Hospice Aide Responsibilities Explained
When a loved one is in hospice, some of the most meaningful support they receive comes from a hospice aide. These certified professionals provide direct, hands-on assistance and compassionate support at the bedside.
Their role is to help with daily activities, keep a gentle eye on the patient's well-being, and serve as a comforting presence for both patients and families.
The Heart of the Hospice Care Team
At Central Coast VNA & Hospice, our Hospice Aides are indispensable members of the interdisciplinary care team. For over 74 years, these dedicated professionals have delivered hands-on support that preserves dignity and enhances quality of life. An aide’s role is a cornerstone of our nonprofit mission across Monterey County, San Benito County, Santa Cruz County, and South Santa Clara County.
The responsibilities of a Hospice Aide are broad, blending practical help with a profound emotional connection. They are specially trained to assist with sensitive personal tasks, always putting the patient's comfort and respect first. This support is a key piece of a comprehensive hospice plan, designed to support the entire family. You can learn more about what hospice care is to see how the whole team works together.
This image breaks down the primary duties an aide takes on.
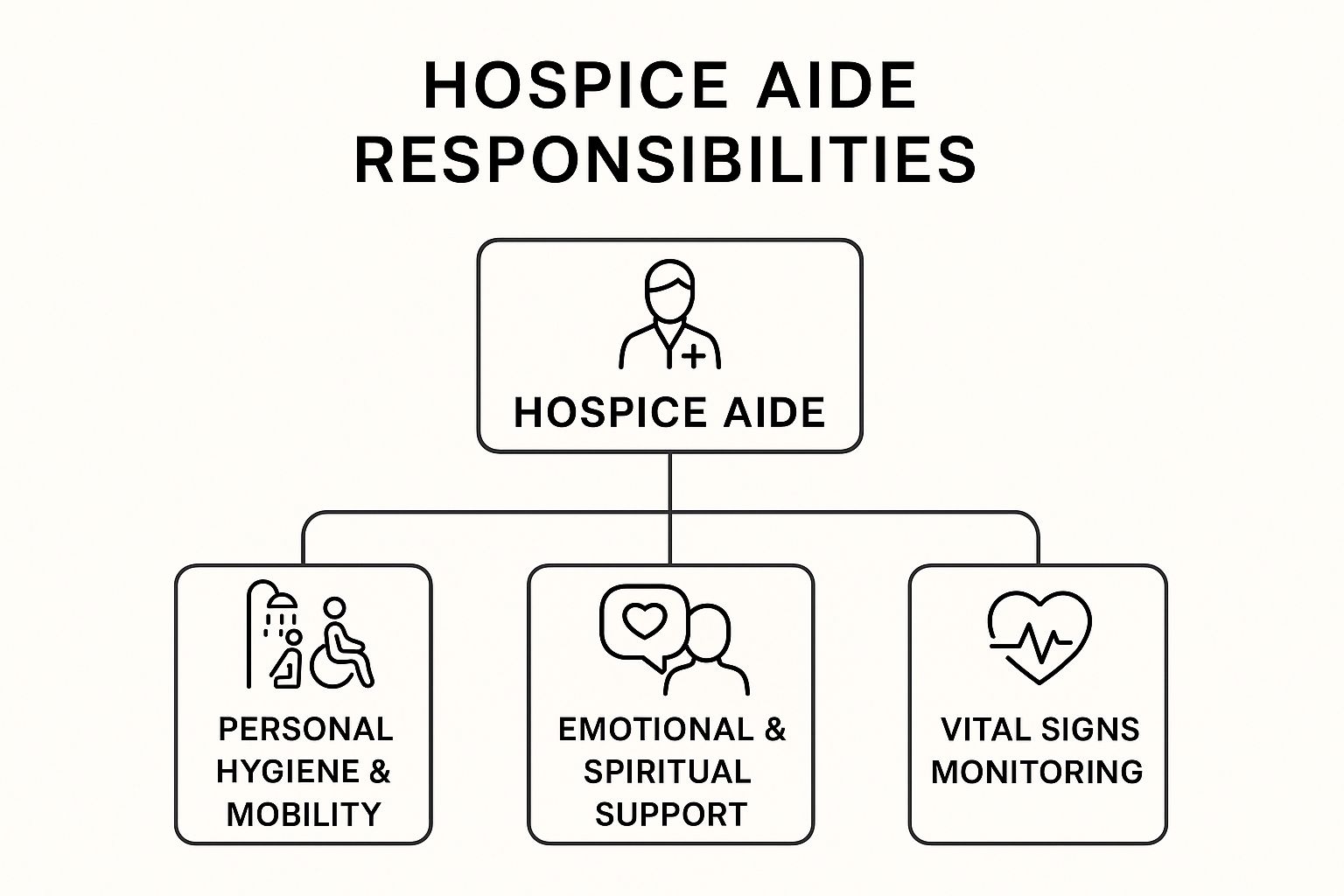
The job is a delicate balance of physical care, like help with hygiene and moving safely, and equally important emotional support. These duties ensure the care we provide is not just clinically sound, but deeply human.
A Quick Look at Hospice Aide Responsibilities
To give you a clearer picture, here’s a breakdown of the core duties a hospice aide performs to support patient comfort, safety, and dignity.
| Area of Responsibility | Primary Duties |
|---|---|
| Personal Care | Assisting with bathing, grooming, dressing, and toileting. |
| Mobility & Safety | Helping patients move, repositioning them for comfort, and ensuring a safe environment. |
| Comfort & Support | Providing companionship, listening, and offering emotional reassurance to patients and families. |
| Health Monitoring | Observing changes in condition, taking vital signs, and reporting updates to the nurse. |
| Light Housekeeping | Tidying the patient's immediate space and doing light laundry to maintain a clean environment. |
Ultimately, a hospice aide’s goal is to make each day the best it can be for the patient. They ensure patients feel cared for, respected, and comfortable.
Providing Dignified Personal Care and Assistance

Providing hands-on personal care is one of the most vital hospice aide responsibilities. This fundamental support protects a patient's comfort, hygiene, and sense of self-respect during a vulnerable time. Our compassionate aides at Central Coast VNA & Hospice are specially trained to handle these sensitive tasks with the utmost professionalism and gentleness.
This assistance goes far beyond a simple checklist; it’s about preserving a sense of normalcy and dignity. When patients feel clean and comfortable, it has a profound and positive impact on their emotional well-being.
Why This Support Matters
When a hospice aide steps in to help with daily activities, they reinforce a patient’s humanity. They provide a type of comfort that words often cannot.
This hands-on support can include:
- Bathing and Grooming: Helping with a bath or shower, caring for hair, or shaving isn't just about hygiene; it helps patients feel more like themselves.
- Dressing: Assisting a patient in choosing and putting on comfortable clothes for the day can bring back a sense of routine and personal choice.
- Mobility: Gently helping a patient move from a bed to a chair, or simply repositioning them for comfort, can prevent sores and reduce stiffness.
- Toileting: Providing respectful and discreet assistance with toileting and incontinence care is a critical part of maintaining a patient's dignity.
By managing these physical needs, our Hospice Aides also offer a significant gift to families. This support frees family members from the physically and emotionally taxing role of full-time personal care. It allows them to simply be a spouse, a child, or a cherished loved one again.
This shift allows families to focus their energy on creating meaningful moments and sharing quality time together. It’s a core part of how our nonprofit, mission-driven team approaches hospice care across Monterey and San Benito counties.
Serving as the Eyes and Ears of the Care Team

While hands-on support is vital, one of the most critical hospice aide responsibilities is acting as the eyes and ears for the entire care team. Because aides spend so much direct, consistent time with patients, they are in the perfect position to notice subtle shifts that others might miss.
This constant presence allows them to pick up on the smallest changes in a patient’s physical condition, mood, or appetite. These observations are a real-time snapshot of a patient's well-being and are essential for keeping the care plan effective.
The Observation and Reporting Process
A significant part of an aide's day involves carefully documenting and communicating what they see to the patient’s Registered Nurse (RN) Case Manager. This constant feedback loop makes a care plan a living document that responds to a patient’s changing needs.
This collaborative process usually looks like this:
- Noticing Changes: An aide might see that a patient seems more tired than usual, has a new spot of redness on their skin, or is verbalizing more anxiety.
- Accurate Documentation: These details are then recorded in the patient’s chart with clarity and objectivity, creating a reliable record for the clinical team.
- Timely Communication: Any significant findings are reported immediately to the RN, who can then assess the situation and adjust the care plan.
This flow of information is the bedrock of our care model at Central Coast VNA & Hospice. By listening closely to our aides, we ensure our care isn't just pre-planned but is constantly adapting to what the patient needs in the moment.
Qualitative research confirms that aides view their role as the 'eyes and ears' of the hospice team. You can read the full research on aide perspectives to see just how crucial their input is. At CCVNA, we actively work to ensure our aides’ voices are always heard and valued.
Offering Essential Emotional and Social Support

Beyond physical tasks, a hospice aide provides profound emotional and social support. This part of the job is less about doing and more about being there—offering a steady, reassuring presence that can cut through anxiety and isolation. The human connection an aide builds is the heart and soul of hospice care.
A simple chat about a favorite memory or even just sitting together in comfortable silence can make a world of difference. For our patients at home in Monterey County or San Benito County, our aides often become a familiar and welcome part of the daily routine.
The Power of a Compassionate Presence
This support naturally extends to the whole family. Hospice aides become a trusted listening ear for the patient and for family members who are often feeling overwhelmed.
This compassionate approach includes:
- Active Listening: Giving patients and their families a safe, non-judgmental space to share fears, tell stories, or just talk about their day.
- Offering Companionship: Fighting off loneliness by engaging in simple, shared activities like watching a favorite TV show or listening to music.
- Providing Reassurance: Being a calm and gentle presence that helps soothe anxieties when moments get tough.
At Central Coast VNA & Hospice, this focus on emotional and social well-being is fundamental to our philosophy. We believe that comfort comes from caring for the whole person—body, mind, and spirit.
This compassionate support doesn't end when a loved one passes. Families can find comfort through our specialized hospice bereavement services, which are designed to help them navigate grief. We are committed to caring for families through their entire journey.
Creating a Safe and Comfortable Environment
A hospice aide is often the one who makes a house feel like a sanctuary. One of their most important jobs is to create a peaceful, safe, and comfortable environment for the patient.
This focus on the immediate surroundings is a hands-on expression of our mission here at Central Coast VNA & Hospice. We’re dedicated to providing dignified care at home in communities like Santa Cruz County and South Santa Clara County. A calm, clean space can directly boost a patient's physical safety and psychological well-being.
Enhancing Safety and Peace of Mind
Simple actions by a hospice aide can drastically reduce everyday hazards and bring a sense of tranquility. Their work in this area often includes:
- Changing Bed Linens: Fresh, clean bedding is essential for both hygiene and comfort, making a patient feel cared for and refreshed.
- Tidying the Patient’s Room: Keeping the immediate area organized and uncluttered can significantly reduce a patient's anxiety and create a restful atmosphere.
- Ensuring Clear Pathways: Removing obstacles to prevent falls is absolutely critical, especially for patients who have limited mobility.
This careful attention to the patient’s personal space helps prevent accidents and fosters a sense of order. The demand for these professionals has grown significantly. According to the National Hospice and Palliative Care Organization (NHPCO), over 1.72 million Medicare beneficiaries received hospice services in 2020 (NHPCO, 2021).
Families can also review our guide on hospice eligibility requirements to better understand when this level of care may be the right choice.
A Partnership on the Hospice Journey
The bond between a hospice aide, the patient, and their family is a true partnership built on trust. A hospice aide’s role goes far beyond a list of tasks; it’s about delivering compassionate, hands-on support that honors a patient’s dignity.
Our aides at Central Coast VNA & Hospice are dedicated local professionals who become trusted figures on this profound journey. This commitment to partnership is the cornerstone of our nonprofit mission across Monterey, Santa Cruz, San Benito, and South Santa Clara counties. For over 74 years, our team has been woven into the fabric of this community.
A Commitment to Our Community
The hospice field is facing a tough reality with staffing shortages impacting a staggering 98% of hospice organizations nationwide. In fact, 72% have had to turn away patient referrals simply because they don't have enough staff. You can discover more insights about these hospice workforce statistics to see the full picture.
At Central Coast VNA & Hospice, our deep local roots and nonprofit model help us foster a supportive environment for our dedicated team. This ensures we can be there for our community.
We are committed to being your reliable partner through it all. If your family needs support and a team you can count on, contact us today to learn more.
Frequently Asked Questions About Hospice Aide Responsibilities
When a loved one begins hospice, families have questions about the care team. It's important to know who is doing what, especially when it comes to hands-on care.
Here are answers to some of the most common questions we hear about the vital role of a Hospice Aide.
What is the difference between a Hospice Aide and a Nurse?
A Registered Nurse (RN) is a licensed medical professional who manages the clinical care plan, administers medications, and assesses medical symptoms. A Hospice Aide is a certified professional who provides direct, personal, hands-on support, helping with activities like bathing, dressing, and mobility. The aide also acts as the "eyes and ears" for the nurse, reporting any changes in the patient's condition.
Can a Hospice Aide administer medications?
No, Hospice Aides are not licensed to administer medications of any kind, including pills, injections, or oxygen. This responsibility belongs solely to licensed medical professionals, like a Registered Nurse. An aide can, however, remind a patient when it's time to take medication that has already been prepared by a nurse or family member.
How often will a Hospice Aide visit?
The frequency of aide visits is determined by the personalized care plan developed by the hospice team with your family's input. Typically, you can expect visits a few times per week, but this schedule is flexible. As a patient's condition changes, visits can be adjusted to provide the right level of support.
Do Hospice Aides help with housekeeping?
Hospice Aides perform light housekeeping tasks directly related to the patient’s care and immediate environment. This includes changing bed linens, doing the patient's personal laundry, and tidying their living space to ensure it is safe and comfortable. They do not perform heavy or general household cleaning.
Can we request a specific Hospice Aide?
We always strive to promote consistency and build a trusting relationship between the aide, the patient, and the family. While we cannot guarantee a specific individual for every visit due to scheduling and availability, we do our best to assign a primary aide to each patient. Our goal is to ensure you feel comfortable and familiar with the professionals supporting you.
To get a better sense of how the entire process works, you can explore what to expect from hospice and see how our services in Monterey County and the surrounding areas are built around your family's needs.
At Central Coast VNA & Hospice, our dedicated Hospice Aides are committed to providing compassionate, dignified support. If you have more questions about our services, please contact us at https://ccvna.com.
In-Home Support to Avoid Nursing Home Care
For most families, the preference is crystal clear: they want compassionate, effective in-home support to avoid nursing home placement altogether. This allows loved ones to age with dignity in the place they know and cherish. They can be surrounded by a lifetime of memories and the simple comfort of their own community.
The Growing Desire to Age with Dignity at Home

Deciding to age in place is not just about logistics; it’s a deeply emotional choice. The sense of independence and normalcy that comes from being at home is something you cannot replicate in an institutional setting.
The data backs this up. AARP has found that a vast majority of seniors want to stay in their own homes as they age. Often, the financial side also makes sense, since in-home care can be more affordable than a residential facility.
For over 74 years, Central Coast VNA & Hospice has been dedicated to making this happen for families across Monterey County, San Benito County, Santa Cruz County, and South Santa Clara County. As a local, mission-driven nonprofit, our commitment is to one thing: helping people live well, right where they belong.
Why Home Is Where the Health Is
Staying at home means staying connected. It's about keeping vital links to neighbors, friends, and the familiar routines that are so important for mental and emotional well-being. This continuity helps sidestep the stress and confusion that often come with moving to a new environment.
And let's not forget independence. The simple things—making a meal in your own kitchen, sleeping in your own bed—give a person a sense of self-worth and control over their own life.
When you bring professional support into the home, you create an environment that honors a person's desire for independence while making sure their health and safety are covered. It becomes a true partnership between the clinical team, the patient, and their family.
To give you a clearer picture, let's look at how professional home support stacks up against a nursing home facility.
Comparing In-Home Support and Nursing Home Care
This table offers a clear, at-a-glance comparison between professional support at home and traditional nursing home care. It focuses on key differences in environment, cost, and personalization.
| Feature | In-Home Support | Nursing Home Facility |
|---|---|---|
| Environment | Familiar, comfortable, and private setting. | Institutional environment with set schedules. |
| Personalization | Highly personalized, one-on-one care tailored to individual needs and routines. | Standardized care for multiple residents. |
| Independence | Promotes autonomy and preserves daily routines. | Limited independence due to structured living. |
| Cost | Often more affordable, with flexible service hours. | Can be very expensive, with all-inclusive daily rates. |
| Family Involvement | Family can be closely involved in daily care. | Visiting hours and facility rules may limit involvement. |
Ultimately, the choice depends on individual needs. For many, the benefits of staying home are undeniable.
A Continuum of Care Tailored to Your Needs
Healthcare needs change, and we understand that. Central Coast VNA & Hospice provides a seamless range of services that adapt as a patient's condition evolves, ensuring there are no gaps in care.
Our services include:
- Home Health: Skilled nursing and therapy to help you or your loved one recover from surgery, illness, or an injury.
- Palliative Care: Specialized support focused on managing symptoms and improving quality of life for those with serious illnesses.
- Hospice Care: Compassionate end-of-life care that provides comfort, dignity, and support for patients and their families.
Sometimes, small things make a huge difference in preserving that feeling of independence. Simple assistive devices, like adjustable over-bed tables, can make daily activities much easier and safer.
Choosing in-home support is a powerful decision that puts comfort, dignity, and personal choice first. By understanding the options and finding a trusted partner, you can confidently create a plan that truly honors your loved one’s wishes. You can explore our expert guidance on aging in place care services to see exactly how we can help.
Decoding Your In-Home Care Options

