Guide: How Do I Get Help at Home if Insurance Doesn’t Cover Everything?
When families ask, "How do I get help at home if insurance doesn’t cover everything?" the answer can feel overwhelming. This question often comes up when a loved one needs support, but coverage is limited or ends too soon. Families are left wondering: “Who fills in the gaps?”
It’s a journey that involves understanding your loved one's needs and exploring financial aid like Medi-Cal or VA benefits. It also means connecting with local nonprofits that can help. For families on the Central Coast, Central Coast VNA & Hospice is an essential guide for this exact challenge.
The Reality of Home Care Insurance Gaps
Discovering that insurance or Medicare won't cover all the in-home support your loved one needs can be jarring. Many families are shocked to find a gap between what insurance pays for and what is needed for safe living at home.

This gap exists because most plans, including Medicare, cover skilled medical care. This is care a doctor deems medically necessary, like short-term visits from a Registered Nurse. You can learn more in our guide on Medicare home care eligibility.
What Insurance Often Excludes
The problem arises when a person needs help with Activities of Daily Living (ADLs). Insurance usually calls this "custodial" care and does not cover it. Yet, these tasks make aging in place possible.
So what's left out? A lot.
- Personal Assistance: Help with bathing, dressing, and grooming.
- Companionship: Social interaction to fight loneliness.
- Household Help: Cooking, light housekeeping, and errands.
- Respite for Family: Giving a family caregiver a much-needed break.
Most older adults want to stay home as they age. In fact, 75% of adults over 50 say they want to remain in their homes. But nearly 95% have at least one chronic condition, requiring more care than insurance fully covers.
The table below shows what insurance typically handles versus what often needs other funding.
Home Health Insurance Common Coverage Gaps
| Type of Care | Typically Covered by Insurance | Often Requires Other Funding |
|---|---|---|
| Skilled Nursing | Wound care, IV therapy, medication management by an RN. | Medication reminders, transportation to appointments. |
| Therapy | Physical, occupational, or speech therapy post-injury or illness. | General exercise assistance, mobility support around the house. |
| Personal Care | Very limited, only if part of a skilled care plan. | Help with bathing, dressing, grooming, and toileting. |
| Household Support | Not covered. | Meal preparation, light housekeeping, laundry, shopping. |
| Companionship | Not covered. | Social interaction, safety supervision, accompanying to events. |
Understanding this difference is the first step toward finding a sustainable care solution.
A Common Scenario in Monterey County
Let's look at a real-world example. Imagine a family in Salinas whose father is recovering from a fall. His insurance covers a physical therapist twice a week and a nurse to check his vitals. But who helps him get to the bathroom at night or ensures he eats nutritious meals?
This is the gap where families feel the most pressure. The skilled medical needs are met, but the daily support for safety and quality of life is not. This leaves family members trying to fill in the blanks, often at great personal and financial cost.
At Central Coast VNA & Hospice, we see this all the time. Our role is to help families in Monterey, San Benito, Santa Cruz, and South Santa Clara counties build a complete circle of support. We help you understand these gaps and find solutions.
Creating a Clear and Actionable Care Plan
Before looking for funding, you need a map of the required help. A detailed care plan is that critical first step. It helps you understand your loved one's needs and communicate them to agencies.
Many people assume home health care covers everything from bathing to companionship. But medical home health is often short-term and clinical. Non-medical needs, like personal care or respite, may not be included.
This is why a thorough assessment is vital. You should plan early for how to supplement medical home health with local resources. Consider family caregiving schedules, adult day programs, and local volunteer support.
Evaluating the Full Spectrum of Needs
An effective care plan looks at the whole person. It ensures their safety, comfort, and emotional well-being are covered. Break down the needs into key categories to make it less overwhelming.
Grab a notepad and ask specific questions:
- Medical and Skilled Needs: Do they need wound care? Can they manage medications correctly? Do they need monitoring for a chronic condition?
- Personal Care Needs: Do they need help with bathing or dressing? Can they get to the bathroom safely?
- Household and Daily Living: Can they prepare nutritious meals? What about housekeeping, laundry, or grocery shopping?
- Social and Emotional Support: Are they lonely? Would companionship or community activities improve their quality of life?
This assessment is more than a checklist. It is a document that paints a clear picture of daily life. This plan helps organizations connect you with the right resources.
How a Professional Assessment Provides Clarity
Figuring this out alone can be daunting for families on the Central Coast, from Santa Cruz to Hollister. An expert assessment from a provider like Central Coast VNA & Hospice can make all the difference.
Our team of Registered Nurses and Medical Social Workers can conduct a professional evaluation in the home. This isn't just about finding problems; it's about providing a clear, actionable plan. We help you set priorities and build a solid support system.
Finding Financial Aid for In-Home Care
Once you know what care is needed, the next question is how to pay for it. The answer often lies beyond your traditional insurance policy.
Thankfully, several other funding sources are available. Many are specific to residents on California's Central Coast. Navigating these programs can feel complex, but you don't have to do it alone.
Exploring Government and State Programs
Several government programs help cover long-term care at home. For many families, these options are a lifeline.
Here are a few important programs to explore:
- Medi-Cal: California's Medicaid program offers initiatives for long-term care. The In-Home Supportive Services (IHSS) program can pay for non-medical help for eligible low-income seniors.
- VA Benefits: Veterans and their surviving spouses may qualify for benefits like Aid and Attendance. This pension supplement can be used to pay for in-home care.
- Area Agency on Aging (AAA): Your local AAA is a great resource. They often manage grants that provide support for seniors, including respite care, meal delivery, and transportation.
The first step is to break down the care plan into medical, personal, and household needs. This helps match the right need to the right funding source.
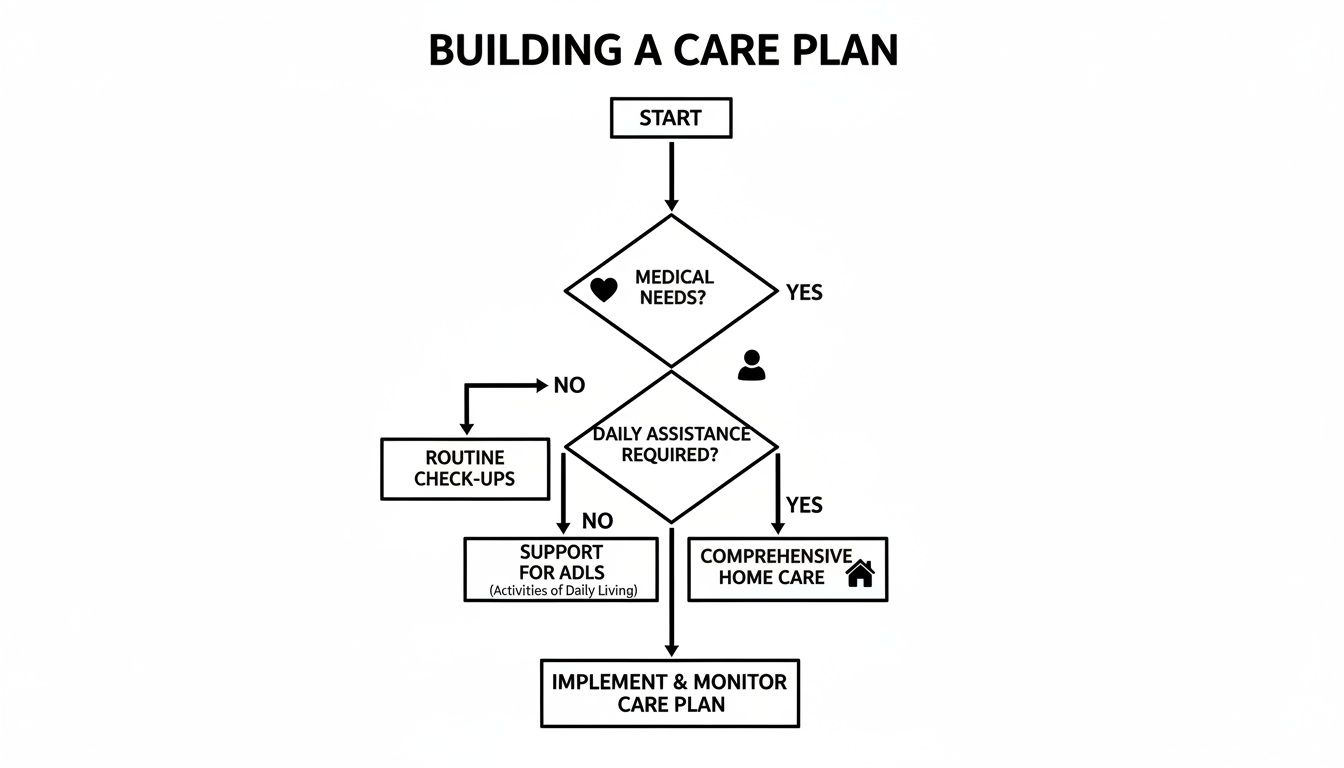
Separating these needs makes it easier to find programs designed for each type of care.
Tapping Into Disease-Specific and Nonprofit Aid
Beyond government aid, many foundations offer financial help for specific illnesses. Groups like the Alzheimer's Association or the American Cancer Society often have grants or local programs.
For those facing serious financial strain, looking into financial hardship grants can also provide relief.
This is where a mission-driven organization can be a powerful ally. Central Coast VNA & Hospice doesn’t just provide skilled nursing. Our team guides families through the entire care journey, helping you plan and coordinate services.
Because of our nonprofit status, our mission-driven support can include services like volunteer help and bereavement care. Learn more about how families can afford in-home care long-term in our guide.
Here’s a summary of some available programs.
Potential Funding Sources for Home Care
| Funding Source | Who It Typically Helps | What It May Cover |
|---|---|---|
| Medi-Cal (IHSS) | Low-income seniors and adults with disabilities in California. | Personal care (bathing, dressing), household help, meal prep. |
| VA Benefits (Aid & Attendance) | Eligible veterans and their surviving spouses. | Monthly pension supplement to pay for in-home care services. |
| Area Agency on Aging | Seniors in a specific geographic area (e.g., Monterey County). | Respite care, meal delivery, transportation, information services. |
| Disease-Specific Foundations | Individuals with specific diagnoses like Alzheimer's, ALS, or cancer. | Grants for care, equipment, or respite for caregivers. |
| Nonprofit Home Care Agencies | Community members, often regardless of ability to pay. | Skilled nursing, therapy, and support services on a sliding-fee scale. |
These programs exist to help families bridge the financial gap. Our Medical Social Workers at Central Coast VNA & Hospice are experts at this. They can help you identify which programs your family may qualify for and assist with applications.
Tapping Into Local Community and Nonprofit Support
When insurance falls short, money is only one part of the solution. The most meaningful support can come from people in your own community. Local and nonprofit resources can fill critical gaps in care.

We advise families to plan ahead. Think about blending skilled medical home health with community resources. Central Coast VNA & Hospice offers care coordination and can connect families to resources like veteran support, music therapy, or grief services.
Finding Community-Based Services
Across the Central Coast, from Santa Cruz to Hollister, a network of organizations offers support insurance rarely covers. These programs improve quality of life and help people stay safe at home.
It’s worth looking into these options:
- Local Senior Centers: Many run adult day programs with social activities, meals, and health monitoring. This combats isolation and gives family caregivers a break.
- Volunteer Services: Local nonprofits and faith-based groups often have volunteers who help with companionship, errands, or rides to appointments.
- Respite Care Grants: Some community organizations offer grants or low-cost respite services, giving family members a chance to rest. Find more advice on how to get real support as a family caregiver on the Central Coast.
These services are often funded by community donations and grants. This makes them accessible regardless of ability to pay. To learn how these organizations operate, you can explore the diverse sources of funding for nonprofits.
The Nonprofit Advantage at Central Coast VNA & Hospice
As a nonprofit serving our community for over 74 years, Central Coast VNA & Hospice is part of this local support network. Our mission-driven approach means we offer services that go beyond what’s medically billable.
Our own volunteer programs are a perfect example. We provide specialized services like pet therapy, music therapy, and bereavement support for families. These are all funded by the generosity of our community.
These programs are an essential part of our holistic care model. They address emotional and spiritual needs, providing comfort and connection. This commitment ensures families in Monterey, San Benito, and Santa Cruz counties receive comprehensive, compassionate support.
How Central Coast VNA & Hospice Bridges the Gap
Trying to arrange care when insurance falls short is like solving a puzzle with missing pieces. Central Coast VNA & Hospice can help. We are not just a medical provider; we are a partner here to guide your family.

Our team-based approach means every need—medical, emotional, or spiritual—gets attention. We bring all the support you need under one roof.
A Continuum of Compassionate Care
At Central Coast VNA & Hospice, we offer a continuum of care that adapts to your loved one's changing needs. A patient can move smoothly between our services without the stress of finding new providers.
Our services are designed to work together:
- Home Health: Our skilled nurses and therapists help patients recover from surgery or manage chronic conditions at home.
- Palliative Care: For those with a serious illness, our palliative team relieves symptoms and boosts quality of life.
- Hospice Care: When the time is right, our hospice team provides compassionate end-of-life care focused on comfort and dignity.
This integrated model ensures consistent, high-quality care every step of the way. See the difference we make by reading about how Central Coast VNA & Hospice impacts lives across the Central Coast.
Our Nonprofit Mission in Action
As a nonprofit with over 74 years of local roots, our commitment goes beyond what's billable. Thanks to community donations, we provide essential support that insurance does not cover. This can include volunteer visits, family bereavement counseling, and specialized therapies.
Our mission is to ensure every eligible person receives the care they deserve, regardless of their financial situation. We are here to help you understand your options and build a plan that works.
If you’re in Monterey, Hollister, Santa Cruz, or Salinas, our team can help. We can help you understand what your insurance covers and what your options are when it doesn’t. Call us at (831) 372‑6668 to speak with a care coordinator about in-home care planning.
Frequently Asked Questions About Funding Home Care
Navigating home care funding can be confusing. Below are answers to common questions we hear from families.
What should I do if my insurance denies a claim for home health care?
First, don't panic. Read the denial letter to understand the reason for the refusal. You have a right to appeal the decision.
Next, reach out to your provider, like Central Coast VNA & Hospice. Our team can provide medical documentation to build a stronger case. You can also contact California's HICAP (Health Insurance Counseling & Advocacy Program) for free help.
Does Medicare ever pay for long-term personal care at home?
Generally, no. Medicare does not cover long-term custodial or personal care. This includes help with daily tasks like bathing, dressing, or preparing meals.
Medicare covers short-term, skilled care prescribed by a doctor. For long-term personal care, you'll need to look at other funding routes. You can learn more in our resources on how to pay for hospice care.
Are there specific programs for veterans in Monterey County?
Yes. The Department of Veterans Affairs (VA) has programs to help veterans pay for in-home care. The most well-known are the Aid and Attendance or Housebound benefits.
These programs can provide a monthly stipend to eligible veterans and their surviving spouses. Central Coast VNA & Hospice can connect you with VA social workers and other resources to help secure these benefits.
How can a nonprofit like CCVNA help if I can’t afford care?
Our mission is to provide care to everyone in our community who needs it, regardless of ability to pay. Our focus is on the patient's well-being, not the bottom line.
Because of generous community donations, we can sometimes offer services on a sliding-fee scale. Our Medical Social Workers are experts at finding financial assistance and community resources to build a care plan that fits your family's budget.
What is the difference between medical home health and private-duty care?
Understanding this distinction is very important. They sound similar but are very different.
- Medical Home Health: This is the skilled, clinical care that Central Coast VNA & Hospice provides. It includes services like nursing and physical therapy prescribed by a doctor. This is often covered by Medicare and other insurance.
- Private-Duty Care: This refers to non-medical services like personal care, meal prep, and companionship. This type of care is typically paid for directly by the family.
The journey to find the right in-home support can be complex, but you don't have to do it alone. Central Coast VNA & Hospice is here to bring clarity and compassionate guidance to families in Monterey, San Benito, Santa Cruz, and South Santa Clara counties. Contact us today to learn more about your options at https://ccvna.com.
Why Palliative Care Isn’t Just for the End of Life
Many people think palliative care is about giving up. But it’s really about adding support.
Think of it as an extra layer of care. It focuses on improving your quality of life, and it's for anyone with a serious illness. You can start right from the moment of diagnosis. The simple truth is that you can—and should—get palliative care while actively pursuing treatments to cure your condition.
Understanding What Palliative Care Truly Is

Here on the Central Coast of California, families often confuse palliative care with hospice. It's a common misunderstanding. But it stops people from seeking help that could make a world of difference much earlier.
Palliative care works alongside your curative medical treatments. It does not replace your primary doctor or specialists. Instead, it adds a dedicated team focused on relieving symptoms, pain, and stress from serious illnesses like cancer or heart failure.
Palliative Care Quick Facts: What It Is vs. What It Isn't
To clear up any confusion, let's break down what palliative care really means. We will look at some common myths.
| Common Misconception | The Reality of Palliative Care |
|---|---|
| It’s the same as hospice. | It’s a separate specialty focused on quality of life and can be provided alongside curative treatment. |
| You have to give up your own doctors. | You keep your entire medical team. The palliative team collaborates with them. |
| It means you’re dying. | It can be started at any stage of a serious illness, even right at diagnosis. |
| It’s only for managing physical pain. | It addresses physical, emotional, and spiritual needs for the patient and family. |
This table shows that palliative care is a flexible resource. It is designed to help you live as well as possible, for as long as possible.
An Extra Layer of Support When You Need It Most
Imagine your medical team is focused on treating your illness. That’s their main job. A palliative care team works with them, but their focus is on you as a whole person. This support improves your daily life and helps you feel strong enough to continue treatment.
This support system helps you:
- Manage difficult symptoms like pain, shortness of breath, fatigue, or nausea.
- Reduce stress and anxiety by offering emotional and spiritual support.
- Improve communication between you, your family, and your entire medical team.
- Align your care with your personal goals and what truly matters most to you.
It's so important to understand that palliative care is about living with a serious illness. It is not just about preparing for the end of life. You can take a deeper dive by exploring what is palliative care in more detail on our site.
Rooted in Community and Compassion
For over 74 years, Central Coast VNA & Hospice has been the trusted local nonprofit provider of this care. Our mission is to bring this support to patients in their homes. We serve people throughout Monterey County, San Benito County, Santa Cruz County, and South Santa Clara County.
We believe everyone deserves to live with dignity. We want you to have the best possible quality of life at every stage of illness.
How Palliative Care Works With Your Medical Team

