cons |
|---|---|
| Broad Selection & Price Transparency: You can compare a wide range of individuals and their hourly rates, often leading to lower costs than agency care. | Requires Paid Membership: A subscription is required to message or hire individuals, and memberships are often nonrefundable. |
| Direct Control Over Hiring: You are in charge of the entire process, from interviewing to selecting the person who will care for your parent. | Family Assumes Employer Role: You are responsible for vetting, interviewing, and managing payroll and taxes. Background checks are an extra cost. |
| Flexible Care Options: It's ideal for finding help with non-medical tasks like companionship, meal prep, and medication reminders. You can learn more about the differences between home care and other senior care services here. | Variable Quality: Since providers are independent, their experience and reliability can vary widely. The vetting process falls entirely on the family. |
Care.com is a valuable tool for families who are comfortable taking on the role of an employer. It is best for those who primarily need non-medical, personal, or companion care.
Website: https://www.care.com/caregivers
5. CareLinx (by Sharecare)
CareLinx is a marketplace that helps families directly hire and manage professional non-medical assistance. Backed by the digital health company Sharecare, it offers a modern solution for personal care needs. The platform lets you find, vet, and communicate with local individuals.
Unlike traditional agencies, CareLinx allows you to browse detailed profiles. You can review experience, certifications, rates, and availability. You can filter by specific needs and hire a professional who feels like the right fit.
Key Features and How to Use Them
The platform is designed to give families control over the hiring and management process. It provides tools to ensure transparency and safety.
- Detailed Profiles: Search by ZIP code to review profiles in areas like Monterey or San Benito County. Each profile includes background, skills, rates, and reviews.
- Sharecare VERIFIED Screening: The platform emphasizes safety with a comprehensive screening process. This includes background checks and verification of credentials.
- In-App Care Coordination: The CareLinx app allows you to create digital care plans, schedule visits, and receive real-time updates.
- Optional Payroll & Tax Services: CareLinx can handle the complexities of being an employer, including payroll processing and tax compliance.
Pro Tip: Use the messaging feature to interview several potential candidates before hiring. Ask specific questions about their experience with conditions relevant to your parent, like dementia or mobility challenges.
Pros and Cons of Using CareLinx
CareLinx provides a powerful way to find help, but it’s a marketplace, not a full-service agency.
| Pros | Cons |
|---|---|
| Flexibility & Choice: You have complete control to choose your professional, set schedules, and define duties, often at a lower cost than traditional agencies. | Limited Scope: This platform is for non-medical personal and companion care. It does not list Medicare-certified agencies that provide skilled nursing or therapy. |
| Safety & Transparency: The Sharecare VERIFIED background checks and in-app visit tracking provide significant peace of mind for families. | Membership Required: You typically need a paid subscription to message and hire individuals, which adds to the overall cost. |
| Employer Support: The optional payroll and tax services simplify the legal and financial responsibilities of hiring someone directly. | Variable Availability: The number and quality of individuals can vary significantly depending on your specific location. |
CareLinx is an excellent resource for families who want a hands-on approach to finding and managing non-medical assistance. It offers the tools to make a safe, informed hiring decision.
Website: https://www.carelinx.com/
6. Home Instead
Home Instead is a large, franchised network that specializes in non-medical support. It provides companionship, personal care, and assistance with daily activities. This makes it a frequent answer for those seeking in-home help for aging parents.
Unlike online directories, Home Instead connects families with local franchise offices. These offices employ, train, and manage their own teams of professional staff. This agency model simplifies the process of finding reliable, non-clinical help.
Key Features and How to Use Them
The platform connects you with a local office that assesses your family's needs. The office then creates a customized plan. This helps families avoid the complexities of hiring an independent provider.
- Local Office Locator: Use your ZIP code to find the nearest franchise, such as those serving Santa Cruz or Hollister. The local office will conduct an in-home consultation to create a care plan and provide a quote.
- Specialized Programs: Many locations offer specialized training for staff in areas like Alzheimer's and dementia care. This ensures your parent receives knowledgeable assistance.
- Full-Service Management: The agency handles everything from recruiting and background checks to payroll and scheduling backup staff. This relieves families of significant administrative burdens.
Pro Tip: When you contact a local Home Instead office, be ready to discuss your parent's daily routines and challenges in detail. This information will help them match you with the right support professional.
Pros and Cons of Using Home Instead
While its model offers convenience, it's important to understand its focus on non-medical care.
| Pros | Cons |
|---|---|
| Less Administrative Burden: The agency manages all aspects of employment, including vetting, scheduling, supervision, and providing backups. | Higher Cost: This full-service model is typically more expensive than hiring an independent provider directly. |
| Specialized Training: Home Instead often provides its teams with consistent, specialized training programs for conditions like dementia. | Variable Local Policies: Because it's a franchise system, prices and service offerings can vary between local offices. |
| Safety and Reliability: The company's hiring processes provide a layer of safety and peace of mind. You can discover more reasons to choose in-home care here. | Non-Medical Focus: Home Instead does not provide skilled nursing or clinical services like wound care or physical therapy. |
Home Instead is an excellent choice for families needing reliable, non-medical companionship and personal care. It provides a structured, safe, and professionally managed alternative to hiring independently.
Website: https://www.homeinstead.com/
7. Visiting Angels
Visiting Angels is a well-known name in non-medical home care. It operates as a nationwide network of franchised agencies. This makes it an accessible option for families looking for companionship, personal care, and dementia support.
The platform connects you with a local office in your area, such as Santa Cruz or Monterey County. Each office is an independent business that follows the brand's service model. They provide vetted professionals for in-home assistance.
Key Features and How to Use Them
Visiting Angels focuses on making the process of finding non-medical support straightforward. Their website is the central hub for locating and engaging with their local care teams.
- Office Locator: The main tool on the site is a search function where you can enter your ZIP code. This directs you to the franchise serving your community so you can request a free in-home consultation.
- Flexible Scheduling Options: Most locations offer a wide range of scheduling to fit a family's needs. This includes hourly assistance, overnight care, and even 24-hour or live-in arrangements.
- Clear Service Descriptions: The website details the types of non-medical services available. These typically include personal care, companion care, and respite care.
Pro Tip: During your consultation, ask about their hiring process, background checks, and how they match staff with clients. Since each franchise is independently owned, these specifics can vary.
Pros and Cons of Using Visiting Angels
As a franchise-based agency, Visiting Angels offers distinct advantages and some potential inconsistencies.
| Pros | Cons |
|---|---|
| Large U.S. Footprint: With locations across the country, it's highly likely you can find a local office with a quick-start option. | Franchise Variation: Pricing, services, and staff availability can differ from one franchise location to another. |
| Agency-Managed Care: The agency model means staff are vetted, insured, and supervised. They also handle replacements if a professional is unavailable. | Lacks Pricing Transparency: Many offices require you to call for a rate quote, as pricing is rarely published online. |
| Specialized Programs: Many offices offer specialized programs for conditions like Alzheimer's, dementia, and fall prevention. | Non-Medical Focus: Visiting Angels does not provide skilled medical care, like nursing services or physical therapy. |
Visiting Angels is a strong choice for families seeking reliable, non-medical companion and personal care from an established agency. It provides a structured, supervised alternative to hiring independent professionals.
Website: https://www.visitingangels.com/
7 In-Home Care Providers Comparison
| Service | Implementation complexity (🔄) | Resource requirements & speed (⚡) | Expected outcomes (⭐ 📊) | Ideal use cases (💡) | Key advantages (⭐) |
|---|---|---|---|---|---|
| Central Coast VNA & Hospice | 🔄 Moderate–high: interdisciplinary coordination and clinical referrals required | ⚡ Insurance-dependent (Medicare/Medi‑Cal/private); 24/7 hospice access; local office visits | ⭐⭐⭐⭐ · 📊 High-quality clinical care, symptom control, continuity across stages | Care requiring skilled nursing, palliative or hospice care at home in Central Coast | Local nonprofit, integrated team model, specialty programs, 24/7 hospice |
| Medicare Care Compare | 🔄 Low for users: searchable directory and comparisons | ⚡ Free, nationwide; web-based (requires JavaScript); quick lookup by ZIP | ⭐⭐⭐ · 📊 Standardized quality & patient-experience metrics for Medicare providers | Comparing Medicare-certified home health or hospice providers and checking coverage | Government-sourced data, nationwide quality ratings and HHCAHPS surveys |
| Eldercare Locator | 🔄 Low: referral hub with live assistance | ⚡ Free national service; phone/chat support; response varies by locality | ⭐⭐ · 📊 Connects to local Area Agencies on Aging and subsidized services | Finding publicly funded supports, respite, meals, transportation, eligibility help | Free government service, live local referrals and funding guidance |
| Care.com | 🔄 Moderate: families post jobs, interview, and hire independently | ⚡ Marketplace with visible rates; membership often required to contact; background checks extra | ⭐⭐ · 📊 Flexible, cost-transparent non-medical care; quality varies by caregiver | Hiring companion care, personal care, transportation, short-term help | Large selection, hourly rates visible, often lower cost than agencies |
| CareLinx (by Sharecare) | 🔄 Moderate: platform-mediated hiring with app tools | ⚡ ZIP-based search; messaging/membership often required; optional payroll/tax service | ⭐⭐⭐ · 📊 Professional caregiver options with app-based scheduling and tracking | Families wanting CNAs/HHAs with visit tracking and employer-of-record payroll | Sharecare-verified screening, in-app care plans, optional payroll compliance |
| Home Instead | 🔄 Low for families: agency-managed recruitment and supervision | ⚡ Franchise-based pricing (can be higher); agency handles staffing/backups | ⭐⭐⭐ · 📊 Consistent non-medical care and specialized dementia programs | Long-term personal care, dementia support, families preferring agency oversight | Agency handles hiring, training, insurance, and replacement staff |
| Visiting Angels | 🔄 Low: agency model with local franchise coordination | ⚡ Franchise-dependent rates and availability; flexible scheduling options | ⭐⭐⭐ · 📊 Reliable companionship and personal care; flexible shifts incl. live‑in | Hourly, overnight, or live‑in non-medical care with flexible scheduling | Large footprint, local teams, free consultations, flexible scheduling options |
Making the Right Choice for Your Family's Peace of Mind
Finding the right support for your aging parent is a major decision. The question, "who provides in-home care for aging parents near me?" can be overwhelming. But this guide shows you have many powerful tools and dedicated providers available on the Central Coast.