When you're trying to find the right in-home support to avoid nursing home placement, the terminology can be confusing. "Home health," "palliative," and "hospice" are often used interchangeably. However, they represent very different types of care designed for specific points in a person's health journey.
Understanding the distinctions is the key to getting the right help at the right time.
At Central Coast VNA & Hospice, we provide this full spectrum of services. Families in Monterey County and the surrounding areas never have to search for a new provider as needs change. Our nonprofit mission is to create a seamless experience, offering stability and trust when you need it most.
Home Health Care: Focused on Recovery
Think of home health care as short-term, skilled medical support prescribed by a doctor. It is designed to help someone recover from an illness, injury, or surgery. It’s for individuals who are considered homebound and need clinical expertise to get back on their feet safely.
For example, imagine a Santa Cruz County resident just home after a hip replacement. A CCVNA Registered Nurse might visit to manage medications and check the surgical wound. A Physical Therapist would guide them through exercises to regain mobility in their own living room.
Home health is all about active, goal-oriented rehabilitation. It provides the specific clinical support a patient needs to restore their independence and get back to their life.
Palliative Care: For Comfort and Quality of Life
Palliative care is specialized support for people living with a serious illness. Unlike home health, it is not limited by time and can begin at any stage of a diagnosis. It can even be provided while pursuing curative treatments.
The entire focus is on improving quality of life by managing symptoms, pain, and stress.
Let’s say a family in South Santa Clara County is caring for a loved one with a progressive lung condition. A CCVNA palliative care team—which could include a Nurse Practitioner, Medical Social Worker, and Chaplain—works alongside the patient's other doctors. They might help manage breathing issues, address anxiety, and offer emotional support to the entire family. To see how our teams can help, you can learn more about skilled nursing at home and our other specialized services.
Hospice Care: A Shift to Compassionate Comfort
Hospice is a special kind of care for individuals with a life-limiting illness, where the focus shifts from cure to comfort. It's typically for those with a prognosis of six months or less if the disease takes its natural course. Hospice provides expert pain and symptom management, as well as emotional and spiritual support for both the patient and their family.
In San Benito County, a CCVNA Hospice Aide could help a patient with personal care. A Registered Nurse would ensure their pain is completely under control. A Chaplain or Medical Social Worker might also be there to provide counseling, helping the family navigate this difficult time with peace and dignity.
As a nonprofit with over 74 years of local history, our promise is to deliver this comfort wherever a patient calls home. The U.S. home care industry statistics show a compelling financial reason for staying home as well.
How to Accurately Assess Your Loved One’s Needs
The first real step toward arranging in-home support to avoid nursing home care is getting a clear, honest picture of what your loved one actually needs. This isn't just a quick check-in. It's a gentle but thorough look at their daily life, the challenges they face, and where they could use a helping hand.
The goal is to move past vague worries like, "Dad seems to be struggling," and get to specific, actionable insights. For instance, "Dad has forgotten his blood pressure medication three times this week and I've noticed he has a hard time getting up from his favorite chair." This level of detail is what turns a concerned conversation into a productive plan.
This infographic lays out the key steps families can take to get organized. It helps coordinate the right kind of in-home support.
As you can see, it highlights a simple, logical flow—from the initial assessment to ongoing management. Having a structured approach makes all the difference.
Key Areas for Assessment
A good assessment goes far beyond a medical diagnosis. You need to look at the whole person. This includes their physical abilities, specific medical needs, the safety of their home, and their emotional well-being.
Breaking it down into categories makes this feel much less overwhelming. Think of these areas as a guide for your observations and conversations.
Medical and Clinical Requirements
This is where you focus on the specific health tasks that might require a skilled professional.
- Medication Management: Is Mom or Dad taking the correct doses at the right times? Who is managing the refills?
- Wound Care: Are there any post-surgery incisions, pressure sores, or other wounds that need professional attention?
- Symptom Control: Are they dealing with unmanaged pain, shortness of breath, nausea, or other persistent symptoms from a chronic illness?
- Medical Equipment: Is your loved one using oxygen, a catheter, an IV line, or other specialized medical devices that require monitoring?
Activities of Daily Living (ADLs)
ADLs are the absolute basics of self-care. When these become a struggle, it’s often one of the first signs that help is needed.
- Personal Hygiene: Is bathing, grooming, or getting dressed becoming difficult or unsafe?
- Mobility: Can they get around the house safely? What about standing up from a bed or chair?
- Toileting: Is using the bathroom independently becoming a challenge?
- Eating: Can they feed themselves once a meal is prepared?
Instrumental Activities of Daily Living (IADLs)
These are the more complex activities necessary for living independently in the community.
- Meal Preparation: Are they able to plan and cook nutritious meals, or are they relying on snacks and toast?
- Housekeeping: Can they keep their living space reasonably clean and safe from clutter and fall hazards?
- Managing Finances: Are bills getting paid on time? Is mail piling up unopened?
- Transportation: Can they still drive safely, or can they arrange rides to the doctor or grocery store?
Social and Emotional Well-Being
A person’s mental and emotional state is every bit as important as their physical health. Do not overlook it.
- Companionship: Do they seem lonely or isolated? Are they withdrawing from hobbies or friends?
- Safety: Are you worried about them being alone? Have there been falls, or even near-misses?
- Cognitive Function: Have you noticed any troubling memory loss, confusion, or changes in their judgment or personality?
A Note on Starting the Conversation: These topics can be really sensitive. It's best to frame questions from a place of love and concern. Instead of saying something that sounds critical, try, "I was wondering if having someone help with meals a few times a week might make your days a little easier?"
The Importance of a Professional Assessment
While your family’s observations are invaluable, a professional assessment is the next critical step. A Registered Nurse from Central Coast VNA & Hospice can come to the home and conduct a thorough evaluation. This creates a formal, personalized plan of care that meets clinical standards.
This professional assessment is often essential for qualifying for home health care and ensuring that services are covered by Medicare or other insurance.
Our clinicians are trained to see the full picture. They can identify needs you might have missed and connect them to the right services. This step is what transforms your loving concern into a concrete action plan, allowing your loved one to age safely and comfortably at home.
Navigating the Financials of Home-Based Support

Let's be honest: for most families, figuring out how to pay for care is the biggest hurdle. The financial side of things can feel overwhelming, but it doesn't have to be. There are well-established ways to cover the costs of professional medical support right at home.
With a 74-year history of serving the Central Coast, we at Central Coast VNA & Hospice have guided countless families through this process. As a Medicare-certified nonprofit, our mission is to ensure every eligible person in Monterey, San Benito, Santa Cruz, and South Santa Clara Counties can get the care they need. Our nonprofit status and community support make this possible.
Medicare Coverage for Home Health and Hospice
Medicare is often the first stop and the primary payer for many clinical services you'd receive at home. The key is understanding what it covers and under what circumstances.
- Both Medicare Part A and Part B will cover intermittent skilled nursing, physical therapy, occupational therapy, and speech therapy services delivered in your home.
- To qualify, a patient must be under a doctor's care, have a physician-established plan of care, and be certified as homebound.
- The Medicare Hospice Benefit is a comprehensive package that covers nearly every aspect of hospice care, from nursing services and medical equipment to medications.
This coverage is what makes skilled home health care services a real, financially sound option for so many seniors. It's important to remember that Medicare generally doesn't cover 24-hour care at home or personal care if that's the only type of support you need.
Other Key Funding Sources
Beyond Medicare, several other resources can help families manage the costs of staying at home. You just need to know where to look.
Medi-Cal
California's Medicaid program, Medi-Cal, is an essential resource. It often picks up where Medicare leaves off, covering services like long-term personal care. Eligibility is tied to income and medical need, and our team can help you determine if you or a family member might qualify.
Private Insurance Plans
Many private health insurance plans, including Medicare Advantage (Part C) plans, offer their own benefits for home health care. The details, like co-pays and deductibles, can vary from one plan to the next. The best approach is always to call the insurance provider directly, or let our care coordinators handle it.
Veterans Affairs (VA) Benefits
Veterans may be eligible for a range of home-based care benefits through the VA. This can include skilled home health care, homemaker services, and specialized hospice care. Our team has deep experience working with the VA to coordinate care for local veterans.
Navigating these different payment systems requires real expertise. As a trusted local nonprofit, we help families understand their benefits and coordinate directly with payers to ensure a smooth, stress-free process.
Your Nonprofit Partner in Care
Because Central Coast VNA & Hospice is a nonprofit organization, our one and only focus is on patient care. We focus on the well-being of our community, not on generating profits for shareholders. This is a fundamental difference.
The generous donations from our community allow us to provide care to all eligible patients. We help bridge financial gaps whenever they appear.
We truly believe that financial worries should never stand in the way of receiving high-quality, compassionate care at home. Contact us today to speak with one of our knowledgeable team members. We can help clarify your coverage options and guide you toward the best solution for your family.
Creating a Safe and Supportive Home Environment
Effective in-home support to avoid nursing home placement is about more than just scheduled medical visits. It’s about looking at the entire home environment. The goal is to transform it into a space that truly supports independence and minimizes risk.
The first step is always a practical look at the living space. Here at Central Coast VNA & Hospice, our teams conduct professional home safety assessments. We walk through homes across Monterey, San Benito, Santa Cruz, and South Santa Clara Counties to spot potential hazards and suggest simple modifications.
Practical Steps for a Safer Home
Making a home safer doesn't have to be a massive, expensive project. Some of the most effective changes are surprisingly simple. The number one priority is fall prevention, because a single fall can easily lead to a hospital stay.
Start with these key strategies to boost home safety:
- Clear the Decks: Walk through every room and clear pathways of any clutter. Small throw rugs are notorious trip hazards, so either secure them with double-sided tape or remove them.
- Light It Up: Good lighting is non-negotiable. Make sure hallways, stairways, and bathrooms are brightly lit. A few well-placed nightlights can create a safe, illuminated path for middle-of-the-night trips.
- Install Grab Bars: These are essential. Place sturdy grab bars next to the toilet and both inside and outside the shower or bathtub.
- Keep Communication Easy: A phone should always be within arm's reach. Program important contacts into the phone and make sure the numbers are easy to read. A medical alert system provides peace of mind.
A safe home environment is the foundation of successful aging in place. It builds confidence, reduces family anxiety, and allows clinical care to be delivered more effectively, ultimately preventing the need for facility-based care.
Don't Forget Emotional Well-Being
Physical safety is just one side of the coin. A person's emotional and social health is just as critical for maintaining a high quality of life at home. Loneliness can quickly lead to depression and a decline in physical health.
Keeping someone socially engaged can be as straightforward as arranging regular visits from friends. Setting up video chats with family or finding a local community group can also help. It’s all about keeping the mind active and the spirit lifted.
The COVID-19 pandemic gave us all a stark reminder of the benefits of being at home. Research from the time reinforced what many of us already knew—home is often the safest place to be. You can learn more by reviewing the research on nursing home statistics to understand the full scope.
Our teams are dedicated to working with families to build a supportive atmosphere. We look after both physical safety and emotional needs, ensuring home truly is the best place to be.
Frequently Asked Questions About In-Home Support
1. How do we know when it's the right time for help?
The best time to ask for help is when you start wondering if you need it, not during a crisis. If you notice an increase in falls, difficulty with daily tasks like managing medication, or a recent hospitalization has taken a toll, it's a good time to explore options. An early assessment provides a clear path forward.
2. What is the difference between home health, palliative, and hospice care?
Think of them as a continuum. Home Health Care is short-term, skilled medical care prescribed by a doctor for recovery. Palliative Care focuses on improving quality of life for those with serious illness, at any stage. Hospice Care is for those with a life-limiting illness, shifting the focus to comfort and dignity.
3. Will Medicare pay for in-home support?
Yes, Medicare Part A and Part B cover eligible home health services, such as skilled nursing and physical therapy, if a patient is certified homebound by a doctor. The Medicare Hospice Benefit is also comprehensive. However, Medicare generally does not cover 24-hour care or personal care services alone.
4. What makes Central Coast VNA & Hospice different from other agencies?
As a local, independent nonprofit with over 74 years of service, our sole mission is patient care, not profit. We reinvest all resources back into our community and staff. Our dedicated team of employees ensures a higher standard of care and accountability to families in Monterey County, San Benito County, Santa Cruz County, and South Santa Clara County.
5. How do we start the process with CCVNA?
Getting started is simple. You, a family member, or your doctor can call us to begin the conversation. To officially start services, we need a physician's referral. Our team will then help verify insurance and schedule an in-home assessment with a Registered Nurse to create a personalized care plan.
Taking that first step to secure quality care at home can bring an enormous sense of relief. The experienced, compassionate team at Central Coast VNA & Hospice is here to guide you through every question. We can help ensure your loved one can stay safely and comfortably right where they want to be.
Contact us today or visit us online at ccvna.com to learn more about how we can support your family.
Find Aging in Place Care Services Near You Today
When a loved one starts needing more support at home, figuring out what kind of help they actually need can be overwhelming. A quick search for "aging in place care services near me" will likely pull up a list of options like home health, palliative care, and hospice.
While they might sound similar, each service is designed for very different needs along a person's health journey. Getting this right from the start means your family member receives the right support at the right time.
Decoding Your In-Home Care Needs
Choosing to age in place is a powerful goal for so many older adults. It means staying in the home they love, surrounded by memories and a familiar community. As health needs shift, that decision often requires bringing in some extra support.
This is not a niche situation. The U.S. is experiencing a major demographic shift—by 2030, one in five Americans will be 65 or older. That number is projected to hit 95 million by 2060, and a huge number of them will be managing chronic health issues.
In fact, according to the CDC, about 85% of older adults have at least one chronic health condition, and 60% have at least two (CDC, 2023). These situations demand specialized, coordinated care right in the home, which is why understanding your options is the critical first step.
Understanding the Continuum of Care
The health journey for an aging adult is rarely a straight line. Needs evolve. What starts as a temporary need for skilled nursing after a hospital stay can later become a long-term need for symptom management or, eventually, a focus on comfort at the end of life.
This is where the idea of a continuum of care becomes so important. It’s about creating a smooth, seamless pathway from one type of care to another, ideally all under the umbrella of one trusted, nonprofit organization.
As a nonprofit provider with over 74+ years of service in Monterey County, San Benito County, Santa Cruz County, and South Santa Clara County, Central Coast VNA & Hospice was built on this integrated approach. Our teams are structured to support patients and their families as needs change:
- Home Health Care: Perfect for recovering from surgery, an injury, or learning to manage a new diagnosis.
- Palliative Care: Focused on managing the symptoms and stress of a serious illness, at any stage of that illness.
- Hospice Care: Dedicated to providing comfort, dignity, and quality of life when a cure is no longer the goal.
This model allows families to build a real, lasting relationship with their care team. It removes the immense stress of having to search for new providers at what are often the most critical and emotional moments.
As you figure out your in-home care needs, it’s also smart to see how technology can play a supporting role. You can explore the top senior living technology solutions to discover innovations that can really enhance safety and independence alongside professional care.
A key advantage of a nonprofit provider is the focus on community well-being over profits. This mission-driven philosophy ensures that patient care, staff expertise, and family support are always the top priorities.
Navigating this path requires a thoughtful look at your loved one’s current health and what might lie ahead. Our guide on how to help seniors live at home safely is packed with more practical insights and actionable tips.
To help you get a clearer picture, it's useful to see these services side-by-side. Each one has a distinct purpose and is meant for a different point in a person's health journey.
A Quick Guide to In-Home Care Services
Use this table to quickly compare Home Health, Palliative Care, and Hospice Care and see which service best fits your family's current situation.
| Service Type | Primary Goal | Who It's For | Provided By |
|---|---|---|---|
| Home Health | Recovery and rehabilitation | Individuals recovering from surgery, illness, or injury; short-term needs. | Registered Nurses, Physical/Occupational/Speech Therapists, Social Workers |
| Palliative | Pain and symptom management; improve quality of life | Individuals with a serious, chronic illness at any stage; can receive curative treatment. | A specialized team of doctors, nurses, and other specialists. |
| Hospice | Comfort, dignity, and emotional support | Individuals with a life-limiting illness; prognosis of 6 months or less. | An interdisciplinary team including medical, spiritual, and emotional support. |
Seeing the goals and intended recipients laid out like this can make it much easier to identify the right starting point for your conversation with a healthcare provider.
Finding Trusted Local Care Providers
Once you have a clearer idea of your loved one's needs, the next step is finding the right team to provide that support. A simple search for "aging in place care services near me" is a good starting point, but building real confidence means looking much deeper.
Frankly, the most reliable referrals often come from trusted professionals who already understand the local healthcare landscape. Your family physician, a hospital discharge planner, or a social worker are all excellent resources.
These professionals work directly with various agencies day in and day out. They can recommend providers known for quality and reliability right here in Monterey County or surrounding areas. Their firsthand experience can point you toward organizations that consistently deliver compassionate and effective care.
Evaluating a Provider's Credibility Online
When you start reviewing websites for potential providers, look for signs of stability and a true commitment to the community. An organization that has served the area for decades shows a level of dedication that newer, for-profit companies might not have.
Look for these key indicators on their website:
- A Long-Standing History: A provider with deep local roots, like Central Coast VNA & Hospice's 74+ years of service, demonstrates a serious long-term commitment to the community.
- Nonprofit Status: As a mission-driven nonprofit, our focus at CCVNA is entirely on patient well-being, not on generating profits for shareholders. This distinction is crucial for ensuring care decisions are always made in the patient's best interest.
- Comprehensive Services: Does the provider offer a full range of care—from home health to hospice? This is important because it means they can support your family as needs change, preventing the stress of having to find a new team later on.
You can learn more about the specifics of our home health care services in Monterey to see how this continuum of care begins.

Tapping Into Community Resources
Beyond professional referrals, don't underestimate the experiences of friends, neighbors, or members of local support groups. A personal recommendation can offer invaluable insight into how an agency truly interacts with families day-to-day.
These are the people who can share stories about the professionalism of the clinical staff, the responsiveness of the office, and the overall compassion of the care team.
When you choose a local, nonprofit provider, you are partnering with an organization that is woven into the fabric of your community. Their reputation is built on decades of trust and successful patient outcomes right here on the Central Coast, from Santa Cruz County to San Benito County.
Ultimately, your goal is to find a team that feels like a true partner. This means gathering information from multiple trusted sources to build a complete picture of who will be coming into your loved one's home.
Essential Questions to Ask Any In-Home Care Agency
That first phone call or meeting with a potential in-home care agency is a big deal. It’s more than just a screening—it’s the start of a relationship built on trust.
Walking in prepared with a solid list of questions is the best way to get a real feel for who they are and whether they’re the right fit for your family. You're not just looking for "aging in place care services near me"; you're looking for a true partner in your loved one's care.

