Spiritual Care in Hospice: What Families Should Know
When people hear "spiritual care," they often think of religion. But in hospice, it’s much more than that. It’s about caring for the human spirit and helping people find peace and meaning at the end of life.
This care helps people with big questions, like “Did my life matter?” It is for everyone, respecting all beliefs—whether religious, spiritual, or non-believing.
Understanding Spiritual Care and Its Importance
When a loved one enters hospice, the first focus is often on physical pain. But emotional and spiritual health are just as important for a peaceful journey. This is why spiritual care is a key part of the support we provide at Central Coast VNA & Hospice.
For over 74 years, our nonprofit mission has been to care for the whole person. We use a concept called "total pain," which recognizes that suffering is not just physical. It can also be emotional, social, and spiritual. Spiritual care addresses this type of pain, helping patients and families with grace.
What Does Spiritual Care Address?
This support is very personal, so it looks different for everyone. It’s not about following a checklist. It's about meeting people where they are.
This might include:
- Finding Meaning: Helping a patient reflect on their life and legacy.
- Coping with Fear: Creating a safe space to talk about fears of death.
- Facilitating Forgiveness: Guiding conversations to heal old wounds with family or oneself.
- Offering Presence: Simply being there to listen, especially when words are hard to find.
This complete approach is seen worldwide as a vital part of quality hospice services.

As you can see, spiritual care provides emotional comfort. It also creates space for meaningful rituals and connection.
Core Elements of Spiritual Care
To help families understand what spiritual care involves, here are its key parts. Think of these as the tools our Chaplains use to support your loved one.
| Component | What It Means for Your Family |
|---|---|
| Life Review | A guided talk about important life events to find meaning and a sense of completion. |
| Legacy Work | Helping your loved one create memories, like writing letters or recording stories. |
| Ritual & Ceremony | Leading familiar religious rituals or creating new ones that honor your loved one's beliefs. |
| Emotional Support | Providing a compassionate ear for conversations about fear, hope, and love without judgment. |
| Connecting to Beliefs | Supporting your loved one’s connection to their source of strength, whether it's God, nature, or family. |
These elements work together to bring peace during a difficult time.
At Central Coast VNA & Hospice, our Chaplains are trained to listen deeply and honor each person’s journey. They are a core part of the team serving families across Monterey, San Benito, Santa Cruz, and South Santa Clara Counties.
This team approach ensures that every part of a person's well-being is cared for. To learn more about end-of-life support, you can read about what hospice care is in our guide.
Meet Your Spiritual Care Team
When you hear "spiritual care," you might think of formal religion. But in hospice, it’s broader and more personal.
At Central Coast VNA & Hospice, our spiritual care team includes professionally trained listeners. They are experts in helping people with the big emotions that come up during life’s challenges. A Chaplain often guides this team.
Their role is not to push a specific religion. Their focus is to create a safe space for patients and families to have difficult but important conversations.
Who Are the Members of the Team?
The spiritual care team is part of a larger group that works together. This ensures your loved one receives true whole-person care. This teamwork is central to our mission in Monterey County and nearby areas.
Your team will likely include:
- A Chaplain: This person often leads spiritual support, offering guidance and a compassionate ear.
- Specially Trained Volunteers: These individuals can provide companionship, read aloud, or just sit quietly. You can learn more about how to volunteer for hospice on our site.
- Your Primary Hospice Team: Your Registered Nurse, Hospice Aide, and Social Worker work with the spiritual care team to provide seamless support.
This model makes sure spiritual comfort is part of the daily care plan. The team knows that emotional and spiritual health can affect physical comfort.

What Does the Spiritual Care Team Do?
The support provided is personal and flexible. Our team members meet people exactly where they are on their journey.
A Chaplain might help a patient explore their life's story or find peace with past regrets. Sometimes, their most important role is to offer a calm presence when words are not needed.
For example, a team member could help a patient write down life lessons for grandchildren. They might also support families as they process their own grief. This compassionate expertise is a mark of our 74+ years of nonprofit service on the Central Coast.
How Spiritual Care Helps in Real Life
To understand spiritual care, you have to see it in action. This service is a personal experience shaped by an individual's life and values. It's where theory becomes real comfort.
Think of a Chaplain sitting with a veteran, helping them find peace with difficult memories. Or picture a spiritual care professional guiding a family as they share favorite stories. These are real interactions that honor a person's unique journey.

Real-World Scenarios of Spiritual Support
Spiritual care brings comfort in many ways. It often comes down to creating the right space for connection and reflection.
Here are a few examples of how our team helps:
- For the Non-Religious Patient: Someone with no religious beliefs may want to talk about their legacy. A spiritual care professional can guide them through a life review to see their positive impact.
- For the Grieving Family: Sometimes, a family has old conflicts. Our team can help mediate tough conversations, creating a space for forgiveness to happen.
- For the Traditional Believer: For many, religious rituals are a source of comfort. A Chaplain can lead prayers or work with the family’s own faith leader to meet their needs.
These moments show how our team at Central Coast VNA & Hospice adapts to each person. Our 74 years of local, nonprofit service have taught us to meet people where they are.
Spiritual care is about listening to the stories, fears, and hopes that define a lifetime. It offers a compassionate presence that says, "You are not alone on this journey."
Practical Ways Spiritual Care Makes a Difference
Spiritual care in hospice gives real benefits to patients and families. This support helps address deep questions and brings a sense of calm. It helps people find answers to questions like, "Did my life have meaning?"
This support often shows up in a few key ways:
- Reducing Anxiety: It gives patients a safe place to talk about their fears of dying.
- Strengthening Family Bonds: It can bring families closer by opening up communication.
- Providing Closure: It helps patients work through regrets and find forgiveness.
For those looking to deepen their own spiritual practice, resources on how to establish consistent prayer habits can help. This focus on the whole person is a key part of the spiritual care in hospice we provide. Learn more about our commitment to hospice care with comfort and dignity in Monterey County.
Finding Peace for Patients and Families
The benefits of spiritual support touch not just the patient but everyone involved. For patients, this care often brings a deep sense of peace. It creates a safe space to find meaning and prepare for the end with dignity.
This whole-person focus is at the heart of Central Coast VNA & Hospice's nonprofit mission. For over 74 years, we've believed that supporting the spirit is as important as caring for the body. This is how we ensure a dignified experience for everyone we serve in Monterey County and the surrounding areas.

A Source of Strength for Families
Families often find spiritual care to be a great source of strength. Saying goodbye is one of the hardest experiences a person can go through. Our spiritual care professionals are there to walk with you.
They can offer gentle guidance on how to have tough conversations. This helps create an atmosphere of honesty and love.
This support continues after a loved one passes. Our team helps families begin grieving and finding inward healing amidst devastation. We also offer dedicated hospice bereavement services, which are available to anyone in our community.
How Spiritual Care Addresses Common Challenges
The end of life brings unique challenges. Spiritual care is designed to meet these concerns with compassion. The table below shows how this support can make a real difference.
| End-of-Life Challenge | How Spiritual Care Offers Support |
|---|---|
| Feelings of Fear or Anxiety | Provides a calming presence and a safe space to discuss fears about death. |
| Unresolved Regrets | Guides life review and talks about forgiveness, helping people find peace with the past. |
| Loss of Meaning or Purpose | Helps patients reflect on their life’s impact and legacy, reaffirming their sense of identity. |
| Family Grief and Stress | Offers guidance for family discussions and emotional support for loved ones. |
At Central Coast VNA & Hospice, our approach is centered on the individual. We are committed to helping patients and families find peace on their own terms.
How to Access Spiritual Care for Your Loved One
Getting this support for your loved one is a simple part of our hospice program. At Central Coast VNA & Hospice, spiritual care is available to every patient and family. We believe in providing comfort for the whole person, including their spirit.
The conversation often starts during the first hospice meeting with a Registered Nurse. Our team will gently ask about your loved one’s spiritual preferences and needs. This is just an invitation to share.
Starting the Conversation
Our first step is always to listen. We want to understand what brings your loved one comfort and peace. There are no expectations; our only goal is to provide support that feels right for them.
You can ask for spiritual care at any time in the hospice journey. A simple talk with your hospice nurse or social worker is all it takes.
It's a Standard Part of Hospice Care
Many families are relieved to know that spiritual support is a standard part of hospice. It's covered by Medicare and most private insurance. This means there are usually no extra costs for these services. To learn more, read our guide on how to pay for hospice care.
This reflects a big shift in healthcare. The preference for home-based care is growing. According to the National Hospice and Palliative Care Organization (NHPCO), 67.2% of hospice care was provided in a patient's home in 2021 (NHPCO, 2023). This shows a desire for personal support in a familiar setting. You can explore more insights on global hospice care trends.
At Central Coast VNA & Hospice, we see spiritual care as a core part of compassionate end-of-life support. It’s included in every care plan we create for families in Monterey, San Benito, Santa Cruz, and South Santa Clara Counties.
How to Take the Next Step
If you think your loved one could benefit from our continuum of care, we encourage you to reach out. Our team is here to answer your questions.
You can get started by:
- Talking to your doctor: Ask for a referral to Central Coast VNA & Hospice.
- Calling us directly: Our team can walk you through our services.
- Exploring our resources: Learn more about our hospice care services on our website.
Taking that first step ensures your loved one receives the complete, whole-person care they deserve.
FAQs About Spiritual Care in Hospice
It is normal for families to have questions about spiritual care in hospice. Many people are not sure what it means. Our goal is to offer clear answers to help you feel more informed.
We want to address the most common concerns. This way, you can see how this support is designed to meet your family’s specific needs.
Does my loved one have to be religious to receive spiritual care?
Not at all. Spiritual care is for everyone, no matter their beliefs. It is designed to support the human spirit, not just a person's religious faith. Our Chaplains are trained to connect with people who are religious, spiritual, agnostic, or atheist with deep respect.
What is the difference between spiritual and religious care?
This is a great question. Religious care is often tied to specific traditions and texts of a particular faith. Spiritual care is much broader. It's about a person's inner life—their values, purpose, and connections to what gives them strength.
Will a Chaplain try to convert my family member?
Absolutely not. A hospice Chaplain’s role is to listen and offer comfort, never to impose their own beliefs. They are trained to create a safe space where your loved one can explore their own feelings without any outside pressure.
Can our family’s own pastor or spiritual leader be involved?
Yes, of course. We strongly encourage the involvement of your family’s own clergy or spiritual advisor. Our spiritual care team is happy to coordinate with your trusted leaders to create a seamless circle of support for your loved one.
What if we do not want spiritual care services?
That is perfectly fine. All of our hospice services, including spiritual care, are optional. You and your loved one are always in control of your care plan. We will always honor your wishes without question.
For over 74 years, Central Coast VNA & Hospice has provided compassionate, whole-person care to families across Monterey, San Benito, Santa Cruz, and South Santa Clara Counties. If you have more questions about hospice or our nonprofit mission, please contact us today to learn how we can support you.
Medicare Home Care Eligibility: Your Guide to Coverage
To qualify for Medicare home health care, a doctor must certify that you need skilled medical care. You also need to be considered homebound. This means it is a major effort for you to leave your house.
This benefit is for short-term recovery after an illness, injury, or surgery. It is not for long-term help with daily personal tasks.
Understanding Medicare's Home Health Benefit

When a doctor suggests care at home, it is normal to feel a bit lost. The term "home care" can be confusing, but Medicare’s benefit is very specific. It focuses on providing clinical services to help a patient recover and regain independence.
Think of it as bringing skilled hospital services to your home for a limited time. This is not for ongoing help with chores, cooking, or errands. It is targeted medical support from licensed professionals like a Registered Nurse.
What Is the Goal of Medicare Home Health Care?
The main goal is to help you or a loved one get better at home. This care is important for managing a new diagnosis or recovering from a hospital stay. It can also keep a chronic condition from getting worse.
At Central Coast VNA & Hospice, our mission for over 74 years has been to provide this compassionate care. We are a nonprofit, Medicare-certified agency. We proudly serve families in Monterey, San Benito, Santa Cruz, and South Santa Clara counties.
To make sure everything is handled correctly, Medicare has specific rules. A doctor must certify that the patient is homebound and needs part-time skilled care. A face-to-face visit with a doctor is also required. Most importantly, the care must come from a Medicare-certified agency.
To learn more about what Medicare home care includes, you can read about home healthcare services. Our team is here to walk you through each step.
Medicare Home Health Eligibility Checklist
Here is a quick list of the five main requirements for Medicare home health care. This checklist can help you see if you or a loved one might be eligible.
| Requirement | What It Means |
|---|---|
| 1. Doctor's Certification | A doctor must confirm that you need skilled nursing care or therapy. |
| 2. Be Homebound | Your doctor must state that leaving home is a major effort for you. |
| 3. Need Skilled Care | Your care needs must be medical, like physical therapy or wound care. |
| 4. Face-to-Face Encounter | You must have an in-person visit with a doctor about your condition. |
| 5. Medicare-Certified Agency | Your care must come from an agency approved by Medicare, like CCVNA. |
Meeting these requirements is the first step toward getting professional care at home. If you have questions about any of these points, we are here to help.
The Four Pillars of Medicare Eligibility
Figuring out Medicare’s rules for home health care can feel like a puzzle. To make it simpler, let's think of medicare home care eligibility as a structure built on four pillars. If a patient meets all four, they almost always qualify.
This approach breaks down complex rules into clear, manageable parts. It makes it easier for families to understand what Medicare requires.
The infographic below shows how these pillars work together.

As you can see, each requirement builds on the last. Together, they create a solid foundation for receiving care at home.
1. You Must Be Homebound
The first pillar is the homebound requirement. It is also one of the most misunderstood. Being "homebound" does not mean you are stuck in bed or can never leave the house.
It means that leaving home takes a lot of effort. Medicare understands that you may need to go to doctor's appointments or attend short outings. But if you can still drive, go shopping, or regularly attend social events, you likely won't be considered homebound.
2. You Must Need Skilled Care
Next, you must need skilled care. This means medical services that can only be done safely by a licensed professional. This is a key part of qualifying for Medicare home care.
Skilled care is not the same as personal care or help with daily tasks. While a Home Health Aide might help with bathing, the main reason for care must be clinical.
Here are a few common examples of skilled care:
- Skilled Nursing from a Registered Nurse (RN) for things like wound care or IV therapy.
- Physical Therapy to help regain strength and balance after an injury or surgery.
- Speech-Language Pathology to help with swallowing or communication problems.
- Occupational Therapy to help relearn how to safely handle daily tasks like bathing.
3. A Doctor Must Oversee Your Care
The third pillar is that a doctor must be involved through a plan of care. Before services can start, a doctor must create and approve a detailed plan. This plan outlines what medical services you need and the goals of your treatment.
This plan is a roadmap for the home health team. It ensures that every service provided by the clinicians at Central Coast VNA & Hospice is medically necessary. A doctor must review and re-certify this plan at least every 60 days.
A doctor’s plan of care is the foundation of Medicare-covered home health. It confirms medical necessity and guides the entire clinical team.
4. You Must Use a Certified Agency
Finally, all services must come from a Medicare-certified home health agency. These agencies meet strict federal health and safety standards. This ensures you receive high-quality care.
Central Coast VNA & Hospice is a nonprofit, Medicare-certified agency. We have over 74 years of experience serving our communities. These include Monterey County, San Benito County, Santa Cruz County, and South Santa Clara County. Choosing a trusted, local agency ensures you receive compassionate, expert care. To see how these rules apply in our state, learn more about qualifying for home health care in California.
What Services Are Covered by Medicare?