Many families are relieved to learn palliative care doesn't mean giving up their trusted doctors. It's the opposite. It is a collaborative service, adding a team of specialists who work with your current physicians.
Your primary doctor manages the main treatment plan to fight the illness. A palliative care team works as expert consultants. They make sure everything runs as smoothly and comfortably as possible.
This team approach means you get the best of both worlds. Your specialists can focus on treating the disease. Meanwhile, your palliative team concentrates on managing tough symptoms, pain, and stress.
Your Dedicated Support Team
Here at Central Coast VNA & Hospice, our palliative care team includes professionals from different backgrounds. They are all centered on your well-being. This ensures your care addresses not just physical symptoms, but your emotional and spiritual needs, too.
Your specialized team typically includes:
- A Registered Nurse or Nurse Practitioner specializing in pain and symptom management.
- A Medical Social Worker who provides emotional support and practical assistance.
- A Chaplain who offers spiritual support that respects your personal beliefs and values.
This team model provides holistic support. It recognizes that a serious illness impacts every part of a person's life. True comfort comes from caring for the whole person—body, mind, and spirit.
This coordinated effort lifts a huge burden off patients and families. You have a team of advocates making sure your care plan aligns with what matters most to you. You can learn more about how we integrate home health and palliative care for seamless support.
Creating a Coordinated Care Plan
This partnership is built on communication. Your palliative care team stays in regular contact with your other doctors. They share insights into how you're feeling and responding to treatments. This leads to better, more personalized care.
The result is a unified approach that keeps you at the center. The team helps explain complex medical information. They empower you to make informed decisions that reflect what is most important to your quality of life.
This proactive support also helps people stay comfortable at home. It can reduce emergency room visits and hospital stays. You can read more about these palliative care findings and their impact.
The Benefits of Starting Palliative Care Sooner
Many families wait too long to talk about palliative care. This is a common mistake. It often means missing out on the greatest benefits.
The best time to add this extra layer of care is at the beginning of a serious illness. This lets you and your loved ones manage symptoms and reduce stress from day one.
This proactive approach shows why palliative care isn't just for the end of life. It’s about improving your quality of life for all the days you have. By bringing in a team focused on comfort, you can better manage a serious illness while still pursuing treatments.
Improve Your Daily Quality of Life
One of the first things people notice after starting palliative care is how much better they feel. A serious illness often comes with a heavy burden of pain, fatigue, or nausea. These symptoms drain your energy and spirit.
The palliative care team works with your doctors to fine-tune medications and other therapies. Their goal is to make you feel better. This frees you to regain strength, get back to activities you love, and hold onto your independence.
At Central Coast VNA & Hospice, our nonprofit mission drives us to bring this compassionate support to your home. We serve patients across Monterey, Salinas, Hollister, and Santa Cruz. You can learn more in our guide to the benefits of palliative care.
Reduce Stressful Hospital Visits
Nobody enjoys frequent trips to the ER or hospital stays. They are a massive source of stress. Early palliative care can cut down on these events.
By actively managing symptoms at home, the team can often get ahead of problems before they become a crisis. This means more time spent in the comfort of your own home. For families, it means less worry.
This approach can prevent avoidable hospital admissions. It allows people to age in place with dignity.
Strengthen Emotional and Family Support
A serious illness is an emotional battle for the entire family. Palliative care understands this. That’s why the team includes Medical Social Workers and Chaplains.
This support system helps everyone by:
- Facilitating difficult conversations about care goals and future wishes.
- Providing counseling to help cope with the anxiety and stress.
- Connecting families with community resources for practical help.
- Offering spiritual guidance that respects your personal beliefs.
This comprehensive support ensures no one faces the challenges alone. For those hoping to maintain independence, an aging in place checklist can be a great step. By starting palliative care sooner, you give your family the gift of support and peace of mind.
Who Is a Good Candidate for Palliative Care?
Deciding if palliative care is the right choice can feel complicated. But it boils down to something simpler: Could you or your loved one use extra support to manage a serious illness?
This is not about timelines. It is about need. Palliative care is for patients of any age at any stage of a serious illness. That is why palliative care isn’t just for the end of life—it’s for living better, right now.
Common Conditions That Benefit from Palliative Care
Many serious illnesses have a heavy burden of symptoms and stress. Palliative care is especially helpful for people managing:
- Cancer: To control pain, nausea from chemotherapy, and fatigue.
- Heart Disease: Including congestive heart failure (CHF), to ease shortness of breath.
- Lung Disease: Such as Chronic Obstructive Pulmonary Disease (COPD), to improve breathing.
- Kidney Disease: To help with symptoms like fatigue and discomfort.
- Dementia or Alzheimer’s Disease: To navigate behavioral changes and support the family.
- Neurological Conditions: Like Parkinson’s disease, ALS, or the effects of a stroke.
Getting the right support is critical. For instance, families often find value in resources like guides on caring for dementia patients, which complement help from a palliative team.
Look for the Signs, Not Just the Diagnosis
More important than the diagnosis are the real-world challenges. You do not have to wait for a doctor to bring it up. If this sounds familiar, it’s time to ask about palliative care:
- Uncontrolled Symptoms: There is persistent pain, fatigue, nausea, or shortness of breath.
- Frequent Hospital Visits: You have had multiple trips to the ER or hospital in the past year.
- Decreased Ability to Care for Oneself: Daily activities like bathing or dressing have become difficult.
- Significant Stress and Anxiety: The illness has left you or your family feeling overwhelmed.
Recent data shows that 95% of people over 60 have at least one chronic condition. Palliative care helps manage symptoms and stress, even years before hospice is needed.
If these challenges sound familiar, our Central Coast VNA & Hospice team is here to help. We can help you understand your options in Monterey County, San Benito County, and the surrounding areas.
Palliative Care vs. Hospice: Clarifying the Key Differences
To make the best decision, it’s vital to know how palliative care and hospice are different. Both focus on comfort. But they serve different needs at different times.
The biggest myth we see on the Central Coast is that they are the same. This is not true. Palliative care is an extra layer of support you can get at any stage of a serious illness, alongside curative treatments.
Hospice care is a specific type of palliative care for people near the end of life. It begins only when curative treatments have stopped. The focus shifts entirely to comfort and peace.
Palliative Care and Hospice at a Glance
For families in Monterey, Salinas, and Hollister, healthcare terms can feel overwhelming. This table makes the differences clear.
| Feature | Palliative Care | Hospice Care |
|---|---|---|
| When It Starts | At any stage of a serious illness, right from diagnosis. | When life expectancy is six months or less, and curative treatments have stopped. |
| Treatment Goals | To relieve symptoms and stress while you continue curative treatments. | To provide comfort, peace, and dignity when a cure is no longer the goal. |
| Who It's For | Patients of any age with a serious illness like cancer, heart disease, or COPD. | Patients with a terminal diagnosis who have chosen to focus on quality of life. |
| Where It's Provided | Often delivered at home, alongside your regular doctor visits. | Primarily provided at home, but also in facilities, with 24/7 on-call support. |
The core difference is that palliative care works with curative treatment. Hospice care is for when treatment has stopped. This is why palliative care isn’t just for the end of life—it’s a powerful resource for living better with a serious illness.
Making the Right Choice for Your Family
Choosing between these options isn’t about giving up. It's about getting the right support at the right time. Palliative care offers relief and strength during a long illness. Hospice provides comfort for the final chapter of life.
The following graphic shows some of the conditions that lead families to consider palliative support.
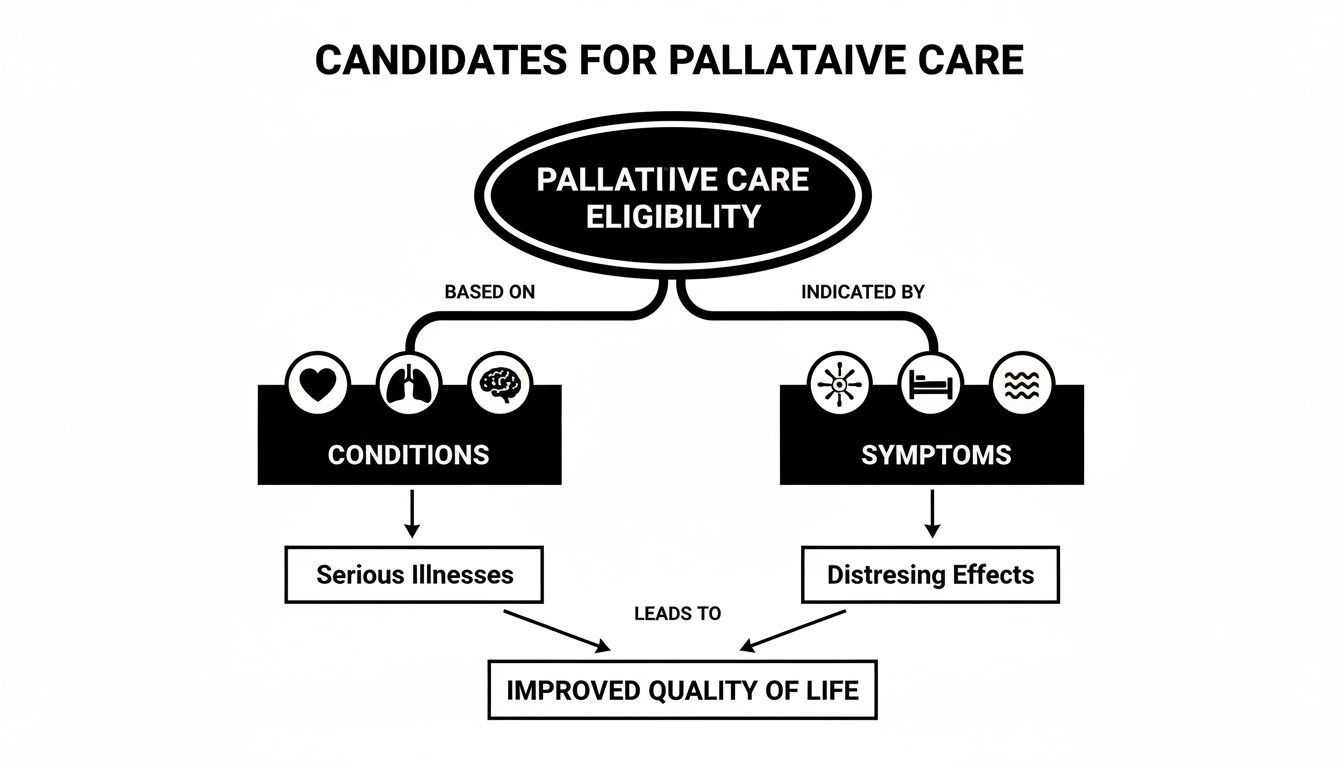
This visual shows how palliative care addresses the whole person. The goal is to improve quality of life by managing symptoms from a serious health condition.
At Central Coast VNA & Hospice, our continuum of care means we are the local nonprofit offering home health, palliative care, and hospice. This provides a seamless transition if a patient’s needs change. For a deeper look, learn more about the real differences between hospice and palliative care.
How To Get Started With Palliative Care On The Central Coast

Taking the first step is simpler than you might think. If your loved one could benefit from better symptom management, the process starts with one conversation.
Reaching out is not a final commitment. It is an exploration of the support available to you. This is a big reason why palliative care isn’t just for the end—it’s a resource you can use anytime to improve comfort.
Starting The Conversation With Your Doctor
Your first move is to talk to your physician or specialist. Palliative care almost always requires a doctor's referral. They are the natural starting point.
When you go to the appointment, be ready to talk about specific challenges. Explain which symptoms are causing the most trouble.
You can be direct and ask, "Could palliative care help us manage these symptoms?" This helps your doctor focus on your needs. Remember, asking for help is a sign of strength.
Accessing Palliative Care At Home
Once you have a referral, Central Coast VNA & Hospice makes the rest of the process easy. As a trusted local nonprofit with over 74 years of service, our mission is to bring expert care to your doorstep. We serve patients in their homes across Monterey County, San Benito County, Santa Cruz County, and South Santa Clara County.
Our palliative care team will coordinate with your doctor to build a support plan. We handle the logistics so you can focus on feeling better. You can learn more about our local services by exploring information on palliative care near me.
Understanding Your Insurance Coverage
One of the first questions families ask is about cost. The good news is that palliative care is covered by most insurance plans. This makes it an accessible option.
Here is a quick breakdown of typical coverage:
- Medicare Part B: This covers palliative care services like any other specialist visit.
- Medi-Cal: Provides coverage for palliative care consultations and follow-up visits.
- Private Insurance: Most private and employer-sponsored health plans include palliative care benefits.
Our team at Central Coast VNA & Hospice can help you verify your coverage. We believe financial worries should never stand in the way of getting compassionate care.
Ask your provider whether your loved one qualifies for palliative care—not just hospice. Look for services that provide both, so transitions can be handled smoothly later if needed.
If you're caring for someone with a serious illness in Monterey, Salinas, Hollister, or Santa Cruz, our VNA team can help you understand your options without pressure. Visit ccvna.com or call 831‑372‑6668 to speak with a nurse.
Frequently Asked Questions (FAQs)
It’s normal to have questions as you explore care options. Here are some common ones we hear from families on the Central Coast.
1. Does choosing palliative care mean I’m giving up?
Absolutely not. It is the opposite. This is a key reason why palliative care isn't just for the end of life. Palliative care works with your curative treatments, like chemotherapy. Its job is to help you manage symptoms and stress. By helping you feel stronger, it empowers you to stick with your doctor's plan.
2. Who is on a palliative care team?
You get a whole team of specialists. The goal is to address your physical, emotional, and spiritual well-being. At Central Coast VNA & Hospice, our team includes a Registered Nurse, a Medical Social Worker, and a Chaplain. This team works with your own doctors to coordinate care.
3. Is palliative care only for people with cancer?
No, not at all. It is for anyone living with a serious or chronic illness. This includes conditions like heart disease (CHF), lung disease (COPD), kidney failure, and dementia. The focus is always on improving your quality of life right now.
4. Where do you provide palliative care?
Palliative care can be offered in hospitals or clinics. But at Central Coast VNA & Hospice, we bring that support directly to you, wherever you call home. We provide care in your house or an assisted living facility. We serve communities across Monterey County, San Benito County, Santa Cruz County, and South Santa Clara County.
5. How is palliative care paid for?
Most people are surprised to learn that palliative care is treated like any other medical specialty. It is typically covered by Medicare Part B, Medi-Cal, and most private insurance plans. Our team at Central Coast VNA & Hospice can help you figure out your specific coverage.
If you're caring for someone with a serious illness in Monterey, Salinas, Hollister, or Santa Cruz, you don't have to figure this out alone. Our team at Central Coast VNA & Hospice can help you understand your options without any pressure. Visit our website or call 831‑372‑6668 to speak directly with a nurse.
The Shift Driving More Seniors to Stay at Home in 2026
A quiet but powerful shift is happening in homes across the Central Coast and the nation. More seniors are choosing to age in place, surrounded by the comfort and memories of the homes they love. This is a fundamental change in how we think about long-term care.
This movement is driven by personal choice, financial sense, and a deep desire for safety.
The Unmistakable Trend: Why More Seniors Are Choosing Home

