When a patient goes home from the hospital, the real work of recovery begins. Preventing a return trip hinges on providing solid, coordinated care that supports them after discharge.
A seamless transition from hospital to home, guided by skilled professionals from Central Coast VNA & Hospice, is the most effective way to ensure recovery is safe and lasting. It’s all about addressing common post-discharge challenges before they become major problems.
Why Hospital Readmissions Happen and How to Prevent Them

For patients and their families, returning to the hospital shortly after coming home is incredibly frustrating and disruptive. These readmissions are often preventable and usually signal a breakdown in the continuity of care.
The first step to building a better path to recovery is understanding why they happen in the first place. Many readmissions are the result of gaps that appear once a patient is back home, feeling overwhelmed without professional support.
Common Causes of Hospital Readmissions
The shift from the structured, 24/7 environment of a hospital to the independence of home can be jarring. Patients suddenly face new medication routines, may not fully grasp their condition, or end up missing crucial follow-up appointments.
Some of the key factors we see contributing to readmissions include:
- Medication Confusion: Juggling multiple new prescriptions is tough. It’s easy to get confused about dosages, timing, and potential side effects.
- Lack of Follow-Up: Patients often fail to schedule or attend necessary appointments with their primary doctor or a specialist after they get home.
- Unrecognized Symptoms: Many people simply don't know which warning signs or "red flag" symptoms require immediate medical attention and which ones can wait.
- Inadequate Support at Home: Recovery can be derailed by a simple lack of help with daily activities, preparing meals, or personal care.
One of the biggest, and most frequently overlooked, factors is a patient's confidence. When individuals and their families feel unprepared to manage care on their own, anxiety shoots up. Small issues can quickly escalate, often leading to an unnecessary trip back to the emergency room.
The Role of a Coordinated Care Continuum
The best strategy for preventing hospital readmissions is creating a coordinated continuum of care that bridges the gap between the hospital and the home. This is where Central Coast VNA & Hospice excels, offering expert support across Monterey County, San Benito County, Santa Cruz County, and South Santa Clara County.
As a trusted nonprofit with over 74 years of service, we ensure patients get the right care at exactly the right time. Our compassionate, mission-driven approach weaves together several crucial services.
- Home Health Care: Our team of Registered Nurses and therapists brings skilled medical care right into the patient’s home. They perform safety assessments, reconcile medications to avoid dangerous errors, and provide hands-on education to ensure a stable recovery.
- Palliative Care: For patients managing serious or chronic illnesses, our palliative care at home focuses on managing symptoms and improving quality of life. This proactive approach helps prevent the kind of crises that frequently lead to re-hospitalization.
By creating a smooth transition and offering expert guidance, we empower both patients and their families. This compassionate, in-home support ensures that recovery continues safely and effectively, keeping our community members healthy and where they want to be—out of the hospital.
Contact us today to learn how our services can help you or a loved one.
Building A Strong Foundation Before Hospital Discharge
A successful recovery doesn’t start when a patient walks out the hospital doors. It begins long before that. The most effective strategies for preventing hospital readmissions are proactive, built on a strong foundation of thoughtful pre-discharge planning.
This is where hospital staff and home health agencies like Central Coast VNA & Hospice collaborate to set the stage for a safe, smooth transition home. This isn’t just about checking boxes; it’s a dynamic, hands-on process involving real conversations and clear communication.
Proactive Assessments And Personalized Care Plans
At Central Coast VNA & Hospice, our work often starts right inside the hospital. Our Registered Nurses conduct thorough pre-discharge assessments to get the full picture—not just the medical diagnosis, but the entire home environment and any potential roadblocks to healing.
We look closely at a few key areas:
- Medication Complexity: We review all prescriptions to spot potential conflicts, confusing schedules, or cost issues that might tempt someone to skip a dose.
- Mobility and Safety: We get a real sense of the patient’s physical abilities and scout for fall risks or other hazards in the home that need immediate attention.
- Support System: We talk with family members to understand what they can handle and give them the training they need to feel confident, not overwhelmed.
- Symptom Management: We create a clear, easy-to-follow plan for managing symptoms to stop a crisis before it starts. You can learn more about the benefits of palliative care for managing long-term illnesses.
From this deep dive, a truly personalized care plan is born. Think of it as a roadmap for those first critical days and weeks at home, outlining specific actions, goals, and "red flag" symptoms.