The journey begins with understanding your options. We have explored a variety of resources, from federal databases like Medicare Care Compare to private agencies like Home Instead. Each serves a unique purpose.
Key Steps to Move Forward
As you move from research to action, remember that a middle path exists. You do not have to do everything yourself or choose a facility. In-home clinical care is often the most compassionate and effective choice.
Here are the actionable next steps to take:
- Assess Your Parent’s Needs: Clearly define what kind of support is required. Is it skilled nursing and therapy, or is it help with daily activities and companionship? This will narrow your search.
- Evaluate Provider Types: Differentiate between agencies providing skilled medical care (like Central Coast VNA & Hospice) and those offering non-medical care. Your parent's health status will determine which is appropriate.
- Prepare Your Questions: Create a list of questions for potential providers. Ask about staff qualifications, scope of services, insurance coverage, and how they create personalized care plans.
- Involve Your Parent: Whenever possible, include your aging parent in the decision-making process. Their comfort and preferences are essential for a successful care arrangement.
Financial and Long-Term Considerations
Choosing a provider is also a financial decision. It's crucial to understand what Medicare, private insurance, or other benefits will cover. Resources like a guide to aged care financial planning can help you make sustainable choices.
Ultimately, your goal is to find a trusted partner who provides peace of mind. For families in Monterey County, Salinas, Hollister, or Santa Cruz, a local, mission-driven organization with deep community roots is often the best choice.
Making this choice is an act of love. By arming yourself with knowledge, you can ensure your parent receives the exceptional care they deserve in the comfort of their own home.
Frequently Asked Questions (FAQs)
1. What is the difference between home health care and other in-home care?
Home health care is skilled clinical care prescribed by a doctor. It includes services like nursing, physical therapy, and wound care. Other in-home care is non-medical and helps with daily tasks like meal prep, bathing, and companionship.
2. How do I know if my parent is eligible for home health care through Medicare?
Medicare covers home health if a doctor certifies that your parent is homebound and needs skilled nursing or therapy services. Central Coast VNA & Hospice can help you verify eligibility and navigate the requirements.
3. What services does Central Coast VNA & Hospice offer?
As a nonprofit, CCVNA offers a full continuum of care. This includes home health for recovery, palliative care for symptom management of serious illness, and hospice care for end-of-life support, all delivered at home.
4. How can I find a provider in Monterey County or Santa Cruz County?
For skilled medical care, you can contact Central Coast VNA & Hospice directly or use the Medicare Care Compare tool. For non-medical care, you can explore platforms like Care.com or agencies like Home Instead and Visiting Angels.
5. What should I look for in a quality in-home care provider?
Look for a provider with a long-standing local reputation and a team-based approach. Ensure their staff are licensed and credentialed. Ask about their communication process and how they develop personalized care plans.
Ready to take the next step with a trusted local provider? Contact Central Coast VNA & Hospice to learn how our 74+ years of nonprofit service can support your family. Explore our services today and find the compassionate care your loved one deserves.
Finding Senior Care in Monterey County: Your Guide to Local Services
When you're juggling a career, family, and the needs of an aging parent, one question comes up often. “Can I get help at home, or do I have to put Mom in a facility?” Many families in Monterey County feel caught between these two choices.
This can lead to burnout and stress. But it's an either/or way of thinking that isn't accurate. Most seniors want to stay in their own homes. In fact, 75% of adults over 50 say this is their goal.
With the right support, aging in place is possible. This guide will show you what senior care services are available in Monterey County. It will help you find the best local options for your family.
Instead of feeling overwhelmed, you can build a support system. This system can honor your loved one's wish for independence. It will also make sure they are safe and healthy.
1. Central Coast VNA & Hospice: A Continuum of In-Home Clinical Care
For families exploring what senior care services are available in Monterey County, Central Coast VNA & Hospice (CCVNA) is a trusted nonprofit provider. With over 74 years of service, CCVNA offers a full range of clinical care in the comfort of a patient’s home. This approach supports seniors through different health stages.
Many families think they must choose between doing it all themselves or using a facility. CCVNA bridges this gap. Their teams of nurses, therapists, and other professionals bring medical support right to the home.
This model helps seniors age in place with dignity. It is especially helpful for those managing chronic conditions or recovering from surgery. CCVNA serves Monterey County, San Benito County, Santa Cruz County, and South Santa Clara County.
Key Strengths and Differentiators
What makes Central Coast VNA & Hospice a standout choice? It provides three levels of in-home clinical care from one coordinated organization. This ensures smooth transitions for patients as their needs change.
- Integrated Continuum of Care: CCVNA offers skilled home health, palliative care, and hospice care. A patient can move from home health to palliative care to hospice with the same trusted team.
- Expert Interdisciplinary Teams: Care is delivered by a team of professionals. This includes Registered Nurses, therapists, Medical Social Workers, and Chaplains. For hospice patients, this team offers 24/7 clinical support.
- Nonprofit, Mission-Driven Focus: As a local nonprofit, CCVNA’s mission is patient well-being, not profit. This focus allows them to reinvest in compassionate care for our Central Coast communities.
Understanding the Services
CCVNA’s website, ccvna.com, clearly explains its core services. It also provides helpful resources for families.
- Skilled Home Health: This service is for patients recovering from illness, injury, or surgery. It includes skilled nursing care and physical therapy ordered by a doctor.
- Palliative Care: This care aims to improve quality of life for those with serious illnesses. It focuses on managing symptoms and pain.
- Hospice Care: For patients with a life-limiting illness, hospice provides comfort care. It focuses on dignity, peace, and support for the patient and family. To learn more, read about how hospice and palliative care support families.
Access and Eligibility
Accessing services usually starts with a doctor's referral for home health care. CCVNA works with local hospitals and doctors throughout its service areas.
The organization accepts many insurance plans. These include Medicare, Medi-Cal, Central California Alliance for Health, Blue Shield, and many private insurance plans. Families can contact CCVNA to ask about coverage.
- Home Health Referrals: (831) 372-6668
- Hospice Referrals: (831) 751-5500
2. Monterey County Aging & Adult Services (AAS)
When you first explore senior care in Monterey County, the options can seem overwhelming. The Monterey County Aging & Adult Services (AAS) website is the official starting point. It acts as a central hub for information and referrals.

The main job of AAS is to connect you with the right services. They guide you to the right agency or program. This could be for in-home support, nutrition, or Adult Protective Services.
Key Features and How to Use Them
The most valuable tool AAS offers is its live helpline. You can speak with a staff member who can assess your situation. They can then provide referrals to trusted local agencies.
- Information, Referral & Assistance (IRA) Helpline: This is your direct line to a knowledgeable guide.
- Salinas: (831) 755-4466
- King City: (831) 385-7400
- Monterey County Aging & Disability Resource Guide: This downloadable guide is a full directory of services.
- Adult Protective Services (APS): AAS provides a direct link to APS for reporting elder abuse or neglect.
Pro Tip: Before calling the helpline, write down a list of your loved one’s needs and your questions. This will help the representative give you the most accurate referrals quickly.
Why It Stands Out
AAS is the official, county-run resource. The information is up-to-date and the referrals are to trusted local partners. While it is not a direct service provider, its role as a central navigator is key for families.
