How to Navigate Costs: How Do Families Afford In-Home Care Long-Term?
When families explore long-term in-home care, one of the first questions is always, "How can we afford this?" The answer is usually a mix of different funding sources. These can include private savings, government programs, and insurance benefits.
Most health insurance plans were not designed to cover ongoing personal assistance. Building a realistic financial roadmap is the most important step you can take. This helps make long-term care sustainable for your loved one.
Understanding the Real Cost of In-Home Care

Many families in Monterey County are surprised by the actual cost of in-home care. It is a compassionate goal to help a loved one age at home. But the financial side can be overwhelming without a plan.
The first step is to look beyond simple hourly rates. The true cost depends on the level of support your loved one needs. This can range from a few visits a week to full-time skilled care from a Registered Nurse.
What Does In-Home Care Typically Include?
In-home care is a wide range of support tailored to an individual's needs. Understanding the different levels helps you estimate costs. It also helps you build a budget that works for your family.
Services generally fall into a few main categories:
- Companion Care: This covers basics like help with errands, preparing meals, and light housekeeping. It also provides important social engagement.
- Personal Care: A Hospice Aide or Home Health Aide can help with activities of daily living (ADLs). This includes things like bathing, dressing, grooming, and mobility.
- Skilled Nursing Care: This is provided by a Registered Nurse (RN) or Licensed Vocational Nurse (LVN). It involves medical tasks like wound care, medication administration, and monitoring vital signs.
For many families, the ideal solution is a blend of these services. A family member might handle daily companionship. A professional aide could visit a few times a week for personal care. For those needing advanced medical support, it is helpful to understand what in-home nursing can offer your loved one in Monterey.
Estimated Weekly In-Home Care Costs at a Glance
This table provides estimated weekly costs for different levels of in-home care. The numbers are based on national averages. This can help families see the potential financial commitment.
| Hours of Care Per Week | Average Weekly Cost (Companion Care) | Average Weekly Cost (Home Health Aide) |
|---|---|---|
| 20 Hours | $660 | $700 |
| 44 Hours (Full-Time) | $1,452 | $1,540 |
| Live-in/24-Hour | Varies Greatly | Varies Greatly |
These figures are a starting point. Actual costs can vary based on your location and the specific services required. They show the importance of planning ahead.
Facing the Financial Reality
It is important to approach the cost of care with open eyes. The national average cost for nonmedical in-home care is projected to be around $33 per hour in 2025. This figure can change depending on the state and the level of care needed.
These numbers can seem high. But in-home care is often more manageable and preferred over a nursing facility. The key is to avoid financial missteps, like assuming Medicare will cover all long-term personal needs.
A common mistake is thinking Medicare or health insurance will cover long-term personal care. But Medicare only provides limited coverage for short-term, skilled nursing needs. It does not cover the ongoing help with daily activities most people need.
As a nonprofit with over 74 years of experience, Central Coast VNA & Hospice helps families in Monterey, San Benito, Santa Cruz, and South Santa Clara counties create realistic care plans. Our team can help you understand your insurance coverage. We connect you with resources to build a sustainable support system for your loved one.
Figuring Out Insurance for In-Home Care
One of the biggest challenges families face is figuring out what insurance will pay for. It is a common mistake to assume a health insurance policy covers everything for long-term care at home. When coverage is not there, families are left scrambling for a new financial plan.
Most insurance, including Medicare, was designed for short-term medical problems. It was not built for the ongoing personal support many seniors need. The key is to have realistic expectations from the start.
The Role of Medicare in Home Care
Medicare is the first place most people look for help. While it is a huge help, its role is very specific and limited. Medicare Part A and Part B may cover certain home health services, but only if a doctor certifies the person is "homebound" and needs skilled care.
These services are not designed for long-term support. Think of it this way: Medicare is there to help you recover from an illness, injury, or surgery.
For a limited time, Medicare typically covers things like:
- Skilled Nursing Care: Visits from a Registered Nurse or Licensed Vocational Nurse on an intermittent basis.
- Physical, Occupational, or Speech Therapy: Services to help a patient regain function and independence.
- Medical Social Services: Help for patients dealing with the social and emotional side of their illness.
Here is the critical point: Medicare does not pay for "custodial care." This means help with daily activities like bathing, dressing, or eating if that is the only care you need.
This gap in coverage surprises many families. For a deeper look at the specific rules, you can learn more about the Medicare home care eligibility criteria.
Medi-Cal as a Vital Lifeline
For Californians who meet specific income and asset limits, Medi-Cal can be a true lifeline. Unlike Medicare, Medi-Cal is designed to cover long-term care services for those who qualify.
Programs like In-Home Supportive Services (IHSS) provide funding for personal care. This makes it possible for loved ones to stay home. The eligibility rules for Medi-Cal are complex, but for those who qualify, it is a key funding source.
Private Insurance and Long-Term Care Policies
Most private health insurance plans follow Medicare's model. They cover short-term skilled care but not ongoing personal assistance.
If your loved one has a Long-Term Care Insurance (LTCI) policy, now is the time to read it carefully. These plans are specifically designed to pay for custodial care. But they have their own rules, like waiting periods and daily benefit limits.
At Central Coast VNA & Hospice, our team helps families in Santa Cruz, San Benito, Monterey, and South Santa Clara counties understand their benefits. As a nonprofit provider with over 74 years of experience, we work with Medicare, Medi-Cal, and private insurance. We help you build a care roadmap that is both realistic and compassionate.
Unlocking Government and Veterans Benefits

When families learn that insurance does not cover most long-term personal help, the financial worry can be great. But there is good news. Several government and veterans programs are designed to fill this exact gap.
For many families in Salinas and South Santa Clara County, these benefits are the missing piece of the puzzle. Navigating them can feel complex. But taking the time to understand them is one of the most important things you can do.
Medi-Cal’s Home and Community-Based Services
One of the most powerful tools for affording long-term care in California is Medi-Cal. It offers Home and Community-Based Services (HCBS) waivers. The goal is simple: give people the support they need to live in their own homes instead of institutions.
HCBS waivers can fund a range of services that Medicare will not, including:
- Personal Assistance: Help with daily activities like bathing, dressing, and preparing meals from a certified Home Health Aide.
- Respite Care: Giving family caregivers a much-needed break to rest and recharge.
- Home Modifications: Minor changes like installing grab bars or ramps to make a home safer.
Eligibility depends on both medical needs and financial status. A nonprofit partner like Central Coast VNA & Hospice can walk you through the process. You can also explore our guide that explains how to pay for hospice care, which touches on various funding sources.
Honoring Service Through Veterans Benefits
For veterans and their surviving spouses, the Department of Veterans Affairs (VA) offers benefits that can make a huge difference. These are earned benefits meant to honor their service. Too often, families do not know these resources exist.
The most important program for in-home care is VA Aid and Attendance. This is a monthly, tax-free payment added to a VA pension. It is for veterans who need help with daily activities.
The VA Aid and Attendance benefit provides a large monthly payment to qualifying wartime veterans and their surviving spouses. These funds help cover the costs of in-home care, assisted living, or nursing home services.
To qualify, a veteran must meet service, income, and asset requirements. A doctor must also certify their need for daily assistance. The funds can be used to hire professional support from organizations like ours.
These programs are the foundation of long-term care funding for millions. In fact, according to KFF, Medicaid paid for 59% of all long-term services and supports in the U.S. in 2021. Meanwhile, VA benefits help over 1.5 million veterans fund their care. For federal employees, understanding programs like the Federal Long Term Care Insurance Program is also a critical piece of the planning puzzle.
As a nonprofit with deep roots in the Central Coast community, we help families in Monterey, San Benito, and Santa Cruz counties access every available resource. Our care team can guide you through these options. We help you honor your loved one with the compassionate care they deserve.
Using Private Pay and Long-Term Care Insurance
When you find that public benefits will not cover everything, the next step is looking at private funding. This is a common part of building a care plan. Using your own resources gives you the most control over your loved one’s care.
The key is to use these resources smartly to avoid a financial crisis later. You want to make informed choices that help your savings last. This ensures your loved one gets the compassionate care they need.
The Role of Long-Term Care Insurance
Long-Term Care Insurance (LTCI) is a policy designed to pay for services that regular health insurance does not cover. This usually means help with bathing, dressing, or preparing meals. If your family has an LTCI policy, it can be a powerful tool for affording in-home care.
But these policies have important details you must understand.
- Elimination Period: This is a waiting period, like a deductible. You will have to pay for care out-of-pocket during this time before the policy starts.
- Daily or Monthly Benefit Limit: The policy will only pay up to a set amount each day or month. It is critical to know this number when creating a budget.
- Covered Services: Always check the policy to see exactly what types of care it covers. Most modern policies are flexible.
To get a clear picture of how these policies work, it helps to read a detailed resource like this one on Long Term Care Insurance Explained. It can help you make sense of all the details.
Leveraging Personal Savings and Assets
For many families, personal savings and retirement accounts are the main source of funding for long-term care. This approach, called "private pay," is the most direct way to hire help.
Families typically use a mix of sources:
- Checking and savings accounts
- Retirement funds like a 401(k) or IRA
- Pensions or annuity payments
- Stocks, bonds, and other investments
One of the biggest mistakes we see is waiting until a crisis to figure out the financial picture. Planning ahead gives you the chance to structure your assets. This helps them last as long as possible.
The first step is always to create a realistic budget. For a detailed breakdown of how to approach this, check out our guide on how to fund home health care costs.
Funding Sources for Long-Term In-Home Care
Navigating the different ways to pay for care can feel overwhelming. Here is a quick comparison of the most common funding sources. It shows what they are best for and key things to keep in mind.
| Funding Source | Best For | Key Consideration |
|---|---|---|
| Medicare/Medi-Cal | Short-term, skilled nursing care after a hospital stay (Medicare); low-income individuals (Medi-Cal). | Strict eligibility rules and limited coverage for non-medical, long-term custodial care. |
| Long-Term Care Insurance | Families who planned ahead with a policy to cover custodial and skilled care needs. | Be aware of elimination periods, benefit caps, and specific covered services. |
| Personal Savings/Assets | Maximum flexibility and immediate access to funds for any type of care. | Can deplete savings quickly without a solid budget and long-term financial plan. |
| Reverse Mortgage | Homeowners 62+ who need to access home equity without selling their home. | The loan must be repaid when the homeowner moves out or passes away, impacting inheritance. |
| VA Benefits | Eligible veterans and their spouses who need assistance with daily living activities. | The application process can be lengthy and requires specific service-related criteria. |
Each of these options has its place. Many families use a combination of two or more to create a sustainable plan.
Other Private Funding Strategies
What happens when savings are not enough? Some families explore other financial tools.
One option is a reverse mortgage. This lets homeowners aged 62 and older turn home equity into cash. They do not have to sell their home. The loan is paid back when the homeowner sells the house or no longer lives there.
Another route is a life insurance conversion. This involves selling a life insurance policy for its current cash value. These are complex financial moves, so it is essential to talk with a financial advisor first.
Creating a Sustainable Long-Term Care Plan
Answering "how do families afford in-home care long-term?" requires a plan that is financially and emotionally sustainable. A good care plan is a roadmap that blends professional support with family and community resources.
This approach helps manage costs and prevent caregiver burnout. It ensures your loved one gets consistent, compassionate support. It is about creating a strong network, not relying on a single person or funding source.
The process below shows how families often layer different financial tools. They start with savings before using insurance or home equity.
This layered strategy helps create a stable financial base for care as needs change.
Building a Blended Care Team
A sustainable plan combines different roles to meet your loved one’s needs. This is what a blended care team looks like.
Imagine a family member helps with companionship and meals. This personal touch reduces the need for paid help for these tasks.
Then, you can bring in professional support for specific needs:
- A Hospice Aide or Home Health Aide can visit a few times a week to help with bathing, dressing, and mobility.
- A Registered Nurse can manage medications, provide wound care, and oversee the medical side of the plan.
- Community volunteers can offer companionship, giving family caregivers a much-needed break.
This approach makes professional care more affordable. Our guide on in-home support to avoid a nursing home offers more tips on finding this balance.
The Value of a Nonprofit Partner
A local, nonprofit provider like Central Coast VNA & Hospice can make a world of difference. With over 74 years of experience, we help families build a comprehensive plan.
Our team serves Monterey, San Benito, Santa Cruz, and South Santa Clara counties. We help you align your financial reality with your loved one’s care needs. We work with Medicare, Medi-Cal, and private insurance to maximize every benefit.
A key part of sustainability is having one point of contact that understands the entire continuum of care. As needs change, a nonprofit partner can seamlessly transition support from home health to palliative care, and eventually to hospice care. This avoids the stress of starting over with a new organization.
Planning for the Long Haul
A care plan is a living document. You need to revisit it as your loved one's health and financial situation changes.
Regular family meetings are essential. These check-ins allow everyone to discuss what is working and what is not. This proactive communication helps share the emotional and logistical weight of caregiving.
By blending formal and informal support, you create a resilient and affordable system. You ensure your loved one gets high-quality care at home. They are supported by a network of family, community, and trusted professionals.
FAQs: Answering Your Questions About Affording In-Home Care
Here are some of the most common questions families ask about paying for long-term care.
What happens when Medicare or other insurance runs out?
This is a common fear, but it doesn't mean you are out of options. When short-term benefits end, other funding sources are designed to take over. Families often turn to a mix of Long-Term Care Insurance, Medi-Cal for those who qualify, Veterans benefits, or private savings. The key is to create a backup plan before the initial coverage runs out to avoid gaps in care.
How can we start a conversation about money with our parents?
This can be a sensitive topic. Frame the conversation around their wishes, not just their finances. Say something like, “Mom, to honor your wish to stay at home, it would help if we could plan the finances together.” Using "we" and "us" makes it a team effort. Bringing in a neutral expert, like a care coordinator from Central Coast VNA & Hospice, can also make the conversation easier.
What is the very first step we should take?
The most important first step is to get organized. Create a clear picture of your loved one’s needs and financial resources. Gather their health information, a list of daily tasks they need help with, and a basic financial summary including income, savings, and all insurance policies. Having this information in one place empowers you to build a realistic plan.
Is full-time, 24/7 in-home care affordable?
For most families, paying for 24/7 professional care out-of-pocket is not sustainable. A more affordable approach is to create a 24/7 support system. This often involves a creative blend of family members covering nights and weekends, with a professional Home Health Aide providing support during weekday work hours. This blended model makes continuous care much more achievable.
How do we know which government programs we qualify for?
Navigating eligibility for programs like Medi-Cal and VA benefits can be complex. Each has specific income, asset, and medical need requirements. The best approach is to connect with a knowledgeable resource. A local nonprofit agency like Central Coast VNA & Hospice has care teams that can help you understand the criteria, gather the necessary documents, and guide you through the application process for services in Monterey County, San Benito County, and our other service areas.
Figuring out how to pay for long-term care takes compassion, creativity, and a trusted guide. For over 74 years, Central Coast VNA & Hospice has been that guide for families on the Central Coast. If you are in Monterey, San Benito, Santa Cruz, or South Santa Clara County and need help, our team is here.
Top 4 Misconceptions About Hospice—Debunked for 2026
For many families on California's Central Coast, the word "hospice" can bring up feelings of fear. It is often associated with loss and the end of hope.
However, the reality of modern hospice care is vastly different. It is about maximizing the quality of life and providing compassionate support. As we look toward 2026, it is important to understand what hospice truly is.
Central Coast VNA & Hospice has served Monterey County, San Benito County, Santa Cruz County, and South Santa Clara County for over 74 years. We have seen how outdated beliefs can prevent families from accessing comfort and dignity. Misinformation can lead to delayed care and unnecessary suffering.
This article addresses the top 4 misconceptions about hospice with clear facts for 2026. We will debunk common myths to help you see hospice as care focused on living fully. Our goal is to empower you with knowledge to make informed decisions.
1. Myth: Hospice Means Giving Up
One of the most damaging views is that choosing hospice means surrendering. Many families believe enrolling a loved one means giving up hope. This could not be further from the truth.
Hospice care is a shift in focus, not an end to it. It moves away from aggressive treatments toward a philosophy of living comfortably. It is an active choice to prioritize dignity and meaningful moments.
The Reality: Hospice is About Living Well
Hospice is about living well, not giving up. Patients can receive hospice care for months. They have access to pain relief, emotional support, and personalized care at home.
At Central Coast VNA & Hospice, our focus is on comfort, dignity, and patient goals—not surrender. Our interdisciplinary team creates a care plan that honors what matters most. This is about redefining hope to focus on connection and peace.
Hospice is not the absence of hope. It is the practice of hoping for a peaceful passing, meaningful time with family, and a life free from pain.
What This Looks Like in Our Community
- A patient in Salinas with end-stage heart failure receives hospice care at home. A CCVNA Registered Nurse manages her pain. This allows her to spend afternoons gardening, an activity she loves.
- A Monterey County family was hesitant about hospice for their father. After enrolling, a Hospice Aide provided gentle personal care. A volunteer read to him, bringing moments of peace they thought were gone forever.
Ultimately, hospice empowers patients to live their final chapter on their own terms. To understand how our team provides this support, you can learn more about our hospice care services.
2. Myth: Hospice is Only for the Final Days
Many assume hospice is a last resort for the final days of life. This misconception can prevent people from receiving support when they need it most.
The fact is, hospice is designed to provide care for six months or longer, if the illness continues its expected course. Choosing it earlier means more time for families to connect meaningfully.
The Reality: Early Hospice Improves Quality of Life
Studies show that early hospice care results in better symptom control. For some patients, it may even lead to a longer life. The goal is to maximize quality of life for as long as possible.
When a patient enrolls sooner, our team has more time to manage symptoms. We can provide emotional and spiritual support to the entire family. This proactive approach adds life to days, not just days to life.
Hospice eligibility is based on a prognosis of six months or less, but the focus is always on the quality of each day, not counting them.
What This Looks Like in Our Community
- A man in Aptos with advanced COPD enrolls in hospice. Our team manages his breathing, allowing him to enjoy visits from his grandchildren without stressful hospital trips.
- A woman in Hollister with late-stage cancer begins hospice sooner. This gives her months of quality time with her family, free from the harsh side effects of curative treatments.
To see if you or a loved one might be eligible, you can learn more about our hospice eligibility requirements.
3. Myth: Hospice Means Leaving My Doctor