Questions About Your Care Team and Their Qualifications
The clinical staff who will be in your parent’s home are the absolute core of the service. You need to be confident in their skills, the agency’s hiring standards, and how they support their team.
Get specific about who they employ. For an organization like Central Coast VNA & Hospice, this means asking about the distinct roles of Registered Nurses, Hospice Aides, and Medical Social Workers.
- Licensing and Training: "Are all of your clinical team members licensed and bonded? What kind of ongoing training do you provide?"
- Team Consistency: "Will my loved one have a consistent care team, or will different people be visiting each time?"
- Supervision: "How is the clinical staff supervised? Who oversees the care plan—is it a Registered Nurse or a clinical manager?"
- Emergency Protocols: "What happens if there's a medical emergency? What’s your backup plan if a scheduled team member can't make their visit?"
When you find yourself asking, "who offers the best hospice care near me for my aging parent?", the answer almost always comes down to the quality and compassion of the people on the ground. You want to see that an agency truly invests in its staff and prioritizes consistent, relationship-based care.
Understanding the Scope of Services
Next, you need to make sure the agency can handle your family’s specific—and often changing—needs. This is particularly important if you’re looking for a provider that offers a full continuum of care, from home health to palliative and hospice services.
- Customization: "How do you build a personalized plan of care? How often is it reviewed and updated?"
- Service Range: "Do you offer the full spectrum of services—home health, palliative, and hospice—all under one roof?"
- Coordination: "How does your team coordinate with my parent's primary care doctor and any other specialists?"
- Support for Families: "What support do you offer for the rest of the family? Things like education, respite care, or bereavement services?"
For families here in Monterey County and San Benito County, knowing an agency has served the community for over 74 years offers a deep sense of security. That kind of history isn't just a number; it shows a profound understanding of local needs and a lasting commitment.
How to Assess a Provider's Quality and Reputation
Once you have a shortlist of agencies, it's time to dig deeper. You need to look past the glossy brochures and pretty websites to understand the real quality of care your loved one will receive.
This is the most important step in finding reliable aging in place care services near me. This is about making sure your family gets safe, consistent, and genuinely compassionate support.
A non-negotiable starting point? Medicare certification. This is the baseline, confirming the agency meets federal health and safety standards. Any reputable home health or hospice provider you consider must have this.
Differentiating Between Provider Types
Here’s something many families don't think about: the difference between nonprofit and for-profit agencies. As a nonprofit that has served the Central Coast for over 74 years, Central Coast VNA & Hospice operates on a mission, not a profit margin.
Our focus is squarely on patient well-being and community health, not generating returns for shareholders.
That patient-first philosophy has a direct impact on the care we provide. Our resources are reinvested right back into the community—hiring expert clinical staff, providing constant training, and developing programs that meet the specific needs of families in Monterey, San Benito, Santa Cruz, and South Santa Clara Counties.
Reading Between the Lines of Online Reviews
Online reviews can be helpful, but you have to read them with a bit of wisdom. Don't get hung up on one stellar review or one really negative one. Instead, look for patterns.
Are families repeatedly mentioning the professionalism of the Registered Nurses? The kindness of the Hospice Aides? Those consistent themes tell you a lot more about the agency's culture.
The desire for seniors to stay home is growing fast. By 2025, about 75% of Americans over 50 want to age in place, but finding enough qualified staff is a major challenge. You can read more on these home care industry trends to get the bigger picture.
When you're evaluating a provider, think about the entire journey, not just the immediate need. We offer a guide that explains what is hospice care in detail. Finding an agency that excels across the full spectrum of care gives you true peace of mind for whatever comes next.
Navigating the Journey from Home Health to Hospice
Health needs are rarely static. They can change slowly over time or shift in an instant. This is why having a seamless care journey is so critical when you’re looking for aging in place care services near me.
Choosing one organization to handle every stage of care means you won’t be scrambling to find new providers during the most vulnerable moments.
Let's walk through a common scenario. A father comes home from the hospital after a tough battle with pneumonia. Right away, he needs skilled home health nursing to manage his recovery, keep an eye on his breathing, and work with a physical therapist to get his strength back.
The Value of a True Continuum of Care
As he starts to recover, it becomes clear that his underlying heart condition is still causing a lot of fatigue and shortness of breath. He doesn't need the same level of intensive home health anymore, but his quality of life is suffering.
This is the exact moment when a smooth handoff to palliative care makes all the difference. With a provider like Central Coast VNA & Hospice, that transition feels natural.
The palliative team, already up to speed on his medical history, can step in to focus on managing his symptoms. The goal shifts from short-term recovery to long-term comfort, helping him stay as active and engaged as possible.
Later on, if his condition progresses, the family might face the difficult choice to focus entirely on comfort-focused, end-of-life care. Instead of a frantic search for a new agency, they simply transition to the hospice services offered by the same organization they already know and trust.
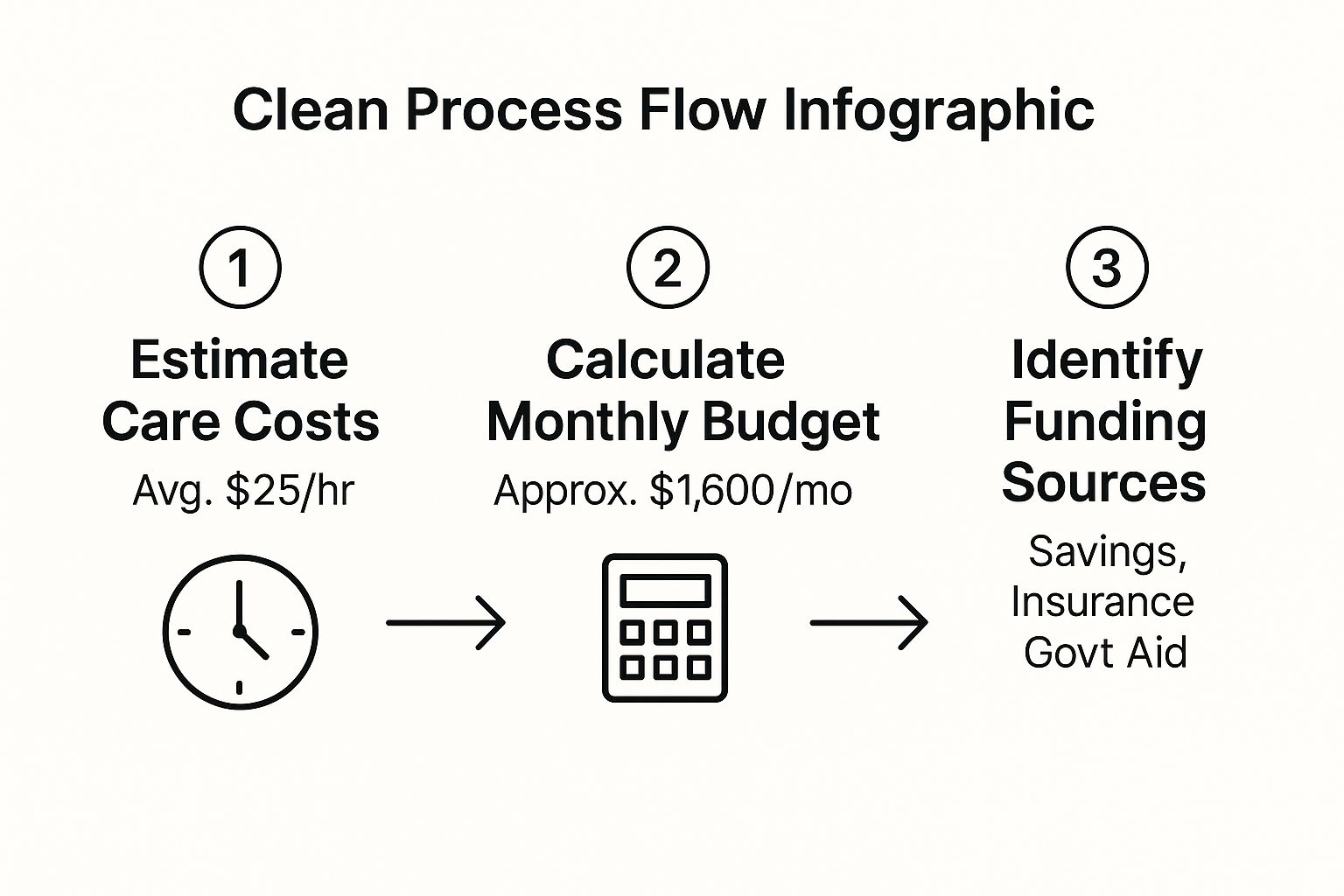
The data in the chart really drives home the need to plan ahead by estimating hourly costs, setting a monthly budget, and looking into all the different ways to fund care.
Integrated Models and Modern Care
This all-in-one approach is quickly becoming the gold standard for high-quality care. The entire aging services field is moving toward models that blend medical and social support to help older adults thrive at home.
As a leading nonprofit with over 74 years of local service, CCVNA was championing this model long before it became a buzzword. You can learn more about these innovative aging services models to see how they're shaping the future of senior care.
A continuum of care means your family builds a relationship with a single, dedicated team. It replaces uncertainty and stress with consistency, trust, and peace of mind, allowing you to focus on your loved one, not on logistics.
For families across Monterey, San Benito, Santa Cruz, and South Santa Clara Counties, this kind of pathway offers profound reassurance. You can learn more about our dedicated hospice care for Veterans and see how we tailor our support to their specific experiences and needs.
Frequently Asked Questions About Aging in Place
When you start exploring in-home care, a lot of questions come up. It's completely normal. As a nonprofit that’s been serving families on the Central Coast for over 74 years, we’ve heard them all.

1. Which service is right: home health, palliative, or hospice care?
This is often the first hurdle, but each service is designed for a very different point in a person's health journey. Here's a simple breakdown:
- Home Health Care: Short-term, skilled support to help someone recover safely at home after a hospital stay, surgery, or new illness.
- Palliative Care: Starts at any stage of a serious illness to manage symptoms and improve quality of life, even during curative treatment.
- Hospice Care: Focus shifts from a cure to comfort and peace at the end of life. Find more detail in our guide on hospice care eligibility.
A professional assessment from a provider like Central Coast VNA & Hospice can clarify your loved one’s specific situation and recommend the right support.
2. Is this care covered by Medicare or other insurance?
Yes, in many cases, it is. Professional medical care provided at home is often covered by insurance.
Medicare Part A and Part B, for example, typically cover 100% of eligible home health and hospice services. Palliative care is also frequently covered, though details can vary by insurance plan. We can help you make sense of your benefits.
3. Who offers the best hospice care near me for my aging parent?
When families ask this, we tell them to look for the key signs of quality care. More often than not, the "best" hospice is a nonprofit, community-based provider with deep roots in the local area.
Look for a long history of service, a comprehensive care team (including Registered Nurses, Hospice Aides, Social Workers, and Chaplains), and a strong reputation in places like Monterey or San Benito County. An organization like CCVNA, with over seven decades of local experience, is built on these patient-first principles.
4. What's different about a nonprofit care provider?
The biggest difference is our mission. As a nonprofit, Central Coast VNA & Hospice puts every resource back into patient care, staff training, and community programs. There are no shareholder profits to worry about.
This model allows us to put the needs of patients and their families in Monterey, San Benito, Santa Cruz, and South Santa Clara Counties above everything else.
5. How do I start the conversation with Central Coast VNA & Hospice?
It couldn't be simpler, and there’s absolutely no pressure or obligation. Just give our office a call to set up a consultation.
Our compassionate team is here to listen to your story, answer every question you have, and guide you through each step. We can help you understand all your options and create a personalized plan of care that feels right for your family.
The journey to find the right aging in place care services near me starts with a single, supportive conversation. The compassionate, expert team at Central Coast VNA & Hospice is here to guide you with decades of experience serving families in Monterey, San Benito, Santa Cruz, and South Santa Clara Counties. Contact us today to learn how we can support your family.
Skilled Nursing at Home: Your Complete Guide to In-Home Care
When a loved one is recovering from an illness or managing a chronic condition, you may think a hospital is the only option for medical care. However, that is not always the case. Skilled nursing at home offers a powerful alternative, bringing clinical expertise into the comfort of a person’s own home.
This care is delivered by licensed professionals like Registered Nurses, providing compassionate support where patients feel most at ease.
What Does Skilled Nursing at Home Really Mean?
Skilled nursing at home is a specific type of medical care that licensed health professionals provide inside a patient's residence. This is clinical care prescribed by a doctor to help someone recover from surgery, heal from an injury, or manage a complex health issue. It is not about assistance with daily chores.
It helps to think about the difference this way: personal home care focuses on life’s necessities, like preparing meals or running errands. Skilled nursing, on the other hand, is like having a member of the hospital's clinical team come to your home to handle medical needs.
For families across Monterey County, San Benito County, Santa Cruz County, and South Santa Clara County, understanding this distinction is key. It ensures your loved one gets the right level of support to heal safely and live as independently as possible.
Comparing Skilled Nursing and Personal Care
To make it even clearer, let's break down how these two types of care differ. One is medical in nature, while the other provides non-medical support for daily living.
| Feature | Skilled Nursing at Home (CCVNA) | Personal Care / Companion Care |
|---|---|---|
| Type of Services | Medical treatments like wound care, IV therapy, injections, medication management, and patient education. | Non-medical help with daily activities like bathing, dressing, meal prep, light housekeeping, and errands. |
| Provider Qualifications | Provided by licensed medical professionals like Registered Nurses (RNs) or Licensed Vocational Nurses (LVNs). | Provided by individuals who may have some training but are not licensed medical professionals. |
| Typical Patient Needs | Patients recovering from surgery, managing a chronic illness (e.g., heart failure, COPD), or needing complex medical procedures at home. | Seniors needing help to live safely at home, individuals with disabilities, or those needing companionship and basic assistance. |
As you can see, the choice between them really comes down to the specific, doctor-ordered needs of the patient.
Medical Expertise in a Familiar Setting
The purpose of skilled nursing at home is to deliver medical care that would otherwise require a stay in a clinical facility. It’s a vital service for anyone who wants to recover surrounded by the familiarity and comfort of their own home.
This isn't a niche preference. In fact, a study by the National Hospice and Palliative Care Organization (NHPCO) found that 88% of adults prefer to receive end-of-life care in their homes (NHPCO, 2022).
This image really highlights the core components of skilled nursing care at home.
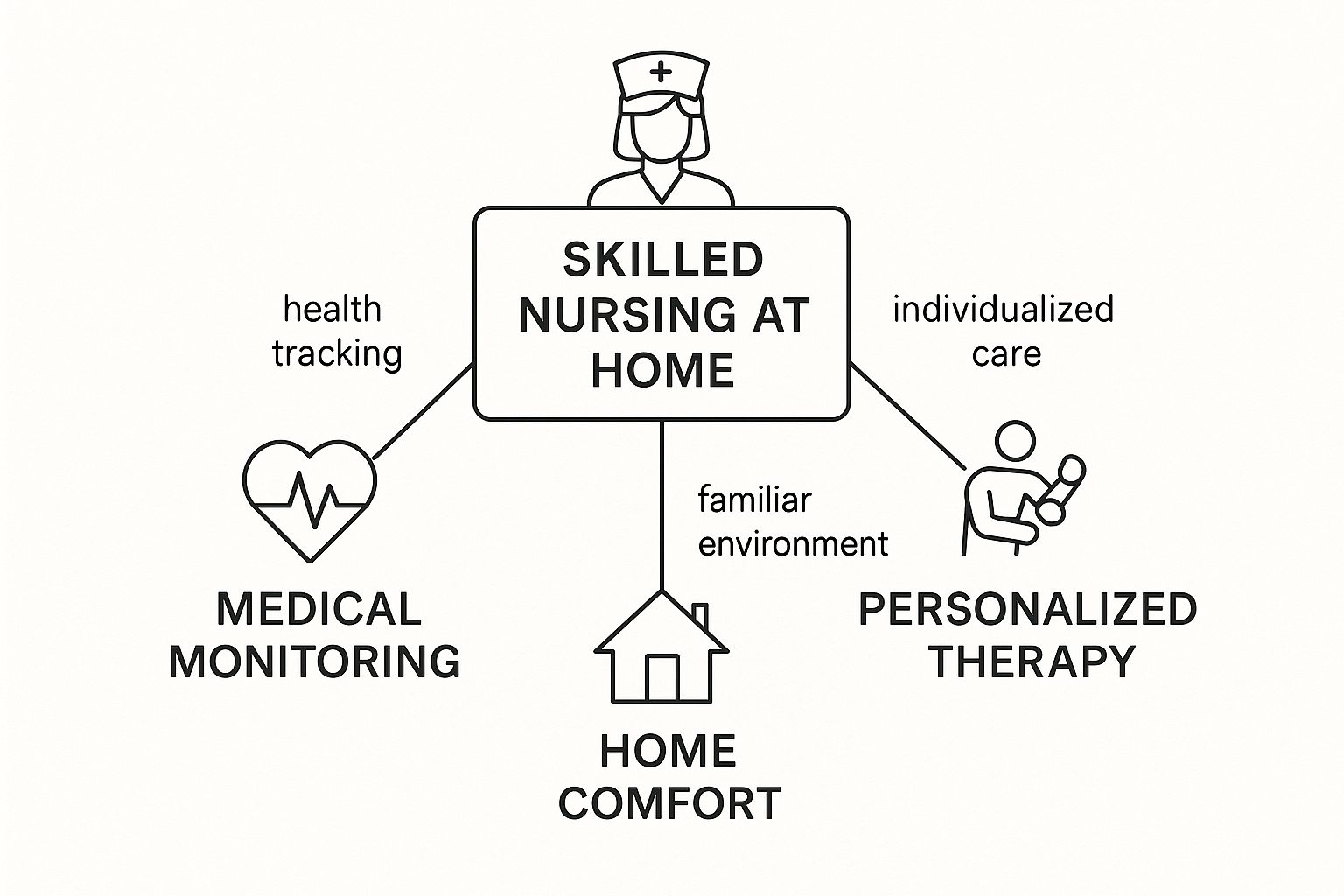
It’s about blending that crucial medical monitoring and therapy with the healing environment of home, creating a complete support system for recovery.
The Central Coast VNA & Hospice Approach
For more than 74 years, Central Coast VNA & Hospice has been this region's trusted nonprofit provider for these essential services. Our mission is to offer compassionate, high-quality medical care that honors every person’s wish for independence and comfort. Our team of Registered Nurses and other licensed professionals works directly with your physician to build a personalized care plan.
This personalized plan might include services like:
- Wound Care: Carefully dressing and watching over surgical wounds or pressure sores to prevent infection and help them heal properly.
- IV Therapy and Injections: Administering medications, fluids, or nutrition through an IV, a task that absolutely requires a licensed professional.
- Disease Management: Teaching patients and their families how to manage long-term conditions like diabetes, heart failure, or COPD.
- Post-Surgical Care: Monitoring vital signs, managing pain, and ensuring a safe and steady recovery after being discharged from the hospital.
By bringing this level of professional care into the home, we help people avoid frustrating and costly readmissions to the hospital and get back on their feet faster. It puts patients back in the driver's seat of their own recovery journey.
This focus on empowerment is crucial for helping people help seniors live at home safely and with dignity. Because of our deep local roots and nonprofit status, CCVNA's focus will always be on the health of the communities we are proud to serve.
Who Benefits Most from In-Home Skilled Nursing?
Skilled nursing at home is a powerful service designed for people who need medical care but can receive it safely outside of a hospital. It acts as a bridge, connecting the clinical support of a hospital to the healing environment of home. This service is vital for helping people transition after a hospital stay and manage chronic illnesses.
It's especially valuable for those recovering from a major medical event. Being in a familiar, comfortable space can make a world of difference, often improving well-being and speeding up the healing process.
Patients Recovering from Surgery or Injury
One of the most common reasons for skilled nursing at home is for support after surgery or a serious injury.
Imagine a grandfather in Monterey County who just had joint replacement surgery. A Registered Nurse from Central Coast VNA & Hospice can visit him at home instead of him facing a long rehab stay.
This nurse would provide critical post-op care, including:
- Wound Care: Changing dressings, watching for any signs of infection, and making sure the surgical site is healing properly.
- Pain Management: Coordinating with his doctor to manage pain effectively, which is key to being able to participate in physical therapy.
- Mobility Support: Helping him move safely and guiding him through exercises to regain strength and prevent complications like blood clots.
This direct, professional support at home can make recovery smoother and helps prevent setbacks. For families, it offers peace of mind to know a medical expert is monitoring their loved one’s progress.
Individuals Managing Chronic Health Conditions
For people living with long-term illnesses, skilled nursing at home is a game-changer. It provides the steady medical oversight and education they need to manage complex conditions. This empowers them to stay in control of their own health.
Take, for instance, a mother in San Benito County recently diagnosed with diabetes. A skilled nurse can offer personalized support in her own kitchen, helping her build the confidence to manage it all. The same goes for someone with a chronic heart condition or COPD, as regular monitoring can help them avoid frequent hospital trips.
These services fundamentally shift healthcare from being reactive to proactive. By catching potential issues early and teaching people how to effectively manage their own health, skilled nursing helps them live fuller, more stable lives right where they want to be—at home.
The need for this kind of long-term support is on the rise. It's estimated that two out of three older adults with disabilities already get their long-term care services at home. This highlights a significant shift toward home-based medical care. You can explore more about these trends and the growing importance of home-based support.
Patients with Complex Medical Needs
Sometimes, a person’s medical needs are too complex for family to handle safely. Skilled nursing at home bridges this gap, bringing high-level medical treatments into the home.
This includes care for patients who need:
- IV Therapy: Receiving antibiotics, hydration, or nutrition through an intravenous line.
- Catheter or Ostomy Care: Managing and maintaining catheters or ostomy bags to prevent infections and keep the patient comfortable.
- Specialized Injections: Administering medications that demand precise dosages and techniques.
For people in Santa Cruz County or South Santa Clara County facing these challenges, having a provider like Central Coast VNA & Hospice means they can receive these treatments at home. It’s all about ensuring every person can get the expert care they need, wherever they call home.
What’s Included in a Skilled Nursing Plan?