If your loved one meets Medicare home care eligibility requirements, what help can they get? Knowing what Medicare covers helps you set realistic expectations. This allows you to plan for any other support your family might need.
Think of Medicare’s home health benefit as a short-term recovery tool. It is designed to provide skilled medical care to help a patient get back on their feet. Our clinical teams at Central Coast VNA & Hospice are experts in delivering these services.
Skilled Services Included in Your Plan of Care
Your doctor will create a specific "plan of care," which is a roadmap for recovery. This plan outlines which services are medically necessary. The services covered by Medicare fall into a few key categories.
These services are the core of the home health benefit. They are provided by agencies like CCVNA throughout our service areas.
The primary skilled services include:
- Skilled Nursing Care: Delivered by a Registered Nurse (RN), this includes wound care, injections, and medication management.
- Physical Therapy (PT): A Physical Therapist works with patients to restore movement and build back strength.
- Occupational Therapy (OT): An Occupational Therapist helps patients safely perform daily activities again, like bathing and dressing.
- Speech-Language Pathology Services: A speech therapist helps patients who have trouble swallowing or communicating.
Medicare may also cover medical social services. When skilled care is being provided, a Home Health Aide might also assist with personal care. To see a full list, feel free to explore our home health care services.
What Medicare Does Not Cover
Understanding what is not covered is just as important. This knowledge helps families arrange for any non-medical support that is needed.
Medicare’s benefit is for intermittent, skilled care, not continuous support. Understanding its limits is key to creating a complete care plan.
As a rule, Medicare will not pay for:
- 24-hour-a-day care at home.
- Meal delivery services.
- Homemaker services like shopping, cleaning, and laundry.
- Personal care (like help with bathing) if it is the only care you need.
Your Journey From Hospital to Home Care
Bringing a loved one home from the hospital is a big step. It can feel like a huge responsibility. But knowing what to expect can make all the difference.
The path to Medicare-covered home health care often starts before your loved one leaves the hospital. A discharge planner or social worker will help map out a safe transition. They coordinate everything needed for continued medical care at home.
The Doctor's Role and the Referral Process
It all begins with a doctor's order. This is a formal certification required by Medicare. The doctor must decide that it is medically necessary for your loved one to receive skilled care at home.
This is often where Central Coast VNA & Hospice comes in. For over 74 years, we have built strong partnerships with local hospitals. Our team works with discharge planners to make the referral process simple.
The Face-to-Face Encounter and First Visit
One of the most important steps for medicare home care eligibility is the "face-to-face encounter." This is a documented, in-person visit between your loved one and their doctor.
This meeting must happen within 90 days before or 30 days after home health care starts. It is Medicare's way of checking that a doctor has seen the patient and agrees home care is right. This is a required part of the process.
The doctor's face-to-face encounter is the cornerstone of a successful transition to home care. It validates the need for skilled services.
Once the referral is complete, a Registered Nurse will schedule the first home visit. During this meeting, the nurse reviews the doctor's orders and develops a personal plan of care. This first visit sets the stage for a safe and effective recovery at home. To learn more about our coordinated care, see our page on home health and hospice care in Santa Cruz.
How to Navigate Common Eligibility Roadblocks
Families can run into unexpected hurdles when trying to secure Medicare home care eligibility. Most of these roadblocks can be solved once you know what to look for. Being prepared can make a big difference.
Often, delays are due to simple misunderstandings or incomplete paperwork. For example, a doctor might not write down enough detail in the plan of care. Or, the "homebound" certification might not be clear enough.
Overcoming the "Homebound" Hurdle
One common issue is the strict "homebound" definition. It is easy to get a denial if medical records show activities that seem to conflict with this status.
To avoid this, the doctor's notes need to be very clear. They should explain exactly why leaving home is difficult and medically ill-advised. This builds a much stronger case for home health care.
Ensuring Your Paperwork Is Complete
Another reason for delays is incomplete paperwork. Every document must be filled out perfectly. A single missing signature can stop the whole process.
Think of the eligibility process as building a case. Each document is evidence that your loved one meets Medicare’s rules.
This is where working with an experienced agency like Central Coast VNA & Hospice helps. Our team has guided countless families in Monterey County, San Benito County, and Santa Cruz County. We are very careful about making sure every piece of paper is in order.
If you do hit a roadblock, you are not alone. Our staff are experts at fixing these issues. We can work with your doctor's office to get missing information, making your path to care as smooth as possible. You can learn more about our dedicated home health care in Monterey and how we help families.
When Your Loved One Needs More Support
A health journey is rarely a straight line. As your loved one's needs change, their care plan may also need to change. Medicare home health is a great resource, but it is often just one step in a longer journey.
Sometimes, a patient’s condition stabilizes, but they are still living with a serious illness. This can bring on symptoms like chronic pain. In these moments, another layer of support can make a world of difference.
Shifting the Focus to Comfort and Quality of Life
This is where palliative care can help. Palliative care is specialized medical support focused on providing relief from symptoms. The main goal is to improve the quality of life for both the patient and their family.
As a mission-driven nonprofit, Central Coast VNA & Hospice offers this vital support. We serve families throughout Monterey, San Benito, and Santa Cruz counties.
Understanding the Continuum of Care
In some cases, an illness progresses to where the focus shifts from a cure to comfort. This is when hospice care becomes an invaluable resource. It provides compassionate support centered on dignity and peace.
Hospice is not about giving up. It is about a philosophy of care that prioritizes comfort and supports the entire family.
At Central Coast VNA & Hospice, we provide a full continuum of care. We are here to guide you through transitions—from home health to palliative and, when the time is right, to hospice. Learning about the criteria for this support can help you make informed decisions. You can read our guide on hospice care eligibility. Exploring essential home modifications for elderly safety and comfort can also help create a safer environment.
Frequently Asked Questions (FAQs)
How much does Medicare home health care cost?
For patients who qualify, Medicare Part A and/or Part B covers 100% of approved home health services. This means no deductible or coinsurance for skilled care. You will be responsible for a 20% coinsurance for any durable medical equipment (DME), such as a walker or hospital bed.
How long can someone receive home health care?
Medicare covers skilled care as long as you meet the eligibility rules. A doctor must review and recertify your plan of care every 60 days. This confirms that the services are still medically necessary.
Do I get to choose my home health agency?
Yes, you always have the right to choose any Medicare-certified home health agency in your community. A hospital may give you a list of local providers, but the final choice is yours. Choosing a provider with deep community roots, like Central Coast VNA & Hospice, can make a positive difference.
What happens when a patient no longer qualifies?
If your health improves and you no longer need skilled care or are not homebound, your services will end. Your clinical team will work with you and your doctor. They will plan for a safe and smooth discharge.
What if Medicare denies our request for home care?
If a claim is denied, you have the right to appeal. The denial notice from Medicare will have instructions on how to start the appeals process. Your home health agency can often help you make sure all the paperwork is in order to support your case.
Navigating medicare home care eligibility can feel overwhelming, but you don't have to do it alone. The compassionate team at Central Coast VNA & Hospice is here to answer your questions. Contact us today to learn more about our trusted home health, palliative, and hospice services. https://ccvna.com
Effective Patient Engagement Strategies for Better Care
Patient engagement means patients are active partners in their own health journey. Instead of just receiving care, they work with their healthcare team. This teamwork leads to better health, higher satisfaction, and more control for patients and families. For nonprofit organizations like Central Coast VNA & Hospice, this partnership is key to our mission. We have served Monterey County, San Benito County, Santa Cruz County, and South Santa Clara County for over 74 years.
When patients are involved, they are more likely to follow their care plans and make smart decisions. This is very important for home health, palliative care, and hospice, where care happens at home. Exploring proven strategies to improve patient satisfaction helps build strong patient engagement.
Our team of Registered Nurses and Hospice Aides sees how good patient engagement strategies change the care experience. This article will cover nine powerful ways to improve healthcare. These strategies help you and your loved ones take an active role in your care.
1. Harnessing Technology with Patient Portals
Secure online platforms called patient portals are changing how people access health information. These tools give you 24/7 access to medical records and let you talk securely with your care team. This access is a key part of modern patient engagement strategies because it puts important information in your hands.
How Patient Portals Enhance Care
For families in home health or hospice, a patient portal is a central place for information. You can see care plans from your Registered Nurse, medication lists, and appointments. This makes things less stressful and reduces the need for phone calls. These tools build trust between patients and providers, a value Central Coast VNA & Hospice has practiced for over 74 years.
Making Portals Work for Everyone
To work well, portals must be easy to use. This means training patients and families who are new to the technology. Key features include:
- User-Friendly Design: Simple menus and clear language help everyone find what they need.
- Mobile Accessibility: A design that works on phones and tablets lets you access information anywhere.
- Responsive Communication: Care teams should reply to messages quickly to keep your trust.
This infographic shows the main benefits of patient portals.
These features help create a better and more informed care experience. Portals are very helpful for services that help seniors with aging in place safely and comfortably. By using these digital tools, we make managing health easier for everyone.
2. Shared Decision Making (SDM)
Shared Decision Making (SDM) is when clinicians and patients make healthcare choices together. This approach combines the provider's medical knowledge with the patient's values and goals. It turns patients into active partners, which is a key part of successful patient engagement strategies. This teamwork makes sure the care plan fits what is important to you.
How SDM Enhances Care
For families in home health or hospice, SDM helps create a care plan that respects the patient's wishes. A Registered Nurse might discuss different ways to manage symptoms, explaining the good and bad of each. This allows the patient and family to choose what aligns with their comfort, giving them a sense of control.
Making SDM Work for Everyone
Good SDM needs a thoughtful and kind approach. Key parts for success include:
- Use Helpful Tools: Patient decision aids can explain complex choices with clear, simple information.
- Allow Enough Time: Important talks about care goals should not be rushed.
- Train Providers: Clinicians need training to lead these sensitive talks well.
This process is very important when planning for future medical needs. Learning about advance care planning can help families feel more prepared. By using SDM, we make sure care is not just medically correct but also personal and respectful.
3. Mobile Health (mHealth) Apps
Mobile health (mHealth) apps are tools on smartphones and tablets that help manage health. These apps can track symptoms, manage medications, or monitor long-term conditions. As a modern part of patient engagement strategies, mHealth apps offer a handy way for people to be involved in their own care.

How mHealth Apps Enhance Care
For patients at home, mHealth apps can improve how they manage their health. For instance, a diabetes app can log blood sugar levels and share them with a Registered Nurse. This real-time information helps the care team give advice quickly, which can prevent problems.
Making Apps Work for Everyone
For mHealth apps to be effective, they must be easy to use. It is important to choose apps that are simple for patients of all ages. Key features for success are:
- Proven Clinical Value: Choose apps that are backed by evidence and provide helpful information.
- Data Security: Make sure any app is HIPAA-compliant to protect patient health information.
- Simple Onboarding: Give clear instructions to help patients and families use the app correctly.
These apps help create a more connected healthcare experience. By using technology patients already have, we can help them be more independent.
4. Patient Education Programs
Patient education programs help people understand their health conditions, treatments, and self-care. These programs turn patients into active partners in their care. This is a key part of effective patient engagement strategies, as people who know more can make better decisions.
How Education Enhances Care
For families in home health or hospice, education gives them clarity and confidence. A good program can explain medical terms and teach skills for managing symptoms at home. For example, learning about and understanding and managing the psychological effects of breast cancer is very important for mental well-being. This knowledge helps reduce worry and gives families more control.
Making Education Work for Everyone
To have a real impact, education must be tailored to the person. This means using different learning styles and simple language. Key features include:
- Teach-Back Method: Clinicians ask patients to explain things in their own words to check if they understand.
- Visual Aids: Using charts, videos, and simple graphics can make information easier to learn.
- Accessible Materials: Information should be available in different languages and formats, like large print.
Using these methods helps providers make sure important information is understood. This leads to a stronger partnership, better health, and a more positive care experience.
5. Care Coordination Programs
Care coordination programs organize a patient's care across different providers and services. They make sure everyone on the care team works together smoothly. This is a vital patient engagement strategy, especially for those with complex health needs.
How Care Coordination Enhances Care
For families in home health or hospice, care coordination prevents confusion. It creates one clear plan that includes doctors, nurses, and therapists. This makes care less confusing and ensures the patient's wishes are always the focus. This helps build trust and encourages active involvement in the care plan.
Making Coordination Work for Everyone
Good care coordination relies on clear communication. It helps make transitions, like going from the hospital to home, much smoother. Key features include:
- Dedicated Care Coordinator: One person, often a Registered Nurse, guides the patient and family through the system.
- Shared Care Plans: All providers use a single care plan that is updated regularly.
- Proactive Communication: The care team meets often to discuss progress and plan next steps.
This organized approach is key to managing complex symptoms and improving quality of life. This is a main goal of our palliative care services. By coordinating care well, we empower patients and families on their healthcare journey.
6. Telemedicine and Virtual Care
Telemedicine and virtual care use technology to provide healthcare from a distance. Patients can talk with their care team through video calls or phone calls. This is a powerful part of patient engagement strategies for people managing an illness at home.