A common fear is that starting hospice means cutting ties with a trusted primary physician. This is not true. Patients can continue seeing their doctor while receiving hospice services.
Hospice care is designed to be a collaborative effort. Your doctor remains an important part of the care team.
The Reality: Hospice Care is Coordinated with Your Physician
At Central Coast VNA & Hospice, care is coordinated with your existing providers. Our team works alongside them to ensure a seamless experience. We value the relationship you have with your doctor.
We also provide a full interdisciplinary team. This includes a Registered Nurse, social workers, chaplains, Hospice Aides, and volunteers. This team adds an extra layer of support without replacing your primary doctor.
Hospice does not eliminate medical care; it re-centers it on the patient’s well-being. The question changes from "Can this cure me?" to "Will this improve my comfort today?"
What This Looks Like in Our Community
- A patient in Santa Cruz County continues to see her long-time family doctor for consultations. Our CCVNA hospice team communicates with the doctor to align the care plan.
- A man in San Benito County has a complex condition. His primary physician and our hospice medical director collaborate on his pain management plan.
Our approach ensures you get comprehensive, coordinated support. To learn more, you can learn more about our approach to hospice pain management.
4. Myth: Hospice is Only for Cancer Patients or Happens in a Facility

Two outdated beliefs often merge into one. People think hospice is only for cancer patients and that it takes place in a special building. Both of these ideas are incorrect.
In reality, most hospice care is delivered right at home. Hospice also supports people with many conditions, not just cancer.
The Reality: Hospice is for Many Illnesses, Wherever You Call Home
Hospice supports people with heart failure, dementia, COPD, ALS, and more. If someone is facing a life-limiting illness, hospice may be the right choice regardless of diagnosis.
Central Coast VNA & Hospice brings expert care to where patients feel most comfortable. This includes private homes, assisted living communities, and skilled nursing facilities. We serve patients across the Central Coast.
Hospice eligibility is based on prognosis, not diagnosis. It's about when a person needs comfort care, not just what illness they have.
What This Looks Like in Our Community
- An 85-year-old Hollister resident with advanced dementia receives hospice care at home. A CCVNA Hospice Aide helps with personal care to maintain his dignity.
- A 62-year-old in Santa Cruz with end-stage COPD lives in an assisted living facility. Our hospice team coordinates with facility staff to manage his breathing difficulties.
Ultimately, understanding the true scope of hospice empowers families to seek support. To learn more, you can learn more about our in-home hospice care.
Bringing Peace of Mind with Compassionate Hospice Care
Navigating end-of-life decisions is a profound challenge. By addressing the top 4 misconceptions about hospice, we can replace fear with clarity. The truth is that hospice is about choosing to live with dignity and comfort.
The most critical takeaway is that hospice is about living well. It reframes the journey from one of medical crisis to one of meaningful connection. This earlier access to support allows for better symptom management and more cherished time together.
Taking the Next Step with Confidence
Moving forward, the best action you can take is to start conversations early. Discussing wishes before a crisis occurs is invaluable. To bring peace of mind, it's essential to plan for future medical care with documents like healthcare directives.
For over 74 years, Central Coast VNA & Hospice has been the region's trusted nonprofit provider. We are deeply rooted in the communities of Monterey, San Benito, Santa Cruz, and South Santa Clara counties. Our compassionate teams are dedicated to honoring your wishes.
Confused about what hospice really is? Central Coast VNA & Hospice offers clear, compassionate guidance for families throughout Monterey, Santa Cruz, Salinas, Hollister, and nearby areas. Contact us to learn how hospice can bring peace—not fear—in 2026.
Ready to learn more about how hospice care can support your family? Visit us at VNA and Hospice to start the conversation today.
Frequently Asked Questions (FAQs)
1. How long can a person receive hospice care?
A patient is eligible for hospice with a prognosis of six months or less if the illness runs its normal course. However, care can continue for much longer than six months as long as a physician recertifies that the patient remains terminally ill.
2. Is hospice care covered by insurance?
Yes, hospice is covered by Medicare, Medicaid, and most private insurance plans. The Medicare Hospice Benefit is an all-inclusive package covering services, medications, and equipment related to the terminal illness, often with no out-of-pocket costs for the patient.
3. Where is hospice care provided?
The vast majority of hospice care is provided in the place the patient calls home. This can be a private residence, an assisted living facility, or a skilled nursing facility. Central Coast VNA & Hospice brings expert care directly to patients throughout Monterey, San Benito, Santa Cruz, and South Santa Clara counties.
4. What services does a hospice team provide?
A hospice team is interdisciplinary and includes a Registered Nurse, Hospice Aide, social worker, chaplain, and volunteers. They provide expert pain and symptom management, personal care assistance, emotional and spiritual support for the patient and family, and bereavement counseling.
5. Can I still see my own doctor if I am on hospice?
Absolutely. Hospice care is provided in collaboration with your primary physician. The Central Coast VNA & Hospice team will coordinate with your doctor to ensure your care plan aligns with your goals and needs.
5 Common Hospice Myths—and the Truth About Hospice Care
Making decisions about care for a serious illness is one of the hardest journeys a family can face. In the Central Coast communities of Monterey, San Benito, Santa Cruz, and South Santa Clara counties, families often struggle with difficult questions. Misconceptions about hospice care can add to the confusion and delay much-needed support.
Many people believe hospice is about giving up, is only for the final days, or means ending all medical treatment. These myths can stop patients from getting compassionate care that improves their quality of life. According to the National Hospice and Palliative Care Organization (NHPCO), only 49.1% of Medicare beneficiaries who died in 2022 received hospice, showing this gap is still a problem nationwide.
At Central Coast VNA & Hospice, our nonprofit organization has served our local communities for over 74 years with clear, compassionate guidance. We believe choosing hospice is not about giving up. It is about choosing to live the rest of your life with dignity, comfort, and support. This article will explain 5 common hospice myths—and the truth, so your family can make informed decisions.
1. Myth: Hospice Means Giving Up Hope
Truth: Hospice Focuses on Comfort and Quality of Life
One of the biggest hospice myths is that it means a person is giving up on life. Families often put off talking about hospice because they see it as surrender. This misunderstanding prevents patients from receiving support that could improve their final months.

The truth is, hospice is not about dying; it is about living as fully and comfortably as possible. Hospice care shifts the focus from curing an illness to managing its symptoms. This allows patients to focus on comfort, dignity, and meaningful time with loved ones.
Redefining Hope in Care
When a cure is no longer an option, hope changes, but it doesn't disappear. Hospice helps patients and families find new things to hope for.
- Hope for comfort: Managing pain and other symptoms to feel at ease.
- Hope for connection: Spending quality time with loved ones.
- Hope for peace: Getting support from Chaplains and Social Workers.
- Hope for dignity: Making personal choices about care at home.
This approach honors the whole person, not just their illness. It is a choice to embrace support, not a passive acceptance of death. A patient can always choose to leave hospice care if their condition improves or if they want to try a new curative treatment.
Central Coast VNA & Hospice helps families in Monterey County and surrounding areas redefine hope. Our local team provides care that supports the patient and their loved ones, focusing on what matters most in the final chapter of life.
2. Myth: Hospice Is Only for the Last Few Days of Life
Truth: Hospice Is Available for Six Months or More
A common mistake is thinking hospice is only for the last few hours or days of life. This belief causes families to wait too long for support. They miss out on months of valuable care that could improve comfort and reduce stress.

The truth is, hospice care can provide support for weeks or even months. A patient is eligible for hospice if a doctor certifies they have a life expectancy of six months or less if the disease follows its normal course. Starting hospice earlier allows the care team to build trust, manage symptoms well, and support the entire family.
The Benefits of Starting Hospice Sooner
When hospice starts earlier, patients and families get the full benefits. This support helps prevent emergencies and improves well-being.
- Better Symptom Control: A dedicated team of Registered Nurses and Hospice Aides can manage pain and other symptoms before they become a crisis.
- Stronger Relationships: The patient and family build a bond with their care team, which includes a Social Worker and Chaplain.
- Fewer Hospital Visits: With expert care at home and 24/7 on-call support, patients can often avoid stressful trips to the emergency room.
Starting hospice care sooner is not about giving up; it is about maximizing life. It provides a strong support system to help patients live more comfortably and meaningfully for as long as possible.
3. Myth: Hospice Hastens Death
Truth: Hospice Provides Comfort and Does Not Speed Up the Dying Process
One of the most harmful myths is that hospice teams hasten death with medication. This fear often comes from confusion about pain management. It can cause families to refuse care that could ease a loved one's suffering.
The truth is that hospice care works to preserve and improve the quality of life, not shorten it. The main goal is to manage symptoms, so patients can live as fully as they can. Hospice follows strict ethical and legal rules that do not allow any action meant to hasten death.
The Role of Medication in Hospice
Hospice clinicians are experts in managing pain, shortness of breath, or anxiety. They use medications like morphine safely and effectively to bring relief.
- The goal is comfort: These medicines are used to relieve suffering, not to end life. Doses are carefully managed to meet the patient’s needs.
- Euthanasia is not hospice: Euthanasia and physician-assisted death are legally and ethically separate from hospice. Hospice care supports the natural dying process.
A hospice nurse administers medication only to relieve a distressing symptom, like pain. The intent is never to impact the patient’s lifespan. In fact, when severe pain is managed well, patients are often more alert and engaged. To learn more, explore expert hospice pain management.
4. Myth: Hospice Is Only for People with Cancer
Truth: Hospice Serves Patients with Many Serious Illnesses
An old belief is that hospice is only for people with cancer. While the modern hospice movement started with cancer care, this narrow view is no longer true. It stops many people with other illnesses from getting vital comfort-focused care.