When a doctor orders skilled nursing at home, they prescribe a personalized roadmap for recovery. This is a dynamic plan of care focused on helping someone heal and regain independence at home.
At Central Coast VNA & Hospice, our nonprofit mission is about more than just checking boxes. Our Registered Nurses see themselves as partners in health, empowering patients and families. Every service is delivered with a focus on healing the whole person.
Expert Wound Care for Safer Healing
Proper wound care is essential after surgery or a hospital stay and is a cornerstone of skilled nursing. A skilled nurse is trained to assess a wound, clean it with sterile techniques, and apply the right dressings.
Why is this so critical? An infected wound can lead to serious complications, prolonging recovery and even causing rehospitalization. By managing wounds expertly at home, our nurses help patients across Monterey and Santa Cruz counties heal safely.
Medication Management and Education
Juggling multiple prescriptions can be overwhelming and dangerous, especially with new medications after a hospital stay. A skilled nurse brings clarity and safety, ensuring medications are taken correctly and watching for side effects. They also teach the patient and family what each drug is for.
This service is about empowerment, not just dispensing pills. It helps a patient in San Benito County understand their treatment. That knowledge reduces medication errors and gives patients confidence to take an active role in their health.
A skilled nursing plan transforms a confusing medication schedule into a clear, manageable routine, ensuring safety and promoting patient independence. This proactive approach is a hallmark of high-quality skilled nursing at home.
Advanced Clinical Interventions
Many medical treatments that once required a hospital can now be performed safely at home by a licensed professional. This allows people to remain where they feel most comfortable. These advanced services showcase the clinical expertise a home health agency can provide.
Our skilled nurses at CCVNA are proficient in various complex clinical tasks, including:
- IV Therapy and Injections: Administering IV antibiotics, hydration, and other vital medications as prescribed.
- Catheter and Ostomy Care: Providing meticulous care to prevent infections while ensuring patient comfort and dignity.
- Disease-Specific Education: Teaching patients and families how to manage chronic conditions like heart failure, COPD, or diabetes.
Many of our care plans now also incorporate advanced remote patient monitoring systems for an extra layer of oversight. These tools let our team keep a close eye on patients in South Santa Clara County and beyond. This helps us catch potential problems before they become emergencies.
By bringing this high level of clinical skill into the home, we help people avoid rehospitalization and maintain their quality of life. Learn more about our comprehensive home health care services and how they can support your family's recovery.
Understanding Your Compassionate Home Health Team
Effective skilled nursing at home is a team effort. Real recovery is built on the expertise of dedicated professionals who work together to support a patient's journey back to health. This team approach ensures that every part of a person’s well-being is addressed with expert care.
At Central Coast VNA & Hospice, our model is built on this idea. For over 74 years, our nonprofit, mission-driven team has provided this integrated support. We know recovery is about more than just healing; it’s about restoring confidence and function for families across Monterey County, San Benito County, and our entire service area.
Who Is on Your Home Health Team?
Your home health team is a group of specialists, each with a unique skill set, all coordinated by a Registered Nurse. They work closely with each other and your doctor to create a seamless care experience. Think of them as a personal support system focused on one goal: your loved one’s successful recovery at home.
The professionals involved will depend on the patient's individual needs as outlined in their physician-ordered plan of care. This ensures the care is always personalized and effective.
Here’s a look at the key professionals who may be part of your compassionate care team:
- Physical Therapists (PTs): These experts focus on restoring mobility and strength. They help patients regain the ability to walk safely, climb stairs, and get in and out of bed.
- Occupational Therapists (OTs): OTs help patients relearn essential activities of daily living. This could mean adapting the home or teaching new techniques for tasks like dressing or bathing.
- Speech-Language Pathologists (SLPs): Following a stroke, SLPs work with patients to recover their ability to speak, understand language, or swallow safely.
- Medical Social Workers (MSWs): These professionals provide crucial emotional and social support. They connect families with community resources and help with advance care planning.
- Hospice Aides: Under the supervision of a Registered Nurse, Hospice Aides provide essential personal care to support comfort and dignity.
This interdisciplinary approach is the cornerstone of high-quality home health care. It guarantees that care is holistic, addressing not just the medical diagnosis but the entire person and their environment.
A Coordinated Approach to Care
The real magic of a home health team is its coordination. Team members are in constant communication, sharing updates and adjusting the care plan as needed. For example, a Physical Therapist might notice a patient is discouraged and can pass that to the Medical Social Worker for emotional support.
This coordinated effort is managed meticulously. A key part of a competent home health team is maintaining accurate patient records. Exploring advancements like specialized medical documentation software shows how modern teams manage this task, ensuring every detail is tracked.
This level of collaboration prevents fragmented care and ensures a smooth journey. Our deep local roots in Santa Cruz County and South Santa Clara County mean we are intimately familiar with local resources.
When you choose Central Coast VNA & Hospice, you get an entire team of advocates. Explore our home health care in Monterey to see how we support families like yours.
How to Navigate Medicare for Home Health Services

Figuring out the financial side of healthcare can be stressful. For many families, Medicare is the key to getting essential skilled nursing at home, but its rules can feel like a maze. The good news is that with the right guide, the process is far less intimidating.
At Central Coast VNA & Hospice, our nonprofit mission is to help families in Monterey County and surrounding communities get the care they’re entitled to. We believe in empowering you with clear, compassionate information so you can make confident choices.
What Does Medicare Require for Coverage?
For Medicare to cover skilled nursing care at home, a few specific conditions must be met. The official language might sound formal, but the ideas are straightforward.
First, a doctor must certify that the patient needs this medical care and create an official plan of care. After that, the patient needs to meet two main conditions:
- Be considered "homebound": This doesn't mean you're a prisoner in your home. It means leaving takes a considerable and taxing effort due to illness or injury.
- Need "intermittent" skilled care: This means the care needed is from a licensed professional, like a Registered Nurse or therapist, on a part-time basis.
We work directly with your doctor to ensure all criteria are properly documented, lifting that burden from your shoulders. For a deeper dive, check out our guide on qualifying for home health care to see the specifics.
Understanding Key Terms in Plain Language
The term “homebound” often trips people up, but Medicare’s definition is practical. Someone can still be considered homebound if they leave for doctor’s appointments, religious services, or an occasional trip to the barber. The key is that leaving home is a significant challenge.
“Intermittent skilled need” refers to medical tasks that only a licensed professional can perform safely. This includes wound care, IV therapy, or injections.
Think of it this way: Medicare’s goal is to provide the necessary medical support to help someone recover or stabilize in the most appropriate and cost-effective setting. For many, that setting is their own home.
This focus on home-based care is more important than ever. The global skilled nursing market is expected to grow significantly, fueled by the growing population of older adults needing specialized support. You can learn more about the global trends in skilled nursing care to see what’s driving this change.
As the trusted nonprofit provider for the Central Coast for over 74 years, we are here to help you through this. Our teams are committed to clarifying your options and helping you access every benefit you deserve.
Choosing the Right Central Coast Home Health Agency
Deciding on a provider for skilled nursing at home is a critical healthcare choice. It’s not just about clinical services; it’s about inviting someone into your home during a vulnerable time. You need a relationship based on trust, reliability, and genuine compassion.
Making the right choice starts with knowing what to ask. Any agency worth considering should be transparent and ready to answer your questions clearly.
Key Questions to Ask Any Home Health Agency
Think of this process as an interview. Your goal is to assess their qualifications, processes, and philosophy of care. This will help you find a perfect match for your family's needs.
Here are the essential questions that should guide your conversation:
- Accreditation and Licensing: Is the agency Medicare-certified and licensed by the state? This is the baseline requirement for meeting federal health and safety standards.
- Staff Credentials and Training: Who exactly will be coming into your home? Ask about the qualifications of their Registered Nurses and other clinicians.
- Emergency Preparedness: What happens if there's a medical emergency? A good agency will have a clear protocol for a rapid and effective response.
- Communication Practices: How will the clinical team keep you and the doctor in the loop? A solid communication plan shows respect for your role in the care journey.
- Personalized Care Planning: How is the plan of care created and adjusted? The best care should be a collaborative effort including the patient, family, and doctor.
Finding the right partner means looking beyond clinical skills. You want an agency that shows a deep commitment to compassionate, patient-centered support. This is the difference between simply receiving services and feeling truly cared for.
The Central Coast VNA & Hospice Difference
For families in Monterey County, San Benito County, Santa Cruz County, and South Santa Clara County, CCVNA has been that trusted partner for generations. As a local nonprofit with over 74 years of service, our mission is focused on our community’s well-being, not profits.
Our deep roots and mission-driven purpose are what truly set us apart. We don’t just provide care; we build lasting relationships founded on trust and respect. We ensure every patient receives care that is not only clinically excellent but also delivered with warmth and genuine compassion.
Choosing an agency is a big decision. For more in-depth advice, you can review our guide on finding the best home health agency for seniors to help you move forward with confidence.
Contact Central Coast VNA & Hospice today to learn more about our commitment to your family’s health and peace of mind.
Frequently Asked Questions About Skilled Nursing at Home

Exploring in-home medical care is a big step, and it’s normal to have questions. Getting clear, straightforward answers brings confidence and peace of mind. We've gathered some common questions we hear about skilled nursing at home to help you.
Here at Central Coast VNA & Hospice, our mission is to empower you with information. As a trusted nonprofit serving the Central Coast for over 74 years, we believe in transparent and compassionate guidance.
How is skilled nursing different from hospice care?
While both involve expert medical care at home, they serve different purposes. Skilled nursing focuses on recovery and rehabilitation after an illness, surgery, or injury. The goal is to help a person heal and regain independence.
Hospice care, on the other hand, is for individuals with a life-limiting illness when a cure is no longer the focus. Hospice care aims to provide comfort, manage symptoms, and ensure the best possible quality of life.
How long can my loved one receive skilled nursing services?
The duration of skilled nursing care depends on medical need, not a set schedule. Services continue as long as a physician's plan of care documents a need for professional medical support.
As your loved one recovers, visits may decrease. The service ends when health goals are met, their condition stabilizes, or they no longer need a licensed clinician for their care.
What does 'homebound' mean for Medicare purposes?
The term "homebound" can be confusing. For Medicare, it means leaving home requires a considerable and taxing effort due to illness or injury.
A person can still be homebound even if they leave for medical appointments, religious services, or occasional short trips. The key factor is the difficulty of leaving home, not a strict rule against it.
Can our family doctor request services from CCVNA?
Yes, absolutely. A referral from a physician is required to start any skilled nursing service. This ensures the care is medically necessary and fits into the patient's overall health plan.
We have a long history of working closely with doctors throughout Monterey County, San Benito County, Santa Cruz County, and South Santa Clara County. These partnerships create a coordinated team approach to recovery.
What if my loved one’s needs change during care?
Health needs can change, and our team is built to adapt. During every visit, our clinicians are constantly assessing the patient's condition.
If they improve, we work with their doctor to adjust the care plan. If needs become more complex, we modify the plan to provide more support. This might lead to a conversation about transitioning to a different level of care, like palliative or hospice services, ensuring they always have the most appropriate support.
For over 74 years, Central Coast VNA & Hospice has been the trusted nonprofit provider of in-home medical care for our communities. If you have more questions or believe your family could benefit from our services, please reach out.
Contact us today to learn how we can help.
A Guide to Palliative Home Health: Improving Quality of Life at Home
When you or a loved one is living with a serious illness, it can feel like your entire world has been turned upside down. Between the constant doctor's appointments, a confusing array of medications, and the sheer physical and emotional toll, it’s easy to feel overwhelmed.
This is where palliative home health comes in. It’s a specialized type of medical care that adds an extra, crucial layer of support, all from the comfort of your own home. The focus is simple but profound: to relieve the symptoms, pain, and stress of a serious illness, ultimately improving the quality of life for both you and your family.
Defining Palliative Care at Home

It’s a common and understandable point of confusion, but palliative care is not the same thing as hospice. They are two distinct philosophies of care designed for different stages of a health journey.
The most important difference is this: palliative care is available at any age and at any stage of a serious illness, and you can receive it right alongside treatments meant to cure you. Hospice care, on the other hand, is for individuals who have decided to no longer seek curative treatment and have a life expectancy of six months or less.
Palliative Home Health vs. Hospice Care at a Glance
To help clarify, here's a quick comparison of the two:
| Care Aspect | Palliative Home Health | Hospice Care |
|---|---|---|
| Timing of Care | Can begin at diagnosis and be provided alongside curative treatment. | Begins after stopping curative treatment, typically with a prognosis of 6 months or less. |
| Primary Goal | To improve quality of life and relieve symptoms of a serious illness. | To provide comfort and support at the end of life. |
| Treatment Focus | Works in conjunction with curative treatments (chemotherapy, dialysis, etc.). | Focuses exclusively on comfort care and symptom management; curative treatments are stopped. |
| Patient Eligibility | Anyone with a serious, chronic, or complex illness, regardless of prognosis. | Individuals with a terminal illness and a life expectancy of 6 months or less. |
Understanding this distinction is key for families to access the right support at the right time. Palliative care is about adding support, not taking away hope.
Your Extra Layer of Support
Think of palliative home health as a dedicated support team focused entirely on your comfort and well-being. This isn't about giving up on your recovery; it's about gaining more control over your day-to-day life and finding genuine relief from the burdens of your condition. A palliative care team creates a plan that is clear and individualized, reflecting your needs, preferences, and goals. This focus on the whole person—not just the disease—is what makes this type of care so impactful.
For over 74 years, Central Coast VNA & Hospice has delivered this exact kind of mission-driven, nonprofit care. Our skilled teams of Registered Nurses, Medical Social Workers, and other compassionate professionals serve patients across Monterey County, San Benito County, Santa Cruz County, and South Santa Clara County.
Our primary goal is to improve your quality of life by:
- Managing complex symptoms like pain, fatigue, nausea, and shortness of breath.
- Providing vital emotional and spiritual support for both you and your family.
- Coordinating care between all of your different doctors and specialists to ensure everyone is on the same page.
- Helping you navigate difficult medical decisions so you feel empowered and informed.
This collaborative approach ensures your care is seamless and that your voice is always at the center of the conversation. To learn more, explore the details of our palliative care services.
The Real Benefits of Receiving Care at Home
Navigating a serious illness often means a whirlwind of doctor's offices, hospital stays, and medical tests. It's draining, to say the least. Palliative home health care offers a different path—one that allows you or your loved one to manage symptoms and stress from the most healing place there is: home.
This isn't just about convenience. It’s about getting back a sense of control and normalcy. Being in your own space, surrounded by family, and sticking to familiar routines can dramatically lower stress and anxiety, often leading to fewer ER trips and hospital stays.
Improving Quality of Life Daily
The most significant benefit of in-home palliative support is its focus on your overall quality of life. This goes way beyond just treating pain or nausea with medication. It’s about figuring out how those symptoms are getting in the way of what matters to you, whether that's enjoying a meal or tending to your garden.
At Central Coast VNA & Hospice, our teams of Registered Nurses and Medical Social Workers look at the whole picture. We work not only to ease physical symptoms but also to provide the emotional and practical support that brings back peace of mind and dignity.
The core of palliative home health is its patient-centered philosophy. It empowers you and your family to take a more active role in the care journey, ensuring that your personal values and goals guide every decision.
This personalized care is becoming recognized as a vital part of modern healthcare. The global need for these services is on the rise, with the palliative care market expected to hit USD 18.9 billion by 2032 (Dataintelo, 2024). This trend shows a growing understanding of how supportive care truly helps people living with chronic illness. You can find more details on this trend from the global palliative care market report.
A Collaborative and Supportive Team
Our team approach is all about providing complete, wrap-around support. For our patients in Monterey County, San Benito County, Santa Cruz County, and South Santa Clara County, that means you have a dedicated group of professionals all working together on a single, unified care plan.
Think of this plan as a living document that changes as your needs do. It makes sure everyone—from your family doctor to your CCVNA nurse—is on the same page. This level of coordination is key to managing symptoms well and helping you feel more secure and supported every step of the way. To see how this fits into our broader mission, take a look at our home health care services and get the full picture of the support we offer.
Who Can Benefit From Palliative Home Health?

