When a hospital stay ends, the journey to recovery is often just beginning. For many, Medicare skilled nursing coverage provides a critical bridge between hospital care and returning home, but it's a benefit that's frequently misunderstood.
This coverage is designed specifically for short-term rehabilitation—not long-term care. It helps you regain your strength and independence after a qualifying hospital stay.
What Medicare Skilled Nursing Coverage Really Means

Trying to figure out healthcare options after a hospitalization can feel incredibly overwhelming for both patients and their families. One of the most important things to grasp is the role of a Skilled Nursing Facility (SNF) under Medicare Part A.
Its main purpose is to deliver the kind of intensive, daily medical support you need to recover. This is care that just isn't possible to manage at home yet.
Think of it this way: a hospital provides acute care to get you stable during a serious medical event. A SNF, in contrast, acts as a short-term rehab center. It’s the place you go to work with therapists and Registered Nurses to build back the strength and skills essential for a safe return to your daily life.
To give you a clearer picture, here’s a quick breakdown of what Medicare’s SNF coverage looks like.
Medicare SNF Coverage At a Glance
| Coverage Component | Description |
|---|---|
| Qualifying Event | Must follow a hospital stay of at least 3 consecutive days. |
| Purpose | Short-term rehabilitation and recovery, not long-term residency. |
| Care Provided | Daily skilled nursing care, physical therapy, occupational therapy, and speech therapy. |
| Goal | To help you regain independence and transition to a less intensive care setting, usually home. |
This table highlights the key elements, showing that the entire benefit is structured around active recovery.
The Goal is Recovery, Not Residency
A very common mix-up is thinking that SNF coverage is the same as long-term nursing home care. The reality is that Medicare’s benefit is strictly for restorative care right after a specific health crisis, like major surgery, a stroke, or a severe illness.
The entire focus is on making progress. Your care plan will be built around clear, achievable goals, such as:
- Regaining the ability to walk safely after a hip replacement.
- Improving speech and swallowing functions after a stroke.
- Learning how to manage complex wound care or new medications on your own.
Understanding this difference is vital for families planning the next steps. The whole point of medicare skilled nursing coverage is to get you well enough to move to a less intensive care setting—ideally, right back to your own home.
Your Local Partner in Post-Hospital Care
For over 74 years, Central Coast VNA & Hospice has been a trusted, nonprofit partner for families navigating these exact transitions. We work hand-in-hand with patients and hospitals across Monterey County, San Benito County, Santa Cruz County, and South Santa Clara County to make sure care continues smoothly.
As a mission-driven organization, our focus is entirely on your well-being. We help you understand your options so you can make informed decisions that honor your health goals.
Once your stay in a skilled nursing facility is complete, our team is ready to support your continued recovery. Many of our patients find that moving from a facility to receiving care at home is the perfect next step. Our professional team provides expert medical support in the comfort and familiarity of your own surroundings. You can learn more about how we bring skilled nursing care directly to your home.
How to Qualify for SNF Care Under Medicare
Trying to figure out Medicare's rules for skilled nursing facility (SNF) care can feel like a real head-scratcher. But getting a handle on the specific requirements ahead of time is the best way to make sure you get the benefits you're entitled to.
This empowers you to work with the hospital's discharge planner and sets you up for a much smoother transition.
At the core of Medicare skilled nursing coverage are a few non-negotiable rules. Think of these as firm requirements, not suggestions, that have to be met for Medicare Part A to step in and cover your stay.
The Critical Three-Day Hospital Stay
First and foremost, you must have a three-day qualifying hospital stay. Before Medicare will even consider covering SNF care, you have to be formally admitted to a hospital as an inpatient for at least three consecutive days.
A crucial detail: the day you are discharged doesn't count toward this total.
It's so important to understand the difference between being an "inpatient" versus being under "observation." Time spent in a hospital under observation, even if you’re in a regular hospital bed getting care, does not count toward this three-day requirement. You should always ask and confirm your admission status with the hospital staff to avoid any surprise gaps in coverage.
