Why Central Coast VNA Is the Best Choice for Home Health Care
When a health challenge arises, finding the right support is key. Expert medical care at home can help you heal and stay independent. On California's Central Coast, families have trusted one partner for this journey for over 74 years.
Central Coast VNA & Hospice (CCVNA) has provided compassionate, high-quality care. It has become a pillar of the community. But what makes a home health agency stand out?
It is a mix of experience, comprehensive services, a dedicated team, and a mission that puts patients first. Knowing how to pay for care is also important. For example, you can explore health insurance options for seniors to help with costs.
This guide will explain why Central Coast VNA is the best choice for home health care on the Central Coast. We will cover services in Monterey, San Benito, Santa Cruz, and South Santa Clara Counties. We'll show you why CCVNA is a leader in home health.
1. Over 74 Years of Trusted In-Home Clinical Excellence
When choosing a home health agency, experience matters. It shows trust, reliability, and expertise. Central Coast VNA & Hospice (CCVNA) has been a cornerstone of community health for over 74 years.
This long history across Monterey, San Benito, Santa Cruz, and South Santa Clara Counties is a key reason why CCVNA is the best choice for home health care. Our deep local roots mean we understand the community's healthcare needs. We have built strong relationships with area hospitals and doctors.
This ensures that care transitions for every patient are smooth. Our mission is to put patients first, providing care guided by compassion, not profit.

A Legacy Built on Local Trust
For generations, families have trusted CCVNA for skilled care at home. This shows our commitment to quality and patient-centered service. Choosing CCVNA means you get the most experienced home health care on the Central Coast.
Our team has grown with the community's needs. This deep connection makes a real difference in patient outcomes.
- A patient leaving a local hospital gets a smooth transition to home health care without delays.
- A family in a rural part of San Benito County gets support from a team that knows the area.
- A doctor confidently refers a patient to CCVNA, knowing our history of high-quality care.
To learn more about CCVNA's history and mission on our website, see how our legacy translates into excellent care today.
2. Comprehensive, Team-Based Home Health Services
Effective home health care involves more than one person. It requires a skilled, multidisciplinary team working together. Central Coast VNA & Hospice provides comprehensive care from a team of clinical experts.
Our teams include Registered Nurses (RNs), Licensed Vocational Nurses (LVNs), and therapists. We also have physical, occupational, and speech-language pathologists. Medical social workers complete the team to support every aspect of your well-being.
This team-based approach is a key reason why Central Coast VNA is the best choice for home health care on the Central Coast. It ensures your care plan is truly holistic.

Individualized Care from Skilled Professionals
Your health needs are unique. That's why we create an individualized care plan just for you. Our team collaborates with you, your family, and your doctor to set goals.
This ensures everyone is working toward the same outcome. It leads to better results and a more positive experience.
- An RN provides skilled nursing for wound care or medication management.
- A physical therapist creates a program to help you regain strength and mobility.
- A medical social worker connects you with community resources to ease stress.
You can explore some of the local health care resources on our website to understand how our community connections benefit you.
3. A Nonprofit Mission That Puts Patients First
In healthcare, the mission behind the care matters. Central Coast VNA & Hospice is a nonprofit organization. This means our primary focus is on patient well-being, not on making a profit.
This mission-driven approach is a core reason why Central Coast VNA is the best choice for home health care on the Central Coast. All our resources are reinvested into providing high-quality, compassionate care. This commitment is supported by generous community donors.
Our nonprofit status ensures that care decisions are guided by your needs. We work to make our services accessible and fair for everyone in our community.

Care Guided by Compassion, Not Profit
Choosing a nonprofit provider means you are choosing a partner dedicated to service. Our goal is to provide the best possible care, regardless of a patient's financial situation. We believe everyone deserves dignity and respect.
Our commitment to the community runs deep. We have been a trusted local resource for over 74 years.
- A patient without full insurance coverage receives help finding financial assistance.
- Care plans are designed to achieve the best health outcomes, not to maximize revenue.
- Community donations help us provide specialized programs and support for all families.
You can learn more about our commitment to quality care on our website, where we detail the high standards that guide our services.
4. Continuity of Care Through Integrated Services
A person's health needs can change over time. It's important to have a provider that can adapt with you. Central Coast VNA & Hospice offers a full continuum of care.
This means we provide a seamless transition between our Home Health, Palliative Care, and Hospice programs. Patients receive the right care at the right time, without disruption. This integrated approach is a major reason why CCVNA is the best choice for home health care.
It prevents gaps in care and ensures your journey is smooth. You can stay with one trusted organization as your needs evolve.

Seamless Transitions for Peace of Mind
Navigating healthcare can be confusing. Our integrated system simplifies the process. If a home health patient's condition progresses, they can easily move to palliative care for extra support.
If end-of-life care is needed, our hospice team is ready to help. All of your medical information and care preferences move with you.
- A home health patient with a serious illness begins palliative care to manage symptoms.
- The same team of clinicians continues to provide care, offering comfort and familiarity.
- The transition is coordinated smoothly, so the patient and family feel supported.
Explore our skilled nursing services at home on ccvna.com to see how our professionals make a difference every day.
5. Technology Integration and Care Coordination
Modern healthcare uses technology to provide safe, high-quality care. Central Coast VNA & Hospice uses electronic health records (EHR) to coordinate care. This ensures clear communication between clinicians, doctors, and patients.
This use of technology is another reason why CCVNA is the best choice for home health care. Our secure EHR system gives the care team instant access to your health history. This helps prevent errors and ensures decisions are well-informed.
We combine compassionate, hands-on care with modern efficiency.
A Modern Approach to In-Home Care
Our technology helps us monitor health and educate patients. This makes care more interactive and responsive. It allows our teams to manage health conditions proactively and prevent hospital visits.
Choosing CCVNA means you get the best of both worlds. You receive personal care supported by accurate, modern technology.
- A patient with a heart condition uses remote devices to send vital signs to their nurse.
- A family member can join a care meeting by video call to stay involved.
- An electronic medication system helps a patient manage their prescriptions safely.
You can contact our team directly to learn more about how our technology enhances patient care.
6. Insurance Acceptance and Financial Accessibility
Healthcare costs can be a concern for many families. Central Coast VNA & Hospice works to make our services financially accessible. We accept a wide range of insurance plans, including Medicare, Medi-Cal, and most private insurance.
This commitment to access is a key reason why CCVNA is the best choice for home health care. It means more families can get the expert care they need without financial stress. Our team helps you understand and use your benefits.
As a nonprofit, our goal is to serve the community. Our commitment to quality includes exploring advancements like the benefits of medical voice charting for accurate records.
- A patient on Medicare gets skilled nursing care fully covered after a hospital stay.
- Our team gets pre-authorization from a private insurer for speech therapy.
- A family receives counseling to find resources to help manage the cost of care.
You can learn more about Medicare eligibility for home care and how our team can help you.
7. Patient-Centered Care Approach and Family Involvement
True healing happens when care is tailored to the individual. Central Coast VNA & Hospice uses a patient-centered approach. We honor each person's unique values, preferences, and goals.
This is a fundamental reason why CCVNA is the best choice for home health care. We actively involve family members in the care process, seeing them as essential partners. This creates a supportive environment for everyone.
A Partnership Built on Respect and Collaboration
At CCVNA, your voice matters most. We believe care plans should be created with you and your loved ones. This ensures our clinical expertise aligns with your personal priorities.
This partnership leads to greater comfort and better health outcomes. We put you at the center of every decision.
- A care plan is designed to respect a patient's cultural or religious preferences.
- Family members receive training from a nurse to help with care at home.
- Visit schedules are flexible to work around a patient's daily routines.
You can explore our patient engagement strategies on our website to learn more about how we foster this collaborative environment.
Your Trusted Partner in Health, at Home
Choosing a home health provider is a big decision. It is about trusting a team to come into your home to care for you or a loved one. The right choice can empower recovery and provide peace of mind.
Throughout this guide, we have shown why CCVNA is the premier provider in our community. From our deep local roots to our patient-first nonprofit mission, we are dedicated to compassionate care. For over 74 years, we have built a legacy of trust.
Key Takeaways: Your Path to Confident Care
Let’s review the core reasons why Central Coast VNA is the best choice for home health care on the Central Coast:
- Over 74 Years of Trust: Our long history in Monterey, San Benito, Santa Cruz, and South Santa Clara Counties means proven clinical excellence.
- A Complete Continuum of Care: We offer seamless transitions between home health, palliative care, and hospice, all from one trusted provider.
- Patient-First, Nonprofit Mission: Our decisions are guided by your needs, not profit, ensuring high-quality, accessible care for all.
- Expert, Multidisciplinary Teams: Your care is managed by a coordinated team of RNs, therapists, and other specialists who create a plan just for you.
Taking the Next Step with Confidence
The journey to better health starts with a simple step. If you or a loved one need skilled support at home, start a conversation with us. You have the right to choose your home health provider.
Talk to your doctor or hospital discharge planner. Tell them you choose Central Coast VNA & Hospice for its proven track record and compassionate approach. You are not just selecting a service; you are choosing a partner who will support you at home.
Ready to experience expert care at home? Discover how the team at VNA and Hospice can support you. Visit VNA and Hospice or call 831-372-6668 to learn more.
Frequently Asked Questions (FAQs)
1. What is home health care?
Home health care is skilled medical care provided in a patient's home. It is ordered by a doctor and includes services like nursing care, physical therapy, and occupational therapy to help patients recover from illness, injury, or surgery.
2. Who is eligible for home health care from Central Coast VNA?
Patients living in Monterey, San Benito, Santa Cruz, or South Santa Clara Counties may be eligible. A doctor must certify that you need skilled care and are "homebound," meaning it is difficult for you to leave home. Our team can help determine your eligibility.
3. How is home health care paid for?
Home health care is often covered by Medicare, Medi-Cal, and most private insurance plans. As a nonprofit, CCVNA is committed to making care accessible and can help you understand your coverage options.
4. What is the difference between home health, palliative care, and hospice?
Home health care focuses on recovery and rehabilitation. Palliative care provides an extra layer of support to manage symptoms of a serious illness at any stage. Hospice care is for patients nearing the end of life, focusing on comfort and quality of life. CCVNA provides all three services.
5. How do I start services with Central Coast VNA & Hospice?
You can start by talking to your doctor, who can make a referral. You can also contact us directly at 831-372-6668 or visit our website to learn more. We will coordinate with your physician to begin services.
A Practical Guide to Recovering From Surgery at Home
Recovering from surgery at home is more than just getting rest. It's about making your space safe and comfortable to help your body heal. This guide covers preparing your home, managing pain, and eating right.
This journey is a big step toward getting back your strength and independence. We are here to help you feel ready.
Your Healing Journey Begins at Home

Coming home after the hospital is a big moment in your recovery. You get to heal in a familiar place, surrounded by your own things. This guide will help you and your family feel more confident.
We will share simple, practical steps for a smooth recovery. From setting up your home to knowing what your body needs, you will find clear advice here. You are not alone on this journey.
Feel Confident in Your Recovery
Our goal is simple: to give you the knowledge you need for a good recovery at home. Moving from the hospital back home can feel like a lot. With the right support, it can be a positive experience.
A well-planned recovery lowers stress and reduces the risk of problems. For more details on this important step, this guide on home care after hospital discharge has great tips.
At Central Coast VNA & Hospice, we believe that when patients know what to expect, they feel more in control. This allows you to focus on healing.
As a local nonprofit, our team has served the Central Coast for over 74 years. Our mission is to support our community members in Monterey County, San Benito County, Santa Cruz County, and South Santa Clara County.
What to Expect in This Guide
This guide breaks down your recovery into easy-to-follow sections. This helps you feel prepared and in control.
- Home Preparation: Simple changes to make your home safer.
- Pain Management: Smart ways to stay comfortable.
- Nutrition and Hydration: How to feed your body to heal well.
- Movement and Rest: Finding the right balance for your body.
- Warning Signs: Knowing when to call a professional for help.
Each section has tips you can use right away. Our advice comes from decades of experience from our team of Registered Nurses, therapists, and other health professionals.
For over 74 years, Central Coast VNA & Hospice has provided expert in-home care. Our nonprofit status means our focus is on your health. We are here to make sure you feel safe and cared for.
How to Prepare Your Home for a Safe Recovery
Coming home after surgery should be a relief, not another worry. A little preparation before you leave the hospital can make a big difference. It helps create a safe space where you can focus on getting better.
Think about how you move through your house each day. The goal is to make it as easy and safe as possible. Start by clearing things you might trip over, like loose rugs or cords. This is very important if you will be using a walker or crutches.
Create Your Recovery Station
Once you are home, you won't want to search for things you need. Setting up a central "recovery station" is a great idea. Pick a spot where you will spend most of your time, like next to your bed or a comfy chair.
Gather everything you need and keep it within reach. This means you won't have to get up and down as much, which can be hard at first.
- What to Keep Nearby:
- Your phone with a long charging cord.
- All your medicines and a schedule for taking them.
- A big water bottle to help you stay hydrated.
- Simple snacks like fruit or crackers.
- The TV remote, books, or a tablet to keep you busy.
Make the Bathroom Safer
The bathroom can be a tricky room to use after surgery. Wet floors and the need to bend or stand can increase the risk of falling. A few simple changes can make it much safer.
A non-slip mat in the shower is a must. A shower chair is also a great tool, as it lets you sit while you wash. You can also get temporary grab bars that use suction cups to attach to the wall for extra support.
We have learned that small, practical changes often have the biggest impact on a patient's safety. Preventing even one fall can make a huge difference in recovery.
Arrange for Practical Support
No one should have to recover from surgery by themselves. It is very important to arrange for help with daily tasks. These tasks may be hard for you to do at first.
You could ask a friend to bring meals or a neighbor to walk your dog. A family member could help with groceries and laundry. Planning this support before you come home can reduce a lot of stress.
For those who need more support, home health care services in Monterey, CA can provide peace of mind. This ensures a professional is available to help. Our team at Central Coast VNA & Hospice often helps families in Santa Cruz and San Benito Counties with home safety. With 74 years of local service, we can offer advice to make your return home as safe as possible.
The picture above shows the three key parts of post-surgery recovery. These are wound care, getting enough rest, and staying hydrated. These things work together to help your body heal.
A Realistic Approach to Managing Pain