The message from older adults is clear: they want to stay home. Instead of moving to a facility, they are opting to receive care where they feel most comfortable. This preference is reshaping healthcare for families and providers alike.
The reasons are both practical and personal. Home is a lifetime of memories, a connection to neighbors, and the freedom to live by one's own rules. For many, preserving that dignity is essential.
The Driving Forces Behind Aging in Place
Several powerful factors are making in-home care a more appealing choice. This is true for families in Monterey County, San Benito County, Santa Cruz County, and South Santa Clara County.
- A Desire for Autonomy: At home, seniors decide their own schedule. This simple independence is something they value deeply.
- Emotional Well-being: Being in a familiar space has a huge impact on mental and emotional health. It brings an undeniable sense of peace.
- Health and Safety: For many families, home now feels like the safest place to receive care. It helps minimize exposure to illnesses often found in group settings.
The numbers tell the same story. A recent poll found that an overwhelming 75% of adults 50 and older say they want to age in place. This desire is a major driver behind the growing demand for at-home senior care services.
This preference is also fueled by cost. Professional home-based care is often a much more sustainable option for many families compared to expensive facility care.
Key Drivers for Seniors Choosing Home Care in 2026
The shift toward home is pushed by a few key motivations. This table breaks down what is behind this growing preference.
| Driving Factor | Impact on Seniors and Families |
|---|---|
| Personal Independence | Seniors maintain control over their daily routines, diet, and social life. |
| Emotional Comfort | Staying in a familiar environment reduces stress and promotes mental well-being. |
| Financial Savings | Home care is often more affordable than facility-based options. |
| Health & Safety | Reduces exposure to infections common in congregate settings. |
| Family Connection | Makes it easier for family and friends to visit and stay involved in care. |
These factors create a compelling case for why home is becoming the preferred setting for long-term care.
Creating a Comfortable and Safe Home
As more seniors decide to age in place, making the home environment supportive is key. Simple adaptations can make a world of difference. This might include adding grab bars, improving lighting, or selecting furniture like the best recliners for seniors.
For families on the Central Coast, organizations like Central Coast VNA & Hospice meet this growing need. You can learn more about why home health care is growing fast on the Monterey County coast on our blog.
Exploring the Forces Behind the At-Home Movement
The growing desire for seniors to stay home is not a coincidence. It is a powerful shift driven by personal wishes, practical finances, and a major change in our population. Understanding these forces helps families prepare for what lies ahead.
Three big drivers are fueling this trend here on the Central Coast and across the nation. Each one is reshaping the future of senior care.
The Demographic Wave
First and foremost, America is getting older. This simple fact is the engine behind the at-home movement. A significant 4.1 million Americans turned 65 in 2024, creating a huge wave of new seniors.
This is a generation that has always prized its independence. This is a local reality for families in Monterey, Salinas, and Hollister. As more of our neighbors enter their senior years, the demand for healthcare that fits their values is skyrocketing.
The Economic Reality of Senior Care
The second powerful force is the financial difference between care facilities and aging at home. The costs of nursing homes can quickly become overwhelming. This often creates incredible stress for families.
In-home care offers a much more manageable financial path. Services are designed to fit specific needs, so families only pay for the support required.
This could include:
- Skilled Nursing Visits: A Registered Nurse can handle medical needs like wound care or medication management at home.
- Therapy Services: Physical, occupational, or speech therapy can be delivered in a patient's own living room.
- Palliative and Hospice Care: Specialized support for serious illness or end-of-life care can be provided at home.
This flexibility makes professional home-based care a practical choice. It lets families in Santa Cruz and San Benito counties put resources toward targeted medical help. You can learn more by reading about the 6 home care trends Central Coast families should watch in 2026.
The Powerful Preference for Independence
Finally, we have the most personal force of all: the deep need for comfort and independence. Home is a sanctuary filled with memories and familiar routines. Leaving that behind can feel like losing a piece of yourself.
Staying at home means seniors can keep their daily rhythms. This sense of control is directly linked to emotional well-being and quality of life.
A home care plan is built around the individual. It adapts to their life, rather than forcing them to adapt to an institution. For over 74 years, Central Coast VNA & Hospice has helped families build these kinds of personalized plans.
The Growing Gap Between Senior Needs and Available Care
The desire to age in place is running up against a hard reality. The healthcare system is not always built for it. As seniors choose to remain home, a gap is opening between the care they need and what is available.
This leaves families scrambling to find consistent, reliable in-home care. This is especially true when different services are isolated from one another.
A Family's Journey Through Uncoordinated Care
For healthcare providers and families, this shift means more pressure. They must manage chronic conditions and mobility issues without facility placement. The current system often makes this difficult.
Organizations that treat home health, palliative care, and hospice as isolated offerings risk confusing patients. Without clear guidance across the continuum of care, families may delay decisions. This can lead to preventable health crises or costly ER visits.
This kind of fragmented care creates real pain points:
- Disjointed Communication: Families are forced to be the messenger between different agencies that rarely talk to each other.
- Preventable Hospital Visits: Small problems can quickly turn into major health crises without one team seeing the big picture.
- Emotional and Physical Burnout: Juggling appointments, medications, and different care teams is exhausting for family members.
The Looming Supply Crunch
Finding care is already tough, and it may get harder. The construction of new senior living facilities is not keeping pace with our aging population. This will push even more seniors to seek care at home.
This "development/demand divide" is setting the stage for a challenge. Demand is set to explode as the oldest Baby Boomers turn 80. You can explore more data on senior living trends to see the full scope of the issue.
This is the problem Central Coast VNA & Hospice was founded to solve. For over 74 years, our nonprofit mission has been to offer a seamless continuum of care under one roof. Our integrated model is designed to close that care gap for families in Monterey, San Benito, Santa Cruz, and South Santa Clara counties.
How a Continuum of Care Bridges the Gap for Seniors
The growing gap between what seniors need and what our healthcare system offers can be frustrating. There is a better way, built on the idea of a continuum of care. This approach helps families avoid disjointed services.
Think of it like having a trusted guide for a long journey. This guide walks alongside you and anticipates the twists and turns ahead. That is what an integrated continuum of care does for families.
Understanding the Integrated Care Model
A continuum of care is an integrated system that follows a patient through every stage of their health journey. It connects home health, palliative support, and hospice under one coordinated team. This model eliminates the confusion many people experience.
As a patient's needs change, the transitions are seamless. The same trusted team that already knows your history and wishes stays involved. This is how we can address the shift driving more seniors to stay at home in 2026.
This growing gap between what seniors need and what a disconnected system can provide is a real challenge.
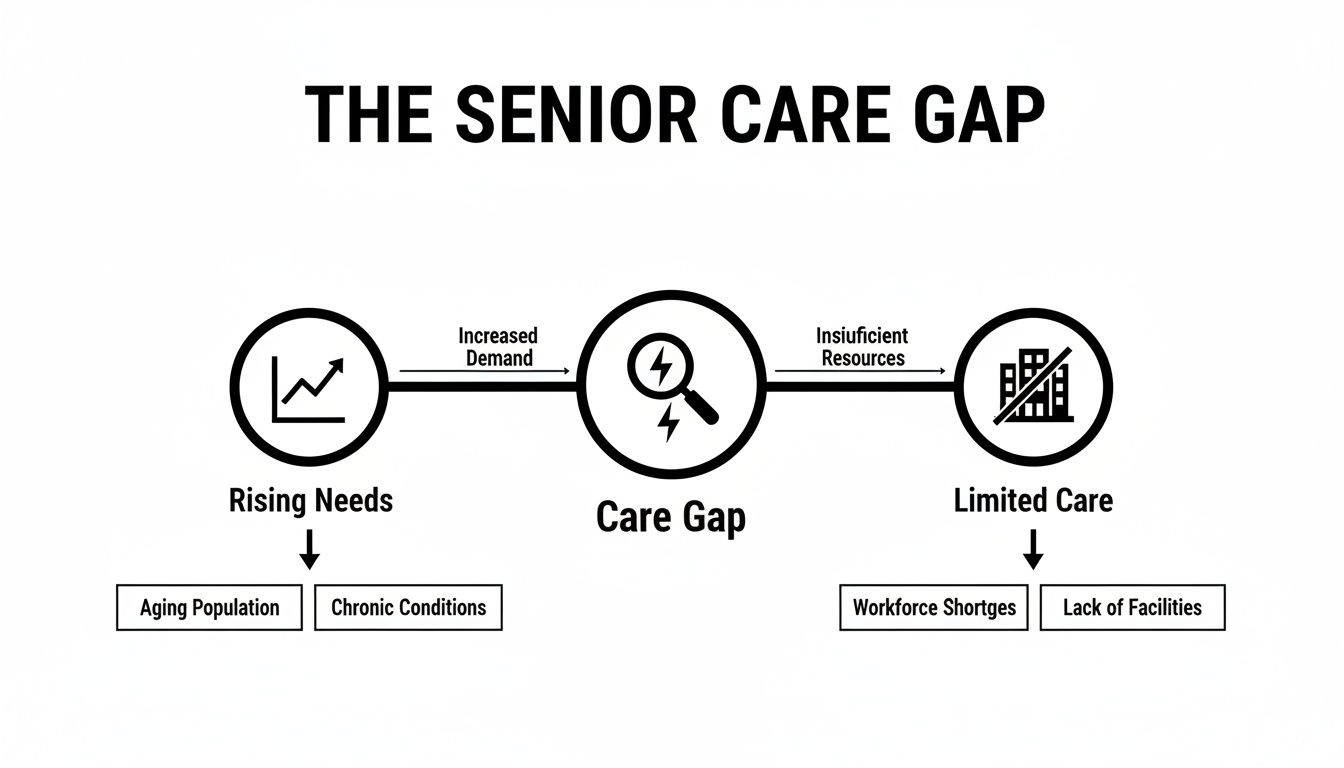
The visual above shows why a unified approach is essential. It ensures seniors get consistent, reliable support.
How a Single Provider Makes a Difference
When one organization provides the full spectrum of home-based care, the benefits are immediate. Central Coast VNA & Hospice has spent over 74 years perfecting this model. Our approach is built on core principles.
- Seamless Transitions: If a home health patient’s illness progresses, our team can introduce palliative care without disruption. The transition to hospice is handled with compassion by clinicians who already know them.
- Coordinated Communication: Our Registered Nurses, therapists, social workers, and Hospice Aides are all part of the same team. They communicate constantly so you never have to repeat your story.
- Clinically Superior Outcomes: This leads to better health outcomes. By managing symptoms proactively, we can reduce preventable hospitalizations and improve quality of life.
At its heart, the continuum of care is about providing the right care, at the right time, in the right place. It replaces confusion with clarity and stress with support.
For families in Monterey, Hollister, Santa Cruz, or South Santa Clara County, this means you have a dedicated partner. You can see this model in action by learning more about how our expert teams provide skilled nursing at home.
Why a Nonprofit Mission Matters
As the only local provider offering this full continuum of care, Central Coast VNA & Hospice operates as a nonprofit. This is a critical distinction. Our mission is driven by the needs of our community, not by shareholder profits.
This focus allows us to pour our energy into what truly matters. We deliver compassionate, high-quality care that honors each person's wish to remain at home.
What Integrated Home-Based Care Really Means for You

Choosing an integrated care model goes far beyond convenience. It delivers real benefits that improve a patient’s quality of life and give families peace of mind. This unified approach makes the wish to stay home a safe reality.
When a single, mission-driven team oversees a patient's entire journey, the care becomes smarter. It is more responsive and deeply personal. It is the difference between a stressful experience and a seamless one.
No More Broken Telephone
With separate agencies, families often find themselves playing messenger. An integrated model eliminates this risk.
At Central Coast VNA & Hospice, our Registered Nurses, therapists, and Hospice Aides are part of one connected team. Proactive communication helps us catch potential issues before they become serious problems.
Keeping You Safely Out of the Hospital
One of the biggest wins with coordinated home-based care is a drop in avoidable ER visits. Our clinical teams work in sync to manage symptoms and teach families how to handle challenges at home. This is more important than ever as the shift driving more seniors to stay at home in 2026 picks up speed.
Integrated services make this possible, keeping patients safely out of hospitals. This helps to reduce hospitalizations and support seniors to age safely in their own homes.
By offering a steady, watchful eye, integrated care teams can address health concerns before they escalate. This preserves a patient’s well-being and a family's emotional resources.
Care Plans That Evolve With You
A person's health needs are not static. The beauty of an integrated continuum is that the care plan adapts just as smoothly. This model ensures the right level of support is always there.
Here’s how a care journey can evolve under one roof:
- Home Health: Following a hospital stay, a patient gets skilled nursing and physical therapy to rebuild strength.
- Palliative Care: As a chronic illness progresses, the focus can shift to managing symptoms, often while other treatments continue. Our article on using telehealth in hospice and palliative care shows how technology helps us do this.
- Hospice Care: If the time comes, the transition to hospice is handled with compassion by a team that has earned the family’s trust.
Integrated care also provides practical solutions for daily living. Guides on finding the best lift chairs for seniors can make a huge difference in comfort and independence.
For over 74 years, Central Coast VNA & Hospice has delivered this connected care to families. We serve Monterey, San Benito, Santa Cruz, and South Santa Clara counties.
Getting Your Network Ready for the Future of Senior Care
For healthcare providers on the Central Coast, the message is clear. By 2026, a massive wave of seniors will be choosing to age at home. This shift puts pressure on our local health systems.
Discharge planners and physicians in Monterey, Hollister, Salinas, and Santa Cruz should evaluate their care networks now. If we wait, we risk serious service gaps. A fragmented approach no longer works for our community.
Central Coast VNA & Hospice is a local partner ready to help. As a nonprofit with over 74 years of local experience, we offer an integrated continuum of care under one trusted roof. Our coordinated model creates seamless transitions and personalized support.
We are ready to partner with providers to help meet the rising need for aging-in-place services. Let's work together to strengthen our community’s ability to support seniors.
To learn how you can partner with a trusted, mission-driven leader, visit us at ccvna.com or call 831-372-6668 to speak with our team.
Frequently Asked Questions About In-Home Senior Care
Figuring out the world of in-home care brings up many questions. As the shift driving more seniors to stay at home in 2026 becomes clearer, getting a handle on your options is the first step. Here are answers to common questions.
How do I know if my loved one is eligible for home health care?
Eligibility for home health care usually depends on a few key things set by Medicare. A patient needs to be under a doctor's care and require skilled services on an intermittent basis. This may include visits from a Registered Nurse or a physical therapist.
The patient must also be considered "homebound," meaning it is a major effort to leave the house. A physician must certify that the care is medically necessary. Our team can work with your loved one's doctor to determine eligibility.
What should I expect from a home-based care team?
A professional home-based care team brings expert medical support to your home. At Central Coast VNA & Hospice, our teams are led by experienced healthcare professionals. Their team-based approach ensures we care for the whole person.
Depending on a patient's needs, their team might include a Registered Nurse, a Physical Therapist, or a Medical Social Worker. This approach addresses physical, emotional, and social needs with skill and heart.
How does home health care coordinate with my primary doctor?
Great coordination with a primary doctor is the foundation of quality home health care. Our clinical team becomes the doctor's eyes and ears in the home. We provide regular, detailed updates on your loved one's progress.
This constant communication loop ensures the care plan is always in sync with the doctor's orders. This partnership helps catch issues early and manage symptoms better. It also reduces the chance of an unnecessary trip back to the hospital.
What is the difference between palliative and hospice care?
This is a very common and important question. Both palliative and hospice care are centered on comfort and quality of life. However, they are designed for different situations.
Palliative care can start at any stage of a serious illness and can be given alongside curative treatments. Hospice care is for individuals with a terminal illness who have decided to stop seeking curative treatments. Central Coast VNA & Hospice offers both, ensuring a smooth transition if needs change.
How do I start the conversation about in-home care with my parent?
Bringing up this topic requires sensitivity. Frame it as a way to support their independence and honor their wish to stay at home. You could say, “Let’s talk about getting a little extra help to make it easier and safer for you to stay here.”
Focus on the benefits, like having a skilled nurse visit or a therapist to build up strength. For more tips, you can read our article on how to get help caring for an aging parent at home. Approaching it as a partnership is key.
At Central Coast VNA & Hospice, we are your local, nonprofit partner. We are dedicated to providing compassionate, integrated care for families across Monterey, San Benito, Santa Cruz, and South Santa Clara counties. Contact us today to learn how our 74+ years of experience can support your loved one’s wish to age safely and with dignity at home. Learn more at https://ccvna.com.
A Guide to Choosing Hospice in Salinas: What Local Families Search for Most
When families begin choosing hospice in Salinas, what local families search for most often comes down to trust and local understanding. They want a provider with deep roots in the community. They also look for clear guidance on Medicare and compassionate support.
This search is about finding a partner who understands the unique needs of communities from Monterey to Santa Cruz. It's about feeling seen and supported every step of the way.
What Salinas Families Truly Prioritize in Hospice Care
Making the decision to start hospice care is incredibly personal. For families in Salinas, certain priorities consistently rise to the top. It is not just about finding a medical service.
It is about finding a genuine community partner during a profound time. This means you need an organization that truly understands the Salinas Valley. When local families search online, their queries tell a story.
Phrases like "Medicare hospice options" and searches for Spanish-language materials reveal practical, real-world concerns. These are not abstract questions. They reflect the immediate challenges families face.
The Importance of a Local, Nonprofit Mission
In a community like ours, a good reputation is earned over decades, not days. Families naturally trust providers with a long-term, unwavering commitment to the area. This is where a nonprofit, mission-driven provider like Central Coast VNA & Hospice stands apart.
With over 74 years of service, our focus has always been on patient care, not profit margins. Being a nonprofit means we reinvest resources back into our care programs and community support. This model, built on compassion, aligns with what local families tell us they need most.
Seamless Support Through a Continuum of Care
Another major priority we hear about is the desire for a smooth care journey. Families are already under enough stress. They should not have to worry about switching agencies as a loved one's health needs change.
That's why having a continuum of care is so important. Finding an organization that offers home health, palliative care, and hospice under one roof provides invaluable stability.
- Home Health: Provides skilled nursing and therapy at home, often after a hospital stay.
- Palliative Care: Focuses on aggressive symptom management and support during a serious illness.
- Hospice Care: Shifts the focus entirely to comfort and quality of life at the end of life.
This integrated approach means a single, trusted team can support a family through every stage. A Registered Nurse from a home health visit might later join the hospice team. This continuity builds a powerful foundation of trust when it's needed most.
The Monterey County 2022 Community Health Needs Assessment revealed that reliable access to healthcare is a top concern for residents, especially when it comes to managing the chronic conditions that affect over 20% of seniors. This reality is what drives the search for local, trusted providers like Central Coast VNA & Hospice, which has been delivering in-home care here since 1951.
To feel confident in your decision, it helps to have a clear picture of the journey. You can learn more by reading this guide on what to expect from hospice care.
Decoding Local Searches: What Families Truly Need
When families in our community search online for hospice, their keywords reveal their deepest needs. Understanding this can help you clarify your own priorities. Santa Cruz families often search for "in-home hospice near me," concerned with comfort and natural surroundings.
Meanwhile, Monterey users explore "quality ratings" and "continuum of care" benefits. Salinas families prioritize "Medicare hospice options" and often seek Spanish-language materials.
| Common Search Term | The Underlying Family Need | How Central Coast VNA & Hospice Responds |
|---|---|---|
| "Hospice care Salinas" | Finding a provider with a strong local presence and reputation. | We've served the Salinas community for over 74 years, building generations of trust. |
| "Medicare hospice coverage Monterey County" | Needing clear, straightforward answers about costs and insurance. | We are 100% Medicare-certified and guide families through every step of the process. |
| "Hospice care en español" | The critical need for culturally sensitive care and bilingual staff. | We offer bilingual team members and culturally inclusive hospice guidance for Latino families. |
| "In-home hospice near me" | The desire for a loved one to remain in the comfort and familiarity of their own home. | The vast majority of our hospice care is provided right where patients live, from Santa Cruz to Hollister. |
| "Hospice for veterans Salinas" | Seeking a provider who understands and honors a veteran's unique needs. | We are a proud partner in the We Honor Veterans program, offering specialized support. |
This table shows that behind every search is a family looking for reassurance and compassionate care. Central Coast VNA & Hospice is dedicated to meeting these specific, local needs.
Your Practical Guide to Evaluating Local Hospice Options
Taking the first step toward choosing hospice care can feel like a big task. Think of this as a clear, practical roadmap for families in Salinas and our neighboring communities. We will move beyond a simple checklist to give you real guidance.
First, let's talk about how hospice is paid for. For most families, the answer is the Medicare Hospice Benefit. This plan, also covered by Medi-Cal and private insurance, typically pays for 100% of the costs.
This means the hospice team's services, medical equipment, and medications are all covered. This lifts a major financial weight off your shoulders.
Gather Essential Medical Information
Before you start calling, pull together some key medical information. Having this ready will make your conversations more productive. It helps ensure you find a team that can meet your loved one’s specific needs.
Your goal is to paint a clear picture of their current health.
- Primary Diagnosis: What is the main illness leading to hospice consideration?
- Key Symptoms: What are the biggest challenges right now, such as pain or shortness of breath?
- Current Medications: Make a quick list of all prescriptions and supplements.
- Physician Information: Jot down the names of their primary doctor and any specialists.
With this information, a potential hospice provider can quickly confirm eligibility. They can also start thinking about a personalized care plan.
Understand the Nonprofit Difference
As you begin your search, you'll see for-profit and nonprofit hospice agencies. This is a critical distinction. As a nonprofit organization serving this community for over 74 years, Central Coast VNA & Hospice has a mission-first focus.
Our priority is always the patient and their family, not shareholders.
A nonprofit structure means all our resources go directly back into patient care, staff training, and community programs. This allows us to provide compassionate care to everyone who needs it in Salinas, Hollister, and across Monterey and San Benito Counties, regardless of their financial situation.
When you choose a mission-driven provider, you can be confident that every decision is guided by your loved one’s comfort.
This decision tree helps visualize the key priorities that Salinas families weigh when choosing a hospice provider.
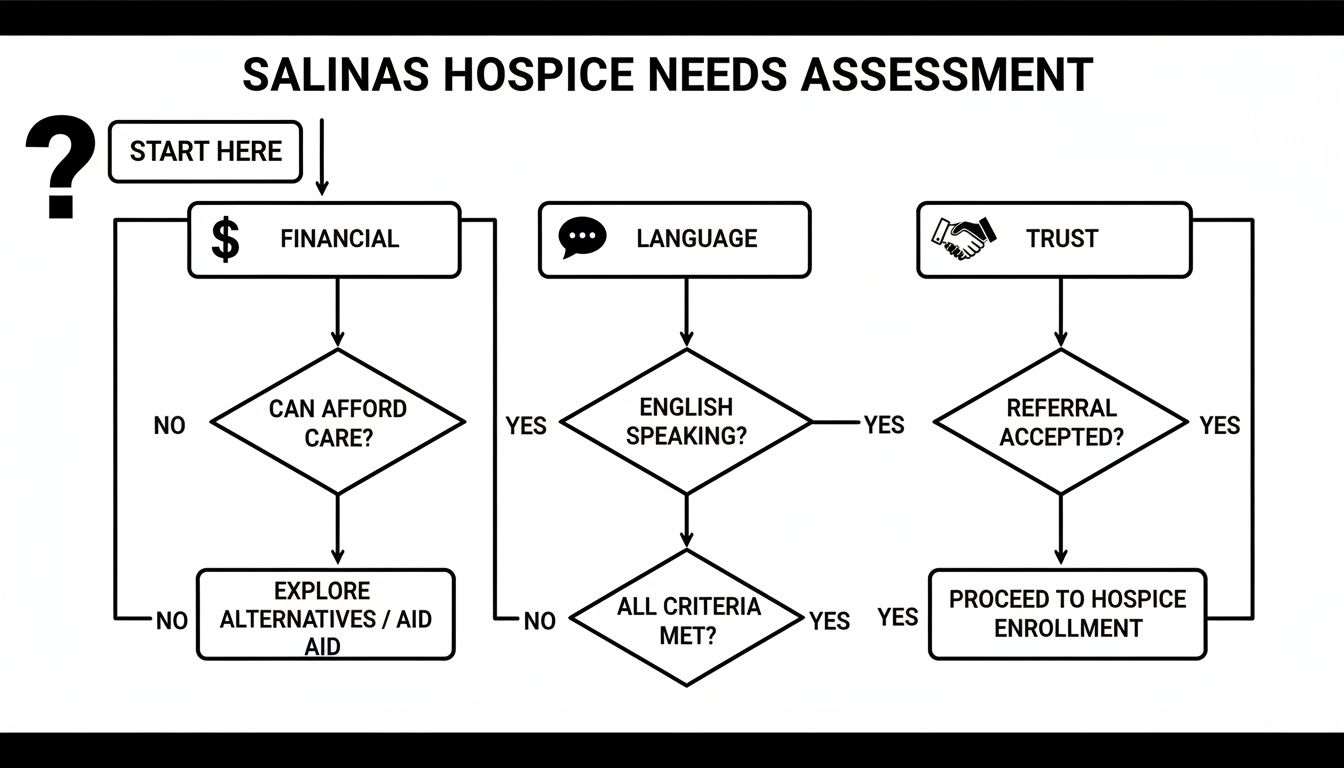
As you can see, these core concerns are all connected. Addressing them is fundamental to making a compassionate choice for your family.
Schedule Consultations and Prepare Questions
The final piece is to schedule informational meetings with providers. These consultations have no obligation. They are your chance to ask questions and get a feel for the organization.
Come ready with questions that go deeper than the basics. What matters most to your family? Is it 24/7 access to a nurse, spiritual support from a Chaplain, or a compassionate Hospice Aide?
Building confidence in your choice often comes down to transparency. You can read our guide on trust, transparency, and testimonials when choosing a hospice to learn more.
Getting to Know a Potential Hospice Provider
Talking with a potential hospice agency is your chance to see if they're the right fit. Once you've narrowed your list of providers in the Salinas area, a thoughtful conversation can tell you what you need to know. This is about more than a list of services.
It’s about finding a team you trust during a sensitive time. Think of this as building a foundation of confidence. Asking the right questions helps you understand the day-to-day reality of their care.
Who Is on the Care Team?
The heart of any hospice agency is its people. This team will become a regular presence in your life. It's essential to understand who they are and how they work together.
Their roles are different, but they should be coordinated to provide complete support.
- Registered Nurse (RN) Visits: How often will the RN visit? Can we ask for more visits if needed?
- Hospice Aide Support: What personal care tasks does the Hospice Aide help with?
- Team Communication: How does the entire team stay on the same page?
- Staff Consistency: Will my loved one see the same familiar faces?
Knowing who to expect can bring incredible comfort. To get a better feel for what a top-notch provider looks like, see our guide on the 7 signs you’ve found the right hospice for your parent.
What Happens After Hours and in an Emergency?
Pain and medical questions don't stick to a 9-to-5 schedule. It's critical to understand how a hospice in Salinas handles after-hours support. Knowing help is a phone call away, day or night, is crucial for peace of mind.
When a symptom flares up late, you need immediate access to expert guidance.
A hospice’s true value often shines in a crisis. Their 24/7 on-call system should be staffed by their own clinical team, not a third-party call center. This ensures the person on the other end of the line understands hospice care.
Ask directly about their emergency protocols. How quickly can a Registered Nurse respond to a late-night call or visit a home in Salinas? This responsiveness is a key marker of a high-quality agency like Central Coast VNA & Hospice.
Do They Have Specialized Experience?
Every patient's journey is unique. If your loved one is a veteran or has a complex condition, find a provider with relevant experience. Specialized training ensures the care team understands the unique challenges involved.
Ask if they have specific programs or staff with credentials in these areas. For example, Central Coast VNA & Hospice is a proud participant in the We Honor Veterans program. This means our team has special training to address the needs of those who have served.
Side-by-Side Hospice Provider Comparison
To make your decision easier, use this checklist. It helps you compare providers on what matters most to families in Salinas.
| Question or Feature | Provider A | Provider B | Central Coast VNA & Hospice |
|---|---|---|---|
| Is 24/7 support staffed by their own nurses? | ☐ Yes ☐ No | ☐ Yes ☐ No | ✅ Yes |
| Do they have a consistent care team? | ☐ Yes ☐ No | ☐ Yes ☐ No | ✅ Yes |
| Are they a We Honor Veterans Partner? | ☐ Yes ☐ No | ☐ Yes ☐ No | ✅ Yes |
| Do they have specialized dementia training? | ☐ Yes ☐ No | ☐ Yes ☐ No | ✅ Yes |
| Is the agency nonprofit? | ☐ Yes ☐ No | ☐ Yes ☐ No | ✅ Yes |
| How long have they served the community? | 74+ years | ||
| What is their nurse response time after hours? | |||
| What is their staff-to-patient ratio? |
Once you've filled this out, the right choice often becomes clearer. The goal is to find a partner who makes you feel heard, respected, and supported.
What Does In-Home Hospice in Monterey County Actually Look Like?
When families think about hospice, they hope their loved one can stay at home. Here in Salinas and across Monterey County, in-home hospice care makes that a reality. It's about transforming the home into a sanctuary of comfort.
It is natural to wonder what daily life will be like. In-home hospice isn't about constant medical intrusion. It is about creating a circle of support with scheduled visits designed to enhance quality of life.