Website: https://www.countyofmonterey.gov/government/departments-i-z/social-services/adult-services
3. Monterey County Public Authority for In-Home Supportive Services (IHSS) – Registry
For families seeking hands-on in-home care, the IHSS Registry is a key resource. It is a county-run service that connects eligible seniors with individual providers. This allows seniors to hire and manage their own care provider.

The Public Authority acts as a bridge. It supports both the senior and the provider by maintaining a list of available aides. This model is ideal for those who qualify for Medi-Cal’s IHSS program.
Key Features and How to Use Them
The Registry website guides both clients and potential providers through the process. Seniors and their families get a list of vetted providers to choose from. This personalized approach is a core part of local government programs.
- Provider Matching: The Registry matches clients with providers based on specific needs. This includes personal care tasks, schedule, and location.
- Provider Screening: Aides on the Registry have passed a background check and orientation. This provides a layer of security for families.
- Client and Provider Support: The Public Authority offers guidance on how to join the registry and conduct interviews. You can call them at (831) 755-4466 for help.
Pro Tip: When you get a list of providers, prepare interview questions. Focus on experience, reliability, and communication style. Finding a good personality fit is very important.
Why It Stands Out
The IHSS Registry is unique because it connects directly with a state benefit program (IHSS). It puts the power of choice in the hands of the consumer. The trade-off is that you must first be approved for IHSS benefits.
For those needing skilled medical care, you may need other options. You can explore in-home support to avoid a nursing home that can work alongside IHSS services.
Website: https://www.countyofmonterey.gov/government/departments-i-z/social-services/adult-services/public-authority-ihss
4. 211 Monterey County (United Way Monterey County)
When you need quick information on local support, 211 Monterey County is a powerful tool. This free and confidential service is run by United Way Monterey County. It acts as a 24/7 hotline and online database.
Unlike resources focused only on aging, 211 covers a wide range of needs. This includes food, housing assistance, and transportation. A single call can lead to referrals for multiple challenges.
Key Features and How to Use Them
The strength of 211 is its accessibility. Trained specialists are available around the clock. They provide live, local referrals in multiple languages.
- 24/7 Live Navigation: Simply dial 2-1-1 from any phone. You can speak with a specialist who will connect you to local resources.
- Text and Chat Options: For quick help, text your zip code to 898-211 or use the live chat on their website.
- Searchable Online Database: The website has a large directory of community resources. You can search by keyword and location.
Pro Tip: Use the online database to look for categories like "Senior Services" first. This can help you find specific programs to ask about when you call 2-1-1.
Why It Stands Out
211 Monterey County is special because of its 24/7 availability and multilingual support. It is a no-cost, one-stop shop for finding solutions to challenges that often come with aging. While 211 is a referral service, it is great at connecting you with organizations that provide direct care.
Website: https://211montereycounty.org
5. Alliance on Aging (Monterey County)
Navigating Medicare and finding support can be hard. The Alliance on Aging is a local nonprofit that has served Monterey County since 1970. It acts as a guide for older adults and their families.
The main role of the Alliance on Aging is to empower seniors. They help people understand their benefits and access services. Their community-focused approach is a great resource for the non-medical side of aging.
Key Features and How to Use Them
The Alliance on Aging offers several free programs. Its services are available through offices in Salinas and Monterey. They also do outreach across the county.
- Medicare Counseling (HICAP): Trained counselors provide free, unbiased help. They can help you understand Medicare benefits and compare plans.
- The HUB Community Center: Located in Salinas, The HUB is a central point for resources. It hosts a Memory Café for people with cognitive decline and their care partners.
- Benefits Counseling & Peer Support: The Alliance helps seniors apply for benefits. It also offers a peer counseling program for companionship.
Pro Tip: Before Medicare's Annual Election Period (October 15 - December 7), schedule a free HICAP appointment. Counselors can help you compare plans to make sure your coverage still meets your needs.
Why It Stands Out
The Alliance on Aging is a trusted, nonprofit advocate. Its HICAP counselors provide completely unbiased advice. This organization bridges the gap between needing help and knowing where to find it.
While the Alliance is great for counseling, it is not a medical provider. For hands-on medical help at home, you will need to explore skilled in-home care. Understanding all of the senior and elderly care services available will help you create a full support plan.
Website: https://allianceonaging.org
6. Medicare Care Compare (Medicare.gov)
When your loved one is eligible for Medicare, finding certified providers is a top priority. The official Medicare Care Compare website is the government's tool to help you. You can search for and evaluate Medicare-certified home health agencies and hospice providers.
The main purpose of this platform is to provide quality ratings and patient survey results. This lets you compare local agencies side-by-side. It takes the guesswork out of choosing a provider.
Key Features and How to Use Them
The most powerful feature of Medicare Care Compare is its search tool. You can enter your zip code to find providers in Monterey County. Then you can compare them based on official star ratings.
- Side-by-Side Comparisons: Select multiple local agencies. You can view their quality ratings and patient experience scores in an easy-to-read table.
- Detailed Quality Metrics: Explore specific data, like how well an agency managed patients' pain.
- Direct Medicare Information: The site provides clear links to what Medicare covers for services. You can learn more about Medicare home care eligibility to understand the requirements.
Pro Tip: Use the "star ratings" as a starting point, but don't stop there. Click into the "Details" for each provider to read patient survey results.
Why It Stands Out
Medicare Care Compare is essential because it is credible. As the official U.S. government site, it is the most unbiased source for data on Medicare-certified providers. However, the site does not list non-Medicare or private-pay-only agencies.
Website: https://www.medicare.gov/care-compare
7. California Department of Social Services (CDSS) – Facility Search
When you’re researching what senior care services are available in Monterey County, this tool is helpful. The CDSS Facility Search offers a statewide directory of licensed care facilities. It also lists Home Care Organizations.
Key Features and How to Use Them
-
Search by County or City
Enter “Monterey” to list all licensed facilities and home care agencies in your area. -
Licensing Status
View whether a facility’s license is active. This helps you know it meets state rules. -
Inspection & Complaint Reports
Access records of health and safety inspections. You can also see any complaints filed in the last five years. -
Consumer Guidance
Read tips on what to look for during tours. The site also defines different care levels. -
Email Alerts
Sign up to get automatic notices if a facility’s status changes. -
Downloadable Records
Save PDF copies of reports to review or share with family.
Pro Tip: Use the site’s filtering options to narrow results by services offered, such as memory care. Note the facility number so you can call directly for pricing and availability.
Comparison at a Glance
| Feature | CDSS Facility Search | Commercial Websites |
|---|---|---|
| Licensing Information | Up-to-date licensing status and history | Varies by provider, may lack compliance details |
| Inspection Reports | Full five-year complaint and violation history | Not always available or complete |
| Pricing & Availability | Not provided, requires direct contact | Often displays starting costs and room availability |
| User Interface | Government functional design | More intuitive filters, photos, and user reviews |
Why It Stands Out
CDSS Facility Search is the only tool backed by the state’s licensing authority. It delivers unbiased, official data you cannot find on commercial sites. This makes it ideal for checking on a facility before you visit.
However, it does not list private pricing or real-time availability. You must call each facility directly to learn costs and open spaces.
Website: https://www.cdss.ca.gov/inforesources/community-care-licensing/facility-search-welcome
Monterey County Senior Care Services — 7-Provider Comparison
| Service | Implementation Complexity 🔄 | Resource Requirements ⚡ | Expected Outcomes ⭐📊 | Ideal Use Cases 💡 | Key Advantages ⭐ |
|---|---|---|---|---|---|
| VNA and Hospice (Central Coast VNA & Hospice) | Moderate–High: interdisciplinary coordination, 24/7 clinical support | High: skilled clinicians, therapy, volunteers, equipment | High: symptom management, seamless transitions, psychosocial & spiritual support | In‑home skilled care, palliative/hospice needs, complex care coordination | Comprehensive in‑home continuum; strong local nonprofit trust; insurance‑friendly |
| Monterey County Aging & Adult Services (AAS) | Low–Moderate: referral and navigation processes | Low: helpline staff, curated county resources | Moderate: faster access to appropriate county programs and eligibility info | Older adults/disabled individuals needing referrals, APS, eligibility guidance | Official county source with up‑to‑date eligibility and live phone assistance |
| Public Authority – IHSS Registry | Moderate: eligibility verification and matching workflow | Medium: screened caregiver pool and admin support | High for eligible clients: matched caregivers to remain at home | IHSS‑eligible people who want to hire/manage paid caregivers | County‑run matching integrated with IHSS; supports client‑directed hiring |
| 211 Monterey County (United Way) | Low: simple contact methods (phone/text/chat) with specialists | Moderate: 24/7 call center, large searchable database | High: rapid multilingual referrals across many service types | Immediate non‑emergency needs (food, transport, community supports) | 24/7 multilingual navigation and broad, no‑cost community directory |
| Alliance on Aging (Monterey County) | Low: counseling, classes, peer support programs | Low–Moderate: HICAP counselors, outreach staff, community HUB | Moderate: improved Medicare decisions, caregiver support, peer connection | Medicare enrollment help, caregiver education, memory/social programs | Free unbiased Medicare counseling (HICAP); long‑standing local presence |
| Medicare Care Compare (Medicare.gov) | Low–Moderate: searchable data + technical quality metrics | Low: public online tool; internet access and data literacy needed | High for Medicare providers: transparent CMS quality and patient experience metrics | Comparing Medicare‑certified home health, hospice, skilled nursing providers | Authoritative CMS ratings and standardized quality metrics |
| CDSS Facility Search (California) | Low–Moderate: search and interpret licensing/inspection records | Low: state database access; internet required | High for regulatory checks: licensing status, inspections, complaints | Screening RCFEs/assisted living or home care organizations before visits | Official regulator‑maintained licensing, inspection and complaint histories |
Your Next Step: Partner with a Trusted Local Expert
Finding senior care in Monterey County can feel like a big task. But now you have explored many helpful tools and services. You've learned about government agencies, nonprofit resources, and online databases.