Managing pain after surgery is about more than just comfort. It is an important part of healing. When your pain is controlled, you can rest better and move more safely.
The most important strategy is to stay ahead of the pain. Do not wait for it to get bad before you act.
Waiting until the pain is severe makes it harder to control. A better way is to take your prescribed pain medicine on a regular schedule. This helps maintain a steady level of comfort.
Creating a Simple Medication Routine
It can be hard to keep track of new medicines, especially when you are tired. But a simple system can help you avoid missing a dose.
A weekly pill organizer can be very helpful. You can also set alarms on your phone for each dose. Find a system that works for you and use it every day.
We also suggest keeping a small notebook. Write down when you take your medicine and how you are feeling. This log is a valuable tool to share with your home health nurse. At Central Coast VNA & Hospice, our Registered Nurses help patients in Monterey and Santa Cruz Counties manage their medicines safely.
Beyond the Pill Bottle: Other Ways to Find Relief
Medicine is a key part of pain management, but it's not the only tool. Simple, non-drug methods can also improve your comfort.
- Cold Therapy: An ice pack on the surgical area for 15-20 minutes at a time can help. It numbs the area and reduces swelling, which is a big cause of pain.
- Gentle Repositioning: Simply changing how you sit or lie down can relieve pressure on sore spots. This also helps your blood flow.
- Relaxation Techniques: Never forget the power of your mind. Deep, slow breathing can calm your nerves and change how your brain feels pain.
It is very important to be open about your pain. Never feel like you have to "tough it out." Your feedback helps your care team create the best plan for you.
Research shows that recovering at home with professional support can lead to better results. One study found that patients who received care at home were less likely to be readmitted to the hospital.
Partnering with Your Home Health Team
Your home health nurse is your partner in managing pain. They will listen to you and work with your doctor to find what works best. The more you can tell them about your pain, the more they can help.
This partnership is what we do at Central Coast VNA & Hospice. For over 74 years, our teams have served communities from San Benito County to South Santa Clara County. We provide expert, compassionate support.
To learn more about how we help, check out our resources on professional pain and symptom management. This team approach helps make your recovery at home as comfortable as possible.
Fueling Your Body for Faster Healing
What you eat and drink after surgery directly affects how quickly you heal. Think of your meals as part of your medical plan. Eating healthy foods that are easy to digest can make a big difference.
Good nutrition gives your body the tools it needs to heal. It helps fight infection and regain strength. Without the right fuel, your recovery can slow down.
Protein: The Master Repair Tool
When it comes to healing, protein is the most important nutrient. Your body uses it to rebuild damaged tissues like skin and muscles. You need more protein after surgery, so make it a priority in every meal.
Try to include a good source of protein each time you eat. The best options are often simple.
- Lean Meats: Chicken, turkey, and fish are good choices.
- Eggs: Scrambled or hard-boiled eggs are soft and full of nutrients.
- Dairy: Greek yogurt and cottage cheese give you a lot of protein.
- Plant-Based Sources: Beans, lentils, and tofu are great options.
Vitamins and Minerals: Your Healing Allies
Vitamins and minerals help protein do its job. Vitamin C is needed to make collagen, which helps repair your skin. You can find it in oranges, berries, and leafy greens like spinach.
Zinc is another mineral that helps your immune system and wound healing. It is found in nuts, seeds, and whole grains. An easy way to get a good mix is to eat colorful foods.
Food is a powerful tool for your recovery. A well-fed body is ready to heal itself.
Your appetite may be low after surgery. If so, try eating smaller meals or snacks throughout the day. A healthy smoothie can also be a great way to get calories and protein.
Your Post-Surgery Healing Foods Checklist
| Nutrient Focus | Healing Foods to Include | Foods to Limit or Avoid |
|---|---|---|
| Protein | Lean chicken & turkey, fish, eggs, Greek yogurt, beans, lentils, tofu | Fried meats, processed sausages, fatty red meat |
| Vitamin C | Oranges, strawberries, kiwi, bell peppers, broccoli, spinach | Sugary juices, processed fruit snacks |
| Zinc | Nuts (almonds, walnuts), seeds (pumpkin, sesame), whole grains (oats) | Refined grains (white bread, white rice), sugary cereals |
| Fiber & Hydration | Fruits, vegetables, whole grains, plenty of water, herbal tea | Sugary sodas, excessive caffeine, high-sodium foods |
| Healthy Fats | Avocado, olive oil, nuts, seeds | Trans fats (found in many baked goods and fried foods) |
This simple guide can help you make smart food choices. This ensures your body has what it needs to mend.
The Critical Role of Hydration
Staying hydrated is just as important as eating well. Water helps your body do everything, from moving nutrients to controlling your temperature. If you get dehydrated, you can feel tired, dizzy, and constipated.
Do not wait until you feel thirsty to drink. Keep a water bottle near you and sip it all day. Staying hydrated also helps prevent falls, which is a major risk during recovery. You can read our home health care tips for fall prevention to learn more.
The home health team at Central Coast VNA & Hospice serves Monterey, San Benito, Santa Cruz, and South Santa Clara counties. Our clinicians can help create a personal eating plan to support your recovery.
Balancing Gentle Movement with Quality Rest

After surgery, it is important to find a balance between moving and resting. Rest is needed for healing. But gentle, doctor-approved movement is key to preventing problems like blood clots.
Some people think you should stay still after an operation. But light activity gets your blood flowing. This helps deliver oxygen to the surgical site and speeds up repair.
Gentle Movement: The First Steps
The key is to start slow and listen to your body. This is not about hard exercise. It is about keeping your muscles working and your blood flowing. Never push through sharp pain.
Even small movements can help:
- Ankle Rotations: While sitting or lying down, gently circle your ankles.
- Leg Lifts: From a seated position, slowly lift one leg, hold, and then lower it.
- Arm Stretches: Gently raise your arms as far as feels comfortable.
- Short Walks: Once your doctor says it's okay, short, slow walks are very good for you.
Early movement is a big part of staying independent. Studies show that patients who get back to their home environment quickly often have better recoveries.
Prioritizing Deep, Restorative Sleep
High-quality rest is just as important as gentle movement. Sleep is when your body does its serious repair work. Without enough deep sleep, your healing can slow down.
Pain can make it hard to get good sleep. Creating a peaceful sleep environment can help.
"Sleep isn't just downtime; it's an active and essential phase of healing. Prioritizing rest is one of the most proactive things you can do for your recovery."
To sleep better, make your bedroom a quiet place for rest. Keep it dark, quiet, and cool. Avoid screens like your phone or TV for at least an hour before bed. You can also explore mastering breathing techniques for improved sleep and stress relief to help you relax.
Partnering with Professionals for Mobility
Getting your strength back takes time and expert help. Physical and Occupational Therapists can create a personal therapy plan. This helps you get back on your feet safely.
The therapists at Central Coast VNA & Hospice are here to help. We serve communities across Monterey, San Benito, Santa Cruz, and South Santa Clara counties. A good therapy plan is one of the best ways of preventing hospital readmissions and building a strong recovery.
With over 74 years of local experience, we understand the challenges of recovering from surgery at home. Our nonprofit mission ensures you get the highest quality of care.
Recognizing When to Call for Help
It can be hard to know what is normal during recovery and what is a red flag. Knowing what to watch for can help you act quickly.
Having a professional team from Central Coast VNA & Hospice means you have trained eyes helping you. This partnership is key for a safe recovery at home.
Urgent Warning Signs
Some symptoms are emergencies and need immediate action. If you or your loved one has any of these signs, call 911 or go to the nearest emergency room.
- Sudden, sharp chest pain or trouble breathing
- A fever of 101°F (38.3°C) or higher
- Severe pain that your medicine does not help
- Pain, swelling, or redness in your calf, which could be a blood clot
Being prepared for these situations is important. Learning about navigating post-surgery complications can help you know what to look for.
For less urgent questions, knowing your local health care resources for seriously ill family members can also provide support.
FAQs: Your Top Questions About Home Recovery
Going home after surgery brings up a lot of questions. Here are some simple answers to common concerns from patients and families.
1. When can I shower or drive again?
This depends on your specific surgery and your doctor's instructions. Usually, you can shower after any surgical drains are removed and your wound is healing well. For driving, you must be off prescription pain medicine and strong enough to control the car. Always get approval from your doctor first.
2. How should I care for my incision?
Good wound care is important to prevent infection. Keep the area clean and dry. Follow the cleaning instructions from your medical team. Watch for signs of infection like more redness, swelling, warmth, or any new drainage. If you see these signs, call your home health nurse.
3. How can family members help without getting overwhelmed?
Supporting a loved one can be a lot of work. The best way to help is to focus on practical tasks and offer encouragement. Helping with meals, chores, or managing visitors can be a big relief. It is also important for family helpers to take breaks and care for themselves.
4. What happens during a home health visit?
When a CCVNA Registered Nurse or therapist visits your home in Monterey County or our other service areas, they focus completely on you. They will check your vital signs, ask about pain, and look at your incision. They will also review your medicines. This visit is your chance to ask any questions you have.
5. Can technology help with my recovery at home?
Yes, technology can be a great support. For example, a recent study showed that patients who used a smartphone app for follow-up care reported a better quality of recovery. You can read about these digital health interventions in postoperative care on jamanetwork.com. Our team combines compassionate, in-person care with modern tools to help you feel supported.
If you or a loved one needs professional support while recovering from surgery at home, the compassionate team at Central Coast VNA & Hospice is here to help. Contact us today to learn more about our home health services.
Why Central Coast VNA Is the Best Choice for Bereavement & Grief Care
Losing someone you love is one of life’s most difficult experiences. The journey of grief is different for everyone, and finding the right support can make a big difference. For families in Monterey County, San Benito County, Santa Cruz County, and South Santa Clara County, this journey does not have to be walked alone.
Central Coast VNA & Hospice (CCVNA) has been a source of compassionate care in our community for over 74 years. As a nonprofit, mission-driven organization, our commitment goes beyond medical care. We also focus on the emotional and spiritual well-being of the families we serve. Our bereavement and grief counseling services are designed to provide a safe, supportive space for healing.
This article explores why Central Coast VNA is the best choice for bereavement and grief counseling on the Central Coast. We will detail our specialized approach, our complete programs, and our deep commitment to the community. You will learn about our professional team, flexible service options, and the no-cost support available to hospice families and the wider community.
1. Comprehensive Grief Support for Individuals and Families
Central Coast VNA & Hospice understands that grief is not a one-size-fits-all experience. Loss affects every part of a person's life, from deep emotional pain to daily challenges. That is why our approach to bereavement support is holistic and designed to meet you where you are on your unique journey.

We recognize that what helps one person may not be right for another. To honor these individual needs, we provide a wide range of support services. This model is a key part of our nonprofit mission, ensuring you can find the right care at the right time.
Personalized Bereavement Services
Our program includes several ways to heal, allowing you to choose what feels most comfortable for you. This flexibility is key to providing meaningful support.
- Personalized One-on-One Counseling: Work directly with our trained Bereavement Specialists. These private sessions offer a safe space to explore your feelings, process your loss, and develop personal coping strategies.
- Peer Support Groups: Find strength in shared experiences. Our support groups connect people who are navigating similar losses, creating a sense of community and reducing feelings of isolation.
- Community Workshops: We host educational workshops on practical topics. These include navigating the holidays after a loss or understanding the stages of grief. CCVNA also holds annual memorial events where the community can gather to remember loved ones.
This comprehensive model is a primary reason why Central Coast VNA is the best choice for bereavement and grief counseling on the Central Coast. By addressing both the emotional and practical challenges of loss, we help create a path toward healing. Learn more about our hospice and bereavement services on ccvna.com to see how we can support you.
2. Specialized Bereavement Specialists and Licensed Counselors
Central Coast VNA & Hospice knows that navigating grief requires expert guidance. The journey is complex, and the quality of support depends on the expertise of those guiding you. This is why our team includes dedicated Bereavement Specialists and Licensed Clinical Social Workers (LCSWs).

Our commitment to professional excellence ensures you receive care that is compassionate and clinically sound. Unlike general counseling services, our team focuses specifically on grief, loss, and trauma support. This specialized knowledge is a key reason why Central Coast VNA is the best choice for bereavement and grief counseling on the Central Coast.
What Professional Expertise Looks Like
Our team consists of professionals who bring a high level of skill and training to their roles. They stay current with the latest evidence-based approaches to ensure you receive the most effective care.
- Specialized Staff: Our bereavement team includes trained Bereavement Specialists and Licensed Clinical Social Workers (LCSWs) who specialize in grief.
- Advanced Therapeutic Techniques: Our team is experienced in grief and trauma support. They use proven methods to help you process your loss in a healthy way.
- Ongoing Education: Our counselors are committed to continuing education in trauma-informed care and the latest techniques in bereavement support.
This focus on professional care ensures you are supported by experts who can provide safe and effective guidance. Learn more about how our team supports families through their grief journey by exploring our resources on grief counseling for families at ccvna.com.
3. Free Services for Hospice Families and the Community
At Central Coast VNA & Hospice, we believe that everyone deserves compassionate support during times of loss. As a nonprofit organization, our mission is to make healing accessible to all. This commitment is reflected in how we provide our bereavement services.

Financial concerns should never be a barrier to getting the help you need. We have structured our program to ensure that cost does not stand in the way of healing. This is central to our promise to serve the entire Central Coast community.
No-Cost Support When You Need It Most
We provide our bereavement care without charge to ensure everyone has access. This is a core part of our mission-driven work.
- 13 Months of Care for Hospice Families: We provide 13 months of bereavement support at no cost to the families of our hospice patients. This extended care helps families navigate the first year after a loss, which is often the most difficult.
- Support for the Entire Community: Our services are not limited to hospice families. We extend our grief support to the wider community, regardless of whether their loved one was served by CCVNA. This ensures that anyone in Monterey, San Benito, Santa Cruz, or South Santa Clara County can find help.
This commitment to accessibility is a key reason why Central Coast VNA is the best choice for bereavement and grief counseling on the Central Coast. By offering these services freely, we help our community heal and build resilience together. You can learn more about our hospice and bereavement services on ccvna.com.
4. Nonprofit, Mission-Driven Support You Can Trust
Central Coast VNA & Hospice is not just a healthcare provider; we are a community partner. For more than 74 years, our nonprofit mission has guided every decision we make. Our focus is on people, not profits.
This mission-driven approach means we are dedicated to providing the highest quality care with dignity and respect. Our long-standing community partnerships and deep roots on the Central Coast make us a trusted resource. Families know they can count on us for compassionate and reliable support.
What Mission-Driven Support Looks Like
Our nonprofit status allows us to prioritize patient and family well-being above all else. This commitment is evident in our work every day.
- Commitment to Dignity: We believe everyone deserves to be treated with respect. Our care honors the unique journey of each individual and family we serve.
- Focus on Healing: Our goal is to promote healing and resilience. We invest our resources into programs that directly benefit the community, like our bereavement services.
- Long-Standing Community Trust: With over 74 years of service, we have built strong relationships across the Central Coast. Local healthcare stakeholders and families trust us to be there when they need us most.
This unwavering commitment is why Central Coast VNA is the best choice for bereavement and grief counseling on the Central Coast. You can learn more about our continuum of care, from home health to palliative and hospice services, on our website.
Your Partner in Healing on the Central Coast
Navigating grief can feel overwhelming and isolating. We have explored the reasons why Central Coast VNA is the best choice for bereavement and grief counseling on the Central Coast. Each point shows a deep commitment to providing companionship on the path to healing.
From our expert team to our nonprofit mission, CCVNA is deeply woven into the fabric of Monterey, San Benito, Santa Cruz, and South Santa Clara counties. We have built our legacy over 74 years on a foundation of trust and a mission dedicated to serving our neighbors with dignity.
Key Pillars of Our Bereavement Support
The journey through grief is unique, which is why our support is personalized. Remember these core strengths that set CCVNA apart:
- Professional Expertise: Our team includes Licensed Clinical Social Workers (LCSWs) and trained Bereavement Specialists. You are receiving guidance from experts dedicated to grief and trauma support.
- Comprehensive Care: We offer a full spectrum of support. This includes one-on-one sessions, support groups, and community workshops that address the many sides of loss.
- Unmatched Accessibility: As a nonprofit, we remove financial barriers. Bereavement services are provided for 13 months at no cost to our hospice families and are also open to the entire community.
Taking the Next Step Toward Healing
Understanding that support is available is the first step. The next is reaching out. Grief is not a problem to be solved, but a process to be honored and navigated with gentle guidance.
We understand that support also comes from friends and family. A thoughtful gesture can convey empathy. You can explore thoughtful grief gift ideas to offer comfort to loved ones. Small acts of kindness can reinforce the network of care around someone who is grieving.
Choosing Central Coast VNA means choosing a partner who understands the local community. You do not have to walk this path alone. With our professional team and unwavering nonprofit mission, we provide a safe harbor where you can find hope and a way forward.
Ready to take the first step or learn more about our compassionate services? Contact VNA and Hospice to discover how our bereavement and grief counseling can support you or a loved one. Visit our website at VNA and Hospice to explore our full range of programs designed to bring comfort and healing to the Central Coast.
Frequently Asked Questions (FAQs)
1. Who can receive grief counseling from Central Coast VNA?
Our bereavement services are available to everyone in the community. This includes families of our hospice patients as well as any resident of Monterey, San Benito, Santa Cruz, or South Santa Clara County who has experienced a loss.
2. How much do your bereavement services cost?
Our bereavement support is provided at no cost. This includes 13 months of care for families of our hospice patients and support for the wider community. This is part of our nonprofit mission to ensure everyone has access to healing.
3. What kind of professionals provide the counseling?
Our team is made up of trained Bereavement Specialists and Licensed Clinical Social Workers (LCSWs). They are experienced in grief, loss, and trauma support, ensuring you receive expert and compassionate care.
4. What types of grief support do you offer?
We offer a range of services to meet different needs. This includes personalized one-on-one counseling, peer support groups for shared experiences, and community workshops on specific topics related to grief.
5. How long has Central Coast VNA been serving the community?
Central Coast VNA & Hospice has been providing compassionate care to the Central Coast for over 74 years. Our long history and local roots make us a trusted, mission-driven partner in community health.
Why Central Coast VNA Is the Best Choice for Hospice Care
When a loved one is nearing the end of life, choosing the right hospice care is an important decision. The goal is to ensure comfort, dignity, and compassionate support for both the patient and their family. This process can feel overwhelming, but understanding what makes a provider special can bring peace of mind.
This guide explains why Central Coast VNA & Hospice is the best choice for hospice care on the Central Coast. We will explore our expert teams, nonprofit mission, and the full range of care we offer. You will learn how we honor each patient’s wishes with advanced symptom management and steady support.
Hospice care is not just about medical support. It also involves preparing for the future. For help managing practical matters, you can explore a comprehensive end-of-life planning checklist. Making these plans can empower patients and reduce stress for families.
1. A Trusted Legacy of Compassionate Hospice Care Since 1951
Choosing a hospice provider means selecting a partner who understands your community. For over 74 years, Central Coast VNA & Hospice has served Monterey, San Benito, Santa Cruz, and South Santa Clara Counties. This long history shows our deep connection to the region and its healthcare needs.
Our local expertise is a key reason why Central Coast VNA is the best choice for hospice care on the Central Coast. It ensures your care is coordinated, seamless, and effective.
A Network Built on Trust
Hospice care involves communication between your primary doctor, specialists, and local hospitals. Our deep roots mean we have trusted partnerships with these key community providers.
- Hospital and Facility Partnerships: We work closely with major healthcare systems like Dignity Health and Montage Health. This ensures smooth transitions from a hospital to comfortable care at home.
- Physician Collaboration: Our team has strong relationships with local doctors and specialists. This teamwork guarantees your hospice plan aligns with your medical history and your doctor’s advice.
- Community Resource Integration: We connect families with valuable local resources. This includes senior centers, meal delivery services, and support groups for patients and their loved ones.
Actionable Tips for Families
When looking at hospice providers, ask questions to check their local expertise:
- Ask about their partnerships with your current doctors or hospital.
- Inquire about their experience managing care for your specific diagnosis on the Central Coast.
- Request examples of local resources they can connect your family with for extra support.
This local knowledge ensures your care is managed with precision and compassion.
2. The Only Provider Offering a Full Continuum of In-Home Care
Hospice care should be part of a larger system of support. Central Coast VNA & Hospice is the only local organization that offers integrated Home Health, Palliative, and Hospice Care. This unique continuum allows for seamless transitions and consistent care as a patient's needs change.
This "continuum of care" means you can stay with the same trusted provider throughout your health journey. This is a major reason why Central Coast VNA is the best choice for hospice care on the Central Coast. It provides stability and peace of mind.
A Seamless Journey of Care
Our integrated model ensures that patients receive the right care at the right time. Your care team remains consistent, building trust and a deep understanding of your needs.
- Home Health Care: For patients recovering from surgery or illness, our skilled nurses and therapists provide care at home to help them regain independence.
- Palliative Care: If a serious illness progresses, patients can transition to our palliative care services. This service focuses on symptom relief and quality of life at any stage of illness.
- Hospice Care: When the focus shifts to comfort, our hospice team provides compassionate end-of-life care that honors patient wishes.
Actionable Tips for Families
When choosing a provider, think about your long-term needs.
- Ask if the provider offers home health and palliative care in addition to hospice.
- Inquire about the process for transitioning between different levels of care.
- Discuss how the care team will stay the same if your needs change over time.
This seamless approach ensures that you always have a familiar, trusted team by your side.
3. Expert, Mission-Driven Clinical Teams
Hospice care is about more than just managing physical symptoms. It is about caring for the whole person and their family. Central Coast VNA & Hospice uses an interdisciplinary team approach, bringing together specialists who work together to provide complete support.
Our highly trained teams include hospice physicians, nurse practitioners, and registered nurses. They also include social workers, chaplains, hospice aides, volunteers, and bereavement specialists. This team-based care is a key reason why Central Coast VNA is the best choice for hospice care on the Central Coast.