The truth is that hospice supports anyone with a life-limiting illness. Care is available for a wide range of conditions when the focus shifts from cure to comfort. This includes patients with end-stage heart, lung, kidney, or liver disease, as well as dementia and other neurological conditions.
Who Can Receive Hospice Care?
Hospice eligibility is based on a doctor’s prognosis of six months or less, not a specific disease.
- Heart Disease: Patients with end-stage congestive heart failure get support to manage symptoms at home.
- Dementia and Alzheimer's Disease: Hospice provides specialized care focused on dignity and comfort in the final stages.
- Lung Disease (COPD): Individuals receive expert respiratory support to ease breathing.
- Neurological Conditions: Hospice assists patients with conditions like Parkinson's disease or ALS.
Hospice is not defined by a single disease but by a patient's need for comfort, dignity, and support. As a trusted local provider on the Central Coast, Central Coast VNA & Hospice offers this care for patients with a wide range of diagnoses.
5. Myth: Hospice Care Is Too Expensive
Truth: Hospice Is Covered by Medicare, Medicaid, and Most Private Insurance
A major worry for families is the cost of hospice care. Many assume that this level of specialized support comes with a high price tag. This fear can cause delays in getting help that would bring comfort and relief.
The reality is that hospice is a covered benefit for most eligible patients. Financial concerns should not stop anyone from receiving compassionate end-of-life care. Most families find that hospice is more affordable than repeated hospital visits.
How Hospice Is Paid For
The hospice benefit is designed to be an all-inclusive package of care.
- Medicare Coverage: The Medicare Hospice Benefit covers 100% of the costs related to the terminal illness. This includes the care team, medical equipment, supplies, and medications.
- Other Insurance: Most state Medicaid programs and private insurance plans offer a similar comprehensive hospice benefit.
- Nonprofit Support: As a nonprofit organization, Central Coast VNA & Hospice is dedicated to providing care regardless of a patient's ability to pay. Our team helps families find financial assistance when needed.
This structure is designed to ease financial stress, allowing families to focus on their time together. Hospice care from Central Coast VNA & Hospice in Monterey County and surrounding areas is accessible to all who need it.
Your Next Step: Guidance from a Trusted Local Partner
Navigating a serious illness is overwhelming. Throughout this article, we’ve shared the truth behind 5 common hospice myths to replace fear with facts. Understanding these truths helps families make choices that honor a loved one’s wishes for dignity and peace.
The most important takeaway is that hospice is a powerful choice to embrace a different kind of hope. It is a proactive decision to focus on quality of life. As a nonprofit healthcare provider with over 74 years of service to the Central Coast, we are here to provide clarity.
Central Coast VNA & Hospice is the trusted partner for families in Monterey County, San Benito County, Santa Cruz County, and South Santa Clara County. Our local teams provide care that addresses the whole person. If you are unsure if it's time for hospice, our team can explain your options with no pressure.
Frequently Asked Questions (FAQs)
1. What is hospice care?
Hospice is a special type of care focused on comfort and quality of life for a person with a serious illness who is approaching the end of life. It provides physical, emotional, and spiritual support to both the patient and their family.
2. When is the right time to start hospice?
A person is generally eligible for hospice when a doctor determines they have a life expectancy of six months or less if the illness runs its natural course. It's best to start the conversation early to get the full benefit of hospice support.
3. Where is hospice care provided?
Hospice care is most often provided in the comfort of a person's own home. It can also be provided in nursing homes, assisted living facilities, or a dedicated hospice facility.
4. Does choosing hospice mean we can no longer see our regular doctor?
No, your regular doctor can continue to be involved in your care. The hospice team will work closely with your physician to coordinate a plan of care that meets your goals.
5. What services does Central Coast VNA & Hospice provide?
As a nonprofit, mission-driven provider, we offer a continuum of care that includes home health, palliative care, and hospice. Our hospice team includes Registered Nurses, Hospice Aides, Social Workers, Chaplains, and volunteers who provide expert medical care, emotional support, and spiritual guidance.
Ready to explore your options with a compassionate, local expert? Contact VNA and Hospice to learn how our team can help your family navigate the journey ahead with dignity and support. We are here to provide the truth about what hospice care truly offers.
Is It Safer to Age at Home Instead of a Nursing Home?
Safety Benefits of Aging at Home

Aging at home with skilled support can lower many hidden risks. Personalized visits by a Registered Nurse, real-time fall reporting, and hands-on medication checks add up to safer daily life.
- Transparent Fall Reporting tracks every incident.
- Tailored Care Visits adjust as health needs change.
- Medication Reviews catch dosage issues early.
- Familiar Surroundings reduce confusion and stress.
A 2025 report from the U.S. Department of Health and Human Services Office of Inspector General found nursing homes failed to report 43% of serious falls among Medicare residents (Read the full study on fall reporting transparency). Real-time home health data gives families immediate insight and action steps.
Contact Central Coast VNA & Hospice today to explore home safety options.
Current Safety Statistics
Families often compare real numbers before choosing a care setting:
- Nursing homes host about 1.24 million residents in 14,742 CMS-certified facilities, averaging 9.5 deficiencies per survey with 27% flagged as serious (Discover insights about nursing facility characteristics on KFF).
- Home health care teams logged 424 million visits in 2020 and report a 91% satisfaction rate (home health statistics on BoostHomeHealth).
That snapshot shows how home health nursing can surface hazards faster than intermittent facility surveys. Seniors at home benefit from deeper data and personalized plans.
Key Insight
Skilled home visits and targeted environmental changes often reduce emergency trips and improve peace of mind.
How to Choose Between Home and Facility Care
Deciding whether to age in place or move to a nursing home depends on four core factors:
-
Clinical Needs
- Can scheduled RN visits handle wound care, IV therapy, and medication management?
- Is 24/7 nursing essential for stability?
-
Functional Abilities
- Does the person need help dressing, bathing, or moving safely?
- Could physical therapy and adaptive equipment meet those needs at home?
-
Social Engagement
- Are family meals, volunteer visits, or virtual support groups available?
- Does isolation raise fall or depression risks?
-
Home Environment
- Are grab bars in place?
- Is lighting bright and layouts clear of trip hazards?
Often a hybrid plan works best: short facility stays for acute care, combined with ongoing in-home therapy and nursing.
Learn more about in-home nursing in Monterey County: Whether In-Home Nursing Is Right For Your Loved One In Monterey.
Making Home Safer for Aging

Simple upgrades can match many facility safety features. Focus on high-traffic areas and pair fixes with clinical support.
- Install grab bars in bathrooms and hallways.
- Secure loose rugs and remove cords from floors.
- Add motion-sensor lighting by stairs and entrances.
- Widen doorways for walkers or wheelchairs.
- Use non-slip mats in showers and by sinks.
Pair these changes with professional care:
- Registered Nurses monitor vitals, adjust medications, and flag concerns.
- Physical and Occupational Therapists build balance, strength, and teach safe routines.
- Telehealth check-ins solve issues quickly.
- Hospice Aide support helps with light chores and errands to reduce clutter.
Case Example: Mrs. Smith saw a 30% reduction in falls after eight weeks of balance training and home modifications. Her confidence grew as injuries fell.
For more tips, see our guide on preventing falls in the home.
Central Coast VNA & Hospice Support Services

With over 74 years as a nonprofit, mission-driven provider, Central Coast VNA & Hospice brings home health nursing, therapy, and palliative care to Monterey, San Benito, Santa Cruz, and South Santa Clara counties.
Their full continuum of care includes:
- Skilled Home Health Nursing for medication management and post-hospital recovery
- Physical & Occupational Therapy to boost strength and prevent falls
- Palliative Care Consultations for symptom relief and comfort at home
- Social Work Coordination for equipment loans, meal services, and transportation
- Compassionate Hospice Support led by physicians, Chaplains, and Hospice Aides
- Call CCVNA at 831-372-6668 to discuss needs.
- Schedule a no-cost in-home assessment with a Registered Nurse.
- Receive a personalized care plan.
- Begin visits that support safe, dignified aging in place.
Learn more: guide to home health and hospice services or Read more about our community impact here.
Frequently Asked Questions
Q1. What home changes cut fall risks?
Install grab bars, brighten lighting, and secure rugs. An Occupational Therapist will spot hidden hazards.
Q2. How does home health nursing compare to facility care?
Home visits offer real-time incident reports and tailored medication reviews. Facilities rely on scheduled inspections that may miss day-to-day events.
Q3. Can palliative care at home manage chronic symptoms?
Yes. Palliative consults focus on pain control, emotional support, and care coordination, just as in a facility.
Q4. What costs should families compare?
Compare in-home visit fees, equipment rentals, and renovations versus facility room rates and care-level charges. Factor in Medicare, Medi-Cal, and private insurance.
Q5. When should care decisions be revisited?
Review every 3–6 months or after a fall or hospital stay. Check clinical indicators, functional ability, and family support capacity.
Contact us today to explore how aging at home can be safer and more comfortable.
Central Coast VNA & Hospice
Fall Risks for Seniors Rise on the Central Coast as Temps Drop
As seasons turn on California's Central Coast, the crisp air is a welcome change. But for older adults, lower temperatures bring a quiet danger. The simple truth is that fall risks for seniors rise as temps drop locally, turning homes into potential hazards.
The Invisible Threat of Cooler Weather on the Central Coast
When cooler weather settles into Monterey, Santa Cruz, and San Benito Counties, it brings more than a chill. For seniors, it creates new challenges that increase the chance of a fall. This seasonal shift creates environmental and physical risks that catch many families off guard.
Slippery sidewalks after a morning frost in Salinas can be a problem. Earlier sunsets leave rooms dimly lit, and cold-induced stiffness makes joints ache. What might seem like a minor stumble can lead to serious injuries, hospital stays, and a loss of independence.
This flowchart shows the link between colder weather and the hazards that follow.
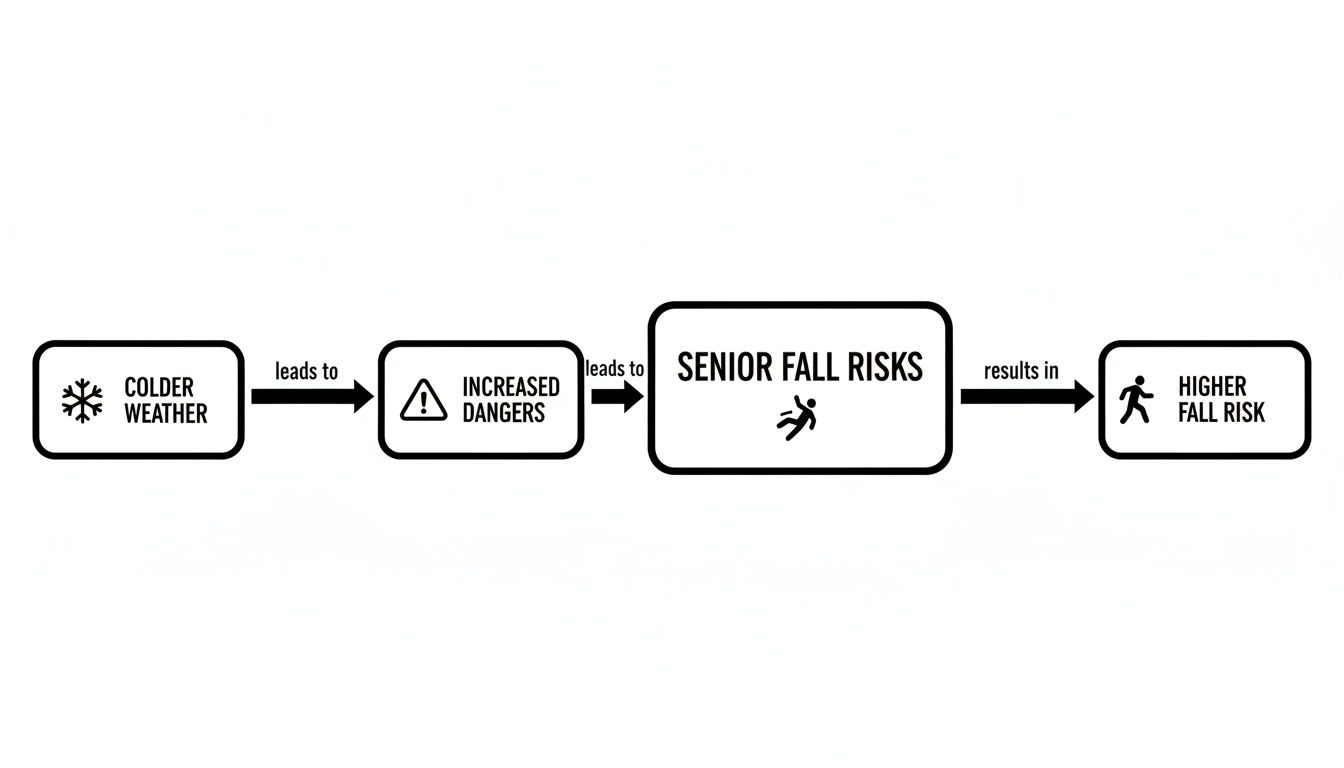
As you can see, falling temperatures set off a cascade of new dangers, directly elevating the risk of a fall.
Understanding the Seasonal Spike in Falls
This connection is backed by data. National studies show a clear seasonal pattern. Fall-related emergency room visits for adults aged 65 and older spike during the winter months.
A simple fall can be a life-altering event. It is a leading cause of both fatal and non-fatal injuries for older Americans. This makes prevention a critical part of senior wellness.
For families across our local communities, from Hollister to South Santa Clara County, understanding this threat is the first step. Once you recognize the risk, the need for proactive solutions becomes clear. The table below breaks down common hazards seniors face on the Central Coast during colder months.
Common Winter Fall Risks for Seniors on the Central Coast
This table shows the main factors that increase fall risk for seniors during colder weather in our local communities.
| Risk Factor | Description | Example in Monterey or Santa Cruz |
|---|---|---|
| Environmental Hazards | Slippery surfaces from morning frost, dew, or rain become more common. | A senior in Santa Cruz walks out to get the newspaper and slips on a walkway that is unexpectedly slick from morning moisture. |
| Reduced Visibility | Earlier sunsets and overcast days lead to lower indoor and outdoor light, obscuring trip hazards. | An older adult in Monterey misjudges a step inside their home during the dimly lit late afternoon hours. |
| Physiological Changes | Cold temperatures can cause joint stiffness, muscle tightness, and slower reaction times, affecting balance. | After sitting for a while in a cool room, a senior in Hollister stands up too quickly and feels unsteady due to stiff knees. |
| Increased Indoor Activity | Spending more time indoors can increase the risk of tripping over household clutter like rugs and cords. | A resident in Salinas, staying inside to avoid the cold, trips over a throw rug they usually navigate around easily. |
At Central Coast VNA & Hospice, our mission is to provide proactive support. With over 74 years of nonprofit service, our teams of Registered Nurses and therapists understand local challenges. We are dedicated to providing in-home care to keep your loved one safe and secure at home.
How Cold Weather Affects a Senior's Body and Balance
When an older loved one falls during the winter, it’s easy to blame obvious things like ice. But the biggest threat isn't always underfoot. A key reason fall risks for seniors rise as temps drop locally is due to subtle changes happening inside their bodies.
The cold itself changes how muscles, nerves, and joints work. This creates a hidden vulnerability. Cold makes muscles and joints stiff and less responsive, like a rubber band left in a freezer.
Stiff Joints and Tight Muscles
On a chilly day, the body tries to save heat by constricting blood vessels. This reduces blood flow to the legs and feet. Less blood flow means less warmth for muscles and joints, causing stiffness.
For an older adult, this change makes simple movements harder. Here’s how it plays out:
- Slower Reaction Times: Stiff muscles can't contract as quickly. This makes it hard to catch oneself during a stumble.
- Reduced Range of Motion: When hips and knees are tight, a person’s gait can change. They might start shuffling their feet, which increases the risk of tripping.
- Increased Arthritis Pain: Cold, damp weather can make arthritis flare up. Chronic pain can make a senior hesitant to move, leading to instability.
These factors quietly disrupt a person’s balance. They make falls more likely, even in the familiar setting of home.
Numbness and Reduced Sensation
Another change happens in the nervous system. Cold temperatures can slightly numb nerve endings in the feet. This is a problem because it dulls the feedback the brain needs to maintain balance.
Imagine walking across an uneven floor while wearing thick socks. You wouldn't feel the dips and bumps beneath you. That’s what happens when cold reduces sensation in a senior's feet.
The Impact of Medications
Winter also brings cold and flu season, which means more over-the-counter medications. Many of these remedies can cause drowsiness or dizziness. These are major risk factors for a fall.
When added to a senior's existing prescriptions, the risk can multiply. For help, exploring professional medication management for elderly loved ones can be a game-changer. A medication review with a skilled clinician from Central Coast VNA & Hospice is a vital part of winter safety.
Our Registered Nurses help families in Hollister, Salinas, and surrounding areas understand side effects. We organize medication schedules to lower risks. By identifying these internal threats, we help build a stronger foundation for fall prevention.
Creating A Fall-Proof Home For Winter
Making a home a safe haven for winter doesn't require a massive overhaul. Simple changes can make the biggest difference in preventing falls. As fall risks for seniors rise as temps drop locally, walking through the living space is a powerful way to protect a loved one.
The stakes are high. According to the CDC, millions of older adults fall each year, with many resulting in serious injury. A few thoughtful adjustments can dramatically lower the odds of an accident.