How Virtual Care Enhances Care
In home health and hospice, telemedicine helps between in-person visits from a Registered Nurse or Hospice Aide. It allows for quick check-ins to manage symptoms or give emotional support. This immediate access to the care team can prevent trips to the emergency room. It reflects the kind, responsive care model Central Coast VNA & Hospice has provided for over 74 years.
Making Virtual Care Work for Everyone
For virtual care to work, it must be simple for everyone. The goal is connection, not complicated technology. Key features include:
- Reliable Technology: A stable and secure platform helps with clear communication.
- Patient and Family Education: Offer simple instructions on how to use the virtual visit tools.
- Integrated Care: Connect virtual visit notes with the patient’s health record so the whole team is informed.
Virtual care is a handy way to improve communication and provide ongoing support. By using telemedicine, we offer more flexible interactions to help patients feel comfortable at home. This is especially helpful for services like palliative care.
7. Patient Advisory Councils
Patient Advisory Councils (PACs) are groups of patients and family members who work with healthcare organizations. They give feedback on policies and care to make sure the patient's voice is heard. This teamwork is one of the most direct patient engagement strategies for improving services.
How Patient Advisory Councils Enhance Care
For home health and hospice agencies, a PAC offers a way to get real feedback from the people we serve. Members can share their thoughts on everything from communication to emotional support. This helps organizations like Central Coast VNA & Hospice improve services to meet the needs of families at home.
Making Councils Work for Everyone
A good PAC needs real partnership and a promise to take action. To work well, councils should be set up with care. Key parts include:
- Diverse Representation: Include patients and families from different backgrounds to get a wide range of views.
- Clear Expectations: Give members training and clear goals so they can contribute in a meaningful way.
- Actionable Feedback: Create a process for leaders to review and use the council's ideas.
These councils are a great way for people to give back, much like our VNA & Hospice volunteer program. By listening to our community, we can build a better care system for everyone.
8. Gamification in Healthcare
Gamification uses game-like elements, such as points and badges, to encourage healthy habits. This can turn tasks like taking medicine or doing physical therapy into fun challenges. This is one of the newer patient engagement strategies that uses our natural desire to achieve goals to improve health.
How Gamification Enhances Care
For patients managing long-term conditions at home, gamification can make treatment plans feel less like a chore. An app might give points for checking blood sugar on time or a badge for taking medicine every day for a week. This positive feedback helps build healthy habits and makes patients more involved in their care.
Making Gamification Work for Everyone
To work well, gamified health programs must be simple and have a clear purpose. The health goal should always be the main focus. Key features include:
- Meaningful Goals: Connect challenges and rewards to important health goals, like better mobility.
- Simple Gameplay: Make sure the rules are easy to understand for people who are not used to technology.
- Progressive Difficulty: Start with easy goals and add new challenges over time to keep it interesting.
When designed well, gamification can boost motivation for patients. This is helpful for complex treatment plans, like those in our palliative care programs, by adding fun to daily health tasks.
9. Peer Support Programs
Peer support programs connect patients with trained people who have had similar health experiences. These groups use shared understanding to provide emotional support and encourage self-care. This is a key part of patient engagement strategies because it builds a community of trust and empathy.
How Peer Support Enhances Care
For people managing a long-term illness or facing end-of-life care, feeling understood is very important. Peer support offers a safe place to share fears, celebrate small wins, and give practical advice. This connection helps people feel less alone and more empowered to manage their health.
Making Peer Support Work for Everyone
To build a good program, training and structure are key. The goal is to create a safe and supportive space. Key elements include:
- Comprehensive Training: Peer supporters must learn how to listen well, keep information private, and set boundaries.
- Thoughtful Matching: Pairing people based on similar conditions or backgrounds can create stronger connections.
- Professional Integration: These programs work best when they support clinical care and have clear communication with the healthcare team.
These programs create a strong support network that improves well-being and health. By connecting people who understand each other, we can offer deeper comfort. Learn more about the group support for patients and families at Central Coast VNA & Hospice.
Your Partner in Health on the Central Coast
Becoming an active partner in your healthcare is the way of the future. The nine patient engagement strategies in this article all have one goal. They aim to empower you and your loved ones to take a main role in your health journey. This change leads to better health and care that fits your personal values.
At Central Coast VNA & Hospice, these ideas have been the foundation of our care for over 74 years. We believe the best patient engagement strategies are built on trust, communication, and respect. Our dedicated teams of Registered Nurses, Hospice Aides, and Medical Social Workers live this idea every day.
Putting Engagement into Action
By understanding these ideas, you can change your relationship with healthcare. It means asking questions, using digital tools to track your progress, and stating your wishes for your care. For families on the Central Coast dealing with serious illnesses, this active role is very important. It makes sure care plans are tailored to your unique needs.
As a local, nonprofit provider serving Monterey, San Benito, Santa Cruz, and South Santa Clara counties, our commitment is to you. We offer a full range of care from home health to palliative and hospice services. This ensures you get steady, kind support as your needs change.
By building strong partnerships, we help you have the best possible quality of life, on your terms. True engagement is more than a strategy. It is our promise to honor your journey with dignity and respect. Contact us today to learn more about our services.
Frequently Asked Questions (FAQs)
1. What is patient engagement?
Patient engagement is the process of involving patients as active partners in their own healthcare. It means they work together with their providers to make informed decisions about their treatment and health management. This teamwork often leads to better health outcomes and higher satisfaction with care.
2. Why are patient engagement strategies important for home health and hospice?
In home-based care settings, patients and their families have more responsibility for daily care. Strong engagement strategies empower them with the knowledge, tools, and confidence to manage symptoms, follow care plans, and communicate effectively with their team. This is essential for ensuring safety and quality of life at home.
3. How does Central Coast VNA & Hospice support patient engagement?
As a nonprofit serving Monterey County and surrounding areas for over 74 years, we focus on building trust and partnership. Our clinicians use shared decision-making, provide thorough patient education, and coordinate care closely with all providers. Our mission is to ensure every patient's voice is heard and their care plan reflects their personal goals.
4. Can technology really help older adults engage in their care?
Yes. When designed to be user-friendly, tools like patient portals and telemedicine can be very helpful for older adults. They provide convenient access to health information and make it easier to communicate with providers from home. We offer education to help patients and families feel comfortable using these tools.
5. What is the difference between palliative care and hospice care?
Palliative care can be provided at any stage of a serious illness and focuses on relieving symptoms and stress to improve quality of life. Hospice care is a specific type of palliative care for individuals with a life-limiting illness who are nearing the end of life. Both are part of Central Coast VNA & Hospice's continuum of care.
Ready to experience a healthcare partnership built on trust and empowerment? Learn how the dedicated teams at VNA and Hospice integrate these patient engagement strategies into our home health, palliative, and hospice care. Visit VNA and Hospice to discover how our nonprofit, mission-driven approach puts you at the center of everything we do.
How to Care for Elderly Parents at Home: Essential Tips
Caring for your parents at home is a journey that starts with heartfelt conversations. The goal is to figure out their needs together. This helps create a plan that respects their independence while making sure they are safe and well.
Starting Your At-Home Care Journey
Deciding to care for an aging parent at home is a major commitment. It is an act of love and respect. This transition rarely happens overnight, often beginning when you notice small changes in their daily life.
The most important first step is to talk with them. These conversations build a foundation of trust. You are not there to take over; you are there to partner with them in their care.
Initiating the Conversation
Finding the right moment for this chat is key. Look for a quiet, comfortable time when no one feels rushed. Frame the conversation around your concern for their well-being, not as if you are trying to control their life.
A gentle approach with open-ended questions works best. You could try saying something like:
- "I've noticed you seem a bit worn out lately. How have you been feeling?"
- "Are there any chores around the house that are getting harder to manage?"
- "What would you think about getting a little help with groceries or getting to appointments?"
These questions can open the door to a real discussion. Remember to listen more than you talk. Hearing their concerns makes all the difference.
Assessing Their Needs Together
Once you have started talking, you can explore their needs together. When they feel like part of the process, it helps preserve their dignity. This gives them a sense of control over their own lives.
It’s important to remember that most families providing at-home care also manage chronic health conditions. In the U.S., 86% of home health care recipients are aged 65 or older (CDC, 2021). Creating a supportive and safe home is critical.
A big part of this assessment is knowing when to bring in professional help. For families in Monterey County, San Benito County, Santa Cruz County, or South Santa Clara County, Central Coast VNA & Hospice offers a wide range of services. Learn more about our in-home care for seniors to see how our skilled team can support your family.
Initial Care Needs Assessment Checklist
| Care Category | Key Questions to Ask | Potential Next Steps |
|---|---|---|
| Personal Care | Do they need help with bathing, dressing, or grooming? | Consider a Hospice Aide for a few hours a week. |
| Household Tasks | Are they struggling with cooking, cleaning, or laundry? | Look into meal delivery services or a housekeeping service. |
| Health Management | Can they manage their medications? Are they getting to doctor's appointments? | Use a pill organizer; explore professional in-home nursing support. |
| Mobility & Safety | Have they fallen recently? Is the home safe from trip hazards? | Install grab bars, improve lighting, and consider a medical alert system. |
| Social & Emotional | Do they seem lonely or isolated? Are they staying engaged with friends? | Schedule regular visits, encourage social outings, or find local senior programs. |
This checklist is a starting point to guide your conversations and planning. Every family's situation is unique, so you will adapt it to fit your parent's specific circumstances.
Creating a Safe and Supportive Home Environment

Making a home safe for an aging parent is one of the most practical steps you can take. A secure environment does more than prevent accidents. It empowers your parent to maintain their independence for as long as possible.
The goal is not just to remove hazards. It is about creating a living space where your parent feels capable and comfortable. This means making thoughtful adjustments that adapt to their changing needs.
Prioritizing High-Risk Areas
Some parts of the house are riskier for seniors. The bathroom, kitchen, and stairways should be at the top of your list. Focusing your efforts here can prevent common accidents like falls.
Take the bathroom, for instance. A quick fix is installing non-slip mats in the tub and on the floor. Adding sturdy grab bars near the toilet and inside the shower provides crucial support.
Practical Modifications for Everyday Safety
Small tweaks throughout the home can make a world of difference. These modifications are about improving visibility and clearing pathways. They also ensure everything is within easy reach.
Think about the way people move through the house. Are there obstacles that could cause a trip? Taking time to address these hazards can create a much safer environment.
- Improve Lighting: Swap out dim bulbs for brighter ones, especially in hallways and stairwells. Nightlights in bedrooms and bathrooms can make navigating at night much safer.
- Secure Rugs and Cords: Get rid of small throw rugs that slide easily. Secure larger area rugs firmly to the floor and tidy up electrical cords along walls.
- Rearrange Furniture: Create wide, clear paths between rooms. Make sure there is plenty of space for your parent to move easily, especially if they use a walker or cane.
Establishing a Supportive Routine
A safe home is also about creating supportive systems. This helps reduce stress for everyone. It ensures that help is always close by if needed.
One of the most important systems is for medication management. A simple weekly pill organizer, clearly labeled, can prevent missed doses. Setting daily reminders on a phone can also be a huge help.
Having an emergency plan is another key element. This should include a list of important contacts and medical information posted in a visible spot. Many families also get peace of mind from a medical alert system.
Finally, remember to protect against invisible dangers. Promoting carbon monoxide awareness and ensuring detectors are working can save lives. Small steps like these build a powerful safety net.
Managing Daily Health and Medical Needs

Juggling your parent's medications and appointments can be demanding. Creating a structured system is for their health and your peace of mind. An organized approach helps ensure nothing gets missed.
It's estimated that approximately 70% of people who turn 65 will need some form of long-term care (U.S. Department of Health and Human Services, 2020). This reality shows why having a solid home care plan is so important.
Organizing Medications and Prescriptions
For many older adults, the day revolves around multiple prescriptions. The first thing to do is create a single, comprehensive list of every medication they take. This list should include prescription drugs, over-the-counter medicines, and supplements.
For every item, document:
- The name of the medication and its dosage
- The reason it is being taken
- The prescribing doctor’s name and phone number
- The time of day it needs to be taken
- Any special instructions, like taking it with food
Once you have this list, a weekly pill organizer is very helpful. Set aside time once a week to fill it. This simple routine is one of the best ways to prevent medication errors.
Making the Most of Doctor Visits
Doctor's appointments can feel rushed and overwhelming. Preparation is everything. Before each visit, jot down any new symptoms, concerns, or questions.
Always bring your updated medication list to the doctor. It also helps to take notes during the appointment. This simple habit helps you leave the office feeling confident.
When to Seek Professional Home Health Support
While family members provide loving support, some medical needs require trained professionals. Knowing when to bring in help is a crucial part of providing the best care. This is where an organization like Central Coast VNA & Hospice can become part of your team.
For over 74 years, our nonprofit has served families in Monterey County, San Benito County, Santa Cruz County, and South Santa Clara County. Our mission is to provide compassionate, mission-driven care right in the comfort of home.
Professional home health services can be a game-changer. A Registered Nurse can handle complex wound care or IV therapy. A Physical Therapist can help your parent regain strength and mobility.
Understanding what support is out there can lift a huge weight off your shoulders. The goal is to build a team around your parent. For those "what if" scenarios, it's wise to be prepared by understanding the best AEDs for home use.
Nurturing Emotional and Social Well-Being
Caring for an elderly parent at home is more than just managing physical needs. You are also nurturing their spirit. You help them feel connected, valued, and engaged with life.
This part of the journey is about protecting their sense of identity and purpose. It means truly listening and showing empathy. Focusing on their emotional well-being contributes to a higher quality of life.
Fostering Connection and Combating Loneliness
One of the toughest challenges for seniors is social isolation. As their world gets smaller, it is essential to create opportunities for connection. This protects their mental health.
Simple, consistent actions have power. A short, meaningful visit can be more impactful than a large, overwhelming gathering. It is about quality over quantity.
Here are a few practical ideas:
- Schedule Regular Visits: Set aside dedicated time for family and friends to stop by. A shared calendar can help coordinate visits so your parent has consistent social interaction.
- Embrace Technology: A user-friendly tablet can open up a new world of connection. Video calls or online groups for seniors can make a huge difference.
- Explore Local Programs: Many communities in Monterey and Santa Cruz County have senior centers or clubs. These provide a sense of purpose and community.
Encouraging Hobbies and Purposeful Activity
Keeping up with hobbies is vital for cognitive health. When a parent can no longer do their favorite activities, they can feel a profound sense of loss. The key is to help them adapt activities or introduce new ones.
For example, if they loved gardening, set up a few raised garden beds. If they loved to read, an e-reader or audiobooks can keep their passion alive. The goal is to focus on what they can do, not what they cannot.
Recognizing Signs of Emotional Distress
Emotional challenges like depression or anxiety can surface. It is crucial for family members to be aware of the signs. They can sometimes be brushed off as a normal part of getting older.
Keep an eye out for changes in their behavior or mood. This might look like a loss of interest in activities, shifts in appetite, or increased irritability. These can be indicators of a deeper issue.
When these signs appear, seek professional support. A Medical Social Worker from Central Coast VNA & Hospice can provide counseling. Our Chaplains also offer spiritual support to people of all faiths.
For parents managing a serious illness, this emotional support is key. Learn more about how our teams provide this support through our palliative care services. This type of care focuses on improving quality of life.
Understanding the Continuum of Care on the Central Coast
As your parent's health changes, the support they need will also change. This progression is called the Continuum of Care. For over 74 years, our team at Central Coast VNA & Hospice has walked this path with families, ensuring every transition is compassionate.
Knowing the difference between home health, palliative, and hospice care is key. It helps you make confident decisions for your loved one. The goal is to get the right care at the right time.
The First Step: Home Health Care
Home Health care is skilled medical support focused on recovery. A doctor typically orders it after a hospital stay or surgery. The main objective is to help your parent regain strength and independence at home.
For instance, after a surgery, a Central Coast VNA & Hospice Registered Nurse and Physical Therapist would visit. They would manage wound care and guide your parent through exercises. This care is goal-oriented to get patients back on their feet.
This type of care is designed to help patients recover. You can find out more about how we help families in our community with home health care services in Monterey, CA.
When Palliative Care Is the Right Choice
Palliative care is for people living with a serious illness. Its focus is on providing relief from symptoms and stress. It is an extra layer of support.
The main goal is to improve quality of life for both the patient and the family. A person can receive palliative care at any stage of a serious illness. They can even get it while undergoing curative treatments.
Comfort and Dignity with Hospice Care
Hospice care is for individuals nearing the end of their lives. This is usually when a doctor believes they have six months or less to live. The focus shifts from curing the illness to ensuring comfort and peace.
Hospice is not about giving up. It is about choosing to live the remainder of one’s life as fully and comfortably as possible. This is done with a compassionate support system.
This support comes from a team of physicians, nurses, Hospice Aides, and Chaplains. They work together to manage pain and provide emotional support. For families across Monterey, San Benito, Santa Cruz, and South Santa Clara counties, our hospice team is available 24/7.
Understanding the Continuum of Care Services
| Service | Primary Goal | Who It's For | Common Services Provided |
|---|---|---|---|
| Home Health Care | Recovery and rehabilitation | Patients recovering from surgery, illness, or injury at home. | Skilled nursing, physical/occupational therapy, wound care, medication management. |
| Palliative Care | Symptom relief and quality of life | Patients at any stage of a serious illness, often alongside curative treatment. | Pain management, emotional support, help with treatment side effects, family counseling. |
| Hospice Care | Comfort, dignity, and peace | Patients with a life expectancy of six months or less, when curative treatment has stopped. | 24/7 symptom control, spiritual care, personal care assistance, bereavement support for family. |
Each service plays a unique and vital role. By matching the right care to your loved one’s current needs, you ensure they receive the most effective support.
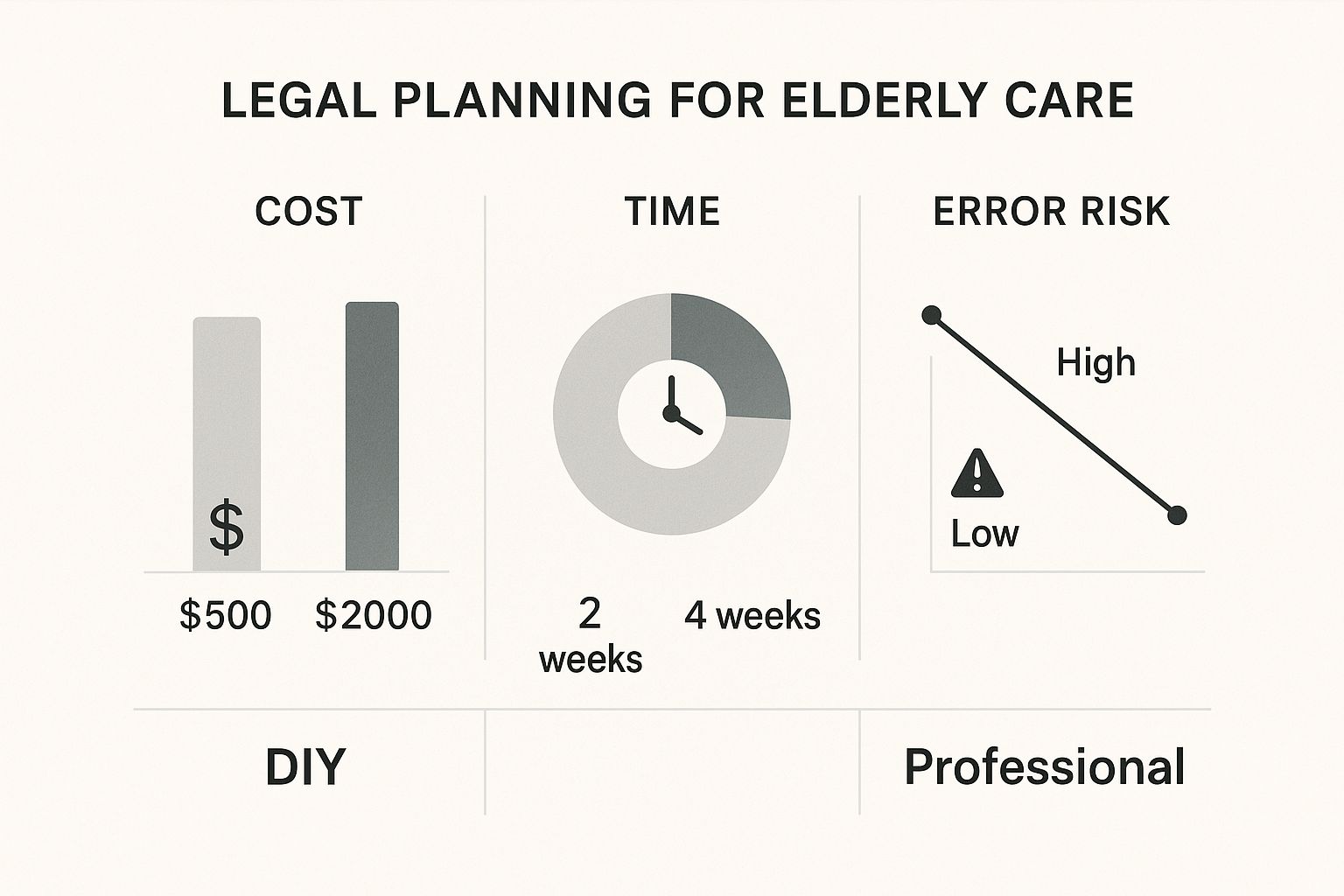
Professional guidance can lower the risk of costly mistakes while navigating elder care. This is especially true as technology like telehealth helps seniors live safely at home longer.
Frequently Asked Questions (FAQs)
How can I balance caregiving with my own life?
Preventing burnout is essential for your well-being. Set up a shared family calendar to schedule tasks and personal time. Ask for help from family and friends, and consider professional respite care for scheduled breaks.
What financial help is available for in-home care?
Explore several options for financial assistance. Long-term care insurance policies often cover in-home services. Medicare may cover certain home health services prescribed by a doctor, and veterans may be eligible for VA benefits.
When should we consider professional home health?
It is time for professional help when medical needs become too complex. This includes tasks like wound care or managing difficult medication schedules. If you feel overwhelmed or your parent's health declines, it is a clear sign to contact a professional home health agency like Central Coast VNA & Hospice.
How do I talk to my parent about their future care needs?
Choose a calm moment and express your love and concern. Use "I" statements like, "I've been worrying about..." to avoid sounding demanding. Listen to their fears and wishes, and understand this may take several small talks over time.
What are the most important legal documents we need?
Getting legal documents in order ensures your parent's wishes are honored. Key documents include a Durable Power of Attorney for Healthcare, a Durable Power of Attorney for Finances, and an Advance Directive (or Living Will). An elder law attorney can help ensure everything is legally sound.
Navigating at-home care is a journey you don't have to take alone. For over 74 years, Central Coast VNA & Hospice has provided compassionate, professional support to families across the Central Coast. If you have questions or need guidance, our team is here to help.
Contact us today to learn more about our services at https://ccvna.com.
Pain and Symptom Management: A Compassionate Guide
When you or a loved one lives with a serious illness, the focus should be on you, not just the disease. Pain and symptom management is a compassionate approach to healthcare. It looks beyond medicine to relieve physical, emotional, and spiritual distress.
Our goal is simple: improve your quality of life so you can focus on what matters. This supportive care is the heart of our home health, palliative, and hospice services. At Central Coast VNA & Hospice, we are committed to your comfort.
A Compassionate Approach to Your Comfort

