Hospice at Home: A Compassionate Guide
Hospice at home is a special kind of care. It allows someone with a life-limiting illness to spend their final months where they feel most comfortable—their own home. It brings a team with medical, emotional, and spiritual support directly to the patient. The focus is on managing symptoms and making sure quality of life is the top priority.
This approach is about dignity and peace, not treatments that are no longer working.
Shifting the Focus to Comfort and Dignity

Many families in Monterey County worry that choosing hospice means giving up. The truth is the opposite.
Hospice at home is about redefining hope. It is a choice to shift focus from finding a cure to living each day to its fullest. This means being surrounded by familiar comforts and the people who matter most.
This decision empowers patients to stay in control of their journey. The goal is simple: to be as comfortable and pain-free as possible. This creates space for meaningful moments with loved ones.
A Mission of Compassionate Community Care
For over 74 years, Central Coast VNA & Hospice has been a trusted, nonprofit partner for families. Our mission is to provide expert, compassionate care that honors the wishes of every person we serve. We are a community-based organization, deeply rooted in Monterey County, San Benito County, Santa Cruz County, and South Santa Clara County.
We believe end-of-life care should be filled with comfort, respect, and peace. Our dedicated team works with the patient and the entire family. We provide a circle of support for physical, emotional, and spiritual needs.
More people want this kind of care. According to the National Hospice and Palliative Care Organization (NHPCO), over 1.72 million Medicare beneficiaries received hospice services in 2020 (NHPCO, 2021). This trend shows a powerful desire for patient-centered care at home.
Understanding the Hospice Journey
Making the decision to start hospice at home is a big one. It’s natural to have questions. Our professional team is here to walk you through the process with clear guidance. We handle the medical details so you can focus on what’s important: sharing love and creating memories.
To get a better sense of the overall journey, this general guide on what to expect from hospice care can be a helpful resource.
At Central Coast VNA & Hospice, we support every family with professionalism and warmth. We make sure your loved one’s final chapter is lived with dignity.
The Comforts and Benefits of In-Home Care

Most people want to spend their final chapter at home for a reason. Choosing hospice at home offers a level of comfort that a hospital cannot match. Being surrounded by photos, a favorite chair, or a familiar window makes a big difference.
This sense of normalcy helps preserve a person's independence and dignity. It allows life to continue with its familiar rhythms. That feeling of peace is the foundation of quality end-of-life care.
Keeping Families Together
One of the greatest gifts of in-home hospice is being together without the stress of hospital visits. Strict visiting hours and long commutes are a heavy burden. When care comes to you, families can share quiet, spontaneous moments that mean so much.
It creates space for sharing memories or just holding a hand. The experience becomes more personal and intimate. The focus shifts from hospital rules back to love and connection.
By bringing expert medical support into the home, Central Coast VNA & Hospice allows families to set aside the role of medical manager. They can return to being a spouse, a child, or a grandchild. We handle the details so you can focus on love.
This is a growing trend. Recent Medicare data shows Routine Home Care is the most common level of hospice service. The number of hospice days provided at home is rising each year.
Empowering Families with Expert Support
It’s normal to feel overwhelmed by a loved one’s medical needs. That’s why our team at Central Coast VNA & Hospice empowers families with education and support. Our Registered Nurses and Hospice Aides are always there to answer questions and provide clear guidance.
We teach family members how to help with daily tasks and what to watch for. This partnership reduces anxiety. It builds a circle of trust for both the patient and their loved ones.
The Practical Advantages of Home-Based Care
Beyond the emotional side, hospice at home has practical benefits. It is designed to reduce stressful trips to the emergency room or hospital.
Here are a few key advantages:
- Personalized Care Plans: Care is built around your loved one’s specific needs and wishes at home.
- Reduced Financial Strain: Hospice is a fully covered benefit under Medicare and most private insurance.
- Consistent Care Team: The same dedicated team provides care, building a trusting relationship with the patient and family.
We manage symptoms and provide 24/7 on-call support. This helps keep things stable and prevent crises. To learn more, check out our article on the benefits of home health care. This approach gives everyone much-needed peace of mind.
Meet Your Compassionate Hospice Care Team
When you choose hospice at home, you are not alone. A dedicated team from Central Coast VNA & Hospice provides a circle of support. We ensure every need—physical, emotional, and spiritual—is met with expertise and kindness.
Think of it as having a group of specialists focused on one goal. That goal is maximizing your loved one's comfort and honoring their wishes. This team-based approach allows families in our service area to feel completely supported.
Your Hospice at Home Care Team Roles
The strength of hospice at home comes from its team spirit. Our professionals work together to create a seamless care plan. This plan adapts as your family's needs change. This model relieves burdens on family and brings you peace of mind.
Here’s a look at the professionals on your core support system.
| Team Member | Primary Role and Responsibilities |
|---|---|
| Registered Nurse (RN) | The cornerstone of medical care. Manages pain and symptoms, makes regular home visits, coordinates with the physician, and educates the family on care techniques. |
| Hospice Aide | A certified professional providing essential, hands-on personal care. Assists with bathing, dressing, and grooming to help your loved one maintain comfort and dignity. |
| Medical Social Worker | Offers counseling for emotional and practical challenges. Helps with advance care planning and connects families to community resources. |
| Chaplain | Provides spiritual care to people of all faiths, beliefs, and those with no religious affiliation. Offers a comforting presence to help navigate spiritual questions and find peace. |
A hospice physician or your loved one's own doctor will oversee the medical plan. Trained volunteers also play a key part by offering companionship. This gives family members a much-needed break.
This infographic breaks down the primary areas of focus for the hospice at home team.
As you can see, medical monitoring, pain management, and emotional counseling are the three pillars of our hospice support.
The Vital Role of the Hospice Aide
While every team member is essential, the Hospice Aide often becomes a familiar and comforting face. They provide the gentle, hands-on care that makes a difference in a patient's daily comfort.
Their work is both practical and deeply personal. They might help with meals or simply be there to listen.
This support allows family members to shift their focus from physical tasks back to what matters most. To learn more, you can read about the responsibilities of a Hospice Aide on our website.
Comprehensive Services Included in Home Hospice

When families in Monterey County choose hospice at home, they get more than medical support. Central Coast VNA & Hospice delivers a complete circle of care. We bring comfort, dignity, and peace right into the home.
This coordinated approach makes sure the patient and their family have everything they need. By handling the practical details, we lift a heavy weight off your shoulders. This frees you to focus on being present for one another.
Expert Medical Care and Symptom Management
The main goal of home hospice is to keep your loved one comfortable and pain-free. Our Registered Nurses are experts in managing symptoms that come with a life-limiting illness. These include pain, shortness of breath, anxiety, and fatigue.
Regular nursing visits are the foundation of our care. Nurses check the patient's condition, give medications, and adjust the care plan as needed. They also provide key education to the family so you feel confident.
Hospice care is about actively managing symptoms. This gives your loved one the best possible quality of life for every single day they have. This proactive approach helps prevent crises and reduces trips to the hospital.
Personal Support and Daily Assistance
Maintaining personal dignity is critical. Our certified Hospice Aides provide gentle, hands-on help with daily activities.
This support includes help with:
- Bathing and grooming: Making sure your loved one feels clean and refreshed.
- Dressing: Providing a helping hand to make this daily routine easier.
- Light meal preparation: Helping with nutrition when appetite is low.
- Mobility: Assisting with moving safely around the home.
This one-on-one care not only supports the patient. It also gives family members a much-needed break.
Emotional and Spiritual Guidance for the Whole Family
A serious illness affects everyone. Our Medical Social Workers and Chaplains support the entire family. They help you navigate the emotional and spiritual challenges of this journey.
Our Medical Social Workers offer counseling and help with advance care planning. They create a safe space to talk through fears or concerns.
Our Chaplains provide non-denominational spiritual support that honors all beliefs. They are great listeners who bring a calming presence. They help patients and families find peace and meaning.
Medical Equipment and Supplies
Having the right equipment makes a home a safe place for care. As a patient of Central Coast VNA & Hospice, all needed medical equipment and supplies are delivered to your door.
This typically includes items like:
- A hospital bed to improve comfort.
- An oxygen concentrator for breathing support.
- A wheelchair or walker to help with mobility.
- Essential medical supplies like bandages and catheters.
We take care of all the logistics for equipment and supplies. This removes another layer of stress for families. You can explore our detailed breakdown of hospice care services. This all-inclusive support ensures you can focus on your loved one.
Understanding Hospice Eligibility and Costs
When families look into hospice at home, two questions often come up first. "Does my loved one qualify?" and "How will we pay for this?" These are normal concerns, and the answers are often reassuring.
Getting a clear picture of the requirements can lift a huge weight off your shoulders. Our goal is to give families in Monterey County and nearby areas the confidence to make informed decisions.
Who Is Eligible for Hospice Care
Hospice care is for someone with a life-limiting illness. The focus shifts from curing the disease to comfort and quality of life. The general guideline is a doctor's prognosis that the person has six months or less to live if the illness runs its natural course.
But it's not just about a date on a calendar. It’s about what a person needs and wants right now.
Common conditions for hospice eligibility include:
- Advanced-stage cancer
- End-stage heart, lung, or kidney disease
- Late-stage Alzheimer's disease or other dementias
- Conditions like ALS or Parkinson's disease
Criteria can vary by location. It can help to look into state-specific eligibility requirements. A simple conversation with us can clarify if hospice is the right path for your family.
How Hospice Care Is Paid For
This part brings most families a huge sense of relief. The cost of hospice care is rarely a financial burden. For most patients, hospice is a fully covered benefit.
Hospice is a benefit covered 100% by Medicare Part A. This includes all services, medications, supplies, and medical equipment related to the terminal illness. There are no deductibles or copayments for the patient.
This full coverage is there to remove financial stress. Beyond Medicare, hospice is also covered by:
- Medi-Cal (California's Medicaid program)
- The Department of Veterans Affairs (VA)
- Most private insurance plans
You can get more details in our guide on how to pay for hospice care. Our team is here to help you navigate your specific coverage.
Our Nonprofit Mission to Serve the Central Coast
As a nonprofit that’s been part of this community for over 74 years, Central Coast VNA & Hospice operates on a simple promise. We believe everyone deserves compassionate end-of-life care, no matter their financial situation. We are committed to providing hospice at home to every eligible person in our service area.
This commitment reflects a growing understanding of how vital this care is. More people recognize the value of comfort-focused care.
Because of our nonprofit status, a person's ability to pay will never get in the way of receiving dignified, expert care.
Starting the Conversation About Hospice Care
Bringing up hospice care can feel tough. But it’s not about giving up. It’s a discussion rooted in love and courage. It is a way to honor your loved one’s wishes and ensure their final chapter is lived with dignity and comfort.
A gentle way to begin is by focusing on their goals. Try asking questions like, "What is most important to you right now?" This simple shift puts them back in control. It centers the talk on their quality of life, not their illness.
Finding the Right Words and Time
Choose a quiet, calm moment when you won't be rushed. This is not a conversation to have with one eye on the clock. Your role is to listen more than you talk.
Involving their physician is another helpful step. A doctor can offer a clear medical perspective. This often helps the entire family get on the same page.
Approaching this conversation with empathy transforms it. It becomes a meaningful opportunity to connect and reaffirm your commitment to their well-being.
We Are Here to Help You Begin
You don’t have to have this conversation alone. Central Coast VNA & Hospice offers no-obligation consultations for families. We serve Monterey County, San Benito County, Santa Cruz County, and South Santa Clara County. Our compassionate team is here to answer your questions.
Taking this first step empowers your family with knowledge and support. Contact us today to learn how we can support your family and help you begin this journey with peace of mind.
Frequently Asked Questions About Hospice at Home
When a loved one faces a life-limiting illness, it’s normal to have questions. Getting clear answers is the first step toward feeling more in control. Below are answers to some of the most common questions we hear.
When is the right time to consider hospice care?
The best time to explore hospice is when care goals shift from curing an illness to maximizing comfort. This often begins when a doctor estimates a prognosis of six months or less. Starting hospice early provides months of meaningful support for the patient and family.
Can my loved one still see their own doctor?
Yes, absolutely. A patient's trusted physician is a vital part of their care. We encourage them to stay as involved as they’d like. Our team works hand-in-hand with your family’s doctor to ensure the care plan is seamless.
What happens if their condition improves?
It’s not uncommon for a person's health to stabilize with hospice care. If a patient's condition improves, they can be discharged from hospice at any time. They can resume curative treatments, and the door to hospice is always open if needed later.
Does choosing hospice mean giving up hope?
Not at all. Choosing hospice is about redefining hope. The focus shifts from hope for a cure to hope for comfort, dignity, and making the most of the time you have together. It’s hope for a gentle journey filled with meaningful moments.
What is the family's role in hospice at home?
The family is the heart of the hospice team. Our professional team handles medical tasks, but the family provides irreplaceable love and comfort. We support you with training and resources, so you can focus on simply being a spouse, child, or friend again.
At Central Coast VNA & Hospice, we are committed to guiding families in Monterey County, San Benito County, Santa Cruz County, and South Santa Clara County with compassion and expertise. If you have more questions or want to learn how our services can support your family, we are here to help.
Contact us today to learn more about our compassionate hospice care.
A Guide to Safe Recovery: Discharge Planning from Hospital
Leaving the hospital is a big step. But a safe recovery starts on your first day there. Discharge planning from hospital is a roadmap for your transition back home. It makes sure you have the support you need to heal well and avoid another hospital visit.
Why a Solid Discharge Plan Matters from Day One

Thinking about going home might seem early when you've just arrived at the hospital. But the best discharge plans are made from the very first day. When we start early, a stressful event becomes a calm, structured process for patients and their families.
This early approach gives the hospital team a head start. We get a full picture of your home life, your support system, and what you might need after you leave. This gives everyone time to arrange important services, like follow-up appointments or skilled in-home care.
The Power of Early Conversations
When discharge planning starts early, there are no last-minute surprises. A key part of this is setting an Estimated Date of Discharge (EDD) soon after you arrive. This simple step gives you and your family a clear timeline to prepare.
Studies show that setting an EDD within the first 24 hours cuts down on discharge delays. This one practice improves care coordination and patient satisfaction. It can even shorten the hospital stay. You can read the full study on improving discharge timeliness.
To help you understand this early planning, here are the key things your care team will start working on with you.
Key Elements of Early Discharge Planning
| Planning Element | What It Means for You | Why It Matters |
|---|---|---|
| Initial Assessment | The team will ask about your home, family support, and daily routines. | This helps find challenges (like stairs or living alone) from the start. |
| Setting Goals | You'll discuss your recovery goals and what you want to achieve at home. | Your personal goals shape the plan, making sure it’s right for you. |
| Education Begins | You'll start learning about your condition, medications, and any new care needs. | Early education prevents feeling overwhelmed on your last day. |
| Family Involvement | Your family or support persons are included in talks from day one. | This ensures everyone is on the same page and ready to help you at home. |
Starting these talks early gives everyone time to create a plan that truly works for you. This makes for a smooth transition home.
Connecting Hospital to Home
For over 74 years, Central Coast VNA & Hospice has worked with hospitals across Monterey, San Benito, Santa Cruz, and South Santa Clara counties. Our nonprofit mission is to create a seamless bridge from the hospital to your home. Our team of Registered Nurses and therapists works with hospital discharge planners to make sure your recovery plan is clear and supported.
This early partnership is key to a safe transition. It ensures that medications, medical equipment, and home health visits are all set up before you leave the hospital. By taking these steps together, we can lower the risk of problems. We talk more about this in our guide on preventing hospital readmissions.
Our goal is to turn worry into confidence. This allows you to focus on what matters most: your recovery.
Who Is on Your Hospital Discharge Team