A Room-By-Room Safety Checklist
This is a practical guide to fixing common household hazards. These steps can create a safer environment for an older adult this winter.
Hallways and Main Walkways:
- Light It Up: Use brighter bulbs in hallways, stairwells, and entryways. Nightlights can make a difference for late-night trips to the bathroom.
- Clear the Path: Get rid of clutter that could cause a trip. This includes mail, shoes, and small items in walking areas.
- Secure All Rugs: Use double-sided tape or non-slip backing to anchor area rugs. It's often best to remove small throw rugs entirely.
Living Areas:
- Tame the Cords: Neatly tuck away electrical and phone cords along baseboards.
- Rethink Furniture Placement: Make sure there are wide, clear paths through every room.
Bathroom:
- Add Non-Slip Surfaces: Place non-slip mats inside the tub or shower. Use a non-slip bathmat on the floor right outside of it.
- Install Grab Bars: Securely install grab bars next to the toilet and inside the shower. Towel racks are not built to support a person's weight.
- Bring in a Shower Chair: A shower chair provides stability and helps reduce fatigue.
Kitchen:
- Keep Things Within Reach: Store frequently used items on lower, easy-to-reach shelves. This prevents the risky need for a step stool.
- Wipe Up Spills Immediately: A little water or grease on the floor is a serious slipping hazard.
- For peace of mind, consider installing non-slip vinyl flooring in high-risk areas.
A fall-proof home is about smart choices that support independence and safety.
When You Need An Expert Eye
While these DIY tips are a great start, some hazards are not obvious. This is where a professional’s expertise helps. At Central Coast VNA & Hospice, our Occupational Therapists are trained to perform expert home safety evaluations.
During a visit, our therapists look at daily routines and identify specific risks. They provide personalized recommendations and can help with adaptive equipment. This guidance ensures your loved one's home is truly optimized for their needs.
For a deeper dive into creating a secure living space, check out our guide on preventing falls in the home. These small changes can add up to a season of safety.
Taking Action Before A Fall Happens
The best time to deal with a fall is before it happens. A proactive approach is the most effective way to help a loved one stay safe. As the seasons change, this becomes more important than ever since fall risks for seniors rise as temps drop locally.
Waiting for an accident can have serious consequences. Building a safety net now can address the root causes of instability. This means taking a professional look at their health, mobility, and medications.
An Integrated Approach to In-Home Safety
At Central Coast VNA & Hospice, our mission is built around providing proactive, in-home support. We know that preventing a fall requires a coordinated effort. For over 74 years, our nonprofit teams have served Monterey, Santa Cruz, and nearby communities.
Our teams work together to create a personalized safety plan. This continuum of care makes sure your loved one gets the right support.
Here's how our different services come together:
- Skilled Nursing: Our Registered Nurses conduct medication reviews to spot prescriptions that might cause dizziness. They work with doctors to minimize dangerous side effects.
- Physical Therapy: Our Physical Therapists design custom exercise programs. They focus on building strength, improving balance, and increasing flexibility.
- Palliative Care: For those with a serious illness, our Palliative Care team provides extra support. They manage symptoms like pain and fatigue that contribute to falls.
Palliative Care: A Key Layer of Support
Many families think Palliative Care is only for hospice, but it plays a key role in fall prevention. It is specialized care for people with a serious illness, available at any age or stage.
Its goal is to relieve symptoms and stress, which directly impacts stability. By managing symptoms, our Palliative Care specialists help seniors feel stronger. This reduces their risk of falling.
The table below shows how our core services work together to keep your loved one safe.
How CCVNA Services Reduce Fall Risk
| Service | How It Helps Prevent Falls | Who It's For |
|---|---|---|
| Skilled Nursing | Conducts medication reviews to identify and manage prescriptions that cause dizziness or drowsiness. Monitors overall health to catch issues early. | Seniors recovering from surgery, managing a new diagnosis, or needing complex medical care at home. |
| Physical Therapy | Develops personalized exercise plans to build strength, improve balance, and increase flexibility. Teaches safe ways to move and use assistive devices. | Individuals who feel unsteady, have lost mobility, or are recovering from an injury or illness that affects their physical abilities. |
| Palliative Care | Manages symptoms like chronic pain, fatigue, and shortness of breath that contribute to instability. Focuses on improving overall comfort and quality of life. | Anyone with a serious illness (like heart disease, COPD, or dementia) needing an extra layer of support, at any stage of their illness. |
This integrated approach ensures we are actively preventing problems.
Central Coast VNA & Hospice is the only provider on the Central Coast offering this full spectrum of care under one roof. Our mission is to keep seniors in our community safe and independent at home. If you are looking for ways to help seniors live at home safely, our team is here to help.
Warning Signs Your Loved One Is At Risk
Recognizing subtle red flags of a fall risk is a powerful tool for families. These signs often get brushed off as just “getting older.” But they are signals that a loved one needs more support, especially as fall risks for seniors rise as temps drop locally.
For families in Hollister, Salinas, and across the Central Coast, paying attention to small shifts can reveal a bigger picture. Trust your gut. If you notice something feels off, it probably is.

Physical and Behavioral Clues To Watch For
These warning signs often appear gradually. They are clear indicators that balance and confidence are fading. Being observant is the first step toward prevention.
Keep an eye out for these easy-to-spot signs:
- "Furniture Walking": Holding onto walls or furniture for support while moving through a room.
- Difficulty Standing Up: Struggling to get out of a chair or pushing off forcefully with their arms.
- Shuffling or Unsteady Gait: A change from a confident stride to short, shuffling steps.
- Avoiding Certain Activities: Stopping daily walks, using the stairs, or carrying groceries due to fear.
Verbal Cues That Signal Trouble
Sometimes, the most important clues are in what your loved one says. Pay attention to complaints that might seem minor but point to bigger issues. Any mention of dizziness, lightheadedness, or feeling "woozy" should be taken seriously.
Other verbal signs include:
- Expressing a direct fear of falling.
- Complaining of numbness in their feet.
- Mentioning they’ve had a "close call" or nearly stumbled.
If you’ve noticed any of these cues, it may be time for a professional evaluation. Our guide on the 5 warning signs elderly parents need home health care can provide more insight. Contact Central Coast VNA & Hospice to ask about an in-home evaluation.
Partner With CCVNA For A Safer Winter
You don't have to navigate these challenges alone. We've seen how fall risks for seniors rise as temps drop locally. Partnering with Central Coast VNA & Hospice is a powerful move toward a safer winter.
For over 74 years, our nonprofit mission has been to deliver expert care at home. We are woven into the communities we serve, from Monterey to Hollister. We understand the unique challenges our local seniors face.
Your Local Partner in the Continuum of Care
We empower families with a seamless range of support. Our services are designed to work together to create a comprehensive safety net.
- Home Health: Our Registered Nurses and therapists address immediate health concerns, from medication management to physical therapy.
- Palliative Care: This service provides an extra layer of support. It focuses on managing symptoms that lead to instability.
- Hospice Care: Should the need arise, we provide compassionate end-of-life care focused on comfort and dignity.
This integrated approach solidifies our role as your dedicated local partner.
Central Coast VNA & Hospice is the only organization on the Central Coast providing this full spectrum of care under one roof. Don't wait for a fall to happen. Taking action today can preserve independence and give you peace of mind. To see how our teams make a real difference, learn more about how VNA helps seniors live safely at home in Monterey.
Compassionate, professional help is just a phone call away. Contact Central Coast VNA & Hospice today to learn how we can support your family this winter.
Frequently Asked Questions About Senior Fall Prevention
As temperatures drop on the Central Coast, many families worry about their aging loved ones. Protecting them from a fall is a top priority. Here are answers to some of the most common questions we receive.
How can I tell if my parent is at risk for a fall?
The earliest signs are often subtle changes in daily movements. A professional home health evaluation from Central Coast VNA & Hospice is the best way to get a clear picture. Watch for signs like "furniture walking," struggling to stand up, shuffling their feet, or mentioning dizziness.
Isn't home health care just for after a hospital stay?
While home health is essential for recovery, it is also a powerful tool for prevention. Proactive care is key, as fall risks for seniors increase as temperatures drop. If your loved one is becoming weaker or managing a chronic illness, they may qualify for our preventive services.
Does CCVNA help people in the rural parts of the Central Coast?
Yes. As a local nonprofit provider for over 74 years, our commitment extends to every corner of our community. Our mobile clinical teams bring expert care to your loved one’s front door, whether you live in town or in a rural part of Monterey or San Benito Counties.
What's the difference between palliative and hospice care?
Palliative care can start at any point during a serious illness, alongside curative treatments. It focuses on managing symptoms that can increase fall risk. Hospice care is for the end of life when the focus shifts entirely to comfort, peace, and dignity.
How do I start the conversation about fall prevention with my parent?
Approach the topic with compassion and as a partnership. Frame it as a way to help them maintain their independence. Say something like, “I want to make sure you can keep living here safely. Could we look at a few things together to make the house safer for winter?” This respects their autonomy while addressing your concerns.
If you've noticed any of these warning signs in someone you love, please don't wait. The team at Central Coast VNA & Hospice is here with the expert support your family needs to get through the winter safely. Contact us today to learn more about our home health, palliative care in Monterey County, and hospice care services.
What Does Aging in Place Really Mean for Families? A Practical Guide
For many families, aging in place means helping a loved one stay in their own home. But it is much more than that. It is a promise to help them live safely and independently in a place full of memories. This journey often puts you in new roles, like care coordinator and safety expert.
The True Meaning of Aging in Place for Your Family

Many families in Monterey and Santa Cruz Counties want to honor a loved one's wish to stay home. It is a strong desire. In fact, AARP found that 75% of adults aged 50 and older want to remain in their homes as they get older.
But making this wish a safe reality takes work. Aging in place is not a single decision. It is an ongoing process of changing a home and support system to meet new needs. It is about finding a balance between your loved one's freedom and the need to manage health issues.
Beyond the Simple Definition
To understand aging in place, you have to look deeper. It brings a new set of tasks that most families do not think about until a crisis happens.
Suddenly, you may find yourself taking on several new jobs:
- Care Coordinator: You schedule doctor visits, manage medications, and talk to healthcare providers.
- Safety Inspector: You learn to spot dangers like loose rugs, poor lighting, or slippery floors to prevent falls.
- Financial Planner: You figure out what Medicare or private insurance covers and what the family needs to pay for.
- Emotional Supporter: You offer comfort and help your loved one handle the emotional changes that come with aging.
This journey is rewarding, but it can also be very demanding. The key is to build a support network before you need it.
Aging in Place Hopes Versus Family Realities
It is normal to have an ideal idea of what aging in place will look like. However, families must be realistic about the daily work of caregiving. This table can help you prepare.
| Common Hope | Practical Reality for Families |
|---|---|
| "Mom will be happy and independent in her own home." | Independence often requires a lot of support, like managing pills, making meals, and getting to appointments. |
| "The house is fine; it's where she's always lived." | A familiar home can have new risks. It may need changes like grab bars, ramps, or better lighting to prevent falls. |
| "We'll save money by avoiding a nursing home." | Home care, home changes, and medical supplies can add up. It is important to plan for these costs. |
| "Our family can handle everything ourselves." | Caregiving is a long journey. Relying only on family can lead to burnout, stress, and difficult relationships. |
| "We'll figure it out as we go." | Waiting for a crisis to make a plan is stressful. Planning for care, money, and legal matters ahead of time is much better. |
Facing these realities does not mean aging in place is impossible. It just means that planning and support are necessary for success.
For families on the Central Coast, this does not have to be overwhelming. As a nonprofit provider with deep local roots, Central Coast VNA & Hospice has helped families with these plans for over 74 years. By working with experts who know the healthcare system in Monterey, San Benito, Santa Cruz, and South Santa Clara Counties, you can get the right support at the right time.
You can learn more about the different types of in-home care for seniors that can make aging in place a safe and positive experience.
Navigating the Daily Demands of At-Home Support