One of the biggest misunderstandings about palliative care is that it's only for the end of life. That couldn’t be further from the truth. Eligibility for palliative home health isn't about a person's prognosis; it's all about their current quality of life and the challenges of living with a serious illness.
If you or a loved one is living with a condition that causes difficult symptoms and makes daily life a struggle, you are likely a candidate. The whole point is to provide relief and support right now, regardless of what the long-term outlook might be.
Recognizing the Need for Support
It can be tough to admit when you need extra help, but palliative care is specifically designed to be brought in early on in a health journey. It works hand-in-hand with your current medical treatments, adding a layer of support, not replacing them.
You may benefit from palliative care if you are dealing with:
- A serious illness: Conditions like cancer, chronic heart failure (CHF), COPD, kidney disease, dementia, or ALS often bring a heavy symptom burden that’s hard to manage alone.
- Difficult-to-manage symptoms: This can be anything from persistent pain, shortness of breath, and fatigue to nausea, loss of appetite, or anxiety that gets in the way of your day.
- Frequent hospitalizations: If you’re making regular trips to the ER or being admitted to the hospital, palliative care at home can help manage symptoms before they reach a crisis point.
The key thing to remember is that you can—and absolutely should—seek this support while still pursuing treatments meant to cure, like chemotherapy or dialysis. For families across the Central Coast, from Monterey to Santa Cruz County, simply recognizing these signs is the first and most important step toward a better quality of life.
Who Is a Good Candidate?
Palliative home health is for anyone whose physical and emotional well-being is being worn down by a serious medical condition. Think of someone going through cancer treatment who is struggling with severe nausea and fatigue. A palliative team can step in to manage those side effects, making it possible for them to continue their life-saving therapy with far greater comfort.
Or, consider someone with advanced heart failure who experiences constant shortness of breath and the anxiety that comes with it. A palliative team can provide medication management and coping strategies right at home, which often reduces those stressful, late-night trips to the emergency room. This is completely different from end-of-life care, a topic you can learn more about by understanding what hospice care is and how it serves a very distinct purpose.
Ultimately, if an illness is getting in the way of living your life, palliative care can help. The best way to know for sure is to talk with your doctor or contact Central Coast VNA & Hospice directly to see if this supportive service is the right fit for your family.
Meet Your Compassionate Care Team
When you choose palliative home health, you're not just getting a single professional. You're bringing an entire team of dedicated professionals into your corner. This group works in concert to build a care plan that looks beyond physical symptoms to address the emotional, social, and spiritual weight that a serious illness can bring.
At Central Coast VNA & Hospice, this is the heart of what we do. With over 74 years of nonprofit service across Monterey, San Benito, Santa Cruz, and South Santa Clara Counties, we’ve learned that real comfort means caring for the whole person. Think of your team as a circle of support, walking right beside you and your family on this journey.
Who Is on Your Palliative Care Team?
Each person on your team has a unique role and a special set of skills, making sure every part of your well-being is looked after. It's an integrated approach designed so that nothing falls through the cracks and your care feels as seamless as possible.
Your core team will generally include:
- Registered Nurse (Case Manager): This is your go-to person. They’re experts in managing pain and other symptoms, explaining medications, and coordinating all the clinical pieces of your care.
- Medical Social Worker: They provide a steady hand for emotional support and counseling. They also help with the practical side of things, like figuring out insurance or connecting you with helpful community resources.
- Chaplain: Offering nondenominational spiritual support, our chaplains are here to help you and your family find a sense of peace and meaning, whatever your personal beliefs may be.
- Home Health Aide: These compassionate professionals assist with personal tasks like bathing and dressing. Their help preserves dignity and eases the daily physical burden on family members.
Working Together for You
The real power of palliative care is how these different experts come together. For instance, your Registered Nurse might notice that your pain seems worse when you're feeling anxious. They can then pull in the Medical Social Worker to explore coping strategies while the Chaplain offers spiritual comfort, tackling the root of the distress from every angle.
This wrap-around support model is what defines high-quality palliative care. It’s a commitment to your total well-being, ensuring that physical relief is matched with emotional and spiritual peace. For this to work, great communication is essential. The team has to be in constant contact, sharing insights and adjusting the plan as your needs change.
This level of teamwork is becoming more important than ever as families seek out more complete support. In fact, the global palliative care market is projected to hit $265 billion by 2031 (iHealthcareAnalyst, 2024), a clear sign that more people are recognizing the need for this kind of multidimensional care. You can learn more about this trend by reading the full research on the global palliative care market.
Your Palliative Care Journey Step by Step
Starting a new kind of care can feel like a lot to take in, but beginning palliative home health is a clear, supportive process that always puts you first. At Central Coast VNA & Hospice, we walk you through every step, making sure there's no confusion. We want you and your family to feel confident and secure, knowing we're in this together.
It all starts with a simple referral. This can come straight from your doctor, or you or a family member can request it. Once we have it, our team gets in touch to set up an initial conversation. That first meeting is really all about listening to hear about your health challenges and understand your personal goals.
Developing Your Personalized Care Plan
After our initial talk, our interdisciplinary team works together to map out your personalized care plan. This isn't some one-size-fits-all document; it’s a living, breathing roadmap built entirely around what you need and want. The plan outlines exactly how we'll manage your symptoms, how often your Registered Nurse and other team members will visit, and how we'll coordinate everything with your other doctors.
You and your family are at the very center of this planning. Nothing is decided without your input and approval. This plan becomes our shared guide to making your quality of life the best it can be.
This infographic gives a simple snapshot of how we track your progress and adjust your care to keep you comfortable and meet your goals.
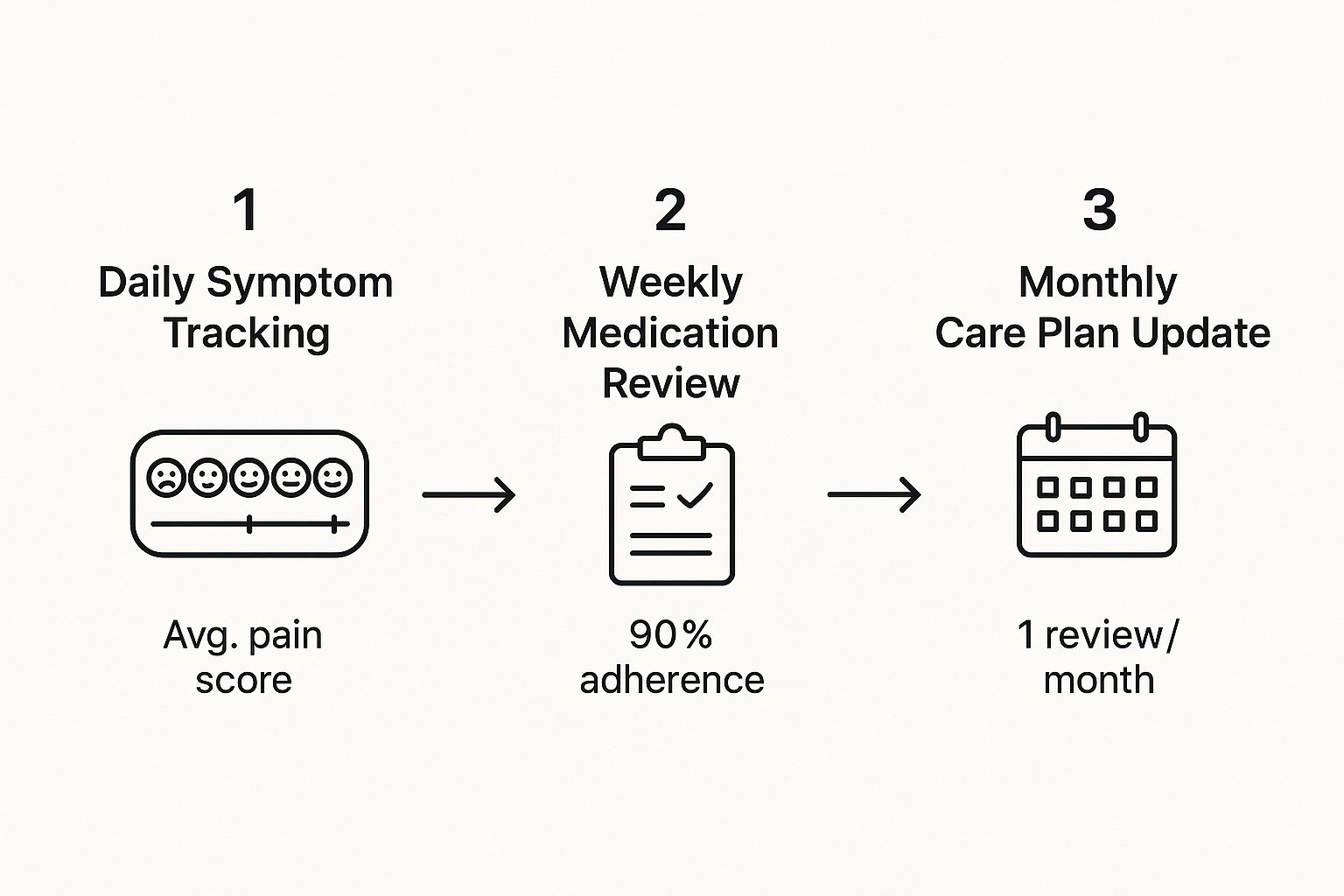
As the image shows, it's a continuous cycle of monitoring symptoms, reviewing medications, and updating your plan. This ensures your care is always in sync with your current needs. For many, an important part of the palliative care journey involves making sure future wishes are understood and honored. Using an end-of-life planning checklist can be a huge help in guiding those important family conversations.
Regular Visits and Ongoing Support
Once your care plan is set, your team will start making regular home visits. These visits are much more than just medical check-ins; they're our chance to build a real, trusting relationship with you. Your Registered Nurse will assess symptoms and manage medications, while other team members are there to provide emotional and practical support.
Your palliative home health team is a consistent, reliable presence in your life. We are your advocates, partners, and a constant source of support, available by phone whenever you need us between scheduled visits. This steady support, delivered right in the comfort of your home in Monterey County, San Benito County, or our other service areas, is what makes the journey manageable.
How Is Palliative Home Health Funded?

When families first consider palliative home health, one of the very first questions that comes up is, "How are we going to pay for this?" It's a completely valid concern. Financial worries should never stand in the way of getting the comfort and support your family needs.
The good news is that palliative care is recognized as a medical specialty, just like cardiology or oncology. This means it's generally covered by Medicare Part B, Medi-Cal, and most private insurance plans. Our team at Central Coast VNA & Hospice is here to help you make sense of your specific coverage and clear up any financial questions you have.
How Insurance Covers Palliative Services
It helps to think about palliative care coverage in the same way you would for any other specialist visit. Your plan helps pay for the services of our expert team, which includes Registered Nurses and Medical Social Workers who work right alongside your primary doctor.
It’s really important to know that this is completely separate from the Medicare Hospice Benefit. Palliative care is a distinct service you can receive while you are still pursuing treatments to cure your illness, and the way it's funded reflects that. Getting this distinction right is key to accessing the proper care at the right time. For more on end-of-life care funding, you can learn more about how hospice care is funded in our detailed guide.
The most important thing to remember is that palliative care is a covered medical service designed to be accessible. For families here in Monterey, San Benito, Santa Cruz, and South Santa Clara counties, our commitment as a nonprofit is to give you clear, straightforward information. We believe in empowering you with the knowledge to make confident decisions about your health and well-being.
Frequently Asked Questions About Palliative Home Health
When you're navigating a serious illness, it’s natural to have a lot of questions. We’ve put together answers to some of the most common ones we hear from families considering palliative home health. Our goal is to give you clarity and confidence as you explore your options.
Can I Keep My Current Doctor?
Yes, absolutely. Think of our palliative team as an extra layer of support for you and your family. We work with your primary doctor and any specialists you’re already seeing, supplementing the trusted medical relationships you've built—not replacing them.
Do I Have to Stop My Other Treatments?
No, you don’t. This is one of the biggest differences between palliative care and hospice. You can receive palliative home health while you’re actively pursuing treatments meant to cure or control your illness, like chemotherapy or radiation.
How Often Will the Palliative Team Visit?
The frequency of our visits is built around you. After our first assessment, we’ll work with you and your family to create a personalized visit plan. If your needs change, we adjust the schedule, and we’re always just a phone call away between visits.
Is Palliative Care Only for Cancer?
Not at all. Palliative care is here to support anyone living with the challenges of a serious illness. We often help people with conditions like heart failure (CHF), COPD, kidney disease, Alzheimer's or other dementias, and ALS (Lou Gehrig's disease).
Who Is on the Palliative Care Team?
Your team is a group of specialists working together for you. It typically includes a Registered Nurse for symptom management, a Medical Social Worker for emotional and practical support, a Chaplain for spiritual care, and a Home Health Aide for personal care assistance.
How Do We Get Started With Central Coast VNA & Hospice?
Getting started is simple. You can ask your doctor for a referral to Central Coast VNA & Hospice for palliative care, or you can just give us a call directly. Our team is ready to walk you through the process and answer any other questions you might have for our service areas in Monterey County, San Benito County, Santa Cruz County, or South Santa Clara County.
Are you ready to add an extra layer of compassionate support to your care journey? The team at Central Coast VNA & Hospice is here to help you live more comfortably and with greater peace of mind. Learn more about our services and contact us today.
Senior Home Care to Age in Place: A Guide to Thriving at Home
For many older adults, the idea of leaving their home is simply out of the question. Senior home care makes it possible to get the skilled medical support and personal help they need, all without leaving the comfort and familiarity of the place they love. It's an approach that champions independence and dignity. It gives countless families a way to help their loved ones manage health challenges while living a safe, fulfilling life.
Staying Home: How In-Home Care Fosters Independence

There's a powerful emotional connection to home. It’s where memories are made, routines are established, and life feels most comfortable. This desire to "age in place" isn't just about familiarity; it’s about holding onto a sense of self and control. Professional senior home care is what makes this a safe, practical reality instead of just a wish.
This isn't a niche preference, either. The numbers show it's what most people want. According to AARP, approximately 75% of Americans over age 50 say they want to stay in their homes as they get older (AARP, 2021). This underscores the critical need for reliable in-home care services.
For families across Monterey County, San Benito County, Santa Cruz County, and South Santa Clara County, Central Coast VNA & Hospice has been the go-to nonprofit partner for over 74 years. Our entire mission is built around providing the clinical expertise that allows people to age successfully right where they want to be.
The Real-World Impact of Professional Home Support
Choosing home care over a facility often comes with huge emotional and practical benefits. It means your loved one can stay surrounded by their own memories, pets, and neighborhood connections. This is incredibly important for their well-being and helps avoid the stress of moving to an unfamiliar environment.
But the support from a professional team goes far beyond just meeting basic needs. It’s about building a solid foundation for health and true independence.
At the end of the day, senior home care is about respecting a person's life and choices. It delivers the structured, clinical support required to manage health conditions well, giving families genuine peace of mind and helping seniors live confidently in the one place they love most.
Our services bring expert medical care directly to the front door. A dedicated team, led by a Registered Nurse, can provide a variety of clinical services at home, including:
- Skilled Nursing: Handling tasks like complex medication schedules, wound care, and close monitoring of chronic conditions like heart failure or COPD.
- Rehabilitative Therapies: Physical and occupational therapy to rebuild strength, improve mobility, and reduce the risk of falls.
- Personalized Care Planning: A team effort between the patient, their family, and their doctor to create and work toward specific health goals.
By integrating this level of professional support into the home, Central Coast VNA & Hospice helps seniors do more than just live—we help them thrive. Our focus is on creating a safe environment that encourages long-term wellness. Explore our guide on how to help seniors live at home safely to learn more.
Figuring Out Your Family's Specific Care Needs