The journey often starts with one key question. “What senior care services are available in Monterey County that can help my loved one stay safely at home?” This article shows that you have more options than you think. A much better path exists than the all-or-nothing choice.
Key Takeaways for Your Family
As you move forward, keep these key points in mind:
- Aging in Place is a Realistic Goal: Most older adults want to age in their homes. With the right support, this is an achievable goal for many local families.
- A Spectrum of Care Exists: Senior care is not one-size-fits-all. It ranges from help with daily tasks (IHSS) to skilled clinical care at home (Central Coast VNA & Hospice).
- Proactive Planning Reduces Stress: Do not wait for a crisis to explore your options. Learning about these resources now will help you make calm, informed decisions later.
- Professional Guidance is Invaluable: You do not have to create a care plan alone. A local expert can provide a clear roadmap and ensure your loved one gets coordinated care.
Making Your First Actionable Step
So, where do you begin? A direct conversation with a clinical care provider is often the most effective first step. This is true if your loved one is managing chronic illnesses or recovering from surgery.
Start by looking at your loved one’s specific needs.
- Is medical care required at home? If yes, focus on Medicare-certified home health agencies. These groups provide skilled nursing and therapy that non-medical services cannot.
- Is comfort and symptom management the priority? Palliative care provides an extra layer of support for those with serious, long-term illnesses.
- Is the focus on dignity at the end of life? Hospice care provides compassionate support for individuals with a life-limiting illness.
By focusing on the type of care needed, you can narrow your search. This saves time and helps you connect with a team that can meet your family’s needs.
For families in Monterey, San Benito, Santa Cruz, and South Santa Clara counties, Central Coast VNA & Hospice is a trusted, nonprofit partner. We have served our community for over 74 years. We offer a full continuum of care, guiding patients from home health to palliative and hospice care.
Our interdisciplinary teams are compassionate experts. They are dedicated to honoring your loved one’s wishes and bringing peace of mind to your family. Choosing a local, mission-driven organization ensures the focus is always on patient well-being.
Frequently Asked Questions (FAQs)
1. What is the difference between home health, palliative care, and hospice?
Home health care provides skilled nursing and therapy to help patients recover from an illness, injury, or surgery. Palliative care focuses on symptom management for serious illnesses and can be given with other treatments. Hospice care provides comfort and support for patients with a life-limiting illness when curative treatment is no longer the goal.
2. How do I know if my parent qualifies for in-home skilled care?
A doctor must determine that your parent needs skilled medical care at home. This often happens after a hospital stay or if a health condition worsens. Agencies like Central Coast VNA & Hospice can help coordinate with your parent's doctor to assess eligibility.
3. Are these services covered by Medicare?
Yes, Medicare Part A and Part B cover eligible home health care, palliative care, and hospice care. Most services have specific eligibility requirements, so it's important to check with the provider.
4. Can I get help if my parent doesn't need medical care but struggles with daily tasks?
Yes. In-Home Supportive Services (IHSS) is a program for Medi-Cal eligible seniors who need help with tasks like bathing, dressing, and meal preparation. You can contact Monterey County Aging & Adult Services to learn more.
5. What should I look for in a home health or hospice agency?
Look for a local, nonprofit provider with a long history in the community, like Central Coast VNA & Hospice. Use Medicare Care Compare to check quality ratings. Also, ask if they provide a full continuum of care to ensure smooth transitions if needs change.
Don't navigate this journey alone. When you need a trusted partner to help you understand what senior care services are available in Monterey County, turn to the local experts at Central Coast VNA & Hospice. Visit us online to see how our nonprofit home health, palliative, and hospice programs can bring compassionate, professional care directly to your home.
When Should Someone with Dementia Go on Hospice? A Compassionate Guide
Families caring for a loved one with dementia often face a difficult question: when should we ask about hospice? Unlike illnesses with a clearer timeline, dementia’s decline is gradual. This can leave families wondering, “Are we there yet?”
Recognizing certain changes can help. If your loved one is speaking very little, needs help with all daily tasks, has lost significant weight, or sleeps most of the day, it may be time to talk about hospice.
Choosing hospice isn't about giving up. It is about adding a layer of comfort-focused care to provide the best quality of life possible.
Navigating the Gentle Path to Hospice for Dementia

Unlike cancer or heart disease, dementia progresses slowly and unpredictably. This gradual decline can leave families feeling uncertain about when to seek additional support.
Too often, families wait for a crisis to explore hospice. A fall, a serious infection, or a hospitalization can force a quick decision.
Waiting for an emergency means missing out on weeks or even months of valuable support. Hospice care is not just for the final few days of life; it can provide comfort for much longer. According to the National Hospice and Palliative Care Organization, over 51.7% of Medicare beneficiaries who died received hospice, but many enrolled too late to get the full benefit (NHPCO, 2021).
Reframing the Hospice Decision
Thinking about hospice brings up strong emotions. For many, it involves the profound challenge of letting go. It is helpful to reframe this choice as a transition to a different kind of care focused on dignity and peace.
Choosing hospice is an active decision to give your loved one comfort and expert symptom management. It supports the entire family during a difficult time.
This guide will explain the signs that it may be time for hospice and how eligibility works. At Central Coast VNA & Hospice, we have supported families in Monterey County, San Benito County, and Santa Cruz County for over 74 years.
Our local, nonprofit teams are here to guide you with compassion. Knowing when is the right time for hospice is the first step.
Recognizing the Key Signs for Hospice Consideration
Deciding when someone with dementia needs hospice can be confusing. The decline is often a series of small changes, not one single event. Knowing the specific signs of advanced dementia can help you feel more prepared.
It is rarely one single symptom. Instead, it is a collection of changes that show the body is slowing down. Recognizing these shifts can help you start a conversation about comfort-focused care.
Changes in Communication and Awareness
A significant decline in verbal communication is a key sign of advanced dementia. Your loved one may go from telling stories to struggling for words, or speaking very little at all.
This reflects deep changes happening in the brain. You might notice that they:
- Speak six or fewer intelligible words in a typical day.
- Rely on repetitive phrases or sounds instead of clear sentences.
- No longer recognize close family members or confuse them with others.
- Seem more withdrawn and less responsive to their surroundings.
This communication barrier shows the disease is affecting core brain functions. Comfort and non-verbal connection become more important than ever. Learn more in our guide on how to know when hospice is needed.
Increasing Physical Dependence
As dementia progresses, the ability to manage simple, everyday activities fades. This growing need for help is a key sign that your loved one may be ready for hospice support.
They may need total help with all activities of daily living (ADLs). This means they depend on others for basic self-care, including:
- Bathing and grooming
- Dressing and undressing
- Getting in and out of a bed or chair
- Using the toilet
When someone requires this level of hands-on care, it often signals the final stages of the disease. A skilled team, including Hospice Aides, can provide immense relief for both your loved one and the family.
Decline in Physical Health
You will likely see other significant physical changes. These signs point to a systemic decline and are crucial in determining hospice eligibility.
The checklist below can help you track these changes. Seeing several of these signs may mean it is time to speak with a doctor about a hospice consultation.
Observable Signs Your Loved One May Be Ready for Hospice
| Symptom Category | What to Look For |
|---|---|
| Weight Loss | Unintentional loss of 10% or more body weight in the last six months. |
| Swallowing Issues | Frequent coughing, choking, or holding food in the mouth while eating. |
| Increased Sleep | Spending most of the day asleep or in bed; showing little interest in activities. |
| Recurrent Infections | Repeated urinary tract infections, pneumonia, sepsis, or other infections. |
| Mobility Decline | Inability to walk without assistance; eventually confined to a bed or chair. |
| Skin Issues | Developing pressure ulcers (bedsores) despite good care. |
Seeing just one of these signs might not be a trigger. When you notice a pattern of several occurring together, it paints a clearer picture.