Key Focus Areas for Pre-Discharge Planning
| Focus Area | Objective | CCVNA Professional Involved |
|---|---|---|
| Medication Reconciliation | Ensure patient understands new medication schedule, purpose, and side effects. Address any cost or access concerns. | Registered Nurse (RN) |
| Home Safety Evaluation | Identify and mitigate fall risks and other hazards. Recommend necessary modifications or equipment. | Physical/Occupational Therapist, RN |
| Patient & Family Education | Empower the patient and family members with knowledge on symptom management, diet, and when to seek help. | RN, Dietitian, Medical Social Worker |
| Follow-up Coordination | Schedule the first home health visit and necessary physician appointments before the patient leaves the hospital. | RN, Care Coordinator |
| Emotional & Social Support | Assess the patient’s support system and connect them with community resources or counseling if needed. | Medical Social Worker (MSW) |
This structured approach ensures that our plan is not just comprehensive but also practical, addressing the real-world challenges patients face when they return home.
Real-World Scenarios In Pre-Discharge Planning
Let’s put this into practice. Imagine a patient in Monterey County recovering from heart surgery. Before they’re discharged, a CCVNA Registered Nurse meets with them and the hospital team. The nurse learns the patient lives alone in a two-story house and has five new medications to manage.
A proactive plan means addressing risks before they become emergencies. By identifying challenges early, we empower patients with the tools and support needed for a confident recovery journey.
Recognizing the high risk for both a fall and medication mix-ups, the nurse builds specific solutions right into the care plan. A Physical Therapist is scheduled for the very first day home to teach the patient how to safely navigate their stairs. The nurse also creates a simplified, large-print medication chart.
This infographic breaks down the core steps we follow to create a safe and effective plan for when a patient goes home.
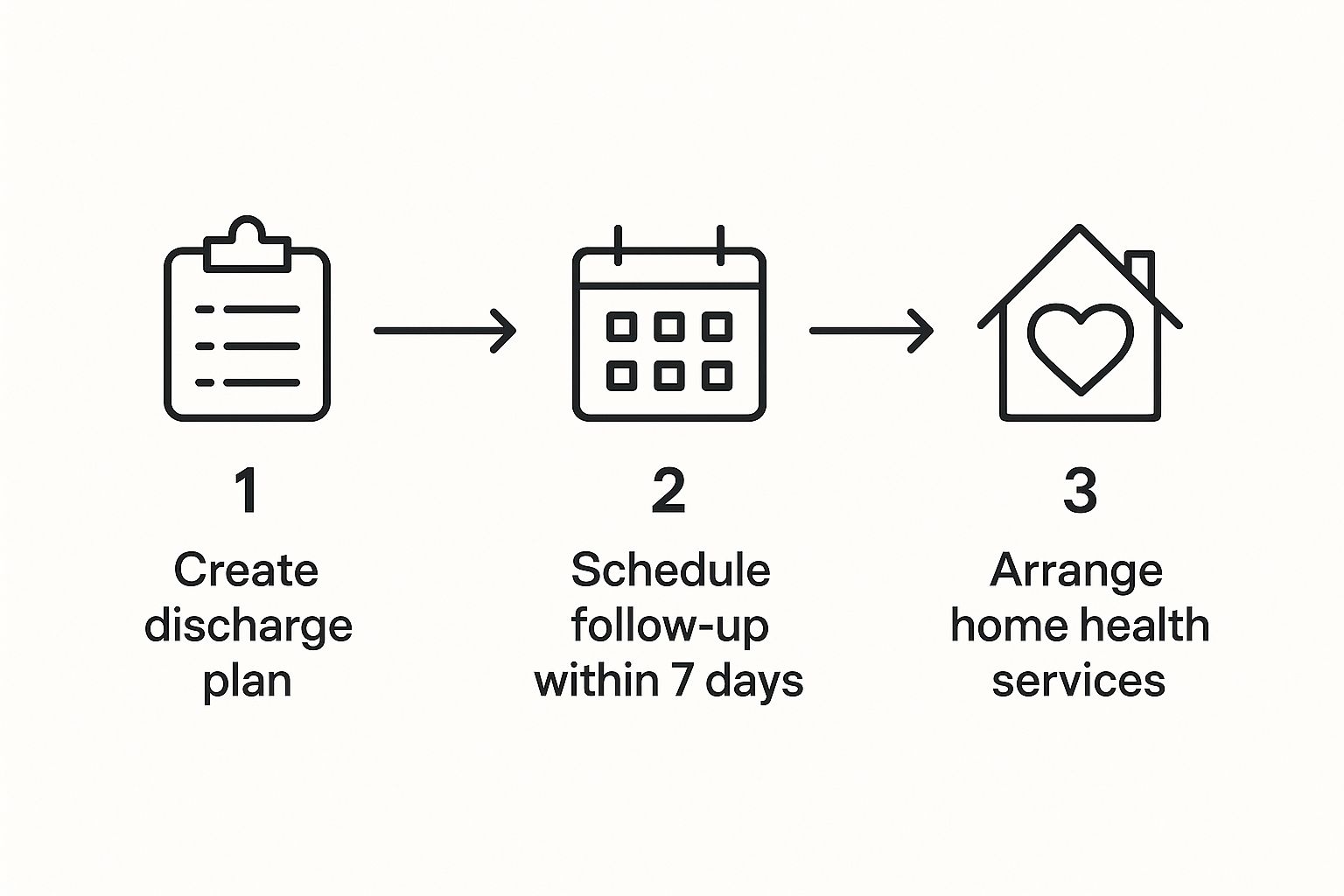
As you can see, a solid discharge plan, quick follow-ups, and professional home health services are all connected. When we address each piece systematically, the risk of readmission drops significantly.
This early, coordinated effort provides incredible peace of mind. Patients and their families in our service areas—Monterey, San Benito, Santa Cruz, and South Santa Clara counties—leave with a dedicated partner and a clear, actionable plan.
How Patient and Family Education Empowers Recovery

When it comes to preventing hospital readmissions, knowledge is one of the most powerful tools we have. But real patient education isn’t about handing someone a stack of pamphlets.
It's about building confidence and turning anxious loved ones into capable partners in the healing journey. A patient who understands their condition and care plan is far more likely to have a smooth recovery.
Moving Beyond Instructions to Real Understanding