Supporting a loved one at home is more than just keeping them company. It involves hands-on tasks that take time, patience, and emotional energy every day.
Families in communities like Salinas and Hollister quickly learn that caregiving is not just one role—it is many. It also requires a new set of skills you might not have expected to learn.
You will likely help with two main types of daily needs. The first is Activities of Daily Living (ADLs), which are basic self-care tasks. The second is Instrumental Activities of Daily Living (IADLs), which are more complex tasks needed to live alone.
What Caregiving Actually Looks Like Day-to-Day
To understand what aging in place means for your family, it helps to see what these duties look like. Your daily routine might include a mix of the following:
- Personal Care (ADLs): This could mean helping with bathing, dressing, or using the toilet. These are private moments that require kindness and trust.
- Mobility (ADLs): You may help your loved one get from the bed to a chair, walk safely, or get in and out of the car.
- Meal Preparation (IADLs): This is more than just cooking. It includes grocery shopping, planning meals for special diets, and sometimes helping with eating.
- Medication Management (IADLs): Handling multiple prescriptions and correct doses can be one of the most stressful parts of caregiving.
- Transportation (IADLs): Driving to doctor’s visits, physical therapy, or the pharmacy can become a regular part of your week.
Each of these tasks adds up. Soon, many family members find that caregiving has become a part-time or even full-time job.
Research shows how big this commitment is. You can learn more about the impact of caregiving on families here.
The Unspoken Risk: Family Burnout
When one or two people handle all these duties, caregiver burnout is a real risk. Burnout is a state of complete physical, emotional, and mental tiredness. It happens when you try to do too much for too long without enough help.
You might feel overwhelmed, worried, or easily annoyed. This is not a sign that you do not care. It is a sign that you need more support.
This is why it is so important to understand the reality of aging in place. When you see the full picture, you can plan for help before you reach a breaking point.
You Don't Have to Do This Alone
You are not meant to carry this weight all by yourself. Central Coast VNA & Hospice offers professional home health services to share the load. Our skilled clinicians, including Registered Nurses and therapists, can manage complex medical needs at home.
For example, a Registered Nurse can handle wound care, IVs, and a complex medication schedule. This ensures your loved one gets expert medical care. This frees you up to be a son, daughter, or spouse again. Check out our guide on 5 expert tips to prevent medication errors at home for more.
Working with a trusted nonprofit provider like us means you are bringing a team of caring experts into your circle. It lets your family focus on love and support.
Making Your Home a Safe Haven for a Loved One
A safe and easy-to-use home is the foundation for aging in place. When your loved one’s home supports their changing needs, they can keep their independence. This means taking a practical look at the home to find and fix common dangers.
This is not about bubble-wrapping the house. It is about making smart changes that make a real difference. The main goals are to prevent falls, improve lighting, and make it easy to move around.
Practical Steps for a Safer Home
Creating a safer home often starts with the highest-risk areas: the bathroom, hallways, and stairs. A few thoughtful changes can greatly lower the chance of an accident.
- In the Bathroom: This room is a common place for falls. Installing grab bars near the toilet and in the shower is a must. Add non-slip mats and think about a shower chair for extra stability. A walk-in shower for seniors can be a great upgrade.
- In Hallways and Living Areas: Clear paths are very important. Remove clutter, secure loose rugs, or get rid of them. Make sure electrical cords are tucked away so no one can trip.
- On the Stairs: Strong handrails on both sides of the stairs are essential. Make sure the lighting is bright over the stairs. Consider adding non-slip strips to each step.
There is often a gap between wanting to stay home and being able to do it safely. Nearly 95% of people over 60 have at least one chronic condition. This creates a growing need for skilled support at home.
The Role of Technology in Home Safety
Today's technology also gives us powerful tools to improve safety. These devices can provide peace of mind when you cannot be there.
A medical alert system is a great place to start. It lets your loved one call for help with the push of a button. Other helpful tools include automatic stove shut-off devices and motion-activated night lights.
For families, what aging in place really means is creating layers of support. Combining home changes with smart technology creates a strong system for independence and safety.
Professional Guidance for Your Unique Home
Figuring out the right changes on your own can be hard. Every home is different, and so is every person’s health. This is where getting professional advice is so valuable for families in Monterey County.
At Central coast VNA & Hospice, our Physical and Occupational Therapists are experts in home safety. They visit your loved one’s home to do a full safety check. This is not a generic checklist. It is a personal review based on your loved one's health and home layout.
Our therapists give professional advice made just for your family. Their expert guidance helps you spend your time and money on the changes that will help the most. For more tips, our guide on preventing falls in the home offers more practical advice.
Building a Support System Before a Crisis Happens
Most families wait to create a care plan until a crisis happens, like after a fall. This approach leads to rushed, stressful decisions.
The real key to successful aging in place is to plan ahead. It is about building a strong support system before you need it.
Thinking ahead gives you time to understand the different types of care. This is often called the Continuum of Care. It is a series of services that can change as your loved one's needs change over time.
When families in Salinas and Hollister understand this model, they can get the right care at the right time. This helps avoid the stress of emergency planning.
This diagram shows how home safety is a basic part of that planning.

As you can see, simple safety measures are key first steps in creating a secure home.
Understanding the Layers of In-Home Care
So, what does aging in place look like when medical needs arise? It means knowing who to call. The continuum of care has three main parts that provide full support at home.
- Home Health Care: This is skilled medical care from licensed professionals like a Registered Nurse or a Physical Therapist. It is often for recovery after a hospital stay or for managing a new health problem.
- Palliative Care: This is special support for someone with a serious illness. The goal is to improve quality of life by managing pain and stress. Palliative care can be given at the same time as treatments meant to cure an illness.
- Hospice Care: This is comfort care for people near the end of life. When treatments to cure an illness are no longer working or wanted, hospice focuses on comfort and dignity. A full team supports the patient and family.
How These Services Work Together
Imagine a loved one in Monterey County is recovering from pneumonia. They might start with home health care for nursing and therapy at home. As they recover, they may still have trouble breathing from a chronic condition.
This is a good time to add palliative care. The team can help manage their breathing problems and make them more comfortable. This helps avoid future trips to the hospital.
Later, if their condition gets worse, the family can smoothly move to hospice care. This ensures they get comfort and dignity at home, with the people they love.
As the only provider on the Central Coast offering this full range of care, Central Coast VNA & Hospice ensures your loved one gets steady support from a team they trust as their needs change.
This continuum of care prevents gaps in support and reduces family stress. Knowing where to turn next provides great peace of mind. You can also learn about respite care for family caregivers to see how you can get needed breaks.
The True Costs: Navigating the Financial and Emotional Landscape
When a family chooses aging in place, they often talk about home changes and care schedules. But the real journey includes managing big financial and emotional costs. Understanding these costs is key to a plan that works for everyone.
Talking honestly about these costs early on helps prevent problems later. It ensures everyone feels supported.
The Financial Side of Aging in Place
One of the biggest mistakes families make is thinking insurance will cover everything. Programs like Medicare and Medi-Cal are important, but you need to know what they do and do not cover.
- What Medicare Actually Covers: Medicare's home health benefit is for short-term, skilled care. It covers things like a Registered Nurse visit for wound care or a Physical Therapist to help you get stronger.
- The Big Coverage Gap: What Medicare does not pay for is long-term custodial care. This is the non-medical, daily help with bathing, dressing, and making meals that is often needed most.
This gap means families often have to pay for ongoing help out of pocket. In some cases, financial safety nets can help fund long-term care, similar to how Long Term Disability (LTD) benefits in Canada support individuals, though rules vary.
Families in Monterey and Santa Cruz Counties who plan for these costs are better able to provide steady care without a financial crisis.
The Emotional Weight on Families
Beyond money, aging in place has a deep emotional weight. Family members often feel a mix of love, duty, guilt, and stress. It is a journey with rewarding moments, but also big challenges.
Caregiving is an act of deep love, but it asks a lot of the person giving care. Admitting the emotional cost is the first step toward building a strong support system for the whole family.
These feelings are just as real as the financial costs. Burnout or frustration can happen, no matter how much you love the person you are caring for. Pushing these feelings away can harm relationships.
Finding Support for Everyone Involved
This is where a complete care model makes a difference. At Central Coast VNA & Hospice, our 74+ years of service have taught us that supporting a patient means supporting their family. Our nonprofit, mission-driven approach goes beyond just medical care.
Our team includes professionals who are here for the family’s well-being:
- Medical Social Workers: These team members are experts at connecting families with community resources. They help with confusing insurance questions and difficult family talks.
- Chaplains: Our chaplains offer spiritual and emotional support to people of all beliefs. They provide a caring ear for both patients and family members.
By caring for the whole person—and the whole family—we help you manage all the costs of aging in place. This support helps you find balance and focus on what matters most.
Your Local Partner in Compassionate Home Care

The journey of aging in place is a team effort. Your family does not have to do it alone. For over 74 years, Central Coast VNA & Hospice has been a trusted local partner for families in Monterey, Santa Cruz, San Benito, and South Santa Clara Counties. We are part of this community, and we are here to offer the compassionate guidance you need.
Our services create a full continuum of care, delivered in your loved one’s home. From skilled nursing and therapy to palliative and hospice support, our expert clinicians empower your family. We help you create a plan that honors your loved one’s wishes while keeping them safe.
A Growing Need for Local Support
The wish to age at home is a global trend. By 2050, the world's population of people aged 65 and older is expected to grow. You can learn more about this global demographic trend and what it means for communities.
At Central Coast VNA & Hospice, our nonprofit mission is to ensure professional, compassionate support is always available on the Central Coast. We don’t just treat patients—we help families coordinate care, create safety plans, and stay involved every step of the way.
If you’re helping a loved one age in place in Monterey, Santa Cruz, Salinas, or Hollister, you don’t have to do it alone. Our guide to expert aging-in-place services near you in Monterey can give you more specific information.
Contact Central Coast VNA & Hospice today to learn how our dedicated team can help you build a successful aging-in-place plan.
Frequently Asked Questions About Aging in Place
Thinking about aging in place brings up many questions. Having clear, honest answers helps families feel ready. Here are some of the most common questions we hear from families on the Central Coast.
When Is the Right Time to Plan for Aging in Place?
The best time to start planning for aging in place is long before a medical crisis happens. Planning early gives you time for calm talks about what your loved one wants for their future. This proactive approach lets you research support options and make home changes without the stress of an emergency.
Does Medicare Cover All In-Home Care Services?
This is a very important point. Medicare does not cover all types of in-home care. Medicare's home health benefit is for short-term, skilled services like nursing care after a hospital stay. It does not pay for 24-hour care or long-term help with daily tasks like bathing and dressing. Our team at Central Coast VNA & Hospice can help you understand what your insurance covers.
What Is the Difference Between Home Health and Palliative Care?
It is easy to confuse these two services. Home Health Care is focused on recovery. It brings clinical experts like a Registered Nurse or Physical Therapist to you to help you heal after an illness or surgery. Palliative Care is focused on comfort. It provides relief from symptoms and stress for someone with a serious illness and can be given at any stage of an illness.
How Can Our Family Avoid Caregiver Burnout?
Avoiding caregiver burnout is necessary for a successful aging-in-place plan. The key is to accept that you cannot do it all alone. Set realistic limits, and lean on professional support, like the services from Central Coast VNA & Hospice. Regular family meetings can also help you share the duties and talk openly.
What if a Loved One's Needs Become Too Great to Manage at Home?
Sometimes, a person's medical needs become too much to manage safely at home. When this happens, it is not a failure. It is a natural change in the care journey. Our team at Central Coast VNA & Hospice can help your family with a gentle transition to a different level of care. This may include our compassionate hospice services, which focus on comfort and dignity.
For over 74 years, Central Coast VNA & Hospice has been the community’s trusted, nonprofit partner, helping families through every stage of care. Contact us today to learn more about how our home health, palliative, and hospice services can support your family.
Supporting Your Family: 5 Ways Family Caregivers Can Avoid Burnout in 2026
Caring for a loved one is a profound act of love. But in 2026, the pressures on family caregivers are higher than ever. With increasing demands, the role can quickly lead to exhaustion and burnout.
This guide provides practical solutions. We will explore 5 ways family caregivers can avoid burnout in 2026. You will learn how to find respite, use technology, and build a support network.
The journey of caring for someone with a chronic illness can feel overwhelming. But you are not alone. Help is closer than you think, right here on California's Central Coast.
1. Embrace Respite as a Necessity, Not a Luxury
In 2026, family caregiver stress is at an all-time high. One of the best ways to combat this stress is respite care. Many caregivers wait too long to ask for help, viewing a break as a luxury.

Respite provides temporary, professional relief. It gives you time to rest and recharge without guilt. Respite isn't a luxury—it’s essential for your well-being.
How to Implement Respite Care
Integrating respite into your routine is a proactive step. It allows a trained professional, such as a Central Coast VNA & Hospice Aide or Registered Nurse, to provide support while you focus on your needs.
- Schedule It Like an Appointment: Block out regular time for respite on your calendar. Consistency is key, whether it's a few hours a week or a full day once a month.
- Start Small: Begin with short respite periods of an hour or two. This helps your loved one build trust with the visiting professional from CCVNA.
- Be Intentional: Use your break for activities that truly restore you. This could be a doctor's visit, lunch with a friend, or simply a quiet walk.
Know When to Ask for Help
The best time to arrange for respite care is before you feel overwhelmed. Common signs of caregiver burnout include sleep loss, irritability, and feeling overwhelmed. If you’re nodding yes, it’s time to talk with a professional.
Central Coast VNA & Hospice offers compassionate professionals who provide a range of services. This includes personal care and symptom management. To learn more, explore our hospice care services.
When planning your break, consider these practical tips for planning a stress-free vacation. By embracing respite, you preserve your ability to care for the person who depends on you.
2. Implement Structured Boundaries and Self-Care Routines
In the demanding world of family caregiving, it is easy to lose your personal identity. Setting structured boundaries is a key strategy to prevent burnout in 2026. This means treating your well-being with the same seriousness as your care schedule.

Creating boundaries is an act of self-preservation. It enables you to provide better, more sustainable care. It involves defining when your duties start and end and carving out time for yourself.
How to Implement Boundaries and Self-Care
A proactive approach to scheduling personal time is critical. Build self-care directly into your weekly plan. Setting clear routines is fundamental, and a resource like a realistic stay-at-home mom daily schedule can offer useful ideas.
- Establish 'Caregiving Hours': If possible, define a block of time for your primary tasks. Communicate these hours kindly but firmly to your loved one and other family members.
- Schedule Self-Care: Block out time for a weekly dinner with friends or 30 minutes of reading. Treat these appointments as seriously as a doctor's visit.
- Delegate Specific Tasks: Identify duties that others can handle, like picking up prescriptions. Assigning these tasks frees up your mental and physical energy.
When to Reinforce Your Boundaries
Set boundaries before resentment and exhaustion take over. If you find yourself consistently canceling personal plans or feeling irritable, it is time to act. Protecting your time allows you to be a more present caregiver.
Central Coast VNA & Hospice can provide the professional support needed to make these boundaries a reality. Our in-home palliative care and hospice services can manage complex symptoms. For more ideas on managing pressure, explore these tips on how to reduce daily stress.
3. Leverage Technology and Smart Home Solutions
In 2026, digital tools can ease the load of caregiving. Technology and smart home solutions are practical aids that can automate monitoring and enhance safety. For family caregivers, these tools reduce the need for constant hands-on help.

This approach allows your loved one to maintain independence while being monitored. From automated medication dispensers to fall detection sensors, these solutions provide peace of mind. Leveraging them is a key strategy for a more manageable caregiving journey.
How to Implement Technology
Integrating technology into a care plan should be a gradual process. The goal is to introduce tools that solve specific problems without being overwhelming.
- Start with One Solution: Begin with a single device that addresses the most pressing need. This could be a medication reminder app or a wearable device with fall detection.
- Prioritize User-Friendliness: Choose devices with simple interfaces that your loved one can use. Voice-activated assistants like Amazon Alexa are great for medication reminders.
- Coordinate with Family: Use shared digital calendars and care apps. This keeps all family members and the professional care team informed.
When to Use Smart Home Solutions
Technology is most effective when used proactively to prevent crises. If you worry about falls, missed medications, or safety, it is time to explore tech support. These tools create a safety net, reducing caregiver anxiety.
These tools are helpful for individuals with mobility or cognitive challenges. Remote monitoring systems allow you to check in visually via a secure camera. To learn more about adapting a home for safety, review these tips to help seniors live at home safely.
4. Build and Engage a Support Network
The saying "it takes a village" is especially true in caregiving. In 2026, isolation is one of the greatest threats to a family caregiver's well-being. Building a support network is a powerful way to combat loneliness.