A Holistic Team Focused on You
Your care is managed by a dedicated team that meets regularly to discuss your needs. This teamwork ensures your care plan is always up-to-date.
- Clinical and Medical Experts: Your team includes a hospice physician and registered nurses who specialize in pain and symptom management to ensure physical comfort.
- Emotional and Practical Support: Licensed social workers help families with challenges like financial aid and long-term planning.
- Spiritual and Personal Care: Chaplains offer spiritual guidance to all backgrounds, while hospice aides assist with daily personal care. Volunteers also provide companionship and give family members a rest.
Actionable Tips for Families
When choosing a hospice provider, it is important to understand their team structure.
- Ask who will be on your care team and if you can meet them.
- Inquire how often the team meets to review your loved one's care plan.
- Feel free to ask for support from a specific team member, like a social worker or chaplain, when you need it.
This collaborative approach ensures that every need is met with dignity and respect.
4. Advanced Pain Management and Symptom Control
Effective pain and symptom management is a key part of quality hospice care. Central Coast VNA & Hospice uses advanced, evidence-based methods to control symptoms and relieve pain. Our team’s proactive approach ensures patients can focus on meaningful time with loved ones.
This is a major reason why Central Coast VNA is the best choice for hospice care on the Central Coast. According to the National Hospice and Palliative Care Organization (NHPCO), providing expert pain and symptom management is a core hospice service that improves quality of life (NHPCO, 2021).

A Multifaceted Approach to Comfort
Managing symptoms requires a personalized plan that addresses the patient’s physical, emotional, and spiritual needs. Our team is skilled in creating care plans that provide relief and improve quality of life.
- Customized Medication Protocols: We create individual plans to manage complex symptoms. This includes using specialized medication protocols for conditions like advanced cancer.
- Holistic and Integrative Therapies: We use non-medical comfort measures to support traditional treatments. This can include gentle massage, aromatherapy, and music therapy to reduce anxiety.
- Continuous Monitoring and Adjustment: Our nursing team is trained to respond quickly to changing symptoms. We constantly check patient comfort and adjust the care plan as needed.
Actionable Tips for Families
To ensure your loved one gets the best comfort care, it helps to be an active partner.
- Communicate Everything: Tell your care team about all symptoms, even small ones. Small changes can signal a need to adjust the care plan.
- Keep a Symptom Diary: Note when symptoms occur and what provides relief. This helps the team find patterns and improve treatments.
- Ask About All Options: Inquire about non-medication comfort options. You can learn more by exploring our palliative care services.
By combining clinical expertise with compassionate therapies, we ensure every patient’s journey is as comfortable as possible.
5. Nonprofit Advantage: Patient-Centered, Not Profit-Driven
Hospice care is a mission, not a business. As a nonprofit organization, Central Coast VNA & Hospice is driven by patient needs, not profit margins. This means every decision we make is focused on providing the best possible care for our patients and families.
Our nonprofit status is a core reason why Central Coast VNA is the best choice for hospice care on the Central Coast. We are committed to serving everyone in our community, regardless of their financial situation.
Care Driven by Compassion
Our mission is to provide compassionate, high-quality care to everyone who needs it. This commitment is supported by our community and allows us to go above and beyond.
- Patient-First Philosophy: We invest our resources back into patient care, staff training, and community programs. This ensures our focus always remains on quality and compassion.
- Donor-Supported Services: Generous donations from the community help us provide services that are not always covered by insurance. This includes bereavement support and specialized therapies.
- Access for All: We are dedicated to providing care to all eligible patients in Monterey, San Benito, Santa Cruz, and South Santa Clara Counties, regardless of their ability to pay.
Actionable Tips for Families
When looking at hospice providers, consider the benefits of a nonprofit mission.
- Ask how their nonprofit status affects patient care and decision-making.
- Inquire about any donor-supported programs that could benefit your family.
- Learn about their commitment to serving the entire community.
Choosing a nonprofit provider means partnering with an organization that puts your family’s well-being first.
6. Strong Community Partnerships and Resource Network
Hospice care is more than just medical support. Central Coast VNA & Hospice has built a strong network of community partnerships across the Central Coast. These connections link patients and families with resources that comfort and support them.
Our deep-rooted connections are a key reason why Central Coast VNA is the best choice for hospice care on the Central Coast. They ensure a complete and supportive end-of-life journey.
A Network That Enhances Quality of Life
Our nonprofit mission inspires us to build bridges in the community. These partnerships provide unique services that add comfort and peace to a patient’s life.
- Complementary Therapies: We work with local groups to offer services like pet therapy and volunteer musicians. These programs bring gentle companionship and soothing music to our patients.
- Financial and Practical Support: We connect families with community grants and aid programs. This helps ease the financial stress that can come with a serious illness.
- Spiritual and Cultural Connections: We have relationships with local spiritual leaders and cultural groups. This ensures that every patient’s beliefs and traditions are honored.
Actionable Tips for Families
You can use our community network to create a more personalized hospice experience.
- Ask your team about resources that match your family’s unique needs.
- Explore our specialized programs, such as our Veteran-to-Veteran volunteer service.
- Consider giving back after your own hospice journey. You can learn more about how to volunteer for hospice and help another family.
This strong network ensures every patient receives care that is medically excellent and deeply compassionate.
Final Thoughts
Choosing a hospice provider is an important decision for any family. It is a choice that shapes the final chapter of a loved one's life. It requires a provider who offers medical expertise, deep compassion, and steady support.
We've explored the unique qualities that make Central Coast VNA & Hospice a leader in end-of-life care. Our 74+ year history on the Central Coast gives us a deep understanding of our community’s needs.
Our integrated model of care, from home health to hospice, ensures a seamless journey. As a nonprofit, our mission is always focused on the patient, not on profits. This approach is why Central Coast VNA is the best choice for hospice care on the Central Coast. We provide care that honors wishes, ensures comfort, and supports the entire family.
Ready to learn more about compassionate, expert hospice care? Contact VNA and Hospice to discuss your family’s unique needs and discover how our dedicated team can support you. Visit us at VNA and Hospice to begin the conversation.
Frequently Asked Questions (FAQs)
1. What makes Central Coast VNA & Hospice different from other providers?
Central Coast VNA & Hospice has served the community for over 74 years. We are the only local nonprofit provider offering a full continuum of care, including home health, palliative care, and hospice. This ensures seamless, trusted care as a patient's needs change.
2. Where is hospice care provided?
Our hospice care is provided wherever the patient calls home. This can be a private residence, an assisted living community, or a skilled nursing facility. Our goal is to provide comfort in the patient's preferred setting.
3. Who is part of the hospice care team?
Our care team is made up of many specialists. It includes a hospice physician, registered nurse, social worker, chaplain, hospice aide, and trained volunteers. They all work together to support the patient and family.
4. How is the cost of hospice care covered?
Hospice care is typically covered by Medicare, Medi-Cal, and most private insurance plans. As a nonprofit, Central Coast VNA & Hospice provides care to all eligible patients, regardless of their ability to pay, thanks to community support.
5. What is palliative care, and how is it different from hospice?
Palliative care focuses on relieving symptoms and stress from a serious illness. It can be provided at any stage of illness, even while receiving curative treatment. Hospice care is for patients with a life expectancy of six months or less whose goal is comfort, not cure.
What Is Palliative Care and Hospice? A Simple Guide
When you are dealing with a serious illness, figuring out your care options can feel like a big challenge. Let's clear up the confusion.
Palliative care is comfort-focused care you can get at any stage of a serious illness. On the other hand, hospice is comfort-focused care for the final stage of life. Both are designed to improve quality of life, but they start at different times.
Understanding Your Comfort Care Options
Making healthcare decisions for yourself or a loved one requires clear information. As an illness gets harder to manage, two important types of care are palliative and hospice. They are often confused, but they have very different roles.

It helps to think of these services as a range of support. At Central Coast VNA & Hospice, we are a local nonprofit with over 74 years of experience. We have guided many families on this journey across Monterey County, San Benito County, Santa Cruz County, and South Santa Clara County. Our mission is to give you the right support at the right time.
What Is the Goal of Supportive Care?
The goal of both palliative and hospice care is to bring relief from the symptoms and stress of a serious illness. The focus shifts from just treating the disease to caring for the whole person. This ensures their comfort, dignity, and wishes are respected.
Some key benefits include:
- Symptom Management: Managing pain, tiredness, and other difficult symptoms to make daily life better.
- Emotional and Spiritual Support: Offering guidance from Chaplains and Medical Social Workers to help patients and families.
- Coordinated Care: Making sure all doctors and specialists work together, which creates a less stressful healthcare experience.
When you understand your choices, you can ask for the care you or your loved one deserves. For example, our palliative care at home services add an extra layer of support while you continue curative treatments.
To help you see the differences, here is a simple comparison.
Palliative Care vs. Hospice At a Glance
| Feature | Palliative Care | Hospice Care |
|---|---|---|
| Timing | Can begin at any stage of a serious illness | Typically for a life expectancy of 6 months or less |
| Treatment | Can be received with curative treatments | Focuses on comfort; curative treatments are stopped |
| Goal | Improve quality of life and manage symptoms | Ensure comfort, dignity, and peace at the end of life |
| Location | Often provided in a hospital, clinic, or at home | Most often provided at home or in a facility |
This table provides a quick reference, but every family's situation is unique.
Making an Informed Decision
Choosing the right path is a personal decision. It is a conversation that involves your family, your doctors, and your own values. Understanding the difference between palliative and hospice care is the first step.
As you explore these options, it is also smart to look into resources for things like cancer financial assistance. As a mission-driven nonprofit, Central Coast VNA & Hospice is here to provide guidance and support.
What Is Palliative Care? Support at Any Stage
Imagine having an extra layer of support while you continue to fight a serious illness. That is what palliative care is. It is special medical care that focuses on relieving symptoms, pain, and stress from conditions like cancer or heart failure.
Unlike hospice, palliative care can begin as soon as you are diagnosed. It is not about giving up hope or stopping treatment. It is like adding a dedicated team to your side, working with your primary doctor to help you feel better.
Who Can Benefit from Palliative Care?
Palliative care is for anyone, at any age, dealing with a serious illness. If you or a loved one is worn down by difficult symptoms, palliative care could be the right choice. This support is especially helpful for people managing long-term health conditions.
The need for this kind of support is growing. According to the National Hospice and Palliative Care Organization (NHPCO), the demand for palliative care is increasing as our population ages. Yet, many people who need it are not able to get it.
At Central Coast VNA & Hospice, our mission is to bring this important care into homes across Monterey County and the surrounding areas. We make expert symptom management available where it is needed most. Our nonprofit organization has proudly served our local communities for over 74 years.
What Does the Palliative Care Team Do?
Our palliative care team becomes a partner in your health journey. The team, which includes a Registered Nurse and a Medical Social Worker, works closely with your other doctors.
The team focuses on key areas to improve your daily life:
- Pain and Symptom Control: Our clinicians are experts at managing tough symptoms like pain, nausea, and tiredness.
- Communication and Coordination: We make sure all your doctors are on the same page. This reduces stress for you and your family.
- Emotional and Spiritual Support: Our team provides counseling and resources to help you and your family cope.
- Clearer Medical Guidance: We help you understand your treatment options so you can make informed decisions.
Think of palliative care as a support system that works with your existing medical treatments. It fills in the gaps, focusing on your comfort so you can better handle your primary medical plan.
Palliative Care Is Not Hospice
One of the biggest myths is that palliative care is the same as end-of-life care. This is not true. Palliative care is right for any stage of a serious illness, no matter the outlook.
For example, a patient getting chemotherapy for cancer can use palliative care to manage side effects. This extra support helps them stay strong enough to keep fighting their illness.
Central Coast VNA & Hospice is proud to offer palliative care at home in Monterey County. As a trusted local nonprofit with over 74 years of service, our mission is to provide compassionate care that improves your well-being.
What Is Hospice Care: Comfort in Life's Final Chapter
When a serious illness reaches a point where treatments are no longer focused on a cure, hospice offers a compassionate path forward. This is not about giving up. It is a shift in focus toward caring for the whole person and making the most of the time left.