Just telling a patient what to do is never enough. Our Registered Nurses are trained to make sure both patients and their families understand the why behind every instruction.
One of the most effective tools we use is the “teach-back” method. After a nurse explains a medication schedule, they'll ask the patient or family member to explain it back in their own words. This isn't a quiz; it's a conversation that immediately shows us if there are any gaps in understanding.
This method helps confirm everyone is on the same page about crucial details, such as:
- The purpose of each medication and what side effects to look out for.
- How to properly care for a wound to prevent infection.
- What dietary or activity changes are essential for recovery.
Spotting Early Warning Signs
One of the biggest reasons patients end up back in the hospital is because a small, manageable issue isn't caught in time. A minor symptom can quickly escalate into a crisis if it's ignored.
That’s why a huge part of our education process is teaching families exactly what to watch for. This proactive approach is a cornerstone of how our team—with over 74+ years of local experience—helps keep our community safe and comfortable at home.
Empowering patients and families to identify warning signs isn't about creating alarm. It's about providing a clear, calm plan of action that replaces uncertainty with confidence, ensuring they know exactly when and how to seek help.
For instance, with a patient recovering from heart failure, our nurse will create a personalized list of "red flag" symptoms. This isn’t vague advice. It’s concrete, measurable guidance like, "Call us if you gain more than three pounds in one day," or "Contact your doctor if you feel short of breath and resting doesn't help."
Building Confidence and Setting Realistic Expectations
Recovery is a journey, not a destination. A critical part of education is setting realistic expectations for the healing process.
Our team, which includes Physical and Occupational Therapists and Medical Social Workers, helps patients and families understand the typical recovery timeline. We also focus on the emotional side of recovery.
Having open conversations about care preferences and future health decisions is vital. For a closer look at this important topic, you can explore our resources on how advance care planning is made simple. This complete approach ensures that families feel prepared not just for the medical tasks, but for the emotional journey, too.
Contact Central Coast VNA & Hospice today to learn more about how our home health and palliative care services can support your family.
Making the Transition to Home Health Care Seamless
The first 48 hours after a patient leaves the hospital are incredibly high-stakes. This is the window where a recovery can either take root or start to unravel, making it the most critical time for preventing hospital readmissions.
A smooth, professionally managed transition from the hospital back to home life acts as a crucial safety net. It’s all about catching potential problems before they escalate into full-blown emergencies.