The Team That Comes to Your Door
The Central Coast VNA & Hospice team is a coordinated group of specialists. Each one brings a unique skill set to your home. We schedule visits based on your loved one's specific needs.
Here’s a look at the core team members:
- Registered Nurse (RN): The RN is the clinical leader, managing pain and other symptoms.
- Hospice Aide: Our aides provide essential personal care with dignity, such as bathing and dressing.
- Medical Social Worker: This person is a lifeline for the family, offering emotional support and resources.
- Chaplain: Our chaplains provide non-denominational spiritual support for people of all backgrounds.
If you want to dig deeper into this philosophy, exploring explanations of palliative care services at home can provide a broader perspective.
Answering the Questions That Keep You Up at Night
Bringing a care team into your home is a big step. It’s normal to have questions about managing medications or equipment. These are valid concerns, and a great hospice provider will have clear answers.
With Central Coast VNA & Hospice, you're never alone. Our team gives you training on how to safely manage medications and use equipment. We set everything up to be as simple as possible.
The biggest source of peace for families is knowing that expert help is just a phone call away. Central Coast VNA & Hospice provides 24/7 on-call nursing support. If a symptom worsens at 2 a.m., a Registered Nurse is there to give immediate guidance.
That round-the-clock availability is what quality in-home hospice is all about. This is the bedrock of our hospice at home program.
Understanding Hospice Costs and Coverage in Salinas
When your family is facing a serious illness, you should not have to worry about money. A common question from Salinas families is, "How are we going to pay for this?" The good news is that comprehensive hospice care is often available at no cost.
Let’s clear up the financial side so you can focus on what matters.
The Medicare Hospice Benefit
For most families in Monterey County, the Medicare Hospice Benefit is key. This federal benefit is thorough. It typically covers 100% of all costs related to the terminal illness.
That means no deductibles or copayments for core services. This benefit ensures everyone eligible can access dignified end-of-life care without financial strain.
What’s included?
- Visits from your entire care team—the Registered Nurse, Hospice Aide, Medical Social Worker, and Chaplain.
- All medications needed for pain relief and symptom management.
- Medical equipment like a hospital bed or oxygen, delivered to the home.
- 24/7 on-call access to clinical staff for any urgent needs.
Coverage Options Beyond Medicare
While Medicare is common, it's not the only path. In Salinas, many residents are covered by Medi-Cal or the Central California Alliance for Health. Both provide a hospice benefit that works like Medicare's.
Private insurance plans also almost always offer comprehensive hospice coverage. The team at Central Coast VNA & Hospice can verify your plan’s benefits and handle the paperwork for you.
According to the National Hospice and Palliative Care Organization (NHPCO), over 1.72 million Medicare beneficiaries received hospice services in 2020 (NHPCO, 2021). This highlights how vital this benefit is for families across the country, including right here on the Central Coast.
The Unmatched Value of a Nonprofit Provider
This is where choosing a nonprofit provider like Central Coast VNA & Hospice makes a difference. With over 74 years of history, our focus is on patient care, not profit.
Thanks to generous community donors, we can provide care to every eligible patient, regardless of their financial situation. This mission guarantees that no one in our service area, from Salinas to Santa Cruz County, is turned away because they can't pay.
For a deeper dive into payment options, you can learn more about how to pay for hospice in our detailed guide. We want to give you clear information to put financial worries to rest.
Your Trusted Community Partner in Salinas
When you’re looking for hospice care in Salinas, you are really searching for a partner you can trust. It’s a decision that goes beyond medical charts. It is about finding a team that understands our local community.
That's who we are at Central Coast VNA & Hospice. We have been part of the Monterey County community for over 74 years.

Our nonprofit mission is simple. Every decision we make is guided by your family’s comfort and dignity, not a corporate bottom line. We put resources back into patient care, ensuring anyone who needs support can get it.
A Legacy of Comprehensive Care
We offer a full spectrum of services—from home health and palliative care to hospice. This creates a seamless journey for our families. There’s peace of mind in knowing the same trusted organization can support you as needs change.
Our team of Registered Nurses, Hospice Aides, Chaplains, and Medical Social Workers cares for the whole person. We also have specialized programs, like our partnership with We Honor Veterans. We are dedicated to providing reliable, accessible, and compassionate care rooted right here at home.
Choosing a hospice provider is one of the most significant decisions a family can make. It’s about ensuring your loved one’s final chapter is filled with peace, respect, and the highest quality of life possible. Our long-standing legacy is a promise to deliver just that.
Let’s Start the Conversation
If you’re exploring hospice options, we invite you to have a warm, no-obligation conversation with us. We are here to answer your questions. We want to help you understand how our team can support your family.
If you’re a provider working with families in the Central Coast, partner with us to ensure your patients have access to local, compassionate care. Contact Central Coast VNA & Hospice today at 831-372-6668 or visit us at ccvna.com to learn more. We are here for you.
Frequently Asked Questions (FAQs)
What's the main difference between hospice and palliative care?
Palliative care focuses on relief from the symptoms of a serious illness and can begin at any time. Hospice is a specific type of palliative care for those with a life expectancy of six months or less who are no longer seeking curative treatment.
How do most families pay for hospice care?
The vast majority of hospice care is covered 100% by the Medicare Hospice Benefit. This coverage is also typically provided by Medi-Cal and most private insurance plans.
Can my loved one receive hospice care in a nursing home?
Yes, absolutely. Hospice is a philosophy of care that comes to you, wherever you call home. This includes private residences, assisted living facilities, and skilled nursing homes in Monterey County and surrounding areas.
What professionals are on the hospice team?
A hospice team is interdisciplinary. It includes a Registered Nurse, Hospice Aide, Medical Social Worker, Chaplain, and trained volunteers who all work together to support the patient and family.
How do we know when it is the right time for hospice?
This is a personal decision, often made with family and doctors. It may be time when treatments are no longer effective or their burden outweighs the benefits, and the focus shifts to comfort and quality of life.
Does Central Coast VNA & Hospice serve areas outside of Salinas?
Yes. As a long-standing community provider, we serve families across Monterey County, San Benito County, Santa Cruz County, and South Santa Clara County.
Do you offer support for family members?
Yes. Our support extends to the entire family. Our Medical Social Workers and Chaplains provide emotional and spiritual support, and we offer bereavement services for up to 13 months after a loved one's passing.
New Hospice Audits Are Here: What Families Should Know in 2026
If you've heard about new hospice audits coming in 2026, you might wonder what it means for your family. The simple answer is that Medicare is increasing its oversight. This ensures every family receives high-quality and compassionate care.
This change highlights the importance of choosing a trusted provider for your loved one. It’s more critical than ever to select an agency known for transparency and quality.
Understanding the New Wave of Hospice Audits