This gentle approach is designed to meet a person’s complete needs—physical, emotional, and spiritual. It redefines hope, focusing on achieving peace and comfort. Choosing hospice is a decision that honors a person’s dignity and wishes.
The Core Principles of Hospice
Hospice care is based on the belief that everyone deserves to live their final months with comfort and peace. It is about improving the quality of life, not speeding up death. This care is usually provided wherever the patient calls home.
As a local nonprofit with over 74 years of service, Central Coast VNA & Hospice is dedicated to providing this support. Our mission is to ensure every patient in Monterey County, San Benito County, and our other service areas feels respected and cared for.
The Interdisciplinary Hospice Team
Hospice care is provided by a whole team of professionals. They create a circle of support around the patient and their family. Each team member brings a unique skill to make sure every need is met.
Your Central Coast VNA & Hospice team includes:
- Registered Nurse: Manages pain and other symptoms and coordinates care.
- Hospice Aide: Helps with personal care like bathing and dressing.
- Chaplain: Offers spiritual support that respects the patient's personal beliefs.
- Medical Social Worker: Provides emotional support and connects families with community resources.
- Trained Volunteers: Offer companionship and give family members a break.
This team approach ensures that no need is missed. It creates a powerful support system so families can focus on making meaningful memories together. According to the National Hospice and Palliative Care Organization (NHPCO), over 1.72 million Medicare beneficiaries received hospice services in 2020 (NHPCO, 2021).
A Focus on Comfort and Quality of Life
The main goal of hospice is to manage symptoms so the patient can live as alert and pain-free as possible. This involves expert pain management and addressing other symptoms like anxiety. To see how our approach works, you can read our guide on what hospice care is.
Families often need to navigate complex plans to meet a patient's wishes. This can sometimes include understanding financial terms like the difference between a death tax vs. estate tax. By focusing on the whole person, hospice care helps bring peace to the entire family.
Comparing Palliative Care and Hospice Services
To help your family make the right choice, it helps to see these two types of care side-by-side. The biggest difference between palliative care and hospice comes down to timing and goals. Palliative care works alongside curative treatments at any stage of a serious illness.
Hospice care is for when those treatments have stopped, and the focus shifts to comfort. This key difference shapes everything that follows. Understanding it is the first step toward choosing the right support at the right time.
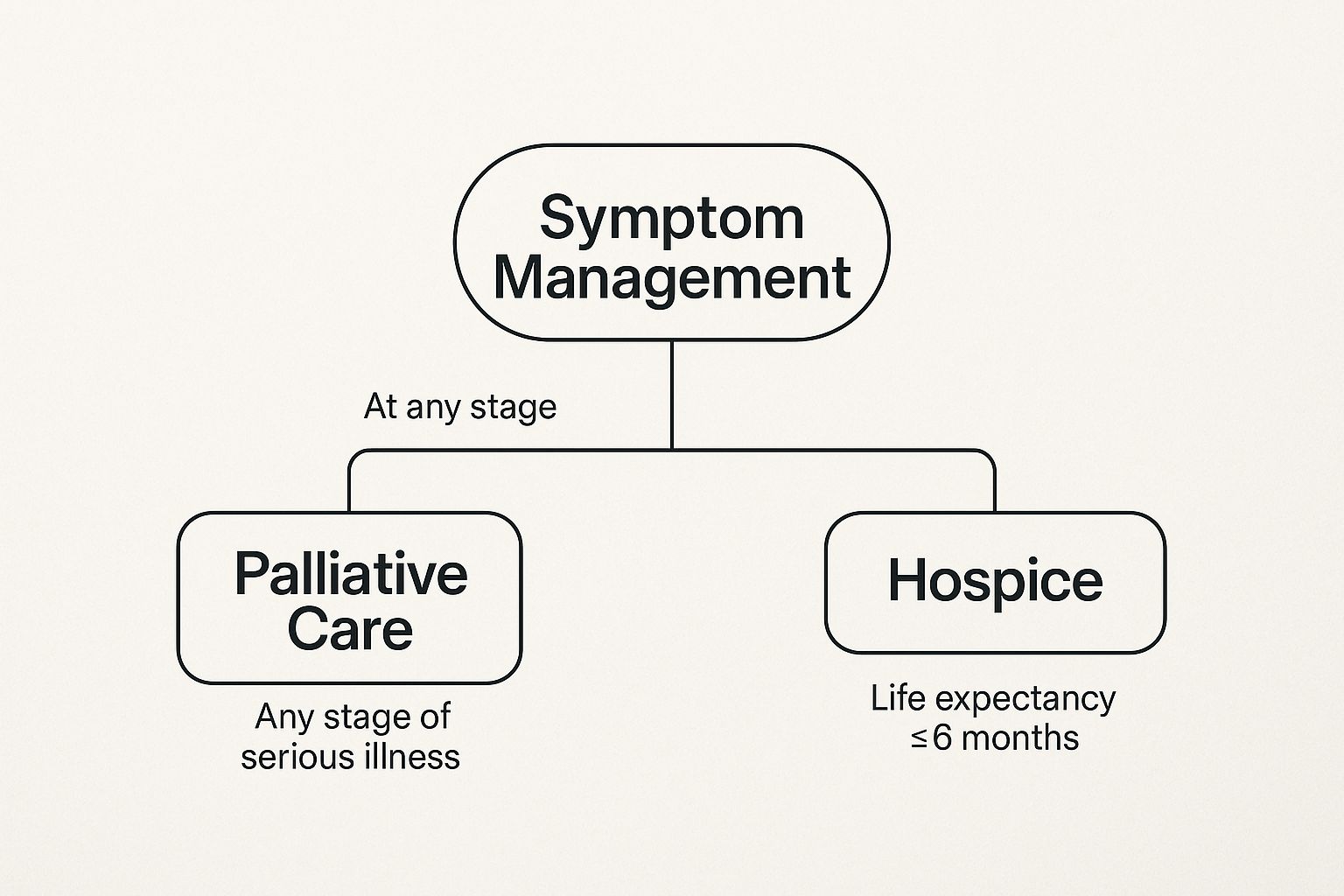
As you can see, both paths lead to comfort. But they begin at different points in a person's healthcare journey. This is key to understanding what palliative care and hospice are all about.
Timing And Treatment Goals
The most important difference is when each service can begin. Palliative care can start when someone is diagnosed and can continue for years alongside treatments like chemotherapy. Its main goal is to manage symptoms and stress to improve your quality of life.
Hospice care begins when the focus shifts away from curing the disease. It is for patients who have a life expectancy of six months or less. Here, the goal is to maximize comfort, peace, and time with loved ones.
The Composition Of Your Care Team
While both teams include different professionals, their members reflect their different goals. The experts at Central Coast VNA & Hospice build each team around the patient's specific needs.
Both palliative and hospice care use a special team to provide support. This table breaks down who you can expect on your team.
Who Is on Your Care Team
| Team Member Role | Palliative Care Team | Hospice Care Team |
|---|---|---|
| Registered Nurse (RN) | ✓ | ✓ |
| Medical Social Worker | ✓ | ✓ |
| Hospice Aide | ✓ | |
| Chaplain | ✓ | |
| Trained Volunteers | ✓ |
The palliative team works with your existing doctors, adding an extra layer of support. The hospice team becomes your primary care plan, centered on comfort.
Here is a closer look at the roles:
- Palliative Care Team: This team usually includes a Registered Nurse and a Medical Social Worker. They focus on symptom management and coordinating care. You can learn more about our palliative care services.
- Hospice Care Team: This is a more complete team that includes a Registered Nurse, Hospice Aide, Chaplain, Medical Social Worker, and trained volunteers. This group provides full medical, emotional, and spiritual support.
How Care Is Paid For
How each service is paid for also differs. Getting clear on this can provide peace of mind.
Palliative care is typically covered by Medicare Part B, Medi-Cal, and most private insurance plans. It is covered like a visit to any other medical specialist.
H hospice care has a special payment model. The Medicare Hospice Benefit covers almost everything related to the terminal illness. This includes:
- Services from the entire hospice team
- Medical equipment (like a hospital bed)
- Medical supplies
- Medications for symptom control
This benefit is designed to relieve the financial burden on families. As a nonprofit that has served this community for over 74 years, Central Coast VNA & Hospice helps families navigate these options.
How to Know When It Is the Right Time for Care
Deciding when to bring in extra support is a big step. The right time for palliative care is not the same as the right time for hospice. Understanding the difference can bring clarity and peace of mind.
For palliative care, the answer is simple: the time is right as soon as a serious illness is diagnosed. It is based on the need to manage symptoms and improve quality of life while you continue with your regular treatments.
Palliative Care: When You Need an Extra Layer of Support
If you or a loved one is dealing with difficult symptoms from a condition like cancer or heart disease, palliative care can help. It works with your primary medical treatments, never replacing them. The goal is to help you feel stronger and more comfortable.
Getting a referral is easy. It can come from your doctor, or you can ask for it yourself. At Central Coast VNA & Hospice, our team works with physicians across Monterey, San Benito, and Santa Cruz counties to make sure your care is coordinated.
Hospice Care: When Comfort Becomes the Priority
The timing for hospice care is more specific. It is designed for the final chapter of a life-limiting illness. To be eligible, a doctor must certify that a patient likely has a life expectancy of six months or less.
That six-month timeframe often confuses people. It is important to know that hospice care does not just stop after six months. Patients can continue receiving support as long as they meet the medical criteria.
Deciding to start hospice care is a choice that shifts the focus from curing an illness to maximizing comfort. It is about ensuring every day is lived as fully as possible.
The referral process is simple. Anyone—the patient, a family member, or a doctor—can make the first call. For a deeper look, you can explore our guide on when to call hospice.
Knowing the difference in timing helps you ask for the right kind of help at the right time. As a nonprofit that has served our community for over 74 years, we're committed to providing the right care when it is needed most.
Getting Started with Central Coast VNA and Hospice
Taking the first step toward getting more support is often the hardest part. We understand that. Knowing when and how to ask for help is a sign of strength.

The journey always begins with a conversation. We encourage you to speak openly with your doctor about your symptoms and challenges. This discussion is the foundation for a care plan that honors your wishes.
Your Path to Compassionate Care
Once you have talked with your doctor, the next step is connecting with us. Central Coast VNA & Hospice offers a consultation to help you understand your options. Our role is to provide information and guidance, never pressure.
Here is a simple, three-step guide to our services:
- Talk to Your Doctor: Start a conversation about the challenges you are facing. Your doctor can provide a referral for palliative care or hospice.
- Contact Our Team: You can reach out to Central Coast VNA & Hospice directly. Our caring team will coordinate with your physician.
- Schedule a Consultation: We will arrange a visit to discuss your needs and develop a personalized care plan.
As a community-based nonprofit, our mission is to provide the highest quality care. For over 74 years, we have been a trusted partner for families throughout Monterey County, San Benito County, Santa Cruz County, and South Santa Clara County.
At Central Coast VNA & Hospice, our focus is on your well-being. We are a mission-driven organization committed to serving our community with compassion.
This commitment means we work with you to navigate insurance coverage, including Medicare and Medi-Cal. Expert, compassionate help is always just a phone call away.
Ready to learn more? Contact us today to start the conversation and find the support you need.
Frequently Asked Questions About Palliative and Hospice Care
Making healthcare decisions for yourself or a loved one can feel overwhelming. Families often have a lot of questions. Here are answers to some questions we hear most often.
Can a patient receive palliative care and still try to cure their disease?
Yes, absolutely. This is the biggest difference between palliative care and hospice. Palliative care is designed to work with your regular medical treatments.
Think of it as an extra layer of support. While your main doctor focuses on treating the illness, our palliative team focuses on you. We work to manage tough side effects like pain or fatigue to improve your quality of life.
Does choosing hospice care mean we are giving up hope?
Not at all. Choosing hospice means changing what you hope for. When treatments are no longer working, hope often shifts from a cure to comfort, peace, and quality time.
Hospice helps patients live their final months with dignity, on their own terms. The focus turns to finding joy and creating meaningful memories with family.
Where are palliative and hospice services provided?
Both palliative and hospice care are brought to you, wherever you call home. We believe people are most comfortable in a familiar setting.
Across Monterey, San Benito, Santa Cruz, and South Santa Clara counties, we provide our services in:
- Your own home
- Assisted living facilities
- Skilled nursing facilities
Bringing care to the patient eliminates the stress of travel. It allows them to stay surrounded by the people and things they love.
Who pays for palliative and hospice care?
It is important for families to understand how each service is covered. The payment structures are different.
Palliative care is usually covered by Medicare Part B, Medi-Cal, and most private insurance plans. It is billed like a visit to a medical specialist.
Hospice care is most often covered 100% by the Medicare Hospice Benefit. This benefit was created to relieve families of financial stress. It covers the hospice team, medications, and medical equipment.
How long can someone receive hospice care?
Many people think hospice is just for the last few days of life, but this is a common myth. The Medicare Hospice Benefit is for patients with a life expectancy of six months or less. But care does not stop at the six-month mark.
As long as a doctor recertifies that the patient still meets the medical criteria, they can continue receiving hospice support. You can learn more about hospice care eligibility. This ensures patients and families receive care for as long as they need it.
At Central Coast VNA & Hospice, our mission is to provide clear answers and compassionate support to guide you through your healthcare journey.
Contact us today to learn more about how we can help your family.
What Is Comfort Care for a Serious Illness?
When a serious illness affects your family, you may hear new terms. One of them is "comfort care." But what does that mean for you and your loved ones?
Comfort care is an approach that focuses on relief from symptoms and stress. The main goal is to improve quality of life for the patient and their family.
Understanding the Purpose of Comfort Care

At its heart, comfort care puts the patient's well-being first in every decision. It is all about making sure a person's final days or months are as peaceful as possible. It supports the entire family with relief, dignity, and peace during a difficult time.
This philosophy is the foundation of the support we provide at Central Coast VNA & Hospice. With over 74 years of dedicated service, we have deep roots helping families in our community. We serve Monterey County, San Benito County, Santa Cruz County, and South Santa Clara County.
The Core Principles of This Approach
The main idea behind comfort care is to treat the whole person, not just the disease. This means looking beyond physical symptoms. We address every need to achieve the best possible quality of life.
Here is a quick breakdown of the core principles of comfort care.
Comfort Care at a Glance
| Core Principle | What It Means for Patients and Families |
|---|---|
| Symptom Management | Our team actively works to relieve pain, shortness of breath, and other symptoms to bring peace and rest. |
| Emotional and Spiritual Support | We provide counseling and spiritual guidance from a Chaplain to help patients and families cope. |
| Family-Centered Focus | We support the entire family with education and resources, recognizing they are a key part of the journey. |
| Dignity and Respect | We honor the patient's wishes and values at every stage, ensuring they remain in control of their care. |
This complete approach is what makes comfort care so meaningful. It shifts the focus from fighting an illness to living life with the best support system. As a local, nonprofit provider, we are committed to the well-being of our community.
The True Goals of a Comfort-Focused Plan

Comfort care is not about passively waiting. It is an active plan with clear and meaningful goals. The first goal is to manage pain and other difficult physical symptoms.
This allows a patient to find true rest and relief. But this compassionate approach goes much deeper than just physical wellness. It also addresses the emotional, spiritual, and practical needs of the patient and their family.
Honoring Wishes and Maximizing Independence
A key principle of comfort care is honoring a person’s wishes and values. Our care team works with the patient and family. We create a plan that reflects what is most important to them.
This often means finding ways to maximize their independence for as long as possible. The plan helps patients keep doing things that bring them joy. This could be spending time with family or listening to music.
Comfort care is not about 'giving up.' It is about choosing to live the remaining time with dignity and peace.
The need for this kind of support is large and growing. According to the World Health Organization, an estimated 56.8 million people need palliative care each year (WHO, 2020). To find out more about this specific type of care, you can explore our guide on what is palliative care.
Providing Comprehensive Emotional Support
Beyond managing physical symptoms, a comfort plan provides emotional support. A serious illness can bring fear and anxiety for everyone involved.
At Central Coast VNA & Hospice, our team includes Medical Social Workers and Chaplains. They provide counseling, spiritual guidance, and a reassuring presence. This support extends to the entire family, helping them navigate this challenging journey.
This dedicated support helps families in Monterey County and nearby areas feel less alone. It ensures they have the resources and compassionate guidance needed to focus on their time together.
Determining When Comfort Care Is the Right Choice