These physical markers show that the body is struggling to maintain its basic functions. Shifting the goals of care toward symptom management and comfort becomes the most loving path forward.
If you are seeing these signs, it may be the right time to explore what hospice can offer. The team at Central Coast VNA & Hospice can provide an expert assessment to guide your family.
Understanding How Hospice Eligibility for Dementia Works
The official requirements for hospice care can seem complex, but they are often straightforward. Doctors and hospice teams use specific tools to determine when a person with dementia is medically ready for this care.
A key benchmark for Medicare is the Functional Assessment Staging Tool (FAST). This scale measures how dementia has progressed by looking at a person’s ability to handle daily activities. Stage 7 is the most advanced phase of the disease.
What Does Stage 7 on the FAST Scale Look Like?
When someone reaches Stage 7, they need a tremendous amount of help with daily life. This goes far beyond memory loss. It is a sign that dementia has deeply affected the brain's ability to control the body.
A person in this stage will typically show a combination of these signs:
- Very Limited Speech: They might speak fewer than six words on an average day.
- Loss of Mobility: They can no longer walk without assistance.
- Need for Total Assistance: They are completely dependent on others for personal care like bathing and dressing.
This level of dependence is a strong signal that the illness has reached its final phase. The focus of care naturally shifts toward ensuring comfort. For more details, see our guide on hospice eligibility requirements.
More Than Just a Number
A FAST score is just one piece of the puzzle. Medicare also looks for other serious health issues that confirm the disease is advancing. These other conditions show how much dementia is impacting their overall health.
This visual decision tree shows how factors like communication, physical abilities, and eating all signal when hospice may be appropriate.
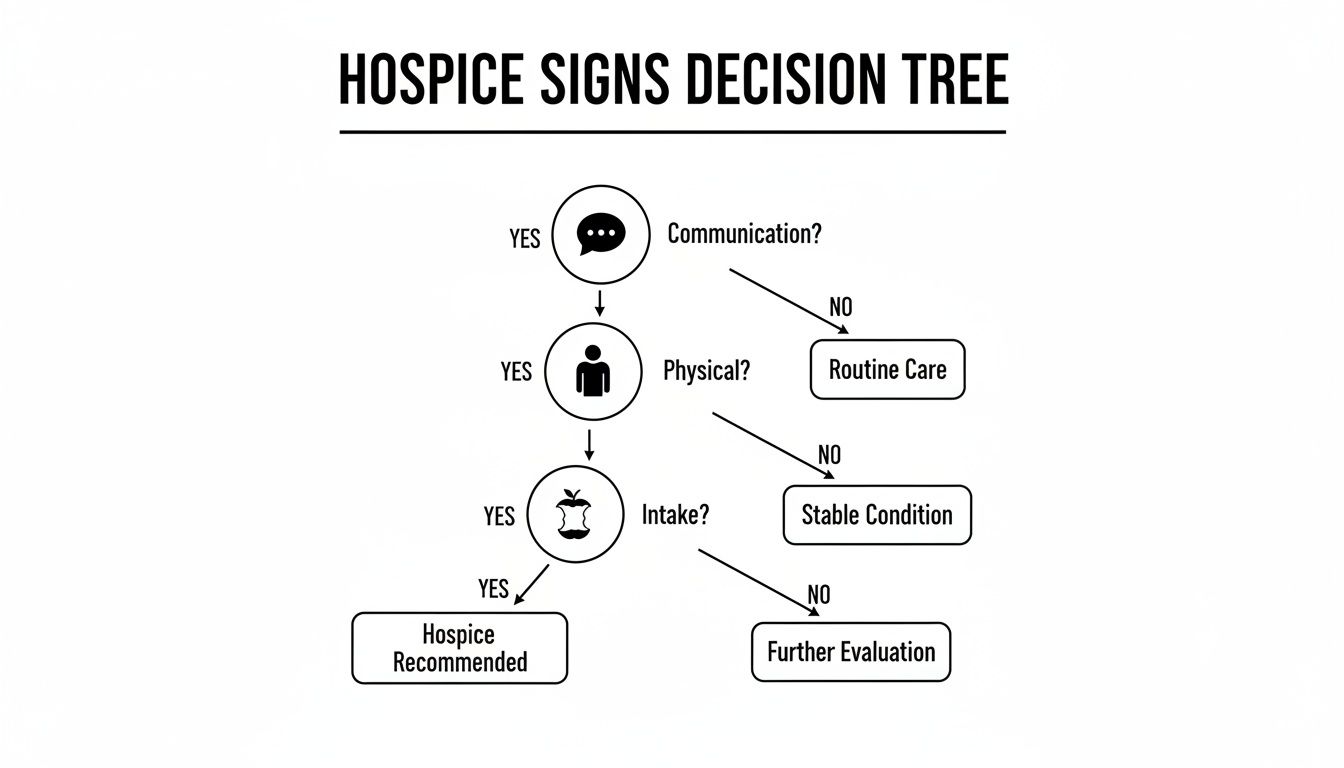
As the graphic shows, a decline across multiple areas usually opens the door to a hospice conversation.
Common Co-Occurring Conditions
A physician will look for at least one of the following health problems from the past year to complete the eligibility picture:
- Recurrent Infections: This could be pneumonia, urinary tract infections (UTIs), or sepsis.
- Significant Weight Loss: An unintentional loss of 10% or more of their body weight in the last six months.
- Difficulty Swallowing (Dysphagia): This can lead to choking and poor nutrition.
- Pressure Ulcers: The development of advanced bedsores (Stage 3-4) even with good daily care.
When one or more of these conditions appear with a FAST score of 7, it creates a clear medical basis for a hospice referral. This framework ensures your loved one gets the right care at the right time.
The Comfort and Support of Choosing Hospice Sooner

A common myth about hospice is that it is only for the last few days of life. This misunderstanding causes families to wait until a crisis, missing out on months of meaningful support.
Choosing hospice sooner is not giving up. It is a loving act that shifts the focus from cure to comfort, ensuring your loved one’s final chapter is lived with dignity.
Enhancing Comfort for Your Loved One
For a person with advanced dementia, symptoms like pain, agitation, and anxiety can be difficult to manage. An early hospice referral provides access to a team of experts trained in dementia care.
Our Registered Nurses work with your loved one’s doctor to manage symptoms, helping them stay calm and comfortable. This specialized attention can dramatically improve their daily experience.
Research shows that hospice care improves quality of life for dementia patients. A 2022 study found that 59% of dementia patients in hospice received 'excellent' care ratings from families, compared to just 28% for those not in hospice. Learn more about the benefits of hospice in dementia care from UCSF research.
A Circle of Care for the Whole Family
Hospice is a vital support system for the entire family. Caring for someone with advanced dementia is emotionally and physically exhausting. Our team at Central Coast VNA & Hospice steps in to share that load.
You gain a dedicated team offering essential support:
- Medical Social Workers provide emotional counseling and help you navigate difficult decisions.
- Chaplains offer spiritual guidance that respects your family’s beliefs.
- Hospice Aides can assist with personal care, like bathing and dressing, giving you a break.
- Specially trained volunteers offer companionship for your loved one, which gives you time to rest.
This network helps reduce stress, allowing you to focus on spending quality time together. You can explore more about the real benefits of starting hospice early in our related article.
How We Support Families on the Central Coast

Choosing a hospice provider is a decision built on trust. At Central Coast VNA & Hospice, our mission is to deliver expert, compassionate care to our neighbors.
We are a local, nonprofit organization with roots in this community going back more than 74 years. Our focus is your family’s comfort and well-being.
We understand the unique challenges of dementia care. From Salinas to Monterey and Hollister to Santa Cruz, we’re here to support you.
Your Dedicated Dementia Care Team
When you choose us, you get an entire team trained in dementia care. They work together to create a personalized plan that honors your loved one and supports your family.
Our team includes:
- Registered Nurses who are experts at managing symptoms like pain or agitation.
- Hospice Aides who provide gentle, hands-on help with personal care.
- Medical Social Workers who offer emotional support and practical guidance.
- Chaplains who provide spiritual care tailored to your family’s beliefs.
- Trained Volunteers who offer companionship for your loved one and respite for you.
This team approach ensures that every aspect of care—physical, emotional, and spiritual—is thoughtfully addressed.
A Seamless Continuum of Care
As the only organization on the Central Coast offering a full spectrum of home-based services, from home health to palliative care to hospice, we make the journey smooth. Many families already know us through our other programs.
When needs change, transitioning to hospice is a natural next step within a system they already trust. This continuum of care means your loved one can stay with a familiar, trusted team.
If you live in Monterey County, San Benito County, Santa Cruz County, or South Santa Clara County, our local team is ready to help. We can meet with you at home or in your loved one’s care facility to talk about your needs. There is never any pressure—just guidance from a team that has served this community for decades.