At Central Coast VNA & Hospice, our home health care services are built to bridge this exact gap. We provide immediate, in-home support to make sure care continues safely and without interruption.
The Critical First Visit Home
The moment a patient gets home, our team is ready to go. A Central Coast VNA & Hospice Registered Nurse (RN) almost always makes the first visit, usually within 24 to 48 hours of discharge.
This isn't just a quick check-in. It’s a comprehensive clinical assessment designed to establish stability and map out a clear path forward.
During this vital first meeting, our RN zeroes in on a few key actions:
- Confirming the Medication Plan: The nurse meticulously reviews all hospital paperwork and compares it with the medications the patient has at home. They check for discrepancies and explain what each prescription is for.
- Performing a Hands-On Assessment: The nurse conducts a thorough physical assessment. This means checking vital signs, looking at how wounds are healing, and gauging pain levels to establish a baseline.
- Evaluating the Home Environment: Is the lighting dim? Are there loose rugs waiting to cause a fall? The nurse scans the home for these kinds of safety risks and gives immediate, practical advice to fix them.
This first visit builds a foundation of trust and safety. It’s our way of letting patients and their families know they aren't going through this alone.
Tailoring a Comprehensive Care Team
Every person's recovery is different, so a one-size-fits-all approach doesn't work. Based on that initial assessment, the RN works with the patient’s doctor to put together a personalized care team.
This team brings a whole range of expertise right into the home, focusing on exactly what the patient needs.
A tailored care team does more than just treat symptoms; it addresses the whole person. By integrating skilled nursing, therapy, and personal support, we build a robust circle of care that promotes physical healing and emotional well-being.
The professionals who might join a patient’s support system include:
- Registered Nurses to handle complex medical needs, from wound care to IV therapy.
- Physical and Occupational Therapists to help regain strength, mobility, and independence with daily tasks.
- Speech Therapists to help with swallowing or communication issues after a stroke or other illness.
- Medical Social Workers to connect families with helpful community resources and offer emotional support.
- Hospice Aides to give essential, dignified help with personal care like bathing and dressing.
This kind of teamwork makes sure every angle of the patient's recovery is covered. You can explore our full range of home health care services to see how we support patients across Monterey County, San Benito County, Santa Cruz County, and South Santa Clara County.
Managing Chronic Illness with Palliative Care at Home

When someone is living with a serious or chronic illness—like heart failure, COPD, or cancer—the focus shifts. It’s no longer just about recovering from a single hospital stay, but about preventing the next one.
Managing these long-term conditions at home demands a proactive strategy that puts comfort and quality of life first. This is where palliative care at home provides a powerful layer of support.
Palliative care, a core service at Central Coast VNA & Hospice, is specialized medical support that can begin at any stage of a serious illness. It is not the same as hospice and can be received alongside curative treatments.
A Team-Based Approach to Comfort and Quality of Life
One of the biggest strengths of palliative care is that it brings an entire interdisciplinary team right to the patient's home. This team works together to care for the "whole person," not just the disease.
At Central Coast VNA & Hospice, this compassionate team includes:
- Registered Nurses who are experts in managing pain and other difficult symptoms.
- Medical Social Workers who offer emotional support and connect families with essential community resources.
- Chaplains who provide spiritual guidance and support that respects the patient's personal beliefs.
- Hospice Aides who help with personal care, preserving both dignity and comfort.
This collaborative approach ensures every part of a patient's well-being is looked after, from physical pain to emotional distress. This level of comprehensive support can stabilize a patient’s condition and significantly reduce the likelihood of another hospital stay.
Proactively Managing Symptoms to Prevent Crises
For patients with chronic illnesses, uncontrolled symptoms are a primary driver of hospital readmissions. A sudden spike in pain or severe shortness of breath can quickly turn into an emergency.
Palliative care is all about getting ahead of these problems before they become unmanageable. This constant, in-home vigilance can prevent the kind of crisis that would otherwise land a patient back in the hospital.
The goal of palliative care is not just to manage illness, but to enhance life. By focusing on comfort, dignity, and personal goals, we empower patients to live more fully, even while facing serious health challenges.
This proactive stance helps patients feel more in control and less anxious. For those navigating their condition, having access to resources like a guide to living with cancer and thriving can offer more strategies for staying well at home.
Navigating Complex Decisions and Providing Emotional Support
Living with a serious illness often involves making tough decisions about treatments and personal care goals. The palliative care team is skilled at facilitating these important conversations, making sure the patient's voice is heard.