The Doctor's Certification and Medical Necessity
On top of the hospital stay, your doctor has to certify that you have a medical need for daily skilled services. This means your condition requires a level of care that can only be safely and practically delivered in an SNF setting.
This care must be provided by or under the watch of professionals like a Registered Nurse or a therapist.
These skilled services must be for the same condition that was treated during your hospital stay, or for a new issue that popped up while you were in the SNF. This "medical necessity" rule is how Medicare ensures the care is directly tied to your recovery.
Understanding the Benefit Period
Medicare coverage works in what's called a benefit period. A benefit period kicks off the day you're admitted as an inpatient to a hospital or SNF.
It only ends after you’ve gone 60 consecutive days without receiving any inpatient hospital or SNF care.
Once a benefit period ends, you have to have another three-day qualifying hospital stay to start a new one. This structure is designed to support recovery from distinct medical events rather than providing continuous, long-term care.
This is a really key concept to grasp when you're planning for care after a hospital visit. If you use up your 100 days of SNF coverage within a single benefit period, you'll be on the hook for the full cost until you can start a new one.
This infographic breaks down the costs you can expect for Medicare skilled nursing coverage within one benefit period.
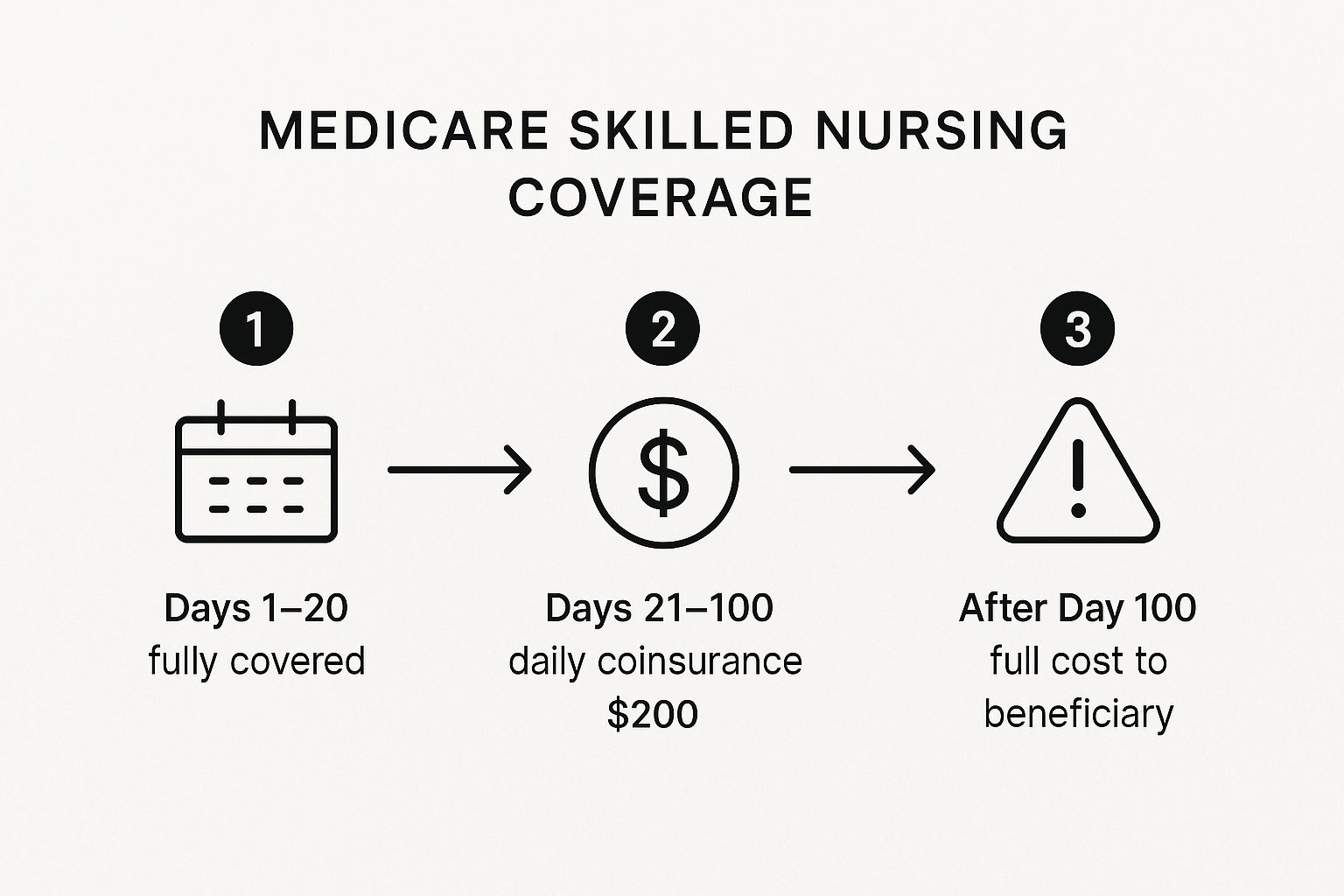
As you can see, what you pay out-of-pocket goes up quite a bit after the first 20 days of your SNF stay.
Connecting the Dots to Your Next Step
Meeting these requirements is the first hurdle to clear on your road to recovery. Once you qualify, you can be admitted to a Medicare-certified SNF.
For many families in Monterey County and the surrounding areas, this is when they start thinking about what comes next. Transitioning from the facility to skilled care at home is often the goal.
While SNF and home health care have their own distinct rules, knowing how to access both is a huge advantage. To help you prepare, you can review our guide on qualifying for home health care.