Starting in 2025, Medicare introduced the Hospice Special Focus Program. This triggered tougher audits and more oversight for providers across the country. Over half of U.S. hospices have already been audited.
Think of these audits like routine quality checks. They are similar to health inspections for restaurants. The goal is to ensure hospices meet high standards for patient safety and care.
This is happening to protect patients and their families. Inconsistent care from some providers raised concerns about patient well-being. These new rules hold every agency accountable for delivering on their promises.
Why This Matters for Your Family
The new audits are a response to growth in hospice services. With more people using hospice, the government is taking a closer look. This helps prevent improper billing and upholds care standards.
Medicare's changes mean more site visits and claim reviews are coming. This helps verify that providers are fully operational and following the rules. You can find more details in these insights on CMS program integrity efforts.
For families in Monterey County, San Benito County, Santa Cruz County, and South Santa Clara County, this is a call to look beyond glossy brochures. Many providers are being flagged for inconsistent care or staff shortages. Accountability and transparency matter more than ever when choosing a provider.
Choosing a hospice provider is one of the most important decisions a family can make. These new audits empower you to select an agency based on proven quality and a deep commitment to patient care.
The key is finding an organization that has always operated with high standards in mind.
A Quick Guide to the 2026 Hospice Audits
| What Is Changing | Why It's Happening | What It Means for Families |
|---|---|---|
| Increased Audits: Medicare is conducting more frequent and thorough reviews of hospice providers. | Protecting Patients: To address inconsistencies in care and ensure high standards are met across the board. | Greater Assurance: You can have more confidence that your chosen provider is held accountable for quality care. |
| Hospice Special Focus Program: This program targets providers with a history of quality issues for closer monitoring. | Financial Integrity: With rising hospice spending, the goal is to prevent fraud and improper billing. | Empowered Choices: This push for transparency helps you ask better questions and choose a provider with a proven track record. |
| More Site Visits: Expect more unannounced visits to verify providers are fully operational and compliant. | Accountability: The aim is to ensure all hospice agencies deliver the care they promise. | Focus on Quality: Reputable providers will be prepared, while others will be required to improve their services. |
These changes raise the bar for everyone, which benefits you.
As a nonprofit organization with over 74 years of service to the Central Coast community, Central Coast VNA & Hospice embraces this new era. Our mission has always been to provide compassionate, high-quality care. Our clinical oversight and documentation protocols already exceed these standards.
Understanding how hospices are funded is a key part of making an informed choice for your loved one.
Why Medicare Is Strengthening Hospice Oversight
As hospice becomes a more familiar option, Medicare is ensuring every patient receives ethical care. The increased oversight for 2026 is not meant to create hurdles. It is about building a stronger foundation of trust.
Think of it like hiring any professional for your family. You expect a certain standard of quality. Medicare is now making that expectation official for every hospice nationwide.
These new rules protect you and your loved ones. They give you peace of mind when it matters most.
The Difference Between For-Profit and Nonprofit Care
When choosing a hospice, it helps to understand the difference between for-profit and nonprofit providers. This difference often reveals an organization's priorities. This is even more critical with the new audit rules.
- For-Profit Hospices: These agencies are businesses owned by investors. Their main goal is to generate profit. This model can create pressure to cut costs, which might impact staffing or services.
- Nonprofit Hospices: Mission-driven organizations like Central Coast VNA & Hospice operate differently. We are accountable to our community, not shareholders. Any revenue is put back into improving patient care and training our staff.
As a nonprofit, our bottom line is patient well-being. With over 74 years of service, our legacy is built on compassionate care that puts people first.
This mission-first approach is why Central Coast VNA & Hospice is ready for this new era. Our practices have always been based on transparency and clinical excellence. We do it because it’s the right thing to do.
Navigating the Financial Realities of Hospice Care
The new audits are also tightening financial rules for hospice providers. As families look toward 2026, it is wise to be aware of these shifts. They can affect a provider's long-term stability.
For instance, the 2026 Hospice Final Rule includes a payment increase. However, Medicare margins for hospices have been shrinking. You can learn more in this breakdown of the 2026 Hospice Final Rule on alorahealth.com.
This financial pressure means choosing a stable, mission-driven provider is more important than ever. A hospice that is financially sound is better equipped to provide steady support. This commitment to integrity is why Central Coast VNA & Hospice is a reliable partner for families on the Central Coast.
For more information on what Medicare covers, check out our guide on Medicare home care eligibility.
How These Audits Directly Impact Your Family's Care
The new hospice audits for 2026 might sound like government paperwork. However, their impact is deeply personal for families like yours. This is not about bureaucracy—it's about accountability.
Increased oversight leads to a higher standard of care for your loved one. It is a shift from promises on paper to proven, consistent support.
Stricter documentation means every detail of your loved one’s care is tracked. This ensures the plan for managing pain and providing comfort is followed precisely. For families, this brings peace of mind.
From Inconsistent Care to Reliable Support
The real goal here is simple. It is to close the gap between the care a family expects and the care they receive.
Sadly, inconsistent practices and staff shortages from some providers prompted Medicare to act. These audits act as a quality benchmark. They help you identify the most dependable hospice organizations.
This chart shows how increased oversight is designed to create better outcomes for patients and families.
Ultimately, Medicare's audits are a response to quality issues. They are pushing the entire industry toward a more compassionate care environment.
Tangible Benefits of a Compliant Provider
When you partner with a hospice that is ready for these higher standards, you feel the difference. It is the difference between hoping for good care and knowing you will receive it.
Here’s what you can expect:
- Better Communication: Audit-ready agencies have strong communication systems. You’ll get regular updates from the Registered Nurse and other team members.
- More Reliable Symptom Management: With detailed documentation required, there’s less room for error in managing pain. Medication schedules and comfort measures are carefully recorded.
- A Deeper Commitment to Dignity: These audits reinforce what matters most: patient dignity. The focus remains on the patient's physical, emotional, and spiritual well-being.
Families who choose a provider aligned with Medicare’s new standards can trust they’ll receive consistent communication, proper symptom management, and a focus on dignity during one of life’s most sensitive transitions.
At Central Coast VNA & Hospice, our nonprofit, mission-driven approach has always put these values first. With over 74 years of serving our communities, our way of doing things is built on trust. A well-documented hospice care plan is the heart of delivering this reliable support.
Families also often face the task of figuring out how to settle an estate. Choosing a hospice that provides clear support can ease that burden. This allows you to focus on what matters most.
What to Look for in a Hospice Provider Now
With new hospice audits coming in 2026, how families choose a provider is changing. Vague promises are no longer enough. The focus must be on proof of quality, transparency, and compassionate care.
Many industry peers offer vague promises but avoid discussing quality metrics. That leaves families unsure how to judge which providers are truly reliable. Making an informed choice means looking for specific signs of a trustworthy agency.
For families in Monterey, San Benito, Santa Cruz, and South Santa Clara counties, this is your guide. It will help you find a provider you can truly trust.
A Legacy of Trust and Community Roots
In this new landscape, a provider’s history matters more than ever. An agency with deep community roots and decades of service has a proven track record. Central Coast VNA & Hospice's 74+ years of nonprofit care show a long-term commitment to our neighbors.
This history shows stability and a dedication to quality. It was in place long before any new regulations.
The Importance of a Complete Care Team
High-quality hospice care is never a one-person job. It takes the expertise of a full team working together. This team supports not just the patient, but their entire family.
When you evaluate a provider, make sure they offer a complete team, including:
- A Registered Nurse (RN) available 24/7 for urgent needs.
- A dedicated Hospice Aide to help with personal care.
- A Medical Social Worker to help navigate challenges.
- A Chaplain to provide spiritual support.
- Trained Volunteers who can offer companionship.
This complete approach ensures every aspect of your loved one’s well-being is addressed.
Verifiable Quality and Audit Readiness
A transparent provider will not shy away from talking about its quality metrics. Do not hesitate to ask about their patient satisfaction scores. This is critical as the Office of Inspector General (OIG) increases its scrutiny.
For example, recent OIG audits in Texas found significant non-compliance issues leading to overpayments. Similar reviews are planned nationwide. Knowing a provider is prepared for this level of review protects your family.
A provider’s readiness for an audit is a direct reflection of its day-to-day commitment to clinical excellence. A well-run agency operates with meticulous care every single day.
Central Coast VNA & Hospice delivers care with full clinical oversight. Our robust documentation protocols and 24/7 nurse availability ensure we meet these new standards. As a nonprofit home healthcare provider, we have built a 74+ year legacy of trusted and compassionate hospice care.
Your 2026 Hospice Provider Checklist
Use this comparison to evaluate hospice providers. Identify the signs of high-quality care that your family deserves.
| What to Look For | A Compliant Provider (Like CCVNA) | Potential Red Flags |
|---|---|---|
| Years of Service | Decades of community-based, nonprofit care. | Recently established for-profit agency with little local history. |
| Care Team | A full team (RN, Aide, Social Worker, Chaplain, Volunteers) is standard. | Vague descriptions of staff or reliance on only a few roles. |
| 24/7 Support | A Registered Nurse is available by phone and for visits 24/7. | Calls go to an answering service or a non-clinical person after hours. |
| Transparency | Openly shares quality scores and compliance processes. | Avoids answering direct questions about quality or audit readiness. |
| Documentation | Meticulous, patient-centered record-keeping is part of their daily routine. | Rushed intake process or minimal communication about the care plan. |
| Mission & Focus | Mission-driven, focused on patient comfort and family support. | High-pressure sales tactics or focus on enrollment numbers. |
Choosing a hospice is a personal decision. By focusing on these key areas, you can find a partner committed to dignity and peace of mind. For more guidance, read our article on choosing the right hospice for your loved one.
Critical Questions to Ask Any Hospice Agency
Choosing a hospice provider is one of the most important decisions your family will make. With new audits coming in 2026, it is crucial to ask direct questions. These questions should go beyond marketing brochures.
The right questions will reveal an agency's true commitment to quality care. You should feel empowered in these conversations. A trustworthy provider will welcome your questions with clear answers.
Questions About Audit Readiness and Compliance
First, you need to know how prepared an agency is for this new era. An agency's readiness for an audit reflects its everyday commitment to excellence. Vague answers are a big red flag.
Start with these questions:
- How is your agency preparing for the 2026 Medicare audits and the Hospice Special Focus Program? A prepared provider can describe their documentation protocols and staff training.
- Can you share your most recent patient satisfaction scores or quality metrics? Transparent agencies are proud of their work and should share this information.
- What is your staff-to-patient ratio? This number gives you a sense of how much personal attention your loved one will receive.
These questions get to the heart of an agency's operational strength.
Questions About Patient Care and Family Communication
Beyond compliance, you need to understand how the hospice will care for your loved one. Consistent communication and dependable support are the cornerstones of quality hospice care.
A provider’s ability to clearly explain their communication process is a strong indicator of the support your family will receive. Vague answers may suggest a lack of structured family support.
Consider asking these things:
- How do you guarantee a Registered Nurse is available 24/7 for urgent needs? Listen for details. Will you speak directly with a nurse after hours?
- Can you walk me through your process for communicating with families about the care plan? A great provider will have a system for regular updates.
- How does your team handle spiritual and emotional support for the patient and the family? This helps you see if they offer holistic care.
It is also important to ask how they handle documents like healthcare directives and living wills. These are vital in ensuring your loved one's wishes are respected.
At Central Coast VNA & Hospice, our answers are grounded in our 74-year legacy of nonprofit care. We have always operated with full clinical oversight and transparent communication. Our team welcomes these questions because they highlight our high standards.
How Central Coast VNA & Hospice Delivers Peace of Mind
As your local, nonprofit hospice provider for over 74 years, we hold ourselves to the highest standards. We see Medicare’s new audit program as a validation of our compassionate care. Our mission-driven approach means our focus is always on patient comfort and family support.
This is why families in Monterey, Salinas, Hollister, and Santa Cruz have trusted us for generations. We built our legacy on robust clinical oversight and meticulous documentation. This new era of accountability shines a light on the values we've upheld all along.
A Seamless Continuum of Care
Navigating healthcare can feel overwhelming, especially when needs change. That is why we offer a full continuum of care. Our services provide stability and support under one roof.
This integrated approach includes:
- Home Health: Skilled nursing and therapy to help patients recover at home.
- Palliative Care: Specialized support to manage symptoms and improve quality of life.
- Hospice Care: Compassionate end-of-life care focused on dignity and comfort.
This means your loved one can receive care from a team they already know and trust. It minimizes stress and ensures consistency. Our entire team works together to provide a safety net of support.
For families on the Central Coast, choosing a provider with a long history of compliance means choosing peace of mind. Our nonprofit status ensures every decision is guided by what is best for our patients.
Your Trusted Partner in Compassionate Care
The new hospice audits for 2026 are about ensuring every family receives quality care. Central Coast VNA & Hospice has always been ready for this accountability. We welcome any questions you have about our services or our quality metrics.
We invite you to explore why Central Coast VNA is the best choice for hospice care on the Central Coast.
If you’re seeking a hospice provider in Monterey, Santa Cruz, Hollister, or Salinas, ensure they’re prepared for these new regulations. Central Coast VNA & Hospice welcomes questions and offers transparent guidance. Contact us today at 831‑372‑6668 or visit us online at ccvna.com to learn more.
Frequently Asked Questions About Hospice Audits
1. Will these audits interrupt my loved one's care?
No, these audits should not interrupt care. A compliant provider like Central Coast VNA & Hospice handles audits behind the scenes. Our team’s focus remains on providing seamless support for your loved one.
2. What happens if a hospice provider fails an audit?
A provider that fails a Medicare audit can face serious consequences. These may include financial penalties or removal from the Medicare program. This is why choosing a provider with a proven history of compliance is so important.
3. Are all hospice agencies being audited?
Medicare is strengthening its oversight for all providers. However, it tends to focus on those with red flags like unusual billing or patient complaints. Reputable agencies welcome this accountability as it validates the high-quality care they already provide.
4. How can I check a hospice's quality record?
Medicare offers a free tool called Care Compare on its official website. It provides objective data on hospices in your area. You can find family satisfaction survey results and scores on patient care measures.
5. Why should I choose a nonprofit hospice?
As a nonprofit, Central Coast VNA & Hospice is driven by a mission, not profit. We reinvest resources back into patient care, community programs, and staff training. Our 74+ year legacy serving Monterey, San Benito, Santa Cruz, and South Santa Clara Counties shows our commitment to compassionate care.
Navigating hospice care can be overwhelming, but you are not alone. The team at Central Coast VNA & Hospice is here to provide clear answers and support your family. Contact us today to learn more about our services at https://ccvna.com.
How Can I Get Help Caring for My Elderly Parent at Home in Monterey?
Caring for an elderly parent in Monterey can feel overwhelming. Many adult children assume they have only two choices: do everything themselves or move their loved one into a facility.
But there is a better way. Professional, in-home clinical support from a nonprofit like Central Coast VNA & Hospice brings skilled nursing, therapy, and compassionate care right to your parent's home. This approach respects their wish to age in place while keeping them safe.
The Reality of Caring for an Aging Parent in Monterey
If you are juggling your career, family, and your parent’s growing needs, you are not alone. It is a common challenge for families in Monterey County.
Many families believe they must choose between handling it all themselves or placing a parent in a facility. This "either/or" thinking often leads to burnout. It overlooks a crucial third option: professional in-home clinical care.
Understanding the Local Need
Monterey County's population of adults aged 60 and older is growing. Projections show that the number of residents over 75 will continue to increase.

This trend means more of us will become family caregivers. The good news is that most seniors want to stay in their own homes. According to AARP, 75% of adults over 50 share this goal, and it is achievable with the right support.
The goal is not to replace family support. It is to supplement it with professional clinical expertise, which keeps your parent safe and improves their quality of life.
At Central Coast VNA & Hospice, we provide a full continuum of nonprofit in-home care. Our services range from home health to palliative and hospice care. Our interdisciplinary teams include Registered Nurses, therapists, and medical social workers who deliver expert care in the home.
If you live in Monterey County, Salinas, Hollister, or Santa Cruz, we can help. Central Coast VNA & Hospice has been a trusted local provider for over 74 years. We can guide you through your options with compassion.
Decoding the Types of In-Home Medical Support
Navigating healthcare terms can be confusing. Understanding your options is the first step to finding the right help for your parent at home in Monterey.
Let's break down the main types of in-home clinical care. This clarity helps you match your parent's needs with the right professional team.
Home Health Care for Recovery and Rehabilitation
Home Health Care is skilled medical support provided in your parent's home. It helps them recover from an illness, injury, or surgery. A doctor must prescribe this care, which is short-term and goal-oriented.
Think of it as bringing hospital rehabilitation services to your parent's living room. A Home Health team often includes:
- Registered Nurses who manage medications and teach you about the care plan.
- Physical Therapists who work on building strength and improving balance.
- Occupational Therapists who help your parent relearn daily tasks safely.
This service is ideal for a parent returning home after surgery or managing a new health condition.
Palliative Care for Comfort and Quality of Life
Palliative Care is specialized medical support for people with a serious illness. The goal is to provide relief from symptoms and stress. It improves the quality of life for your parent and your family.
A common myth is that palliative care is only for the end of life. This is not true. Your parent can receive it at any stage of an illness, often alongside curative treatments.
Hospice Care for Compassionate End-of-Life Support
Hospice Care is for someone in the final phase of a terminal illness. The focus shifts from curing the disease to providing comfort and dignity.
Hospice supports the whole person by addressing physical, emotional, and spiritual needs. This care is essential in Monterey County, where many seniors face complex health challenges. You can find more insights into our local senior population from the California Department ofAging.
Choosing the right care depends on the primary goal. Is it recovery (Home Health), symptom relief (Palliative), or comfort (Hospice)?
To help you see the differences, here is a simple breakdown.
In-Home Clinical Care Options in Monterey County
| Type of Care | Primary Goal | Who It's For (Example Scenario) | Covered by Medicare? |
|---|---|---|---|
| Home Health | Recovery & Rehabilitation. Help patients regain independence after an illness, surgery, or hospital stay. | An 80-year-old recovering at home after hip surgery who needs physical therapy and nursing to manage their recovery. | Yes |
| Palliative | Comfort & Symptom Management. Improve quality of life for those with a serious illness, at any stage. | A 75-year-old undergoing cancer treatment who needs help managing pain and nausea while still pursuing a cure. | Yes |
| Hospice | Dignity & Peace. Provide compassionate comfort care for individuals in the final months of a terminal illness. | A 92-year-old with end-stage heart failure who has chosen to focus on quality of life at home rather than further treatment. | Yes |
Central Coast VNA & Hospice is a nonprofit provider offering this full continuum of care. This means your parent can transition smoothly between services as their needs change.
How to Assess Your Parent’s Needs for Home Care
Before you can find the right help, you need a clear picture of what your parent needs. This process is about working together to ensure their safety and comfort.
Start by observing their daily routines. Also, have an open and compassionate conversation with them. This creates a partnership where you make decisions together.
Key Areas to Evaluate
To get a complete view, focus on a few critical areas. This helps you pinpoint specific challenges where professional care can help.
Consider these four categories:
- Medical Management: Are they taking medications correctly? Look for missed doses or confusion about their prescriptions.
- Personal Care: Do they need help with bathing, dressing, or grooming? Changes in personal hygiene can be a sign of struggle.
- Mobility and Safety: Have you noticed changes in their balance? Assess their home for safety risks like loose rugs.
- Emotional Well-being: Are they experiencing loneliness or social isolation? Changes in mood can indicate a need for more support.
For more guidance, you can review these 5 warning signs that elderly parents may need home health care. It is also wise to learn about essential tips for preventing elderly falls.
This decision tree shows how different needs point to specific types of in-home care.
As you can see, there is a specialized care path for nearly every situation. This makes it easier to match your parent’s condition to the right clinical support.
Your observations are valuable. They provide the foundation for a personalized care plan that addresses your parent's unique needs.
Once you have a clearer picture, you can contact providers like Central Coast VNA & Hospice. This allows our clinical team to recommend the right level of care for your family.
Navigating Insurance Coverage for Home Services
Many families worry about how to pay for care. The good news is that skilled home health, palliative, and hospice care are often more affordable than you think.
Let's review how coverage typically works in Monterey County. Knowing your options can bring peace of mind.
Understanding Medicare's Role
For most people 65 and older, Medicare is the primary payer for these services. Medicare Part A and/or Part B will often cover 100% of the costs for home health care.
To qualify, a patient must be under a doctor's care and need skilled services. They also must be "homebound."
Being 'homebound' does not mean your parent must be bedridden. It means that leaving home requires a considerable and taxing effort.
Hospice care is another essential service fully covered under Medicare Part A. This benefit is comprehensive and relieves financial burdens during a difficult time.
Other Coverage Options on the Central Coast
Besides Medicare, other plans provide coverage for home-based clinical care. It is important to know all of your options.
Other common payers include:
- Medi-Cal: California's Medicaid program covers home health and hospice for low-income individuals.
- Central California Alliance for Health: This is the local Medi-Cal managed care plan for Monterey, Santa Cruz, and San Benito counties.
- Private Insurance: Many private insurance plans also offer benefits for home-based care.
As a nonprofit organization, Central Coast VNA & Hospice works with all these payers. Our team can help you verify benefits and understand what is covered.
Choosing the Right Home Care Provider in Monterey
You have figured out what kind of help your parent needs. Now, it is time to find the right partner to provide that care.
Asking the right questions will help you find a team you can trust. You are looking for an agency with expertise and local roots in Monterey County.

You need to understand their philosophy and the quality of their clinical team.
Questions About the Clinical Team and Services
The quality of care depends on the people providing it. Look for an agency with a well-rounded, interdisciplinary team.
Here are a few questions to ask:
- What are the qualifications of your clinical staff? Ensure the agency has Registered Nurses, licensed therapists, and other certified professionals.
- How do you create a personalized plan of care? The answer should describe a team effort that includes the patient and family.
- What does after-hours support look like? A quality provider will have a Registered Nurse on call 24/7.
- How does your team coordinate with my parent’s doctor? The agency should work as an extension of your parent’s medical team.
An interdisciplinary team shows a commitment to whole-person care. This approach ensures every aspect of your parent's well-being is addressed.
Questions About the Organization's History and Local Roots
Choosing a provider with deep community ties is a real advantage. An established local agency understands the needs of residents in Monterey County, Salinas, and Hollister.
Consider asking these questions:
- How long have you been serving the Central Coast? Central Coast VNA & Hospice has over 74 years of local service and a proven track record.
- Are you a nonprofit or a for-profit agency? A nonprofit, mission-driven provider reinvests its resources into patient care and community programs.
- What is your service area? Confirm they cover your parent’s town in Monterey, San Benito, Santa Cruz, or South Santa Clara County.
For more insights, check out our guide on finding the best home health agency for seniors.
Taking Your Next Step with Confidence
You do not have to figure out your parent's care alone. Professional support is available right here on the Central Coast.
This process begins with a simple conversation. It's also a good time to consider legal matters; understanding Power of Attorney is crucial for making decisions on their behalf.
If you are ready to explore your options, let’s talk. A consultation with Central Coast VNA & Hospice can provide the clarity your family needs.
Frequently Asked Questions About In-Home Care
Here are answers to some of the most common questions we hear from families.
1. What’s the difference between home care and home health care?
Home care is non-medical help with daily living, like meal prep or companionship. Home health care is skilled medical support prescribed by a doctor, provided by professionals like Registered Nurses and therapists. Central Coast VNA & Hospice provides home health care.
2. How do I know when it’s time for professional help?
If you are starting to worry, it is time to explore options. Signs include trouble with medications, increased falls, or difficulty managing a chronic illness. A professional assessment can provide a clear plan.
3. Can my parent receive palliative care and curative treatment at the same time?
Yes. Palliative care is designed to be an extra layer of support alongside other treatments. It focuses on managing symptoms and improving quality of life at any stage of a serious illness.
4. Does my parent have to be bedridden to qualify for home health?
No. To qualify for Medicare coverage, a patient must be "homebound." This means leaving home requires a significant effort, but they can still attend medical appointments or infrequent outings.
5. How quickly can we start services in Monterey County?
After a doctor's referral, services can start quickly. Central Coast VNA & Hospice can typically schedule an in-home assessment within 24 to 48 hours to create a care plan and begin services.
You are not alone in this journey. The team at Central Coast VNA & Hospice has provided compassionate, nonprofit home health, palliative, and hospice care in our community for over 74 years.
Contact us today to learn how we can support your family.
Top 6 Home Care Trends Central Coast Families Should Watch in 2026
Families across Monterey, San Benito, and Santa Cruz counties are increasingly choosing to support their loved ones at home. The way we approach home-based medical care is changing. New technologies and a better understanding of what families need are driving these shifts.
As we look toward 2026, staying informed about these trends is crucial. It helps you make confident decisions for your family. This article outlines six key home care trends Central Coast families should watch.
Understanding these developments will empower you to plan more effectively. This is true whether you are considering home health nursing, palliative support, or hospice care. Each trend offers new ways to improve quality of life, enhance safety, and ensure compassionate care.
1. More Seniors Want to Stay Home
One of the most significant trends is the strong desire for seniors to age in place. Nearly 90% of adults over 65 say they want to stay in their own homes as they get older. This means more families in Monterey, Salinas, and Hollister are looking for in-home options.
Home health care provides clinical support right where seniors feel most comfortable. This approach avoids the disruption of moving to a facility. It allows them to maintain independence while receiving the medical attention they need from skilled professionals.
How This Benefits Central Coast Families
For families in our community, this trend means more accessible, personalized care. A loved one can receive skilled nursing visits or physical therapy without leaving their familiar surroundings. This stability is incredibly valuable for their well-being.
This preference for aging at home is supported by advancements in smart home technology. These tools create a supportive and responsive living environment for older adults. They work alongside the clinical care provided by organizations like Central Coast VNA & Hospice.
Key Takeaway: The overwhelming preference to age at home is driving demand for high-quality home health services. This shift empowers families to choose care that honors their loved one's wishes for comfort and independence.
How to Prepare
Planning for in-home care is a proactive step.
- Assess the Home: Look for potential safety hazards and consider simple modifications. A home health professional can help with this assessment.
- Discuss Preferences: Talk with your loved one about their wishes for future care. Having this conversation early makes decisions easier later on.
- Explore Local Options: Research local, nonprofit providers who have a long history of serving the community. You can learn more about how to help seniors live at home safely.
2. Local Searches Are Up
More families are actively seeking local home health solutions online. Searches for terms like "home health nurse near me" have jumped 22% in just one year. This shows a growing reliance on local providers to fill care gaps.