A good discharge planning from hospital experience is a team effort. The most important team members are you and your family.
You are surrounded by dedicated professionals. They all work toward the same goal: getting you home safely. Knowing who these people are and what they do can help you feel more in control of your recovery.
The hospital’s discharge planner leads this operation. This person is usually a social worker or a nurse. Their job is to coordinate all the moving parts of your plan. They will assess your needs and arrange for any services you need after you leave.
Your Core Hospital Team
Besides the discharge planner, other key professionals are part of your care plan. Each one brings special expertise to make sure you're ready for what's next.
- Physicians and Specialists: Your doctors give the final medical orders for your discharge. They decide when you are stable enough to leave. They also outline the care you'll need at home, like new prescriptions or follow-up visits.
- Hospital Nurses: The nurses at your bedside understand your daily condition. They teach you how to manage medications, care for wounds, and spot warning signs.
- Pharmacists: Before you go home, a hospital pharmacist will review your medications. This is a critical step to avoid risky drug interactions.
This teamwork creates a full circle of care around you. Remember, you are not going through this alone. Feel free to ask questions until you understand the plan completely.
Extending the Team to Your Home
For many people, the care team doesn't stop at the hospital doors. It extends right into your home. This is where a trusted home health partner becomes a key part of your recovery.
As a nonprofit that has served the Central Coast for over 74 years, we are an extension of your hospital care. When a patient in Monterey or San Benito County is discharged and needs more support, our professionals are ready to help.
A Registered Nurse from Central Coast VNA & Hospice can coordinate with your hospital discharge planner before you leave. This communication ensures that medical equipment, medications, and therapy visits are ready for you at home. Our clinicians bring expert care right to where you're most comfortable.
This team approach brings specialized care directly to you, including:
- Skilled Nursing: For medication management, wound care, and monitoring your recovery.
- Physical and Occupational Therapy: To help you regain strength, mobility, and independence safely.
- Medical Social Workers: To connect you with community resources and provide emotional support.
By working together, your hospital team and home health providers create a strong safety net. To learn more about expert care at home, read our guide on what is skilled nursing care. This teamwork ensures you receive continuous, compassionate support every step of the way.
Building Your Personalized Discharge Plan
Your recovery journey is unique. Your plan for leaving the hospital should be unique, too. A general checklist isn't enough. Real discharge planning from hospital means creating a personal roadmap for your health needs, home life, and recovery goals.
Think of this plan as your guide to a safe return home, not just another piece of paper. It should be clear and tailored to you. If it isn't, it is important to speak up and ask for more details until you feel confident.
Key Components of Your Plan
A strong discharge plan is built on several key pieces of information. Your team should walk you through each one before you go home.
- A Clear Hospital Summary: You should get a simple summary explaining why you were in the hospital and what treatment you received.
- Detailed Medication List: This is very important. It needs to include every medication, the exact dose, and when to take them.
- Follow-Up Appointments: Your plan must list all scheduled follow-up visits, including the doctor's name, location, and date.
- Diet and Activity Rules: Make sure you understand any new diet restrictions or limits on physical activity to avoid problems.
- Warning Signs: You need a clear list of symptoms to watch for and instructions on who to call if they appear.
Teamwork between hospital staff and your at-home support is vital here. Imagine someone in South Santa Clara County recovering from surgery. Their plan might include a physical therapist from Central Coast VNA & Hospice visiting them at home. Our therapist would help them follow activity rules and make steady progress.
You can learn more about our dedicated home health care services that support these important transitions.
The infographic below shows the critical process of checking your medications—a key part of any safe discharge plan.
This process shows the effort between clinicians and pharmacists to ensure every prescription is accurate. This is crucial for preventing errors once you are back home.
Arranging for Home Support
Your plan also needs to cover your practical needs for recovery. It is all about thinking through what you will need at home.
Your discharge plan should be reviewed with you and your family. This gives you time to ask questions and confirm you understand every part of it before you leave the hospital.
Arranging for the right support ahead of time makes a big difference. This might include:
- Medical Equipment: Do you need a hospital bed, a walker, or oxygen? Your discharge planner will help get these items delivered to your home.
- Home Health Care: If you need skilled support, like wound care from a Registered Nurse or therapy to regain mobility, these services will be scheduled.
As a nonprofit with over 74 years of experience serving communities like Monterey and San Benito County, we at Central Coast VNA & Hospice partner with hospitals to make sure this support is ready. Our mission is to provide the expert, compassionate care you need to recover safely at home.
Improving Communication for a Safer Transition
Clear communication is the bridge between a messy hospital discharge and a safe return home. Think of it as the final, most important step.
When everyone—the patient, family, and at-home care team—is part of the conversation, the plan is clear. Without that shared understanding, important details can be missed. This is where recovery can get off track.
Speak Up Until It’s Crystal Clear
Never be afraid to ask for things to be explained. If you hear a medical term you don't know or an instruction seems unclear, it is vital to speak up. Your hospital team wants you to succeed at home. Your questions help them give you better guidance.
A great way to make sure you understand is to repeat the instructions back in your own words. This simple method works wonders. It confirms you're on the same page and lets the clinician clear up any confusion. Taking this step is one of the most effective patient engagement strategies you can use.
Know Exactly Who to Call and When
Once you’re home, it can be stressful not knowing who to call with a question. Your discharge plan must include a clear list of names and phone numbers for your doctors and your home health agency.
This list is your safety net. It gives you quick access to professional help when you need it most. This can prevent small issues from becoming big problems.
For people in Monterey, San Benito, Santa Cruz, and South Santa Clara counties, Central Coast VNA & Hospice often becomes that key point of contact. Our Registered Nurses and therapists are in direct contact with your doctors. This creates a seamless link, ensuring your care stays coordinated.
Sadly, communication problems during discharge are a global issue. Even in developed countries, communication gaps can affect the quality of care. This shows the need for well-organized care where everyone has a clear role. You can read more about these international findings on care transitions.
With over 74 years of local, nonprofit service, our mission is to make sure you feel supported and heard. We become your advocate, ensuring your entire care team is on the same page. Open communication helps turn a stressful transition into a confident step toward recovery at home.
How Home Health Care Supports Your Recovery
Leaving the hospital doesn't mean your recovery is over. This transition is a key time when the right support can make all the difference. This is where professional home health care becomes a vital part of your discharge planning from hospital.
For people across Monterey, San Benito, Santa Cruz, and South Santa Clara counties, Central Coast VNA & Hospice is that vital bridge. As a nonprofit with over 74 years of experience in our community, our mission is to bring expert medical care to your home. This support helps you heal safely in the place you want to be most—your own home.
Skilled Support Tailored to You
Home health care is more than just convenient. It's about getting personalized, skilled services that match your recovery needs.
For example, a Registered Nurse can provide expert wound care or help you manage a new medication schedule. A physical therapist can guide you through exercises to rebuild your strength without risking a setback.
This level of professional support lowers the risk of problems that could send you back to the hospital. It brings peace of mind, knowing an expert is checking in, monitoring your progress, and talking with your doctor.
A Continuum of Care That Adapts
As you heal, your needs will change. Your care plan should be able to change with you.
Central Coast VNA & Hospice offers a full Continuum of Care, from home health to palliative and hospice services. This means we can adjust the level of support as you get stronger. We can also bring in more specialized care if your condition becomes more complex.
The entire healthcare industry sees how crucial post-discharge support is. The global market for these services is expected to grow from $288.13 billion in 2024 to $335.86 billion by 2025. This shows how essential it is to support patients after they leave the hospital. You can discover more insights about these transitional care market trends.
When you include home health in your discharge plan, you are creating a safety net of continuous, expert care. This proactive approach empowers you to heal with confidence.
Frequently Asked Questions About Hospital Discharge Planning
Leaving the hospital can feel rushed, and it’s normal to have questions. Getting clear answers is the best way to feel prepared for the transition home. We've put together answers to some of the most common concerns about discharge planning from hospital.
When does discharge planning start?
Effective discharge planning should start within 24 hours of your admission to the hospital. Your healthcare team will begin assessing your needs, your home life, and the support you'll require after you leave. This early approach prevents last-minute stress and ensures services, like home health care from Central Coast VNA & Hospice, are ready for a smooth transition.
What is my role in the discharge plan?
You are the most important person on the discharge planning team. Your role is to speak up—ask questions, share honest information about your home and support system, and voice any concerns you have. Make sure you understand your medications, follow-up appointments, and any diet or activity limits before you go home.
How are home health services paid for?
Home health care is often covered by Medicare, Medi-Cal, and most private insurance plans. It must be prescribed by a physician and be medically necessary for your recovery. The team at Central Coast VNA & Hospice can help you understand your coverage and any potential costs. You can learn more about qualifying for home health care on our website.
What should I do if my condition changes at home?
Your discharge plan should include clear instructions on who to call if your symptoms change or you have questions. It is vital to know this information before you leave the hospital. If you receive home health services from Central Coast VNA & Hospice, you will have access to a Registered Nurse who can assess your condition and contact your doctor.
How can Central Coast VNA & Hospice help after a hospital stay?
For over 74 years, Central Coast VNA & Hospice has helped patients transition safely from the hospital to home in Monterey, San Benito, Santa Cruz, and South Santa Clara counties. Our nonprofit team of Registered Nurses, therapists, and other professionals works with your hospital's discharge planner to create a seamless care experience. We provide the skilled nursing, therapy, and compassionate support you need to recover with confidence at home.
Navigating the transition from hospital to home can feel overwhelming, but you don't have to do it alone. The compassionate team at Central Coast VNA & Hospice is here to provide expert medical care and support every step of the way. Contact us today to learn how we can help you or your loved one recover safely and comfortably at home. Visit us online at https://ccvna.com to learn more.
Palliative Care vs. Hospice Care: Understanding the Key Differences
When a loved one faces a serious illness, you might hear the terms palliative care and hospice care. While both focus on comfort, they serve different needs at different times. Knowing the difference helps you make the best choice.
Palliative care can begin at diagnosis. It works with your regular doctors to manage symptoms while you still seek a cure. Hospice care is for when a cure is no longer the goal, focusing entirely on peace and comfort.

Navigating Your Care Choices on the Central Coast
Making these decisions can feel overwhelming, but you are not alone. As a nonprofit with over 74 years of local service, Central Coast VNA & Hospice is here to help. We support families in Monterey County, San Benito County, Santa Cruz County, and South Santa Clara County.
Our mission is to give you clear information to honor your wishes. The biggest difference between palliative and hospice care is about timing and treatment goals.
| Feature | Palliative Care | Hospice Care |
|---|---|---|
| When It Starts | At any stage of a serious illness, even from diagnosis. | When a doctor expects life expectancy to be six months or less. |
| Treatment Goal | To relieve symptoms and stress while you receive treatments to cure your illness. | To provide comfort and quality of life when treatments to cure have stopped. |
| Team Focus | Works with your current doctors to add an extra layer of support. | A dedicated team manages all care related to the final illness. |
A common myth is that palliative care means you're giving up. That’s not true. It adds support to help you live better while you continue to fight the illness.
If you need more guidance, our resources can show you where to turn when a loved one is seriously ill.
Sadly, not everyone can get this kind of support. A study by the National Hospice and Palliative Care Organization (NHPCO) highlights the importance of local providers like CCVNA. We work to ensure our community gets the compassionate care it deserves.
Comparing Palliative Care and Hospice Care
It’s easy to confuse palliative and hospice care. Both provide comfort and support during a difficult time. However, knowing the key differences is vital for making the right choice.
Palliative care can start when a serious illness is first diagnosed. Think of it as an extra layer of support that works with treatments meant to cure you. For example, a patient getting chemotherapy can use palliative care to manage pain and nausea.
Hospice care begins when treatments to cure an illness stop. The focus shifts completely to comfort for the rest of a person's life. This is for someone a doctor believes has a life expectancy of six months or less.
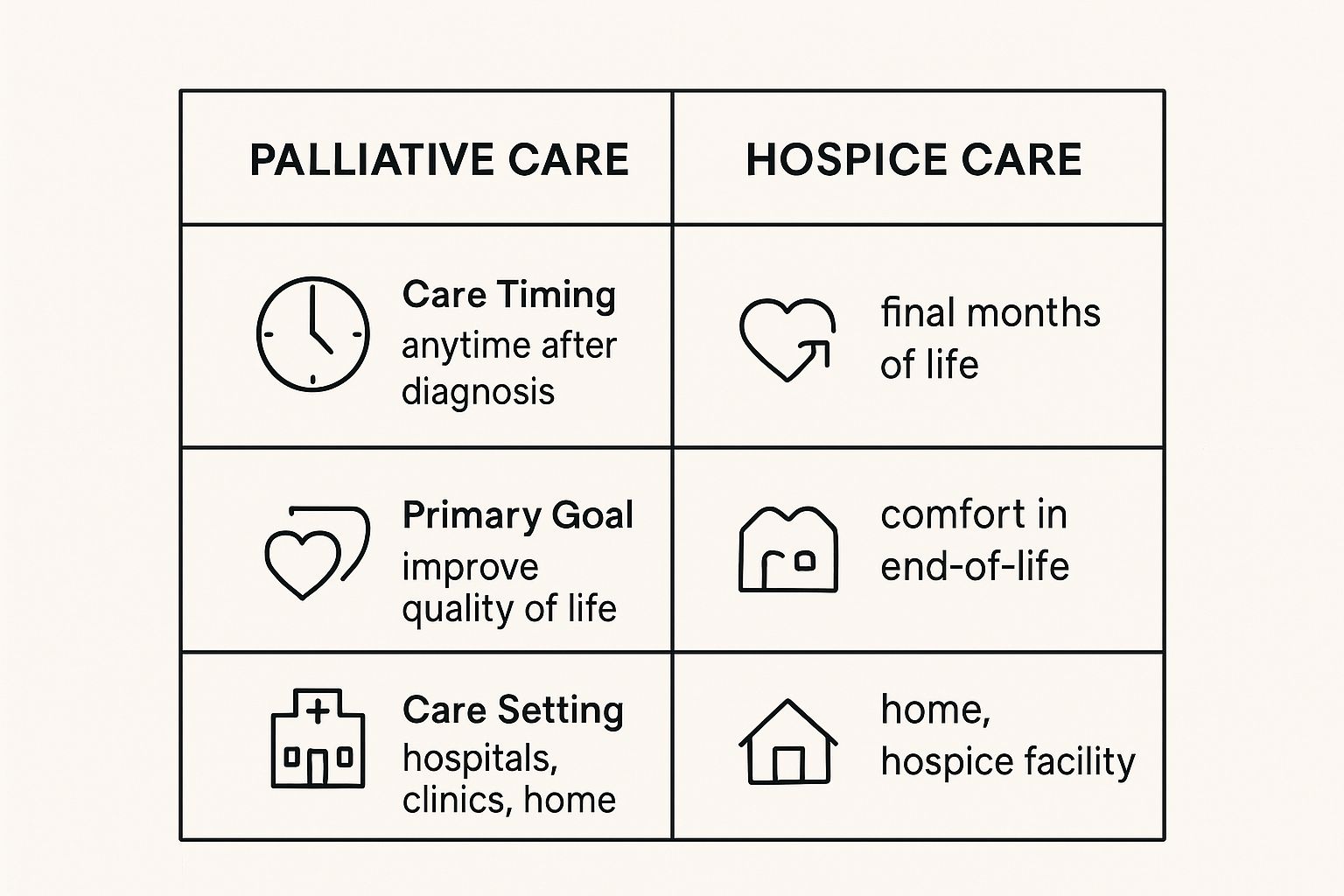
Choosing hospice is not about giving up. It's about choosing to live the time you have left with the best quality of life possible.
Key Differences At a Glance
Navigating these options can be hard. This table gives you a clear overview to help you find the right path for your family.
| Comparison Point | Palliative Care | Hospice Care |
|---|---|---|
| Timing | Can begin at diagnosis, at any stage of illness. | Begins when curative treatment stops; for a prognosis of 6 months or less. |
| Primary Goal | To relieve symptoms, improving quality of life during treatment. | To provide comfort and dignity at the end of life. |
| Curative Treatment | Provided alongside treatments intended to cure (e.g., chemotherapy, surgery). | Focuses on comfort care instead of curative treatments. |
| Duration of Care | Can be provided for years, based on the patient's needs. | As long as the patient meets criteria, even beyond 6 months. |
| Payment | Typically covered by private insurance, Medicare Part B, and Medicaid. | Fully covered by Medicare Part A, Medicaid, and most private insurance. |
| Care Location | Hospital, clinic, long-term care facility, or at home. | Primarily in the patient's home, but also in nursing homes or hospice facilities. |
The main takeaway is simple. Palliative care works with curative treatments, while hospice care is the primary support when a cure is no longer the goal.
Primary Goals and Patient Timing
The main goals are very different. Palliative care helps relieve the symptoms and stress of a serious illness. This helps a patient handle their medical treatments and feel better day to day.
Hospice care has a specific focus. It aims to make a person’s final months as comfortable and meaningful as possible. The entire team—from the Registered Nurse to the Chaplain—works to manage symptoms and provide emotional support.
The core distinction is simple: Palliative care can be provided at any stage of illness, alongside curative treatment, while hospice care is for the final phase of life when the focus is on comfort, not cure.
How Care Works with Other Treatments
It's also important to know how each service fits with other medical care. Palliative care is an add-on to your current care plan.
- Palliative Care: Works with treatments like surgery or chemotherapy. The team coordinates with the patient's other doctors.
- Hospice Care: Replaces curative treatments. The hospice team takes over, focusing only on comfort.
For families in Monterey County and Santa Cruz County, this is key. Our team at Central Coast VNA & Hospice is here to offer expert, compassionate guidance. Learn more about how our palliative care services can support your family.
Who Qualifies for Each Type of Care?
Understanding who is eligible for palliative versus hospice care can be confusing. It depends on the illness, prognosis, and patient's wishes. Getting this right helps you have better talks with your doctor.
Palliative care has broad eligibility. Anyone with a serious, long-term illness can qualify, no matter their age. This includes conditions like cancer, heart failure, or dementia.

Eligibility for Palliative Care at Home
The main requirement for palliative care is a need for symptom relief. If someone is dealing with pain, stress, or side effects, they are likely a good candidate. This care works alongside treatments meant to cure.
A patient does not need a terminal diagnosis to get palliative care. Many people receive this support for years. It helps them live more comfortably while managing their illness.
Hospice Care Eligibility Requirements
Hospice care eligibility is more specific. A patient qualifies when a doctor certifies they have six months or less to live if the illness runs its natural course. This is a crucial difference when looking at palliative care v hospice care.
A common myth is that choosing hospice means "giving up." In reality, it is a powerful choice to prioritize comfort and quality of life when a cure is no longer the primary goal.
This shift in focus allows our team from Central Coast VNA & Hospice to provide full support at home. Our team manages symptoms and offers emotional guidance to the patient and their family. You can learn more in our detailed hospice eligibility requirements.
Services Included with Palliative and Hospice
Knowing the rules for eligibility is one part of the puzzle. The other part is knowing what services each type of care provides. Though both focus on comfort, their services are different.
Palliative care is an extra layer of support. It works with your curative treatments, not instead of them. Its main goal is to manage symptoms and improve your well-being.
What Palliative Care Provides
Palliative care is flexible and tailored to your needs while you continue medical treatments. The goal is always to make your quality of life better.
Services often include:
- Expert Symptom Control: Managing pain, fatigue, nausea, and other symptoms.
- Emotional and Spiritual Support: Helping you and your family cope with stress and anxiety.
- Care Coordination: Making sure all your doctors are on the same page.
The core benefit of palliative care is that you get all this comprehensive support without having to stop treatments meant to cure your illness. This care is available wherever you call home on the Central Coast.
A Closer Look at Hospice Services
Hospice care begins when the focus shifts from cure to comfort. At Central Coast VNA & Hospice, our team provides complete support wherever a patient lives. This can be a private home in San Benito County or a facility in South Santa Clara County.
Our care team is the heart of our hospice program. It includes:
- Registered Nurse: Manages medical care with a focus on pain relief.
- Hospice Aide: Helps with personal care like bathing and dressing.
- Social Worker: Provides emotional support and helps with planning.
- Chaplain: Offers spiritual guidance for all beliefs.
This dedicated team works together to create a peaceful and dignified experience. To learn more, see what to expect with hospice care from our team.
Understanding Insurance and Payment Options
When a loved one is sick, the last thing you want is to worry about money. Financial stress should not be part of this difficult time.
Both palliative care and hospice care are covered by most insurance plans, including Medicare. But the way they are covered is different. Let's break it down.
How Palliative Care Is Covered
Think of palliative care as a specialized medical service, like seeing a heart doctor. It is an extra layer of support that works with your other treatments.
Because of this, it is billed with your existing health coverage:
- Medicare Part B: This is the most common way palliative care is covered. It is treated like a specialist visit, so deductibles apply.
- Private Insurance and Medicaid: Most private plans and Medicaid also cover these services. It's always a good idea to call your provider to check your plan.
This makes it an accessible option for anyone needing help managing symptoms of a serious illness.
The Medicare Hospice Benefit
Hospice coverage is different because it is all-inclusive. The Medicare Hospice Benefit is a plan that covers almost everything related to a patient’s final illness. This is a big difference when comparing palliative care vs. hospice care.
The Medicare Hospice Benefit is designed to be all-inclusive for the terminal diagnosis, often resulting in little to no out-of-pocket costs for the patient and their family. This includes the care team, medications, and medical equipment.
This complete coverage ensures that when the focus shifts to comfort, money worries do not get in the way. Our team at Central Coast VNA & Hospice helps families in Monterey County and nearby areas understand their benefits.
If you have questions, our team can help you get the full support you deserve. Contact us today to learn more.
Navigating Your Journey with Central Coast VNA
Knowing the difference between palliative and hospice care is one thing. Seeing how they work for your family is what truly matters. At Central Coast VNA & Hospice, our nonprofit mission is to provide care that adapts to your needs. We've been a local guide for families in Monterey, San Benito, Santa Cruz, and South Santa Clara counties for over 74 years.