Before you can arrange for senior home care to age in place, you first need to figure out what kind of support is actually necessary. This starts with an honest look at your family’s specific situation. It creates a clear picture of where a professional could step in and make a real difference.
It’s a conversation that absolutely must include the senior themselves. Their voice should be at the heart of every decision, respecting their independence and desires.
Feeling overwhelmed at this stage is completely normal. Most families aren't sure where to begin. It often helps to break down the needs into three main buckets: medical support, personal assistance, and general household help.
A personalized care plan is not a checklist; it's a dynamic roadmap created in collaboration with the patient, their family, and their physician. It respects individual preferences while ensuring clinical needs are met with expertise and compassion from our local, nonprofit team.
Working together this way ensures the final plan of care reflects what’s most important to the person receiving it. It’s what transforms the dream of aging in place into a safe, supported reality.
Pinpointing Medical and Personal Care Needs
The most critical area to get right is the medical support, as this requires the expertise of licensed clinicians. This kind of care is absolutely essential for managing health conditions at home and almost always follows a doctor's direct orders.
Ask yourself if your loved one needs help with any of the following:
- Managing Complex Conditions: This could be anything from monitoring vitals for a senior with heart failure to ensuring insulin is administered correctly for someone with diabetes. A Registered Nurse is equipped to handle this level of oversight.
- Post-Surgery or Hospital Recovery: Coming home from the hospital is a vulnerable time. A skilled nurse can manage wound care, give IV medications, and watch for complications to help avoid a trip back to the hospital.
- Medication Management: Simply keeping track of multiple prescriptions is a huge challenge that a clinical team can easily solve.
Personal assistance, on the other hand, is all about the Activities of Daily Living (ADLs). When someone starts struggling with these tasks, it's often the first clear sign that more daily support is needed. These activities include bathing, dressing, grooming, and moving around safely, all of which a professional Hospice Aide can provide under a nurse's supervision.
Real-World Scenarios and Professional Assessments
Let's look at a situation we see often here in Monterey County. An 80-year-old woman is back home, recovering from surgery for a broken hip. Her doctor has ordered home health care to make sure she heals safely and properly.
In this scenario, she would benefit from a team approach:
- Skilled Nursing: A Registered Nurse from Central Coast VNA & Hospice would visit to check on the surgical incision, manage her pain medication, and teach the family how to assist in her care.
- Physical Therapy: A Physical Therapist would design an exercise program to help her rebuild strength and balance, allowing her to walk safely through her home again.
- Occupational Therapy: An Occupational Therapist would show her how to handle daily tasks like getting dressed or bathing safely while her body is still healing.
This is exactly why a professional assessment is so crucial. At Central Coast VNA & Hospice, our experienced clinicians conduct in-depth, in-home evaluations to get the full picture. We work directly with the patient’s physician in Monterey, San Benito, Santa Cruz, or South Santa Clara County to build a truly personalized care plan.
Our goal isn't just to look at the diagnosis—it's to understand the individual's personal goals for independence. You can learn more about how our home health care services make a difference for so many families right here on the Central Coast.
Figuring Out the Finances and Insurance
Let's be honest—for most families, the biggest question mark hanging over senior care is the cost. It can feel daunting, but breaking down the financial side is the first step toward creating a sustainable plan. The goal is to make aging in place a reality, not a source of stress.
The good news? Keeping a loved one at home is often more affordable than moving them into a facility. It’s not just a preference; it’s a practical financial decision. A 2021 study by Genworth found the median annual cost for home health care was significantly less than residential care.
Let's look at a direct comparison.
Comparing Annual Senior Care Costs
| Care Setting | Estimated Annual Cost |
|---|---|
| Home Health Aide Services | $61,776 |
| Assisted Living Facility | $54,000 |
| Nursing Home (Semi-Private Room) | $94,900 |
| Source: Genworth Cost of Care Survey, 2021 |
As you can see, the numbers speak for themselves. While assisted living costs may seem comparable, home care offers one-on-one attention in a familiar environment—a value you can't put a price on.
This financial reality aligns perfectly with what most seniors actually want.
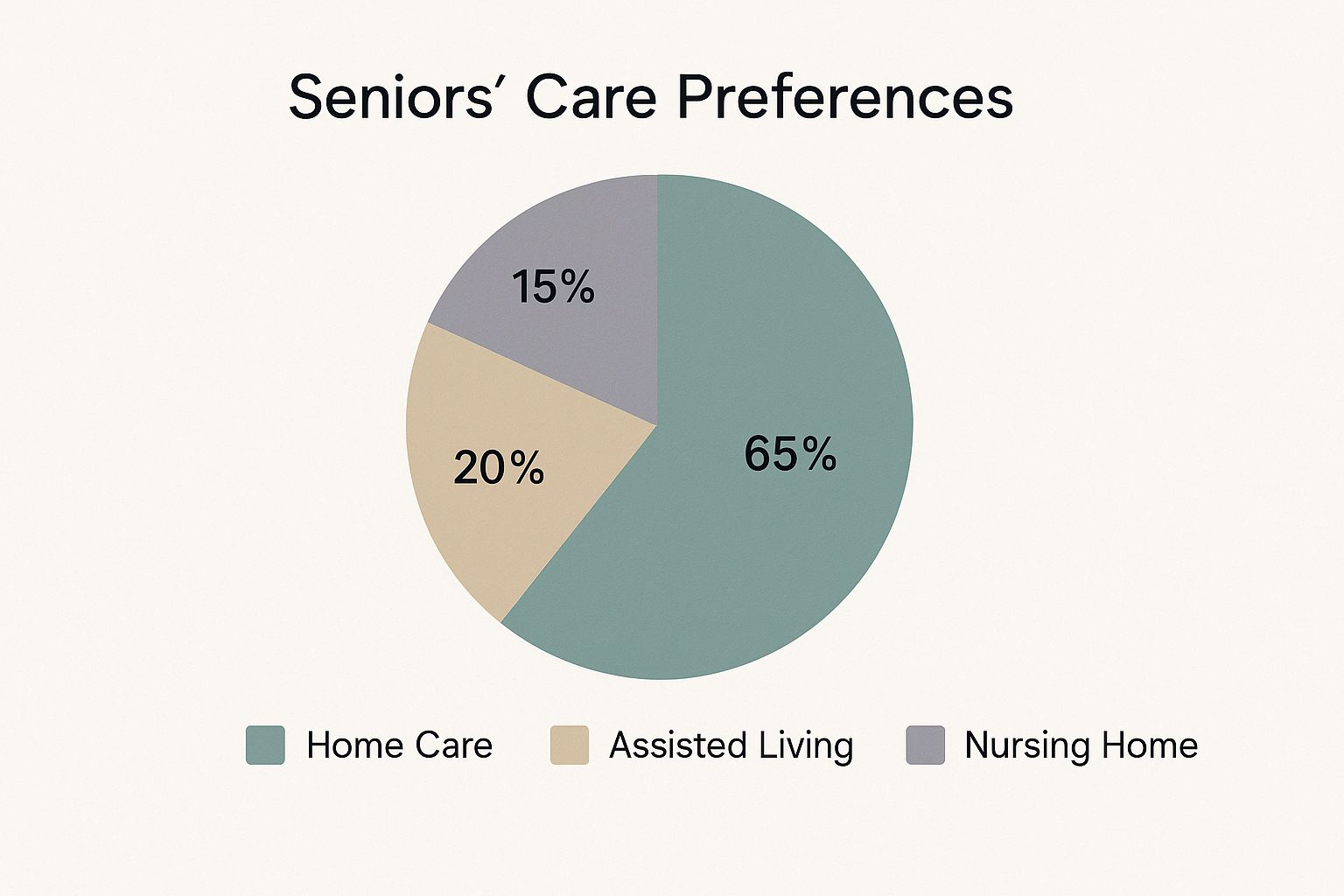
Making this option financially viable is more important than ever.
Understanding Your Coverage Options
So, how do you pay for it? Several resources can help cover the cost of skilled home health care. Getting familiar with them is the key to building a solid financial plan.
- Medicare: This is often the first stop for many families. Medicare can cover intermittent skilled nursing and therapy services when ordered by a doctor and the patient meets specific "homebound" criteria.
- Medi-Cal: As California's Medicaid program, Medi-Cal can cover certain home health services for those who qualify based on income and need.
- Private Health Insurance: Many private plans include benefits for home health care. The amount of coverage depends on your specific policy.
- Long-Term Care Insurance: If you or your loved one planned ahead with a long-term care policy, this is exactly what it was designed for.
How Central Coast VNA & Hospice Can Help
With over 74 years of local, nonprofit service, we at Central Coast VNA & Hospice have helped countless families on the Central Coast work through these financial questions. Our mission has always been to provide compassionate care to everyone who needs it in Monterey, San Benito, Santa Cruz, and South Santa Clara counties.
We’ll help you make sense of your benefits and access the care you need. Our team can verify your insurance coverage and walk you through what services are available under your plan. We’re here to take the guesswork out of it and give you peace of mind.
We firmly believe that financial worries shouldn't stand in the way of receiving excellent medical care at home. That's why we accept Medicare, Medi-Cal, the Central California Alliance for Health, Blue Shield, and a wide range of other private insurance plans. Our intake specialists will work directly with you and your insurance provider to make sure everything is coordinated smoothly.
Planning for Long-Term Financial Health
Thinking ahead is a crucial part of the aging-in-place journey. A little bit of financial planning today ensures that resources will be there when they're needed most. This could mean setting aside savings or looking into safe investments for seniors.
Being proactive gives families the confidence they need to support a loved one's wish to stay at home for the long haul. If you have questions, please reach out. We’re here to help you and your family find the best path forward.
Making the Home a Safe Haven for Aging in Place
For anyone hoping to age gracefully in their own home, making that space safe and functional is non-negotiable. It's about more than just a quick tidy-up. We're talking about thoughtful, practical changes that reduce risks and increase independence.
These aren't massive, disruptive renovations. Think of them as smart tweaks that make everyday life a whole lot easier and safer. When your loved one can move around their home with confidence, you've laid the groundwork for a successful long-term care plan.
Room-by-Room Practical Safety Tips
Often, the simplest changes make the biggest difference. By focusing on the rooms where your loved one spends the most time, you can get some quick wins on the safety front.
- The Bathroom: This is ground zero for falls. Installing grab bars, putting down non-slip mats, and adding a raised toilet seat can be absolute game-changers for safety.
- Living Areas and Hallways: Your main goal here is to create clear, uncluttered paths. Secure any loose rugs with double-sided tape and make sure all cords are tucked safely out of the way.
- The Kitchen: Keep it accessible. Move the dishes, foods, and pots they use most often to lower shelves to eliminate the need for a risky step stool. Good lighting is also a must.
Getting the clutter under control is a huge part of this. For some great ideas, check out these effective decluttering tips for seniors. Little adjustments like these empower seniors by making their home work for them, not against them.
Why a Professional Home Assessment Matters
At Central Coast VNA & Hospice, we know the home environment is just as important as the clinical care we provide. That’s why our Physical and Occupational Therapists are such an essential part of the team. They don't just look at a person's physical health; they look at how that person functions within their own four walls.
A trained therapist brings a clinical eye to the home. They spot the subtle risks that family members, with the best of intentions, might miss—like poor lighting on a stairwell or a favorite armchair that’s become difficult and unsafe to get out of.
During a home visit, our Occupational Therapist might suggest a tool like a long-handled shoehorn to avoid bending. A Physical Therapist will analyze how your loved one moves from the bedroom to the bathroom, ensuring the path is safe. This hands-on, proactive approach is fundamental to preventing falls in the home.
Smart Technology for Extra Peace of Mind
Today’s technology offers some incredible tools that act as a safety net for seniors living alone. These devices are fantastic for adding an extra layer of security, giving both your loved one and your family incredible peace of mind.
This isn't just a niche market; it's a reflection of a major shift in how we approach senior care. Here are a few technologies worth considering:
- Personal Emergency Response Systems (PERS): These are the classic wearable pendants or bracelets with a button that calls for help. They are simple, effective, and life-saving.
- Automated Medication Dispensers: Forgetting medication or taking the wrong dose is a common and dangerous problem. These devices sort and dispense the right pills at the right time.
- Smart Home Devices: Voice-activated lights, thermostats, and even door locks can be a huge help for someone with limited mobility, giving them easy control over their environment.
For families throughout Monterey, San Benito, Santa Cruz, and South Santa Clara counties, our team at Central Coast VNA & Hospice can help you weave these practical strategies into a holistic care plan. By blending professional clinical support with a safe, thoughtfully adapted home, we help seniors live with dignity and independence for years to come.
A Partner for the Entire Journey: CCVNA’s Continuum of Care
When you’re thinking about in-home care, you're not just solving a problem for today. You’re planning for what’s next. A person's health needs rarely stay the same. The real key to aging in place successfully is finding a partner who can adapt right along with you.
This is the very idea our services at Central Coast VNA & Hospice are built on. As the only local nonprofit in our area offering a full continuum of care, we provide consistency and peace of mind from one trusted team. You won’t have to scramble to find a new agency if your loved one’s health changes.
Whether the need is for post-surgery recovery, managing a long-term illness, or providing dignity at the end of life, our team is there for the entire journey. This is our nonprofit mission.
Home Health Care: Bridging the Gap from Hospital to Home
For many families, the journey starts with a need for skilled Home Health care. This isn't long-term assistance; it's short-term, medical support ordered by a doctor to help someone recover safely at home. Think of it as the crucial bridge between intensive medical treatment and getting back on your feet.
Here’s a real-world scenario: A Santa Cruz County resident has a heart attack. After surgery, their doctor orders home health care to ensure their recovery stays on track.
In this situation, our CCVNA team would step in to provide:
- Skilled Nursing: A Registered Nurse visits to check vitals, manage complex cardiac medications, and teach the family about important lifestyle changes.
- Physical Therapy: A Physical Therapist designs a gentle exercise plan to safely rebuild strength and endurance.
- Occupational Therapy: An Occupational Therapist helps them re-learn how to manage daily life—like getting dressed or making a meal—while their body is still healing.
This focused support helps prevent complications and keeps people from ending up back in the hospital. You can see more details about our home health care services and how they work.
Palliative Care: For Comfort and Quality of Life
Sometimes, a person is dealing with a serious, chronic illness like advanced COPD, cancer, or congestive heart failure. They might still be pursuing treatment, but the day-to-day symptoms can become overwhelming. This is exactly where Palliative Care makes a difference.
Palliative Care is an extra layer of support that focuses on providing relief from the symptoms and stress of a serious illness. The goal is simple: to improve quality of life for both the patient and the family, right at home.
A person can receive palliative support at any stage of their illness, even while getting curative treatments. Our specialized team, which includes a Nurse Practitioner and a Medical Social Worker, works directly with the patient’s own doctor to manage symptoms. We also provide crucial emotional and spiritual support.
Hospice Care: Honoring a Final Chapter with Dignity
When an illness progresses and the goal shifts from cure to comfort, Hospice Care begins. It’s not about giving up. It’s a philosophy of care that honors a person’s final chapter by wrapping compassionate support around them and their family.
For over 74 years, our hospice program has been a core part of our nonprofit mission here in Monterey, San Benito, Santa Cruz, and South Santa Clara counties. Our dedicated team—a physician, Registered Nurse, Hospice Aide, Chaplain, and Medical Social Worker—works as one unit. Together, we manage symptoms while providing the emotional and spiritual care that honors a person’s final wishes.
Frequently Asked Questions About Senior Home Care

When you first start looking into senior home care to age in place, it's completely normal to have a long list of questions. This is a big decision for your family, and the responsibility can feel immense. You want to make sure you get it right.
As a local nonprofit with over 74 years of history, our goal at Central Coast VNA & Hospice is to provide clear, reassuring answers. We want to give you the information you need to feel confident and empowered as you move forward.
What is the difference between home health care and personal care?
This is a critical distinction. Home health care is skilled, clinical medical care that must be prescribed by a doctor. It's provided by licensed professionals like Registered Nurses and therapists to help someone recover from an illness or manage a complex health condition.
Personal care, often called "custodial care," is non-medical. This includes assistance with daily tasks like bathing, dressing, and light housekeeping. Central Coast VNA & Hospice specializes in providing expert clinical home health, palliative, and hospice services.
How do we know when it’s the right time for professional home care?
It’s usually not one big event but a series of small, accumulating signs that more support is needed. It might be time to have a conversation about professional care if your loved one is struggling with daily tasks, experiencing more frequent falls, or having trouble managing their medications. It's always better to be proactive; a professional assessment from one of our CCVNA clinicians can give your family a clear picture of the support needed before a crisis hits.
Are CCVNA services available in my area?
Yes. Central Coast VNA & Hospice was founded here and has been a trusted local resource for more than 74 years. Our commitment is to our neighbors. Our dedicated teams proudly serve families and individuals across Monterey County, San Benito County, Santa Cruz County, and South Santa Clara County.
How does the care process begin with CCVNA?
It all starts with a referral. Typically, this comes directly from a physician, a hospital discharge planner, or a specialist who feels you could benefit from skilled medical care at home. Once we get that referral, one of our experienced Registered Nurses will set up an initial in-home visit to conduct a thorough assessment and collaborate with your doctor to build a personalized plan of care.
Can we keep our own doctor if we use CCVNA services?
Of course. The answer is a firm yes. Our job isn't to replace your doctor; it's to become a key part of their care team. Think of our nurses and therapists as an extension of your doctor's practice, bringing their prescribed care plan to life right in your home while keeping them updated on all progress.
Are you ready to learn more about how Central Coast VNA & Hospice can support your family with compassionate, expert care at home? Contact us today to discuss your needs and find out how our continuum of care can help your loved one age in place with dignity and peace of mind. Visit us at https://ccvna.com.
8 Ways to Help Seniors Live At Home Safely in 2025
For many older adults, the ability to remain in their own home is a cornerstone of independence and well-being. This desire often comes with a critical need to ensure the home environment is safe and supportive. For families in Monterey County and surrounding areas, this means finding practical solutions to help seniors live at home safely.
This guide provides actionable strategies and resources designed to foster a secure living situation. We will move beyond generic advice to offer specific, implementable tips that make a tangible difference. This listicle is a practical roadmap for families, seniors, and healthcare providers coordinating support.
Our goal is to empower you with the knowledge needed to create a safe, comfortable, and independent home life. Central Coast VNA & Hospice, with over 74 years of nonprofit service, is committed to supporting our community with compassionate home health, palliative, and hospice care.
1. Conduct a Professional Home Safety Assessment
The first step to help seniors live at home safely is to understand the environment. A professional home safety assessment, conducted by an Occupational Therapist or a Certified Aging-in-Place Specialist (CAPS), provides a comprehensive evaluation. These specialists are trained to identify risks that family members might overlook.
What Does a Professional Assessment Involve?
An assessor performs a room-by-room analysis, focusing on high-risk zones like bathrooms and stairways. They evaluate factors such as lighting, clutter, floor surfaces, and accessibility.
Following the evaluation, they provide a detailed report with prioritized recommendations. These can range from simple fixes, like adding non-slip mats, to more significant renovations like installing a walk-in shower.
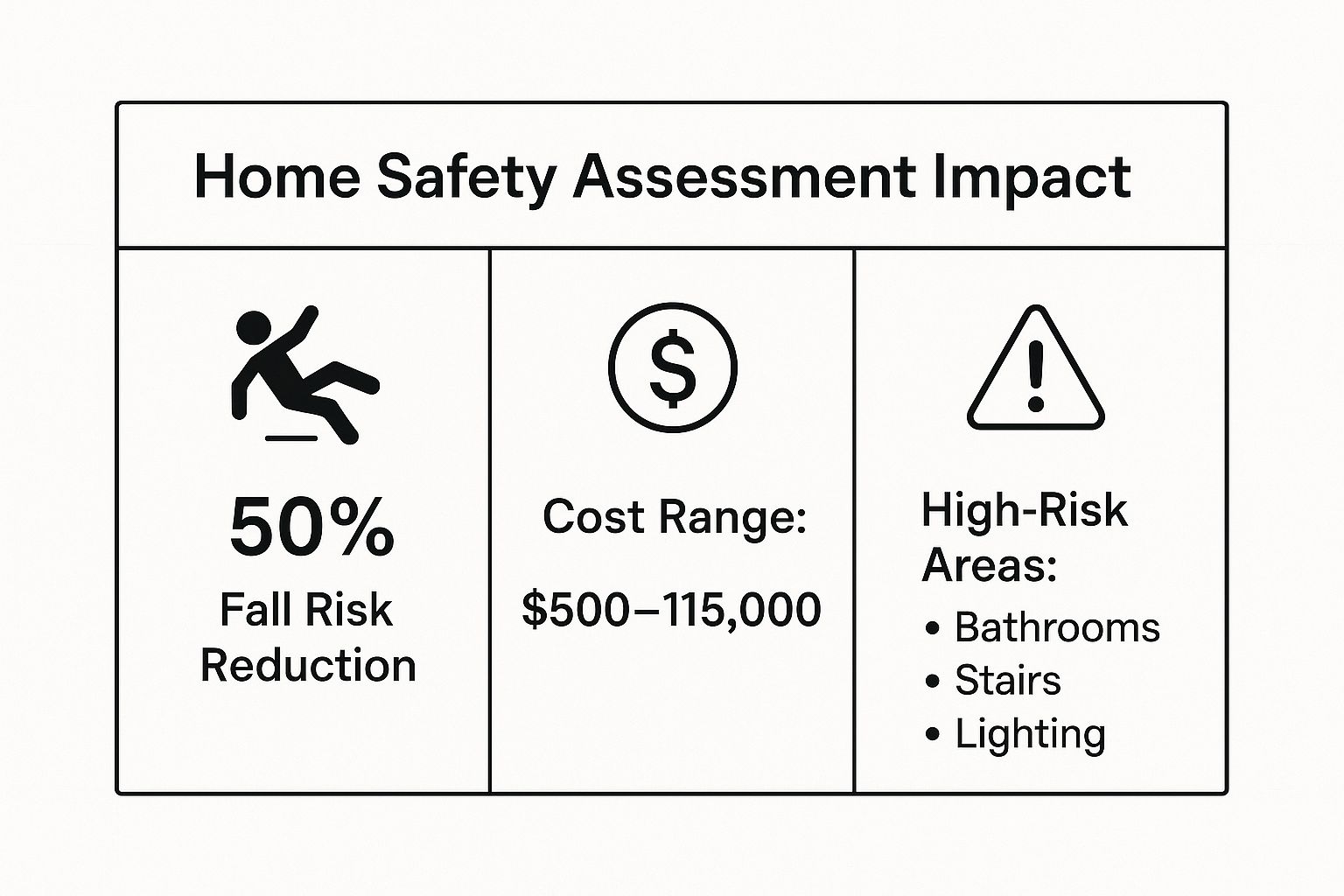
This data highlights how strategic modifications can significantly reduce fall risks. It also shows the wide range of potential costs, from minor adjustments to major renovations.
Why It's Worth the Investment
Investing in a professional assessment is a proactive measure that can prevent accidents and reduce hospital readmissions. It provides peace of mind for the entire family.
By identifying and mitigating risks early, you create a supportive environment. To explore how this fits into a broader strategy, you can learn more about how to help elderly parents age in place.
2. Emergency Response Systems and Medical Alert Devices
Even in the safest homes, accidents can occur. Emergency response systems, or medical alert devices, provide a crucial safety net. They are essential to help seniors live at home safely by offering immediate access to assistance.
Modern systems have evolved far beyond the basic pendant. Many now include advanced features like automatic fall detection, which contacts a monitoring center even if the senior cannot press the button.
GPS-enabled mobile options also provide protection for active seniors when they are away from home. This ensures help is available wherever they go.

What Does a Medical Alert System Involve?
These systems typically consist of a wearable help button and a base station connected to a 24/7 monitoring service. When activated, the device connects the user to a trained operator. The operator can assess the situation, contact family members, and dispatch emergency services if needed.
To maximize effectiveness, it is vital to select the right system and use it correctly. Key considerations include:
- Monthly Testing: Regularly test the system to ensure it functions properly.
- Waterproof Options: Choose a waterproof device that can be worn in the shower or bath, where many falls occur.
- Mobile GPS: For seniors who leave the house independently, a mobile system with GPS is invaluable.
Why It's Worth the Investment
The value of an emergency response system lies in its ability to provide rapid assistance. This can significantly improve outcomes after a fall or medical event.
For family members, these devices offer profound peace of mind. This technology empowers seniors with the confidence to continue living independently, secure in the knowledge that help is just a button-press away.
3. Implement Medication Management Systems
One of the most critical aspects to help seniors live at home safely is managing multiple medications. Polypharmacy, the use of several drugs at once, is common among older adults and increases the risk of errors.
Implementing a robust medication management system is an essential strategy. These systems range from simple weekly pill organizers to advanced automated dispensers with alarms.

What Does Medication Management Involve?
Effective medication management goes beyond simply sorting pills. It’s a comprehensive process that includes regular communication with healthcare providers and proper organization.
For instance, some pharmacy services pre-sort medications into daily packets labeled with the date and time. For those needing more support, smart dispensers can dispense pills at scheduled times and track adherence through an app.
Why It’s a Crucial Safety Measure
An organized system is a powerful tool for preventing medical emergencies. According to a study published in Health Affairs, medication therapy management programs reduced hospitalizations and emergency department visits (Iuga & McGuire, 2014).
Consistent and correct medication intake is fundamental for managing chronic conditions. To ensure effectiveness, it is vital to regularly review all prescriptions with a doctor or pharmacist. You can find more guidance by exploring tips for family caregivers to integrate these practices.
4. Fall Prevention Programs and Exercise
Beyond modifying the home, improving a senior’s physical capabilities is a powerful strategy. Structured physical activity and fall prevention programs are designed to enhance balance, build strength, and improve coordination.
These evidence-based programs empower seniors to move with greater confidence and stability. They are a proactive way to help seniors live at home safely.