Learn more about how Central Coast VNA & Hospice supports lives across the Central Coast.
Taking the Next Step with Confidence
If you feel your loved one might be ready for hospice, the best next step is to talk with their doctor. This conversation can lead to a formal evaluation and bring peace of mind.
Remember, anyone—a patient, family member, or friend—can ask about hospice care. Our team at Central Coast VNA & Hospice is here to provide information and support whenever you need it.
How to Talk to the Doctor
When you speak with the physician, be specific. Share the changes you’ve noticed in their communication, physical strength, or overall health.
Asking direct questions can help start the conversation:
- "Based on the changes we’re seeing, do you think a hospice evaluation would be appropriate?"
- "Would you be surprised if their condition worsened in the next six months?"
- "What medical signs do you look for when deciding if hospice is the right choice?"
Requesting a Hospice Evaluation
A hospice evaluation is a no-obligation consultation to gather information. The doctor can make a referral, or you can call Central Coast VNA & Hospice directly to set one up.
One of our Registered Nurses will meet with you to assess your loved one's needs and see if they meet eligibility criteria. To qualify under Medicare, a person with advanced dementia typically needs to be at FAST Stage 7 and have secondary conditions like recurring infections. You can see the specifics in the official Medicare coverage determination guidelines.
We are proud to serve communities across the Central Coast, including Salinas, Monterey, Hollister, and Santa Cruz. To schedule a consultation, call us at (831) 375-9882 or visit our hospice care page.
Frequently Asked Questions About Hospice for Dementia
Making the decision to start hospice comes with many questions. Here are answers to some common concerns we hear from families.
1. Does choosing hospice mean we are giving up?
Not at all. Choosing hospice is not about giving up. It is about shifting the focus from cure to maximizing your loved one's quality of life. It’s an active choice to prioritize comfort, dignity, and peace.
2. Can my loved one still see their regular doctor?
Yes, absolutely. Our Central Coast VNA & Hospice team works alongside your loved one’s trusted physician. Their primary doctor remains a vital part of the care team, and we keep them informed every step of the way.
3. Does my loved one have to move to a facility?
No. The goal of hospice is to bring care to wherever your loved one calls home. For most families we serve in Salinas, Santa Cruz, and surrounding areas, this means their own private residence. We also provide care in assisted living communities and skilled nursing facilities.
4. How is hospice paid for?
Hospice is a fully covered benefit under Medicare Part A, Medi-Cal, and most private insurance plans. This coverage includes our care team's visits, medical equipment, supplies, and medications related to the dementia diagnosis. Our staff will explain your specific coverage so there are no surprises.
5. What happens if their condition improves?
Sometimes a person’s condition can stabilize or improve on hospice. If that happens, they can be discharged from hospice care. The door is always open to return to hospice later if their health declines again.
If you live in Salinas, Monterey, Hollister, or Santa Cruz, our hospice team can meet with you. Call (831) 375-9882 for guidance. Contact us today to learn more about our hospice care services.
Who Manages Medical Care After Starting Hospice? A Practical Guide
When a loved one starts hospice, families often ask, "Who's in charge of their medical care now?" Many people worry that choosing comfort means losing medical oversight from a doctor.
This is a common fear, but the reality is just the opposite. Medical care doesn't stop; it changes its focus. Instead of treatments to cure an illness, your loved one gets an entire team of specialists focused on comfort and quality of life at home.
Your New Medical Team After Starting Hospice
A big myth about hospice is that you give up medical supervision. In reality, you bring in a dedicated team to lead your loved one’s care plan. This team approach often provides more responsive and personal support than traditional healthcare.
Once hospice begins, this specialized team manages everything related to the patient’s terminal illness. This is a trusted model of care. According to the National Hospice and Palliative Care Organization (NHPCO), over 1.72 million Medicare beneficiaries received hospice services in 2020 (NHPCO, 2021).

This shift in medical management can feel like a big change. Here's a simple way to see how the focus of care changes.
How Medical Management Changes With Hospice
| Care Aspect | Before Hospice (Curative Care) | After Starting Hospice (Comfort Care) |
|---|---|---|
| Primary Goal | Curing the disease and prolonging life | Managing symptoms and maximizing quality of life |
| Primary Manager | The patient's primary care physician or specialist | The hospice interdisciplinary team, led by the hospice physician |
| Focus of Care | Aggressive treatments, hospitalizations, lab tests | Pain relief, emotional support, and personal comfort |
This table shows the move from a cure-focused mindset to a comfort-focused one, with a new team leading the way.
Introducing the Core Medical Team
At Central Coast VNA & Hospice, our team is built on patient-centered care refined over 74+ years of nonprofit service. The primary medical managers for your loved one will include:
- The Hospice Physician: This doctor has special training in end-of-life medicine and is often called the Medical Director. They create the patient's plan of care and lead the entire team.
- The Registered Nurse (RN): The RN is your case manager and main point of contact. They make regular home visits, check on symptoms, give medications, and teach the family how to provide care.
- The Hospice Aide: This certified professional provides hands-on personal care. They help with things like bathing and dressing to maintain a patient's comfort and dignity.
This team structure ensures that medical, emotional, and practical needs are all met. You can learn more in our guide on what happens when someone starts hospice care.
If a patient cannot make their own medical choices, the care team works with their legal representative. It's helpful for families to understand legal matters, like the Role of Guardians in Planning End-of-Life Wishes, to honor their loved one's choices.
The Role Of The Hospice Physician And Nurse
One of the most common worries we hear is that choosing hospice means giving up the patient's doctor. This myth often causes families to wait too long to get the support they need. The truth is, hospice care enhances medical supervision with a team of licensed professionals.
When a patient joins Central Coast VNA & Hospice, their medical care shifts to our specialized team. This model is at the heart of the U.S. hospice system, which serves millions of Americans each year. You can discover more insights about hospice care statistics to see how vital this support is.

The Hospice Physician: The Symptom Relief Expert
Think of the hospice physician as the expert for your loved one's care. This doctor is a specialist in pain and symptom management. They design and oversee the entire plan of care to make sure it works effectively.
The hospice physician works closely with every team member, especially the Registered Nurse. They review the patient’s progress and adjust medications to maximize comfort. While not in the home daily, their medical oversight guides every action the team takes.
The Registered Nurse: Your Hands-On Guide
The Registered Nurse (RN) is your family's case manager and main contact. They are the physician's eyes and ears in the home. The RN makes regular visits to check on symptoms, provide treatments, and update the rest of the team.
Our nurses are also compassionate teachers. They show family members how to handle daily care with confidence, like giving medications or knowing what to do if a new symptom appears. To learn more about the role of skilled nursing care, visit our blog.
At Central Coast VNA & Hospice, our medical team provides 24/7 on-call support. A licensed clinician is always a phone call away, ready to provide guidance or make an in-home visit. Families are never on their own.
Together, the hospice physician and nurse form a powerful partnership. This teamwork ensures medical care is thoughtfully tailored to your loved one’s unique needs. Their skills bring peace of mind to families across Monterey, San Benito, Santa Cruz, and South Santa Clara counties.
How Your Family Doctor Stays Involved
A big worry for families is losing a trusted family doctor. This is an understandable concern. This physician knows your loved one’s history and has built a relationship with them. Many people wrongly believe that hospice means saying goodbye to that doctor.
The truth is, hospice doesn't replace your doctor. It adds a team of specialists to work alongside them. It's a partnership, and you have a say in how your physician stays involved in the care plan.
Your Doctor Can Be Part of the Team
When hospice begins, your family doctor can stay on as the attending physician. In this role, they become a key collaborator with the hospice team. The doctor you know and trust continues to provide guidance and stays informed about your loved one's condition.
The hospice team will manage the day-to-day symptoms related to the terminal illness. This includes things like pain, shortness of breath, or anxiety. At the same time, your attending physician can help manage other health issues not related to the hospice diagnosis.
For example, if your loved one is on hospice for heart disease but also has diabetes, the hospice team will manage heart-related symptoms. Meanwhile, your family doctor can consult on their diabetes care, working with our experts.
At Central Coast VNA & Hospice, we respect the relationships patients have with their physicians. We welcome them as partners in care across Monterey, San Benito, Santa Cruz, and South Santa Clara counties.
A Focus on Collaboration and Comfort
Think of it this way: the hospice team brings expertise in comfort, while your family doctor brings a deep understanding of your loved one’s health history. We communicate regularly with the attending physician to give updates and discuss the care plan.
This teamwork ensures that medical decisions are seamless and honor the patient’s goals. By working together, the hospice team and family doctor create a strong support system. You aren't losing a doctor—you're gaining a whole team.
Understanding Your Full Interdisciplinary Team
The hospice physician and nurse manage your loved one’s direct medical needs. But they are part of a much larger team. Hospice is designed to support the whole person—not just physical symptoms.