This complete support system strengthens a patient's ability to cope, reducing the kind of stress that can worsen physical symptoms. By understanding the different 4 stages of palliative care, families can better see how this support evolves to meet their changing needs.
For families across Monterey, San Benito, Santa Cruz, and South Santa Clara counties, palliative care from CCVNA offers a compassionate path forward. It provides the expert medical and emotional support needed to manage chronic illness effectively at home.
Navigating Healthcare Policies and Measuring Success
Preventing a trip back to the hospital isn't just a clinical goal; it's a national healthcare priority. Federal policies have put a spotlight on patient outcomes, holding entire health systems accountable.
For a mission-driven, nonprofit provider like Central Coast VNA & Hospice, this focus fits perfectly with what we’ve always done. Our commitment to exceptional care strengthens the healthcare ecosystem across Monterey County, San Benito County, Santa Cruz County, and South Santa Clara County.
The Bigger Picture of Readmission Prevention
Policies like the Centers for Medicare & Medicaid Services (CMS) Hospital Readmissions Reduction Program (HRRP) have fundamentally changed how hospitals think about care after discharge. The program uses financial penalties to motivate hospitals to lower preventable readmissions.
This encourages them to build stronger relationships with community-based providers like us. Our skilled teams provide the in-home support that bridges the gap between the hospital and a safe recovery at home.
Preventing a return to the hospital is a shared responsibility. It requires close collaboration between hospitals, physicians, and home health experts to create a safety net that supports patients long after they are discharged.
This national focus is starting to make a difference. According to Advisory Board, an estimated 2,247 hospitals will face readmission penalties in fiscal year 2025 (Advisory Board, 2024). This highlights the ongoing need for effective post-discharge care. You can dig into what these trends mean for providers in a report on readmission penalties.
How We Measure Our Impact
At Central Coast VNA & Hospice, our success is measured one person at a time. Of course, we track data like patient satisfaction and clinical outcomes.
But the real proof is seeing someone regain their independence and avoid the stress of another hospital stay. It’s the foundation of our more than 74 years of service to the Central Coast.
We keep a close eye on our performance to make sure we're living up to the highest standards. This involves:
- Tracking patient progress toward the specific recovery goals they set with their care team.
- Ensuring timely follow-up from our nurses and therapists to catch any issues early.
- Actively listening to feedback from patients and their families so we can keep getting better.
We also believe in helping families prepare for what lies ahead. Proactive conversations and planning are key to preventing future crises. You can learn more by reading our guide on what advance care planning is.
Frequently Asked Questions About Preventing Hospital Readmissions
When a loved one comes home from the hospital, it’s natural to have questions. Here are answers to some of the most common concerns we hear from families in Monterey County and surrounding areas.
1. What is the difference between home health care and palliative care?
Home health care is skilled medical care prescribed by a doctor to help you recover from a specific illness, injury, or surgery at home. Palliative care is an extra layer of support focused on relieving the symptoms and stress of a serious illness and can be received at the same time as curative treatment.
2. How do we arrange for CCVNA services after a hospital stay?
The easiest way is to ask the hospital's discharge planner or social worker for a referral to Central Coast VNA & Hospice. You or your family can also reach out to us directly to discuss your needs and how we can provide support in Monterey, San Benito, Santa Cruz, or South Santa Clara counties.
3. Who will be part of the care team coming to my home?
Your care team is built around your specific recovery needs as ordered by your physician. It may include a Registered Nurse, Physical or Occupational Therapist, Speech Therapist, Medical Social Worker, and a Hospice Aide, all working together to provide coordinated care.
4. Does Medicare cover services to prevent hospital readmissions?
Yes, in most cases. Medicare Part A and/or Part B generally cover home health nursing and therapy services if you meet the eligibility criteria. Palliative care is also often covered by Medicare and many other insurance plans.
5. What are the most important "red flag" symptoms to watch for at home?
While specific to each condition, common red flags include sudden shortness of breath, a fever over 101°F, increased pain that isn't relieved by medication, or signs of confusion. Our team will educate you on the exact symptoms to monitor for your specific situation.
Are you or a loved one in need of support after a hospital stay? Contact Central Coast VNA & Hospice to learn more about our home health, palliative, and hospice services at https://ccvna.com. Our nonprofit organization has proudly served the Central Coast for over 74 years.