A Real-World Scenario
Let's look at a common situation. Imagine someone with advanced Chronic Obstructive Pulmonary Disease (COPD). Their journey might start with our palliative care team to help manage breathing problems.
This support works alongside their regular doctor’s treatments. It helps them feel better and stay at home.
As their illness gets worse, their goals might change. They may shift from aggressive treatments toward comfort. Because they are already with our organization, the move to our hospice program is smooth.
A seamless transition from palliative to hospice care ensures that patients receive consistent, compassionate support from a team they already know and trust, right in their own community.
This connected approach is key to high-quality care. It helps families focus on what truly matters—the patient’s comfort and wishes. It is part of our Continuum of Care, from home health to palliative care to hospice.
Your Local Experts in Palliative and Hospice Care
You should not have to walk the path from diagnosis to end-of-life decisions alone. As a local nonprofit, we provide home health, palliative, and hospice services all under one roof. We are here to offer the right care at the right time.
For families starting to explore their options, learning about palliative care is a great first step. Find out why Central Coast VNA is the best choice for palliative care on the Central Coast. See how our team can support you from the beginning.
Frequently Asked Questions
Making decisions about palliative care versus hospice care brings up a lot of questions. Here are answers to some of the most common ones we hear from families we serve.
When is the right time to call for palliative or hospice care?
The best time for palliative care is at the diagnosis of a serious illness. For hospice care, the conversation usually starts when a doctor determines life expectancy is six months or less. At that point, the focus shifts to comfort.
Can someone be on hospice for more than six months?
Yes. The six-month timeframe is a guideline for eligibility, not a limit. A patient can continue receiving hospice care as long as their doctor confirms they meet the criteria. The goal is to provide support for as long as needed.
Does choosing hospice mean we're giving up hope?
Not at all. Choosing hospice is about redefining hope. It shifts from hope for a cure to hope for peace, comfort, and meaningful time with loved ones. It is a choice to live the final chapter with dignity.
Where does this care take place?
Both palliative and hospice care come to you. Our teams at Central Coast VNA & Hospice provide care wherever you call home. This includes a private house, assisted living, or a nursing home throughout Monterey, San Benito, Santa Cruz, and South Santa Clara Counties.
How is palliative care vs hospice care paid for?
Palliative care is usually covered like other medical care. This includes Medicare Part B, Medicaid, and most private insurance. Hospice care is covered by the comprehensive Medicare Hospice Benefit, which often leaves families with little to no out-of-pocket costs for the terminal illness.
Navigating these choices is hard, but you don't have to do it alone. For over 74 years, the team at Central Coast VNA & Hospice has been a trusted, nonprofit guide for local families. Contact us today to learn how we can support you.
Home Care Palliative Care: Compassionate Support for Your Loved Ones
When a serious illness touches your family, it can feel overwhelming. Home care palliative care is a special kind of medical support. It is designed to bring calm and control back into your life.
This care focuses on relieving symptoms, pain, and stress. The goal is to improve the quality of life for both the patient and the family. This all happens in the comfort of home.
Understanding Palliative Care at Home
Palliative care is not about giving up. It is about living as fully as possible.
Think of your current doctors as your "treatment team." A palliative care team works alongside them as your "comfort team." They manage symptoms like pain, fatigue, and anxiety to help the patient feel as good as possible.
People often confuse palliative care with hospice. They are not the same. Palliative care can start when you are diagnosed, even while you get treatments to cure your illness. Hospice care is for when curative treatments are no longer an option.
To help clear things up, here’s a quick comparison.
Palliative Care vs Hospice Care At a Glance
This table breaks down the main differences. It helps you understand which path is right for your family.
| Aspect | Palliative Care | Hospice Care |
|---|---|---|
| Timing | Can begin at any stage of a serious illness, from diagnosis onward. | Typically begins when life expectancy is six months or less and curative treatments have stopped. |
| Treatment Goal | To relieve symptoms and improve quality of life alongside curative treatments. | To provide comfort and support when a cure is no longer the goal. |
| Location | Home, hospital, or long-term care facility. | Primarily at home, but also available in dedicated hospice facilities or nursing homes. |
| Insurance | Covered by Medicare Part B, Medicaid, and most private insurance plans. | Covered by the Medicare Hospice Benefit, Medicaid, and most private insurance. |
Understanding this difference is important. Palliative care adds an extra layer of support to your current medical care.
A Growing Need for Comfort Care
The need for this kind of compassionate support is growing. According to the World Health Organization, an estimated 56.8 million people, including 25.7 million in the last year of life, are in need of palliative care each year.
This trend shows how vital it is to have expert care providers in our communities. At Central Coast VNA & Hospice, our mission is to bring this support to your doorstep. We are a nonprofit, mission-driven provider with over 74 years of service.
Why Home-Based Care Matters
Receiving care at home feels different because it is different. Being in a familiar place has a positive impact on a patient's well-being. It also gives families peace of mind.
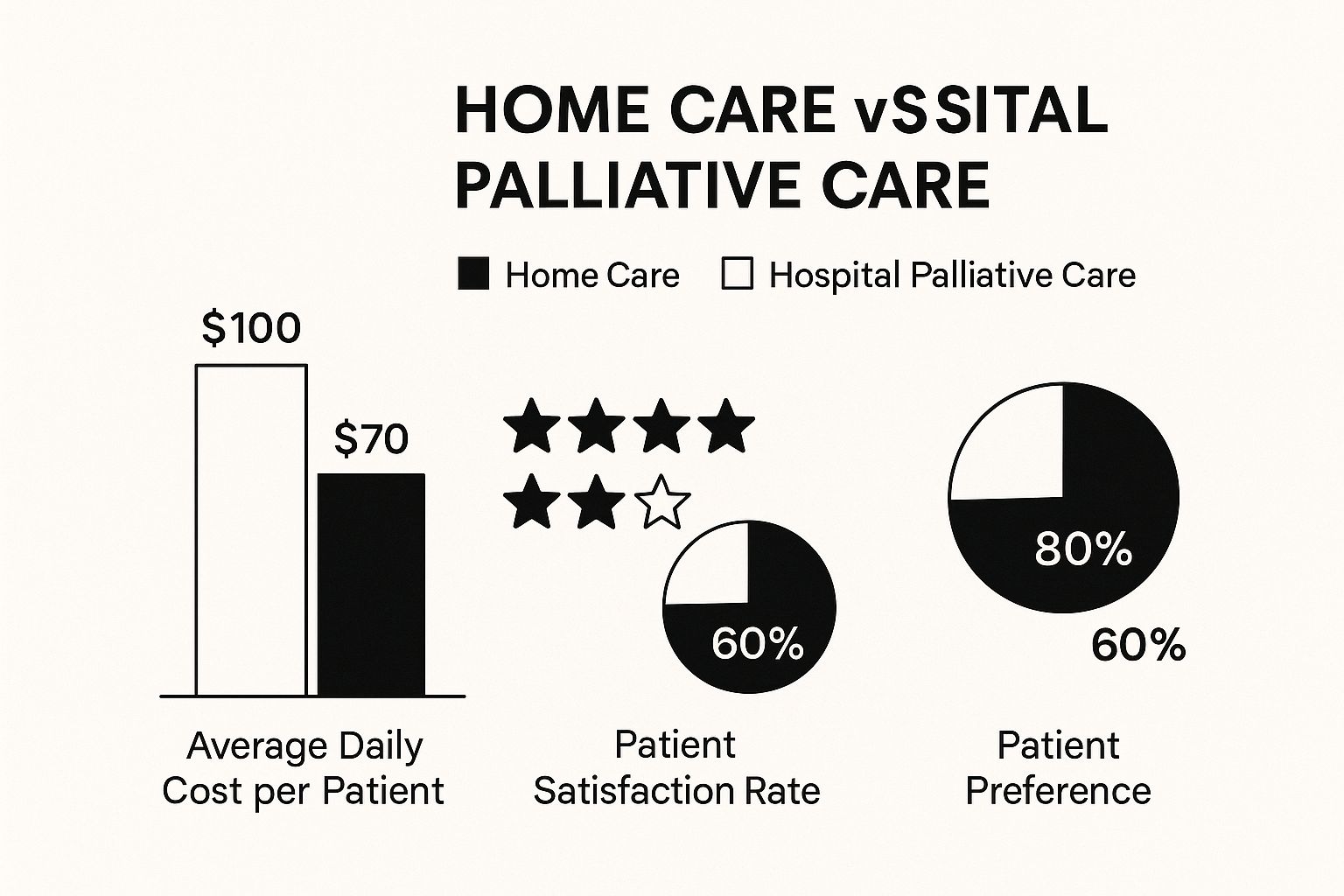
Patients often prefer being at home. They also report higher satisfaction with their care. Our 74+ years of experience show that a healing environment is a loving environment.
Central Coast VNA & Hospice is the trusted local nonprofit. We serve Monterey County, San Benito County, Santa Cruz County, and South Santa Clara County. To learn more, explore our detailed guide on what is palliative care.
Who Can Benefit From Palliative Care
Palliative care is for anyone living with a serious illness. It helps people who need more comfort and a better quality of life. It is an extra layer of care to help people live with dignity and control.
Imagine someone managing a chronic condition. They might struggle with constant pain, fatigue, or anxiety. Home care palliative care can make a world of difference in these situations.

Common Conditions We Support
Palliative care can help with almost any serious illness. Bringing this care into the home allows people to face these challenges in a familiar setting.
For our neighbors in Monterey County and Santa Cruz County, our teams often support individuals with:
- Congestive Heart Failure (CHF): We help manage symptoms to improve daily comfort.
- Chronic Obstructive Pulmonary Disease (COPD): Our focus is on easing breathing difficulties.
- Cancer: We work to address pain, nausea, and other side effects of treatment.
- Dementia and Alzheimer's: We provide comfort and safety for patients and families.
- Kidney Disease: The goal is to ease symptoms like pain and lack of appetite.
- Neurological Conditions: For illnesses like Parkinson's or ALS, we focus on symptom management.
Palliative care focuses on the person, not just the diagnosis. It is about managing the symptoms that get in the way of life.
Beyond the Diagnosis
The decision to start palliative care is about its impact on daily life. Frequent emergency room visits are a strong sign that more support at home could help.
Palliative care is for any age and any stage of a serious illness. Its main purpose is to relieve symptoms and improve quality of life. This helps both the patient and the family.
This focus on the whole person is at the heart of what we do at Central Coast VNA & Hospice. For over 74 years, our nonprofit has served the communities of Monterey, San Benito, Santa Cruz, and South Santa Clara counties. We see how compassionate care at home can transform a person's experience.
Is Palliative Care Right for Your Family?
Ask yourself these questions. Does your loved one struggle with:
- Uncontrolled pain or discomfort?
- Frequent hospitalizations?
- Symptoms from a chronic illness that are harder to manage?
- Stress and anxiety related to their condition?
If you answered yes, home care palliative care could be a valuable resource. It brings an expert team to help make each day the best it can be. This support works with your doctors to add another layer of focused care.
Meet Your Compassionate Care Team
Great palliative care is a team effort. A group of professionals works together to support your family. They meet your loved one's physical, emotional, and spiritual needs.
This team-based approach is how we provide care at Central Coast VNA & Hospice. We treat the whole person, not just the illness. Our team builds a care plan that honors your family’s values and goals.
Your Core Support Professionals
Each patient's team is shaped around their specific needs. A few key members form the heart of our palliative care services. They play a vital role for families across Monterey County and San Benito County.
- Registered Nurse (RN): The RN is the clinical expert for managing pain and other symptoms. They coordinate with your doctor to handle medications and educate your family.
- Medical Social Worker: Your Medical Social Worker is your guide. They connect you with community resources, help with insurance questions, and offer emotional support.
- Chaplain: Our chaplains offer a comforting presence. They listen without judgment and provide guidance for patients and families.
- Hospice Aide: These professionals help with daily living tasks. From bathing to preparing a light meal, their hands-on support preserves a patient’s dignity. You can learn more about the support provided by a hospice aide in our detailed guide.
This team-based model ensures no need is overlooked. It’s a complete circle of support designed to bring you peace of mind.
A Growing Recognition of Team-Based Care
The value of this team-based approach is recognized worldwide. As more people live with chronic conditions, the demand for palliative care is rising. This shows a global shift toward understanding the importance of quality of life for patients.
The palliative care team ensures your family receives support that addresses every aspect of well-being. This includes physical comfort, emotional peace, and practical help.
For over 74 years, Central Coast VNA & Hospice has pioneered this model in Santa Cruz County and South Santa Clara County. As a local nonprofit, our focus is on the well-being of our communities. Our team members are your neighbors, dedicated to providing expert care at home.
How Palliative Care Improves Daily Life
When a serious illness enters your life, a “good day” can feel distant. Palliative care brings those good days back. It offers real, everyday improvements for the patient and their family.
Expert home care palliative care starts with getting symptoms under control. This means less pain and more restful sleep. It gives you the energy for things that matter, like spending time with loved ones.

Reducing Stress and Restoring Control
One of the biggest reliefs for families is fewer stressful trips to the hospital. A dedicated team monitors symptoms at home. This proactive approach helps keep your loved one comfortable where they want to be.
Having a consistent team also improves communication. The palliative team makes sure everyone is on the same page. This clarity helps families feel more confident and in control.
At Central Coast VNA & Hospice, this is the heart of what we do. We provide expert care that brings peace of mind to families across Monterey and San Benito County.
Supporting the Whole Family
A serious illness affects the entire family. Loved ones often take on demanding roles. Palliative care extends its support system to them, too.
Our team provides education and hands-on guidance. We also offer emotional and spiritual support to help reduce anxiety. Finding ways to support caregiver mental well-being is a key part of the plan.
The goal is to lift the burden so families can focus on quality time together. This support helps preserve relationships and create positive memories.
Bringing Comfort Home: A Real-Life Scenario
Think of a family in Santa Cruz County caring for a father with advanced COPD. Constant trips to the ER for breathing emergencies left everyone on edge. His days were consumed by worry.
When they started palliative care with Central Coast VNA & Hospice, things changed. A Registered Nurse began visiting to fine-tune his medications. A Medical Social Worker helped them find community resources.
With his symptoms managed, his energy returned. The family was no longer living in fear. This is the real difference home care palliative care makes.
Navigating Insurance and Eligibility
Figuring out how to pay for home-based palliative care can feel stressful. The good news is these services are usually covered by major insurance plans.
You don't have to sort this out alone. For families in Monterey County and San Benito County, our team is here to help you understand your benefits.
Understanding Your Coverage Options
Paying for palliative care is often more straightforward than people think. Visits from a Registered Nurse or a Medical Social Worker are considered medical care.
Here’s a quick look at common coverage options:
- Medicare Part B: This part of Medicare covers doctor visits and outpatient services. Palliative care generally falls under this.
- Medi-Cal: California's Medicaid program also covers palliative care services.
- Private Insurance: Most commercial health insurance plans include benefits for palliative care.
Our team at Central Coast VNA & Hospice can help you confirm your plan’s details. This way, there are no surprises.
Who Is Eligible for Palliative care?
Eligibility is about a person’s need for support. The main requirement is a diagnosis of a serious or chronic illness. The focus is on managing symptoms, not on a person's prognosis.
The first step is a referral from a physician. This ensures the palliative team can work with your primary doctor. You can learn more in our simple guide to Medicare home care eligibility.
Receiving a palliative care referral is not about giving up. It is about adding another layer of expert support to your team.
Access to this support isn't always easy. This makes it more important to have trusted local providers like Central Coast VNA & Hospice.
As a nonprofit organization with over 74 years of experience, our mission is to ensure everyone in our service areas can access compassionate care. We are here to answer your questions. Contact us today for a personal consultation.
How to Get Started with Palliative Care
Taking the first step to ask for more support can feel hard. We understand. Our goal is to make starting home care palliative care as simple as possible.
This guide will walk you through how to begin. Central Coast VNA & Hospice is here to support your family every step of the way.