Living with a serious illness can bring challenging symptoms like pain, fatigue, and anxiety. These burdens can feel overwhelming. They can make it hard to enjoy daily life or connect with loved ones.
We believe true comfort is more than just the absence of pain. It is a sense of peace that touches every part of your life. A dedicated pain and symptom management plan makes all the difference.
This approach is not about giving up. It is about living as fully and comfortably as possible. It starts with listening to your story to create a care plan that respects your wishes.
More Than Just Medicine
To bring you real relief, we use a combination of strategies. Our team works together to address your complete health picture. We know that true comfort involves more than just a prescription.
We help you find balance by looking at the whole person. Our care plans are designed to address a wide range of needs. This ensures every aspect of your comfort is considered.
The Four Pillars of Holistic Symptom Management
This table breaks down the different types of symptoms our teams address. It shows how our care plans support the whole person.
| Symptom Category | What This Includes | Our Management Goal |
|---|---|---|
| Physical Comfort | Pain, nausea, fatigue, shortness of breath, and other physical symptoms. | To provide relief with carefully planned medication and non-medical therapies so you can feel more like yourself. |
| Emotional Support | Feelings of anxiety, depression, fear, or stress related to your illness. | To offer counseling and compassionate support from Medical Social Workers who are here to listen and help. |
| Spiritual Peace | Questions about meaning, purpose, and navigating complex emotions. | To provide guidance and a listening ear from our Chaplains for you and your family, helping you find peace. |
| Social Well-Being | Maintaining connections with loved ones and community resources. | To ensure you feel connected and supported, helping to ease feelings of isolation. |
Our commitment to your comfort is comprehensive. We often recommend exploring holistic pain management strategies to complement our medical care. This approach ensures your well-being is supported.
At Central Coast VNA & Hospice, our mission is to treat the whole person—not just the illness. We believe everyone deserves to live with dignity and peace, surrounded by a team that truly cares.
For over 74 years, Central Coast VNA & Hospice has been the trusted local nonprofit partner for families. We serve Monterey County, San Benito County, Santa Cruz County, and South Santa Clara County. We are here to help you find relief and peace of mind.
Contact us today to learn how we can support you.
Understanding Your Unique Needs and Goals

Effective pain management starts with one simple action: listening. No two people feel discomfort the same way. This is why a one-size-fits-all approach does not work.
Your story and your personal goals are our most important tools. At Central Coast VNA & Hospice, our entire process is built on partnership. When our Registered Nurse visits your home, their first priority is to understand your unique situation.
This first meeting is a conversation, not an interrogation. Our team is here to gather clues to solve the mystery of your discomfort. We want to understand how it truly affects your life.
Creating a Complete Picture of Your Health
To provide the best support, we look at every factor contributing to your well-being. This goes beyond the physical symptoms you feel right now. Our teams are trained to see the connections between different issues.
This process involves:
- Listening to Your Story: We want to hear about your experiences. This includes what you’ve tried, what worked, and what didn’t.
- Identifying All Symptoms: We help you pinpoint every symptom, even less obvious ones like fatigue or anxiety.
- Understanding Your Goals: We talk about what matters most to you. Is it attending a family event or sleeping through the night?
This first step is guided by our nonprofit mission. Our focus is entirely on your well-being, not on profits. For example, learning about strategies for sleeping better during menopause shows how targeted support can make a difference.
A Foundation Built on Trust
This personal assessment is how we begin to build trust. It shows that we see you as a whole person, not just a list of symptoms. This first step is essential for creating a care plan that brings you genuine relief.
Every person's journey with illness is unique. Our first job is to honor that uniqueness by listening with an open heart and an expert ear, ensuring your voice is the most important one in the room.
This approach is at the heart of everything we do, from home health to hospice. You can learn more about our palliative care approach and see how it focuses on improving your quality of life. By starting with a deep understanding of your needs, we build a plan that brings comfort and dignity.
Building Your Personalized Comfort Plan

Once we understand your story, we build your comfort plan together. This is not a generic checklist. It is a custom roadmap to your comfort, crafted by your entire care team.
At Central Coast VNA & Hospice, our approach is built on teamwork. Our team includes your own doctor, our Registered Nurses, Medical Social Workers, and Chaplains. Each person brings a different perspective to address your total well-being.
This collaborative strategy is a key benefit of choosing a local nonprofit provider. We are rooted in the communities we serve across Monterey, San Benito, Santa Cruz, and South Santa Clara counties. Our focus is always 100% on you.
A Flexible Roadmap to Comfort
A person’s needs can change from one day to the next. Your comfort plan has to be able to change, too. It is a living guide designed to be flexible and evolve with you.
Our teams conduct regular check-ins to see what’s working. We are constantly adjusting the plan to make sure you receive the most effective support. This process guarantees that your comfort remains the top priority.
A great care plan is a partnership. It reflects your voice, respects your choices, and adapts to your journey, ensuring you always feel heard, supported, and comfortable.
This commitment to responsive care is more important than ever. The global market for pain management drugs was valued at USD 84.08 billion in 2023. It is projected to reach USD 125.68 billion by 2034 (Precedence Research, 2024). This growth highlights the need for expert, patient-centered care. You can explore the full research on pain management drugs from Precedence Research.
Integrating Different Types of Support
Your plan will blend various strategies to provide well-rounded support. We know true comfort isn't just about medicine.
Here’s a look at what your plan might include:
- Medical Management: Carefully managed medications prescribed by your doctor and administered by our nurses.
- Emotional and Spiritual Support: Counseling from our Medical Social Workers and guidance from our Chaplains.
- Practical Assistance: Hands-on help from our Hospice Aides with daily activities to preserve your energy.
Our home health care services also use personalized plans to help manage pain after surgery. No matter the situation, your comfort is always at the forefront.
Exploring Effective Management Strategies
There is no single magic bullet for managing pain. The best approach is often a combination of strategies. At Central Coast VNA & Hospice, our teams are experts at blending medical and supportive therapies for the greatest comfort.
This balanced approach allows us to find the right recipe for improving quality of life. We serve families across Monterey, San Benito, Santa Cruz, and South Santa Clara counties.
The Role of Medication
Often, the first line of defense involves medications. Our skilled Registered Nurses work with your doctor to manage medications for pain, nausea, or anxiety.
The goal is always clear: provide the most relief with the fewest side effects. We constantly fine-tune this balance to make sure your comfort plan is safe and effective.
Beyond Medication: The Power of Supportive Therapies
Medications are a critical tool. However, lasting comfort comes from looking at the whole person. This is where non-medical strategies come in.
Our teams weave several non-medication approaches into our care plans:
- Gentle Physical and Occupational Therapy: We focus on helping you maintain mobility and reduce stiffness.
- Calming Breathing Exercises: These simple techniques can help manage anxiety and ease shortness of breath.
- Emotional and Spiritual Support: Our Medical Social Workers and Chaplains offer compassionate guidance to you and your family.
This image shows how different strategies contribute to overall comfort. It reinforces why a combined approach works best.
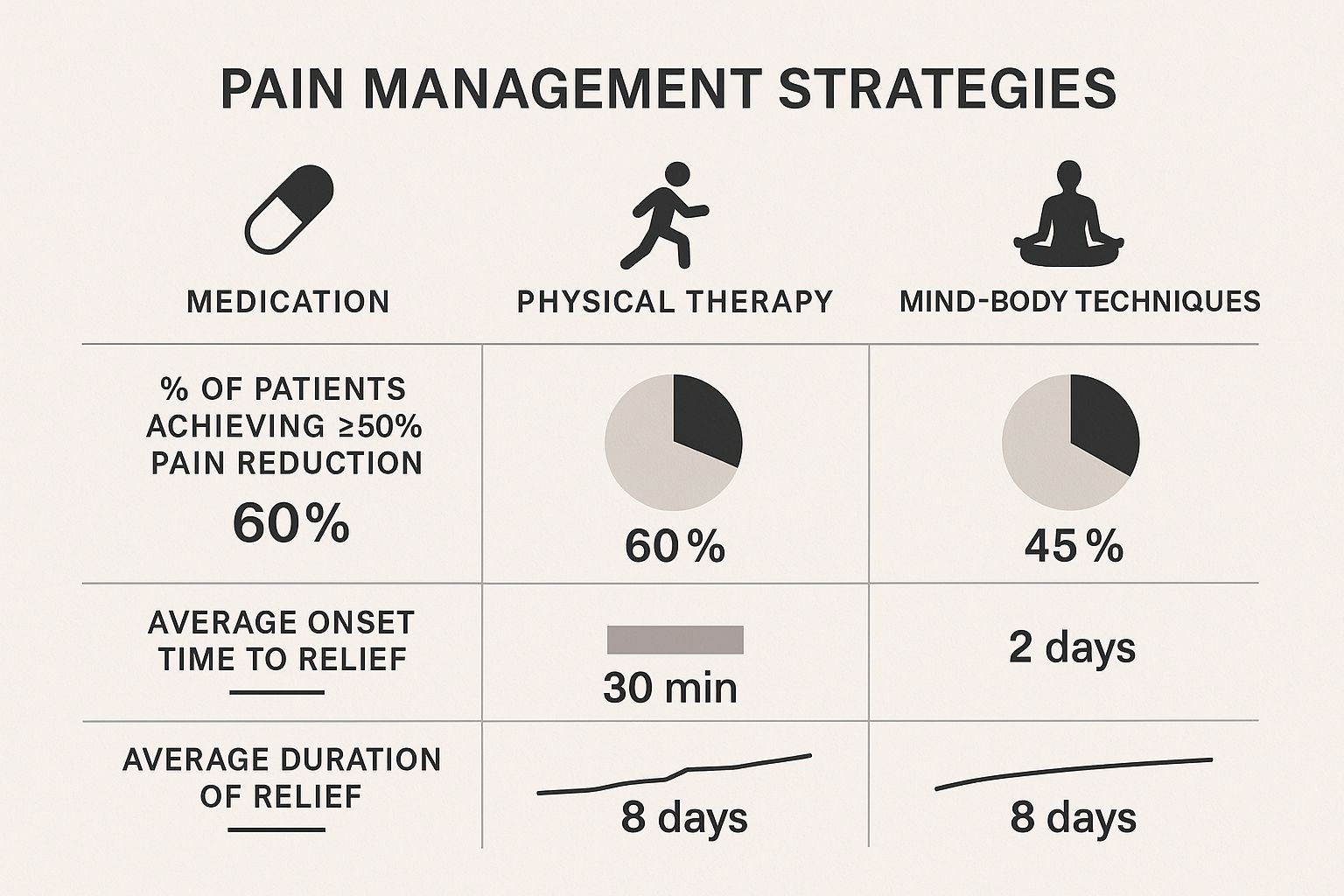
Mixing different methods almost always leads to more sustainable relief. This is the core principle behind our comprehensive care plans.
Creating a Holistic Comfort Environment
You can’t overlook the power of your surroundings. Creating a comfortable environment is an effective part of managing symptoms. Simple changes can make a world of difference.
For people who need more support while resting, exploring hard mattress toppers for ultimate sleep support and easing back pain can be valuable.
A Look at Different Management Strategies
Here's a breakdown of how we combine different approaches. This comparison shows how we layer strategies to create a comprehensive plan for you.
| Strategy Type | Examples We Use | Who It Helps Most |
|---|---|---|
| Medical | Prescription pain relievers, anti-nausea medication, oxygen therapy | Patients with specific, moderate-to-severe physical symptoms like chronic pain or breathing difficulties. |
| Physical | Gentle stretching, light massage, safe positioning techniques | Individuals experiencing stiffness, mobility challenges, or discomfort from being in bed. |
| Emotional/Spiritual | Counseling, guided meditation, chaplain visits, music therapy | Anyone navigating the stress, anxiety, or existential questions that can accompany illness. |
| Environmental | Adjusting room lighting, using calming scents, providing comfortable bedding | Patients who are highly sensitive to their surroundings or who need a peaceful space to rest. |
By weaving these elements together, we address comfort from every angle. This creates a support system that is as unique as the person receiving care.
"The art of care is not just in prescribing the right medication, but in listening to the body and spirit to find the right blend of support that brings true comfort and dignity."
This integrated method is at the heart of our hospice program. To see how this philosophy is put into practice, read more about our hospice pain management philosophy. It’s our commitment to ensuring everyone receives compassionate and effective support.
Seamless Support Across Your Health Journey
Effective pain and symptom management is woven through our entire continuum of care. It is an essential part of the support we provide at every stage. At Central Coast VNA & Hospice, our approach adapts alongside you.
This continuity is what makes a local, nonprofit provider like us so different. We are more than just a service. We are a long-term community partner your family can rely on.
How Our Support Adapts to Your Needs
As your health situation evolves, your care goals may shift. Our team is skilled at modifying your comfort plan to align with these new goals. Your quality of life always remains the top priority.
This flexible approach ensures you get the right care at the right time.
- In Home Health: After surgery or a hospital stay, the goal is recovery. Our home health Registered Nurses manage pain to help you heal comfortably at home.
- In Palliative Care: For those with a serious chronic illness, our focus shifts to long-term comfort. The goal of our palliative care at home is to control persistent symptoms so you can live more fully.
- In Hospice Care: When an illness progresses, the focus becomes peace and dignity. Our hospice team uses their expertise to provide comfort. This allows you and your loved ones to focus on meaningful time together.
The core of our mission is providing unwavering support that meets you where you are. We walk alongside you, adjusting our care to honor your goals every step of the way.
The demand for expert symptom control is growing. The global pain management devices market was valued at USD 7.65 billion in 2022. It is expected to grow by 9.4% each year through 2030 (Grand View Research, 2023), highlighting the critical need for experienced care. You can find more details in the full research about the pain management device market.
Our 74-year legacy in Monterey, San Benito, Santa Cruz, and South Santa Clara counties is built on this promise of seamless, compassionate care.
Your Local Partner for Comfort and Care
Managing pain and other symptoms can feel isolating, but you are not alone. For over 74 years, Central Coast VNA & Hospice has stayed true to its nonprofit mission. We provide expert, compassionate care right here where you live.
We believe everyone deserves to live with dignity and peace. Our goal is to provide exceptional pain and symptom management that honors your wishes. This dedication is the bedrock of our home health, palliative, and hospice care.
Take the Next Step Toward Comfort
If you or a loved one is struggling with the symptoms of a serious illness, support is available. Our experienced teams are ready to build a personalized plan that brings relief. We help you focus on what truly matters.
We are more than just a healthcare provider; we are your neighbors and partners in care, committed to serving the families of Monterey County, San Benito County, Santa Cruz County, and South Santa Clara County.
Don’t wait to find relief. Contact us today to learn more about our services.
Frequently Asked Questions
1. What is the main goal of pain and symptom management?
The main goal is to improve your quality of life. We focus on relieving physical, emotional, and spiritual distress caused by a serious illness. This allows you to live as comfortably and fully as possible.
2. Is pain management only for the end of life?
No, not at all. Pain and symptom management is a key part of all our services, including home health and palliative care. It helps patients recover from surgery, manage chronic illness, and find comfort at any stage of their health journey.
3. Will I get addicted to pain medication?
This is a common concern, but the risk of addiction is very low when medications are managed by a professional medical team. Our Registered Nurses work closely with your doctor to find the lowest effective dose. They constantly monitor for side effects to ensure your safety.
4. What if a care plan isn't working?
A care plan is not set in stone. Our teams regularly check in with you and your family to see how you are doing. If something isn’t providing relief, we will adjust the plan until we find the right combination of strategies for you.
5. Does pain and symptom management include emotional support?
Yes. At Central Coast VNA & Hospice, we care for the whole person. Our teams include Medical Social Workers and Chaplains who provide counseling and spiritual support. This helps address the anxiety, stress, and fear that often come with a serious illness.
6. How are these services paid for?
Most of our home health, palliative care, and hospice care in Monterey County are covered by Medicare, Medi-Cal, the VA, and private insurance. As a local nonprofit, we help you understand your benefits. You can learn more in our guide on how to pay for hospice care.
7 Inspiring Examples of Letters of Grief for Healing
When dealing with the pain of loss, finding the right words can feel impossible. The silence left by a loved one can be overwhelming. Writing letters of grief can be a powerful way to heal.
Putting feelings on paper helps make sense of sorrow. It creates a private space to speak to the person you've lost or document memories. This process helps you reflect and honor a relationship that still matters.
This article shares examples of grief letters for different needs. We will look at the tone, structure, and goal of each one. This will help you write your own meaningful message.
1. C.S. Lewis's Letters to Malcolm: Chiefly on Prayer - Grief Letters
Some of the most powerful letters of grief were never meant to be public. C.S. Lewis wrote to his friend Malcolm after his wife, Joy Davidman, died. These letters show a raw and honest look at loss.