Central Coast VNA & Hospice has a 74-year history of helping families navigate these very transitions. Our team works hand-in-hand with local hospitals and doctors to coordinate care, making sure your recovery continues seamlessly whether you are in a facility or back in the comfort of your own home.
Understanding Your Costs During a SNF Stay

When a health event happens, the last thing you want are financial surprises. That's why getting a clear picture of the costs for Medicare skilled nursing coverage is so important.
When you know how the payment structure works for a Skilled Nursing Facility (SNF) stay, you and your family can prepare and make decisions with confidence.
Let's walk through what you can expect financially during a SNF stay covered by Medicare Part A. The entire system is built around a "benefit period," which kicks off the day you're admitted as an inpatient to a hospital or SNF.
Your Financial Responsibility Day by Day
How much you pay out-of-pocket changes the longer you stay. Medicare breaks down coverage for each benefit period into a few distinct phases, and each one has different rules for what you owe.
-
Days 1–20: Full Coverage
For the first 20 days of your stay in a benefit period, Medicare Part A covers 100% of the approved costs. This means your semi-private room, meals, skilled nursing services, and therapies are all paid for. You shouldn't have any out-of-pocket costs for these covered services. -
Days 21–100: Daily Coinsurance
From day 21 onward, you'll start sharing the cost. You become responsible for a daily coinsurance payment for every day you continue to need and receive skilled care. This dollar amount can change from year to year. -
Days 101 and Beyond: Full Cost
After 100 days in a single benefit period, Medicare coverage for the SNF stay ends. At this point, you are responsible for the full cost of your care.
Having this financial picture from day one is critical. According to Medicare.gov, the daily coinsurance for days 21-100 in 2024 is $200.00 (Medicare.gov, 2024). It's always a good idea to check official sources for the latest details to manage what you'll need to pay.
What Happens if You Are Readmitted
Recovery isn't always a straight line. It's not uncommon for someone to be discharged from a SNF, only to find they need to go back a short time later.
Medicare has specific rules for this exact situation that directly impact your costs.