The First Step: A Conversation with Your Doctor
The path to palliative care begins with your loved one’s doctor. Palliative care is designed to work with their current medical treatments. Your doctor provides the referral that lets our team get involved.
When you talk to the doctor, be open about the challenges at home. Mention uncontrolled symptoms or frequent ER trips. A simple statement like, "We would like to explore palliative care for extra support," is a perfect way to start.
Connecting with Central Coast VNA & Hospice
Once the doctor agrees, they will send a referral to our team. You can also contact us yourself. We can then coordinate with your physician’s office.
Here’s how you can connect with us:
- Call Our Team: A phone call is an easy way to start. Our staff can answer your questions and explain what comes next.
- Request a Consultation: We can arrange a meeting to discuss your family’s specific needs.
- Coordinate with the Doctor: Let us know who your loved one’s physician is. We can reach out to make the referral process seamless.
Our commitment is to make this transition as smooth as possible. We work with medical providers throughout Monterey, San Benito, Santa Cruz, and South Santa Clara counties.
Your Local Partner in Compassionate Care
For over 74 years, Central Coast VNA & Hospice has been the trusted nonprofit provider of home care palliative care. Our local roots mean we are deeply committed to the well-being of the communities we serve.
If you are looking for support, our compassionate team is ready to help. To find out more, explore our resources on finding palliative care near me. Please contact us today to learn how we can support you.
Frequently Asked Questions (FAQs)
1. Is palliative care only for the end of life?
No, not at all. Palliative care can begin at any stage of a serious illness, right from diagnosis. It works alongside curative treatments to improve quality of life. Hospice care is for the end of life when curative treatments have stopped.
2. How is home palliative care different from home health care?
Home health care is typically short-term, skilled care to help a patient recover after a hospital stay or surgery. Home palliative care is long-term support focused on managing symptoms and stress from an ongoing, serious illness to improve quality of life.
3. Can we keep our own doctors?
Yes, absolutely. The palliative care team is an extra layer of support. They work closely with your primary physician and specialists to coordinate care.
4. Who decides when palliative care should start?
The decision is a conversation between you, your loved one, and your doctor. It usually starts when symptoms become difficult to manage. A physician’s referral is needed to begin services.
5. How often will the palliative care team visit?
The visit schedule is based on your family's specific needs and the care plan you create with the team. It is flexible and can change as your needs evolve. Our team is always a phone call away between visits.
For over 74 years, Central Coast VNA & Hospice has been the trusted nonprofit partner for families needing compassionate, expert care at home. As a mission-driven provider, we are committed to our Continuum of Care, guiding families from home health to palliative care and hospice. If you have more questions or believe your family could benefit from our support, please reach out to us. Learn more about our comprehensive services at https://ccvna.com.
What Is Home Care Palliative Care?
When you or a loved one is dealing with a serious illness, it’s about more than just medical treatments. It's about comfort, dignity, and quality of life. Home palliative care brings this support right where you feel most at ease: at home.
Think of it as an extra layer of specialized medical support to relieve symptoms and stress. It works alongside your current doctors and treatments. The goal is to improve your well-being at any stage of a diagnosis.
An Extra Layer Of Support Right At Home
Navigating a serious illness can feel overwhelming. Home palliative care brings an expert, compassionate team to help you and your family. Their job is to add life to your days, not just days to your life.
The goal is to manage draining symptoms like pain, shortness of breath, fatigue, or anxiety. This helps you focus on what truly matters. For over 74 years, Central Coast VNA & Hospice has provided this mission-driven care to families across Monterey, San Benito, Santa Cruz, and South Santa Clara Counties.
The Clear Advantage of Being at Home
There's a reason people say "home sweet home." Receiving care in a familiar environment makes a world of difference. Studies and personal stories show that managing an illness at home often leads to better well-being than a hospital.
This isn't just a feeling; the numbers back it up.
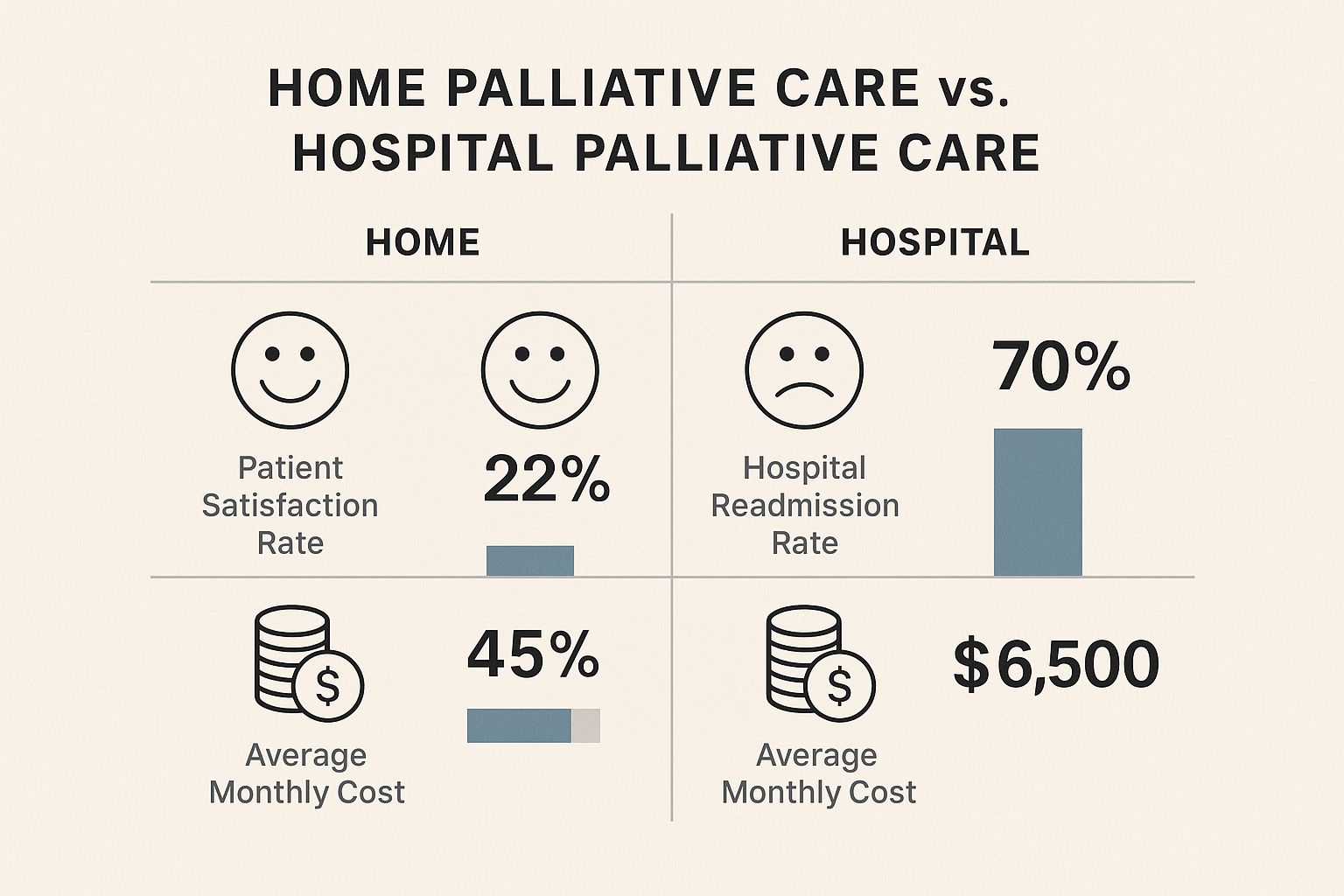
Patients who receive palliative care at home often report higher satisfaction. They also have fewer hospital visits and lower overall costs. It shows what happens when expert medical care meets the comfort of home.
A Focus on the Whole Person
Home palliative care is deeply personal. The approach is built around your unique needs, values, and goals. It is similar to the philosophy of person-centred therapy, which puts you first.
Your dedicated team, often led by a Registered Nurse, works with you, your family, and your doctors. Together, they create a care plan that truly fits. You can learn more about the role of our nurses in our guide to skilled nursing at home.
The need for this support is growing. Globally, the demand for palliative care has jumped by 74% in the last three decades. In 2021 alone, an estimated 73.5 million people needed these services, showing a shift toward prioritizing quality of life.
At its core, palliative care is about making sure every patient’s voice is heard. The care plan revolves around your goals, your values, and what "quality of life" means to you.
Who Benefits Most From Palliative Care at Home?
Palliative care at home is for anyone with a serious illness who wants to feel better. It helps lift the physical and emotional weight of conditions like cancer, heart failure, or kidney disease.
Think of someone going through chemotherapy, drained by fatigue and nausea. Or a person with COPD who struggles for every breath. These are the exact situations where home care palliative care provides an extra layer of support.

Alleviating Symptoms and Restoring Comfort
The main job of a palliative team is to manage symptoms that disrupt your life. For instance, a person with advanced heart failure might deal with pain, shortness of breath, and anxiety. Poorly managed symptoms often lead to ER visits and a lower quality of life.
This is where a dedicated team from Central Coast VNA & Hospice makes a real difference. A Registered Nurse works with your doctors to adjust medications and teaches your family how to manage symptoms. This proactive approach helps keep you comfortable and out of the hospital.
Palliative care is about helping people live as well as possible, for as long as possible. It addresses the person, not just the disease.
This person-first philosophy is changing healthcare. The global palliative care market was valued at USD 15.11 billion in 2024 and is expected to more than double by 2033. This growth is driven by aging populations and chronic conditions. You can discover more insights about these global trends to learn more.
Supporting Families Through Complex Illness
A serious illness affects the whole family. Loved ones often become caretakers, facing new stress and challenges. Home care palliative care wraps its support around the entire family.
Imagine a family in Monterey County caring for a parent with ALS or Parkinson's. They might struggle to understand the healthcare system or cope with the emotional toll. A Medical Social Worker from Central Coast VNA & Hospice can be their guide.
They provide:
- Emotional Support: Offering counseling for both the patient and family.
- Resource Navigation: Connecting families with local services like meal delivery or support groups.
- Care Coordination: Ensuring all doctors and specialists are on the same page.
By supporting the entire family, our team helps create a more stable, less stressful environment. This allows families to focus on spending quality time together. Whether in Monterey County, San Benito County, Santa Cruz County, or South Santa Clara County, our nonprofit mission is to ensure every family has the support they need.
What Your In-Home Palliative Team Provides
When you choose in-home palliative care, you get an entire team of specialists. This team is built to address your physical, emotional, and spiritual well-being. They work together with your other doctors to give you complete support at home.
This team approach means your care is never one-dimensional. We see you as a whole person, along with your family. This philosophy has been at the heart of Central Coast VNA & Hospice for over 74 years in our local communities.
Expert Pain and Symptom Management
The first job of your palliative team is to bring you physical relief. Symptoms like pain, fatigue, nausea, or shortness of breath can drain your energy. Our team focuses on specialized medical care to get these symptoms under control.
A Registered Nurse with special training in palliative care leads this effort. They visit you at home to:
- Assess Symptoms: They take time to understand your symptoms and how they affect your life.
- Coordinate with Doctors: Your nurse works directly with your other doctors to fine-tune medications and treatments.
- Provide Hands-On Care: They offer direct care and teach you and your family how to manage symptoms.
- Educate and Empower: They make sure you understand your condition and treatment options, putting you in control.
By managing difficult symptoms, our team helps reduce stressful ER visits. This allows you to stay comfortably at home. To learn more, see our page on expert pain and symptom management.
Emotional and Practical Family Support
A serious illness impacts the entire family. Loved ones often face new roles and immense stress. Your palliative care team includes professionals focused on supporting everyone involved.
A Medical Social Worker is your family’s advocate and guide. They are experts at identifying challenges and connecting you with community resources. They also offer counseling to help everyone cope.
The goal is to lift the burden from your family’s shoulders. We provide the resources and emotional support needed so you can focus on what matters most—each other.
This support can include helping with advance care planning or finding financial assistance programs. By caring for the whole family, we help create a more stable and peaceful environment.
Spiritual Guidance and Comfort
Serious illness often raises big questions about life and meaning. For many, spiritual comfort is a vital part of well-being. Our team is here to support your spiritual needs with respect, no matter your beliefs.
A Chaplain is available to provide non-denominational spiritual support. They offer a calming presence and a safe space to explore feelings, fears, and hopes. This support is always guided by your beliefs, ensuring it’s a source of comfort.
Together, this team from Central Coast VNA & Hospice provides a complete circle of support. We are proud to serve Monterey County, San Benito County, Santa Cruz County, and South Santa Clara County with compassionate care.
How Palliative Care Works With Curative Treatment
One of the biggest myths about palliative care is that it means you’re giving up. This is not true.
Think of home care palliative care as a partner in your health journey. It works side-by-side with treatments meant to cure your illness. Our team at Central Coast VNA & Hospice collaborates directly with your doctors. The goal is to make you stronger so you can better handle treatments like chemotherapy or radiation.

Strengthening You for the Fight
Imagine you’re running a marathon. Curative treatments are like the race itself—demanding and tough. Palliative care is your support crew, providing water and encouragement to help you keep going.
By managing difficult side effects like pain and nausea, our palliative team improves your well-being. When you feel stronger, you're often better able to stick with your treatment plan. This supportive care empowers you in your fight against illness.
A Bridge in Your Continuum of Care
At Central Coast VNA & Hospice, we see palliative care as a vital bridge in our continuum of care. It fills the gap between traditional home health and hospice. This ensures you get the right level of care at the right time.
Unfortunately, not everyone has access to this type of care. According to one study, only about 14% of people worldwide who need palliative support actually receive it. You can read the full research about these global findings to learn more. This is why having a trusted local provider in Monterey County, San Benito County, Santa Cruz County, or South Santa Clara County is so important.
Palliative care is not about the end of treatment. It’s about ensuring you have the best possible quality of life during treatment.
Palliative Care and Hospice Are Different
It’s important to know that palliative care is not the same as hospice. They serve different purposes at different times.
- Palliative Care: Can begin at any stage of a serious illness and works alongside curative treatments.
- Hospice Care: Is for when curative treatments are no longer being pursued, usually for those with a life expectancy of six months or less.
Choosing palliative care is a proactive step to enhance your medical treatment, not end it. For a deeper explanation, you can read our guide on the differences between palliative and hospice care. Our mission is to ensure every family on the Central Coast understands their options.
How to Access and Pay for Palliative Care
Dealing with a serious illness is hard enough without worrying about insurance and appointments. Starting home-based palliative care is often more straightforward than you might think.
Let’s clear up one of the biggest worries: cost. Palliative care is a medical specialty, like cardiology. It is covered by most insurance plans, including Medicare Part B, Medi-Cal, and most private policies.
Starting the Conversation
The first step is to talk to your doctor. A simple conversation with your physician or specialist is all it takes.
Tell them about the symptoms, pain, or stress you are facing. You can say you're interested in adding support to improve your quality of life. The goal is to ask for a referral to a palliative care team.
Openly discussing your needs with your doctor is the key to accessing palliative care. It ensures your entire medical team is working together for you.
Once you have a referral, you can contact a provider directly. Here at Central Coast VNA & Hospice, our team helps families across Monterey County, San Benito County, Santa Cruz County, and South Santa Clara County figure out the next steps. We can coordinate with your doctor to ensure our services are the right fit.
Understanding Your Insurance Coverage
Navigating insurance can feel complicated, but you don't have to do it alone. Since palliative care is a medical service, your health insurance typically handles the cost.
Here’s a general breakdown of how it usually works:
- Medicare Part B: This covers outpatient services, including the physician and nurse practitioner visits central to palliative care. Learn more in our guide to Medicare home care eligibility.
- Medi-Cal: California’s Medicaid program also provides coverage for palliative care services.
- Private Insurance: Most commercial health plans cover palliative care as they would any other specialty. It's always a good idea to call your insurance company to confirm the details.
Our staff at Central Coast VNA & Hospice can help you verify your insurance coverage. As a nonprofit, our mission is to make this support as accessible as possible. If palliative care could make a difference for your family, please don't wait.
The Value of a Local Nonprofit Care Provider
Choosing a provider for home care palliative care is a deeply personal decision. When you choose a local, nonprofit organization, you partner with a team focused only on your well-being, not profits. This difference changes everything about the care your family receives.
For over 74 years, Central Coast VNA & Hospice has been a mission-driven nonprofit in our community. Our roots are deep in Monterey County, San Benito County, Santa Cruz County, and South Santa Clara County. We are your neighbors, and our promise is to provide the most compassionate care to everyone who needs it.
A Mission Focused on Community
For-profit agencies answer to investors, so their bottom line often comes first. Our mission is different; it's about service.
This allows us to focus our resources on what matters: patient comfort, advanced training, and supporting our community.
As a nonprofit, our success isn't measured on a balance sheet. It's measured by the comfort and quality of life we bring to families.
This patient-first mindset allows us to provide support that often goes beyond what insurance covers. We are committed to ensuring no one is turned away because they can't afford care. It’s a promise we’ve kept for generations.
Deep Local Roots and Trusted Expertise
Choosing a local provider means you’re getting a team that truly understands the Central Coast. Our clinicians live here, and we have long-standing relationships with local doctors and hospitals. This makes coordinating your care seamless.
You can get a closer look at what makes us different here: Why Central Coast VNA is the Best Choice for Palliative Care on the Central Coast. When you’re ready to look at your options, please reach out. Let us show you how our local roots and nonprofit mission can make all the difference for your family.
Frequently Asked Questions About Home Palliative Care
1. Is palliative care the same thing as hospice?
No, they are different. Palliative care can start at any time during a serious illness and works alongside curative treatments. Hospice is for when curative treatments are no longer being pursued, usually for someone with a life expectancy of six months or less.
2. Will insurance cover palliative care at home?
Yes, in most cases. Palliative care is a medical specialty covered by Medicare Part B, Medi-Cal, and most private insurance plans. Our team at Central Coast VNA & Hospice can help you understand your specific coverage.
3. How do we start the process for palliative care?
The best first step is to talk to your doctor about your symptoms and ask for a referral to a palliative care team. You can also contact Central Coast VNA & Hospice directly, and we can coordinate with your physician.
4. Does the palliative team replace our regular doctors?
Not at all. Our palliative team works as an extra layer of support. We partner and communicate with your primary doctor and any specialists to ensure your care is coordinated and comprehensive.
5. Is support available for family members too?
Absolutely. Supporting the entire family is a key part of home care palliative care. Our team includes Medical Social Workers for emotional support and resource navigation, as well as Chaplains for spiritual comfort.
If you have more questions or feel your family could benefit from this extra support, please reach out. The compassionate team at Central Coast VNA & Hospice is here to help you navigate your journey with dignity and comfort. Contact us today to learn more.
A Guide to Home Care Palliative Care
When you or a loved one faces a serious illness, the journey can feel overwhelming. Home palliative care adds a layer of support. It brings specialized medical care to your home to ease symptoms and stress.
This care works alongside your main treatments. Its goal is to improve your quality of life.
A Compassionate Approach to Serious Illness
Dealing with a serious illness is like flying a plane through a storm. Home palliative care is your co-pilot. It helps you manage the rough spots so you can live as comfortably as possible.
This specialized approach offers relief from pain and other symptoms. It also helps with the emotional weight of a serious illness.
Many people think palliative care is the same as hospice, but they are different. Palliative care is for anyone with a serious illness, at any age or stage. You can receive this support while still getting treatments to cure your condition.
While your doctor focuses on treating the illness, the palliative care team focuses on you. They manage symptoms, improve your comfort, and support your family.
Support That Comes to You
The goal of home care palliative care is to improve your life at home. This isn’t about giving up. It's about adding comfort to help you live better every day.
For over 74 years, Central Coast VNA & Hospice has been a trusted nonprofit partner for families. Our team has deep roots in Monterey County, San Benito County, Santa Cruz County, and South Santa Clara County. We are a mission-driven provider dedicated to expert, compassionate care.
This care is part of a larger system of support. To learn more, you can explore the broader aged care sector, which delivers many essential services.
What Does This Care Involve?
Home palliative care is a team effort. A group of skilled professionals works with you and your doctors. They create a care plan tailored to your needs.
This plan is holistic and addresses many challenges.
This can include:
- Pain and Symptom Control: Managing pain, fatigue, shortness of breath, and other difficult symptoms.
- Emotional and Spiritual Support: Offering counseling to help you and your loved ones cope with the illness.
- Care Coordination: Helping you understand the healthcare system and communicate with your doctors.
This approach ensures your physical, emotional, and spiritual needs are met. Bringing this support into your home reduces stressful hospital visits. To learn more, read our guide on what is palliative care.
Contact Central Coast VNA & Hospice to learn how we can support you.
The Real Benefits of Palliative Care at Home