Deciding when to shift from cure-focused treatment to comfort care is a tough conversation. It is a decision rooted in love and compassion.
This type of support is not about giving up. It's about changing the goal. The priority becomes easing symptoms to make sure your loved one is as comfortable as possible.
Think of someone with advanced cancer who finds treatments are no longer effective. Or a person with end-stage heart failure who struggles to breathe. For them, comfort care can be a gift, reducing pain and bringing peace.
- Advanced Cancer: When chemotherapy is no longer the path forward, comfort care steps in to manage pain and nausea.
- End-Stage Heart Failure: Medication adjustments and oxygen therapy can help a patient rest peacefully at home.
- Chronic Obstructive Pulmonary Disease (COPD): Breathing support and relaxation techniques can ease anxiety.
- Dementia: Our team is trained to create a soothing environment with gentle routines that reduce agitation.
Determining Eligibility
The conversation about comfort care often begins with a doctor’s recommendation. This is a sign that the focus should shift to well-being.
Eligibility is not just about a diagnosis. It is about how the condition impacts daily life.
The team at Central Coast VNA & Hospice listens to you and your family. We want to understand your wishes and what your loved one wants. From there, we create a clear, understandable plan for care at home.
Steps to Begin Comfort Care
Getting started is simpler than you might think.
- Talk to your doctor about your goals for care.
- Ask for a referral for comfort-focused support from CCVNA.
- Contact us to set up an assessment with our team.
Our guide on when to call hospice can offer more clarity. Choosing comfort care is a powerful decision that prioritizes peaceful moments.
Meet the Interdisciplinary Comfort Care Team
Great comfort care is a team effort. It takes a group of compassionate professionals working together. At Central Coast VNA & Hospice, we call this the interdisciplinary team.
Each person on this team brings unique skills. This ensures that every part of a patient's well-being is addressed. For families across Monterey County, San Benito County, Santa Cruz County, and South Santa Clara County, this brings peace of mind.
Key Members of Your Support System
The comfort care team provides complete support in the patient's home. Every professional plays a role in creating a personalized care plan.
Here are the experts who may be part of your dedicated team:
- Registered Nurse (RN): The RN is often the main point of contact. They are experts in managing symptoms and medications.
- Hospice Aide: These compassionate professionals provide hands-on personal care. They help with daily activities like bathing and dressing to maintain dignity.
- Medical Social Worker: A Medical Social Worker offers emotional support. They also connect families with community resources.
The strength of the team is its ability to see the whole person, not just the illness. This ensures care is personal, respectful, and centered on what matters most.
Additional Layers of Compassionate Care
Our team also includes members focused on spiritual and emotional well-being. This ensures a truly complete approach to care.
A Chaplain is available to provide non-denominational spiritual support. They offer guidance and a listening ear to patients and families from all backgrounds.
We also have trained volunteers who offer companionship and respite for families. They might read to a patient or simply sit with them, providing a comforting presence.
Together, this team delivers the mission-driven care Central Coast VNA & Hospice has provided for over 74 years. This is part of our Continuum of Care, guiding families from home health to palliative care to hospice.
Comfort Care, Palliative Care, and Hospice Explained
Families often hear the terms “comfort care,” “palliative care,” and “hospice.” This can create confusion during a stressful time.
While they are all connected, they represent different stages of support. Understanding these differences helps you make clear, confident decisions.
Think of comfort care as the guiding philosophy. It is the commitment to relieving symptoms and managing pain. Both palliative care and hospice operate under this same principle.
Palliative Care: An Extra Layer of Support
Palliative care is a specialized type of comfort care. It can begin at any point during a serious illness, even right after diagnosis. A patient can receive palliative support while still pursuing treatments to cure their illness.
The main goal is to provide relief from symptoms and stress. This improves daily life for both the patient and their family.
For instance, someone getting chemotherapy might receive palliative care to help with nausea. You can learn more about our palliative home care services to see how this works at home.
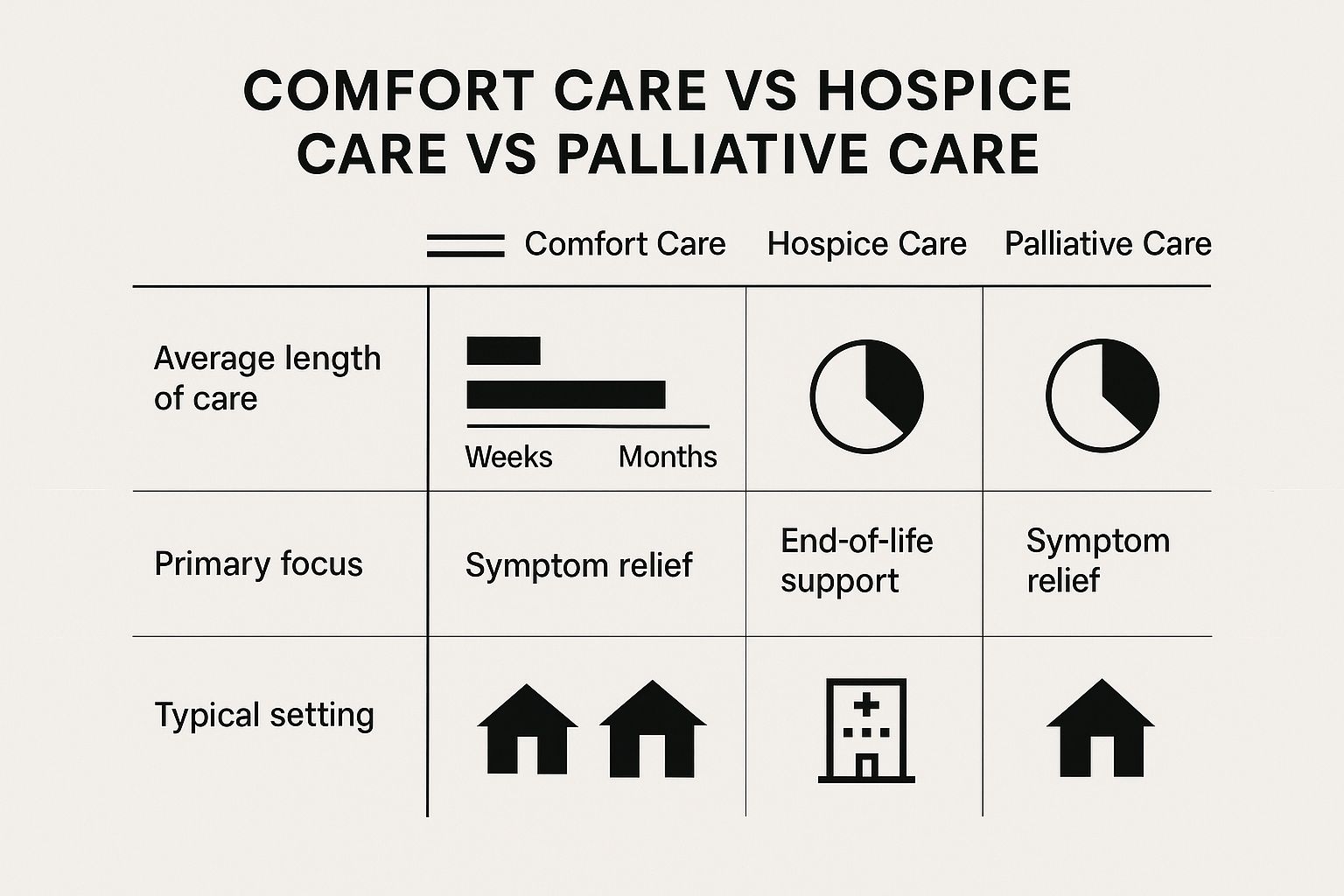

Hospice Care: Comfort for the Final Chapter
Hospice is a type of comfort care for people with a life expectancy of six months or less. It is for those no longer seeking curative treatments. The focus shifts entirely to maximizing comfort, peace, and dignity.
The hospice team provides expert medical, emotional, and spiritual care. It is tailored to the patient's end-of-life wishes.
Comparing Care Options
To make these differences clearer, let's break them down side-by-side.
| Feature | Palliative Care | Hospice Care |
|---|---|---|
| When It Starts | At any stage of a serious illness, from diagnosis onward. | When life expectancy is six months or less. |
| Treatment Goals | Can be provided alongside curative treatments. | Focus is on comfort and quality of life, not curing the disease. |
| Who It's For | Patients with a serious or chronic illness. | Patients with a terminal illness who have stopped curative treatments. |
| Duration | Can last for months or years. | Limited to the final months of life. |
The main difference is timing and treatment goals. At Central Coast VNA & Hospice, our mission is to provide the right care at the right time. Our Continuum of Care ensures a seamless transition for families as their needs change.
How to Access Comfort Care on the Central Coast
Figuring out the next steps can feel overwhelming, but you are not alone. Getting started with comfort care on the Central Coast is often simpler than people think. It begins with a conversation.
The process often starts with your primary care doctor or a specialist. They can provide a referral for our services when the time is right.
Starting the Conversation
You do not have to wait for a referral. You can always reach out to Central Coast VNA & Hospice directly. Our team is here to listen and answer your questions.
Taking this first step gives you the information and support you need. For families across Monterey, San Benito, Santa Cruz, and South Santa Clara counties, our team is a trusted local resource. With over 74 years of nonprofit service, our commitment to our neighbors runs deep.
Contact us today to learn how our comfort care can support your family. Our team can also tell you about our other programs, like our skilled home health care services. We are here to help you navigate your healthcare journey.
Frequently Asked Questions About Comfort Care
Here are answers to some of the most common questions we hear from families. We hope these clear answers bring you peace of mind.
Does choosing comfort care mean we are giving up?
No, not at all. Choosing comfort care is an active decision to shift the focus from trying to cure an illness. The goal becomes making sure the time you have left is as comfortable and meaningful as possible.
Where is comfort care provided?
Most of the time, comfort care is provided where the patient calls home. At Central Coast VNA & Hospice, we bring expert support directly to our patients. This can be a private home, assisted living community, or skilled nursing facility in our service areas.
Is comfort care covered by insurance?
In most cases, yes. When comfort care is provided through a hospice benefit, it is typically 100% covered by Medicare, Medi-Cal, and most private insurance plans. As a nonprofit, we are committed to helping families access the care they need. We can help you understand your benefits and provide more details in our guide on how to pay for hospice care.
How long can someone receive comfort care?
It depends on the patient's needs. Palliative care can be provided for years while a patient continues other treatments. Hospice care is for those with a life expectancy of six months or less, but services can continue as long as the patient is medically eligible.
How does comfort care support the family?
Comfort care is a family-centered approach. Our team provides emotional and spiritual counseling, education, and practical guidance. We also offer bereavement support for up to 13 months to help families heal.
What is the service area for Central Coast VNA & Hospice?
We proudly serve families throughout Monterey County, San Benito County, Santa Cruz County, and South Santa Clara County. Our deep local roots mean we understand the needs of our community.
If you have more questions or want to discuss your family’s needs, our compassionate team is here to listen. Call Central Coast VNA & Hospice today at (831) 372-6668 or visit us online at https://ccvna.com to learn more.
A Guide to In Home Hospice Care for Your Family
When a loved one faces a serious illness, the path forward can feel uncertain. This is where in home hospice care can help. It is a special kind of support that focuses on comfort, dignity, and quality of life.
This care happens in the peaceful, familiar setting of a person's own home. They are surrounded by the people and memories they cherish most. It is not about giving up, but about living the time that remains as fully as possible.
What In Home Hospice Care Truly Means

Hospice is not a place; it is a philosophy of care. It supports the whole person by addressing physical, emotional, and spiritual needs. This approach allows patients to live their final months with peace and respect.
At Central Coast VNA & Hospice, we have provided this support for over 74 years. We serve families in Monterey County, San Benito County, Santa Cruz County, and South Santa Clara County. As a nonprofit organization, our care is always centered on the patient’s wishes.
A Team Approach to Comfort
A key part of in home hospice is the dedicated team that supports the patient and family. This team works together to create a personal care plan. The plan honors the patient’s goals.
Our team includes:
- Registered Nurses who are experts in managing pain and other symptoms.
- Hospice Aides who help with personal care, like bathing and dressing, with great gentleness.
- Medical Social Workers who provide emotional support and connect families with community resources.
- Chaplains who offer spiritual guidance for people of all faiths and backgrounds.
This compassionate, team-based care is highly valued. According to the National Hospice and Palliative Care Organization (NHPCO), over 1.72 million Medicare beneficiaries received hospice services in 2020 (NHPCO, 2021). This shows how many families choose comfort-focused care.
Choosing hospice means choosing to focus on living. For a deeper look into the core principles of this care, you can read our guide on what is hospice care.
The Core Benefits of Choosing Hospice at Home
Deciding on in home hospice care means putting comfort and quality of life first. The biggest benefit is being at home, surrounded by familiar sights and sounds. This creates a sense of security during an uncertain time.
Being at home helps patients stay connected to family, friends, and pets. This can ease feelings of loneliness or anxiety. It also allows them to keep their own routines, giving them more control.
Personalized Care and Family Support
A major benefit of in home hospice is that the care plan is built around the individual. The hospice team works closely with the patient and family. They listen to understand specific needs and wishes.
With over 74 years of nonprofit service, Central Coast VNA & Hospice deeply understands our local communities. Our teams are committed to this personalized model of care. We serve Monterey County, San Benito County, Santa Cruz County, and South Santa Clara County.
Our support also extends to the entire family. We know that caring for a loved one is emotionally and physically difficult. Our hospice services include support systems to help families.
This includes:
- Emotional and Spiritual Counseling: Our Medical Social Workers and Chaplains offer guidance for patients and their loved ones.
- Respite for Family Members: We provide short-term relief for family members, giving them a chance to rest.
- Bereavement Support: Our support continues after a loved one passes. We offer grief support to help families through the healing process.
A Focus on Quality of Life
The goal of hospice at home is to improve the quality of the time that remains. The focus shifts from curing the illness to managing symptoms like pain. This ensures the patient is as comfortable as possible.
This approach is similar to palliative care, which also aims to improve well-being. By managing symptoms well, in home hospice helps patients live more fully. They can create meaningful memories in a loving environment.
This holistic approach is what makes hospice a uniquely compassionate choice. For families exploring options earlier in an illness, you can learn more about our palliative home care services. Our continuum of care ensures you have the right support at the right time.
Who Is Eligible for In Home Hospice Care