This collection shows that grief writing can be messy. It can be a questioning process shared with a trusted friend. Lewis was not afraid to ask hard questions about his faith and loss.
Strategic Analysis & Breakdown
- Tone: The tone is personal, honest, and thoughtful. Lewis is not just sad; he is trying to understand his sadness.
- Structure: The letters are like a conversation. This format allows for exploring complex feelings without pressure.
- Audience: The first audience was one trusted friend. This allowed for total honesty, which makes the letters so powerful.
Actionable Takeaways for Your Own Letters
If this approach feels right for you, here are some tips:
- Find a trusted friend: Share your raw thoughts with someone who will not judge you. This person should be a safe space for your questions or anger.
- Think through your feelings: Use writing to explore big questions. It is okay to analyze your feelings as you navigate grief.
- Don't hide your doubt: Healing involves facing difficult emotions, like doubt or frustration. Your letters can be a place to voice these thoughts safely.
2. Lincoln's Bixby Letter - Condolence to Bereaved Mother
Sometimes, letters of grief are written for a whole country. Abraham Lincoln's 1864 letter to Mrs. Lydia Bixby is a great example. She was a mother thought to have lost five sons in the Civil War.

The letter shows how to offer comfort with dignity. It acknowledges a terrible sacrifice while reminding the family of the honor in their loved one's service. This is a powerful approach for official letters.
Strategic Analysis & Breakdown
- Tone: The tone is formal, serious, and caring. It carries official weight while showing real compassion.
- Structure: The letter is short and to the point. It acknowledges the loss, offers comfort, and ends by honoring the sacrifice.
- Audience: The letter was for a grieving mother, but it also spoke to a nation at war. It validated personal loss on a public level.
Actionable Takeaways for Your Own Letters
To write a letter with dignified comfort, follow these tips:
- Acknowledge the sacrifice: Directly and respectfully state the size of the loss. Do not downplay the pain.
- Connect loss to a larger meaning: If it fits, frame the loss in a context of shared values, like service or community. This can offer a sense of purpose. Organizations like Central Coast VNA & Hospice offer hospice and bereavement support services to help families find meaning.
- Use respectful language: Choose words carefully to show honor. Formal language can create a sense of deep respect.
3. Rilke's Letters on Loss and Solitude
The poet Rainer Maria Rilke saw grief as a deep part of life. His letters to grieving friends treat loss as something that helps us grow. These letters of grief are less about quick comfort and more about making sorrow a part of you.

For Rilke, grief was something that needed time to develop within us. His writings encourage a quiet, patient relationship with sorrow. He often used powerful images, connecting loss to creativity and nature.
Strategic Analysis & Breakdown
- Tone: The tone is deep, patient, and poetic. Rilke’s letters offer a gentle path through pain, framing it as necessary for growth.
- Structure: His letters are thoughtful and use imagery. They are like meditations that guide the reader to a new view of their loss.
- Audience: The audience was usually a friend or mentee dealing with loss. This allowed Rilke to offer personal, thoughtful guidance.
Actionable Takeaways for Your Own Letters
If you like this thoughtful approach, here are some tips:
- Use images: Instead of saying "it will get better," use pictures. For example, describe grief as a cold winter that will turn to spring.
- Frame grief as part of life: Acknowledge that sorrow is a hard but normal part of being human. Writing about grief as a season or journey can help.
- Connect loss to deeper meaning: Your letters of grief can be a place to explore how loss changes your view on life and love. This moves the focus from pain to growth. Finding community is also helpful; learn about bereavement and grief support groups on ccvna.com.
4. Queen Victoria's Letters After Prince Albert's Death
For some, grief is a long and public journey. Queen Victoria’s letters after her husband, Prince Albert, died in 1861 are a powerful example. Her letters show a deep mourning period that lasted for decades.
These letters of grief were sent to family, friends, and officials. They offer a look into her struggle with overwhelming loss. This collection shows grief is a marathon, not a sprint.

The infographic shows how her letter writing changed over many years. It moved from intense private sadness to a mix of personal memory and public duty.
Strategic Analysis & Breakdown
- Tone: The tone is one of deep, lasting sorrow, but also duty. Victoria’s letters are formal yet filled with personal pain.
- Structure: Her letters varied. Some were intimate notes to family, while others were official papers where grief was a reason for her actions.
- Audience: The audience was broad, from her daughter to government ministers. She had to adapt her expression of grief for each person.
Actionable Takeaways for Your Own Letters
If you are grieving while managing big responsibilities, consider Victoria’s approach:
- Integrate, don't hide: Allow your grief to be part of your life. Acknowledge your loss in your communications when it feels right.
- Maintain a connection: Use your writing to talk to or about your loved one. Sharing memories helps maintain a comforting connection.
- Allow a long timeline: Victoria’s long mourning reminds us there is no "right" amount of time to grieve. Let your letters of grief reflect your own journey.
5. Joan Didion's Email Grief Communications
In our digital age, letters of grief have changed. Joan Didion used email to communicate with friends and family during a time of great tragedy. She managed her husband's death and her daughter's critical illness through digital messages.
These emails show how modern communication helps us connect during loss. Her messages were a lifeline, allowing her to share updates and receive support. It shows that grief writing can be urgent and practical.
Strategic Analysis & Breakdown
- Tone: The tone is often direct and factual. Didion's emails focused on clarity over fancy words, showing the crisis she was in.
- Structure: The messages were short and functional, often updates to a group. This highlights a key purpose of modern letters of grief: managing information.
- Audience: The audience was a close network of friends and family. An email list allowed her to reach everyone at once, saving emotional energy.
Actionable Takeaways for Your Own Letters
If you are navigating grief today, consider these strategies:
- Create a communication hub: Use an email list or private group chat to share updates. This saves you from repeating painful news.
- Focus on function: During a crisis, don't worry about perfect writing. Short, direct messages are fine and often better.
- Save important messages: The digital record of support can be a comfort to look back on. Helping others through such times can be a powerful experience; you can learn more about volunteering for hospice to support families in Monterey and Santa Cruz Counties.
6. Military KIA Notification and Response Letters
The exchange of letters of grief in the military is a structured but personal process. When a service member is killed in action (KIA), a formal notice is given. This is often followed by condolence letters from commanders and fellow soldiers.
These letters have great emotional weight. They connect the family's private sorrow with the military unit's shared grief. They honor the soldier's service and sacrifice.
Strategic Analysis & Breakdown
- Tone: The tone is a mix of formal respect and deep personal sadness. Official letters follow rules, while personal replies can be very emotional.
- Structure: The process is structured. It starts with official notice, then condolence letters, and often a response from the family.
- Audience: The audience includes the grieving family, commanding officers, and fellow service members.
Actionable Takeaways for Your Own Letters
If you are navigating a loss in the military community, these ideas can help:
- Balance formality and emotion: It is fine to use formal language. But don't let rules stop you from sharing your true feelings.
- Ask for memories: When writing to your loved one’s unit, ask them to share stories. This can provide a fuller picture of their life.
- Connect with support systems: Writing these letters is very hard. Military grief counselors and support groups for families can help. Preparing for end-of-life decisions is also a critical part of this process; Learn more about advance care planning on ccvna.com.
7. Parent-to-Child Explanation Letters About Death
Some of the most important letters of grief are written from a parent to a child. These letters explain the death of a family member or pet in a simple, honest way. They can be a gentle start to a hard conversation and become a treasured memory.
These letters focus on clarity and emotional safety. For instance, explaining a grandparent's death needs simple words a child can understand without being scared. The goal is to provide a foundation for understanding.
Strategic Analysis & Breakdown
- Tone: The tone must be gentle, reassuring, and direct. It balances honesty about death with a message of love and safety for the child.
- Structure: The letter is usually short with simple sentences. It often states a fact, shares a happy memory, expresses feelings, and ends with reassurance.
- Audience: The audience is a child. The words and ideas must be right for their age.
Actionable Takeaways for Your Own Letters
If you need to write this difficult letter, these tips can help:
- Use simple, clear language: Avoid confusing phrases like "passed away." Instead, use clear terms like, "Grandma's body stopped working, and she died."
- Reassure and validate: Tell the child they are loved and safe. Acknowledge that it's okay to feel sad, angry, or confused.
- Create an opening for talk: End the letter by inviting questions. Let the child know you are there to talk when they are ready. A grief book specifically designed to help children tackle difficult emotions can also help. For more support, families can find information on grief counseling for families.
Comparison of 7 Grief Letter Examples
| Example | Implementation Complexity 🔄 | Resource Requirements ⚡ | Expected Outcomes ⭐ | Ideal Use Cases 💡 | Key Advantages 📊 |
|---|---|---|---|---|---|
| C.S. Lewis's Letters to Malcolm | Moderate - thoughtful, intellectual | Low - personal writing | Deep theological insight on grief | Intellectual/spiritual grief exploration | Honest, comforting, integrates faith & doubt |
| Lincoln's Bixby Letter | Low - formal, concise, scripted | Low - brief official correspondence | Empathy and national solidarity | Official condolence, leadership communication | Balances formality with genuine emotion |
| Rilke's Letters on Loss and Solitude | Moderate - poetic, abstract | Low - personal, artistic writing | Emotional depth, artistic transformation | Artistic and philosophical processing of grief | Elevates grief to meaningful human experience |
| Queen Victoria's Letters After Albert's Death | High - extensive, long-term | Moderate - ongoing written records | Public and private mourning balance | Historical mourning, sustained grief expression | Shows grief as ongoing process, combines duty |
| Joan Didion's Email Grief Communications | Low to Moderate - digital, immediate | Moderate - requires tech access | Fast, widespread emotional support | Crisis communication, digital grief processing | Immediate support, community building |
| Military KIA Notification and Response Letters | High - formal protocols, sensitive | Moderate - official coordination | Structured grieving, honor and support | Military loss notification and family communication | Structured support, honors sacrifice |
| Parent-to-Child Explanation Letters | Moderate - age-appropriate, careful | Low to Moderate - thoughtful crafting | Child-friendly understanding of death | Explaining death to children | Provides comfort, educational, reusable |
Your Story, Your Words: Compassionate Support on the Central Coast
Written words can be very powerful in times of grief. From a president’s formal letter to a mother’s private thoughts, there is no single right way to express sorrow. These examples of grief letters all create a space for honest emotion and connection.
Key Takeaways from Historic and Modern Grief Letters
The main lesson from these examples is authenticity. Whether you write to a friend or for yourself, your true feelings are what matter most. The structure can be simple or deep, but the words should come from a place of genuine care.
Another key lesson is the power of shared experience. Lincoln’s letter acknowledged a shared sacrifice. Writing or receiving a letter reminds us that we are not alone in our grief.
Putting Pen to Paper: Your Next Steps
These examples are practical guides to help you find your voice when words are hard to find.
Here are some steps you can take:
- Start small: A simple, heartfelt note can mean the world to someone who is grieving.
- Share a memory: Sharing a happy memory of the person who has passed helps keep their spirit alive.
- Write for yourself: Writing a letter to the person you lost can be a healing way to process your own grief.
Writing letters of grief is about empathy and courage. It is a skill that helps you offer support and understand your own feelings. If you want to share your story more widely, you might find inspiration in these ideas for a memoir.
Navigating grief is a deeply personal journey, and no one should have to walk it alone. Central Coast VNA & Hospice has provided compassionate care for over 74 years. We are a local, nonprofit organization serving Monterey County, San Benito County, Santa Cruz County, and South Santa Clara County.
Our mission-driven team offers expert emotional, spiritual, and medical support for patients and their families. This support is part of our Continuum of Care, from home health and palliative care to hospice. If you or a loved one needs support, contact us to learn more about our services.
Frequently Asked Questions (FAQs)
1. Why is writing a letter of grief helpful?
Writing a letter of grief helps organize your thoughts and feelings. It provides a private outlet to express love, sorrow, or unspoken words. This process can be a very healing part of the grieving journey.
2. What should I include in a grief letter to a friend?
A good grief letter to a friend should be simple and sincere. Acknowledge their loss, share a fond memory of the person who died, and offer specific support, like bringing over a meal or helping with errands. Avoid clichés and focus on genuine compassion.
3. How can I write about my own grief if I can't find the words?
Start by writing just one sentence about how you feel right now. You don't need to write a perfect letter. You can also try writing a letter directly to the person you lost, sharing memories or feelings you never got to express.
4. What kind of support does Central Coast VNA & Hospice offer for grief?
As a nonprofit serving the Central Coast for over 74 years, we offer comprehensive bereavement services. Our support includes counseling with professional staff like Chaplains, support groups, and resources for families in Monterey, San Benito, and Santa Cruz Counties. These services are designed to help families navigate loss with compassionate care.
5. How do I explain death to a child in a letter?
Use simple, direct language that is appropriate for the child's age. Avoid confusing phrases. Reassure the child that they are loved and safe, and let them know it is okay to feel sad. End the letter by inviting them to ask questions.
Your Guide to Palliative Home Care
Palliative home care is an extra layer of support for anyone managing a serious illness at home. It is specialized medical care focused on relief from symptoms and stress. This care works alongside your primary treatment plan to improve quality of life for you and your family.
Understanding Palliative Care in Your Home