What Do These Programs Involve?
Effective programs are multifaceted and address the core physical factors contributing to falls. They often include a combination of different exercise types led by trained instructors.
For example, Tai Chi programs have been shown to reduce falls significantly. A comprehensive approach might also include a professional gait analysis to improve movement, which identifies and helps correct imbalances.
Why It's a Proactive Strategy
Engaging in regular, targeted exercise is one of the most effective ways to prevent falls. It directly addresses the root causes of instability, such as muscle weakness and poor balance.
These programs not only reduce fall-related injuries but also boost overall health and independence. It is always wise to consult a physician before beginning any new exercise regimen. To understand the profound impact of physical activity, you can explore why exercise is important, even in old age.
5. Smart Home Technology Integration
Integrating smart home technology is a modern and effective way to help seniors live at home safely. Connected devices and automation systems can enhance safety and improve daily routines.
These technologies range from simple voice-activated assistants to sophisticated monitoring systems. They can provide peace of mind for both seniors and their families.
What Does Smart Home Integration Involve?
Integrating smart technology involves setting up a network of devices that can be controlled remotely or automatically. This can start with additions like smart lights that turn on with voice commands to prevent falls in the dark.
More advanced systems allow family members to check in and receive alerts. To further enhance passive safety within the home, consider integrating comprehensive smart home security systems.
Why It's a Powerful Tool
This technology empowers seniors with greater control over their environment while offering a non-intrusive safety net. The key is to select technologies that are user-friendly and address a specific need.
Start with a few simple devices to build confidence. Ensure strong Wi-Fi coverage throughout the home for reliability, and create a backup plan for power outages.
6. Transportation and Mobility Solutions
Losing the ability to drive or move around easily can lead to isolation. Implementing robust transportation and mobility solutions is a key strategy to help seniors live at home safely while remaining active.
This involves addressing both getting around inside and outside the home. It ensures seniors can attend appointments, run errands, and socialize.
What Does This Solution Involve?
This strategy focuses on creating a network of reliable transportation options. It also includes utilizing mobility aids like walkers, canes, or scooters to enhance stability.
Modern services like GoGoGrandparent adapt rideshare apps for seniors without smartphones. Traditional volunteer driver programs are also an excellent option.
Why It's a Critical Component of Aging in Place
Access to transportation is directly linked to a senior’s health and quality of life. Without it, they may miss vital medical appointments or become socially withdrawn.
Proactively arranging transportation services and mobility aids prevents these issues. This approach fosters confidence and preserves dignity, making it a cornerstone of any effective plan.
7. Social Connection and Mental Health Support
An often underestimated element to help seniors live at home safely is addressing their emotional and mental well-being. Social isolation can lead to depression, cognitive decline, and decreased motivation to maintain physical health.
Fostering strong social connections and providing mental health support are crucial. This helps a senior’s ability to thrive independently.
What Does Social and Mental Support Involve?
This holistic approach involves creating opportunities for meaningful interaction. Programs can range from in-person activities at local senior centers to virtual communities.
For instance, Meals on Wheels provides not only nutrition but also a vital daily social check-in. These initiatives combat isolation by providing purpose, routine, and a supportive network.
Why It's a Critical Component of Home Safety
Investing in a senior's social and mental health is as important as installing grab bars. A socially engaged and mentally healthy individual is more likely to stay physically active and manage their health needs.
To find local programs that can help, you can explore comprehensive Monterey senior care services. Building a strong support system is a powerful strategy to ensure your loved one can age in place not just safely, but happily.
8. Healthcare Coordination and Telehealth Services
Managing healthcare needs from home is critical to help seniors live at home safely. This is especially true for those with chronic conditions or mobility challenges.
An integrated approach combining coordinated care teams with telehealth technology ensures consistent medical attention. This proactive health management can prevent complications.
What Does Coordinated Telehealth Involve?
This approach uses technology to connect patients with their healthcare providers remotely. It involves virtual visits, remote monitoring of vital signs, and easy communication with a care team.
For instance, a Registered Nurse can use a video call to assess a wound. A doctor can adjust medications based on remotely transmitted blood pressure readings.
Why It's Worth the Investment
Adopting telehealth and coordinated care is a forward-thinking strategy. It empowers seniors and provides immense relief for families.
This model is particularly beneficial for managing chronic illnesses. For families managing complex needs, you can learn more about comprehensive home health care services. This modern approach to healthcare helps ensure a safer, more independent life at home.
Building a Circle of Support for Safe Aging at Home
Creating a safe home environment for seniors is about weaving together a comprehensive tapestry of support. It's an ongoing, collaborative process that requires proactive planning.
By embracing concepts like structured medication management, fall prevention programs, and telehealth, families can address the challenges of aging. These measures reduce risks and provide invaluable peace of mind.
A truly secure environment also encompasses emotional well-being and consistent healthcare oversight. The integration of smart home technology, transportation solutions, and social support networks are equally vital. These elements combat isolation and empower seniors to remain active and connected.
To build a resilient safety net, consider these actionable next steps:
- Schedule a Family Meeting: Gather key family members and the senior to discuss these tips. Create a collaborative plan that respects their wishes.
- Prioritize a Home Assessment: Walk through the home to identify potential hazards. Decide on practical modifications, like installing grab bars or improving lighting.
- Research Local Resources: Every community offers different programs. Understanding the availability of local caregiving support options can provide additional layers of assistance.
- Consult with Professionals: Connect with healthcare providers, Occupational Therapists, or organizations like Central Coast VNA & Hospice. Their expertise can help tailor a plan for specific health needs.
Ultimately, the goal is to create a dynamic and responsive "circle of support" that adapts as needs evolve. By thoughtfully combining these strategies, families can transform a home into a haven. This enables their loved ones to not just live, but thrive, safely and independently for years to come.
If your loved one requires skilled medical care to manage an illness or recover from an injury at home, Central Coast VNA & Hospice can be a vital part of their safety net. Our expert home health, palliative care, and hospice teams have proudly served Monterey County, San Benito County, Santa Cruz County, and South Santa Clara County for over 74 years, bringing compassionate, professional care directly to you. Contact us today to learn how our Continuum of Care can help your family navigate the journey of aging with confidence and support.
Frequently Asked Questions (FAQs)
1. What is the most important first step to help a senior live at home safely?
The most important first step is a professional home safety assessment. An Occupational Therapist can identify specific hazards in the home and recommend targeted modifications to prevent falls and other accidents.
2. How can Central Coast VNA & Hospice help my loved one stay at home?
CCVNA provides a Continuum of Care, including home health, palliative care, and hospice services. Our skilled teams of Registered Nurses, Therapists, and Aides deliver professional medical care and support directly in the patient's home, helping manage symptoms and improve quality of life.
3. Are medical alert systems expensive?
The cost of medical alert systems varies. While some advanced systems have an initial device cost, many operate on an affordable monthly subscription model, often ranging from $20 to $70.
4. What areas does Central Coast VNA & Hospice serve?
As a local, nonprofit organization, CCVNA has served our community for over 74 years. Our service area includes Monterey County, San Benito County, Santa Cruz County, and South Santa Clara County.
5. How can I help my parent manage their medications correctly?
Implementing a medication management system is key. This can be a simple pill organizer or a smart dispenser with alarms. Always review all medications with their doctor or pharmacist regularly to avoid adverse interactions.
What Is Hospice Care and How Does It Work?
When the goal of treatment shifts from finding a cure, care does not end. Instead, it transforms into a compassionate approach called hospice. The focus moves to maximizing comfort, preserving dignity, and enhancing the quality of life.
Making the decision to start hospice is an empowering choice. It allows individuals to live their final months on their own terms, often in the comfort of home.
Understanding the Heart of Hospice Care

It’s a common misconception that hospice means "giving up." The truth is that choosing hospice is about gaining control over your final chapter. This philosophy of care is designed for anyone with a life-limiting illness, helping them live as fully and comfortably as possible.
According to the National Hospice and Palliative Care Organization (NHPCO), over 1.72 million Medicare beneficiaries received hospice services in 2020 (NHPCO, 2021). This reflects a growing desire for comfort-focused, patient-centered care.
At Central Coast VNA & Hospice, our approach is built on holistic, team-based support. As a nonprofit cornerstone for over 74 years, we serve families across Monterey County, San Benito County, Santa Cruz County, and South Santa Clara County.
Hospice care isn't about the last days of life. It is about the life that remains. It ensures that every moment is lived with comfort, respect, and peace.
This core belief drives everything we do as a mission-driven organization. To better understand this philosophy, here is a summary of how the focus of care shifts.
Hospice Care at a Glance
| Aspect of Care | Focus in Hospice |
|---|---|
| Treatment Goal | Managing symptoms and enhancing comfort, not curing the illness. |
| Location of Care | Primarily in the patient's home, but can be anywhere they reside. |
| Patient's Role | Empowering the patient to make decisions about their daily life and care. |
| Family Involvement | Providing support, education, and bereavement services for the entire family. |
| Emotional & Spiritual | Addressing emotional and spiritual needs alongside physical symptoms. |
As you can see, hospice is about treating the whole person, not just the disease. It's about surrounding the patient and their loved ones with a complete circle of support.
Our dedicated interdisciplinary team works together to address the complete needs of both the patient and their family. This team includes:
- A Registered Nurse to skillfully manage pain and other complex symptoms.
- A Hospice Aide to assist with personal care, making daily life easier and more comfortable.
- A Medical Social Worker to provide vital emotional support and help coordinate community resources.
- A Chaplain to offer spiritual guidance that is always tailored to an individual’s personal beliefs and wishes.
This comprehensive model ensures that physical, emotional, and spiritual needs are met with expertise and compassion. You can learn more about how we provide hospice care with comfort and dignity right here on the Central Coast.
Who Qualifies for Hospice Care?
Navigating healthcare choices during a serious illness can feel overwhelming. Understanding the criteria for hospice care makes the path forward much clearer.
Hospice is an option when a doctor believes a person has a prognosis of six months or less if the illness runs its natural course. It’s important to see this timeframe as a guideline, not a deadline. Many people receive compassionate hospice support for longer, as long as they still meet the criteria.
Common Qualifying Conditions
While hospice is a choice for anyone with a terminal diagnosis, some conditions are more common. This list can help families across Monterey County, San Benito County, Santa Cruz County, and South Santa Clara County recognize when to explore options.
Common diagnoses often include:
- End-stage cancer
- Advanced heart disease (like Congestive Heart Failure)
- Chronic Obstructive Pulmonary Disease (COPD)
- End-stage Alzheimer's disease or other forms of dementia
- Advanced kidney or liver disease
- Amyotrophic Lateral Sclerosis (ALS)
A physician’s certification is needed to start hospice care, but you do not have to wait for them to bring it up. Families can and should initiate this important conversation. At Central Coast VNA & Hospice, our expert team can help facilitate these discussions with you and your doctor.
The decision to explore hospice isn’t about giving up. It's about choosing to live the rest of your life with the greatest comfort and dignity possible, surrounded by a team dedicated to your well-being.
Knowing when to start is a critical step. For a detailed guide, you can learn more about our hospice care eligibility guidelines and how we help families through the process.
What Services Are Included in Hospice?

When a family chooses hospice, they receive a complete circle of support. This support is designed to address every aspect of a person's well-being—physical, emotional, and spiritual. At Central Coast VNA & Hospice, our team builds a personalized care plan that supports the patient and their loved ones.
The goal is to relieve burdens so families can focus on spending meaningful time together. It is a model of care we have refined over 74 years of serving our local communities.
A Team-Based Approach to Comfort
Hospice care is delivered by a dedicated team of professionals. Each member brings unique expertise, ensuring every need is met with compassion and skill.
This team approach is the heart of effective hospice support. The global hospice market reports a growing demand for these services, driven by a greater focus on quality of life.
Our Central Coast VNA & Hospice team includes:
- Registered Nurse: An RN leads the clinical care, expertly managing pain and symptoms to keep the patient comfortable. They are the primary contact for medical questions.
- Hospice Aide: A certified Hospice Aide provides gentle, hands-on help with personal care, like bathing and dressing. This support helps maintain dignity and gives family a much-needed break.
Comprehensive Support for Body, Mind, and Spirit
Beyond physical symptoms, hospice addresses the profound emotional and spiritual challenges of a serious illness. This holistic support makes hospice incredibly valuable for patients and families.
Hospice isn't just about managing a disease; it's about caring for the entire person and their family. It provides a safety net of support that honors the patient’s wishes and life story.
This is where the rest of the interdisciplinary team comes in:
- Medical Social Worker: Our social workers offer emotional support and counseling. They also provide practical guidance on advance directives and connecting with community resources.
- Chaplain: A chaplain provides non-denominational spiritual support tailored to the patient’s beliefs. They offer a calming presence, a listening ear, and a source of peace.
Additionally, hospice care through CCVNA covers the cost of medications, medical supplies, and equipment related to the terminal illness. This includes items like hospital beds and oxygen, removing a significant financial and logistical weight from families.
The True Benefits for Patients and Families

The real value of hospice care is the profound sense of peace it brings. For patients, it is about controlling pain and symptoms and living their final days in a familiar, loving place. It gives them the power to shape their own lives, on their own terms.
The benefits for families are just as life-changing. Knowing an expert team is on call 24/7 offers incredible emotional relief and practical help. Hospice allows family members to step back from caregiving tasks and simply be a spouse, a child, or a friend again.
Empowering Families Through Comprehensive Support
This type of support system is becoming more critical than ever. It's helpful for families to understand what families need to know about end-of-life services to feel truly prepared. This philosophy of relieving stress is also at the heart of the benefits of palliative care, which is another part of our continuum of care.
Hospice care gives families the gift of time—time to talk, to laugh, and to create lasting memories without the constant stress of managing an illness alone.
At Central Coast VNA & Hospice, our support does not end when a loved one passes away. Our compassionate, family-first approach includes bereavement support for up to 13 months. This long-term commitment is a cornerstone of our nonprofit mission to serve the Central Coast community.
How to Start the Conversation About Hospice
Thinking about hospice can be difficult, but starting the conversation is a straightforward first step. It is about being proactive to ensure a loved one's wishes are heard and honored.
Anyone can make the first call—the patient, a family member, or a trusted physician. At Central Coast VNA & Hospice, we have designed our process to be supportive and clear from the start.
It all begins with a simple phone call to discuss your family's situation and answer your questions. The journey from that first call to ongoing support at home is a collaborative one.
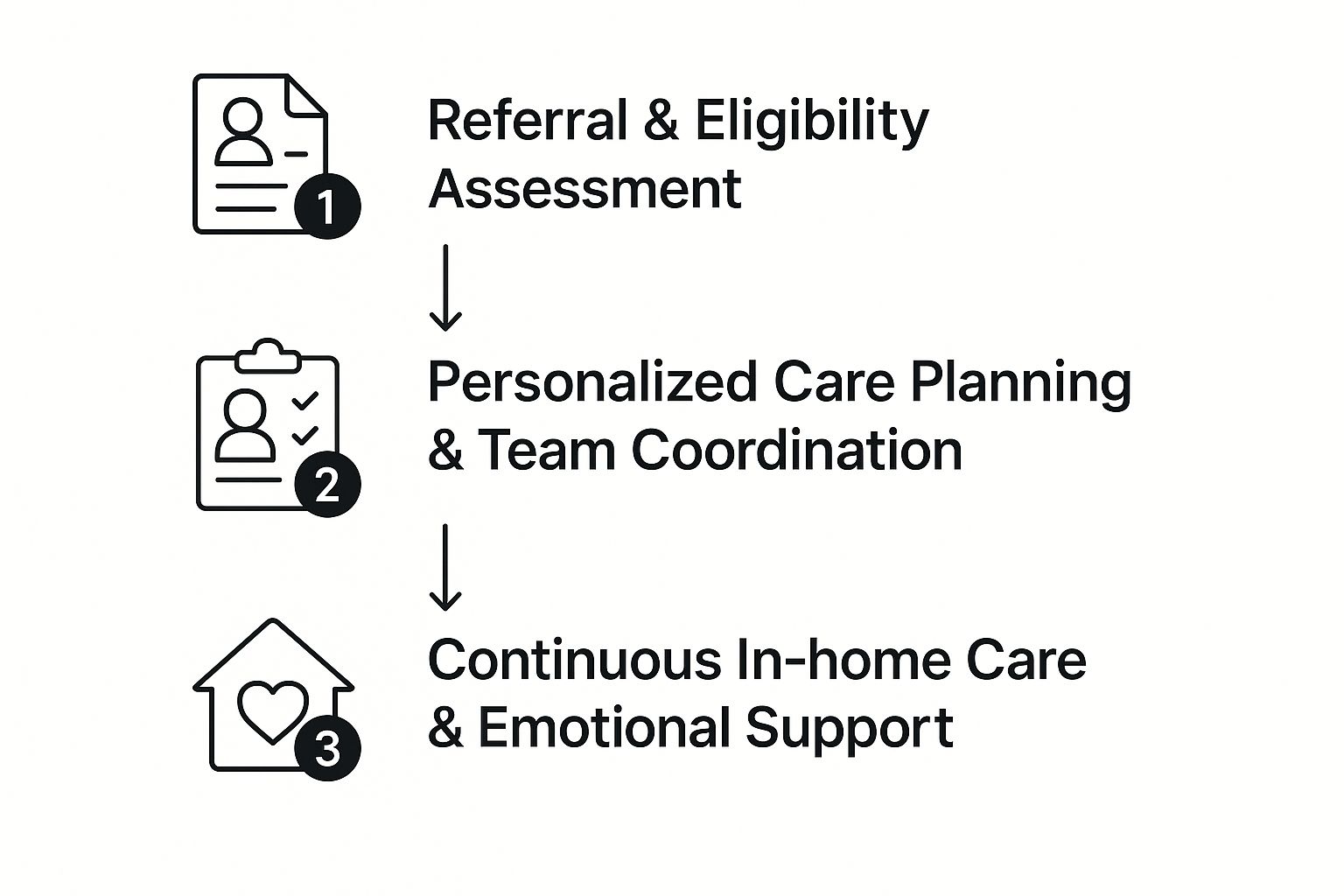
This visual shows how the process is a partnership. We are here to work with you, keeping your family’s needs and goals at the center of everything we do.
Your First Steps With CCVNA
Getting started with hospice support in Monterey, San Benito, Santa Cruz, or South Santa Clara County involves just a few easy steps:
- Contact Us for a Consultation: Call our team for a no-obligation conversation. We are here to listen and bring clarity to what hospice care can offer.
- Coordinate With Your Physician: With your permission, our team will connect with your doctor to confirm eligibility.
- Create a Personalized Care Plan: We will schedule a visit to meet you, listen to your goals, and create a plan of care that respects your wishes.
This initial conversation is informational and designed to empower you with knowledge. Our guide on how to prepare your loved one for hospice care offers helpful tips for these discussions.
Frequently Asked Questions About Hospice Care
Deciding on hospice care is a significant step that naturally comes with many questions. For families in Monterey County, San Benito County, Santa Cruz County, and South Santa Clara County, clear answers are the first step toward peace of mind.
Here are some of the most common questions we hear, along with the honest answers you and your family deserve.
1. Does choosing hospice mean giving up hope?
No, choosing hospice is not about giving up hope; it is about redefining hope. Hope shifts to what matters most in the present moment. This can mean hope for a day without pain, hope for meaningful conversations, or hope for peace and comfort.
2. Is hospice only for the last few days of life?
No. While some families wait, hospice provides support for months, not just days. Patients are eligible when a doctor certifies they have a life expectancy of six months or less. Starting hospice care sooner allows patients and families to receive the full benefit of our support services.
3. Can a patient leave hospice care?
Yes, a patient can choose to stop hospice care at any time and for any reason. If their condition improves or they wish to pursue curative treatment, they can revoke their hospice benefit. If circumstances change later, they can leave and return to hospice care.
4. Where is hospice care provided?
Hospice is a philosophy of care that comes to you, wherever you call home. This includes a private residence, an assisted living community, or a skilled nursing facility. Our team at Central Coast VNA & Hospice brings expert care to patients in their familiar, comfortable surroundings.
5. Who pays for hospice care?
For most people, hospice care is a fully covered benefit under Medicare Part A with no out-of-pocket costs. This benefit typically covers the care team, medications, and medical equipment related to the terminal illness. This comprehensive coverage also extends to Medi-Cal and most private insurance plans.
6. What makes Central Coast VNA & Hospice different?
As a local, mission-driven nonprofit with over 74 years of service, our focus is entirely on patient care, not profits. We serve communities across the Central Coast, offering a full continuum of care from home health to palliative and hospice services. Our deep local roots and compassionate model ensure that you and your family receive the highest quality of support.
Are you or a loved one facing a serious illness? The team at Central Coast VNA & Hospice is here to answer your questions and provide compassionate guidance. Contact us today to learn more about how our continuum of home health, palliative, and hospice care can support your family.
Hospice Care for Veterans: End-of-Life Support with Honor
Those who have bravely served our country deserve a special kind of compassionate care at the end of life. Hospice care for veterans is a dedicated benefit, designed to honor their service. It meets their unique physical, emotional, and spiritual needs with dignity and respect.
This support ensures comfort and quality of life when it matters most. As a nonprofit provider with over 74 years of local experience, Central Coast VNA & Hospice is committed to this mission.
Honoring Service With Compassionate End-of-Life Care