Knowing when it is time for in home hospice care can feel difficult. However, the guidelines are clear and compassionate. Hospice is for anyone with a serious illness who has chosen to focus on comfort instead of curative treatments.
The main requirement is a doctor's certification. A doctor must state that the patient likely has six months or less to live if the illness runs its natural course. It is important to know this is not a strict deadline.
Many people receive hospice care for longer than six months. They can continue with the service as long as a physician recertifies their eligibility. The focus is always on the patient's current needs.
The Admission Process
Getting started is a simple process. It usually begins with a referral from a physician. This leads to a meeting with a hospice provider like Central Coast VNA & Hospice.
Our team will meet with you and your family to discuss your needs. We will answer all your questions and confirm eligibility. Once admitted, a person can receive care for as long as they meet the criteria.
It is also important to remember that hospice is not a permanent decision. A person can stop hospice services at any time. This may happen if their condition improves or if they want to try curative treatments again.
The decision to begin hospice is personal. It always centers on the patient's wishes. It is about making sure their final chapter is lived with dignity and peace.
As a nonprofit, our mission is to empower families in our community. We serve Monterey County, San Benito County, Santa Cruz County, and South Santa Clara County. Understanding the process helps you make choices that honor your loved one. For a detailed breakdown of the requirements, please read our guide on hospice care eligibility.
The Compassionate Care Team Supporting Your Family
Choosing in home hospice care means you are never alone. A dedicated team of professionals from Central Coast VNA & Hospice provides a circle of support. This team approach nurtures your loved one's physical, emotional, and spiritual well-being.
Each team member brings a unique skill. They all share one common goal: to honor the patient’s wishes and improve their quality of life. This team becomes a trusted partner on your journey.
Your Core Support System
The strength of hospice is in its team-based structure. Your loved one's primary doctor is still involved. A specialized group of experts also steps in to manage daily needs.
Let's meet the core members of your support system.
The Roles of Your In Home Hospice Care Team
This table explains the main duties of the professionals who will support you.
| Team Member | Primary Responsibilities |
|---|---|
| Registered Nurse (RN) | The RN is an expert in pain and symptom management. They make regular visits to assess the patient, adjust medications for comfort, and teach the family how to provide care. |
| Hospice Aide | Provides gentle, hands-on help with personal care, such as bathing and dressing. This support is always delivered with respect for the patient’s dignity. |
| Medical Social Worker | Helps with emotional and practical challenges. They offer counseling, support, and connect families with community resources to ease burdens. |
| Chaplain | Provides non-denominational spiritual guidance to patients and families. They respect all beliefs and offer a compassionate presence during a personal time. |
Together, these professionals make sure care is complete. It is centered around the patient's and family's needs.
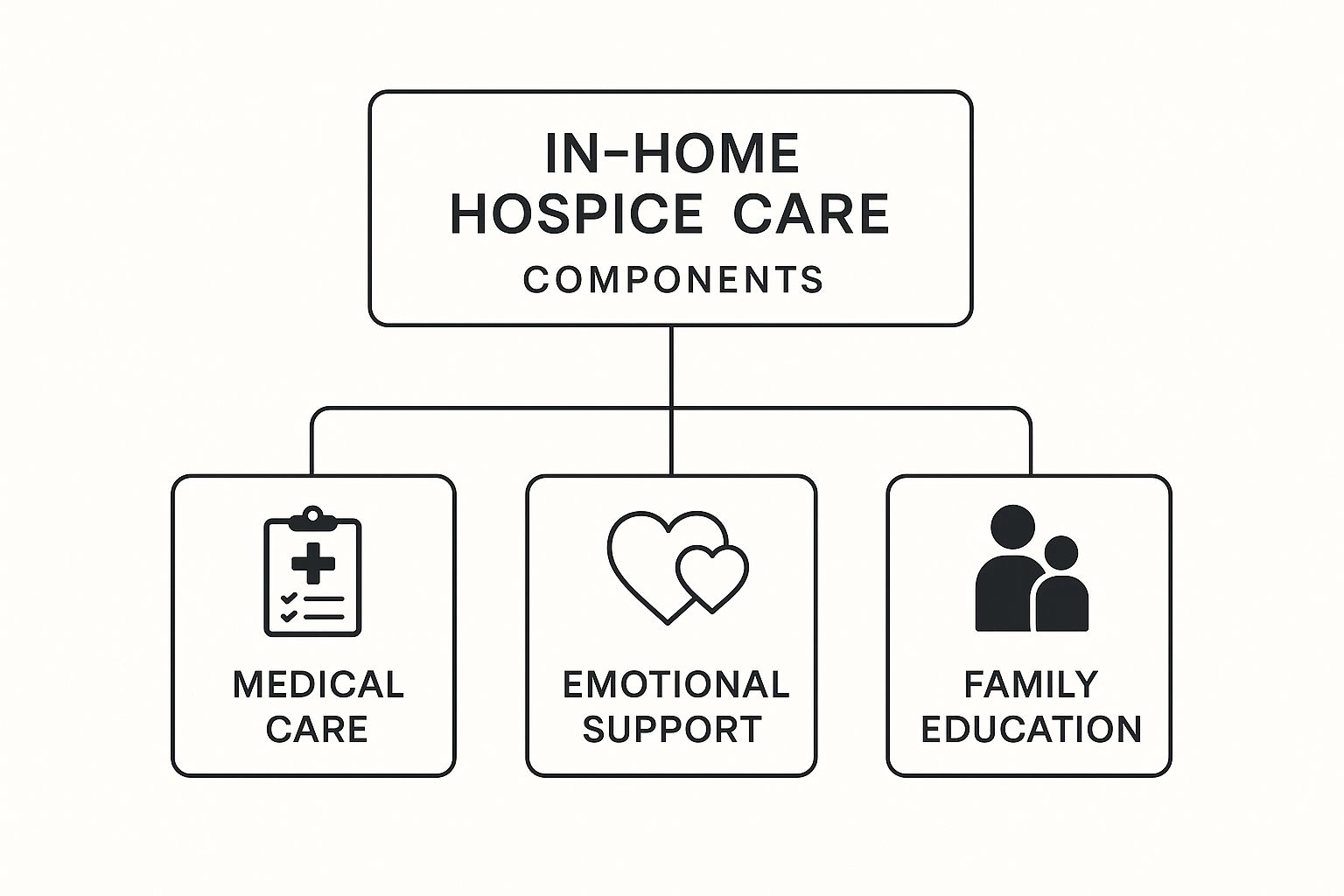
A Mission of Compassionate Care
As a nonprofit organization with over 74 years of service, our mission is rooted in the community. Our local teams in Monterey County, San Benito County, Santa Cruz County, and South Santa Clara County are your neighbors. They are dedicated to delivering care with genuine warmth.
The hospice team ensures the care plan is a living guide. It adapts to the changing needs of the patient and family. This creates a supportive experience for everyone.
This unified approach is what makes in home hospice care so effective. Our promise is that your family will be supported by experts. We are committed to making this time as peaceful and meaningful as possible.
Understanding Hospice Care Coverage and Costs
When you consider in home hospice care, you should not have to worry about the cost. The good news is that this support is designed to be affordable. For most families, hospice is fully covered with no out-of-pocket expenses.
The majority of hospice services are paid for by Medicare Part A. This includes a comprehensive hospice benefit. Medi-Cal and most private insurance plans typically offer the same level of coverage.
What Is Included in the Hospice Benefit
The hospice benefit covers almost everything needed to manage the patient’s comfort at home.
This typically includes:
- Nursing and Physician Services: Regular visits from your Registered Nurse and medical guidance.
- Hospice Aide Services: Gentle help with personal care like bathing and dressing.
- All Medical Equipment: Items like a hospital bed or oxygen are delivered to your home.
- Medical Supplies: This covers wound care supplies, catheters, and other essentials.
- Medications: All prescriptions for managing pain and symptoms are included.
- Counseling and Support: Emotional and spiritual support for both the patient and the family.
This broad coverage allows families to focus on spending meaningful time together. You can do so without the worry of growing medical bills.
At Central Coast VNA & Hospice, our team is here to help you understand your coverage. We work directly with Medicare, Medi-Cal, and private insurance plans. For a deeper dive, you can learn more about how to pay for hospice care.
Contact us today to discuss your insurance plan and get answers to your financial questions. Our mission is to provide compassionate, accessible care to everyone in Monterey, San Benito, Santa Cruz, and South Santa Clara counties.
Choosing the Right Hospice Provider on the Central Coast

Picking a provider for in home hospice care is a very important decision. You are looking for a partner who is compassionate and shares your values. The right fit makes all the difference for your loved one's quality of life.
When looking at your options, it is important to ask thoughtful questions. A good provider will welcome your questions and give clear answers. This is the first step in building a trusting relationship.
Key Questions to Ask Potential Providers
Here are a few things to ask to find the best support for your family.
- Accreditation and Licensing: Is your agency licensed by the state and accredited by a national organization? This shows they meet high standards for quality and safety.
- Staffing and Support: What is the average number of patients for your Registered Nurses? What happens after hours or on holidays? You need to know support is always available.
- Continuum of Care: Do you offer other services, like home health and palliative care? This can make transitions smoother if needs change.
Choosing a nonprofit provider like Central Coast VNA & Hospice means choosing a mission of care, not profit. With over 74 years of local service, our focus is entirely on the patient and family.
Our deep roots in the Central Coast make us a trusted choice for families. Our patients often move smoothly from our home health or palliative programs into hospice. They are guided by a familiar and trusted team.
We invite you to learn more about our specific hospice care services and compassionate approach. Contact us today for a no-obligation consultation to discuss how we can support your family.
Frequently Asked Questions About In Home Hospice Care
Here are answers to some common questions we hear from families in Monterey, San Benito, Santa Cruz, and South Santa Clara counties.
1. What is the difference between palliative care and hospice care?
Palliative care can begin at any stage of a serious illness and can be provided along with curative treatment. Hospice care is for patients who have a life expectancy of six months or less and are no longer seeking a cure. Both focus on providing comfort and improving quality of life.
2. Does choosing hospice mean giving up hope?
Not at all. Choosing hospice is about redefining hope. The hope for a cure shifts to hope for comfort, peace, and quality time with loved ones. It is a choice to focus on living the remaining time with dignity.
3. How often will the hospice team visit?
The number of visits is based on the patient's personalized care plan. A Registered Nurse may visit a few times a week, while a Hospice Aide may visit more often. Other team members, like a Chaplain or Medical Social Worker, visit as needed.
4. What happens if there is an emergency at night?
Central Coast VNA & Hospice provides 24/7 on-call support. You can call our dedicated line anytime to speak with a Registered Nurse. The nurse can provide guidance over the phone or make a visit if needed, helping you avoid trips to the emergency room.
5. Can a patient stop hospice care once it starts?
Yes. A patient can leave hospice care at any time and for any reason. If their condition improves or they decide to seek curative treatment, they can stop services. They can re-enroll later if they meet the eligibility criteria again.
At Central Coast VNA & Hospice, we are committed to providing compassionate answers and expert care to families across Monterey, San Benito, Santa Cruz, and South Santa Clara counties. Contact us today to learn more about our services at https://ccvna.com.
Finding Palliative Care Near Me on the Central Coast
When you search for "palliative care near me," you are looking for a special kind of medical support. This care is designed to improve your quality of life while you manage a serious illness. It is an extra layer of care that works with your current treatments to relieve symptoms, pain, and stress.
Here on California’s Central Coast, Central Coast VNA & Hospice provides this compassionate support right in your home.
What Is Palliative Care and How Does It Help?

Palliative care is a special type of medical care for people with serious illnesses. Its main goal is to provide relief from symptoms and stress. It helps improve the quality of life for both you and your family.
This care is helpful for any age and at any stage of a serious illness. You can receive it at the same time as treatments meant to cure you. Palliative care is not the same as hospice care; it is an extra layer of support to help you live more comfortably.
How Does This Care Work?
A dedicated team works together with your doctors. This team includes a Registered Nurse, a Social Worker, and a Chaplain. They focus on the whole person, addressing physical, emotional, and spiritual needs.
This team approach ensures your care plan matches your personal goals. The need for this support is growing. According to the National Hospice and Palliative Care Organization (NHPCO), an estimated 12 million adults in the U.S. could benefit from palliative care (NHPCO, 2019).
Palliative care helps you regain a sense of control. It’s about living as fully as possible by managing symptoms, communicating clearly, and ensuring your treatment choices reflect what matters most to you.
Your Local Nonprofit Partner
For over 74 years, Central Coast VNA & Hospice has been the trusted nonprofit provider of home-based care. As a mission-driven organization, we serve families in Monterey County, San Benito County, Santa Cruz County, and South Santa Clara County.
We offer a full continuum of care, from home health to hospice. Our palliative care services bring comfort and expert medical management to your home.
The Benefits of Receiving Palliative Care at Home
Being in your own home provides a deep sense of comfort. When you are managing a serious illness, this feeling is more important than ever. Staying home helps you keep a sense of normalcy and independence.
That is why Central Coast VNA & Hospice brings expert palliative care to you. This support is built around your unique needs. Our goal is to help you live as well as possible, with dignity and peace.
This care focuses on three key areas. It relieves physical symptoms, gives emotional support, and improves your overall quality of life.
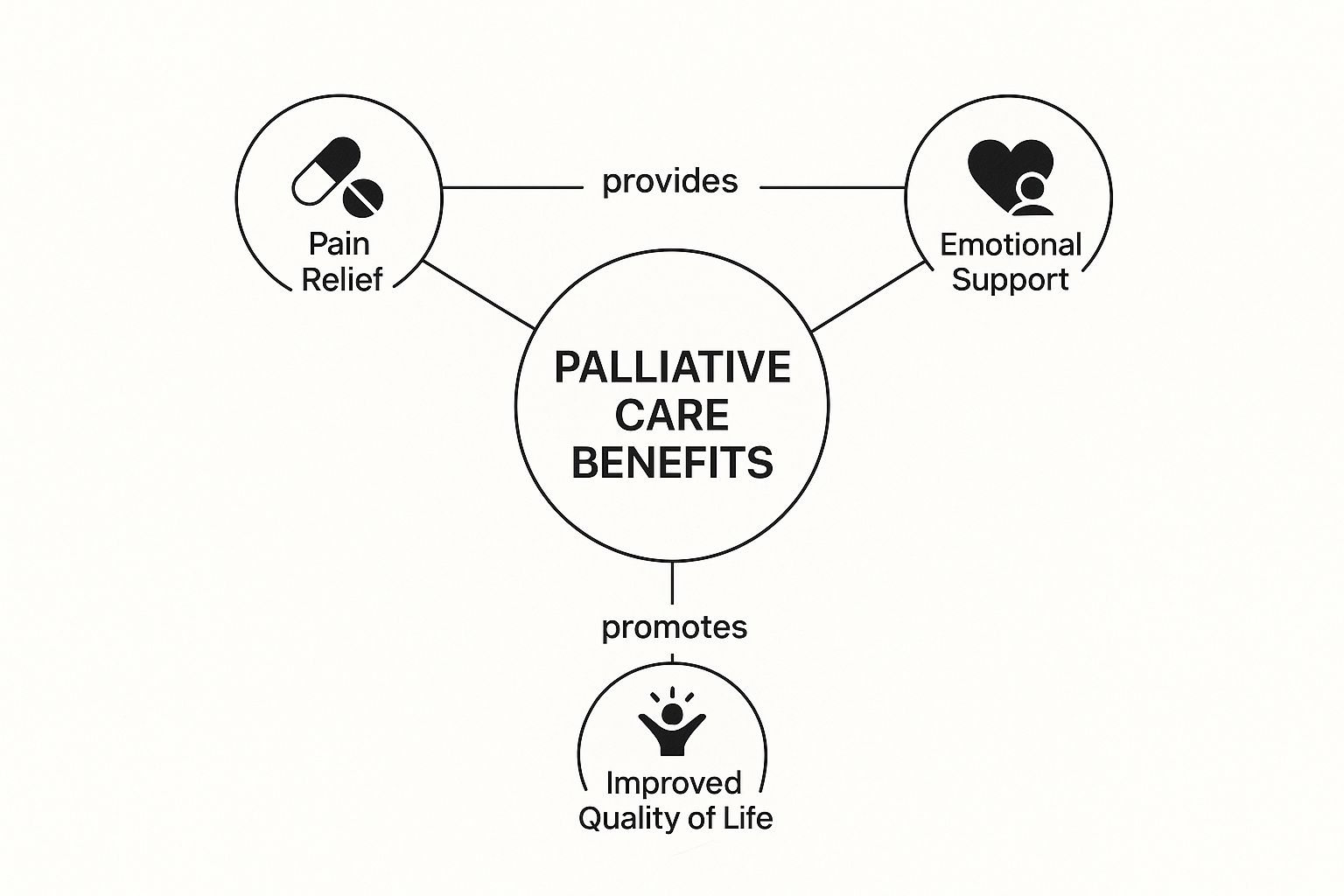
These elements work together to create a strong foundation of support. This benefits both patients and their families.
Comprehensive Symptom Management
A big advantage of in-home palliative care is having experts manage your symptoms. Serious illnesses often cause pain, fatigue, nausea, or shortness of breath. Managing these alone can be overwhelming.
Our team works with you and your doctors to address these issues. A Registered Nurse assesses your needs and creates a personalized plan. This allows you to focus more on your daily life and loved ones.
Emotional and Spiritual Guidance
A serious illness affects more than just the body. When families look for "palliative care near me," they often want support for the whole person. Our team includes Social Workers and Chaplains who provide guidance for you and your loved ones.
Palliative care is about treating the whole person—not just the illness. It focuses on providing comfort, supporting your goals, and ensuring you feel heard and respected throughout your healthcare journey.
This support helps you navigate feelings of anxiety or fear. It also creates a safe space for families to talk and find strength together.
Better Communication and Coordination
Our team acts as a central hub for communication. We connect you, your family, and all your doctors. This ensures everyone is on the same page about your care plan.
This coordinated approach is very helpful for families across Monterey County, San Benito County, Santa Cruz County, and South Santa Clara County. We are your local, nonprofit partner, deeply committed to providing seamless and compassionate care.
Understanding Who Is Eligible for Palliative Care
Many people think palliative care is only for someone at the very end of life. That is not true. Eligibility is much broader and is based on a person's need for support.
The right question is not, "How long does someone have left?" Instead, it is, "Could this person benefit from better symptom management and support?" If the answer is yes, palliative care is likely a good fit.
Who Benefits from Palliative Care
This specialized care helps people manage long-term health conditions. It brings relief and improves daily life for anyone dealing with a difficult illness.
Some common conditions that benefit from palliative care include:
- Cancer: To help manage side effects from treatments like chemotherapy.
- Heart Conditions: For issues like congestive heart failure (CHF).
- Lung Diseases: Including Chronic Obstructive Pulmonary Disease (COPD).
- Neurological Conditions: Such as Alzheimer’s, dementia, or Parkinson’s disease.
- Kidney or Liver Disease: Helping manage difficult symptoms.
Starting the Conversation
Bringing up palliative care with your doctor is a great step toward a better quality of life. The need for this support is growing. Globally, over 40 million people require palliative care each year, but only a small number receive it.
It's also important to know that palliative care and hospice are different. You can learn more in our guide on the differences between palliative vs hospice care. The key is that palliative support is available at any point during a serious illness.
The focus of palliative care is always on the patient. It's about empowering you to live more comfortably by managing symptoms, reducing stress, and aligning your medical care with your personal goals.
Our team at Central Coast VNA & Hospice is here to help you navigate these talks. We work with you and your doctor to see if our services are the right fit. Contact us to learn more about how we can support you.
Your Local Palliative Care Provider on the Central Coast