Living with a serious illness like heart disease or cancer can be stressful. It affects your body and can also be emotionally overwhelming. Palliative home care helps you face these challenges where you feel most comfortable.
Think of your doctors as specialists for different body parts. Your palliative care team is like a coach who looks at your overall well-being. They work with your other doctors to create a coordinated plan.
This team helps manage symptoms like pain, fatigue, and shortness of breath. The goal is to help you feel stronger and more in control of your health.
What Palliative Care Is Not
It is important to know that palliative care is not the same as hospice care. Many families confuse the two, but they have different purposes.
- Palliative Care: You can start this care at any stage of a serious illness. You can get it at the same time as treatments like chemotherapy. The focus is on relieving symptoms and improving daily life.
- Hospice Care: This care is for people with a life expectancy of six months or less. It begins when someone is no longer seeking treatments to cure their illness. The focus is entirely on comfort at the end of life.
Palliative care adds support to help you manage your illness. It is about living as well as possible, for as long as possible. You can get treatment and feel better at the same time.
A Mission of Compassionate Local Support
For over 74 years, Central Coast VNA & Hospice has been a nonprofit provider serving local communities. We bring this supportive care to homes across Monterey County, San Benito County, Santa Cruz County, and South Santa Clara County. Our care is built on respect for your personal goals and values.
Palliative care is a partnership. A dedicated team helps create a clear, individualized care plan that reflects your needs, preferences, and what matters most to you and your family.
By focusing on the whole person—body, mind, and spirit—we help reduce the burden of illness. To learn more about how our expert teams can support you, explore our palliative home care services. Contact us today to learn how we can help.
Who Can Benefit From Palliative Home Care

Palliative home care is for anyone dealing with a serious, long-term illness. It is for people of any age who need help managing difficult symptoms at home.
The entire focus is on improving quality of life. This care can help people with many different diagnoses, not just cancer. It is a proactive step that helps people feel stronger and more in control.
Common Conditions That Benefit From Palliative Care
Palliative care is always tailored to the person, not the illness. However, certain conditions often come with complex symptoms that this support can ease.
Some of these conditions include:
- Heart Conditions: For someone with congestive heart failure (CHF), managing shortness of breath and fatigue is key to their daily comfort.
- Cancer: Patients can receive palliative support alongside treatments like chemotherapy to help with pain and nausea.
- Lung Diseases: Chronic obstructive pulmonary disease (COPD) and other illnesses often require expert help to make breathing easier.
- Neurological Diseases: Conditions like Alzheimer's or Parkinson's bring unique challenges that palliative care is built to address.
- Kidney Disease: For those on dialysis or with advanced kidney failure, symptom management and care coordination make a big difference.
Choosing palliative home care is not about giving up. It is about adding support to live more comfortably and fully.
Recognizing When It Might Be Time for More Support
Knowing when to ask for palliative care is a personal decision. There are common signs that an extra layer of help would make a difference. If you notice frequent hospital trips or hard-to-control symptoms, it might be time.
Palliative care meets you where you are. It acknowledges the physical, emotional, and spiritual toll of a serious illness and provides a team to help carry that burden.
Think about whether you or a loved one is experiencing:
- Frequent hospitalizations or emergency room visits for the same problems.
- Uncontrolled pain, fatigue, or nausea that gets in the way of daily life.
- Emotional distress, like anxiety or depression connected to the illness.
- Difficulty with daily activities, which reduces independence.
- Family members who are feeling overwhelmed and need guidance.
These are the exact challenges palliative care is designed to solve. As a nonprofit provider with over 74 years of service, Central Coast VNA & Hospice ensures families in Monterey County and nearby areas get the compassionate care they deserve. Our mission is to bring comfort and expert support right into your home. For those exploring their options, it can be helpful to use resources that help you determine if palliative home care is right for them.
What Your Palliative Home Care Team Provides
When you choose palliative home care, you get an entire team of professionals. This team works with you, your family, and your primary doctor. They create a complete circle of support.
At Central Coast VNA & Hospice, this team-based approach is at the core of what we do. It ensures every part of your well-being is addressed. Each team member brings their expertise to improve your quality of life.
Your Core Palliative Support Professionals
The strength of palliative home care is its team. This group of specialists all focus on your comfort and goals. They work together to support you.
Here’s a look at the key professionals on your care team.
At the heart of any palliative home care plan is a dedicated expert nurse home service, providing essential medical care and compassionate support right in the comfort of a patient's home.
This table breaks down who you will be working with.
Your Palliative Home Care Team
| Team Member | Role and Responsibilities |
|---|---|
| Registered Nurse (RN) | Your main point of contact. An expert in managing pain and symptoms and coordinating your care with other doctors. |
| Medical Social Worker | Provides emotional support and helps with practical challenges. They connect you with community resources and offer counseling. |
| Chaplain | Offers spiritual comfort for people of all faiths, or no faith. They help you explore sources of peace and meaning during a difficult time. |
Together, this team makes sure your care is seamless and responsive to your changing needs.
This coordinated effort directly leads to a better quality of life and comfort at home.
Comprehensive Services Delivered at Home
Your palliative care plan is built completely around you. The services are designed to bring you comfort and reduce stress. They give you more control over your life.
This approach is more important than ever.
According to the National Hospice and Palliative Care Organization (NHPCO), community-based palliative care programs have increased by 167% since 2008 (NHPCO, 2019). This shows that more people are choosing to receive this supportive care at home.
Here are some of the key services you can expect from your team:
- Expert Symptom Control: We focus on managing pain, fatigue, nausea, and other symptoms to help you feel as comfortable as possible.
- Medication Management: Your team helps you understand your medications and makes sure they are working effectively for you.
- Emotional and Spiritual Support: We provide counseling to help you and your family navigate the emotional journey of a serious illness.
- Care Coordination: Your team communicates with all of your doctors to ensure everyone is on the same page. This helps prevent unnecessary hospital visits.
- Advance Care Planning: We guide you through important conversations about your future healthcare wishes, making sure your voice is heard.
Many of these services are similar to the support provided by our home health care services. Both are part of our commitment at Central Coast VNA & Hospice to providing a full continuum of care for residents in Monterey County, San Benito County, and the surrounding areas.
The Key Benefits of Receiving Care at Home

There’s a reason people say, “There’s no place like home.” Receiving palliative care in your own house has benefits that go beyond medical treatment. Being surrounded by familiar things can be powerful and healing.
For many, home is a safe and comfortable place. Bringing expert palliative home care into this space means you can keep your routines and a greater sense of independence. Your care team comes directly to you.
This approach gives you one-on-one attention focused on your needs. It also lets your family be more involved. They become active partners in your care, which brings comfort to everyone.
Promoting Comfort and Well-Being
The main goal of palliative care is to improve your quality of life. There is no better place to do that than at home. It helps you avoid hospital infections and the anxiety of clinical settings.
Your care plan is designed around your home life. This makes your daily activities as comfortable as possible.
The recognition of these benefits is driving growth in the palliative care field. One study found that patients receiving home-based palliative care had significantly lower rates of hospital admission in the last 30 days of life (Journal of Palliative Medicine, 2017). This shows how home-based models are an effective and compassionate way to meet patients' needs.
Greater Independence and Family Involvement
Receiving care at home keeps you in control. You decide your schedule and when you see visitors. This is key for maintaining dignity and a positive outlook.
It also allows family members to participate more fully in your care. They can learn from your Registered Nurse and Medical Social Worker. This helps build a stronger support system for everyone.
Here’s how home-based care supports the whole family:
- Personalized Care: Your team gets to know you in your own space, leading to a truly personal care plan.
- Reduced Stress: Avoiding travel and hospital stays lessens the strain on you and your loved ones.
- Better Communication: Regular visits from your care team ensure everyone is on the same page.
- Cost-Effectiveness: Palliative home care can often be a more affordable long-term option.
At Central Coast VNA & Hospice, we have been committed to this care model for over 74 years. Our nonprofit mission is to bring high-quality, compassionate support into homes across Monterey County, San Benito County, and our other service areas. You can learn more about the specific benefits of palliative care and how our teams make a difference every day.
How to Start the Palliative Home Care Process
Taking the first step toward getting more support can feel difficult. The good news is that starting palliative home care is usually simple. It is a gentle process designed to bring comfort, not create more stress.
The process often begins with a conversation with a doctor. Your primary doctor or a specialist can make a referral for palliative care. This ensures smooth coordination between your medical teams.
Taking the Initiative for Your Care
You and your family can be proactive. If symptoms are becoming hard to manage, you can reach out directly to a provider like Central Coast VNA & Hospice. You can call and ask to learn more about our support.
This puts you in control of exploring your options. A compassionate professional will listen to your concerns and answer your questions. There is no obligation to start care.
What to Expect During an Initial Consultation
After you connect with a provider, the next step is an initial consultation. This is a calm conversation focused on you and your needs. A Registered Nurse will usually visit you at home.
During this meeting, the team will want to understand:
- Your physical symptoms: Such as pain, fatigue, or shortness of breath.
- Your personal goals: What matters most to you right now?
- Your emotional and spiritual needs: How is the illness affecting you and your family?
- Your current medical treatments: To ensure the new plan works with them.
This assessment is the foundation for creating a personal care plan. The goal is to build a roadmap for improving your quality of life at home.
Discussing Palliative Care with a Loved One
Bringing up palliative care with a loved one requires sensitivity. It helps to frame it as a positive choice to add more expert support. Emphasize that it is not about giving up, but about living better.
You could say, "I learned about a service that can help manage your symptoms better, so you can have more energy for things you enjoy." Focusing on benefits—like more comfort and fewer hospital trips—can make the conversation feel hopeful.
As a nonprofit organization serving Monterey County and the surrounding communities for over 74 years, Central Coast VNA & Hospice is here to guide you. Learn more about our palliative care services and contact us today for a compassionate, no-obligation consultation.
Frequently Asked Questions About Palliative Home Care
When you are navigating a serious illness, having questions is normal. Getting clear answers is the first step toward feeling more in control. Here are answers to some common questions we hear from families in Monterey County and our neighboring communities.
How is palliative care different from hospice care?
Palliative care can be given at any stage of a serious illness, right alongside curative treatments like chemotherapy. Hospice care is for someone with a life expectancy of six months or less who is no longer seeking curative treatments. The focus of hospice is on comfort at the end of life.
Can I keep my own doctors?
Yes, absolutely. The palliative home care team works in partnership with your primary doctor and other specialists. They do not replace your current doctors; they add an extra layer of support.
Is palliative home care covered by insurance?
Yes, in most cases. Palliative care is often covered by Medicare Part B, Medi-Cal, and most private insurance plans. Our team at Central Coast VNA & Hospice can help you understand your specific benefits.
When is the right time to start palliative care?
The best time to start is as soon as a serious illness begins to affect your quality of life. It is better to bring in support early, before symptoms become overwhelming. This gives the team more time to help you feel comfortable and in control.
What kind of professionals are on a palliative care team?
Your team will typically include a Registered Nurse, a Medical Social Worker, and a Chaplain. The Registered Nurse manages your symptoms, the Medical Social Worker provides emotional support, and the Chaplain offers spiritual comfort. They all work together with your other doctors.
For over 74 years, Central Coast VNA & Hospice has been a trusted nonprofit provider on the Central Coast. If you have more questions or think palliative home care could be right for your family, we are here to help. Reach out to us at https://ccvna.com to start the conversation.
7 Therapeutic Grief Activities for Adults
Grief is a deeply personal journey. There is no right or wrong way to navigate it. The path forward often feels uncertain.
Engaging in intentional activities can provide structure and comfort. It can also help you process complex emotions. This is especially true for those managing loss while on hospice care.
This article offers a collection of helpful grief activities for adults. We will explore practical ways to honor your loss and begin to heal. You will find specific steps for each activity, from journaling to connecting with nature.
Each suggestion is a gentle tool, not a requirement. The goal is to help you find what resonates with you. As a nonprofit serving Monterey County and surrounding areas for over 74 years, Central Coast VNA & Hospice offers compassionate support to guide you.
1. Grief Journaling and Writing
Expressive writing is one of the most accessible grief activities for adults. This practice involves putting your thoughts and emotions onto paper. It creates a private space to navigate the complex feelings that accompany loss.

The goal isn't to create perfect writing. Instead, the focus is on honest self-expression. Research shows that expressive writing can improve mental and physical health by helping people process difficult emotions.
How to Start Grief Journaling
Getting started does not have to be intimidating. Your journal is a judgment-free zone where your feelings are valid.
- Create a Comfortable Space: Find a quiet spot where you feel safe. Gather a journal, a favorite pen, and perhaps some tissues.
- Start Small: Commit to just 5-10 minutes a day. Building a consistent habit is more important than writing for long periods.
- Use Writing Prompts: If you’re unsure what to write, prompts can help. Try starting with, "A memory I want to preserve is..."
- Write a Letter: A powerful exercise is writing a letter to your loved one. You can share things you never got to say or tell them about your day.
For those who prefer speaking their thoughts, technology offers a helpful alternative. You can use your phone to record your feelings and then try converting voice notes to text to create a digital journal.
2. Memorial Art and Creative Expression
Channeling emotions into art is a powerful, non-verbal way to navigate loss. Memorial art allows you to create a tangible tribute to a loved one. It can transform feelings of grief into something you can see and touch.

The focus of this grief activity is on the creative journey. The final product is not as important as the process. Engaging in art allows you to process memories and honor your loved one's legacy.
How to Start with Memorial Art
You do not need to be an artist to benefit from creative expression. The goal is simply to create something meaningful to you.
- Gather Meaningful Items: Collect materials that remind you of your loved one. This could include old clothing, photographs, or favorite letters.
- Choose a Medium: Select a project that feels right for you. This could be a memory quilt, a photo collage, or painted rocks for a garden.
- Focus on the Process: Allow yourself to feel whatever emotions come up. The act of creating can be a meditative way to process your grief.
- Create a Tangible Tribute: Creating tributes, like crafting with cross stitch family tree patterns, can honor loved ones.
- Work with Others: Invite family or friends to join you. Collaborating on a project can be a beautiful way to share stories and support one another.
3. Support Group Participation
Sharing your journey with others who understand is a cornerstone of healing. Support groups are one of the most powerful grief activities for adults. They provide a safe space to connect with people who have experienced similar losses.