A support network includes family, friends, and professionals. Relying on this circle prevents the weight of care from falling on one person. You're not alone—help exists in your community.
How to Implement Support Networks
Creating a network transforms caregiving from a solitary duty into a shared responsibility. It requires intentional effort, but the returns are immeasurable.
- Create a Family Care Team: Ask family and friends to join a care team. Hold meetings to delegate specific tasks, like grocery shopping or providing companionship.
- Explore Professional Support Groups: Connect with organizations like the Family Caregiver Alliance. These groups offer a safe space to share experiences with others who understand.
- Leverage Community Resources: Many local churches and community centers offer caregiver support. These can provide practical help like meal delivery or transportation.
When to Seek Network Support
The best time to build your network is before a crisis hits. If you feel isolated or overwhelmed, it is a clear sign to expand your support system. Help is available in Monterey County, San Benito County, and Santa Cruz County.
Central Coast VNA & Hospice can be a cornerstone of your network. Our Social Workers help families find community resources, while our Chaplains provide spiritual comfort. To learn more, explore our guide on building your support network.
5. Pursue Professional Training and Stress Management Education
Navigating caregiving without the right knowledge can be overwhelming. Investing in formal training and stress management education builds confidence. This approach transforms caregiving from a role of anxiety to one of empowerment.
This is about acquiring practical skills. From safe lifting to understanding medications, these skills make daily tasks less daunting. Learning stress-reduction methods also equips you to manage emotional demands.
How to Implement Training and Education
Education reduces anxiety. Central Coast VNA clinicians educate families early and often. This empowers them to make confident, informed decisions with dignity.
- Start with Condition-Specific Knowledge: Seek programs tailored to your loved one’s health condition. Look for resources from groups like the Alzheimer's Association or American Heart Association.
- Master Emergency Skills: Basic certifications like First Aid and CPR provide confidence. You can handle unexpected situations calmly and effectively.
- Practice Stress Management Daily: Enroll in a course like Mindfulness-Based Stress Reduction (MBSR). Practice these techniques for a few minutes each day to build emotional resilience.
When to Seek Educational Support
The best time to seek training is at the beginning of your journey. But it is never too late to learn new skills. If you feel anxious about making a mistake, education can provide significant relief.
Consider how to sign up for a CPR class in Monterey to feel more prepared. By arming yourself with knowledge, you are better equipped to handle challenges with skill and grace.
Your Partner in Care on the Central Coast
Navigating family caregiving can feel isolating, but you are not alone. The strategies in this article offer a roadmap for preventing burnout. By embracing respite, setting boundaries, using technology, and building a network, you create a sustainable foundation for well-being.
Asking for help is a sign of strength, not failure. Recognizing your limits and reaching out is the most loving action you can take. For over 74 years, Central Coast VNA & Hospice has been a steadfast, nonprofit partner for families.
Our mission-driven organization serves Monterey County, San Benito County, Santa Cruz County, and South Santa Clara County. Our continuum of care, from home health to palliative and hospice, is designed to support the whole family. If you’re caring for a loved one and feel stretched thin, our trusted services can support you both.
Don't wait for burnout to take hold. Discover how VNA and Hospice can provide the essential respite, expert clinical care, and emotional support your family needs. Contact us today to learn how our trusted services can help you avoid caregiver burnout in 2026.
Frequently Asked Questions (FAQs)
1. What are the most common signs of caregiver burnout?
Common signs include persistent fatigue, sleep problems, increased irritability, social withdrawal, and feeling hopeless or overwhelmed. Recognizing these signs early is the first step toward getting help.
2. How can Central Coast VNA & Hospice help my family?
As a nonprofit serving the Central Coast for over 74 years, CCVNA provides a continuum of care including home health, palliative care, and hospice. Our teams offer medical support, symptom management, emotional and spiritual counseling, and respite for family caregivers.
3. What is respite care?
Respite care is a short-term break for caregivers. A professional, like a Hospice Aide from CCVNA, steps in to provide care, allowing you to rest, run errands, or attend to your own health needs.
4. Where does Central Coast VNA & Hospice provide services?
We are a local, community-based organization serving Monterey County, San Benito County, Santa Cruz County, and South Santa Clara County.
5. How do I know when it’s time to ask for professional help?
If you are struggling to manage your loved one’s symptoms, feeling constantly exhausted, or your own health is suffering, it is time to ask for help. Contact Central Coast VNA & Hospice for a no-obligation consultation to explore your options.
Hospice vs. Palliative Care: What Families Really Need to Know
When a loved one is facing a serious illness, you will hear two terms: palliative care and hospice care. They may sound similar, but they are very different. Understanding the difference is a key step for your family.
Here is the simplest way to think about it. Palliative care helps with comfort and symptom relief at any stage of a serious illness. This happens even while someone is getting treatment to cure their illness.
Hospice care is a special type of palliative care for the end of life. It is usually for someone with a life expectancy of six months or less who is no longer seeking a cure.
Understanding the Two Paths of Comfort Care
For families in Monterey County, San Benito County, Santa Cruz County, and South Santa Clara County, getting these terms right is important. It helps you make confident healthcare choices. Both paths improve quality of life, but they start at different times.

Confusing the two can cause stress. It might also prevent your loved one from getting the right support at the right time.
Palliative care is a layer of support that can start on the day of diagnosis. It works with a patient’s doctors to manage pain, side effects, and stress. Hospice is a focused type of care for when goals change from curing an illness to maximizing comfort.
At Central Coast VNA & Hospice, we have served our community for over 74 years. Our nonprofit mission is to guide families with clear, compassionate information.
Palliative Care vs. Hospice Care at a Glance
This simple table helps show the main differences. It breaks down the purpose of each service.
| Care Aspect | Palliative Care | Hospice Care |
|---|---|---|
| Timing of Care | Can begin at diagnosis, at any stage of illness. | Begins when a cure is no longer the goal, typically with a prognosis of six months or less. |
| Treatment Goals | To relieve symptoms and stress from a serious illness while you continue active treatment. | To provide comfort, dignity, and quality of life when the illness is no longer curable. |
| Curative Treatment | Provided alongside curative treatments (e.g., chemotherapy, dialysis). | Patients are no longer seeking curative treatments for their terminal illness. |
| Who Provides Care | A specialized team that works with your other doctors. | An interdisciplinary team including a Registered Nurse, Hospice Aide, Social Worker, and Chaplain. |
This comparison is often a helpful first step. For more details, our guide on "What is palliative care?" is a great resource. Central Coast VNA & Hospice is here to guide you, no matter where you are on your journey.
Comparing the Goals of Palliative and Hospice Care
Definitions are a good start. But understanding the heart behind each type of care is what really helps families. Knowing the main purpose helps you see which path fits your loved one’s wishes.
The biggest difference is not just about timing. It is about the entire philosophy of care.
Palliative Care Aims for Comfort During Treatment
Palliative care is all about improving quality of life. Its goal is to add an extra layer of support that works alongside curative treatments. The team focuses on managing difficult symptoms so patients feel stronger.
Imagine a patient in Monterey County getting chemotherapy. The treatment is needed, but it causes nausea and fatigue. This is a perfect time for palliative care at home.
A palliative care team would work with the oncologist to:
- Manage tough side effects of treatment.
- Provide emotional support to cope with stress.
- Coordinate care between all the different doctors.
In this case, the goal is not to replace treatment. It is to make treatment more tolerable. The patient keeps fighting their illness with a dedicated team focused on their comfort.
Hospice Care Aims for Peace at the End of Life
Hospice care shifts its focus to providing peace, comfort, and dignity. This happens when a cure is no longer the goal. This is not about giving up; it’s about choosing to prioritize the quality of time that is left.
For a patient in Hollister with end-stage heart failure, hospice is a great option. The Central Coast VNA & Hospice team, which includes a Registered Nurse and Hospice Aide, focuses entirely on comfort at home.
The goals of care would be:
- Expert Pain and Symptom Control: Making sure the patient is free from pain or other distressing symptoms.
- Emotional and Spiritual Support: A Social Worker and Chaplain help the patient and family find peace.
- Practical Assistance: Offering help with personal care and giving guidance to family.
The hospice mission is to ensure a person's final months are spent with dignity. The focus moves from adding more days to life to adding more life to the days that are left. Understanding these goals helps families make decisions. Contact Central Coast VNA & Hospice to learn how we align care with your goals.
Who Qualifies for Palliative and Hospice Services
Knowing who is eligible for each type of care is very important. Palliative care and hospice have different qualifications. This helps families find the right support at the right time.
Palliative care has broad eligibility. It is available to any patient at any age and at any stage of a serious illness. This could be cancer, heart failure, COPD, or dementia.
A person can start palliative care when they are diagnosed. They can get it alongside treatments like chemotherapy. The main qualifier is having a serious illness that causes symptoms and stress.
Hospice Care Has More Specific Requirements
Hospice care has more defined rules. It is for people who are nearing the final phase of their illness.
To qualify for hospice, a doctor must certify two things:
- The patient has a terminal illness. This means the condition is not curable.
- The patient likely has a prognosis of six months or less to live if the illness runs its natural course.
The six-month timeframe is a guideline, not a strict limit. Patients can be on hospice longer and be recertified if they still meet the criteria. The main decision is shifting the focus from cure to comfort. You can learn more in our guide on hospice eligibility requirements.
This chart helps show the main question that guides the choice.
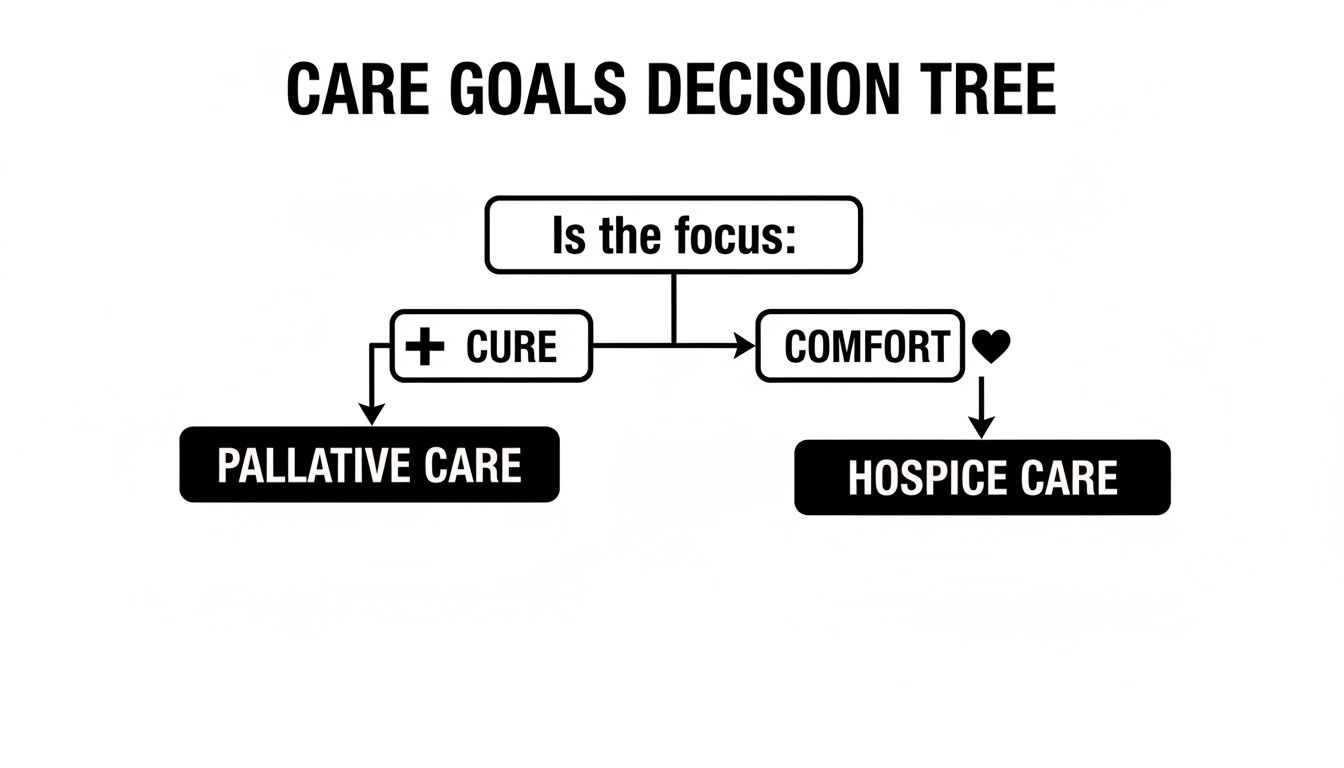
If someone is still seeking a cure, palliative care can help. If the focus is on comfort, hospice is the right path.
Choosing Quality of Life Is Not Giving Up
Many families feel the word "hospice" means giving up. We see it differently. Choosing hospice is a powerful decision to prioritize quality of life, dignity, and peace.
It’s about managing pain and having meaningful moments with loved ones at home. This choice empowers patients to live their final months on their own terms. Hope for a cure may change to hope for a peaceful day or living without pain.
Navigating these choices can feel hard, but you are not alone. Our team at Central Coast VNA & Hospice serves families across Monterey, San Benito, Santa Cruz, and South Santa Clara counties. We can walk you through the options in a compassionate, no-obligation conversation.
Comparing Services Offered By Each Care Team
When choosing between palliative care and hospice, look at the services each team provides. Both focus on comfort, but the teams are structured differently. This helps families understand which is the right fit.
Think of palliative care as an extra layer of support. The team works with your regular doctors to help manage a serious illness while you continue treatment.