This trend applies whether someone needs short-term recovery support after a hospital stay or ongoing nursing visits. Families are looking for trusted, nearby clinical teams. They want professionals who can respond quickly and understand the local area.
How This Benefits Central Coast Families
For families in Salinas, Santa Cruz, or anywhere in between, this means more information is available. It is easier than ever to find and compare local home health agencies. This empowers you to make an informed choice based on your specific needs.
This trend also highlights the importance of choosing a provider with deep local roots. Central Coast VNA & Hospice has served Monterey, San Benito, Santa Cruz, and South Santa Clara counties for over 74 years. Our teams understand the unique needs of our communities.
Key Takeaway: The rise in local online searches shows that families value convenience, trust, and community connection when choosing a home health provider.
How to Prepare
When searching for a local provider, consider these steps.
- Read Reviews: Look at online reviews and testimonials from other local families. This provides insight into the quality of care.
- Verify Services: Ensure the provider offers a full continuum of care. This may include home health, palliative care, and hospice.
- Check for Nonprofit Status: Mission-driven, nonprofit organizations often reinvest in community health and prioritize patient needs over profits.
3. Families Are Planning Sooner
Another key trend is that families are planning for home-based care earlier. In Santa Cruz and across the Central Coast, people are having these important conversations months or even years before a crisis. This proactive approach is becoming more common.
Planning ahead gives you more choices and greater peace of mind. It allows your family to thoughtfully consider options, understand costs, and document your loved one’s wishes. This prevents rushed decisions during a stressful time.
How This Benefits Central Coast Families
When families plan ahead, they feel more in control. It allows for a smoother transition if and when home health services are needed. This forward-thinking approach is a gift to the entire family.
Early planning aligns with the healthcare concept of a community needs assessment. It involves understanding future needs and identifying resources in advance. This ensures you can access the right support when the time comes.
Key Takeaway: Proactive planning for home care reduces stress and ensures that a loved one's wishes are honored. It transforms a potential crisis into a well-managed transition.
How to Prepare
Start the conversation about future care with these steps.
- Document Wishes: Help your loved one complete advance care directives. This ensures their preferences for medical care are known.
- Understand Finances: Research what Medicare and other insurance plans cover for home health, palliative care, and hospice.
- Consult Professionals: Speak with a trusted healthcare provider, like Central Coast VNA & Hospice, to understand the continuum of care. We can help you explore local health care resources for seriously ill family members on the Central Coast.
4. Online Reviews Are Part of the Decision
Before contacting a home health agency, most families check online reviews. Websites like Google and other local directories are now a key part of the decision-making process. Families want to see what others in their community have experienced.

When evaluating providers, look for strong ratings and detailed feedback. Pay attention to comments about clinician-led teams, compassionate care, and reliability. A clear local presence is also important, as it shows a commitment to the community.
How This Benefits Central Coast Families
Online reviews offer transparency and social proof. They help families on the Central Coast identify reputable organizations that consistently deliver high-quality, compassionate care. This digital word-of-mouth is a powerful tool for making an informed choice.
This trend reinforces the importance of a provider's reputation. Central Coast VNA & Hospice has built trust in our community for over seven decades. Our focus on patient-centered care is reflected in the positive feedback we receive from the families we serve.
Key Takeaway: Online reviews have become an essential tool for families. They provide valuable insights into a provider's quality of care, professionalism, and connection to the local community.
How to Prepare
Use online reviews effectively with these tips.
- Look for Themes: Notice recurring comments, both positive and negative. A consistent theme is more telling than a single review.
- Check Multiple Sources: Don't rely on just one website. Look at Google, social media, and other healthcare review sites.
- Consider the Response: See if the provider responds to reviews. A thoughtful response shows they are engaged and value feedback. We also offer resources on how to get real support as a family caregiver on the Central Coast.
5. Local, Skilled Teams Matter
Families are increasingly recognizing the value of local, skilled clinical teams. A provider with deep roots in the community offers significant advantages. Their staff understands the unique challenges and resources of the region.
Central Coast VNA & Hospice has served this region for over 74 years. Our home health team includes Registered Nurses, therapists, and social workers. They understand local needs, from navigating fog delays in Pacific Grove to coordinating rural outreach in San Benito County.
How This Benefits Central Coast Families
A local team means more reliable and responsive care. Clinicians who live in the communities they serve are better equipped to coordinate with local doctors, hospitals, and pharmacies. This ensures seamless, integrated care for your loved one.
This local expertise is crucial for tasks like medication management for the elderly. A local nurse can work directly with a patient's pharmacy in Salinas or Hollister to resolve issues quickly. This level of coordination is harder for large, national corporations to achieve.
Key Takeaway: A local, clinically skilled team provides more than just medical care. They offer community knowledge, established relationships, and a deep commitment to the families they serve.
How to Prepare
When evaluating a provider, ask about their local presence.
- Inquire About Staff: Ask where their clinical staff live and work. A local team is more likely to be familiar with your area.
- Discuss Coordination: Ask how they coordinate with local physicians and hospitals. Strong local relationships are a sign of quality.
- Confirm Service Area: Ensure they have a strong presence in your specific community, whether it's Monterey, Santa Cruz, or San Benito County.
6. Volunteer and Community Programs Add Support
A powerful home care trend involves expanding volunteer and community programs. These programs provide a vital layer of non-clinical support. They complement the work of skilled nurses and therapists.
This approach addresses social needs like loneliness, which is a major health risk. For Central Coast families, this trend means more holistic support. Volunteers can provide companionship, spiritual care, and practical help.
How These Programs Benefit Central Coast Families
In diverse communities from Salinas to Santa Cruz, these programs create meaningful connections. For example, Central Coast VNA & Hospice’s Veteran-to-Veteran volunteer program pairs trained veterans with hospice patients who also served. This fosters a unique and profound bond.
This community-based model allows organizations like Central Coast VNA & Hospice to extend their reach. It helps ensure more patients receive compassionate social and emotional support. This enhances the clinical care provided by our expert teams.
Key Takeaway: Integrating volunteers into home care builds a more resilient and connected care system. It addresses the whole person, improving both health outcomes and quality of life.
How to Prepare
Families can seek out organizations that use community-based models.
- Ask About Support Programs: When choosing a provider, ask about their volunteer services. This may include companionship visits or bereavement support.
- Encourage Connection: If your loved one would benefit from social interaction, inquire about volunteer matching.
- Consider Volunteering: If you have been through a caregiving journey, you might consider becoming a volunteer yourself. Your experience can provide authentic guidance to others.
Your Trusted Partner in Home Care on the Central Coast
The landscape of home-based care is rapidly changing. It is driven by technology, a deeper understanding of patient needs, and a desire for seniors to age with dignity at home. These trends signal a shift toward more integrated and supportive services.
The focus is no longer just on treating illness. It is about supporting the whole person and their family. This includes planning ahead, choosing local providers, and leveraging community support.
Mastering these concepts is invaluable. Understanding these 6 home care trends central coast families should watch in 2026 helps you ask the right questions. It allows you to build a care plan that truly enhances quality of life.
For over 74 years, Central Coast VNA & Hospice has been a pillar of this community. Our local teams of Registered Nurses, therapists, and social workers live and work right here. We serve Monterey, San Benito, Santa Cruz, and South Santa Clara Counties.
We are not just a provider; we are your neighbors. We are committed to delivering the nonprofit, mission-driven care you deserve. As these trends take shape, we are here to support your family's journey.
If you're a homeowner in Monterey, Salinas, Hollister, or Santa Cruz exploring in-home health care for a loved one, we’d love to help. We can help you build a plan that’s compassionate, local, and clinically sound. Let’s start with a free consultation—call 831‑372‑6668 or visit VNA and Hospice.
Frequently Asked Questions (FAQs)
1. What is home health care?
Home health care provides skilled clinical services in a patient's home. This can include services from a Registered Nurse, physical therapist, or occupational therapist. It is typically prescribed by a doctor after a hospitalization or to manage a chronic illness.
2. How is palliative care different from hospice care?
Palliative care focuses on symptom management and quality of life for those with a serious illness. It can be provided at any stage of illness, alongside curative treatments. Hospice care is for individuals with a life-limiting illness who are no longer seeking curative treatment, focusing entirely on comfort.
3. Who pays for home health services?
Medicare, Medi-Cal, and most private insurance plans cover home health care if it is deemed medically necessary by a physician. Our team at Central Coast VNA & Hospice can help you understand your specific coverage.
4. Why should I choose a local, nonprofit provider?
A local, nonprofit provider like Central Coast VNA & Hospice has deep roots in the community. Our mission is focused on patient care, not profits. Our staff are your neighbors, dedicated to serving families in Monterey, San Benito, Santa Cruz, and South Santa Clara counties.
5. How do I start the conversation about home care with my loved one?
Begin by expressing your care and concern for their well-being and safety. Frame it as a way to support their independence and honor their wish to stay at home. Focus on the benefits, like receiving expert care in a comfortable setting.
Is Skilled Nursing Care at Home Better Than a Facility?
When a loved one needs advanced medical support, families often ask: is skilled nursing care at home better than a facility? Many worry about sending someone to a facility after hearing stories of neglect or poor communication. They want to know if it's possible to get that same level of care without leaving home.
While every situation is unique, the answer for most families is yes. Receiving personalized, one-on-one medical care in the comfort of home offers huge advantages. It supports recovery, safety, and emotional well-being without the institutional drawbacks many people fear.
Choosing Between In-Home Care and a Nursing Facility
This tough decision usually comes up after a hospital stay or when a chronic condition gets harder to manage alone. The idea of moving someone you love into a facility can be incredibly stressful. These worries are often fueled by real concerns about neglect, rigid schedules, and a lack of personal attention.
These concerns are valid. But they often stem from a common misunderstanding: that skilled nursing is a place instead of a service.
In reality, skilled nursing is a specific level of medical care from licensed professionals. This includes Registered Nurses (RNs) and physical therapists. This advanced support can be delivered just as effectively—and often more compassionately—right where the patient lives.

It is always a good idea to explore in-home skilled nursing options first. This lets you see what is possible before making a major life change. You can learn more about how in-home support can help avoid a nursing home in our detailed guide.
Quick Comparison At Home vs Facility Care
Deciding between home care and a facility? Here’s a quick overview of what to expect. This table highlights key differences that impact daily life and recovery.
| Factor | Skilled Nursing at Home | Skilled Nursing Facility |
|---|---|---|
| Care Ratio | One-on-one dedicated attention from a clinician during each visit. | One nurse or aide is often responsible for multiple patients at once. |
| Environment | The familiar, comfortable, and safe surroundings of the patient's own home. | An institutional setting with predetermined schedules and less privacy. |
| Family Involvement | Family is central to the care plan and actively participates in recovery. | Visiting hours may be restricted, and family involvement can be limited. |
| Independence | Care is designed to restore independence and adapt to the patient's routine. | Daily life is structured around the facility's schedule for meals and care. |
Seeing this comparison often makes the choice clearer for families. They can prioritize their loved one’s comfort and independence.
Central Coast VNA & Hospice brings this high level of personalized care to homes across Monterey County, San Benito County, Santa Cruz County, and South Santa Clara County. With over 74 years of nonprofit service, our mission is to deliver compassionate, expert care. We help people heal and thrive in the place they feel most comfortable.
Understanding What Skilled Nursing Care Includes
One of the biggest misunderstandings is that "skilled nursing" automatically means moving into a facility. This idea creates unnecessary stress. It can make families feel like their options are limited.
The truth is, skilled nursing care is not a place. It's a high level of medical care that licensed clinicians provide.
These services help people recover after surgery or manage a serious illness. The best part? This expert care can happen right in the patient's home.
This approach is becoming more common, as most older adults already live at home. The statistics might surprise you. Facility living is not the norm.
Only about 1% of people aged 65–74 live in nursing homes. Even for those 85 and older, that number is just 8%. It’s clear that in-home care is a widespread and growing choice.
What Services Are Available At Home
Choosing skilled nursing at home does not mean sacrificing quality. A dedicated team of clinicians brings advanced medical support right to your door. This allows for focused, one-on-one attention that is often hard to find in a busy facility.
Here are some of the core services available at home:
- Wound Care: Professional treatment for surgical wounds or pressure sores to prevent infection and speed up healing.
- IV Therapy: A Registered Nurse can safely manage antibiotics, hydration, or nutrition through an IV line at home.
- Medication Management and Education: We help ensure correct dosages and schedules, while teaching patients and families about their medications.
- Chronic Disease Management: This includes ongoing support for conditions like COPD, heart failure, and diabetes to help prevent hospital trips.
Rehabilitative Therapies in Your Own Home
Skilled nursing also includes therapies that are vital for restoring function. These therapies help people regain strength and confidence in a familiar setting. You can get a complete overview of what is skilled nursing care to learn more about all the services.
Therapeutic services often include:
- Physical Therapy (PT): Helps restore mobility, strength, and balance.
- Occupational Therapy (OT): Focuses on helping patients safely perform daily activities like dressing, bathing, and cooking.
- Speech Therapy (ST): Assists with communication and swallowing difficulties after a stroke or illness.
Therapies like these, especially occupational therapy, play a huge role in rebuilding independence. For a deeper look, understanding the role of occupational therapy in recovery offers great context. At Central Coast VNA & Hospice, our therapists create personalized plans to help each patient achieve their goals at home.
A Detailed Comparison of Care Environments
When you're faced with this decision, it's about more than a simple list of pros and cons. You need to understand the daily reality of receiving care at home versus in a facility. The environment itself plays a massive role in the healing process.
It really boils down to personalization versus standardization. One setting is built around the patient’s life. The other requires the patient to adapt to an institutional schedule.
Patient to Staff Ratio
One of the first things to look at is the level of direct attention your loved one will receive. In a home health setting, every visit from a Registered Nurse or therapist is 100% dedicated to that one person.
This one-on-one focus is a game-changer. It means the clinician has time to do a thorough assessment and answer every question. You never have to compete for attention, which can be a struggle in facilities where one nurse might care for a dozen patients.
In-home care provides a level of individualized attention that is simply not possible in a facility setting. This dedicated time ensures safer medication management, more effective therapy sessions, and a stronger patient-clinician relationship built on trust.
Personalization of Care Plans
When care happens at home, the plan is designed to fit the patient's existing life. Our clinicians work around the patient’s preferred schedule. This supports their sense of independence and dignity.
This flexibility allows for a truly personalized approach to recovery. A physical therapist can design exercises using the patient’s own furniture. This makes the therapy directly relevant to their real life.
The infographic below shows how some key skilled nursing services are adapted for the home.
This visual highlights how core medical services are adapted to provide specialized, one-on-one treatment at home.
To help you see the differences, here’s a quick comparison of the two care environments.
Skilled Nursing Care At Home vs. Facility
| Feature | Skilled Nursing at Home | Skilled Nursing Facility |
|---|---|---|
| Attention | One-on-one care from nurses and therapists. | Shared attention; staff-to-patient ratios can be high. |
| Care Plan | Highly personalized, adapts to the patient’s daily routine and home environment. | Standardized, follows the facility’s schedule and protocols. |
| Family Involvement | Family is an integral part of the care team, receiving training and education. | Involvement is often limited to visiting hours and formal updates. |
| Environment | Comfortable, familiar, and private. | Institutional, less personal, and often a shared living space. |
| Infection Risk | Significantly lower risk of exposure to hospital-acquired infections. | Higher risk due to communal living and frequent contact with other patients. |
| Independence & Dignity | Promotes autonomy by keeping the patient in their own home and in control of their day. | Routines are structured, which can reduce a patient's sense of control. |
| Therapy Realism | Physical and occupational therapy is practiced in the patient's actual living space. | Therapy occurs in a generalized gym setting, separate from daily life. |
This table makes it clear that while both options provide skilled care, the experience is fundamentally different.
The Role of Family Involvement
In-home care actively brings the family into the healing process. Our nurses and therapists teach family members how to support their loved one.
This collaboration is invaluable. It empowers families with the knowledge to spot potential problems early. In contrast, facilities often have restricted visiting hours, leaving families feeling like spectators. For a deeper look, check out our article on the 7 reasons to choose in-home care vs a nursing home.
Environmental Comfort and Safety
You cannot overstate the emotional benefit of being in a familiar place. A person’s home is their sanctuary. Healing in this setting can reduce stress and anxiety.
On top of that, home-based care carries a lower risk of infections. Facilities are communal spaces where illnesses can spread easily. Receiving care at home minimizes exposure and creates a safer environment to get better.
For families in Monterey County, San Benito County, or Santa Cruz County, Central Coast VNA & Hospice offers this personalized care at home. Our team of clinicians is dedicated to your comfort, safety, and independence.
Comparing the Costs and Insurance Coverage
For most families, cost is a huge part of the conversation. It's easy to make assumptions. Some think a facility must be more expensive, while others worry that in-home care will lead to surprise bills.
The reality? For many on the Central Coast, in-home skilled nursing is often the more affordable path. Let's look at the real numbers and see how insurance like Medicare helps.
Breaking Down the Average Costs
When you put the numbers side-by-side, the financial benefit of home health care becomes clear. It’s not just that the monthly cost is lower. The rate at which those costs are rising is also much slower for in-home care.
A recent analysis shows this clearly. Average monthly costs for in-home care are between $6,481 and $6,677. In contrast, a skilled nursing facility costs much more, from $9,555 to $10,965 per month.
But there is a bigger story. While home health costs saw a moderate 3.7% annual increase, facility costs shot up by a staggering 10.9% each year. You can learn more about these healthcare cost trends and what is behind them. This trend means choosing in-home care is a more stable financial road for long-term needs.
Understanding Medicare and Insurance Coverage
Here’s the good news: Medicare often covers skilled nursing care at home. If a patient meets the criteria, Medicare Part A or Part B can cover 100% of the cost. This care must come from a certified agency like Central Coast VNA & Hospice.
Here’s a simple look at how coverage generally works:
- Skilled Nursing at Home: Covered by Medicare as long as a doctor prescribes it and the care is from a Medicare-certified agency. This includes nursing, physical therapy, and speech therapy.
- Skilled Nursing Facility: Medicare covers short-term stays, typically up to 100 days. This is only after a qualifying hospital stay of at least three days and is for rehabilitation, not long-term care.
Navigating these details can feel overwhelming. That is why we created a straightforward guide. We explain how Medicare skilled nursing coverage works to help you make sense of your benefits.
For many, the key takeaway is that Medicare is designed to support recovery and skilled care at home, making it an accessible option for eligible patients in Monterey, San Benito, Santa Cruz, and South Santa Clara counties.
Beyond Medicare, many private insurance plans and Medi-Cal also cover home health services. The team at Central Coast VNA & Hospice has decades of experience helping local families understand their benefits. We believe that financial stress should never stand in the way of receiving compassionate care at home.
How Availability and Access Impact Your Choice
Beyond personal factors, there is a practical challenge that often dictates the choice: availability. Many families are surprised to learn how hard it can be to find a bed in a quality skilled nursing facility.
This is a nationwide trend. The demand for skilled care is rising, but the number of facility options is shrinking. This mismatch creates long waits for families during a stressful time.
The Challenge of Finding a Facility Bed
Recent numbers tell a story of dwindling access. Since 2020, at least 774 nursing homes have closed their doors across the United States. Fewer beds mean fewer options for families.
The problem doesn't stop there. Staffing shortages are forcing facilities to limit who they can accept. Right now, 46% of facilities are limiting new admissions, and 57% have waiting lists. You can read the full report about access to nursing home care to understand the national scope.
When facility waitlists are months long, home health care isn't just a preference—it's the most practical solution. It ensures your loved one gets the skilled medical attention they need without delay.
The Flexibility and Readiness of Home Health
In sharp contrast, home and community-based care is growing. This is driven by both patient preference and the healthcare system’s recognition that healing at home is effective. Home health agencies are built to be responsive and ready to start care quickly.
This flexibility gives families a huge advantage:
- No Waiting for a Bed: A home health nurse can often start visiting within a day or two after a hospital discharge.
- Care That Adapts to You: Services can be scaled up or down as needed.
- Deep Community Roots: Providers like Central Coast VNA & Hospice serve a wide area, including Monterey County, San Benito County, Santa Cruz County, and South Santa Clara County.
This dependable access means high-quality skilled nursing care is available without the uncertainty of a waitlist. When you need immediate, reliable support, choosing a trusted home health provider offers a clear and compassionate path.
How Central Coast VNA Delivers Exceptional In-Home Care
Deciding on skilled nursing at home is a big step. The real difference comes down to the provider you choose. For families here on the Central Coast, that's where we come in.
With over 74 years of nonprofit service, our mission at Central Coast VNA & Hospice is simple. We deliver expert medical care with genuine compassion, right where patients feel most comfortable—their own home. We know you are looking for a partner you can trust, and we build our approach around earning that trust.