Choosing home care palliative care offers powerful benefits. Receiving care in the comfort of your home improves well-being. It means fewer hospital visits and lets family be more involved.
This approach shifts the focus from managing an illness to living with it on your terms. You maintain daily routines and a sense of control. A dedicated team comes to you, easing the burden on loved ones.
The demand for this support is growing. According to the National Hospice and Palliative Care Organization (NHPCO), an estimated 1.72 million Medicare beneficiaries received hospice care in 2020 (NHPCO, 2021). Integrating palliative care early improves quality of life.
A Story of Independence and Dignity
Think about a gentleman we cared for in Monterey County. He was managing advanced heart failure, and hospital stays left him weak. He cherished his independence and his garden.
His doctor referred him to Central Coast VNA & Hospice. Our Registered Nurse worked with his cardiologist to adjust his medications. This reduced his shortness of breath and fatigue.
A Hospice Aide also began visiting to help with personal care. This saved his energy for the things he loved.
This support got him back to his garden. His family could share precious moments with him, knowing he was comfortable and safe.
This is the heart of what we do as a local nonprofit. Our mission is to put your goals first. We help you live life as fully as possible.
Empowering Families Through Support
Palliative care at home is a lifeline for families. Loved ones often become caregivers, which can be exhausting. Our team is here to share that load.
We support families by providing:
- Expert Guidance: We teach family members how to assist with daily care and what to look for as symptoms change.
- Emotional Relief: Our Medical Social Workers and Chaplains offer counseling and a listening ear.
- Care Coordination: We ensure everyone, from family to the primary doctor, is on the same page.
This teamwork empowers families to focus on spending quality time together. To learn more, explore the core benefits of palliative care.
Meet Your Palliative Care Support Team
When you choose home-based palliative care, you gain an entire team of experts. This team is dedicated to your well-being. You and your family are never alone on this journey.
This group works with you, your family, and your doctor. It's a circle of support in your home in Monterey County, San Benito County, Santa Cruz County, or South Santa Clara County. This team approach is key to high-quality care.
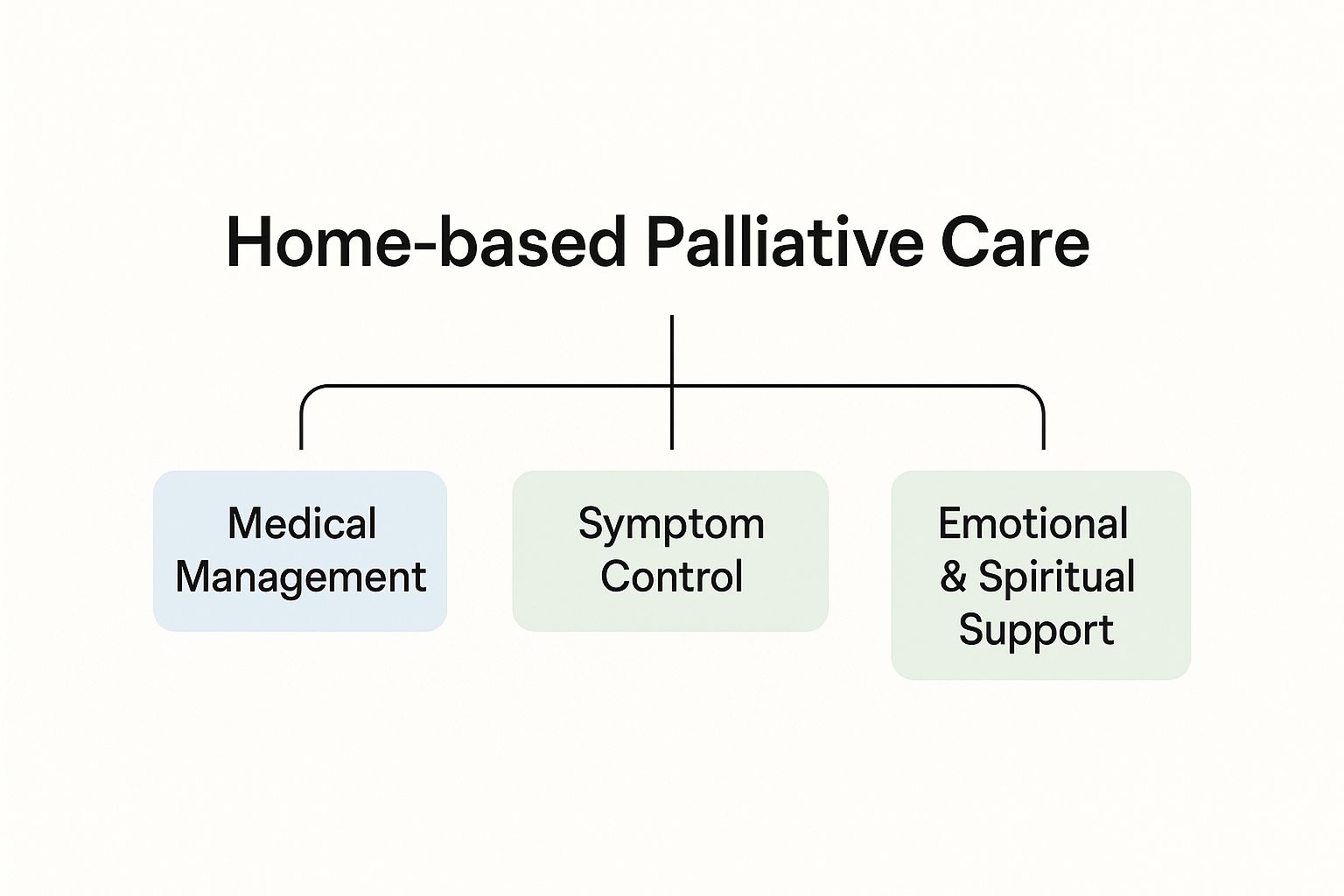
Our team’s efforts focus on medical management, symptom control, and emotional support. They are all connected to care for the whole person. The table below shows who is on your team and what they do.
Your Central Coast VNA Palliative Care Team Roles
| Team Member | Primary Role and Responsibilities |
|---|---|
| Registered Nurse (RN) | Your main point of contact for medical care. The RN manages pain and other symptoms, working with your doctor for maximum comfort. They are also your advocate and educator. |
| Medical Social Worker | Your guide through the healthcare system. They connect you with community resources, provide counseling, and assist with advance care planning. |
| Hospice Aide | The heart of the team, providing hands-on personal care with dignity. They assist with daily activities like bathing and dressing. Their presence offers comfort and relieves family. |
| Chaplain | A source of spiritual and emotional support, regardless of your beliefs. Chaplains are skilled listeners who offer a compassionate presence to help you find peace. |
Let's look at how each professional makes a difference.
The Registered Nurse
Your Registered Nurse (RN) coordinates your medical care. They are experts in managing pain and other symptoms. They work closely with your doctor to adjust treatments so you can feel your best.
An RN also listens and educates. They explain your condition and treatments in a way that makes sense. This empowers you and your family to manage health challenges.
The Medical Social Worker: Your Advocate and Guide
Navigating the healthcare system can be overwhelming. A Medical Social Worker can help. They connect you with the practical support you need.
A Medical Social Worker can help with tasks like:
- Coordinating Community Resources: Arranging services like meal delivery or transportation.
- Counseling and Emotional Support: Offering a safe space to talk through fears and anxieties.
- Advance Care Planning: Guiding you through conversations about future healthcare wishes.
Their goal is to reduce your stress. This lets you focus on your health and time with loved ones.
Providing Comfort and Personal Assistance
Hospice Aides provide hands-on personal care with dignity and respect. They assist with daily activities like bathing, dressing, and grooming. This can be challenging during a serious illness.
Their presence ensures your comfort and safety. It also gives relief to family members. You can read about the key responsibilities of a Hospice Aide on our blog.
Spiritual and Emotional Support
A serious illness often raises deep spiritual questions. Our non-denominational Chaplains are here to provide comfort. They respect your personal beliefs and values.
They are skilled listeners who offer guidance or a quiet presence. This support is for everyone, regardless of faith. A Chaplain helps you and your family find peace during a difficult time.
What Palliative Care Services Actually Look Like

Choosing home-based palliative care brings a complete support system to your home. It is designed to lift the burdens of serious illness. It improves your quality of life where you are most comfortable.
At Central Coast VNA & Hospice, our care plans are built on three pillars. These pillars work together to care for the whole person.
Expert Symptom Management
The first goal is relief. Palliative care focuses on easing difficult symptoms from a serious illness. This goes beyond just managing pain.
Our Registered Nurses are experts at managing issues, including:
- Pain Relief: Using medications and other therapies to keep you comfortable.
- Fatigue Management: Helping you conserve energy for what you love.
- Breathing Difficulties: Addressing shortness of breath.
- Nausea and Appetite Loss: Finding solutions to improve appetite.
- Anxiety and Sleeplessness: Providing support to help you rest.
A nurse might work with your doctor to adjust a medication schedule. They can also teach your family simple techniques to manage symptoms.
Compassionate Emotional and Spiritual Support
A serious illness affects your emotional and spiritual health. Our care goes deeper to offer a steady hand. It is a safe space for you and your loved ones.
Our Medical Social Workers and Chaplains are skilled listeners. They offer guidance and a comforting presence.
This care is about honoring your journey and helping you find strength. We walk alongside you, offering support whenever you need it most.
A Chaplain might help you explore questions of meaning. A Medical Social Worker can counsel your family on coping with stress.
Seamless Care Coordination
Navigating the healthcare system can feel like a full-time job. Our team steps in to be your advocate and guide. We manage the details so you can focus on your well-being.
Our teams use tools like mobile medical computer carts to keep medical information organized. This ensures everyone on your care team is always on the same page. The global need for palliative care is growing, highlighting how critical this support has become.
At Central Coast VNA & Hospice, our palliative care is part of a full continuum of support. It often bridges home health and, if needed, hospice care. This ensures you receive continuous support from a trusted, nonprofit team.
How to Get Started with Home Palliative Care
Getting the right support should not be another source of stress. Starting home palliative care is a simple process. It begins with a conversation.
A common myth is that palliative care is only for the end of life. That is not true. Anyone with a serious illness is likely eligible.
We often work with people with conditions like cancer, heart failure, or dementia. The key is whether the illness causes symptoms and stress.
Starting the Conversation with Your Doctor
The first step is to talk to your primary doctor or specialist. They understand your medical history. They can make a referral for palliative care.
Here’s how you can bring it up:
- Be direct. Ask, "Could palliative care help manage my symptoms?"
- Explain your challenges. Describe your pain, fatigue, or anxiety.
- Focus on your goals. Mention you want to improve your quality of life at home.
Your doctor can then connect you with a provider like Central Coast VNA & Hospice. Our team will work with your physician to build a coordinated care plan.
Understanding Eligibility and Coverage
Worries about cost should not stop you from getting support. Most insurance plans cover palliative care. This includes Medicare, Medi-Cal, and private insurance.
Palliative care is a recognized medical service focused on relief from the symptoms and stress of a serious illness. Its aim is to improve quality of life.
Access to this care is not the same everywhere. The World Health Organization reports many people live where palliative care is underdeveloped. You can read more about the global state of palliative care access.
We are ready to help you sort through your options. We can help you navigate insurance questions. You can also check our guide on Medicare home care eligibility.
Taking the First Step in the Central Coast
If you live in Monterey County, San Benito County, Santa Cruz County, or South Santa Clara County, getting started is easy. Central Coast VNA & Hospice is here to guide you. Our nonprofit mission and 74+ years of service ensure our community can access compassionate care at home.
Call us for a consultation. Our team can answer questions and coordinate with your doctor. We can help you decide if home palliative care is the right choice.
Frequently Asked Questions About Home Palliative Care

Exploring home palliative care brings up many questions. It is normal to want a clear picture of this support. We’ve gathered answers to common questions from our neighbors.
Our goal is to help you feel confident and informed. Each answer is grounded in the expert, patient-first approach of Central Coast VNA & Hospice.
Is Palliative Care the Same as Hospice?
No, they are not the same. While both focus on comfort, they serve different needs at different times. The key difference is that you can receive palliative care at any stage of a serious illness, even while seeking curative treatment. Hospice care is for when curative treatments are no longer working or wanted, focusing entirely on comfort at the end of life.
Can I Keep My Own Doctor?
Yes, absolutely. Our palliative care team works with your existing doctors. We act as an extra layer of support, communicating regularly with your primary doctor to ensure your care is coordinated.
How Are Family Members Supported?
A serious illness affects the entire family, and our support extends to them. Our Medical Social Workers and Chaplains provide emotional support, practical guidance, and connections to community resources. We help prevent burnout and build a stronger circle of care at home.
What Does a Typical Home Visit Look Like?
A home visit is focused, unhurried time dedicated to you. A Registered Nurse will check your vitals and discuss how you've been feeling, including pain, energy levels, and appetite. Based on your needs, they may adjust medications in coordination with your doctor or teach you new ways to manage symptoms, always leaving time to answer your questions.
How Do I Start This Conversation with a Loved One?
Approach the topic gently, framing it as adding support, not giving up. You could say, “I learned about something called palliative care—it's a team that works with your doctor to help with symptoms like pain. It’s an extra layer of support to help you feel stronger.” Emphasize that it is not hospice and that they remain in control of all healthcare decisions. For more answers, please see our palliative care FAQs.
Home Care Palliative Care: A Guide for Families
When a loved one faces a serious illness, medical treatments often take center stage. But what about the stress, discomfort, and emotional strain? This is where home care palliative care can help.
Palliative care is specialized medical support focused on relief. It eases the symptoms and stress of a serious illness, all in the comfort of home. Many people think it is the same as hospice, but it is not. Palliative care is available at any stage of an illness, even while you are getting treatments to cure your condition.
An Extra Layer of Comfort and Support