When you look for "palliative care near me," you want a trusted partner who knows your community. For families on the Central Coast, that partner is Central Coast VNA & Hospice. We are part of your community.
For over 74 years, our nonprofit team has provided compassionate medical care in people's homes. Our history is built on trust, skill, and dedication to every family we serve.
Serving Our Central Coast Communities
We are committed to being there for you where you live. Central Coast VNA & Hospice brings skilled support to your doorstep.
Our service areas include:
- Monterey County: From Salinas to the Monterey Peninsula.
- San Benito County: Serving families in Hollister and surrounding areas.
- Santa Cruz County: Ensuring residents get expert palliative care at home.
- South Santa Clara County: Extending our services to southern parts of the county.
This local focus means our team is always nearby. We know the area’s healthcare system and can coordinate care with your local doctors. This creates a smoother, less stressful experience for you.
Our Seamless Continuum of Care
Choosing Central Coast VNA & Hospice gives you an integrated approach to care. We are the only provider on the Central Coast offering a full continuum of home-based services. This includes home health, palliative care, and hospice care.
This means you work with one familiar team as your needs change. A person might start with home health, then move to palliative care for symptom management. If needed, they can later receive hospice support.
Our continuum of care ensures you never have to start over with a new provider. You and your family benefit from consistent, familiar, and compassionate support every step of the way.
Choosing a local provider means choosing a team invested in your health. Contact us today to learn how our dedicated palliative care team can support you.
How Palliative Care Is Covered by Insurance
When dealing with a serious illness, you should not have to worry about paying for care. Many families worry that specialized support like palliative care is too expensive.
The good news is that most insurance plans cover palliative care. It is treated like other medical specialties, such as cardiology or oncology. This makes getting support much simpler.
For most patients, coverage comes from several common sources. This helps remove financial stress so you can focus on your health.
Common Coverage Options
Palliative care is a medical specialty focused on symptom management. It is typically included in your existing health benefits.
Here is how it usually works:
- Medicare Part B: This part of Medicare covers doctor visits and other outpatient services, including palliative care.
- Medi-Cal: California's Medicaid program also covers palliative care for those who qualify.
- Private Insurance: Most private health insurance plans include benefits for palliative care.
The team at Central Coast VNA & Hospice can help you understand your benefits. We can work with your insurance provider to clarify coverage. While palliative and hospice care are different, you can learn more about payment options in our guide on how to pay for hospice care.
Your focus should be on feeling better, not on navigating complex medical bills. Palliative care is a covered medical service designed to be accessible when you need it most.
As your nonprofit provider, Central Coast VNA & Hospice is committed to making our services accessible. We serve everyone in Monterey, San Benito, Santa Cruz, and South Santa Clara counties. Our team is here to support you.
How to Get Started with Palliative Care

Taking the next step to get extra support should be empowering. Starting palliative care is often simpler than people think. It usually begins with a conversation.
We see this process as a partnership. It is between you, your doctors, and our compassionate team at Central Coast VNA & Hospice. Our goal is to make sure you have everything you need.
Talk to Your Doctor
The most common first step is talking with your doctor. Tell them about your symptoms, like pain or fatigue. Mention that you want to learn more about palliative care.
Your doctor knows your medical history. They can help figure out if this extra support is a good fit for your current treatment plan.
Your voice is the most important one in your healthcare journey. Asking for palliative care is a proactive way to improve your quality of life and ensure your treatment aligns with your personal goals.
The availability of this care can vary. A study found that only 12% of countries have an advanced level of palliative care. This shows how vital it is to have strong, local providers. You can explore more global findings on palliative care development if you are interested.
Contact Us for a Consultation
You do not have to wait for a doctor's referral to get answers. You can contact Central Coast VNA & Hospice directly for a consultation. Our team is ready to listen to your needs and explain how our services can help.
We will walk you through the process and answer your questions. We also help coordinate everything with your doctors. As your nonprofit partner in Monterey, San Benito, Santa Cruz, and South Santa Clara counties, we are here to support you.
Contact us today to learn more about our compassionate palliative care services.
Frequently Asked Questions About Palliative Care
It is normal to have questions when you first learn about palliative care. Let's review some common ones to help you feel more confident about this type of support.
1. Is palliative care only for people who are dying?
No, this is a common myth. Palliative care is for anyone at any age and at any stage of a serious illness. The goal is to improve your quality of life now by managing symptoms and stress.
2. Can I still try to cure my illness with palliative care?
Yes. Palliative care works with your curative treatments, not in place of them. It provides an extra layer of support to help you manage side effects from treatments like chemotherapy.
3. Will I have to give up my own doctor?
No. Your palliative care team joins your existing healthcare team. They work alongside your primary doctor and specialists to coordinate care and ensure everyone is focused on your goals.
4. What does the palliative care team do?
A palliative care team includes professionals like a Registered Nurse, a Social Worker, and a Chaplain. They focus on managing symptoms like pain and fatigue, providing emotional support for you and your family, and coordinating care between all your doctors.
5. Who is on the palliative care team?
Our team includes a Registered Nurse, Medical Social Worker, and Chaplain who work under the supervision of a physician. This team works together to address your physical, emotional, and spiritual needs, providing whole-person care.
The team at Central Coast VNA & Hospice is here to answer your questions and help you figure out if palliative care is the right fit. Get in touch with us today to learn more about our compassionate services. https://ccvna.com
Understanding Your Hospice Care Options
When a family chooses hospice care, they are picking a path that focuses on comfort, dignity, and quality of life. It is important to know that there isn't just one type of hospice care. There are several hospice care options to fit your family's needs.
Understanding the Different Hospice Care Options
Choosing hospice is a big decision, but it opens up many supportive care choices. This care meets your loved one where they are. The focus is on managing symptoms and giving emotional support to the whole family.
At Central Coast VNA & Hospice, we have guided families through these choices for over 74 years. We are a nonprofit provider serving Monterey County, San Benito County, Santa Cruz County, and South Santa Clara County. Our team is here to help create a care plan that honors your loved one’s wishes. To better understand the language used, a medical terminology study guide can be a helpful resource.
The Four Levels of Hospice Care
Hospice care has four main levels. This structure ensures support can change as a person's condition changes. Knowing the difference between them is the first step in making an informed choice. You can learn more about what hospice care is in our detailed guide.
This image helps show the different settings and types of care available.
Each level serves a clear purpose, creating a flexible system for end-of-life care. This patient-first approach is becoming more common. In fact, the hospice care market is projected to reach USD 9.12 billion by 2032, as more families seek comfort-focused services.
Here is a simple breakdown to help you compare the different hospice options.
At-a-Glance Overview of Hospice Care Options
| Care Option | Primary Location | Best For |
|---|---|---|
| Routine Home Care | Patient's home, assisted living, nursing home | Stable symptoms managed with regular visits |
| Continuous Home Care | Patient's home | Short-term symptom crises needing intensive support |
| General Inpatient Care | Hospice facility, hospital, skilled nursing facility | Acute symptoms that cannot be managed at home |
| Respite Care | Hospice facility, hospital, skilled nursing facility | Providing a short-term break for family caregivers |
This table is a starting point. Let’s look at each level so you have a complete picture.
Finding Comfort at Home with Routine Hospice Care
Most people picture being in a familiar space when they think about end-of-life care. That is what Routine Home Care provides. It is the most common level of hospice because it brings support directly to your loved one.
This care can be provided in their own house, an apartment, an assisted living community, or a nursing home.
Staying in a familiar environment makes a big difference. It helps your loved one keep a sense of normalcy during a time of uncertainty.
The numbers support this choice. According to the National Hospice and Palliative Care Organization (NHPCO), over 1.72 million Medicare beneficiaries received hospice services in 2020 (NHPCO, 2021). This shows more families are choosing care that puts comfort first.
What Does Routine Home Care Involve?
With Routine Home Care, you get a whole team of specialists from Central Coast VNA & Hospice who visit regularly. This team works together to care for your loved one's physical, emotional, and spiritual well-being.
Think of it as a support system that comes to your door. No more stressful trips to appointments; the experts come to you.
Your family’s dedicated care team includes several professionals:
- Registered Nurse: This person is your main contact for medical needs. They manage pain, handle medications, and oversee the care plan.
- Hospice Aide: These team members help with personal tasks like bathing and dressing. This helps preserve dignity and comfort.
- Medical Social Worker: They provide emotional support for the patient and family. They can also connect you with community resources.
- Chaplain: A chaplain offers spiritual guidance that respects your family’s beliefs. They provide a source of comfort and peace.
This team approach empowers families throughout Monterey County to be partners in care. You get expert guidance, but you and your loved one are always at the center of every decision.
A Focus on Quality of Life
The goal of Routine Home Care is to manage symptoms and improve quality of life. This means looking beyond physical pain to address emotional and spiritual needs. The focus is on making each day as comfortable and meaningful as possible.
This level of care is a great fit for anyone whose symptoms are stable. For those still seeking treatment for a serious illness but needing symptom help, exploring palliative home care services may be a better option.
By bringing care into the home, Central Coast VNA & Hospice helps preserve a sense of independence and peace for patients. This model allows them to spend precious time with family in a setting that feels safe and secure.
Navigating Acute Symptoms with Inpatient Hospice Care
Most hospice care happens at home. However, sometimes symptoms like severe pain become too much for the family to manage. This is where General Inpatient Care (GIP) can help.
GIP is a short-term, intensive level of care. It focuses on getting severe symptoms under control. It can take place in a hospice facility, a hospital, or a skilled nursing facility with 24/7 care. The goal is always to provide immediate medical attention to stabilize the situation.
It is important to know that GIP is not a permanent move. Once the patient's condition is stable, the plan is to get them back to the comfort of their home. We at Central Coast VNA & Hospice coordinate this process to ensure your loved one gets the right care at the right time.
When Is Inpatient Care Necessary?
The decision to move to inpatient care is made together by the patient, family, and hospice team. This level of care is for times when symptoms are too much for a home environment. It is a better alternative to a stressful trip to the emergency room.
Common reasons for General Inpatient Care include:
- Uncontrolled Pain: When pain is not responding to the current medication plan at home.
- Acute Respiratory Distress: Sudden breathing problems that need constant medical supervision.
- Severe Nausea and Vomiting: Symptoms that can't be managed with at-home treatments.
- Sudden Decline in Condition: An abrupt change in health that requires skilled nursing assessment.
The main purpose of inpatient hospice care is to manage severe symptoms. As soon as the crisis is resolved, the team plans for a safe and comfortable return home.
At Central Coast VNA & Hospice, our team has supported families across Monterey, San Benito, and Santa Cruz counties through these difficult moments. We make sure every decision is guided by compassion and respect for the patient's wishes.
Managing a Crisis at Home with Continuous Care
Most people want to stay home when facing a serious illness. But sometimes, a medical crisis can happen unexpectedly. Symptoms can suddenly become overwhelming.
This is why Continuous Home Care (CHC) exists. It is a special, intensive level of hospice support. It helps avoid a stressful trip to the hospital.
Think of it as bringing the hospital's focused attention to the patient's bedside for a short time. The goal is to manage a brief crisis and get symptoms under control. Then, the patient can return to their normal hospice routine.
What Qualifies as a Crisis?
Continuous Home Care is a short-term solution. It is used when a patient's symptoms flare up so much that regular visits are not enough. It is a powerful tool that helps us honor a person's wish to stay at home.
This intensive support is for situations like:
- Uncontrolled pain that is not responding to the current medication plan.
- Severe nausea and vomiting that will not stop, despite regular treatment.
- Acute respiratory distress, which can cause shortness of breath or anxiety.
- Sudden, severe agitation that needs frequent care to keep the patient safe.
Bringing this level of clinical expertise into the home means we can often get a crisis under control without a disruptive hospital stay. This preserves a sense of peace for both the patient and their family.
How Continuous Care Works
When a crisis occurs, the care plan changes. The focus shifts to providing constant medical oversight in the home.
A Registered Nurse or Hospice Aide from the Central Coast VNA & Hospice team can be in the home for at least eight hours a day. Sometimes, care can be provided up to 24 hours, depending on the patient's needs. For families, this continuous presence brings great relief.
During this time, our clinical team focuses on a few key things:
- Administering Medications: The nurse gives medications as needed to get symptoms under control fast.
- Monitoring Symptoms: With constant observation, the team can see how the patient is responding and make adjustments.
- Providing Personal Care: A Hospice Aide can handle comfort measures to keep the patient feeling clean and dignified.
- Supporting the Family: Having a calm, experienced professional in the house offers reassurance to a family during a stressful time.
This intensive support means we can manage an acute situation in the familiar setting of home. For families in Monterey County, San Benito County, and our other service areas, this brings peace of mind.
Supporting the Family with Respite Care
Caring for a seriously ill loved one is an act of devotion. But it can also be exhausting. Hospice care is designed to support the entire family, not just the patient.
One valuable resource is Respite Care. Think of it as a planned, temporary break for the primary caregiver. It is a healthy way to prevent burnout so you can continue to provide the best support.
How Respite Care Works
Respite care gives you a short break by admitting your loved one into an approved inpatient setting. This break can last for up to five days at a time. The setting could be a hospice facility, a hospital, or a skilled nursing facility.
During this time, a professional team looks after the patient around the clock. This gives you a chance to rest, run errands, or simply catch your breath. You can relax, knowing your family member is safe and receiving compassionate care.
Here at Central Coast VNA & Hospice, we coordinate everything for families in Monterey, San Benito, and our other service areas. You can learn more about our hospice care in Monterey on our website.
Respite care is built on a simple idea: caregivers need care, too. It is an essential part of a compassionate hospice plan.
This focus on the family is central to modern healthcare. The global hospice market is expected to hit roughly USD 5.33 billion by 2025, driven by this holistic approach. You can explore more on this market growth to see how the industry is changing.
The Importance of Emotional Support
The emotional journey can be the hardest part. That's why quality hospice programs include emotional and spiritual support for everyone.
To make sure this support is effective, care teams need to document conversations accurately. Specialized tools like therapy and counseling transcription can be helpful for keeping detailed, confidential records. This commitment to emotional well-being is a core part of comprehensive hospice support.
How to Choose the Right Hospice Option
Figuring out the best path forward can feel overwhelming. The most important thing to remember is that this is not a final decision. It’s a conversation that puts your loved one’s comfort and wishes first.
This is a team effort. The patient, family, and hospice team work together to balance medical needs with personal preferences. Hospice care is designed to adapt as needs change.
Key Questions to Guide Your Decision
To bring clarity to the conversation, it helps to talk through a few key points as a family. Answering these questions can point you toward the best hospice option right now.
- What does my loved one want most? Is staying at home the top priority? Or is the main goal to get a specific symptom, like pain, under control?
- What are the immediate medical needs? Are symptoms stable and manageable with regular nursing visits? Or are you in a crisis that needs constant attention?
- What can our family realistically handle? Are there family members who can provide daily care? Does the primary caregiver need a break to avoid burnout?
You do not have to figure this all out on your own. A talk with an experienced hospice provider can help you sort through these factors and design a plan that honors your loved one.
The level of hospice support can and often does change. For example, someone on Routine Home Care might need a brief stay at an inpatient facility. Once they are stable, they can go right back home.
For families in Monterey, San Benito, Santa Cruz, and South Santa Clara counties, the team at Central Coast VNA & Hospice is here to help. We can also walk you through how to pay for hospice so you have all the information you need.
Frequently Asked Questions About Hospice Care Options
It's normal to have questions when thinking about hospice. This is new for most families. Let's walk through some common concerns.
How do we pay for hospice care?
Most people are surprised to learn that hospice is widely covered. Medicare, Medi-Cal, the VA, and most private insurance plans include a hospice benefit. As a nonprofit, Central Coast VNA & Hospice provides care to everyone who is eligible, regardless of their ability to pay.
Can we change the level of care if needed?
Yes, absolutely. Hospice is designed to adapt to your loved one’s changing needs. A patient comfortable at home with Routine Care might need a short inpatient stay for symptom management before returning home.
Who is on the hospice team?
Hospice is a team effort. Your dedicated team will include a physician, a Registered Nurse case manager, a Hospice Aide, a Medical Social Worker, and a Chaplain. Everyone works together to provide complete physical, emotional, and spiritual comfort.
How do we know when it's the right time?
This is one of the toughest questions a family faces. Generally, it’s time to explore hospice when the goal of treatment shifts from a cure toward comfort and quality of life. We've put together a guide on identifying the right time for hospice to help.
Does choosing hospice mean we're giving up?
No, it is the opposite. Choosing hospice is an act of love to redefine hope. It means focusing all your energy on what matters most: living the time that remains as fully and comfortably as possible.
What areas does Central Coast VNA & Hospice serve?
Our nonprofit has deep local roots. We are proud to provide compassionate care across Monterey County, San Benito County, Santa Cruz County, and South Santa Clara County.
Navigating these choices can feel overwhelming, but you don't have to do it alone. The compassionate team at Central Coast VNA & Hospice has been guiding families on the Central Coast for over 74 years. Our nonprofit, mission-driven approach ensures every patient receives dignified care.
Contact us today to learn more about our hospice care options.
A Guide to Medication Management for Elderly Loved Ones
Managing medications for an elderly loved one can feel like a full-time job. It is often confusing, stressful, and loaded with worry. Getting it right is one of the most important things you can do for their health. Good medication management for elderly loved ones prevents dangerous errors and harmful drug interactions. It also makes sure they get the best results from their treatment.
This process involves organizing prescriptions and understanding dosages. It also means keeping an open line of communication with their doctors.
Why Safe Medication Management Is Essential
Many older adults juggle multiple prescriptions for chronic conditions. This is a normal part of daily life. As we get older, our bodies change how they process medications. This makes careful management more critical than ever.
Without a solid system in place, the risk of medication mistakes goes up. These errors can lead to serious health issues or avoidable trips to the hospital. The goal is to create a routine that is safe, simple, and consistent. This helps them stay independent and feel their best.
Understanding the Risks of Polypharmacy
One of the biggest hurdles in medication management for the elderly is polypharmacy. This is a clinical term for regularly taking five or more medications at the same time. While each drug might be necessary, taking them together increases the risk of side effects.
How common is it? One study found that about 26.3% of older adults are dealing with polypharmacy. Getting a handle on polypharmacy is the first step to avoiding its dangers. You can read the full research about polypharmacy in elderly populations for more details.
A well-organized medication plan is a powerful tool for helping seniors maintain their health. It provides clarity for the individual, peace of mind for the family, and vital information for the healthcare team.
Getting professional support can make all the difference. At Central Coast VNA & Hospice, our home health and palliative care teams help families manage these complex situations. As a mission-driven nonprofit serving Monterey County and surrounding areas for over 74 years, we focus on providing compassionate, expert care. This guidance is key in helping many elderly parents age in place safely.
Build a Comprehensive Medication Master List
One of the best things you can do is create a single, comprehensive medication list. This document is for everything an older adult takes. This includes every pill, vitamin, herbal supplement, and over-the-counter remedy. Think of it as the foundational tool for their safety.