A Team-Based Approach to Healing
Great care is about a dedicated team working together. At Central Coast VNA & Hospice, every patient is backed by an interdisciplinary team. This collaborative model ensures nothing falls through the cracks.
Our teams include specialists such as:
- Registered Nurses who handle complex medical tasks like IV therapy and wound care.
- Physical, Occupational, and Speech Therapists who create personalized programs to rebuild strength and independence.
- Medical Social Workers who offer emotional support and connect families to community resources.
This is not just about treating an illness; it's about treating the whole person. Our focus is on healing, comfort, and helping people regain independence at home.
The Continuum of Care Advantage
Health needs can change. We are the only organization on the Central Coast that offers a complete continuum of care. This means we provide a smooth path for patients as their needs change.
Someone receiving home health services can easily transition to our palliative care or hospice care programs. This continuum eliminates the anxiety of finding new providers. Our team already knows the patient, their history, and their values.
You can learn more about our comprehensive skilled care options in Monterey in this detailed article.
Local Roots and Mission-Driven Service
For families in Monterey County, San Benito County, Santa Cruz County, and South Santa Clara County, choosing us means choosing a local provider. As a nonprofit, our focus is 100% on our patients and our community.
Protecting private health information is non-negotiable. We take data privacy very seriously, as detailed in guides on HIPAA-compliant healthcare faxing practices. We are committed to the highest standards of care, safety, and confidentiality.
Contact us today to learn how our dedicated team can support your family.
Frequently Asked Questions About Skilled Nursing
Making healthcare decisions for a loved one can feel overwhelming. Here, we've gathered answers to the questions we hear most often. Our goal is to give you clarity and confidence as you navigate this choice.
How do we get started with skilled nursing care at home?
The process usually begins with a referral from a doctor or hospital discharge planner. You can also contact Central Coast VNA & Hospice directly. Our team will coordinate with your physician to develop a personalized care plan and guide you through every step.
Is skilled nursing at home covered by Medicare?
Yes, it often is. For eligible patients, Medicare Part A and/or Part B typically cover medically necessary skilled nursing care at home. This includes visits from Registered Nurses and therapists. Our staff can help you verify your specific coverage.
What happens if my loved one's condition changes at home?
Our clinical team constantly monitors your loved one's condition and communicates with their doctor. If needs change, we can quickly adjust the care plan or help arrange a transition to a higher level of care. Our full continuum of services includes palliative and hospice care, ensuring a seamless transition if needed.
Can our family be involved in the care at home?
Absolutely. Family involvement is one of the greatest strengths of home care. Our clinicians educate family members on how to best support their loved one’s recovery. This makes you an empowered and essential part of the care team.
Is it really as safe to receive care at home as in a facility?
Yes, and in many ways, it can be even safer. One-on-one attention from a skilled clinician reduces the risk of medication errors. Being at home also lowers the risk of exposure to infections common in institutional settings. We always start with a thorough home safety assessment to minimize any potential risks.
If you're considering alternatives to a nursing facility in Monterey County, Hollister, Salinas, or Santa Cruz, talk to Central Coast VNA & Hospice about your in-home skilled care options. Call us today at 831-372-6668 or visit https://ccvna.com to speak with a nurse about next steps.
Why Home Health Care Is Growing Fast on the Monterey County Coast
More families along the Monterey County coast are choosing home health care. The reasons are woven into our local way of life.
Our community is aging, and more people are managing long-term illnesses. People also want to heal in a comfortable, familiar place. Skilled medical care at home is now a key part of our healthcare system.
The Growing Need for At-Home Care in Monterey County
 home health nurse greets an elderly patient on a sunlit porch by the ocean." />
home health nurse greets an elderly patient on a sunlit porch by the ocean." />Living on the Central Coast is a unique experience. Our area stretches from seaside towns to the rural farmlands of the Salinas Valley. But for older adults, this beautiful landscape presents a challenge: getting to clinics and hospitals.
For someone with a serious health condition, frequent trips for appointments can be exhausting. This difficulty creates a hidden risk for many of our neighbors.
Without strong local home health options, families face delayed care. This can lead to more ER visits and family burnout. This is especially true in winter when fog and rain make travel harder for seniors.
A Local Solution for Local Challenges
This is where home health care makes all the difference. It brings skilled clinicians directly to a patient's doorstep. It's a model built for our community's needs.
Central Coast VNA & Hospice delivers skilled home health care directly to patients' homes. Their clinicians serve people in coastal Monterey, agricultural Salinas, and rural parts of San Benito County. They coordinate care to reduce unnecessary travel and hospital visits.
The following table breaks down the key reasons for the increased demand for in-home medical services.
Top 4 Reasons Home Health Care Is Expanding on the Monterey Coast
| Driving Factor | Impact on Monterey County Residents |
|---|---|
| Aging Population | A growing number of seniors prefer to age in place, requiring accessible medical support at home. |
| Chronic Disease Management | High rates of conditions like heart disease and diabetes need ongoing care to avoid hospital stays. |
| Geographic Barriers | The distance between rural areas and medical centers makes travel difficult, especially for those with mobility issues. |
| Desire for Comfort & Independence | Patients recover better and maintain a higher quality of life when surrounded by the comforts of home. |
These factors combined create a clear case for why home health is a necessity for so many in our area. The demand is also amplified by our community's specific health profile.
In 2020, heart disease and cancer were the top two causes of death in Monterey County. Diabetes is now ranked as the number one prioritized health need, affecting thousands who require consistent care at home to avoid risky hospital trips.
This is exactly why home health care is growing so quickly on the Monterey County coast. It offers a practical and effective way to manage complex health issues without the stress of constant travel.
The expansion of home care is also including newer services like at-home health testing. By bringing care home, we empower our neighbors to heal and age with dignity.
To better understand all the options available, you can explore our guide on local health care resources for seriously ill family members.
An Aging Population and the Rise of Chronic Illness

Our population on the Monterey County coast is getting older. This is a big reason for the growing need for home health care. As more people enter their retirement years, the demand for accessible medical support is rising.
This isn’t just about treating occasional illnesses. It’s a shift toward managing long-term health challenges at home.
Many older adults live with chronic conditions that need consistent, skilled medical attention. This helps them stay healthy and prevent unnecessary hospital stays. These are not issues that can be fixed with a single doctor's visit.
Managing Chronic Conditions at Home
Conditions like heart failure, diabetes, or COPD require regular monitoring. For a senior in Monterey or Salinas, frequent trips to a clinic can be a huge burden. Home health care offers a safer and more effective way forward.
By bringing skilled clinicians into the home, patients get the care they need. They avoid the physical and mental strain of travel. This is critical for managing conditions where even small changes can lead to serious problems.
Central Coast VNA & Hospice’s Registered Nurses are experts in this kind of care. They help patients manage symptoms, stick to medication schedules, and learn to use medical equipment.
This in-home support also helps prevent avoidable hospital visits. For our aging population, simple balance tests can identify fall risks early. This allows for care that keeps people safe at home. Planning for aging at home on the Central Coast has become a critical first step for families.
Local Health Needs Drive Demand
The specific health challenges in our region highlight this need. Monterey County's population skews older, which means a higher prevalence of serious illnesses.
This is the reality on the ground. It's exactly why home health care is growing fast on the Monterey County coast. It’s a direct response to what our aging neighbors need to manage chronic illness with dignity at home.
Navigating Geographic and Transportation Hurdles
Anyone who calls the Central Coast home knows our communities are spread out. From coastal towns to the Salinas Valley, our region has a diverse geography. This landscape also creates real challenges for accessing healthcare.
For older adults with chronic conditions, this is a major barrier to staying healthy. Frequent trips to a doctor's office can be daunting. Travel can become a significant physical and emotional burden.
The Reality of Travel on the Central Coast
Imagine a senior in a rural part of San Benito County needing weekly check-ups. That often means a long drive and dealing with traffic. During winter, coastal fog or heavy rain can make these drives more hazardous.
This reality often leads to delayed care. When getting to a clinic is too difficult, appointments get missed. This can turn manageable health issues into serious problems. It also places immense strain on family members who provide transportation.
For many local families, the constant worry about transportation becomes a major source of stress. The search for a "home health nurse near me" reflects a powerful desire for a more practical solution that brings care directly to them, eliminating the need for difficult travel.
Bringing Skilled Care to Your Doorstep
This is where home health care offers an effective solution. It brings skilled clinicians directly to the patient's doorstep. Central Coast VNA & Hospice, with its deep local roots, is equipped to serve our entire region.
Our teams of Registered Nurses understand the realities of living on the Central Coast. They deliver expert medical care in the patient's home, ensuring consistent support without the burden of travel. This approach reduces family stress and helps avoid unnecessary hospital visits. We are committed to reaching every corner of our community, which you can read about here: our new van is helping connect with families.
Finding Relief From High Hospital Costs
One powerful reason home health care is booming is cost. A hospital stay can be financially overwhelming for local families. This adds serious stress during an already tough time.
This pressure causes many to look for more sustainable solutions. Home health care offers a high-quality, more affordable path. It allows patients to get expert medical attention without the steep costs of a hospital room.
A More Affordable Path to Recovery
Choosing to recover at home can lead to huge savings. Home health services are typically covered by Medicare, Medi-Cal, and other private insurance plans. This coverage makes professional medical support more accessible for our community.
This is especially true in Monterey County, where hospital charges can be much higher than state and national averages. Research shows that from 2018-2020, local hospitals charged some health plans 4.2 to 4.5 times the rates set by Medicare. As a nonprofit, Central Coast VNA & Hospice focuses on providing accessible care that puts your well-being first. You can discover more insights about local healthcare prices on Berkeley.edu.
On top of cost, physical access to facilities can be a real struggle for many.
Challenges like distance, mobility issues, and even weather can lead to missed appointments. In-home care is a more reliable and effective solution. The differences between hospital and home care go beyond just the bill.
Hospital vs. Home Health Care: A Cost and Benefit Snapshot
| Aspect of Care | Hospital Setting | Home Health Care Setting |
|---|---|---|
| Cost | High overhead leads to significant patient expenses. | Lower overhead translates to more affordable care. |
| Comfort & Environment | Unfamiliar, clinical setting with disruptions. | Familiar, comfortable home environment. |
| Personalization | Standardized care protocols for many patients. | One-on-one, individualized care plans. |
| Family Involvement | Restricted visiting hours and limited participation. | Family can be actively involved in care and support. |
| Infection Risk | Higher risk of hospital-acquired infections. | Lower risk due to being in a private residence. |
| Independence | Limited autonomy and reliance on hospital staff. | Promotes independence and patient empowerment. |
Ultimately, home health care provides a setting where patients feel more in control. This can be a powerful factor in the healing process.
Reducing Hospital Visits and Readmissions
Home health care doesn't just lower the cost of a single recovery. It actively helps prevent future hospital stays. By providing skilled nursing in the home, our clinicians can address health issues before they become severe.
By managing symptoms and educating patients on self-care, home health teams empower patients to stay safely at home. This model is proven to be a key factor in keeping people out of the hospital.
At Central Coast VNA & Hospice, our mission is to deliver this care to our neighbors. We are dedicated to reducing hospital readmissions on the Central Coast. We ensure you receive the best possible care in the most comfortable setting: your own home.
The Comfort and Dignity of Healing at Home

There is a personal reason why home health care is growing on the Monterey County coast. It is the simple desire to heal in a place of comfort and to be treated with dignity.
For someone recovering from a serious illness, the emotional value of being home is huge. The simple act of sitting in a favorite chair can bring a sense of peace that hospitals can't replicate. A positive emotional state often leads to better health outcomes.
Empowering Patients in Their Own Space
At Central Coast VNA & Hospice, our approach is built around honoring our patients. We believe that medical care should adapt to the patient’s home. Our clinicians become trusted partners in the patient’s own space.
When one of our Registered Nurses walks through the door, they are stepping into the patient's world. This builds a unique relationship grounded in trust and respect.
This personal connection makes all the difference. Think about these real-world scenarios:
- A physical therapist helps a patient learn to safely navigate their own kitchen again, restoring confidence.
- A home health nurse teaches a family how to manage a complex medication schedule.
- A Hospice Aide provides compassionate personal care that preserves a patient's dignity.
In every situation, the care is delivered on the patient's terms, in their own environment. This partnership is the heart of our nonprofit mission. It ensures every person receives the honorable, effective support they deserve.
Ultimately, choosing home health care is about choosing a path that respects personal wishes. It’s about making sure that healing and comfort go hand-in-hand.
How Central Coast VNA & Hospice Meets Our Community’s Needs
The reasons home health care is growing on the Monterey County coast are clear. Our aging population, geographic hurdles, and high hospital costs all point to a greater need for skilled care at home.
For over 74 years, Central Coast VNA & Hospice has been the local, nonprofit organization built to meet these exact challenges.
Our deep roots on the Central Coast mean we understand the realities our neighbors face. Whether you live in coastal Monterey, the Salinas Valley, or rural San Benito County, our clinicians are part of your community. We deliver skilled medical support to your doorstep, cutting down on stressful travel.
A Continuum of Care for Every Step
We offer a full continuum of care under one trusted roof. This means a patient can move from home health to palliative care and eventually to hospice. They are supported by the same mission-driven team.
This integrated approach brings consistency and compassion when families need it most.
As a nonprofit, our sole focus is on providing honorable, effective, and accessible care. We prioritize patient well-being over profits.
Our teams of Registered Nurses, therapists, and Hospice Aides are deeply invested in the communities they serve. We coordinate with local doctors to create personalized care plans.
This is what makes us a top choice for home health care on the Central Coast. To learn more, you can read about what sets Central Coast VNA & Hospice apart.
If you are caring for a loved one, you don’t have to do this alone. We are here to provide the expert support your family deserves, right where you feel most comfortable.
Frequently Asked Questions About Home Health Care
Here are some common questions we hear from families across Monterey, San Benito, Santa Cruz, and South Santa Clara counties.
What is home health care?
Home health care is skilled medical care provided in a patient's home. It is ordered by a doctor for someone recovering from surgery, illness, or injury. Services can include nursing care, physical therapy, and other professional support.
Who is eligible for home health care?
A patient is usually eligible if they are under a doctor's care and are "homebound." This means it is very difficult for them to leave their home. The care must be medically necessary and require the skills of a professional like a Registered Nurse or therapist.
How is home health care paid for?
Home health care is typically covered by Medicare for eligible individuals. It is also covered by Medi-Cal and most private insurance plans. Our team can help you understand your specific coverage.
How do I start home health services for a loved one?
The first step is to talk to your loved one's doctor. A physician must order home health care. You can also contact us directly, and we can coordinate with the doctor's office to see if services are appropriate.
Why should I choose a local, nonprofit provider?
A local, nonprofit agency like Central Coast VNA & Hospice has deep roots in the community. Our mission is focused on patient care, not profits. We have served the Central Coast for over 74 years and understand the unique needs of families in Monterey County and surrounding areas.
What should I ask a home health provider?
When choosing a provider, ask if they regularly serve your specific city or rural area. You should also ask how quickly their clinicians can respond if conditions worsen. A good provider will understand the challenges of the Central Coast, including travel during bad weather.
If you’re caring for a loved one in Monterey, Salinas, Hollister, or Santa Cruz, Central Coast VNA & Hospice offers trusted home health care designed for the realities of the Central Coast. Learn more at https://ccvna.com or call 831‑372‑6668.
An Advanced Guide to Managing Senior Care Without Losing Your Mind
Managing senior care often feels overwhelming, but you are not alone. The secret to navigating this journey is shifting from a reactive approach to a proactive, integrated one.
This means partnering with a care provider that coordinates all the moving parts for you. An integrated model ensures seamless transitions and expert support at every stage.
The Reality of Senior Care: Moving Beyond the Basics