This complete approach is where Central Coast VNA & Hospice shines. We bring together specialists who address the emotional, spiritual, and practical needs of the patient and family. This reflects the nonprofit mission we’ve upheld on the Central Coast for over 74 years.
More Than Just Medical Experts
The full care team includes professionals with unique and essential skills. Their roles are just as vital as the medical staff in managing care.
- Medical Social Worker: Our licensed social workers are expert guides. They help families with issues like advance care planning, connect them to community resources, and offer counseling.
- Chaplain: Spiritual care is a core part of hospice for people of all faiths and beliefs. Our chaplains provide a listening ear and support that honors your family’s personal values.
- Hospice Aide: Our certified Hospice Aides provide gentle, hands-on personal care. They assist with daily activities like bathing and dressing, which helps maintain comfort and dignity.
- Volunteers: Our specially trained volunteers offer companionship and a break for families. They might sit with a patient, read a book aloud, or simply provide a quiet, comforting presence.
This diagram shows how the entire hospice team works with your loved one's own doctor.
The key is partnership. The hospice team and attending physician work together closely, ensuring every aspect of care is covered.
At Central Coast VNA & Hospice, our interdisciplinary team meets regularly to discuss each patient’s needs. This ensures coordinated support for families in Monterey County, San Benito County, Santa Cruz County, and South Santa Clara County.
This team model means you are gaining a complete circle of support. For a deeper look, you can explore our family's guide to hospice care at home.
Managing Symptoms And Medications Around The Clock
A great comfort of hospice is knowing that expert medical help is always available. Families often fear being alone during a crisis in the middle of the night. With hospice, that anxiety is replaced by reassurance.
Once hospice begins, our team takes the lead on managing all medications and symptoms related to the terminal illness. Our goal is to keep the patient as comfortable as possible, 24 hours a day, seven days a week.

Around-The-Clock Clinical Support
This constant availability is a key part of hospice care. It allows patients to remain comfortably at home and avoid stressful trips to the emergency room.
At Central Coast VNA & Hospice, our clinical team is always on call. If a new symptom like pain appears at 2 a.m., you just call our number. A Registered Nurse will be on the line to walk you through it.
If needed, a nurse can make an in-home visit—day or night—to assess the situation and adjust treatments. This responsive care model means families in Monterey, Santa Cruz, and San Benito counties are never without expert help. You can read more about our specialized pain and symptom management services.
Expert Medication Management
Managing medications at the end of life can feel overwhelming. The hospice team simplifies this process. They work with the hospice physician to create a medication plan focused on comfort.
The team then coordinates with a pharmacy to have all prescriptions delivered to the home. They continuously monitor symptoms and adjust medications as needed. This proactive approach prevents crises and ensures peace and dignity.
This constant watchfulness is central to who manages medical care after starting hospice. It’s not just about having a plan; it’s about having a team ready to act at a moment’s notice.
How Central Coast VNA & Hospice Coordinates Your Care
A dedicated team manages medical care after starting hospice, not just one person. At Central Coast VNA & Hospice, our approach is built on 74+ years of nonprofit service to our local communities. The best care comes from a team that works together, with your family at the center.
Our interdisciplinary team meets regularly. We discuss each patient's progress and adjust the care plan to meet their changing needs. It's a truly collaborative process that puts your loved one first.
A Seamless Continuum of Care
This coordinated approach is what we are all about. As a local provider offering a full continuum of care, we provide smooth transitions from home health to palliative care and, when the time is right, to hospice care.
This means you work with a familiar, trusted organization every step of the way. You can read more about the difference this makes in our stories about how Central Coast VNA & Hospice impacts lives.
Our deep roots in Monterey County, San Benito County, Santa Cruz County, and South Santa Clara County drive us. We are your neighbors, committed to providing compassionate care to the communities we call home. You can learn more about the importance of teamwork and care coordination here.
Every family’s journey is unique, and our team is here to listen. We honor your loved one's wishes by creating a care plan that reflects their goals for comfort and dignity.
If you’re in Monterey, Hollister, Salinas, or Santa Cruz and have questions about hospice care, our local experts can help. We want families on the Central Coast to feel supported, not overwhelmed.
Contact Central Coast VNA & Hospice today at (831) 375-9882 to learn how our team can support your family. We’ll walk you through what to expect and how our medical team stays involved every step of the way.
Frequently Asked Questions About Hospice Medical Care
It is normal to have questions when considering hospice. Understanding the practical side of medical care can bring peace of mind. Here are some common questions we hear from families.
Who is in charge of medical care in hospice?
The hospice interdisciplinary team manages medical care. This team is led by a hospice physician and includes a Registered Nurse, Hospice Aide, and other professionals. They work together to manage symptoms and create a plan focused on comfort.
Can we keep our family doctor after starting hospice?
Yes, absolutely. Your family doctor can choose to stay involved as the "attending physician." In this role, they collaborate with the hospice team and remain a valued partner in your loved one’s care.
Who pays for medications after hospice starts?
The Medicare Hospice Benefit typically covers medications related to the terminal illness. The hospice team orders these medications and has them delivered to your home. Prescriptions for other conditions are usually still covered by your original insurance plan.
What happens if there is a medical emergency at night?
Instead of calling 911, you call the hospice team directly. Central Coast VNA & Hospice provides 24/7 on-call support from a Registered Nurse. A nurse can provide guidance over the phone or make an in-home visit, day or night, to manage the situation.
Does hospice mean stopping all medical treatments?
No. Hospice care shifts the focus from curing an illness to providing comfort. Medical care continues, but the goal is to manage symptoms and improve quality of life. Any treatment that makes the patient feel better is an important part of hospice care.
At Central Coast VNA & Hospice, our team is always here to provide clear answers and compassionate support. If you have more questions about hospice care in Monterey, San Benito, Santa Cruz, or South Santa Clara counties, contact us today at (831) 375-9882 or explore our services at https://ccvna.com.
Can I Get Skilled Nursing Care Without Moving My Parent?
Yes, you can. It is not only possible to get skilled nursing care without moving your parent into a facility—it is often the best choice for their health and happiness.
This means licensed medical professionals can provide vital services like wound care, medication management, and physical therapy. They deliver this care right in the comfort and safety of your parent's home.
Understanding At-Home Skilled Nursing Options
The conversation about moving a loved one into a nursing home is one of the toughest a family can face. It is filled with worries about their independence, comfort, and quality of care. Families often ask about alternatives when they feel a loved one isn't getting enough attention in a facility or want to avoid placement altogether.
But here is the good news: that move is often not necessary. The belief that "skilled care" can only happen in a facility is a common misstep. In reality, services from licensed professionals can be provided at home.
Skilled Nursing at Home vs. a Nursing Facility
To help you see the differences more clearly, let's break down what each option looks like.
| Feature | Skilled Care at Home | Nursing Home Facility |
|---|---|---|
| Environment | The patient's own comfortable and familiar home. | A clinical, institutional setting with multiple residents. |
| Care Team | A dedicated team of visiting Registered Nurses and therapists. | Rotating shifts of staff members serving many residents. |
| Independence | Promotes maximum independence and personal routine. | Structured schedules for meals, activities, and care. |
| Family Involvement | Family can be present and actively involved in daily care. | Restricted visiting hours and less direct involvement. |
| Cost | Often more cost-effective; may be covered by Medicare. | Can be very expensive, often requiring private pay. |
| Infection Risk | Lower risk of exposure to infections. | Higher risk of exposure due to a communal environment. |
As you can see, the benefits of staying home go far beyond comfort. They often lead to better health outcomes and greater peace of mind for everyone.
Rethinking Where Skilled Medical Care Happens
For many families, hearing that a parent needs advanced medical support brings an immediate, stressful thought: a nursing home. It can feel like an impossible choice between their safety and their desire to stay home.
But the reality is more flexible and hopeful than most people realize. The majority of seniors are aging at home. In fact, only 1% of seniors aged 65-74 and just 8% of those 85 and older live in nursing homes.
The term "skilled care" refers to medical services that must be performed by a licensed health professional, like a Registered Nurse or therapist. It's about who performs the care, not where it happens. Services like wound care, medication management, and rehab therapies can all be done at home.
What Skilled Nursing at Home Really Looks Like
When a doctor orders skilled nursing care at home, it involves specific, complex medical tasks. These can only be handled by a Registered Nurse (RN) or Licensed Vocational Nurse (LVN).
These trained professionals bring their clinical expertise directly to your parent. They are a part of Central Coast VNA & Hospice, a nonprofit, mission-driven provider serving the Central Coast for over 74 years.
For families here in Monterey and Hollister, this means a licensed nurse from Central Coast VNA & Hospice visits to:
- Manage IV Therapy: Administering intravenous medications or fluids is a delicate task that requires precise medical knowledge.
- Provide Complex Wound Care: Changing dressings on surgical wounds or treating pressure sores is crucial for preventing infection.