Think of it this way: your main doctor focuses on treating the disease. Palliative care adds another layer of support to improve your quality of life. The goal is to focus on what matters most to you.
For over 74 years, Central Coast VNA & Hospice has provided this kind of compassionate care. As a local nonprofit, our mission is to deliver expert medical care that honors your wishes. We proudly serve families in Monterey County, San Benito County, Santa Cruz County, and South Santa Clara County.
What Does Palliative Care Actually Do?
Palliative care treats the whole person, not just the illness. It helps with symptoms that make daily life a struggle. This frees you up to focus on your health and loved ones.
At its heart, home palliative care is a philosophy that puts you first. It shares ideas with person-centred therapy by valuing your comfort, dignity, and personal goals.
So, what does that support look like? It can include:
- Symptom Management: Helping with pain, nausea, fatigue, or shortness of breath.
- Emotional Support: Offering guidance to cope with the stress of a serious diagnosis.
- Clear Communication: Helping you and your family understand medical information and make decisions.
This special focus can make a big difference in your daily life. You can learn more about what palliative care is and how it empowers patients.
Palliative Care at a Glance
To clear up any confusion, here is a simple breakdown of what home care palliative care is and what it is not.
| Palliative Care Is... | Palliative Care Is Not... |
|---|---|
| An extra layer of support. | A replacement for your doctor. |
| Focused on quality of life. | Giving up on treatment. |
| For any stage of a serious illness. | Only for the end of life. |
| About the whole person's comfort. | Just about managing pain. |
It is about adding more life to your days, not just days to your life. This is the heart of our mission at Central Coast VNA & Hospice.
The Real Benefits of Choosing In-Home Care
Receiving palliative care at home is a choice centered on comfort and dignity. When you are dealing with a serious illness, being in your own space is powerful. It is about creating an environment where you can feel at peace.
Bringing care into the home means you can keep your own routines. You can sleep in your own bed and stay connected to your memories. This sense of normalcy helps reduce stress and anxiety.
Comfort and Familiarity
There is a special kind of healing that happens at home. Simple things, like sitting in a favorite chair or having a pet nearby, can improve your well-being. This familiar setting helps reduce stress.
In-home palliative care brings expert medical support into your personal space. The care adapts to you and your life. This approach helps you hold onto your independence and feel more in control.
Personalized Symptom Management
A big advantage of palliative care at home is personalized symptom management. Our Registered Nurses work with you and your doctors to control pain, nausea, and other symptoms. This focused attention can prevent symptoms from getting worse and reduce the need for emergency room trips.
This proactive approach keeps your quality of life as the top priority. To learn more, you can see the benefits of our palliative care services for patients and families.
Keeping Families Together
When care happens at home, the whole family is more involved. Loved ones can be present without hospital visiting hours. This strengthens family bonds during a difficult time.
Our team at CCVNA is there for the entire family. We offer education and guidance to help family members feel more confident in their roles. This creates a circle of support that nurtures everyone.
By bringing professional medical services into the home, we create an environment where patients feel secure and families feel supported.
The need for this type of care is growing. The global palliative care market was valued at USD 15.11 billion in 2023. It is expected to grow to USD 32.51 billion by 2033 (Straits Research, 2024). You can discover more about this expanding market and its trends.
Meet Your Dedicated Palliative Care Team
You should not have to face a serious illness alone. With Central Coast VNA & Hospice, a team of compassionate professionals is ready to support you. This team works together to address every part of your well-being.
Your CCVNA team is always in communication. This ensures your care is coordinated and complete. It helps manage medical needs while also supporting your emotional and spiritual health.
The Core of Your Support System
Each person on your palliative care team has unique skills. They all share one goal: improving your quality of life. They are experts at listening and creating a care plan that respects your wishes.
Your dedicated support team makes a world of difference. To help you understand their roles, we have outlined the key professionals who will be by your side.
Your CCVNA Palliative Care Support Team
This table shows the roles of each professional on your care team.
| Team Member | Primary Role and Support Provided |
|---|---|
| Registered Nurse (RN) | Your main clinical contact. The RN is an expert in managing symptoms like pain and fatigue. They work with your doctor to adjust medications for comfort at home. |
| Medical Social Worker | Your guide for practical and emotional challenges. The social worker connects you to community resources and offers counseling for you and your family. |
| Chaplain | A source of spiritual comfort, no matter your beliefs. Our chaplains offer a listening ear and support that aligns with your personal values. |
| Hospice Aide | Provides hands-on personal care. Aides can help with daily activities like bathing and dressing, ensuring you maintain your dignity and comfort at home. |
This team approach ensures you get the right care at the right time.
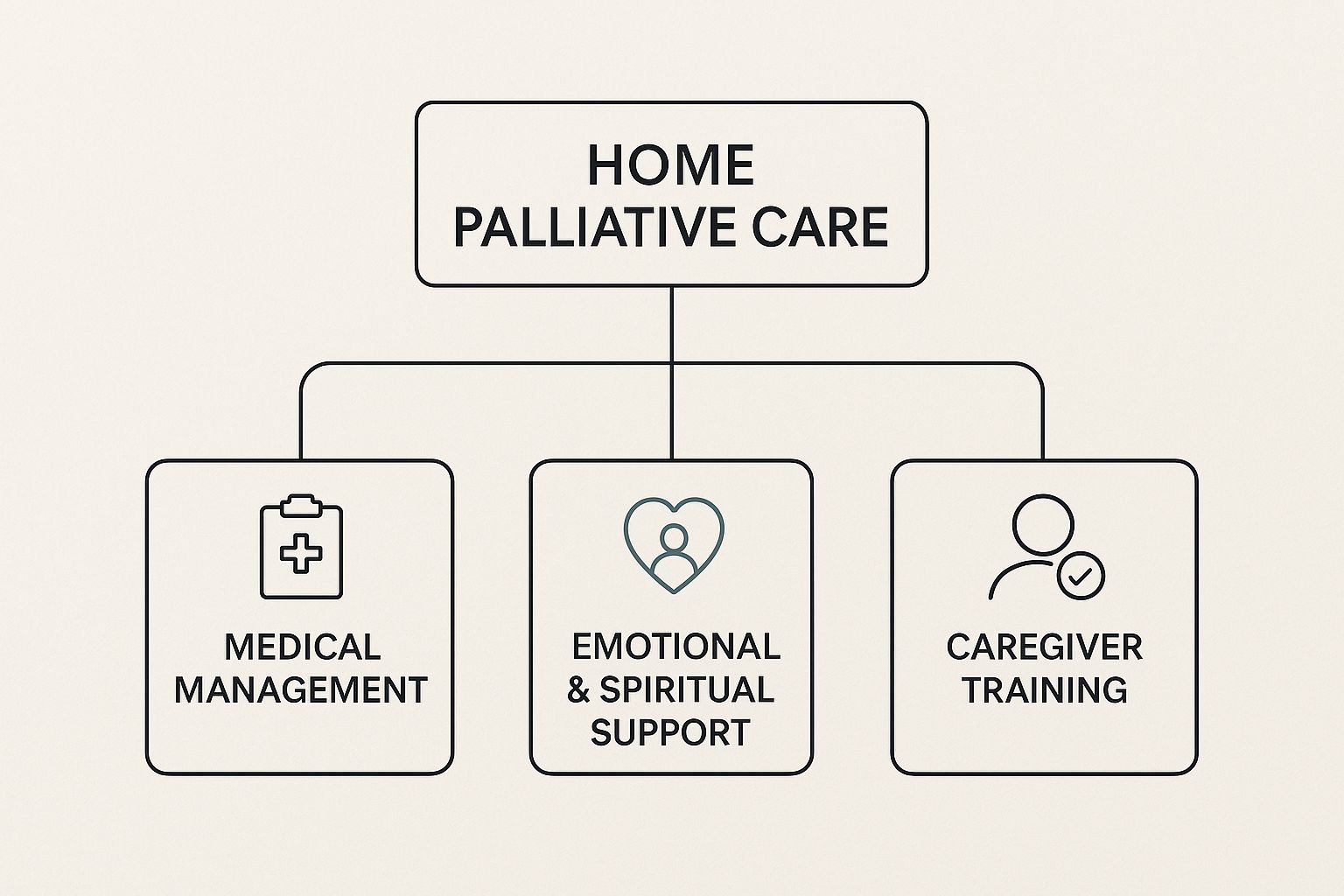
How Your Team Works Together
Think of your team as a hub with you and your family at the center.
For example, a Registered Nurse may notice a new symptom during a visit. They will talk to your physician to adjust your medication. They might also let the Medical Social Worker know, who can then check on your family.
This constant communication ensures nothing is missed. It allows for proactive care that anticipates your needs. To learn more about a nurse's duties, see what a home care nurse does.
The strength of our team is its ability to see the whole person, not just symptoms. We combine medical, emotional, and spiritual expertise to honor each individual.
What Services Our Home Care Program Includes

What does palliative care look like day-to-day? It is a complete system of support. It is designed to tackle physical, emotional, and practical challenges.
The goal is to improve your quality of life. Our home care palliative care program at Central Coast VNA & Hospice brings this support to you. We focus on providing practical help that makes a real difference.
Expert Pain and Symptom Management
The first priority is relief from symptoms. Pain, shortness of breath, and fatigue can drain your energy. Our skilled Registered Nurses are experts at managing these issues at home.
They work with your doctor to create a personalized plan. This proactive approach can reduce the need for emergency room visits. You can learn more about our approach to pain and symptom management.
Medication Management and Coordination
Juggling many medications can be confusing. Our team helps simplify everything. A Registered Nurse will help organize your medications and watch for side effects.
This coordination is a key part of our home care palliative care. We communicate with your doctors and pharmacy to make sure everyone is on the same page. This gives you peace of mind.
Emotional and Spiritual Support
A serious illness affects your emotional and spiritual well-being. Our team includes Medical Social Workers and Chaplains. They provide a safe space for you and your family to work through these feelings.
This support is tailored to your personal beliefs. Our compassionate professionals can help with:
- Coping Strategies: Providing tools to manage stress, anxiety, or sadness.
- Family Communication: Helping with tough conversations and empowering family members.
- Spiritual Comfort: Offering a listening ear to help you find meaning, peace, and hope.
Our commitment is to care for the whole person—body, mind, and spirit. We help patients and their families find strength and resilience.
Guidance with Difficult Decisions
Navigating the healthcare system can feel overwhelming. Your palliative care team acts as your guide. We help you understand your treatment options so you can make choices that align with your goals.
We help you clarify what is most important to you. Then, we make sure your entire medical team understands and respects your wishes. This keeps you in control of your healthcare journey.
How to Get Started with Palliative Care
Taking the first step toward getting support is simpler than you might think. The journey begins with a conversation.
Palliative care usually starts with a referral from a doctor. You can also advocate for yourself or a loved one. Just ask your doctor, "Could palliative care help us?"
Who Is Eligible for Palliative Care
Eligibility for palliative care is based on need, not prognosis. This is a big difference from hospice care. Palliative support is for anyone with a serious illness who is struggling with symptoms or stress.
You can receive palliative care at any age and at any stage of an illness. The main qualification is the need for an extra layer of support. For more details, see our referral information for healthcare professionals and families.
Understanding How Care Is Paid For
Worries about cost should not prevent you from getting support. Home palliative care services are covered by most insurance plans. This makes this vital care accessible in our community.
Here is a quick look at common coverage options:
- Medicare Part B: This usually covers palliative care services from doctors and nurse practitioners.
- Medi-Cal: California's Medicaid program also covers palliative care.
- Private Insurance: Most private health insurance plans include benefits for palliative care.
Our team at Central Coast VNA & Hospice can help you understand your insurance benefits. As a nonprofit serving our community for over 74 years, our mission is to ensure everyone has access to care.
Palliative care is a right, not a luxury. It is specialized medical care to provide relief and support so every patient can live with dignity.
However, access to this care is a global challenge. A 2024 study found that 69% of countries are in the early stages of developing palliative care services (Lupu et al., 2024). You can learn more about these global palliative care findings and see why expanding access is so important.
Taking the Next Step
Getting started is as simple as reaching out. If you or a family member live with a serious illness in Monterey County, San Benito County, Santa Cruz County, or South Santa Clara County, we are here to help.
Contact Central Coast VNA & Hospice today. Our compassionate team is ready to answer your questions about our home care palliative care program.
Understanding Palliative Care Versus Hospice