If you leave the SNF and are readmitted within 30 days, your original benefit period just continues. This is great news, because it means you pick up right where you left off on your 100-day coverage clock without needing a new three-day hospital stay.
This 30-day readmission rule provides a crucial safety net. It ensures that your Medicare skilled nursing coverage can resume quickly if your condition requires it, without resetting your benefit period.
However, if you are out of the facility for more than 60 consecutive days without needing any skilled care, that benefit period officially ends. If you need SNF care again after that point, you would have to start over with a new three-day inpatient hospital stay to qualify for a new benefit period.
Figuring out these financial details is a key part of the recovery journey. For families here on the Central Coast of California who are planning for care after a hospital stay, Central Coast VNA & Hospice is a trusted, nonprofit partner ready to help you make sense of it all. We believe in empowering our patients and their families with clear, straightforward information.
For a wider look at managing healthcare costs, you might find these retirement financial planning resources helpful. It's also important to know how SNF care differs from other options, so feel free to check out our guide on understanding home health care to compare.
What Services Does Medicare Cover in a SNF?

When your doctor confirms that a Skilled Nursing Facility (SNF) is the next step in your recovery, it’s natural to wonder what your medicare skilled nursing coverage actually pays for. You can think of this benefit as a complete support system, designed to provide everything you need so you can focus on one thing: getting better.
It’s meant to be an all-inclusive recovery package. The entire goal is to give you a clear, holistic path back to health and independence.
Your Comprehensive Recovery Plan
During your stay, Medicare Part A covers a surprisingly wide range of services and supplies. This ensures your care team has all the resources they need to follow the recovery plan your doctor ordered.
Here’s a snapshot of what’s typically included:
- A Semi-Private Room: You’ll have a shared room, providing a comfortable space to rest and heal.
- Meals: All your meals are covered, including any special dietary plans prescribed by your doctor to help your recovery.
- Skilled Nursing Care: A Registered Nurse will provide daily skilled services, like administering IV medications or managing complex wound care.
- Medical Supplies and Equipment: Any necessary supplies (like bandages) or equipment (like a wheelchair) used inside the facility are part of the coverage.
- Medications: The medications you require during your stay are covered.
The Core of Your Rehabilitation
The real heart of your SNF stay is the intensive therapy you'll receive to regain function and strength. These services are the building blocks that will help you move forward.
Your rehabilitation is a team effort. Therapists, Registered Nurses, and Medical Social Workers collaborate to create a personalized care plan that addresses your specific needs.
Among the most important services covered, Medicare puts a strong emphasis on proven treatments like evidence-based physical therapy. Your therapy team will likely be made up of specialists in:
- Physical Therapy (PT): To rebuild strength, improve your balance, and get you moving again after an injury or surgery.
- Occupational Therapy (OT): To help you relearn the practical skills for daily life, like dressing, bathing, and eating on your own.
- Speech-Language Pathology Services: To address any communication or swallowing issues that might pop up after a stroke or other medical event.
- Medical Social Services: To offer counseling and help with planning your discharge when it's time to go home.
Once your SNF stay is over, the goal is almost always to continue your recovery at home. The skills and strength you build in the facility are the foundation for a successful transition back to your life.
Central Coast VNA & Hospice offers expert home health care services across Monterey, San Benito, Santa Cruz, and South Santa Clara counties. We bring that same level of professional care from Registered Nurses and therapists right to your door.
Choosing Between SNF and Home Health Care
After a hospital stay, one of the biggest decisions a family has to make is about the next step in recovery. It often comes down to two main choices: a stay in a Skilled Nursing Facility (SNF) or professional care at home.
This can feel overwhelming, but understanding what each option is designed for can bring clarity. Each setting supports a very different stage and intensity of the healing process.
Think of a SNF as an intensive recovery hub. It’s the right choice for someone who needs 24/7 medical supervision and several hours of high-level therapy each day, immediately after leaving the hospital.