Hospice care, on the other hand, provides a complete team for the patient and family. When comfort becomes the main focus, the hospice team manages everything related to the terminal illness.
The Palliative Care Team And Its Services
The palliative care team is designed to add to your medical care, not replace it. The team has special expertise in symptom control and emotional support.
Here’s what to expect from a palliative care team at home:
- Expert Symptom Management: The team is skilled at treating tough symptoms like pain, nausea, and anxiety.
- Support for Medical Decisions: Palliative care specialists help you understand treatment options and talk about your goals.
- Care Coordination: The team connects you, your family, and all your doctors to reduce stress and confusion.
With this support, patients often feel stronger and more in control. This can make it easier to continue curative treatments.
The Hospice Care Team And Its Services
When the focus shifts from cure to comfort, the hospice team offers a more complete approach. For over 74 years, Central Coast VNA & Hospice has provided this nonprofit, mission-driven care.
Our hospice team is a group of professionals who provide physical, emotional, and spiritual support. Hospice is a philosophy of care that honors the whole person. It also provides a strong support system for the family.
Services Offered by Palliative and Hospice Teams
This table compares the support you can expect from our palliative and hospice care programs.
| Service Provided | Palliative Care | Hospice Care |
|---|---|---|
| Symptom & Pain Management | Yes, core service to improve comfort during curative treatment. | Yes, primary focus of all care provided by the team. |
| Medical Decision Support | Yes, helps patients and families align treatment with personal goals. | Yes, guides conversations around end-of-life preferences and comfort. |
| Emotional & Social Support | Provided by palliative specialists and social workers as needed. | Yes, a core component delivered by a dedicated Medical Social Worker. |
| Spiritual Care | Can be arranged upon request. | Yes, a dedicated Chaplain provides non-denominational support. |
| Personal Care (Bathing) | Not typically included; focuses on medical and emotional support. | Yes, a Hospice Aide provides hands-on assistance with daily activities. |
| 24/7 On-Call Nurse | Varies; often coordinated through the primary physician's office. | Yes, a Registered Nurse is always available for urgent needs. |
| Medical Equipment & Meds | Not covered; paid through regular insurance. | Yes, all medications, supplies, and equipment related to the terminal illness are covered by the hospice benefit. |
| Bereavement Support | Not included; focuses on the patient's current care journey. | Yes, grief support is provided to the family for up to 13 months. |
As you can see, the hospice team is designed to meet the complex needs at the end of life. To learn more, read our guide on what to expect from hospice care.
How Insurance and Medicare Cover Care Costs
Money worries should not get in the way of compassionate care. For families on the Central Coast, from Salinas to Santa Cruz, understanding insurance coverage brings peace of mind. The payment for these two types of care is quite different.
Most families are relieved to find that palliative care is covered like other medical services.
How Palliative Care Is Paid For
Palliative care is usually covered by Medicare Part B, Medicaid, and most private insurance plans. It’s treated as a specialist visit, so your plan's deductibles and co-pays will likely apply.
Our team at Central Coast VNA & Hospice can help you understand your coverage. We work with your insurance provider to make sure you get this support without financial stress.
The Comprehensive Medicare Hospice Benefit
Hospice care is covered differently—and often, more completely. The Medicare Hospice Benefit is a plan that covers almost all costs related to the terminal illness. This is an important point for families.
The Medicare Hospice Benefit was designed to remove the financial burden from families at the end of life. It allows everyone to focus on comfort and quality time together.
This all-inclusive benefit covers:
- The full services of the hospice team, including the Registered Nurse, Hospice Aide, Social Worker, and Chaplain.
- All medications needed for pain and symptom management.
- Medical supplies and equipment, such as a hospital bed or oxygen.
- 24/7 on-call support for urgent needs.
For most families, this means no out-of-pocket costs for hospice care. Statistics show that in 2022, only 49.1% of Medicare decedents accessed hospice care, highlighting a need for greater awareness.
For a detailed look at this benefit, you can review our guide on how to pay for hospice care. Our team is always here to help you navigate your coverage.
Navigating Your Journey on the Continuum of Care
A serious illness is a journey with changing needs. A care plan must be flexible enough to change with the person. This is why the continuum of care is so important for families on the Central Coast.

Many families find they start at one point and move to another level of support. That process should feel smooth and reassuring.
From Home Health to Hospice with One Trusted Team
Central Coast VNA & Hospice is the only nonprofit provider in our region offering the full range of home-based care. Our unique model means your family can be supported by one familiar team through every stage. This continuity is a source of great comfort.
Here is a common journey:
- Starting with Home Health: A person in Santa Cruz County is discharged from the hospital. Our home health team, including a skilled Registered Nurse, helps them recover safely at home.
- Transitioning to Palliative Care: Over time, their chronic condition gets worse. They can then transition to our palliative care program for expert symptom control and support.
- Moving to Hospice Care: Eventually, the illness reaches an advanced stage. They can then move smoothly into our hospice program with the same organization they trust.
The greatest benefit of a continuum of care is stability. Instead of searching for new providers, families have a consistent, compassionate partner who knows their story.
Seamless Support for Families in Monterey and San Benito Counties
This seamless approach prevents the stress of starting over with new healthcare teams. For families from Monterey to Hollister, this means one phone number and one trusted resource.
Whether your loved one needs recovery support or end-of-life care, our continuum ensures they get the right care at the right time. By providing home health and hospice care under one roof, we build lasting relationships based on trust.
Frequently Asked Questions About Palliative and Hospice Care
Navigating a serious illness brings many questions. You deserve clear, honest answers. We have gathered some of the most common questions to give you the clarity you need.
1. What is the main difference between palliative care and hospice?
Palliative care can be provided at any stage of a serious illness, alongside curative treatments, to manage symptoms. Hospice care is for patients with a life expectancy of six months or less who are no longer seeking a cure and want to focus on comfort.
2. Can we still see our own doctors?
Yes. With palliative care, our team works with your regular doctors. With hospice care, our hospice physician manages the terminal illness, but you can always stay in touch with your longtime doctor for support.
3. Does choosing hospice mean giving up hope?
Not at all. It means redefining hope. Hope shifts from a cure to goals like living without pain, having meaningful conversations, and enjoying quality time with family.
4. Can a patient stop hospice care?
Yes. A patient can leave hospice care at any time if their condition improves or they decide to seek curative treatment again. They can return to hospice later if they still meet the eligibility criteria.
5. Where is care provided?
Both palliative and hospice care are most often provided wherever the patient calls home. This can be a private home, assisted living facility, or nursing home. Our teams at Central Coast VNA & Hospice serve Monterey County, San Benito County, Santa Cruz County, and South Santa Clara County.
The journey of a serious illness is challenging, but you don't have to navigate it alone. With over 74 years of nonprofit service to the Central Coast, Central Coast VNA & Hospice provides a complete continuum of care—from home health to palliative to hospice—all with one compassionate, trusted team. If you are not sure what care is needed, our team will help guide you.
Contact us today to start a no-obligation conversation about what matters most to your family. Learn more about our mission and services at https://ccvna.com.
A Guide to Aging in Place Care Services on the Central Coast
Most people want to spend their later years in their own home. Aging in place is the term for making that wish a reality. It means having the right support to live safely and independently.
Think of it as gaining a team to help you live life on your terms. Professional aging in place services bring expert support to your home. This helps turn your preference into a long-term plan.
A Proactive Choice for a Better Future
Many families wait for a crisis to think about home-based care. This could be a fall, a sudden illness, or a hospital stay. But the best outcomes happen when planning is done ahead of time.
Exploring your options early lets you create a flexible plan. It makes any future transition smooth and stress-free. This approach gives peace of mind to you and your family.
The goal of aging in place isn't just about staying at home. It's about thriving at home. It is about keeping your dignity and freedom in a familiar place.
The Continuum of Care: A Pathway for Every Need
Understanding the continuum of care is key to aging in place. This concept ensures that as your health needs change, your care can change too. You can often get this support without leaving your house.
This seamless path is designed to meet you where you are. It typically includes:
- Home Health: This is skilled medical care from Registered Nurses and therapists. It's perfect for recovery after surgery or managing a new diagnosis.
- Palliative Care: This is an extra layer of support. It focuses on relieving symptoms and stress from a serious illness.
- Hospice Care: When the focus shifts to comfort, hospice provides compassionate care. It supports both the patient and their family.
Central Coast VNA & Hospice is a nonprofit with over 74 years of experience. We provide this entire continuum of care. We serve communities in Monterey County, San Benito County, Santa Cruz County, and South Santa Clara County.
Our mission is to ensure you get the right care at the right time. Learning about in-home care for seniors is a great first step. It helps secure a comfortable and independent future at home.
Understanding Your Home Based Clinical Care Options
Figuring out home based clinical care can seem complex. But it is often more straightforward than it appears. Professional services fall into three main categories.
Each category gives a specific kind of support. Understanding these options helps you build a care plan with confidence. Central Coast VNA & Hospice offers this seamless care.
This allows patients in Monterey County and nearby areas to move between levels of support. They can do this from the comfort of their home. It is all about having the right team by your side.
This diagram shows the principles that guide great aging-in-place care.

The goal is to build a foundation of safety and comfort. This makes long-term independence possible.
Comparing Home Health, Palliative, and Hospice Care
Let's break down how these services differ. Each one plays a unique role in a person’s care journey.
| Service Type | Primary Goal | Who It's For | Example Scenario |
|---|---|---|---|
| Home Health Care | Recovery & Rehabilitation | Patients recovering from an illness, surgery, or injury who need skilled medical care to get back on their feet. | After knee replacement surgery, a Physical Therapist visits to help with exercises and a Registered Nurse checks the incision site. |
| Palliative Care | Symptom Management & Quality of Life | Patients living with a serious, chronic illness who need help managing symptoms and stress, often alongside curative treatment. | A patient undergoing chemotherapy receives care to manage nausea and fatigue, helping them tolerate their treatments better. |
| Hospice Care | Comfort & Dignity | Patients with a terminal illness (typically a prognosis of 6 months or less) when curative treatment is no longer an option or desired. | In the final months of life, a team provides pain management, emotional support, and spiritual care to ensure peace and comfort. |
Each service is designed to meet you where you are. It provides the exact level of clinical support you need.
Home Health Care for Recovery and Rehabilitation
Home Health Care is skilled medical support ordered by a doctor. It helps someone recover from an illness, injury, or surgery. This care is from licensed professionals like Registered Nurses and Physical Therapists.
For example, someone home from the hospital after knee surgery needs help. A Physical Therapist would visit to rebuild strength. A Registered Nurse might also visit to manage wound care and give medications.
The main goal is always rehabilitation and a return to independence. You can learn more about our specific https://ccvna.com/home-health-care-services/ and how they support recovery.
Palliative Care for Symptom Management
Palliative Care is for people with a serious illness. Its purpose is to relieve symptoms and stress. It improves quality of life for both the patient and their family.
Many people think palliative care is the same as end-of-life care. This is a common misunderstanding.
Palliative Care can be provided at any age and at any stage of a serious illness. It can be delivered right alongside curative treatment.
Imagine someone going through cancer treatment. Their palliative care team focuses on managing side effects like pain and nausea. This support helps them feel stronger and continue with their treatments.
Hospice Care for Comfort and Dignity
Hospice Care is for people nearing the end of their life. When treatments to cure an illness stop, the focus shifts to comfort. Hospice helps a person’s final months be as peaceful as possible.
The hospice team includes a doctor, Registered Nurses, Hospice Aides, and Chaplains. They work together to manage pain and other symptoms. They also provide emotional and spiritual support to the family.
For over 74 years, Central Coast VNA & Hospice has served families. We provide this care in San Benito County, Santa Cruz County, and South Santa Clara County.
Technology is also making care more accessible. The rise of comprehensive telehealth services means expert help can happen from your living room. The desire to stay home is a powerful trend worldwide.
The Real Benefits Of Receiving Professional Care At Home
Bringing professional clinical care into the home is a personal choice. It is often rooted in a desire for comfort and better health. The true advantages of aging in place care services go far beyond convenience.
This approach creates a supportive environment where people can thrive. Care is shaped around an individual's needs and preferences. It is like having a clinical plan designed just for you.

Promoting Better Health And Independence
Home-based care has a big impact on a person’s health and independence. Healing in a familiar setting reduces stress. This often leads to a faster and more comfortable recovery.
Staying home also lowers the risk of exposure to infections. This is a key benefit for anyone with a weaker immune system. Our focus at Central Coast VNA & Hospice is on creating a safe healing space.
We work hard at reducing hospital readmissions on the Central Coast.
Professional home health care empowers individuals by helping them regain strength and manage their conditions effectively. It fosters a profound sense of autonomy.
This desire to stay home is very common. According to the AARP, nearly 90% of adults over 65 want to stay in their current home as they age (AARP, 2021). Home-based care is becoming the new standard.
Providing Peace Of Mind For The Whole Family
Home care helps the entire family. Knowing your loved one gets expert attention brings great relief. It lets family members focus on providing love and emotional support.
This support system also helps prevent family member burnout. Professional respite care services offer needed breaks. This ensures family can recharge and continue their supportive roles.
For over 74 years, Central Coast VNA & Hospice has supported families. We serve people across Monterey County, San Benito County, and nearby areas. Our nonprofit, mission-driven approach means every decision puts the patient first.
How To Proactively Plan For Aging In Place
Successful aging in place is the result of careful planning. Waiting for a health crisis can lead to stress and fewer choices. Taking steps now empowers you and your family.
Think of it as creating a roadmap for the future. This approach gives you time to explore options calmly. That preparation brings peace of mind to everyone.