One of the biggest points of confusion for families is the difference between palliative care and hospice. Both focus on comfort, but they serve different needs at different times. Understanding this is key to making informed decisions.
A simple way to remember the difference is: all hospice care is palliative, but not all palliative care is hospice.
Both services aim to relieve symptoms and reduce stress. They are different stages of a journey, each offering unique support when it is needed most.
When Care Can Begin
The biggest difference is timing and the goals of treatment. Palliative care can start as soon as someone is diagnosed with a serious illness. A patient can receive this support for months or years while continuing curative treatments.
Hospice care begins when curative treatments are no longer working or have been stopped. It is for people with a life expectancy of six months or less. The focus of hospice shifts to ensuring comfort and peace in the final chapter of life.
Goals of Care
The goals of each type of care are also different.
- Palliative Care: The goal is to provide relief from symptoms while you continue to fight the illness. It works alongside your regular doctors.
- Hospice Care: The goal is to provide comfort and dignity when a cure is no longer the focus. It is about making the most of the time that remains.
Understanding this helps you get the right support at the right time.
A Seamless Continuum of Care
At Central Coast VNA & Hospice, we are the only organization on the Central Coast that provides home health, palliative care, and hospice. This creates a Continuum of Care. It allows for a smooth transition between services as a patient’s needs change.
By offering both palliative and hospice services, we ensure that as a patient's journey changes, their care team can remain consistent. This brings peace of mind to families.
If a patient receiving our home care palliative care decides to stop curative treatments, they can move directly to our hospice program. They keep the same familiar nurses, aides, and social workers. For families in Monterey County and our surrounding communities, this consistency is a great comfort.
Frequently Asked Questions About Home Palliative Care
Making decisions about care can feel overwhelming. It is normal to have questions. Here are some straightforward answers to questions we often hear from families.
Can I keep my own doctor if I start palliative care?
Yes, absolutely. Palliative care is an extra layer of support that works with your current doctors, not as a replacement. Our team coordinates directly with your primary physician and specialists to ensure your care is seamless.
When is the right time to start palliative care?
The best time to start palliative care is as early as possible after a serious diagnosis. Starting early helps manage symptoms from the beginning and reduces stress. Patients can receive this supportive care for many months or even years.
Is palliative care only for people who are dying?
No, this is a common misunderstanding. Palliative care is for anyone at any stage of a serious illness, regardless of their prognosis. You can receive palliative care while also getting treatments meant to cure your condition.
Does home care palliative care also support the family?
Yes, supporting the family is a core part of what we do at Central Coast VNA & Hospice. Our team provides emotional and spiritual support to family members. We also offer education and practical guidance to help them feel more prepared.
How is palliative care paid for?
Most insurance plans cover palliative care services. This includes Medicare Part B, Medi-Cal, and many private insurance policies. Our team at CCVNA is here to help you understand your benefits and navigate your coverage.
For over 74 years, Central Coast VNA & Hospice has been the trusted nonprofit provider of compassionate care for families in Monterey County, San Benito County, Santa Cruz County, and South Santa Clara County. If you have more questions or feel that our services could help your family, please reach out.
Contact us today to learn more about our home health, palliative, and hospice services at https://ccvna.com.
A Guide to Home Care Palliative Care
Dealing with a serious illness can be tough. The words “palliative care” might sound confusing or scary.
But home care palliative care is simply an extra layer of support. It is designed to improve your quality of life in your own home. It is not the same as hospice and can be started at any stage of an illness.
A Supportive Co-Pilot for Your Healthcare Journey
Think of managing a serious illness like flying a plane in a storm. Your main doctor is the captain, focused on treating the disease. A palliative care team is like your supportive co-pilot.
Their job is to make your journey as comfortable as possible. They help you manage the turbulence—like pain, stress, and other symptoms. This makes the flight smoother for you and your family.
This special medical care helps everyone cope. It provides relief from the symptoms and stress of the illness.
Palliative Care Is Not Hospice
Many people think palliative care is only for the end of life. This is a common myth.
You can start palliative care at any time after a diagnosis. This can happen even while you get treatments to cure your illness. The focus is on living as well as you can, for as long as you can.
You can learn more in our detailed guide on what is palliative care.
Local, Compassionate Support on the Central Coast
For over 74 years, Central Coast VNA & Hospice has been a trusted nonprofit partner for local families. Our mission is to bring compassionate support right to your home. This helps make a difficult time more manageable.
We proudly serve residents in Monterey County, San Benito County, Santa Cruz County, and South Santa Clara County.
Our dedicated team of Registered Nurses and other professionals works with you and your doctors. We create a care plan that aligns with your personal goals. This team approach ensures you get the best care at home.
The Real Benefits of Receiving Care at Home
Choosing palliative care at home has big advantages. It's about more than just convenience.
It puts you in control of your life, surrounded by what you love. This sense of normalcy is often lost in a hospital.
The main goal of home palliative care is to manage your symptoms where you live. This means getting expert help for pain or fatigue without stressful trips to a clinic. Our teams bring this medical support to your door.
Personalized Comfort and Dignity
At home, care becomes more personal. A hospital has a set schedule, but home care adapts to your routines. Your comfort is the top priority.
This focus on your needs helps preserve your dignity. You decide when to wake up, what to eat, and who visits. All of this happens while you receive expert care from our team.
Our Registered Nurses and Medical Social Workers work with you. They create a plan that respects your wishes. You can learn more about the benefits of palliative care and how it improves daily life.
Reducing Stress for Patients and Families
Hospital visits can be a huge source of stress. Home palliative care is designed to reduce this burden.
Our team manages symptoms proactively. This can prevent a crisis before it starts and brings stability to the family. Having a professional team visit the home gives families peace of mind.
This allows the family to focus on quality time together. It shifts the focus from appointments and travel to connection and comfort.
Greater Family Involvement and Support
When care is at home, your family can be more involved. They become partners in your comfort. They learn from our team how to best support you.
Our Medical Social Workers also support the entire family. They offer counseling and connect you with community resources. They also help with important conversations about care goals.
This support network includes:
- Emotional Support: Helping family members cope with stress and emotions.
- Education: Teaching loved ones about the illness and how they can help.
- Resource Coordination: Connecting you to services in Monterey County or our other service areas.
Central Coast VNA & Hospice empowers your family to face the journey together.
Who Is on Your Palliative Care Team
You should not have to go through a serious illness alone. With home care palliative care, a dedicated team surrounds you. They create a circle of support for you and your family.
Central Coast VNA & Hospice brings this team care to your home. Our team members are your neighbors, serving the Central Coast community. They partner with your doctor to ensure your care is in sync with your goals.
Your palliative care team is built around you. Each professional has a unique skill. But they all share one goal: to improve your quality of life.
Your Central Coast VNA & Hospice Palliative Care Team
| Team Member Role | Primary Responsibilities |
|---|---|
| Registered Nurse (RN) | Manages pain and physical symptoms, gives medications, and educates patients and families. |
| Medical Social Worker | Provides emotional support, helps with advance care planning, and connects you to community resources. |
| Chaplain | Offers non-denominational spiritual support and a listening ear for you and your family. |
The Role of Your Registered Nurse
Your Registered Nurse (RN) is your main contact for clinical care. They are skilled at managing complex physical symptoms.
They work with you and your doctor to create a medication plan. This ensures you get relief as quickly as possible. Your nurse is also your teacher and advocate.
The Support of Your Medical Social Worker
A serious illness affects your emotional health. Your Medical Social Worker provides crucial support.
They are trained to help you and your loved ones navigate stress. They are also experts at guiding you through the healthcare system. Your Medical Social Worker is your champion.
The Guidance of Your Chaplain
Spiritual well-being is a vital part of health for many people. Our Chaplains provide non-denominational spiritual support. They honor your individual beliefs and values.
They offer a comforting presence and a safe space to explore your feelings. This support extends to your entire family.
You can find more information on our palliative care program and its team approach.
What Services Home Palliative Care Includes
You may wonder what home care palliative care looks like day-to-day. It is a practical, compassionate service that addresses the whole person. It is all about making each day better.
Palliative care at home brings comfort back into your life. It is not a one-size-fits-all service. The goal is to improve your quality of life.
Expert Pain and Symptom Management
One of the first benefits is relief from physical symptoms. A serious illness often comes with pain, nausea, or fatigue.
Our skilled Registered Nurses are experts at managing these issues at home. They work with you and your doctor to create a personal plan. This proactive approach means fewer stressful trips to the hospital.
You can learn more about our approach to pain and symptom management.
Emotional and Spiritual Support for Everyone
A serious illness also takes an emotional and spiritual toll. Palliative care provides dedicated support for these important needs.
Our team includes Medical Social Workers and Chaplains. They offer a compassionate ear and a safe space for your family.
- Emotional Support: Medical Social Workers provide counseling to help you cope with stress or anxiety.
- Spiritual Guidance: Our Chaplains offer non-denominational spiritual care that honors your personal beliefs.
This support extends to the entire family. It helps everyone communicate better during a difficult time.
Help with Difficult Decisions and Planning
The healthcare system can feel like a maze. The palliative care team acts as your advocate and guide. They make sure your voice is heard.
Our team helps with important conversations about your goals. This process is called advance care planning. It puts you in control of your choices.
Your team can help you complete documents like an advance directive. This ensures your wishes are clear to your family and doctors. This guidance provides clarity and lifts a heavy burden from your family.
How to Get Started with Palliative Care
Taking the first step to get extra support can feel hard. But starting home care palliative care is easier than most people think. Many families wait because of common myths.
Palliative care is not about giving up. It's about gaining support to make life better. This care is for anyone, at any age or stage of an illness.
Understanding Who Is Eligible
Eligibility for palliative care is based on need, not a timeline. If you are dealing with the stress of a serious illness, you are likely eligible. This care works alongside your current treatments.
You might be a good candidate if you experience:
- Difficult symptoms like pain, fatigue, or nausea.
- Frequent trips to the hospital.
- Emotional distress tied to your illness.
- A need for help with complex medical decisions.
Your Simple Steps to Begin
Getting started is a proactive step toward peace of mind. The process starts with a simple conversation.
Here’s how to get the ball rolling:
- Talk to Your Doctor: Have an open conversation with your physician. Ask, “Would palliative care be right for me?”
- Request a Referral: Your doctor can refer you to a provider like Central Coast VNA & Hospice. We work directly with your doctor’s office. You can point them to our referral information for providers.
- Schedule an Initial Visit: A member of our team will call you to set up a visit in your home. This is our chance to listen and for you to ask questions.
Taking this first step puts you back in control. It ensures your comfort is at the center of your healthcare journey.
Covering the Cost of Care
Worries about cost should not stop you from getting support. Palliative care is a medical specialty. It is covered by most insurance plans.
This essential care is covered by:
- Medicare Part B
- Medi-Cal
- Most private insurance plans
Central Coast VNA & Hospice is a nonprofit organization. Our commitment is to serve everyone in Monterey County, San Benito County, Santa Cruz County, and South Santa Clara County. Our team can help you understand your coverage.
Your Trusted Partner in Compassionate Care
Navigating a serious illness is easier with a true partner. It feels less overwhelming with a team dedicated to your comfort and dignity. This is the heart of home care palliative care.
For over 74 years, Central Coast VNA & Hospice has been that trusted nonprofit partner for local families. We proudly serve our neighbors across Monterey County, San Benito County, Santa Cruz County, and South Santa Clara County.
A Legacy of Local, Nonprofit Service
Because we are a nonprofit, our sole focus is on you. We measure success in the quality of life we help restore. That commitment has been our guide for over seven decades.
Choosing a care partner means choosing someone who understands your community. It’s about finding a team dedicated to putting your needs first. At Central Coast VNA & Hospice, we offer a seamless Continuum of Care.
The Continuum of Care You Can Rely On
We know healthcare needs can change. Your care plan should adapt without adding more stress. We are the only provider on the Central Coast offering a full spectrum of home-based services.
This means we can smoothly transition your care as your needs evolve:
- Home Health: Skilled support to help you recover at home.
- Palliative Care: An extra layer of comfort at any stage of a serious illness.
- Hospice Care: Compassionate support focused on dignity at the end of life.
This integrated approach offers stability for you and your family. You get consistent care from a team you know and trust.
Contact Central Coast VNA & Hospice today. Learn how our compassionate team can help you and your family.
Frequently Asked Questions About Home Palliative Care
It's normal to have questions when making healthcare decisions. Here are clear answers to some common questions about home care palliative care.
1. Is palliative care the same as hospice?
No, they are different. Palliative care is an extra layer of support that can start at any stage of a serious illness, even during curative treatment. Hospice care is for individuals with a life expectancy of six months or less, when curative treatments are no longer the focus.
2. Can I keep my own doctor?
Yes, absolutely. The palliative care team works with your primary doctor and specialists, not in place of them. They are an added layer of support to your existing medical team.
3. How is home palliative care paid for?
Palliative care is a medical specialty and is covered like other medical services. It is typically paid for by Medicare Part B, Medi-Cal, and most private insurance plans. As a nonprofit, CCVNA helps ensure care is accessible to all who need it in our service area.
4. When is the right time to start palliative care?
The best time to start is as soon as you feel you need more support. If symptoms or stress from a serious illness are affecting your daily life, it's the right time to talk to your doctor. Starting earlier often leads to better quality of life for a longer time.
5. What is the difference between home health and palliative care?
Home health care is usually short-term, skilled care to help you recover from a specific event, like surgery. Palliative care is long-term support focused on managing symptoms of a serious, chronic illness to improve comfort and quality of life.
6. Who is on a palliative care team?
A typical palliative care team includes a Registered Nurse to manage physical symptoms, a Medical Social Worker for emotional support and resource connection, and a Chaplain for spiritual guidance. This team works together to support the patient and their family.
7. Does palliative care mean I'm giving up?
Not at all. Palliative care is about adding a layer of support to help you live as well as possible while you continue to navigate your illness. It focuses on improving your quality of life, no matter what your prognosis is.
Navigating a serious illness is a journey you don’t have to take alone. With Central Coast VNA & Hospice, you have a compassionate, local partner dedicated to your comfort and quality of life. Contact us today to learn how our home palliative care team can support you and your family. Learn more at ccvna.com.
Why Central Coast VNA Is the Best Choice for Palliative Care
When you or a loved one are facing a serious illness, navigating healthcare options can feel overwhelming. The goal is to find compassionate, expert care that relieves symptoms and improves quality of life.
Palliative care is designed to do just that. It offers an extra layer of support that focuses on comfort and dignity alongside other medical treatments. On the Central Coast, one provider stands above the rest with a legacy of trust.
This article will explore why Central Coast Vna & Hospice is the best choice for palliative care on the Central Coast. We will detail the unique benefits that set them apart, from their full continuum of care to their nonprofit, mission-driven philosophy.
While Central Coast VNA focuses on enhancing comfort and quality of life through palliative care, it's also important to consider broader aspects of future care. For those seeking guidance on all decisions, you can explore a comprehensive end-of-life planning guide. Read on to discover why thousands of families in Monterey, San Benito, Santa Cruz, and South Santa Clara counties trust Central Coast VNA & Hospice.
1. The Only Local Provider Offering a Full Continuum of Care
Navigating healthcare for a serious illness can be fragmented and stressful. Families often find themselves coordinating between different agencies for various levels of care.
Central Coast VNA & Hospice (CCVNA) stands out as the best choice for palliative care on the Central Coast because it eliminates this challenge. As the only local provider offering a full continuum of care, CCVNA provides integrated Home Health, Palliative, and Hospice services under one roof.
This unified structure means patients and their families experience seamless, consistent support from a single, trusted team. There is no need to switch providers or re-explain a complex medical history as care needs evolve. The focus remains entirely on the patient's comfort and quality of life.
How the Continuum of Care Benefits Patients
Imagine a patient receiving Home Health services from a CCVNA Registered Nurse after a hospital stay. As their illness progresses, they may begin to experience symptoms that require more specialized management.
With CCVNA, the transition to palliative care is a simple, internal process.
- Seamless Transitions: The patient’s existing care team coordinates directly with the palliative team, ensuring a smooth handoff.
- Consistent Support: The clinicians who manage the transition are already familiar with the patient’s history, values, and care goals.
- Unmatched Peace of Mind: This continuity provides reassurance for families in Monterey, San Benito, Santa Cruz, and South Santa Clara counties.
This integrated approach is a cornerstone of why Central Coast VNA & Hospice provides exceptional palliative care. It prioritizes the patient’s journey above all else. You can explore the specifics of their patient-centered approach and learn more about palliative home care services on ccvna.com.
2. Specialized, In-Home Care for Patients with Serious Illness
Palliative care from Central Coast VNA & Hospice delivers personalized, team-based medical care at home. This means patients can receive comfort-focused support where they feel most secure, whether in their private residence or an assisted living facility.
The program is built to relieve pain, manage symptoms, and enhance overall quality of life. Care is provided alongside any curative treatments a patient may be receiving. This extra layer of support helps patients and their families navigate the challenges of a serious illness with greater ease.
Unlike generic health portals, the CCVNA site is dedicated to the local communities of Monterey, San Benito, Santa Cruz, and South Santa Clara counties. It directly addresses the needs of Central Coast residents. This local focus ensures that the information is relevant and actionable.
An Expert Team Focused on the Whole Person
Central Coast VNA & Hospice’s care is delivered by an expert interdisciplinary team. This group works together to address the complete needs of each patient and their family.
The team includes:
- Palliative physicians
- Nurse practitioners
- Skilled nurses
- Social workers
- Chaplains
These professionals address not just physical symptoms, but also the emotional, social, and spiritual needs of the whole person. By visiting the site, you can cut through the noise and get answers straight from the source. You can gain a deeper understanding by reading about the differences between palliative care and hospice on ccvna.com.
3. A Nonprofit, Mission-Driven Approach with a 74+ Year Legacy
When choosing a palliative care provider, trust and verification are paramount. Central Coast VNA & Hospice’s 74+ year legacy as a nonprofit organization is a key reason why it is the best choice for palliative care on the Central Coast.
As a mission-driven provider, CCVNA’s decisions are guided by compassion, dignity, and accessibility—not by profit margins. This approach ensures that patient well-being always comes first. The organization is supported by community donors who believe in its mission to serve families across the Central Coast.
 Hospice and Palliative Care Organization website showing the Central Coast VNA & Hospice provider listing." />
Hospice and Palliative Care Organization website showing the Central Coast VNA & Hospice provider listing." />This commitment to community service is validated by external organizations. The National Hospice and Palliative Care Organization (NHPCO) is a leading authority in the field. CCVNA’s listing in the NHPCO directory confirms it meets rigorous national standards and is accredited by The Joint Commission.
How a Nonprofit Focus Benefits Families
For families making critical decisions, choosing a nonprofit provides peace of mind. It ensures the focus remains squarely on patient comfort and quality of life.
- Verified Credentials: CCVNA is accredited by The Joint Commission, a nationally recognized symbol of quality and safety.
- Clear Service Scope: The NHPCO listing explicitly outlines that CCVNA provides a comprehensive palliative care program.
- Community Roots: Serving the community for over 74 years demonstrates a deep, long-standing commitment to local families.
Using trusted national resources can help you understand the important distinctions between different types of care. You can learn more about the differences between palliative and hospice care at ccvna.com.
4. Strong Local Partnerships and Community Trust
Strong community partnerships are crucial for delivering coordinated healthcare. The affiliation between Central Coast VNA & Hospice and Salinas Valley Health showcases a deep-rooted collaboration between two of the region's most trusted healthcare names.
This partnership solidifies why Central Coast VNA is the best choice for palliative care on the Central Coast. It offers patients a clear and reliable pathway to continued care after a hospital stay.

For families connected with Salinas Valley Health, this partnership serves as a bridge. It introduces them to CCVNA as the designated partner for home health, palliative, and hospice services. The affiliation provides immense credibility and peace of mind.
How This Partnership Benefits Patients
When a patient is discharged from the hospital, the transition home can be stressful. This partnership streamlines that process, ensuring care is continuous and well-coordinated.
- Enhanced Credibility: The endorsement from a major health system like Salinas Valley Health gives families confidence in CCVNA’s quality of care.
- Streamlined Referrals: The affiliation simplifies the process for hospital staff to connect patients directly with CCVNA’s services.
- Clear Contact Information: The page provides direct phone numbers, making it easy for patients and families to reach the appropriate CCVNA team.
This collaboration is a testament to CCVNA’s respected position in the local healthcare ecosystem. You can view the partnership details on the Salinas Valley Health affiliate page.
5. Endorsed by Trusted Community Resources
For families starting their search for palliative care, finding trustworthy information is essential. The Hospice Giving Foundation serves as a key community partner, offering a directory of local hospice and palliative care providers.
This foundation is dedicated to educating families and ensuring they can make informed decisions. It is an invaluable starting point for anyone exploring their care options.
The foundation’s website provides clear resources that help distinguish between different types of care. By featuring established local nonprofits like Central Coast VNA & Hospice, it empowers families to connect with reputable providers in Monterey, San Benito, and Santa Cruz Counties.
How Local Directories Benefit Patients
Imagine a family is new to the area or unfamiliar with palliative care. The Hospice Giving Foundation’s resource page acts as a trusted guide.
- Region-Specific Listings: The directory is focused exclusively on the Central Coast, eliminating confusion.
- Educational Clarity: It provides clear explanations of care types, helping families identify the right fit for their needs.
- Direct Provider Contact: The website lists direct phone numbers, making it easy to reach out to providers like CCVNA.
This community endorsement underscores CCVNA’s deep roots and trusted presence. You can explore the foundation’s provider list and educational materials on the Hospice Giving Foundation website.
6. Accessible and Positively Reviewed by the Community
Practical access and community feedback also play a crucial role when choosing a provider. Yelp offers a valuable window into the real-world experiences of local families.
It serves as a straightforward resource for confirming office details and gauging recent community sentiment for Central Coast VNA & Hospice.
For families in Salinas, King City, or surrounding areas, Yelp provides instant access to contact numbers, hours, and maps. This makes the first step of reaching out for help much easier. Reading reviews can also offer insights into the compassionate interactions that define CCVNA’s care.
How Yelp Helps Families Connect with Care
Navigating a serious illness is complex. Finding the right local office shouldn't add to the burden.
- Verified Local Presence: Easily find and confirm the addresses for offices in Salinas and King City.
- Direct Communication: Use the click-to-call feature on a mobile device to immediately connect with CCVNA staff.
- Community Perspectives: Read unfiltered reviews from other community members to get a sense of their personal experiences.
This grassroots feedback complements the professional accolades of CCVNA. You can see what community members are saying by visiting the CCVNA Yelp page.
7. Transparent and User-Friendly Information
One of the most significant stressors for families is understanding potential costs. Olera.care addresses this concern by providing rare, upfront pricing estimates for home care and home health services.
This platform offers a consumer-friendly profile of Central Coast VNA & Hospice. It is a valuable tool for initial financial planning.
By presenting an estimated hourly rate, Olera.care helps families establish a rough budget before making the first call. This transparency shows a commitment to helping families make informed decisions from the very beginning.
How to Use Olera.care for Preliminary Planning
While final costs depend on specific care needs and insurance, Olera.care is an excellent starting point. It provides a financial baseline and demystifies a part of the healthcare process that is often unclear.
- Budgeting: Use the estimated pricing to get a general idea of private pay costs for home health services.
- Provider Comparison: Review CCVNA’s profile alongside other local options to understand the landscape.
- Informed Questions: Prepare a list of financial questions to discuss during a consultation with CCVNA.
This aligns with CCVNA’s mission to make high-quality care accessible and understandable. You can view the CCVNA profile directly on Olera.care.
Take the Next Step Toward Comfort and Support
Navigating a serious illness is a profound challenge. As we've explored, Central Coast VNA & Hospice is the best choice for palliative care on the Central Coast for several key reasons.
Its status as the only local provider offering a full continuum of care ensures seamless transitions. This integration means you receive consistent, coordinated support without the stress of changing providers as your needs evolve.
The strength of CCVNA also lies in its expert interdisciplinary team. This dedicated group of professionals addresses the whole person, managing physical symptoms while providing critical emotional, social, and spiritual support.
CCVNA’s 74+ year legacy as a nonprofit, mission-driven organization is a testament to its commitment to the community. This dedication ensures that care is guided by compassion, not profit. It’s about preserving dignity and empowering you to live your best possible life.
Frequently Asked Questions (FAQs)
1. What is palliative care?
Palliative care is specialized medical care for people living with a serious illness. It focuses on providing relief from the symptoms and stress of the illness to improve quality of life for both the patient and the family. It can be provided at any age and at any stage of an illness, and it can be delivered alongside curative treatment.
2. Who is on the Central Coast VNA & Hospice palliative care team?
Our palliative care team is an interdisciplinary group of experts. It includes palliative physicians, nurse practitioners, skilled nurses, social workers, and chaplains who work together to address the physical, emotional, social, and spiritual needs of each patient.
3. Does palliative care mean I am giving up on other treatments?
No, not at all. Palliative care is provided along with curative treatments. Its goal is to provide an extra layer of support to manage symptoms and improve your quality of life while you continue to receive treatments for your illness.
4. Where does Central Coast VNA & Hospice provide services?
We serve patients and their families across Monterey County, San Benito County, Santa Cruz County, and South Santa Clara County. Care is typically provided in the patient's home or assisted living facility.
5. How is palliative care paid for?
Palliative care services are often covered by Medicare Part B, Medi-Cal, and most private insurance plans. Our team can help you understand your specific coverage and any potential out-of-pocket costs.
Ready to explore how specialized, in-home palliative care can improve your quality of life? Contact VNA and Hospice to learn more about a care plan tailored to your specific needs. Discover the comfort and compassionate support that has made us the trusted choice on the Central Coast for over 74 years by visiting our website at VNA and Hospice.
Symptoms of Heart Failure in Elderly: What to Watch For
When you hear the term "heart failure," it can sound scary. But it does not mean the heart has suddenly stopped working.
Instead, think of it like a pump that has grown weaker over time. It still works, but it cannot pump blood as well as it used to. For seniors, heart failure means the heart muscle is weak and struggles to pump blood efficiently.