On the other hand, professional home health care in Monterey is for when you’re medically stable enough to be in your own home but still need skilled support. It’s all about continuing your recovery in a comfortable, familiar setting while maintaining your independence.
Comparing the Care Environments
To make the best decision, it helps to see the two options side-by-side. A SNF provides an immersive, clinical environment, while home health care integrates personalized support into your daily life.
| Feature | Skilled Nursing Facility (SNF) | Home Health Care |
|---|---|---|
| Care Intensity | High: 24/7 medical supervision and intensive, daily therapy sessions. | Intermittent: Scheduled visits from a Registered Nurse or therapist a few times a week. |
| Living Environment | Structured: A clinical setting with shared rooms and a set daily schedule. | Familiar: The comfort and independence of your own home and routine. |
| Best For | Patients needing round-the-clock skilled care immediately after a hospital stay. | Patients who are homebound but stable enough to manage with periodic skilled support. |
| Goal | To stabilize and begin intensive rehabilitation to prepare for a return home. | To continue recovery, regain independence, and learn self-care skills at home. |
As you can see, the right choice really boils down to the patient's specific medical needs at that moment.
The Natural Next Step Toward Independence
For many people, the path to recovery is a gradual progression: from the hospital, to a SNF, and finally, to home health care to complete the journey. This continuum of care ensures you get the right level of support at every stage.
Continuing your recovery at home allows you to heal in a familiar, comforting environment. This can have a powerful positive impact on your well-being and progress.
Central Coast VNA & Hospice specializes in making this transition smooth and stress-free. As a trusted nonprofit organization with over 74 years of experience, we bring that continuum of care right to your front door. Our dedicated team of Registered Nurses and therapists provides the expert support you need to confidently finish your recovery at home.
For families in Monterey County, San Benito County, Santa Cruz County, and South Santa Clara County, this means you can have peace of mind knowing professional, compassionate care is always available. We're committed to helping you navigate every step of your recovery with expertise and heart.
Frequently Asked Questions About Medicare SNF Coverage
1. What is the difference between skilled nursing facility (SNF) care and nursing home care?
A Skilled Nursing Facility (SNF) provides short-term, intensive medical care and rehabilitation after a qualifying hospital stay. Its goal is recovery. A nursing home offers long-term custodial care, which is help with daily activities like bathing and dressing. Medicare’s skilled nursing benefit does not cover long-term nursing home care.
2. How much does a SNF stay cost under Medicare?
For each benefit period, Medicare covers 100% of the cost for the first 20 days. For days 21-100, you are responsible for a daily coinsurance payment ($200 in 2024). After day 100, you are responsible for the full cost.
3. What happens if I leave the SNF and need to return?
If you are readmitted to the SNF for the same condition within 30 days of leaving, you can continue your benefit period where you left off without a new 3-day hospital stay. If more than 60 days pass without SNF or hospital care, your benefit period ends and you would need a new qualifying hospital stay to start another one.
4. What should I do if Medicare denies coverage for my SNF stay?
If you receive a denial, you have the right to appeal. The denial notice will explain the reason and the steps for an appeal. You can get free, expert help with this process from the facility’s Medical Social Worker or your local State Health Insurance Assistance Program (SHIP).
5. What if I don't agree with the facility's decision to discharge me?
You have the right to a fast appeal if you feel you are being discharged too soon. The facility must give you a "Notice of Medicare Non-Coverage" at least two days before services end. This notice explains how to request an immediate, independent review of your case.
At Central Coast VNA & Hospice, we know these questions are just the start of a much bigger conversation. As a trusted nonprofit partner with over 74 years of service on the Central Coast, our team is here to provide the compassionate guidance you need. Whether you are transitioning from a SNF to home health or exploring our continuum of palliative and hospice care, we support your journey every step of the way. Contact us to learn more.