Managing a loved one’s complex health needs can be daunting. Most advice explains services like home health or hospice but rarely touches on real-world family experiences.
Families are often left to figure out how services work together. What happens when your parent’s condition suddenly changes? Who coordinates between the hospital, specialists, and the in-home support team?
This gap is where families get lost and overwhelmed. It leads to late-night worries and the constant feeling of being one step behind. This reactive cycle creates stress and can lead to poorer outcomes.
The Unspoken Burden on Families
Many families in Monterey County and Santa Cruz County feel they must manage everything alone. Juggling a job, family, and a parent's appointments is a recipe for burnout.
A typical scenario involves setting up physical therapy, managing new medications, and arranging transportation. According to research, 47% of adults expect to become a caregiver for an aging relative, yet most feel unprepared for the logistical and emotional weight.
The real challenge isn’t just the medical care; it’s the coordination of that care. When services are fragmented, the family becomes the default project manager—a role they are rarely equipped to handle.
This constant pressure takes a significant toll. Partnering with a professional home health agency like Central Coast VNA & Hospice can reduce this burden. It can also dramatically lower hospital readmissions, a key indicator of well-managed care. You can explore more in this detailed industry outlook.
Common Caregiver Challenges vs. Integrated Care Solutions
The difference between going it alone and having a dedicated partner is night and day. An integrated care model provides real solutions to common struggles.
| Common Challenge | The Solo Caregiver Experience | The Integrated Care Solution |
|---|---|---|
| Fragmented Communication | Juggling calls between doctors, specialists, and therapists with conflicting information. | A single point of contact—a care manager—coordinates all communication. |
| Crisis-Driven Decisions | Reacting to emergencies like falls or hospitalizations without a clear plan. | Proactive planning and monitoring help anticipate needs and prevent crises. |
| Navigating Transitions | Figuring out the move from hospital to home health or from palliative to hospice care alone. | Seamless, guided transitions are managed by one team, eliminating gaps. |
| Emotional and Physical Burnout | Feeling isolated, overwhelmed, and exhausted by constant care coordination demands. | The family receives expert guidance and support, reducing their burden. |
| Uncertainty About Next Steps | Guessing what services are needed next and struggling to find qualified providers. | The care team assesses changing needs and connects the family with the right services. |
An integrated approach provides a system of support that protects the entire family's well-being.
A Better Approach Through Integrated Care
The solution is an integrated care model. You partner with one organization that offers a full continuum of care.
For over 74 years, Central Coast VNA & Hospice has served the Central Coast of California. As a nonprofit, mission-driven provider, we offer a seamless experience across all levels of care.
- Home Health provides skilled nursing and therapy after a surgery or illness.
- Palliative Care offers expert symptom management alongside curative treatments.
- Hospice Care ensures comfort, dignity, and peace at the end of life.
Our care managers proactively guide families in areas like Salinas and Hollister through every transition. This expert-guided approach empowers families and restores peace of mind. Contact us today to learn how our integrated model can support your family.
Building a Practical and Adaptive Care Plan
A solid care plan is your roadmap to managing senior care. It turns chaos into a structured, manageable process.
Think of it as a living document that evolves with your loved one's needs. The process starts with a thorough look at their current situation. A professional care manager can provide an unbiased view to help create a complete picture.
Honestly Assess Current Needs
Before building a support system, you must know what needs to be supported. Breaking things down into three core areas ensures nothing is overlooked.
- Medical Needs: List all health conditions, medications, and healthcare providers. Note appointment frequency and any specialized services needed, like wound care from a home health Registered Nurse.
- Daily Living Needs: Look at activities of daily living (ADLs). Can they bathe, dress, and manage their home safely on their own? Be specific about where the struggles are.
- Social and Emotional Needs: Isolation can be as damaging as a physical illness. Assess their social interaction, engagement in hobbies, and overall mood for signs of loneliness.
So many families focus purely on the medical side. A truly effective care plan addresses the whole person—body, mind, and spirit. This is a core principle of the compassionate care we provide at Central Coast VNA & Hospice.
Map Your Current Support System
Once you understand the needs, identify who can help. This includes family, friends, and professional services. Be realistic about what each person can do to avoid burnout.
For families in Monterey County and Santa Cruz County, mapping local resources is critical. This might include meal delivery or senior transportation. A Medical Social Worker from CCVNA can provide a list of vetted community resources to fill any gaps.
Start the Conversation About Preferences and Directives
Talking about future healthcare wishes is one of the most important conversations you can have. It is best to have these talks early, before a crisis. The goal is to understand what "quality of life" means to your loved one.
This is also the time to get essential legal documents in order. These documents give legal authority to your loved one's wishes.
Key Legal Documents to Discuss:
- Living Will: Spells out specific medical treatments a person does or does not want.
- Medical Power of Attorney (Healthcare Proxy): Designates a person to make healthcare decisions if they cannot.
- POLST (Physician Orders for Life-Sustaining Treatment): A medical order that specifies treatments for an emergency.
Navigating these documents can feel overwhelming, but they are vital. You can explore our guide on three common advance directives for more details. Having these forms completed removes the burden of guessing from family members.
Navigating the Journey From Home Health to Hospice
The lines between home health, palliative care, and hospice can feel blurry. Understanding these distinct services is a powerful tool for any family.
Knowing what to look for helps you spot changing needs early. This allows for smooth transitions and can prevent stressful hospital trips.
At Central Coast VNA & Hospice, we provide this full continuum of care. Our teams across Monterey, San Benito, Santa Cruz, and South Santa Clara Counties work together to make transitions feel seamless.
The Clear Differences Between Home Health, Palliative, and Hospice
While all three services can be provided at home, they serve different purposes. Knowing which one fits your situation is key.
- Home Health Care: This service is focused on recovery. It helps someone coming home from the hospital regain their strength and manage their condition with skilled care from a Registered Nurse or therapist.
- Palliative Care: This service provides comfort alongside curative treatment. Palliative care helps patients with serious illnesses manage difficult symptoms like pain and anxiety at any stage.
- Hospice Care: This service focuses on comfort when a cure is no longer the goal. When a doctor believes a patient has six months or less to live, hospice shifts the focus to quality of life, dignity, and peace.
These services can flow one into the next. A person might start with home health, add palliative care, and later transition to hospice. When one integrated provider handles it all, the progression feels natural.
Seeing the Continuum of Care in Action
Let's walk through a real-world scenario. Imagine a patient in Salinas with worsening Chronic Obstructive Pulmonary Disease (COPD).
After a hospital stay, they would start with home health care. A nurse would visit to check oxygen levels and a physical therapist would help rebuild strength.
As the COPD progresses, the patient feels more short of breath. This is the perfect time to transition to palliative care at home. A specialized team would focus on managing these symptoms to improve their day-to-day life.
Finally, when the illness reaches its terminal stage, the focus shifts to comfort. The family might decide it’s time for hospice care. The same trusted organization now brings in a team—including a Hospice Aide and Chaplain—to manage pain and provide support.
This decision tree shows how to think through the key steps when building a truly comprehensive care plan.
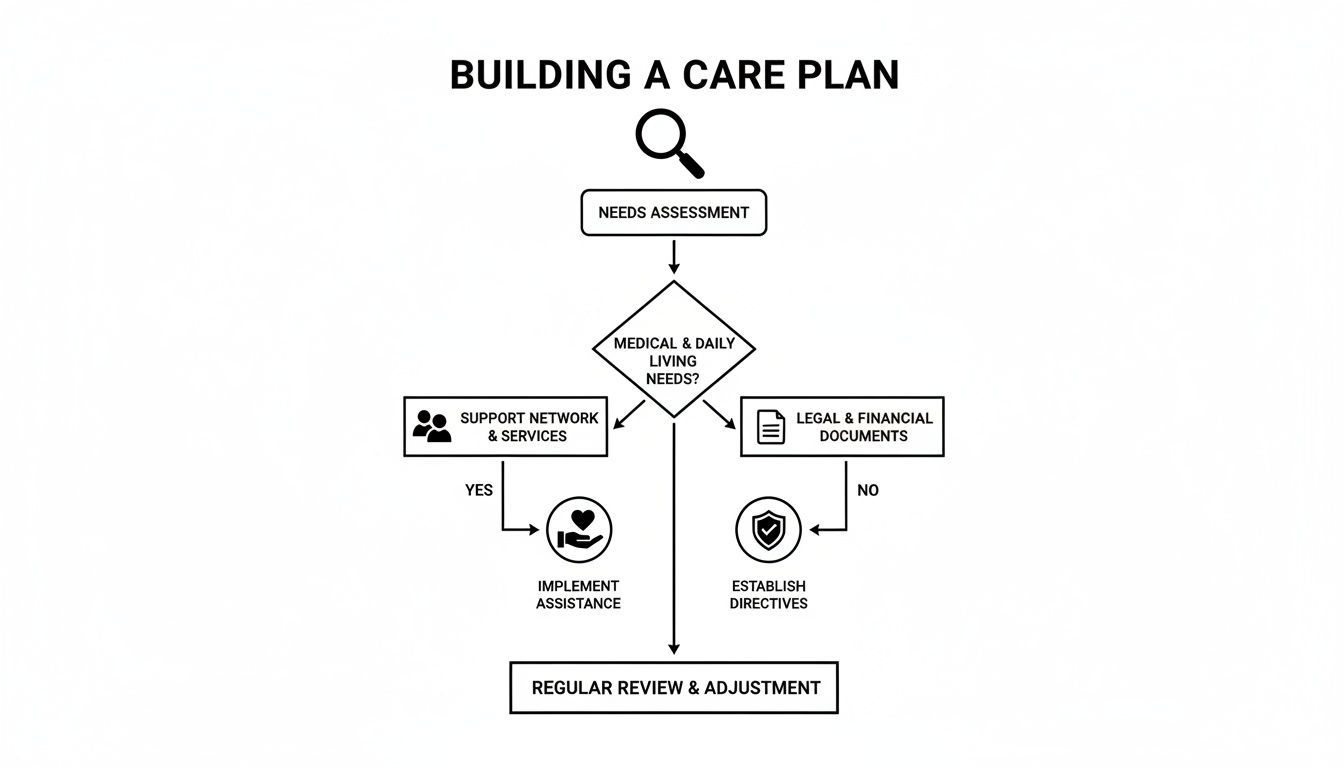
A solid plan always starts with assessing needs. From there, you can build a support network and get essential documents in order.
Advocating for the Right Level of Care
Knowing when to ask for a different kind of support is a game-changer. According to the National Hospice and Palliative Care Organization (NHPCO), over 1.72 million Medicare beneficiaries received hospice services in 2020 (NHPCO, 2021). This data shows how many families rely on this vital support.
Caring for someone with a terminal illness is draining, but hospice can transform that experience. National data also shows that over 90% of hospice patients report their pain is well-controlled.
As the only nonprofit on the Central Coast offering this complete range of services, CCVNA ensures nothing is lost between care levels. Our care managers guide families through each step. To see how these services work together, explore our detailed explanations of home health and hospice care.
Managing Logistics Like a Pro
The daily logistics of senior care are often what burn families out the fastest. Juggling medications, insurance, and communication can feel like a full-time job. The key is to create simple, repeatable systems.
When you establish predictable routines, you free up mental energy. That energy is better spent on being present with your loved one.
Creating a Bulletproof Medication System
Medication management has zero room for error. A straightforward, consistent system is essential for safety and peace of mind.
Gather all prescriptions and supplements in one central spot. Use a pill organizer sorted by day and time to make the routine foolproof. Set daily alarms on a phone as a reliable backup.
Keep a master list of all medications, including dosage, frequency, and prescribing doctor. A Registered Nurse from Central Coast VNA & Hospice can perform a full medication review during a home health visit. You can find more advice in our article, 5 expert tips to prevent medication errors at home.
Navigating Financial and Legal Checkpoints
The financial and legal side of senior care can be a tangled mess. Tackling these issues proactively prevents massive headaches later. For families in Monterey County and surrounding areas, the first step is understanding insurance coverage.
- Understand Coverage: Get familiar with Medicare and Medi-Cal benefits. Ask providers for a clear, written explanation of what's covered to avoid surprise bills.
- Organize Documents: Keep all important documents in one designated binder. This includes insurance cards, Social Security information, and legal papers.
- Establish Legal Authority: Ensure a Power of Attorney for healthcare and finances is in place. These documents allow a trusted person to make decisions if your loved one cannot.
Having Power of Attorney documents completed before a crisis is one of the most important steps you can take. It removes uncertainty and legal red tape during an emotional time.
A Medical Social Worker from Central Coast VNA & Hospice can be an incredible asset. They help families in San Benito County and nearby communities make sense of benefits and connect them with local resources.
Streamlining Family and Provider Communication
Keeping everyone on the same page is crucial for coordinated care and family harmony. A simple communication protocol can change everything.
Here are a few tools that work well for families:
- Shared Digital Calendar: A Google Calendar can track all appointments, medication times, and professional visits. Share access with key family members so everyone is in the know.
- Weekly Email Update: Designate one person to send a short weekly update email. This stops the primary family member from repeating the same information over and over.
- A Central Notebook: This low-tech tool is very effective. Keep a notebook in the home where every professional—from Hospice Aides to nurses—can leave notes.
Finally, home safety cannot be overlooked. An upgrade to advanced wireless interconnected smoke and CO detectors provides another layer of protection. These practical steps create a safer, more manageable care environment.
How to Protect Your Wellbeing and Prevent Burnout

You cannot pour from an empty cup. Protecting your own wellbeing is not selfish; it’s a critical part of providing sustainable, loving care.
Burnout happens when you consistently give more than you have. We are going to cover practical strategies to protect your health. Building resilience starts by accepting that your needs are just as important as your loved one's.
Recognizing the Real Signs of Burnout
Burnout is more than feeling tired. It is a deep state of exhaustion that affects every part of your life. The key is catching the early warning signs before they take hold.
Are you constantly drained, irritable, or anxious? That’s emotional exhaustion. Do you have frequent headaches or trouble sleeping? These are classic physical symptoms.
Another common sign is withdrawal. You might pull back from friends or hobbies you once loved. If this sounds familiar, take a moment to check in with yourself. You can assess your burnout risk with a Burnout Calculator.
Signs of Caregiver Burnout and Practical Counter Strategies
| Warning Sign of Burnout | What It Looks Like | Actionable Step to Take |
|---|---|---|
| Overwhelming Fatigue | Feeling exhausted even after a full night's sleep; lacking energy for basic tasks. | Schedule a 15-minute "do nothing" break each day. Set an alarm and just sit quietly. |
| Increased Irritability | Snapping at family members or the person you're caring for over minor issues. | Practice a 3-minute breathing exercise: inhale for 4 seconds, hold for 4, exhale for 6. |
| Feeling Anxious or Depressed | A persistent sense of dread, sadness, or hopelessness that you can't shake. | Call a trusted friend or family member for a 10-minute chat about something unrelated to caregiving. |
| Social Withdrawal | Declining invitations and avoiding social contact because it feels like too much effort. | Send a simple text to one friend: "Thinking of you." Reconnecting can be a small first step. |
| Changes in Health | Experiencing frequent headaches, stomach issues, or catching colds more often. | Go for a 10-minute walk outside. The fresh air and movement can make a huge difference. |
Recognizing these patterns is the first step. The next is taking small, consistent actions to refill your own cup.
Building Your Personal Support System
No one can do this alone. A strong support network is your most valuable asset. This network should include friends, family, and professional resources.
The most effective support systems don’t just happen—they are intentionally built. Don't wait until you're in a crisis to ask for help.
One of the most practical ways to get support is through respite care. It is a service that provides a temporary break for you to rest. For families in Monterey County and the surrounding areas, this is a necessity, not a bonus. You can learn more about respite care for family caregivers and see how it works.
Setting Boundaries with Love and Firmness
Setting boundaries is vital for preventing burnout. A boundary is a clear line that protects your energy so you can continue to provide care.
- Be clear about your limits. It's okay to be honest about what you can and cannot do. For example, "I can take Mom to her Tuesday appointments, but I need someone else to cover Fridays."
- Learn to say "no" gracefully. A simple, "I wish I could, but I'm not able to take that on right now," is a complete answer.
- Schedule time for yourself. Block out non-negotiable time for yourself in your calendar. Whether it’s a walk or an hour of quiet time, protect it fiercely.
At Central Coast VNA & Hospice, our support extends to the whole family. Our team includes Chaplains and Medical Social Workers who provide emotional and spiritual support to you. We know your wellbeing is the cornerstone of your loved one’s care.
Frequently Asked Questions (FAQs)
What should I do when my parent refuses care?
This is a common experience, often rooted in a fear of losing independence. Start by showing empathy and try to understand their specific fears. Frame care as a tool to help them stay safe and independent at home for as long as possible.
How can our family handle disagreements about care?
Disagreements between siblings can add significant stress. Schedule a dedicated family meeting with a clear agenda and stick to the facts. A neutral third party, like a Medical Social Worker from Central Coast VNA & Hospice, can help facilitate the conversation.
What are our options for paying for services like home health or hospice?
Services like home health nursing and hospice care are often covered by Medicare, Medi-Cal, and private insurance. It is also important to review any long-term care insurance policies or potential Veterans Benefits. Our team can help you understand your coverage options.
When is the right time to consider palliative or hospice care?
Many families wait too long to explore these options. The conversation about palliative care should start when managing symptoms of a serious illness becomes the main challenge. The discussion about hospice care should begin when the focus shifts from finding a cure to maximizing comfort and quality of life. For more details, review these answers to common palliative care questions.
How does a care manager help my family?
A care manager from Central Coast VNA & Hospice acts as your expert guide and single point of contact. They coordinate between doctors and the in-home team, ensuring everyone is on the same page. This proactive approach helps prevent crises and provides peace of mind, so you no longer have to navigate this journey alone.
At Central Coast VNA & Hospice, our nonprofit mission is to provide expert, compassionate guidance. If you are a family in Monterey, Santa Cruz, Salinas, or Hollister feeling overwhelmed, let our team help. Contact us today at 831-372-6668 or visit https://ccvna.com to explore custom care plans that adapt as needs change.