Assessing Current And Future Needs
The first step is a conversation about current abilities. It is about finding areas where extra support could make a difference. Looking at Activities of Daily Living (ADLs) can help.
- Activities of Daily Living (ADLs): These are basic self-care tasks. Think about bathing, dressing, eating, and moving around.
- Instrumental Activities of Daily Living (IADLs): These are more complex tasks. This includes managing money, making meals, and taking medicines.
Thinking through these tasks helps clarify what support might be needed. It also opens the door to discussing "what if" scenarios.
Evaluating Home Safety And Modifications
A safe home is the foundation of aging in place. Simple changes can greatly reduce risks like falls. Over one in four older adults has a fall each year, but many are preventable.
Start by walking through the home to spot common hazards. Look for loose rugs, poor lighting, or cluttered paths. These are often easy fixes with a big impact.
A key part of proactive planning is transforming the living space from a potential obstacle course into a safe haven. Small changes are powerful tools for preserving independence.
Our skilled clinicians at Central Coast VNA & Hospice can help. Our Physical and Occupational Therapists can do a home safety check. You can also start by reviewing our guide on preventing falls in the home.
Navigating Financial And Insurance Options
Understanding how to pay for care is a critical piece of the puzzle. The good news is that many professional aging in place care services are covered. This is especially true when a doctor says they are medically necessary.
Here’s a general overview of what that looks like:
- Medicare: Medicare Part A and B often cover home health services. This is for patients who are "homebound" and need skilled care.
- Private Insurance: Many private health insurance plans also offer benefits. Contact your provider to understand your policy.
Our team at Central Coast VNA & Hospice is here to help families. We serve Monterey County, San Benito County, and other areas. We can help you check coverage and understand your benefits.
Getting Started With Central Coast VNA & Hospice
Taking that first step is simple. Anyone can make a referral to us. This includes a patient, a family member, or a doctor.
Once you reach out, we talk with your physician. We get the necessary orders for care. Then, we schedule a visit to create a personal care plan.
Contact us today to begin the conversation.
Your Trusted Partner For Aging In Place On The Central Coast
Choosing a partner for aging in place care is a personal decision. A local, nonprofit provider offers a different path. For over 74 years, Central Coast VNA & Hospice has served our community.
Our mission is to serve people, not to generate profit. Our roots are deep in Monterey County, San Benito County, Santa Cruz County, and South Santa Clara County. We are your neighbors.
A Legacy Of Compassionate, Connected Care
As a nonprofit, our focus is on delivering exceptional care. We reinvest our resources back into patient services. This allows us to offer a seamless continuum of care.
This integrated approach means you get consistent, high-quality support. You won’t have to learn a new system. Your team adapts right alongside you.
Learn more about why Central Coast VNA is the best choice for home health care.
When you choose a nonprofit provider with deep community roots, you are choosing a partner. Their success is measured by your family’s well-being.
Innovative Models For Modern Needs
The world of home-based care is always improving. We stay at the forefront of that progress. There is a clear shift toward services that help people stay at home.
You can discover more insights about these aging service trends. Central Coast VNA & Hospice embodies this same spirit. Our long history is built on meeting the modern needs of our community.
Start The Conversation Today
Planning for the future can feel overwhelming. You don’t have to do it alone. Our compassionate team is here to answer your questions.
We can walk you through your options. Let us help you create a plan that brings peace of mind.
Contact us today to speak with a member of our team. Let us show you how our legacy of care can support your goal of living safely at home.
Frequently Asked Questions About Aging in Place Care
It is natural to have questions when exploring professional care at home. Getting clear answers is the first step toward feeling confident. Here are some common questions we hear from families.
1. What does "aging in place" mean?
Aging in place means living in your own home safely and independently as you get older. It involves having the right support services to manage health needs. This allows you to stay in a familiar environment.
2. How do I know which home care service is right for me?
The right service depends on your main health goal. Home Health is for recovery after an illness or surgery. Palliative Care helps manage symptoms of a serious illness. Hospice Care provides comfort when a cure is no longer the focus.
3. Are these services covered by Medicare?
Yes, in many cases, they are. Medicare Part A and B often cover Home Health services if a doctor orders them. The Medicare Hospice Benefit provides comprehensive coverage for end-of-life care.
4. What is the difference between home care and Home Health Care?
"Home care" is usually non-medical help, like meal prep or companionship. "Home Health Care" is skilled medical care from licensed clinicians. Central Coast VNA & Hospice provides Home Health Care.
5. How do we get started with Central Coast VNA & Hospice?
Getting started is simple. Anyone—a patient, family member, or doctor—can contact us. We will then coordinate with your physician to create a personalized care plan.
6. What are the first steps to make a home safer?
Start by removing trip hazards like loose rugs and cords. Improve lighting in hallways and bathrooms. Installing grab bars in the shower is another easy change that makes a big difference.
Planning for the future can feel overwhelming, but you do not have to do it alone. The compassionate team at Central Coast VNA & Hospice is here to answer your questions. Contact us today to learn how our 74+ years of nonprofit service can support your family's goal of living safely and independently at home.
Inside Hospice Care at Home: A Family’s Guide
When facing end-of-life decisions, many families feel overwhelmed. Choosing hospice care at home is not about giving up. It is a compassionate choice to prioritize comfort, dignity, and quality of life.
This decision allows your loved one to stay in the familiar peace of their own home. It brings an entire support system directly to your family.
What Hospice Care at Home Really Means
Starting hospice care shifts the focus from curing an illness to caring for the whole person. It means bringing a specialized team into the home to manage symptoms and provide support. This frees you up to share more meaningful moments with your loved one.
For over 74 years, Central Coast VNA & Hospice has served families with this compassionate care model. As a trusted local nonprofit, we bring comfort to homes across Monterey County, San Benito County, Santa Cruz County, and South Santa Clara County.
A Philosophy of Comfort and Support
Hospice at home is more than a service; it is a philosophy. It creates a complete circle of support for both the patient and the family. Every physical, emotional, and spiritual need is met with dignity.
This support system includes:
- Expert Symptom Management: A dedicated Registered Nurse works with your loved one’s doctor to control pain and other symptoms.
- Emotional and Spiritual Guidance: Our Social Workers and Chaplains help your family find peace, respecting all personal beliefs.
- Practical Assistance: Hospice Aides provide gentle, hands-on help with personal tasks like bathing and dressing.
- Comprehensive Coordination: We handle the delivery of medical equipment and medications right to your home, reducing your stress.
This table gives a clear overview of what in-home hospice care includes.
Hospice Care at Home At a Glance
| Care Aspect | What It Means for Your Family |
|---|---|
| Location of Care | Your loved one remains in the comfort and familiarity of their own home. |
| Medical Team | A skilled team, including a Registered Nurse, Social Worker, and Hospice Aide, visits regularly. |
| Symptom Control | We focus on managing pain, nausea, anxiety, and other symptoms to maximize comfort. |
| Emotional Support | Counselors and Chaplains are available for both the patient and family members. |
| Medication & Equipment | All necessary medications, supplies, and equipment are delivered to your home. |
| 24/7 On-Call Help | A Registered Nurse is always available by phone to answer questions or provide guidance. |
| Family Caregiver Support | We provide education, respite, and emotional support to help you in your role. |
| Bereavement Care | Grief support is offered to the family for up to 13 months after a loved one's passing. |
Hospice is a holistic system designed to support everyone involved. It honors the final chapter of life with peace and dignity.
Choosing hospice at home is not just a decision about location; it's about how the final chapter of life will feel. It’s about the familiar view from a window, the comfort of a favorite chair, and the presence of family—all supported by a team of caring professionals.
With Central Coast VNA & Hospice, your family is never alone. Our team is on-call 24/7 for answers and reassurance. This ensures your loved one’s final days are as peaceful as possible. You can learn more about what hospice care is and how it helps families like yours.
The First Steps: How Hospice Begins at Home
One of the biggest questions families ask is, “How do we start?” The process is gentle and reassuring. It begins with a simple conversation.
A referral for hospice care can come from a doctor, a hospital, or a family member. Your first call is a warm, confidential conversation to ask questions.
Your First Call with Our Team
When you reach out, our team listens carefully. We ask about your loved one’s health, comfort goals, and worries. This call gives you a clear picture of how we can help.
There is no pressure or obligation. Our only goal is to provide the information you need. To help guide your thoughts, you can learn more about the right time to call hospice.
The infographic below captures the philosophy behind starting hospice. It's about reframing care, choosing comfort, and getting support.
Starting hospice is a positive choice to prioritize quality of life. It brings a dedicated care team right into your home.
The First Visit: A Conversation About Comfort
After the call, we schedule our first visit. A compassionate Central Coast VNA Registered Nurse comes to your home. This is a heartfelt conversation about your loved one’s wishes.
Our Registered Nurse will listen to you and your family. This conversation is the foundation of the personalized care plan we build together.
Getting Everything in Place
One of the greatest reliefs for families is that we handle all the logistics. Central Coast VNA & Hospice coordinates everything needed for care at home. This reduces stress for the entire family.
We take care of it all:
- Medical Equipment: If your loved one needs a hospital bed or oxygen, we arrange delivery to your door.
- Medications: We work with your pharmacy to get all hospice-related medications delivered.
- Supplies: We provide necessary medical supplies, from bandages to personal care items.
Our team ensures your home is fully equipped for comfort from day one. This allows your family to focus on spending quality time together.
Your Hospice Team: The Caring Faces Who Visit Your Home
Inviting a care team into your home is a big step. At Central Coast VNA & Hospice, our interdisciplinary team members are compassionate local experts. They work together to meet your loved one’s physical, emotional, and spiritual needs.
The strength of hospice care at home lies in this teamwork. Let's introduce the caring faces you will get to know.

The Registered Nurse
The Registered Nurse (RN) is the central coordinator of your loved one’s care. During visits, the RN assesses symptoms, manages medications, and communicates with your family’s doctor. They are your main point of contact and are available 24/7 for on-call support.
The RN also educates your family. They teach you what to expect and how to provide comfort. Their steady, reassuring presence makes a difference during uncertain times.
The Hospice Aide
Our Hospice Aides are the heart of hands-on comfort care. They assist with personal tasks while preserving your loved one's dignity. Their gentle support helps your loved one feel clean and comfortable.
Hospice Aides provide assistance with daily routines like:
- Bathing, dressing, and grooming
- Changing bed linens
- Offering light help with moving in bed
Their warm companionship brings relief to patients and families. You can learn more about the responsibilities of a Hospice Aide.
Hospice is not just a service; it's a team of people who show up for your family. It’s the Registered Nurse who listens, the Hospice Aide who offers a gentle touch, and the Social Worker who helps you find the right words.
The Social Worker and Chaplain
End-of-life care is about more than physical comfort. Our Medical Social Workers provide crucial emotional support for the entire family. They can help you navigate difficult conversations and the stress of this journey.
A Social Worker also connects you with practical community resources. They can guide you with advance care planning and financial questions.
Our Chaplains offer spiritual care that respects all beliefs and backgrounds. They provide a comforting presence and help your loved one and family find peace. This support is available to everyone, regardless of their spiritual views.
Our Dedicated Volunteers
Our trained Volunteers are an essential part of the team. They offer the simple gift of companionship. A volunteer might sit and read with your loved one, giving you a much-needed break.
This entire team works in harmony. Their visits are coordinated to provide seamless support without feeling intrusive.
A Typical Day: Managing Comfort at Home
Families often wonder what daily life will look like with hospice. A common worry is, “Will our home turn into a hospital?” The answer is no. The goal is to create a peaceful, familiar environment.
The rhythm of at-home hospice is a gentle flow of support. We create a coordinated schedule of visits that respects your family’s privacy.
The Rhythm of Care Visits
The frequency of visits is based on your loved one’s needs. In the beginning, the Registered Nurse may visit once or twice a week. Visits can become more frequent if needs change.
A Hospice Aide might visit several times a week for personal care. The Social Worker and Chaplain schedule visits based on your family’s desire for support.
Managing Symptoms for a Peaceful Day
A central goal of hospice is making sure your loved one is free from pain. Our Registered Nurses are experts in symptom management. They work with your doctor to find the right balance of medications and therapies.
Effective symptom management often includes:
- Controlling Pain: We use medications to keep pain at a comfortable level.
- Easing Anxiety: We can provide medications and calming techniques to reduce restlessness.
- Addressing Other Discomforts: We also manage symptoms like nausea or difficulty breathing.
Our team arranges for all necessary medical equipment and medications to be delivered. This removes a huge weight from your shoulders. This process is detailed in our guide to inside hospice care at home.
The Family’s Role in Daily Comfort
You provide the love and familiarity that no one else can. Our job is to support you in that role, never to replace you.
We empower you by teaching practical skills, like how to:
- Recognize subtle signs of discomfort.
- Administer medications safely between nurse visits.
- Provide simple comfort measures, like repositioning pillows.
Your presence is often the most powerful comfort of all. Simply sitting with your loved one, reading a book, or sharing quiet moments can bring immense peace. We are here to manage the medical complexities so you can focus on being present.
Our team actively works to prevent family burnout. With over 74 years of local service, Central Coast VNA & Hospice is your partner every step of the way.
Emotional and Spiritual Support for the Whole Family
Hospice care is about more than physical symptoms. It focuses on caring for the whole person and the entire family. The end-of-life journey is filled with complex emotions, and our team ensures no one walks this path alone.
We provide deep emotional and spiritual resources. This holistic approach brings comfort not just to the body, but to the heart and mind as well.

Guiding You Through Difficult Conversations
Our Medical Social Workers are compassionate guides. They create a safe space for you to talk about your fears and challenges. They can help with tough family conversations, making sure everyone feels heard.
A Social Worker’s support is both emotional and practical. They can help with:
- Navigating complex family dynamics and improving communication.
- Coping with the emotional toll of this journey.
- Connecting you to community resources for extra support.
- Assisting with advance care planning.
Our team is here to provide the deep compassion needed during this time. You can learn more about what emotional support truly means for families.
Finding Peace and Meaning with Spiritual Care
Spiritual well-being is a deeply personal part of this journey. Our Chaplains offer gentle, non-denominational spiritual support. They listen without judgment and provide a comforting presence when it’s needed most.
This care is not about religion; it is about honoring the human spirit. Our Chaplains meet you where you are, helping you find peace. You can learn more about our approach to spiritual care in hospice.
Our Commitment Continues with Bereavement Support
Our promise to care for your family does not end when your loved one passes away. Grief is a long and personal journey. Central Coast VNA & Hospice provides dedicated bereavement support for up to 13 months.
We believe that caring for a family means supporting them through the entire arc of their experience—before, during, and long after their loved one’s passing. Our bereavement services are a testament to that enduring commitment.
This support can include individual counseling, support groups, and resources. We are here for you, offering a steady hand as you begin to heal.
Frequently Asked Questions About Hospice Care at Home
Is hospice care only for the last few days of life?
No, this is a common myth. According to the National Hospice and Palliative Care Organization (NHPCO), hospice is for anyone with a life-limiting illness and a prognosis of six months or less if the illness runs its natural course. Starting early provides more time for symptom management and relationship-building with the care team.
Will we still see our regular doctor?
Yes, absolutely. Your loved one's primary doctor remains a key part of the care team. Our team at Central Coast VNA & Hospice works closely with them to ensure the care plan aligns with their medical guidance.
How is hospice at home paid for?
Hospice care is a comprehensive benefit fully covered by Medicare, Medi-Cal, and most private insurance plans. This coverage typically includes visits from the care team, medications, and medical equipment related to the hospice diagnosis. Our team can help you understand your specific coverage.
What happens if there is a crisis in the middle of the night?
You are never alone. Central Coast VNA & Hospice provides 24/7 on-call support from a Registered Nurse. You can call anytime, and a Registered Nurse will assist you over the phone or make a home visit if needed, preventing stressful trips to the emergency room.
What does the first hospice visit at home feel like?
The first visit is a gentle, compassionate conversation, not a clinical assessment. A Registered Nurse will sit down with your family to listen to your loved one's wishes, understand their symptoms, and learn what a "good day" looks like for them. This discussion forms the basis of a personalized care plan.
Does choosing hospice mean we are giving up hope?
Not at all. It redefines hope. Hope shifts from a cure to what is most meaningful right now. It becomes hope for a day without pain, for quiet family moments, and for a peaceful, dignified journey.
At Central Coast VNA & Hospice, we are here to walk alongside you with compassion and expertise. If you have more questions or want to talk about your family’s situation, we invite you to have a personal, no-obligation conversation with our team.
Contact us today to learn how our 74+ years of nonprofit service to the Central Coast community can support your family. https://ccvna.com