This condition is common in older adults. Understanding its early signs is the first step toward managing it well. Often, it begins with small changes you might think are just normal aging. These can include unusual fatigue, shortness of breath, or swelling in the legs and ankles. Noticing these changes is key to living a good quality of life. For a deeper clinical understanding, it's also helpful to know how the heart is divided into different cardiac segments for diagnostic accuracy.
Why Early Recognition Matters
Spotting the symptoms of heart failure in elderly loved ones early allows for timely medical help. This can slow down how fast the condition gets worse. With the right care plan, seniors can continue living safely and comfortably at home.
Central Coast VNA & Hospice offers a complete continuum of care to support families. With over 74 years of nonprofit service, our mission is to provide compassionate, expert care. We serve Monterey County, San Benito County, Santa Cruz County, and South Santa Clara County. We offer:
- Home Health: A skilled Registered Nurse comes to your home to check symptoms and manage medications.
- Palliative Care: This specialized support focuses on relieving discomfort and improving quality of life at any stage.
- Hospice Care: We provide compassionate end-of-life care when comfort is the main goal.
Recognizing heart failure symptoms is not just about finding a medical issue. It’s about opening the door to support that can make a huge difference. Proper heart failure management helps seniors keep their independence and dignity.
Recognizing the Most Common Heart Failure Symptoms
When the heart does not pump strongly, the body sends signals that something is wrong. Learning to spot these signs is the most important step in managing heart failure. These signs often appear slowly and are a result of the heart's struggle to circulate blood.
One of the first things people notice is shortness of breath, also called dyspnea. An older adult might feel winded after simple tasks, like walking to the mailbox. This happens because the weak heart cannot keep up with the body’s need for oxygen, causing fluid to back up into the lungs.
This next infographic shows how common shortness of breath is. It also shows the different ways it can appear.
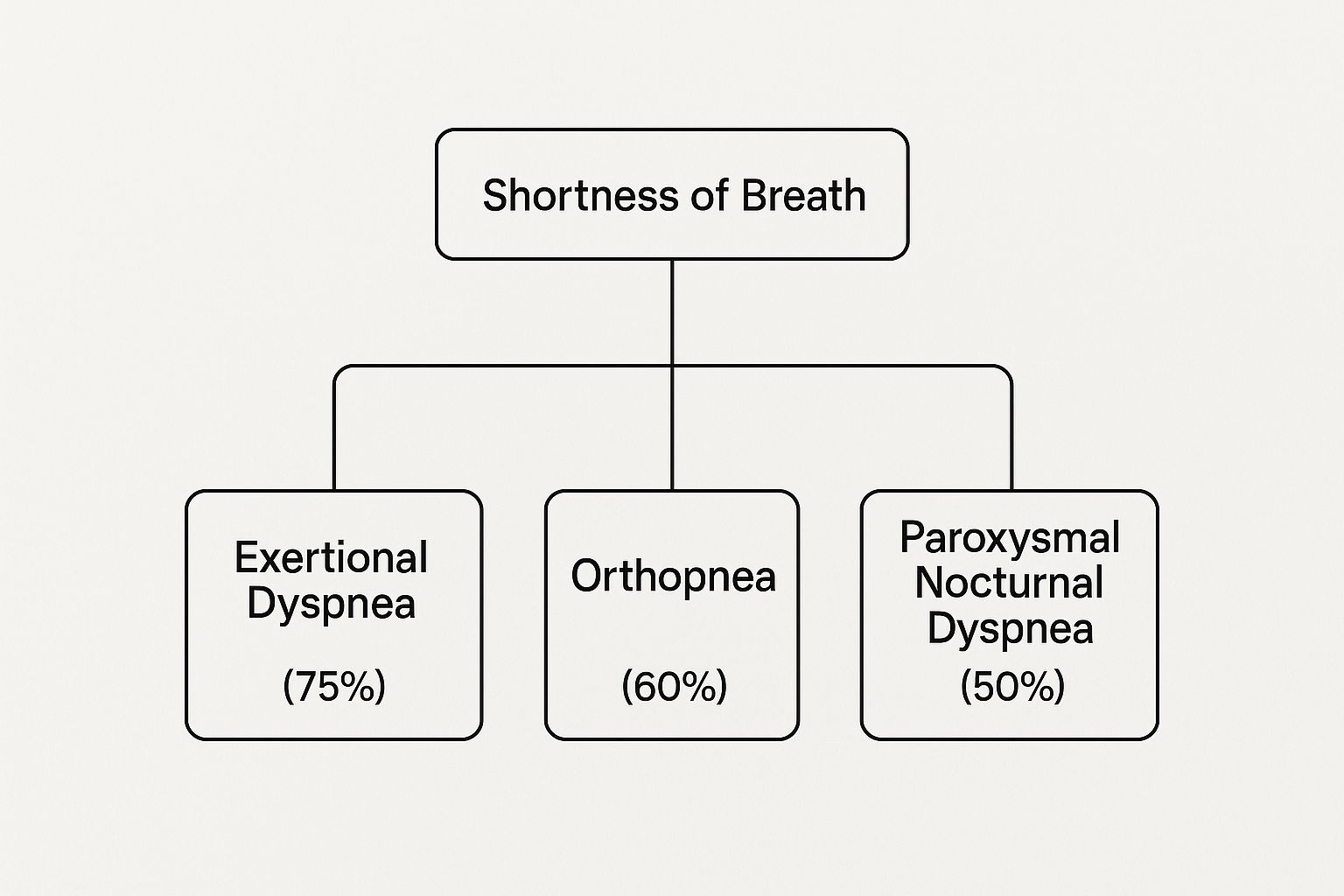
As you can see, feeling breathless during activity is the most common issue. It is also a major problem for people when they are simply lying down.
Fluid Buildup and Swelling
Another key sign of heart failure is noticeable swelling, or edema. This is caused by the body holding onto extra fluid. When the heart cannot pump blood forward well, it backs up in the veins. This pressure pushes fluid out of the blood vessels and into body tissues.
You will typically see this swelling in certain places:
- Legs, ankles, and feet: Shoes might feel too tight, or you may notice an indent in the skin after pressing it.
- Abdomen: The belly area can feel bloated, swollen, and a little tender.
- Sudden weight gain: Gaining a few pounds in a couple of days is a red flag for fluid buildup, not fat.
This same fluid can also go into the lungs. This leads to a persistent cough or wheezing that gets worse at night when lying flat. It is a direct result of the heart struggling to manage the body's fluid.
To make these connections clearer, here is a simple breakdown of the most common symptoms and their causes.
Common Heart Failure Symptoms and Their Causes
| Symptom | What It Looks or Feels Like | Why It Happens (Simple Explanation) |
|---|---|---|
| Shortness of Breath | Feeling winded with activity or when lying down. | The heart can't pump blood well, causing fluid to back up in the lungs. |
| Swelling (Edema) | Puffy legs, ankles, feet, or a swollen belly. Sudden weight gain. | Poor blood flow causes fluid to leak from blood vessels into body tissues. |
| Persistent Cough | A hacking, "wet" cough or wheezing, often worse at night. | Fluid from the lungs (pulmonary edema) irritates the airways. |
| Fatigue | Feeling unusually tired or weak, even after rest. | The body isn't getting enough oxygen-rich blood to the muscles and organs. |
| Rapid Heartbeat | A racing, fluttering, or pounding feeling in the chest. | The heart beats faster to try to make up for its weak pumping action. |
Understanding these links can help you spot the signs early. It also helps you explain them clearly to a healthcare provider.
Changes in Heart Rhythm
A rapid or irregular heartbeat is another key symptom. It can feel like your heart is racing, fluttering, or skipping beats. This happens because the heart is working overtime. It beats faster to try to circulate enough blood.
These feelings can be scary. However, they are the heart’s attempt to keep up with the body's needs. It's important to know the difference between these feelings and other heart problems. You can learn more by reading about the major symptoms of a heart attack.
Heart failure is a major global health issue. It affects an estimated 64 million people worldwide. As the condition gets worse, these symptoms often become more severe, making daily life harder.
Spotting Subtle Symptoms Often Mistaken for Aging
Not every sign of heart failure is dramatic. Many of the earliest warnings are quiet and easy to dismiss as just a part of getting older. Learning to recognize these subtle clues is key to getting help when it matters most.

One of the most common but overlooked symptoms is a deep, lasting fatigue. This is not just feeling a little tired. It is a deep exhaustion that stays even after a full night of rest. When the heart is not pumping strongly, it cannot get enough oxygen-rich blood to the body, leaving a person feeling drained.
Changes in Appetite and Cognition
A sudden loss of appetite or feeling of nausea can also be a quiet signal. If the heart struggles to pump, the digestive system gets less blood flow. This can make eating feel like a chore.
You might also notice moments of confusion, memory loss, or cloudy thinking. This can be scary for families to see, but there is a physical reason for it. Reduced blood flow to the brain can affect how well a person thinks, creating what some call "brain fog."
"My father just wasn't himself. He lost interest in his favorite foods and seemed to get confused during conversations. We thought it was just age, but it was his heart trying to tell us something was wrong."
Often, it is the mix of these symptoms that points to a bigger problem. These subtle changes can disrupt daily life. This is where having support at home is so important. Understanding how to care for elderly parents at home can help you create a safe environment.
Another surprising sign is an increased need to urinate at night, called nocturia. This happens for a specific reason:
- During the day, the weaker heart cannot send enough blood to the kidneys.
- Because of this, the kidneys do not filter out extra fluid from the body very well.
- At night, when the person lies down, gravity helps blood flow back to the heart more easily.
- This improved circulation "wakes up" the kidneys, which start working to process the fluid that built up during the day.
This cycle disrupts sleep. It also adds to the feeling of deep fatigue.
When symptoms interfere with daily comfort, palliative care can help. Central Coast VNA & Hospice offers palliative care services in Monterey County and nearby areas. We focus on managing these symptoms to improve quality of life at home.
When Heart Failure Symptoms Get Worse
Heart failure is a progressive condition. This means symptoms can change and get worse over time. Often, specific triggers can cause a sudden decline. Understanding them is the first step to helping your loved one stay as healthy as possible.
These changes are often caused by everyday things. A diet too high in salt can make the body hold onto fluid, straining the heart. Forgetting to take medications can also upset the balance needed to control symptoms. Even a simple cold can make heart failure symptoms worse.

Knowing When to Call for Help
It is very important to know the difference between a small change and a serious warning sign. This knowledge lets you act with confidence. Being prepared is a big part of preventing hospital readmissions, a major goal for managing a chronic illness at home.
You should call the doctor if you notice:
- A sudden weight gain of 2-3 pounds in 24 hours or 5 pounds in a week.
- More swelling than usual in the legs, ankles, or belly.
- Increased trouble breathing during normal daily activities.
- A persistent dry, hacking cough that seems to be getting worse.
These signs often mean the heart is working too hard. A simple change in medication or diet might be all that is needed. Getting a medical professional involved early can stop a small problem from becoming a big one.
But some symptoms need immediate, emergency attention. If your loved one has severe shortness of breath while resting, chest pain, fainting, or sudden confusion, you should call 911 right away.
How In-Home Care Provides Support
This is where the support of Central Coast VNA & Hospice can make a real difference. Our skilled clinicians work with families across Monterey, San Benito, and Santa Cruz counties to monitor these very changes.
- Home Health: A Registered Nurse can visit the home to check vital signs, track weight, and make sure medications are taken correctly.
- Palliative Care: For those who need more help managing symptoms, our palliative team focuses on relieving discomfort.
- Hospice Care: When goals shift to comfort, our hospice team provides compassionate care and support for the whole family.
Heart failure is the top reason older adults are hospitalized. Studies have found that mortality rates after a hospital stay can be as high as 13.7% within a year (NHPCO, 2021). You can read more about these findings on heart failure trends.
How Professional In-Home Care Can Help
For many families, managing heart failure at home can feel like a full-time job. It's easy to feel overwhelmed with medication schedules, symptom tracking, and daily support. This is where professional in-home care steps in, offering help and peace of mind.
At Central Coast VNA & Hospice, our nonprofit, mission-driven team gives your loved one compassionate support at home. Our skilled clinicians, from Registered Nurses to Hospice Aides, partner with you to manage this condition. We are proud to serve families across Monterey County, San Benito County, Santa Cruz County, and South Santa Clara County.
Expert Monitoring and Symptom Management
Having a clinical expert regularly check on your loved one is a huge relief for families. A Registered Nurse can track vital signs, look for fluid retention, and assess breathing. This helps catch small problems before they become emergencies.
Our clinicians work with your loved one's doctor to create a personal care plan. This often includes:
- Medication Management: Taking the right doses at the right times is key to keeping the heart working well.
- Symptom Tracking: We watch for increased swelling, sudden weight gain, or worsening shortness of breath.
- Dietary Guidance: Our team provides education on low-sodium diets to help prevent fluid buildup.
This hands-on support is proven to reduce stressful hospital visits. By managing symptoms at home, we help your loved one stay stable.
Bringing skilled nursing care into the home changes how families handle chronic illness. It shifts the focus from reacting to crises to providing proactive, compassionate support that improves daily comfort.
Education and Support for the Whole Family
Heart failure affects the entire family, not just one person. Our clinicians take time to educate everyone involved. This gives you the knowledge and confidence to provide support. We will explain which symptoms to watch for and what to do if they appear.
This partnership means you never feel alone. Whether your loved one needs the skilled support of home health, the symptom relief of palliative care, or the comfort of hospice, our team is there. We offer a full continuum of care that adapts as your family’s needs change.
We believe in empowering families with information. You can learn more about our dedicated home health care for congestive heart failure patients to see how we tailor our services. This commitment is central to our 74+ year legacy of nonprofit service to the Central Coast community.
Partnering with a Trusted Local Health Provider
Spotting the signs of heart failure in an elderly loved one is the first important step. It opens the door to getting them the compassionate support they deserve. We know this journey can feel overwhelming, but you do not have to walk it alone.
Having a trusted local partner can make all the difference. It helps in managing symptoms and improving your loved one's quality of life.
For over 74 years, Central Coast VNA & Hospice has been a steadfast, nonprofit healthcare provider in our community. We serve families across Monterey, San Benito, Santa Cruz, and South Santa Clara counties. Our services range from in-home health to palliative and hospice care. Our mission is to provide expert, dignified care that honors your family's needs.
Heart failure is a growing health challenge for older adults. Cases have more than doubled across the globe since 1990. You can discover more about these public health findings. This shows why it is so important to recognize symptoms early and get the right care.
If you have concerns about an older adult in your life, we are here to help. Contact Central Coast VNA & Hospice today to learn how our compassionate team can support your family.
Frequently Asked Questions
When a loved one is diagnosed with heart failure, you may have many questions. Getting clear, simple answers is the first step toward feeling more in control. Here are some of the most common questions we hear from families.
Our goal is to give you the information you need. We want you to understand what is ahead and how the right support can help.
Does heart failure mean the heart is about to stop?
No, not at all. This is a common fear, but heart failure means the heart muscle has weakened. It is not pumping as well as it used to. Think of it as a long-term condition, like diabetes, not a sudden event. With good medical care and support, many seniors live with heart failure for years.
Can heart failure symptoms be reversed or cured?
While there is no cure for heart failure, the symptoms can be managed and often improved. The right medications, a low-salt diet, and regular medical care can make a big difference. These steps can reduce swelling, make breathing easier, and improve a person's quality of life at home.
How can I tell if my mom's fatigue is just old age or heart failure?
This can be tricky. But the fatigue from heart failure is often a deep, lasting exhaustion that does not get better with rest. Look for other clues. Is the fatigue paired with other symptoms of heart failure in elderly adults, like shortness of breath, new ankle swelling, or a cough that won't go away? If she is too tired for her usual activities, it's time to talk to her doctor.
What kind of professional help is available at home?
In-home care provides a great layer of support. A Registered Nurse from Central Coast VNA & Hospice can visit your home to manage medications and watch for symptom changes. Palliative care is another type of support that focuses on relieving the pain, symptoms, and stress of a serious illness. It can be provided right alongside other medical treatments to improve comfort.
When should we consider palliative care or hospice?
Palliative care is a helpful resource that can be started at any stage of heart failure. Its main goal is to make your loved one feel better by managing symptoms. Hospice care is for when the focus shifts from trying to cure the condition to maximizing comfort and quality of life. This usually happens when a doctor believes life expectancy is six months or less.
At Central Coast VNA & Hospice, we're here to help you navigate these challenges with both compassion and clinical expertise. If you have more questions or feel you need support, please reach out. We can help you understand how our home health, palliative, or hospice care can make a positive difference for your family.
Learn more at https://ccvna.com