- Administer Injections: Giving necessary shots for conditions like diabetes or for pain management requires correct dosage and technique.
- Monitor Vital Signs: After a hospitalization, a Registered Nurse checks blood pressure and oxygen levels to track stability and catch issues early.
These duties are just a small sample of the professional support that defines skilled home health.
Patient and Family Education: A Core Part of the Service
Beyond hands-on medical tasks, a huge part of in-home skilled nursing is education. A visiting Registered Nurse from Central Coast VNA & Hospice does more than just treat a condition. They empower your parent and your family to manage it with confidence.
This educational role is vital for long-term health and independence. Think about real-world situations like:
- Teaching a patient how to check their blood sugar and safely administer their own insulin.
- Showing the family how to operate new medical equipment, like an oxygen concentrator.
- Explaining medication schedules, potential side effects, and why each prescription is important.
- Providing practical guidance on diet and exercise to help manage chronic conditions.
This level of professional support builds competence and reduces the anxiety that comes with managing a health condition. The goal is to create a support system that enables your parent to thrive at home.
How to Arrange Skilled Nursing Care at Home
Figuring out how to arrange skilled nursing care at home can feel like a maze, but it usually starts with a single step. The journey often begins with a conversation with a doctor.
The most important piece of the puzzle is a physician's order. Your parent's doctor must certify that the care is medically necessary.
Starting the Conversation with a Doctor
You do not have to wait for a hospital discharge planner to bring up home health care. Being proactive is one of the best things you can do.
Ask for a home health evaluation. If your loved one is homebound and recovering from surgery or managing a chronic illness, in-home skilled nursing may be covered by Medicare or health insurance. You don’t need to wait for a hospital to refer you.
A home health evaluation is a detailed assessment by a qualified clinician. A Registered Nurse will typically:
- Review Medical History: They’ll look at diagnoses, recent hospital stays, and all current medications.
- Assess Physical and Functional Needs: This involves checking mobility, strength, and ability to perform daily tasks.
- Evaluate the Home Environment: The Registered Nurse checks for safety risks and suggests helpful modifications.
- Discuss Goals: They'll talk with you and your parent about what everyone hopes to achieve with in-home care.
Gathering the Necessary Documents
To make everything go smoothly, it helps to have key information ready. When you work with an agency like Central Coast VNA & Hospice, these details speed up the intake process.
This infographic shows some of the core medical tasks that our skilled nursing staff can perform in your parent's home.
As you can see, services like IV therapy and wound care are managed safely at home by licensed professionals.
Try to have the following ready to go:
- Insurance Information: This includes Medicare, Medi-Cal, or private insurance cards.
- Physician’s Contact Information: The name and phone number of the doctor who ordered the care.
- List of Medications: A complete list of all prescriptions, over-the-counter drugs, and supplements.
- Medical History Summary: Key dates for surgeries or major health events are very useful.
Having this paperwork organized makes the first consultation more efficient. It allows the home health agency to verify benefits and start coordinating a plan of care. For more information, see our guide on qualifying for home health care in our guide.
Why Staying Home Is Often the Healthier Choice
The decision about skilled medical support goes beyond clinical care—it is about a parent's whole well-being. Many families find that bringing skilled nursing care into the home leads to better health outcomes. Data supports this, showing advantages when a loved one can recover in a familiar environment.
The comfort of being at home cannot be overstated. Surrounded by personal belongings and daily routines, a parent feels more secure and less anxious.
This sense of normalcy is a powerful part of healing. It reduces the stress that often comes with a stay in an unfamiliar facility. This familiar environment actively contributes to a more positive outlook, which can speed up recovery.
The Power of Consistent, Personal Care
This positive atmosphere translates into real clinical success. One study found home health care led to a 34% drop in hospital readmissions. This is a critical sign of effective, well-managed recovery.
One of the biggest wins for in-home skilled nursing is the consistency of the care team. Your parent can build a relationship with a dedicated group of professionals from a provider like Central Coast VNA & Hospice.
When a Registered Nurse from CCVNA visits, they know your parent’s history and what is "normal" for them. This continuity builds trust and ensures that subtle changes in health are caught right away. It's a level of personal attention that is tough to match in a facility.
Higher Satisfaction and Superior Outcomes
The numbers speak for themselves. Patients who receive skilled care at home often report higher satisfaction. They also tend to have better outcomes than those in institutional settings.
This is the model of care that Central Coast VNA & Hospice is built on. We have been serving California's Central Coast for over 74 years, delivering patient-centered care. For families in Monterey County, San Benito County, and Santa Cruz County, choosing skilled nursing at home means choosing excellent medical oversight and profound personal comfort.
You can read our detailed article about why it’s often safer to age at home instead of a nursing home.
How Central Coast VNA & Hospice Supports Your Family
Navigating the healthcare system for a parent is tough. But you do not have to go through it alone. For over 74 years, Central Coast VNA & Hospice has been a trusted, nonprofit partner for families on the Central Coast.
Our mission is to provide compassionate, top-tier medical care that honors your loved one’s wish to stay home. So when you ask, "Can I get skilled nursing care without moving my parent?" our answer is a confident yes. We are deeply rooted in the communities we serve, from Salinas to Santa Cruz.

A Collaborative Approach to In-Home Care
Effective in-home skilled nursing is a partnership. It is a collaboration between your family, your parent’s doctor, and our clinical team.
Central Coast VNA & Hospice provides skilled nursing care at home through licensed Registered Nurses (RNs), Licensed Vocational Nurses (LVNs), and therapists. Our team works with your physician to create a plan that meets medical needs while keeping your loved one comfortable and safe at home.
This teamwork is vital. It guarantees that every treatment is perfectly aligned with the doctor’s orders and your parent’s health goals.
Our Dedicated Team and Service Areas
This compassionate model is brought to life by our team of seasoned professionals. Every person on our team is committed to treating your loved one with dignity and respect.
We are proud to serve families across four counties. Our Continuum of Care progresses from home health to palliative and hospice care.
Our primary service areas include:
- Monterey County, including Salinas and the Monterey Peninsula.
- San Benito County, including Hollister.
- Santa Cruz County, including Santa Cruz and Watsonville.
- South Santa Clara County.
If your parent lives in one of these communities, our team is ready to help. Learn more about how CCVNA impacts lives across the Central Coast.
The decision to bring skilled care into the home is a powerful one. Our nonprofit mission is to make that choice a successful one for your family. Serving local families in Monterey, Hollister, Santa Cruz, and Salinas, CCVNA helps avoid facility placement when possible.
Is skilled nursing care at home the right fit for your situation? Call (831) 372-6668 to find out if it's the right fit for your situation. Contact us today to learn more about our services.
Frequently Asked Questions About In-Home Skilled Nursing Care
Here are answers to some of the most common questions we hear from families.
1. What is the difference between skilled nursing care and personal care?
Skilled nursing care is medical care that must be performed by a licensed nurse, such as a Registered Nurse (RN). It requires a doctor's order and includes services like IV therapy, injections, and complex wound care.
Personal care involves non-medical help with daily activities like bathing, dressing, and meal preparation. These tasks are typically handled by a home health aide.
2. How is in-home skilled nursing care paid for?
For patients who meet the requirements, Medicare Part A or Part B often covers 100% of the cost for intermittent skilled nursing at home. This includes visits from a Registered Nurse and physical or occupational therapy.
Other payment options include private health insurance, Medi-Cal, VA benefits, or private pay. Our team at Central Coast VNA & Hospice helps families in Monterey and Santa Cruz counties understand their coverage.
3. What does "homebound" mean for Medicare purposes?
"Homebound" is a Medicare term that causes confusion. It does not mean your parent is confined to their bed.
A person is considered homebound if leaving the house takes a considerable and taxing effort. They can still leave for medical appointments and short, infrequent non-medical trips. A doctor must certify that a patient is homebound for Medicare to cover home health services.
4. How often will a Registered Nurse visit my parent?
The frequency of visits is based on your parent’s medical needs, as outlined in the physician-ordered plan of care. A patient recovering from surgery might need daily visits at first. Someone with a chronic condition might only need a visit a few times a week.
The plan of care is flexible. Our clinical team communicates with the doctor to adjust the visit schedule as your parent's condition changes. Learn more in our guide on Medicare skilled nursing coverage.
5. Can we choose our own home health agency?
Yes, absolutely. Federal law guarantees you the right to choose which Medicare-certified agency provides your parent's care.
A hospital or doctor's office may provide a list, but the final decision is yours. Choosing an agency with deep local roots and a strong reputation, like Central Coast VNA & Hospice, helps ensure your parent receives the dedicated support they deserve.
At Central Coast VNA & Hospice, we have been the trusted choice for families on the Central Coast for over 74 years. If you believe your parent could benefit from skilled nursing care at home, contact us today to learn how we can support you. Visit us at https://ccvna.com to get started.