The core benefit of a support group is community and mutual understanding. These groups help normalize the complex emotions of grief. This shared experience can significantly reduce feelings of loneliness.
How to Find and Engage with a Support Group
Finding the right group is a personal process. It is okay to try a few before one feels right. The goal is to find a community where you feel supported.
- Look for Specificity: Seek groups tailored to your specific type of loss. This could include groups for spousal loss or child loss.
- Attend a Few Sessions: Give any group a fair chance. Commit to attending at least three or four meetings before deciding if it is a good fit.
- Participate at Your Own Pace: You are not required to share. Listening can be just as therapeutic, so participate when you feel comfortable.
- Explore Different Formats: Groups meet in various settings, including online. Consider which format best suits your comfort level.
Central Coast VNA & Hospice offers bereavement support in Monterey County and San Benito County. You can explore how to find grief support groups near you to discover local programs.
4. Memorial Rituals and Ceremonies
Creating meaningful rituals is another powerful grief activity. These ceremonies provide a structured way to honor a loved one's memory. Rituals create a dedicated time and space to remember and process your loss.

The purpose of a memorial ritual is to affirm your connection with the person who has died. These acts can be deeply personal and do not need to follow any rules. They serve as an anchor, offering comfort and continuity.
How to Create a Memorial Ritual
Personalizing a ritual makes it more meaningful. It should reflect the unique life and personality of your loved one.
- Reflect Their Personality: Plan an activity that honors who they were. Did they love nature? Plant a memorial tree.
- Involve Others: Invite family and friends to participate. This shared act of remembrance can strengthen bonds.
- Create an Ongoing Tradition: Recurring rituals can provide comfort for years. Consider an annual gathering to share stories.
- Be Flexible: A ritual doesn't have to be rigid. Allow it to change as your grief journey progresses.
Organizations like CCVNA provide guidance and support in creating these tributes. You can learn more about our hospice bereavement services on ccvna.com. Our professional Chaplains and Social Workers help families find ways to honor their loved ones that feel authentic and healing.
5. Physical Exercise and Movement Therapy
Engaging in physical activity can help process the impact of loss. This grief activity uses movement to release tension and improve mood. It provides a constructive outlet for the intense energy that grief can create.
The mind-body connection is central to this practice. Movement releases endorphins, which act as natural mood elevators. For those experiencing grief, which often causes fatigue or physical pain, movement offers a way to address these symptoms.
How to Start with Movement Therapy
Incorporating movement into your grief journey can be simple. The goal is to move in a way that feels supportive, not strenuous.
- Start with Gentle Activities: Begin with low-impact options like short walks, gentle stretching, or a beginner’s yoga class.
- Connect Through Shared Activities: Consider an activity your loved one enjoyed, like hiking a favorite trail.
- Find Social Support: Join a walking group or ask a friend to exercise with you. Social connection can reduce feelings of isolation.
- Listen to Your Body: Grief can be exhausting. Pay attention to your energy levels and adjust your activity accordingly.
Gentle, regular exercise provides significant mental and physical health advantages. You can learn more about how exercise remains important at any age and find ways to stay active safely.
6. Nature-Based Healing Activities
Engaging with the natural world provides a gentle space for healing. Nature-based activities offer a therapeutic escape from grief. This practice helps restore emotional balance and offers perspective when loss feels overwhelming.
This concept is rooted in our innate connection to nature. Practices like "forest bathing" have been shown to reduce stress and improve mood. For those grieving, nature offers a non-judgmental environment to process emotions.
How to Start with Nature-Based Healing
You do not need to be an avid outdoors person to benefit from nature. The key is to intentionally immerse your senses in a natural environment.
- Start Close to Home: Begin with accessible spaces like a local park or your own backyard. The goal is connection, not a strenuous expedition.
- Practice Mindful Observation: Sit quietly and notice details around you. Focus on the feeling of a breeze or the sound of birds.
- Create a Memorial in Nature: Consider planting a tree or a small garden in honor of your loved one. Tending to it can be a meaningful ritual.
- Join a Group: Many communities offer grief hiking groups. Sharing the experience with others who understand can be very validating.
Engaging with nature can be one of the most restorative grief activities for adults. It allows you to find solace and strength in the world around you.
7. Music and Sound Therapy
Music and sound therapy can be a powerful way to process grief. This approach uses sound and melody to help you connect with emotions when words are not enough. It creates a space for you to feel, remember, and express deep feelings.
Sound can unlock memories and feelings in a unique way. Whether it’s listening to a meaningful song or playing an instrument, this practice soothes the nervous system. Music therapy is often used in hospice and bereavement settings to provide comfort.
How to Use Music for Grief
You do not need to be a musician to benefit from sound therapy. The goal is to use music as a tool for emotional release.
- Create Memorial Playlists: Compile songs that remind you of your loved one. You can create playlists for different moods.
- Balance Your Listening: It is okay to listen to sad songs that allow you to cry. Also include music that brings a sense of peace or hope.
- Try Sound Healing: Instruments like singing bowls produce calming vibrations. You can find guided sound bath meditations online.
- Engage Actively: If you feel up to it, try singing or humming. The physical act of creating music can be a powerful emotional release.
Music therapy is a core part of comprehensive end-of-life care. To learn more, explore supportive therapies in hospice pain management.
Your Trusted Partner on the Healing Journey
Navigating grief can feel isolating, but you are not alone. The grief activities shared in this guide are tools to help you process emotions and honor your loved one.
From the quiet reflection of journaling to the strength found in support groups, each activity offers a different path. Creative expression, physical movement, and time in nature all provide unique ways to heal. The most important takeaway is that there is no single "right" way to grieve.
Your healing journey is an active process. We encourage you to choose one activity that feels comforting right now. Schedule time for it, and consider reaching out to a friend or support group.
Embracing these practices helps transform grief into a meaningful part of your story. By actively participating in your healing, you pave the way for hope and peace.
At Central Coast VNA and Hospice, we understand that grief is a long journey. Our compassionate bereavement support services are here for families throughout Monterey, San Benito, Santa Cruz, and South Santa Clara counties. If you or someone you know needs guidance, our dedicated team is here to help.
Contact us today to learn more about our home health, palliative care, and hospice services.
Frequently Asked Questions
1. What are grief activities?
Grief activities are intentional practices designed to help individuals process loss, honor memories, and navigate their emotions. Examples include journaling, creating memorial art, joining a support group, and spending time in nature.
2. How do I know which grief activity is right for me?
The best activity is one that feels authentic and comforting to you. Consider your personality and what normally brings you peace. It is okay to try several different activities to see what resonates most at this time.
3. Can grief activities be done with family and friends?
Yes, many grief activities can be shared. Creating a memorial project, holding a remembrance ceremony, or going for a walk in nature together can provide mutual support and strengthen bonds during a difficult time.
4. How long should I continue with these activities?
There is no set timeline for grief. You can engage in these activities for as long as they feel helpful. Some, like an annual memorial ritual, may become lifelong traditions that evolve as your grief does.
5. Where can I find grief support in Monterey County?
Central Coast VNA & Hospice offers professional bereavement support services for families in Monterey County, San Benito County, and surrounding communities. We provide support groups and individual counseling to help you navigate your healing journey.
Your Guide to In Home Care for Seniors
When a loved one needs more support, in-home care brings professional medical help right to their door. It helps older adults live safely at home and manage health conditions. This service adds a support system that changes as their needs change.
What In-Home Care for Seniors Really Means
In-home care allows seniors to get help without leaving their own house. For families on the Central Coast of California, it means trusted medical professionals provide care where loved ones feel most comfortable. It is a partnership designed to honor their wish to remain at home.
The desire to age in place is very strong. About 75% of Americans over 50 say they want to stay in their current homes as they get older. This preference is a big reason why professional in-home care is so important.
Understanding the Continuum of Care
In-home care is not a single service. It is a range of support that can be adjusted over time. This is often called the continuum of care.
This approach ensures that as a person's health needs shift, their care plan can change too. It creates a smooth and supportive journey. For many, this journey starts with skilled services to manage a new diagnosis or recover after a hospital stay.
- Home Health: This is skilled medical care from a Registered Nurse or therapist. It helps a patient recover from an illness, injury, or surgery.
- Palliative Care: This is specialized support focused on relieving symptoms of a serious illness. The goal is to improve quality of life for the patient and family.
- Hospice Care: This is compassionate end-of-life care. It prioritizes comfort and dignity for the patient and supports their family.
Central Coast VNA & Hospice is the only local nonprofit that offers this full range of services. Our teams work together to ensure patients in Monterey County, San Benito County, Santa Cruz County, and South Santa Clara County get the right care at the right time. This integrated approach gives families peace of mind.
A Holistic and Compassionate Approach
Great in-home care is about more than just medical checks. It requires understanding the whole person, including common health challenges. This means being mindful of issues that affect their quality of life, which includes understanding common senior health challenges like hearing loss.
The goal is to create a supportive environment that not only addresses medical needs but also enhances a senior's overall quality of life, allowing them to live as fully and independently as possible.
With over 74 years of mission-driven service, Central Coast VNA & Hospice is a trusted partner for families. Our focus has always been on delivering compassionate, expert care that honors your loved one's wishes.
Exploring The Types Of In Home Care Services
Thinking about in home care for seniors can feel overwhelming. Understanding the different kinds of support is the first step. It is a range of services that can adapt as your loved one's needs evolve.
This flexible approach is what we call the continuum of care. At Central Coast VNA & Hospice, this philosophy is central to our work. It means we can create a seamless care journey, transitioning between levels of support without stress.
Skilled Medical Care At Home
When people hear "home care," they often think of help with daily chores. However, a huge part of in-home services involves skilled medical care. These are specific services ordered by a doctor to help a patient manage a health condition or recover from surgery.
Some of the key skilled services include:
- Skilled Nursing Care: Provided by a Registered Nurse (RN), this involves complex medical tasks like wound care, IV therapy, and managing medications.
- Physical Therapy: Therapists come to the home to help patients restore strength and mobility after an illness or injury.
- Occupational Therapy: This therapy helps someone regain the ability to perform daily activities like dressing, bathing, and cooking.
- Hospice Aide Support: Working under an RN's supervision, a Hospice Aide provides personal care, like bathing and dressing, to ensure patient comfort.

This image shows what high-quality in-home care is about. It’s more than medical procedures; it's about human connection and emotional support. This truly improves a senior’s quality of life.
Distinguishing Between Home Health, Palliative, And Hospice Care
These services all happen at home, but they have different goals. Getting these distinctions right is critical when making decisions. You can read more about the top reasons seniors prefer home health care in our other guide.
Let's compare the three core services we provide at Central Coast VNA & Hospice.
| Comparing In Home Care Options | |||
|---|---|---|---|
| Service Type | Primary Goal | Who It's For | Common Services Provided |
| Home Health | Recovery and rehabilitation from an illness, injury, or surgery. | Patients needing short-term, skilled medical care to regain independence. | Skilled nursing, physical therapy, occupational therapy, wound care. |
| Palliative Care | Pain and symptom management to improve quality of life. | Patients at any stage of a serious illness who need relief from symptoms. | Symptom control, emotional and spiritual support, care coordination. |
| Hospice Care | Comfort and dignity for someone with a terminal illness. | Patients with a life-limiting prognosis (typically 6 months or less). | Pain management, nursing care, emotional support for patient and family. |
Because our teams work together, patients can move smoothly between home health, palliative, or hospice care as their needs change. This integrated system is a major benefit of choosing a local, nonprofit provider with deep community roots.
The Real Benefits Of Choosing Care At Home
Many families in Monterey and Santa Cruz County choose in home care for seniors for its emotional stability. The comfort of familiar surroundings nurtures well-being.

Being in a home filled with memories can lift spirits in ways a clinical setting cannot. Maintaining daily routines reinforces a positive mindset. It helps preserve a sense of normalcy.
Personalized One-On-One Attention
When a Registered Nurse or Hospice Aide visits, your loved one receives undivided attention. Unlike busy facilities, at-home care means every minute is devoted to one person’s needs.
This focus allows for quick adjustments, whether it’s changing medications or just listening. For over 74 years, Central Coast VNA & Hospice has built its nonprofit model around these trusting relationships.
Promoting Safety And Faster Recovery
Imagine a skilled nurse managing wound care and medications in your own home. This hands-on support speeds healing. It also cuts down on the risk of returning to the hospital.
Understanding how to keep seniors independent makes all the difference. You can find valuable information about in-home support to avoid a nursing home on our blog.
Receiving care at home is about more than just medical treatment; it’s about healing in an environment that feels safe, comfortable, and supportive, which can significantly accelerate the recovery process.
Greater Convenience And Accessibility
The most direct benefit is that care comes to your doorstep. This means no stressful trips to the clinic. This is vital for seniors with limited mobility.
Services we coordinate include:
- Physician and Nurse Practitioner house calls
- Mobile lab services for blood draws
- Specialized appointments, such as home visits for eye tests
Throughout Monterey, San Benito, Santa Cruz, and South Santa Clara counties, Central Coast VNA & Hospice synchronizes these offerings. Our mission is to bring expert healthcare directly to the people we serve.
Figuring Out Who Qualifies for In Home Care