This simple document makes a world of difference. Imagine a Central Coast VNA & Hospice Registered Nurse is visiting your home in San Benito County. Handing them a complete list lets them get to work immediately. It is also critical in an emergency.
What Goes on the List?
First, gather up every single bottle and package. Don't forget things that might not seem like "medicine." This includes daily vitamins, fish oil capsules, or occasional ibuprofen. Even harmless items can interact with prescription drugs.
For every item, log the following details:
- Medication Name & Strength: Write down the brand name, generic name, and strength (e.g., Lisinopril 10 mg).
- Dosage & Frequency: Be precise. "One tablet by mouth, twice daily" is clearer than "take two a day."
- Purpose: Note why they are taking it, such as "For high blood pressure."
- Prescribing Doctor: Jot down the doctor’s name and phone number.
- Special Instructions: Include notes like "Take with a full meal" or "Do not take with dairy products."
This detailed approach means everyone involved is working from the same playbook.
A well-maintained medication list is a vital communication tool. It helps prevent dangerous errors, coordinates care between doctors, and empowers families.
This is a key part of effectively streamlining administrative processes in caregiving. Your goal is to make the master list clear, easy to update, and simple to share.
Here is a straightforward template you can use to build your own master list. It captures all the essential details in one place.
Sample Medication Master List Template
| Medication Name & Strength | Dosage & Frequency | Purpose | Prescribing Doctor | Notes (e.g., take with food) |
|---|---|---|---|---|
| e.g., Lipitor 20 mg | 1 tablet at bedtime | High cholesterol | Dr. Smith | Avoid grapefruit |
| e.g., Metformin 500 mg | 1 tablet with breakfast & dinner | Type 2 Diabetes | Dr. Jones | Take with food |
| e.g., Vitamin D3 2000 IU | 1 capsule daily | Bone health | Over-the-Counter | Take with a meal containing fat |
Filling this out gives you a clear overview of your loved one's entire medication regimen.
Keep It Current, Keep It Close
A medication list is only useful if it’s accurate and easy to find. Make a habit of reviewing and updating it after every doctor's appointment. Also update it any time a change is made to a medication.
Then, put copies where they can be easily found. We recommend keeping one on the refrigerator and a copy in a wallet or purse. A digital version on a smartphone is also a great idea.
Establish a Simple and Consistent Daily Routine
Once you have a complete medication list, it's time to build a simple, consistent daily routine. A predictable schedule is your best defense against missed doses or mix-ups. This transforms medication management from a source of stress into a manageable part of the day.
To make new behaviors stick, it helps to understand the basics of building healthy habits. The trick is to link the new task to an existing one. For example, take pills with breakfast or right after brushing teeth at night. This makes the process feel more natural over time.
Create a Dedicated Medication Station
Having one spot for all medications can cut down on confusion and improve safety. Choose a location that is cool, dry, and out of direct sunlight. A spot on the kitchen counter or a shelf in a pantry usually works well.
The bathroom medicine cabinet is often too humid. This can damage certain medications, so it's best to avoid it.
Make sure the area is well-lit so labels are easy to read. This central hub should have everything needed for the daily routine:
- The weekly pill organizer, filled and ready.
- A glass of water for swallowing pills.
- Your master medication list for a quick check.
- A small notebook to log doses or write questions for the doctor.
Use Practical Tools for Consistency
Simple tools can have a huge impact on keeping the routine on track. A weekly pill organizer is an essential item. Take the time to fill it once a week, so all doses for the upcoming days are sorted.
Forgetting doses is a common issue. Setting alarms on a smartphone, a clock, or a medication reminder device can help. It provides a reliable nudge when it's time for a dose.
A Central Coast VNA & Hospice palliative care professional helped a family in South Santa Clara County set up labeled alarms on their father’s phone. It was a simple change, but it improved his medication adherence. This gave the entire family peace of mind.
This simple graphic breaks down the steps to a successful medication routine.
As you can see, it’s a straightforward flow. Consult with professionals, get organized, and track everything. This process forms the backbone of a safe and effective routine.
Consistency is more important than complexity. A simple, repeatable routine is far more effective than an elaborate system that is hard to maintain.
This structured approach is something our teams emphasize. The reason home health care services make a difference is because our professionals are skilled at setting up these sustainable routines. They empower families to manage care confidently.
Identify and Prevent Common Medication Problems
Being proactive is the heart of keeping an older loved one safe. This goes beyond organizing pills in a container. It’s about having a keen eye for potential issues before they cause harm. A huge part of that is knowing what common problems to look for.

One of the biggest risks is Potentially Inappropriate Medications, or PIMs. These are prescriptions where the risks might outweigh the benefits for older adults. As we age, our bodies process drugs differently. A medication that was fine years ago could now trigger side effects like confusion or dizziness.
This is a widespread issue. A 2022 study revealed that the global use of PIMs among elderly outpatients is 36.7%. Benzodiazepines, often prescribed for sleep, are a common example. They are known for increasing the risk of falls and cognitive problems. You can read the full study to learn more about medication use in older adults.
Watching for New Side Effects
It is critical to pay close attention anytime a new medication is started. Many families think new symptoms are just from "getting older." In reality, they could be a direct side effect of a prescription.
Keep an eye out for any new changes, such as:
- Sudden dizziness or loss of balance, which is a major fall risk.
- New or worsening confusion or memory fog that could be mistaken for dementia.
- Unexplained drowsiness or fatigue that was not present before.
- Changes in appetite or digestive issues like constipation or nausea.
Catching these shifts early is essential. Sometimes, these symptoms are the first of the 5 warning signs that elderly parents need home health care. This signals that it might be time for more professional support.
Regular medication reviews are an essential safety check. Think of it as a periodic tune-up for your loved one's health, ensuring every prescription is still safe and necessary.
The Importance of Regular Medication Reviews
A proactive approach requires regular check-ins with a doctor or pharmacist. An annual medication review should be the minimum. A review is also needed any time a new drug is prescribed or after a hospital stay. This is your chance to ask questions.
At Central Coast VNA & Hospice, our skilled nurses are trained to spot these exact risks. Serving families across Monterey County, San Benito County, Santa Cruz County, and South Santa Clara County, our team works with physicians. We help craft safer, more effective medication plans as part of our continuum of care.
Navigate Financial Hurdles to Medication Adherence
Good medication management goes beyond remembering to take pills. For many older adults, the biggest challenge is affording their prescriptions.
High medication costs create a serious barrier to good health. Seniors are sometimes forced to choose between prescriptions and other expenses like food. This financial stress takes a real toll.
Some will try to stretch a prescription by skipping doses or cutting pills in half. While it might seem practical, it can undermine treatment. As a nonprofit, our teams at Central Coast VNA & Hospice often help families find local resources.
Exploring Cost-Saving Strategies
The best first step is a conversation with your loved one’s doctor and pharmacist. They are your greatest allies in finding affordable solutions. Don't be hesitant to bring up cost concerns.
Here are a few things you can discuss with their healthcare provider:
- Generic Alternatives: Always ask if a generic version is available. They contain the same active ingredients as brand-name drugs but cost less.
- Therapeutic Alternatives: Sometimes, another medication in the same drug class can work just as well but is more affordable.
- Patient Assistance Programs: Many drug companies offer programs that help patients get medications for free or at a reduced cost.
This isn't a small problem. Recent CDC data shows that from 2021 to 2022, cost was a real issue for seniors. 2.2% took less medication than prescribed, while 2.7% delayed filling prescriptions. You can learn more about medication cost challenges from the CDC.
Ensuring a loved one can afford their medication is a critical part of their care plan. No one should have to choose between their health and their financial stability.
Understanding Insurance and Local Support
Insurance plans like Medicare Part D can be confusing, but understanding the coverage is vital. Families should review their loved one’s plan every year during open enrollment.
Formularies change, and a plan that was great last year might not be the best fit now. Switching to a different plan can sometimes lead to significant savings.
For families here in Monterey County, San Benito County, Santa Cruz County, and South Santa Clara County, local resources may be available. Our teams at CCVNA know this community well and can point you toward helpful programs. Understanding broader financial planning, like how to pay for hospice, can also provide a clearer view of available support.
How Professional Home Health Support Can Make a Difference
Managing medications can feel like a heavy burden, but you do not have to carry it alone. Professional home health support offers families peace of mind. It brings clinical expertise into the home, ensuring safety and simplifying complex routines.
For families across Monterey, San Benito, Santa Cruz, and South Santa Clara counties, this support is a game-changer. It transforms daily stress into a well-managed part of your loved one’s care.

Expert Guidance from Skilled Clinicians
Central Coast VNA & Hospice provides a full continuum of care—from home health to palliative and hospice care. We directly tackle the challenges of medication management for elderly individuals. Our mission-driven, nonprofit teams have served the Central Coast for over 74 years, building a legacy of trust and compassionate care.
Our professional support includes a few key services:
- Medication Setup: A Registered Nurse can visit the home to fill weekly pill organizers. This simple act ensures every dose is sorted and helps prevent errors.
- Family Education: Our clinicians take the time to explain what each medication is for. We also discuss potential side effects and how to respond if they occur.
- Physician Coordination: We act as a link between you, your loved one, and their doctor. We can communicate concerns, ask questions, and advocate for simpler regimens.
This hands-on assistance is invaluable. Having a professional team offer dedicated help with administering medication ensures everyone stays safe.
Having a skilled nurse oversee medication management provides a critical layer of safety. It empowers families with knowledge and offers reassurance that their loved one is receiving the best care at home.
Ultimately, getting professional support lifts a weight off family members. With our expertise, you can focus less on pill schedules and more on sharing quality time. You can learn more by exploring our services for in-home care for seniors.
Frequently Asked Questions About Managing Medications
Navigating medication management for an older loved one can be overwhelming. Families often have similar concerns. We've put together answers to some common questions below.
What is polypharmacy?
Polypharmacy means taking five or more medications every day. This number is a critical threshold. It is the point where the risk for harmful drug interactions and side effects starts to climb. A healthcare professional can review a medication list to see if the combination is safe and necessary.
How often should my loved one's medications be reviewed?
A complete medication review should happen at least once a year. However, you should not wait a full year if something changes. It is crucial to schedule a review anytime a new medication is prescribed or after a hospital stay. A Central Coast VNA & Hospice Registered Nurse can help coordinate these reviews with your doctor.
What can I do if my parent keeps forgetting to take their pills?
This is a very common problem. The best approach is to start simple. A weekly pill organizer and daily alarms on a phone or clock can make a big difference. If memory issues still cause missed doses, it might be time for extra support. Home health services can provide medication setup and reminders.
Are over-the-counter medicines safe to mix with prescriptions?
Not always. Many common over-the-counter products, vitamins, and herbal supplements can interfere with prescription drugs. These interactions can sometimes cause dangerous side effects. It is important to list everything your loved one takes and review it with their doctor or pharmacist.
Who can I contact for help with medication management at home?
You don't have to figure this out alone. Central Coast VNA & Hospice offers expert home health and palliative care services that include medication management. Our skilled nurses serve families across Monterey, San Benito, Santa Cruz, and South Santa Clara counties. We are a nonprofit, mission-driven organization with over 74 years of service to the community.
If you need expert support with medication management for elderly loved ones, the compassionate team at Central Coast VNA & Hospice is here to help. Contact us today to learn how our home health and palliative care services can bring safety and peace of mind to your family.