Understanding the rules for in home care for seniors can feel complex. The good news is that the qualifications are quite straightforward. Each type of care—home health, palliative, and hospice—has its own specific criteria.
The universal starting point for any skilled in-home medical care is a physician's order. A doctor must certify that the patient needs specific services. This step confirms that every service is medically necessary.
Qualifying for Skilled Home Health Care
Skilled home health care is about recovery and rehabilitation. To qualify for services covered by Medicare, a patient must meet key requirements.
The main criteria are:
- Needing Intermittent Skilled Services: The patient requires part-time care from a Registered Nurse or therapist for things like wound care or physical therapy.
- Being Homebound: This is a crucial Medicare requirement. It means leaving home takes considerable and taxing effort.
Here at Central Coast VNA & Hospice, we work closely with families and doctors across Monterey County and San Benito County to confirm eligibility.
Understanding Palliative and Hospice Care Eligibility
The rules for palliative and hospice care are different. They focus on the nature of the illness itself. These services bring comfort to patients with serious health conditions.
The core qualification for palliative or hospice care is a diagnosis of a serious, life-limiting, or terminal illness. The focus shifts from short-term recovery to long-term quality of life and comfort.
Palliative care can start at any point during a serious illness. Hospice care is for patients with a prognosis of six months or less who have stopped seeking curative treatments.
Seniors are the main recipients of this kind of compassionate support. Approximately 86% of home health care patients are aged 65 or older (CDC, 2021). Many manage chronic conditions that make them ideal candidates for in-home medical care.
Navigating Costs and Insurance for Home Care
The financial side of healthcare can be a huge source of stress. When you look into in home care for seniors, questions about cost are often top of mind. We are here to give you clear answers.
The good news is that for many families on the Central Coast, skilled medical care at home has little to no out-of-pocket cost. Major insurance plans, including Medicare and Medi-Cal, often cover the full cost. Our team at Central Coast VNA & Hospice will work with your insurance provider to handle the details.
Understanding Coverage for Different Services
It helps to know how insurance plans cover our main services. While every plan is different, some general guidelines apply.
- Medicare Coverage: Medicare Part A and Part B typically cover 100% of costs for skilled home health care if a doctor certifies the patient as homebound. Medicare also covers nearly every aspect of hospice care.
- Medi-Cal and Private Insurance: Medi-Cal and most private insurance plans also provide strong coverage for these services. Our team can quickly verify your benefits.
For more details on the care these plans include, please review the information on our home health care services make a difference. We believe financial concerns should never block exceptional care.
The Cost-Effectiveness of In Home Care
Receiving care at home is often a smart financial decision. When your loved one stays at home, you avoid the high costs of room and board in a nursing home. These expenses can add up quickly.
Choosing in-home care isn't just about comfort; it's also a practical financial choice. By receiving skilled care at home, families can often avoid the significant expense of institutional settings while ensuring their loved one gets personalized, one-on-one attention.
As a nonprofit organization serving Monterey County, San Benito County, Santa Cruz County, and South Santa Clara County for over 74 years, our mission is clear. We provide compassionate, high-quality care to everyone in our community, regardless of their ability to pay.
How to Find the Right In Home Care Provider
Choosing an in home care for seniors provider is a big decision. You are inviting a partner into your home. It is critical to find an agency with a proven history of compassionate, expert care.
Start with the essential qualifications. Any reputable agency must be licensed by the state and certified by Medicare. This is proof that a provider meets high standards for patient safety and quality of care.
Key Questions to Ask Potential Providers
Once you confirm credentials, it's time to dig deeper. The goal is to understand their approach to care and the expertise of their staff. A transparent provider will welcome these questions.
Here’s a checklist to guide your conversations:
- What is your history in our community? Look for an agency with deep local roots. Central Coast VNA & Hospice has served families in Monterey, San Benito, and Santa Cruz counties for over 74 years.
- How do you screen and train your clinical staff? Ensure every staff member, from Registered Nurses to Hospice Aides, is licensed and receives ongoing training.
- How do you create a patient's plan of care? A strong provider will build a personalized plan with the patient, family, and doctor.
- How do you communicate with families? You should expect clear, consistent communication from a designated point of contact.
- What happens if our loved one's needs change? Choose a provider that offers a full range of services for a smooth transition between home health, palliative, and hospice care.
Choosing a nonprofit provider like Central Coast VNA & Hospice ensures that the primary focus is always on the patient's well-being, not on profit margins. Our mission-driven approach prioritizes compassionate, high-quality care for everyone in our community.
Making an informed decision brings peace of mind. By asking these critical questions, you can find an agency that aligns with your family’s values.
Frequently Asked Questions About In-Home Senior Care
1. What is the difference between home health care and personal care?
Home health care is skilled medical care prescribed by a doctor, like wound care from a Registered Nurse. Personal care is non-medical help with daily tasks like bathing or meal prep. Central Coast VNA & Hospice specializes in providing skilled medical home health, palliative, and hospice care.
2. How quickly can in-home care services begin?
Once we receive a referral from your doctor, we move quickly. A Registered Nurse can typically conduct the first in-home assessment visit within 24 to 48 hours to create a personalized care plan.
3. Does my loved one need to be homebound for all services?
The "homebound" rule is a specific Medicare requirement only for skilled home health care. This rule does not apply to our palliative or hospice care services.
4. Can our family be involved in the plan of care?
Absolutely. We see families as our partners in care. The Central Coast VNA & Hospice team works closely with both the patient and family to build a plan of care that reflects everyone’s goals and wishes.
5. What happens if my loved one’s needs change?
Our clinical team constantly reassesses your loved one's condition. If their needs change, we can seamlessly adjust their care plan, such as transitioning from home health to palliative care, with a team you already trust.
Are you ready to learn more about how Central Coast VNA & Hospice can support your family with compassionate, expert in-home care? Contact us today to discuss your loved one's needs.
Learn more about our services at ccvna.com
Palliative Home Care Services on the Central Coast
Palliative home care is a special kind of medical support. It focuses on relieving the symptoms, pain, and stress of a serious illness right in your own home. It is not about giving up on treatment.
Think of it as an extra layer of support. Its goal is to improve the quality of life for both the patient and their family.
What Palliative Home Care Really Means
When you or a loved one has a serious illness, medical appointments can be overwhelming. Palliative care works alongside curative treatments to focus on your comfort. It answers the question, "How can we make today better?"
Imagine your doctors are working hard to fix the engine of a car. Palliative home care adds a "comfort crew." This crew improves the ride by making the journey as peaceful as possible.
This support comes from a team of experts. Central Coast VNA & Hospice, a trusted nonprofit with over 74 years of service, brings this compassionate care to you.
An Extra Layer of Support at Home
Many people think palliative care is the same as hospice. In reality, it can begin at any stage of a serious illness and last for years. It helps you manage symptoms so you can live more fully.
Palliative care helps people gain the strength to carry on with daily life. It improves their ability to tolerate medical treatments and helps them better understand their choices for care.
This means you can continue treatments like chemotherapy while getting expert help for pain or fatigue. The goal is to enhance your comfort and empower you. For a closer look, explore our guide to improving quality of life at home with palliative care.
Palliative Care at a Glance
This table breaks down what our palliative home care team does for you.
| Core Principle | What It Means for You and Your Family |
|---|---|
| Symptom Management | We work to relieve pain, shortness of breath, fatigue, nausea, and other symptoms. |
| Emotional & Spiritual Support | We address the emotional, social, and spiritual needs that come with a serious illness. |
| Coordinated Care | Our team talks with all your doctors to ensure everyone is on the same page. |
| Family-Centered Approach | We support the entire family, providing guidance and resources for your journey together. |
| Focus on Quality of Life | Our goal is to help you live as well as possible, for as long as possible. |
Palliative care is about adding life to your days, not just days to your life.
Your Local, Mission-Driven Provider
As a nonprofit, Central Coast VNA & Hospice is driven by our mission to serve the community. We are deeply rooted in the Central Coast and provide care across:
- Monterey County
- San Benito County
- Santa Cruz County
- South Santa Clara County
Our focus is to deliver caring support that respects your values. We bring comfort, dignity, and peace to every family we serve in the place you feel most comfortable—your home.
Who Benefits From Palliative Care at Home?

Palliative care at home helps people of any age living with a serious illness. Many think it is only for certain situations, but that is not the case.
Eligibility is based on a simple need: better symptom management and quality of life. This support helps people feel more in control of their health at home.
Real-Life Scenarios Where Palliative Care Makes a Difference
Let's look at real-life situations instead of medical terms. Palliative care makes each day more manageable when an illness takes over.
Think of a Monterey County resident getting chemotherapy. Their cancer team fights the disease, while our palliative team visits them at home. We help manage side effects like nausea, allowing them to rest and keep up their strength.
Or, imagine someone in San Benito County with heart failure. They might struggle with shortness of breath. Our Registered Nurses can help manage that symptom, helping them stay active at home.
Common Challenges We Help You Overcome
Palliative care is more than just pain management. Our teams are experts at supporting you through many physical and emotional symptoms.
Here are a few challenges we help people manage:
- Chronic Pain: We work with your doctor to find the right therapies to keep you comfortable.
- Shortness of Breath: We teach breathing techniques to help you feel less anxious.
- Constant Fatigue: We help find the cause of your fatigue and plan how to save energy for what matters.
- Emotional Distress: Our Medical Social Workers and Chaplains offer emotional and spiritual support.
By addressing these issues, we help reduce stressful emergency room visits. You can learn more by exploring our home health and hospice services.
Who Is Eligible for This Support?
Eligibility for palliative care is based on need, not life expectancy. If symptoms from a serious illness impact your daily life, you may be a candidate for our services.
Palliative care is appropriate at any age and at any stage in a serious illness and can be provided along with curative treatment. This specialized support focuses on providing relief from the symptoms and stress of the illness.
You can continue treatments meant to cure your illness while receiving this extra support. Central Coast VNA & Hospice serves individuals across Monterey, San Benito, Santa Cruz, and South Santa Clara Counties with conditions like:
- Cancer
- Heart Disease (like Congestive Heart Failure)
- Kidney or Liver Disease
- Lung Disease (like COPD)
- Neurological Conditions (like ALS or Parkinson's)
This is not a complete list. If you are struggling with any serious illness, our team is here to help you live more comfortably.
Meet Your Compassionate Palliative Care Team

When you start palliative home care, you are not alone. At Central Coast VNA & Hospice, our team of professionals works alongside you and your family.
This team model is the heart of effective palliative care. It ensures every part of your well-being is supported with expertise and compassion. As a local nonprofit, our mission is to bring this complete support to your home.
Your Core Support System
Your care team is a group of specialists who bring unique skills to your care. They work closely with each other and with your own doctor. This ensures your care is coordinated.
Here are the key members of your CCVNA palliative care team:
- Registered Nurse (RN): Your RN is a specialist in managing complex symptoms like pain and fatigue. They are your main clinical contact and provide expert medical care.
- Medical Social Worker (MSW): An MSW is a master of resources. They can connect you to community support, help with advance care planning, and offer counseling.
- Chaplain: Spiritual comfort is a vital part of well-being. Our Chaplains provide a supportive presence, helping you explore feelings of fear, hope, and meaning.
How Your Team Works Together for You
Your care plan is a roadmap to make your journey as comfortable as possible. Each team member helps create that map. They hold regular meetings to talk about your progress and adjust the plan as your needs change.
For example, your Registered Nurse may notice a symptom is causing you anxiety. They will coordinate with the Medical Social Worker for emotional support. The Chaplain can also provide spiritual comfort to ease your mind.
This constant communication means nothing gets missed. It is a proactive way to provide care that helps prevent small issues from becoming big problems.
Your palliative care team acts as a single, unified support system. We partner with your existing doctors to add another layer of expert care, ensuring everyone is working toward the same goal—your comfort and quality of life.
Seamless Coordination with Your Doctor
Families often ask how a new care team will work with their primary doctor. At Central Coast VNA & Hospice, we see ourselves as partners in your care.
Our team keeps an open line of communication with your doctor. We give them regular updates and work together on your care plan. This ensures our palliative home care services complement your other treatments.
As a nonprofit with 74+ years of local service in Monterey, San Benito, Santa Cruz, and South Santa Clara counties, our only goal is your well-being.
How Palliative Care Improves Quality of Life

Improving quality of life is the main goal of palliative care. But what does that mean for you? It is about restoring comfort, dignity, and control while you navigate health challenges.
This focus on well-being makes a real difference. A specialized team comes to your home to ease your burdens and help you find more good days.
As a nonprofit serving the Central Coast for over 74 years, Central Coast VNA & Hospice is built on this patient-first philosophy. Our goal is to provide care that prioritizes your comfort.
Expert Pain and Symptom Management
Palliative care offers expert management of difficult symptoms. Chronic pain, nausea, or fatigue can make it hard to enjoy simple moments.
Our Registered Nurses are specialists in symptom control. They work with you and your doctor to find the right therapies to bring you relief at home. This often reduces the need for stressful emergency room visits.
Easing Emotional and Spiritual Distress
A serious illness affects more than just the body. It can bring a heavy emotional weight for patients and families.
Our team includes Medical Social Workers and Chaplains who provide a safe space to navigate these emotions.
- Medical Social Workers offer counseling and connect you with community resources.
- Chaplains provide non-denominational spiritual support to help you find peace.
This holistic support ensures your mental well-being is given the same attention as your physical health. Find more details on the benefits of palliative care to improve quality of life today.
Coordinated Care Reduces Confusion and Stress
Juggling multiple doctors and appointments can be confusing. Our palliative team acts as your central point of contact. This ensures everyone involved in your care is on the same page.
We maintain open communication with your primary doctor and specialists. This coordination means less stress for you and your family. It ensures your care plan is seamless and aligned with your goals.
The core of our service is to bring clarity and calm to a challenging time. By coordinating every aspect of your care, we reduce the burden on your family, allowing you to focus on what truly matters—spending quality time together.
To learn more about how efficient processes improve care, discover how workflow automation in healthcare can lead to better patient outcomes.
Supporting and Empowering Families
A serious illness impacts the entire family. Loved ones often take on new, stressful roles. Our team is here to support them, too.
We provide education to help family members understand the illness. We also offer guidance on making difficult decisions together. By empowering the whole family, we help strengthen your ability to face challenges.
This commitment to families is the foundation of our nonprofit mission in Monterey, San Benito, Santa Cruz, and South Santa Clara counties.
Understanding the Path From Palliative to Hospice Care
Families are often confused about the difference between palliative and hospice care. They are related but serve different needs at different times.
Getting this distinction right is important. It ensures your loved one gets the right support at the right time.
Think of it this way: all hospice care is palliative, but not all palliative care is hospice. Both focus on comfort and quality of life. The main difference is when they are used. At Central Coast VNA & Hospice, we see them as part of our continuum of care.
The Bridge Between Palliative Support and Hospice
Palliative home care can start with a serious diagnosis and may continue for years. It works alongside curative treatments to help manage symptoms and maintain strength.
Hospice care is for the final chapter of life. It begins when the focus shifts from curing an illness to maximizing comfort. This usually happens when a doctor believes a patient has six months or less to live.
This infographic breaks down how these services are often funded.
Private insurance covers much of the care, but government programs like Medicare and Medicaid also play a large role.
When Is the Right Time to Consider Hospice?
Moving to hospice is a personal choice made with your family and doctor. It is not about giving up. It is about redefining hope toward comfort and meaningful time with loved ones.
How do you know it might be time? Here are a few signs:
- Repeated hospital stays or trips to the emergency room.
- A decline in the ability to handle daily activities.
- Pain or other symptoms become harder to manage.
- The patient wants to stop curative treatments and focus on comfort.
This transition can feel overwhelming. Our team at Central Coast VNA & Hospice provides compassionate guidance. To learn more, see our guide on when to call hospice.
Hospice is not about waiting to die; it is about living every remaining moment to the fullest. The focus is on ensuring the patient is comfortable and supported, surrounded by family and compassion.
According to the National Hospice and Palliative Care Organization (NHPCO), over 1.72 million Medicare beneficiaries received hospice services in 2020 (NHPCO, 2021).
A Seamless Continuum of Care
At Central Coast VNA & Hospice, we are the only provider on the Central Coast offering the full spectrum of care, from home health to hospice. This allows for a smooth transition as your needs change.
If you already receive palliative care from us, the same trusted team can help you move to hospice. You keep the relationships you have built with a local, nonprofit team that knows you.
Our mission across Monterey, San Benito, Santa Cruz, and South Santa Clara counties is to ensure your journey is met with expert care every step of the way.
How to Get Started With Palliative Home Care
Taking the first step toward palliative home care is empowering. It can feel like a big decision, but the process is simpler than you might think. Anyone involved—you, a family member, or your doctor—can start the conversation.
At Central Coast VNA & Hospice, we make getting support as easy as possible. We are here to listen and answer your questions.
A Simple Path to Comfort
Getting started involves a few easy steps. It is about making sure your care is coordinated and personalized.
- Talk to Your Doctor: The best place to begin is by speaking with your physician. Ask if a referral for palliative home care services is a good fit.
- Contact Us Directly: You can also call Central Coast VNA & Hospice directly. We offer a compassionate consultation to help you understand how our services can help.
- Coordinated Assessment: Our team will work with your physician to get a complete picture of your needs. We will create a personalized care plan to improve your daily life at home.
For families exploring different supports, our guide on how do you know when hospice is needed can also be helpful.
Getting help should never be complicated. Our team is here to guide you through the process, ensuring a smooth and stress-free start to receiving the comfort and support you deserve.
The good news is that in-home care is becoming more accessible. You can read more about upcoming shifts in home care accessibility.
If you live in Monterey County, San Benito County, Santa Cruz County, or South Santa Clara County, contact Central Coast VNA & Hospice today to learn more.
Frequently Asked Questions About Palliative Home Care
It’s natural to have questions when considering palliative home care. Getting clear answers is the first step toward peace of mind. Here are some of the most common questions we hear.
1. What is the main goal of palliative care?
The main goal is to improve quality of life for both the patient and their family. It focuses on providing relief from the symptoms, pain, and stress of a serious illness. This care is provided alongside any curative treatments you may be receiving.
2. Is palliative care the same as hospice?
No, they are different. Palliative care can begin at any stage of a serious illness and can be provided with curative treatments. Hospice care is for the last six months of life when curative treatments are no longer being pursued.
3. Who is on a palliative care team?
A typical team at Central Coast VNA & Hospice includes a Registered Nurse for symptom management, a Medical Social Worker for emotional and practical support, and a Chaplain for spiritual comfort. This team works closely with your own doctor.
4. Who pays for palliative care?
Most insurance plans, including Medicare Part B and Medicaid, cover palliative care. As a nonprofit, Central Coast VNA & Hospice is committed to helping you understand your coverage. Our team will review your specific plan with you.
5. How can I start palliative home care services?
You can start by talking to your doctor and asking for a referral. You can also contact Central Coast VNA & Hospice directly. We can speak with you and your family to see if our services are the right fit.
If you have more questions or feel that palliative care might be right for you or a loved one, please reach out. The team at Central Coast VNA & Hospice is here to offer compassionate guidance.
You can learn more by contacting us today at https://ccvna.com.