The sacrifices made by our nation's veterans are profound. Their experiences shape their lives in ways that many of us can't fully grasp.
When a veteran faces a serious illness, those same experiences can deeply influence their end-of-life journey. This can create needs that a standard medical program might overlook. This is exactly why specialized hospice care is so much more than a service—it’s a heartfelt thank you.
At Central Coast VNA & Hospice, we believe in honoring that service with care that is deeply respectful and culturally aware. As a nonprofit, mission-driven organization with over 74 years of experience serving the Central Coast, we are proud to partner with the Department of Veterans Affairs (VA) to deliver this essential support. Our roots in Monterey County, San Benito County, Santa Cruz County, and South Santa Clara County run deep, and our commitment to the community is unwavering.
The Need for Veteran-Centric Support
The need for this kind of specialized care is significant. According to the National Hospice and Palliative Care Organization (NHPCO), about 642,000 U.S. military veterans pass away each year, which is roughly one out of every four deaths in the entire country (NHPCO, n.d.).
Despite this, research has shown that hospice use has often lagged among veterans compared to non-veterans. This data highlights just how crucial it is to have a care model built on understanding and recognition.
It’s about more than just managing symptoms; it’s about acknowledging a life of service. Beyond the medical care itself, a huge part of compassionate end-of-life support involves helping families navigate the emotional challenges of loss. For those looking for resources for grief support, understanding how to comfort loved ones can make all the difference.
A Trusted Local Partner in Your Journey
Navigating healthcare benefits can feel overwhelming, especially during an already difficult time. As a trusted, VA-approved community provider, Central Coast VNA & Hospice is here to guide families through every single step.
We have years of experience coordinating with the VA. Our team knows how to make the process as seamless and stress-free as possible.
Veteran Hospice Care At a Glance
| Aspect of Care | Description for Veterans |
|---|---|
| VA Hospice Benefit | A fully covered benefit for eligible veterans, ensuring no out-of-pocket costs for care related to their terminal illness. |
| Common Care Settings | Most often provided in the comfort of the veteran's home. It's also available in VA facilities, nursing homes, and community hospice centers. |
| Primary Goal | To manage pain and symptoms, provide emotional and spiritual support, and honor the veteran's service with dignity and respect. |
This table just scratches the surface, but it gives a good sense of the support available. Our interdisciplinary teams—which include a Registered Nurse, Chaplain, and Medical Social Worker—are all trained to understand the specific challenges veterans may face.
This guide will walk you through the VA benefits, who is eligible, and what our veteran-centric hospice care services look like. We are completely dedicated to making sure every veteran in our care receives the comfort, honor, and respect they have so rightfully earned.
Understanding Your VA Hospice Benefit and Eligibility

When a loved one is facing a life-limiting illness, the last thing your family should have to do is navigate a confusing system of benefits. The Department of Veterans Affairs (VA) provides a comprehensive hospice benefit. It's designed to honor their service with the comfort and dignity they deserve.
Think of the VA Hospice Benefit as a promise kept. It is a commitment to provide compassionate care that focuses on quality of life when curative treatments are no longer the goal. This is an earned entitlement that ensures veterans can receive expert end-of-life care without creating a financial burden for their families.
Who Qualifies for the VA Hospice Benefit?
Eligibility is one of the first questions families ask, and thankfully, the criteria are straightforward. A veteran just needs to meet a few key requirements to access this support.
A veteran is generally eligible for hospice care for veterans if they meet these conditions:
- Enrolled in VA Healthcare: The veteran must be enrolled in the VA healthcare system.
- Clinical Diagnosis: A physician needs to certify that the veteran has a terminal illness with a life expectancy of six months or less, if the illness follows its natural course.
- Choice of Comfort Care: The veteran decides to receive comfort-focused care (hospice) instead of curative treatments for their illness.
This shift from curative to comfort care is a deeply personal one. It means the focus moves entirely to managing pain, controlling symptoms, and providing emotional and spiritual support to both the veteran and their family. For a deeper look at general requirements, you can check out our guide on hospice care eligibility.
The VA Hospice Benefit is more than a policy; it's a pledge to provide peace, dignity, and respect. It allows families to focus on what truly matters: spending meaningful time together.
Demystifying the Financial Side of Care
One of the most reassuring parts of the VA Hospice Benefit is the financial peace of mind it offers. For a qualifying veteran, the benefit typically covers 100% of the costs related to hospice care for their terminal diagnosis.
This removes a huge source of stress during an already difficult time.
This comprehensive coverage includes:
- Expert Medical Care: Services from the entire hospice team, including physicians, a Registered Nurse, and a Hospice Aide.
- Medications: All medications for managing pain and other symptoms of the terminal illness.
- Medical Equipment: Items like a hospital bed, oxygen, or a wheelchair to ensure comfort and safety at home.
- Support Services: Emotional counseling, spiritual guidance from a Chaplain, and services from a Medical Social Worker for both the veteran and their family.
This all-in-one support system makes sure every aspect of the veteran's comfort is taken care of, with no out-of-pocket costs.
Partnering with Community Providers for Local Care
The VA knows that the best place for care is often close to home, surrounded by loved ones. To make this happen, the VA frequently partners with trusted, community-based hospice providers.
This allows veterans to access high-quality care without having to travel to a VA facility. Central Coast VNA & Hospice is proud to be a VA-approved provider serving Monterey County, San Benito County, Santa Cruz County, and South Santa Clara County.
With over 74 years of nonprofit service to our community, we work hand-in-hand with the VA to coordinate seamless, compassionate hospice care for veterans right where they feel most comfortable. Our team handles all the coordination, so you can focus on your loved one.
What Specialized Hospice Services Do Veterans Receive?

While the VA Hospice Benefit provides the official framework for care, the real heart of the matter lies in honoring a veteran’s unique life journey. Hospice care for veterans isn't just about standard medical support. It’s a deeply personal approach that addresses the physical, emotional, and spiritual needs shaped by military service.
This is anything but a one-size-fits-all model. At Central Coast VNA & Hospice, we build our care on this exact principle.
We know that experiences from military service can deeply influence how a veteran copes with illness, pain, and the end of life. That’s why our care plans are crafted to create a safe space for healing, reflection, and ultimately, peace.
An Interdisciplinary Team Approach
The foundation of truly effective hospice care is a team of professionals working together. This interdisciplinary team collaborates to support both the veteran and their family, creating a personalized care plan that adapts as needs change.
Our team is made up of:
- Registered Nurse (RN): A dedicated RN case manager acts as the main point of contact. They specialize in pain and symptom management, working with physicians to keep the veteran comfortable.
- Hospice Aide: These compassionate professionals help with personal tasks like bathing, dressing, and other daily activities. Their work is essential for maintaining dignity and comfort at home.
- Medical Social Worker: Our Medical Social Workers understand the complex issues veterans and their families may face. They offer counseling, find community resources, and assist with navigating logistical hurdles.
- Chaplain: Spiritual support is available to everyone, regardless of their beliefs. Our Chaplains provide a comforting presence, helping veterans and families find meaning and peace.
Culturally Competent Emotional and Spiritual Support
Military service creates its own powerful culture. Veterans often have a shared language, a unique sense of humor, and a bond forged through experiences most civilians can't fully grasp.
To be effective, hospice care for veterans must be delivered by people who understand this culture. Our team members receive ongoing training on military culture, post-traumatic stress, and moral injury.
This allows them to build trust and offer emotional support that truly connects. They work to create an environment where veterans feel safe to share their stories without judgment.
The goal isn't just to manage physical symptoms, but to help heal the spirit. By acknowledging a veteran’s service and understanding its impact, we can provide a much deeper level of comfort.
A Seamless Continuum of Care
At Central Coast VNA & Hospice, we are the only organization on the Central Coast that offers a full continuum of in-home care. This means our support can start long before hospice, creating a smooth transition as needs evolve.
This journey often moves through three stages:
- Home Health: Skilled nursing and therapy at home to help a veteran recover from an illness or manage a chronic condition.
- Palliative Care: Specialized support focused on managing symptoms and improving quality of life, even while pursuing curative treatments.
- Hospice Care: A shift to comfort-focused care when an illness is terminal, providing holistic support for the veteran and their loved ones.
Knowing the difference between these types of care is crucial. Our guide on palliative versus hospice care can bring more clarity. This integrated approach ensures that veterans in Monterey, San Benito, Santa Cruz, and South Santa Clara counties get consistent care from a team they trust.
The Steps to Accessing Veteran Hospice Care
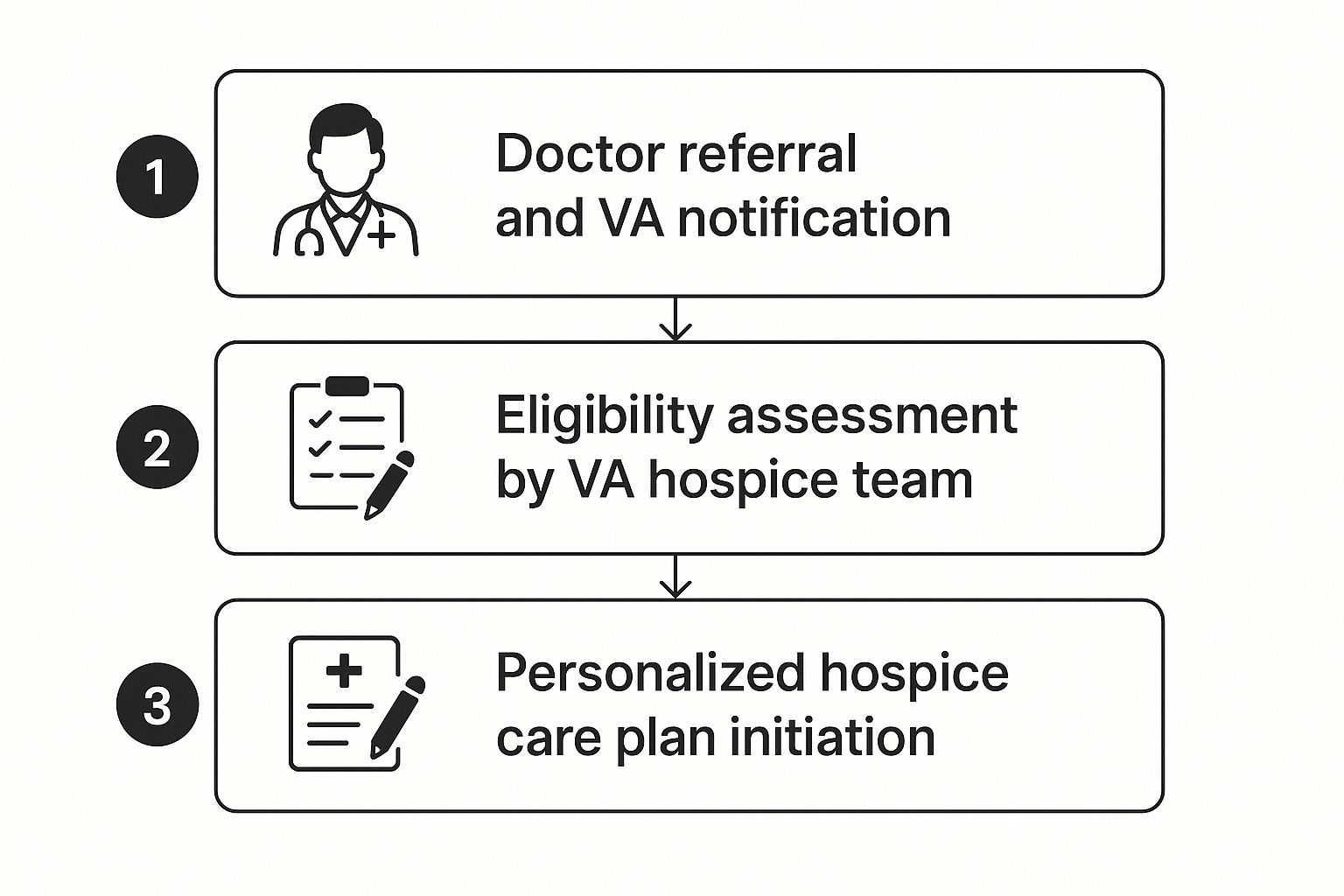
Navigating the steps to secure hospice care for veterans can feel overwhelming, but you can walk this path with confidence. Understanding the process is key to ensuring your loved one receives the compassionate care they’ve earned.
As a nonprofit organization with over 74 years of service on the Central Coast, we at Central Coast VNA & Hospice are committed to making this process easier. We’ve worked alongside countless veterans and their families in Monterey County, San Benito County, Santa Cruz County, and South Santa Clara County.
The First Step: A Medical Referral
It all starts with a conversation between the veteran, their family, and their physician. To qualify for the VA Hospice Benefit, a physician must certify that the veteran has a terminal illness with a life expectancy of about six months or less.
Once the physician agrees that hospice is the right path, they will issue a referral. This is a formal acknowledgment that the focus of care is shifting from cure to comfort.
The Practical Steps to Enrollment
With the physician's referral in hand, the next phase is coordinating with the VA and choosing a hospice provider. A VA social worker or case manager is an invaluable guide in this process.
Here’s a simple roadmap to get started:
- Get the Medical Referral: Talk to the veteran’s primary care physician or specialist to get a formal referral for hospice care.
- Contact the VA: With the referral, reach out to your local VA Medical Center or connect with a VA social worker to start the authorization process.
- Choose a VA-Approved Provider: The VA works with community organizations to provide care close to home. You have the right to choose a VA-approved provider like Central Coast VNA & Hospice.
- Complete the Hospice Admission: After you’ve selected a provider, a Registered Nurse will schedule an admission visit to create a personalized care plan.
Coordinating with Your Hospice Team
The admission process is designed to be reassuring and thorough. Your hospice team will walk you through all available services—from pain management by a Registered Nurse to support from a Medical Social Worker and Chaplain.
If you want to dive deeper into how this kind of care helps, you can learn more about the benefits of palliative care in our detailed guide. Choosing hospice is not about giving up; it is about choosing to live the remainder of one’s life with comfort and dignity.
At Central Coast VNA & Hospice, our admissions team’s primary goal is to listen. We build a care plan that honors the veteran’s wishes. From there, we handle communication with the VA and coordinate all necessary care.
Why Veteran-Centric Care and Recognition Matter
Good medical care is the minimum standard for any hospice. But for someone who has served in the military, real comfort goes beyond managing symptoms. It comes from a place of understanding and a deep respect for their unique life experiences.
This is the heart of veteran-centric hospice care. It's an approach that honors the person, not just the patient. Military service creates its own culture, and a one-size-fits-all approach just doesn't work.
A Commitment to Honoring Service
To formalize this commitment, many healthcare organizations partner with programs designed to elevate care for former service members. One of the most respected is the We Honor Veterans program, a joint effort by the National Hospice and Palliative Care Organization and the Department of Veterans Affairs.
Central Coast VNA & Hospice is a proud participant. This means our staff—from Registered Nurses to Chaplains—receives ongoing training to better grasp the specific needs of veterans.
At its core, veteran-centric care is about grateful acknowledgment. It is our promise to see, hear, and honor the sacrifices a veteran has made for our country.
The Power of Recognition and Validation
Sometimes, the simplest acts of recognition can bring a profound sense of comfort and healing. For a veteran, being seen and thanked for their service can be just as important as pain management.
This recognition often comes to life through special ceremonies and personal tributes. Here are a few examples of how we make this happen:
- Pinning Ceremonies: We hold a formal ceremony where a veteran is presented with a pin and certificate, thanking them for their service in a simple, dignified way.
- Veteran-to-Veteran Volunteers: Whenever possible, we pair a veteran patient with a volunteer who has also served, creating an instant connection.
- Storytelling and Life Review: We encourage veterans to share their stories, helping them process their experiences while creating a lasting legacy for their families.
This dedicated approach is making a real difference. A 2022 survey found that nearly two-thirds of veterans in VA Home-Based Primary Care programs received hospice in their final 90 days. Family caregivers rated the overall quality of this care very highly, with 53% giving an “excellent” rating. You can read more about these positive family perceptions of veteran care.
At Central Coast VNA & Hospice, our mission is to provide care that is not just medically excellent but also deeply respectful. By weaving these practices into our hospice services on the Central Coast, we ensure that every veteran we serve receives the honor they have so rightfully earned.
Your Trusted Partner on the Central Coast
Choosing a hospice provider is a deeply personal decision that hinges on trust. For families seeking hospice care for veterans, that trust must be earned through real expertise, community ties, and a desire to honor a life of service.
At Central Coast VNA & Hospice, these values have been the bedrock of our work for over 74 years. We're a local, mission-driven nonprofit.
That means we aren't accountable to shareholders—we're accountable to you, our neighbors in Monterey County, San Benito County, Santa Cruz County, and South Santa Clara County. Every choice we make is guided by one question: what is best for our patients and their families?
Why Our Local Roots Matter
Unlike national, for-profit chains, our focus has always been the health and well-being of the Central Coast community. We were founded here, we live here, and our team is woven into the fabric of the towns we serve.
Being a VA-approved provider is more than just a credential. It signifies years of hands-on experience navigating the system. We handle the coordination so you can focus on what truly matters.
We believe that providing hospice care for veterans is a sacred responsibility. It’s our chance to give back to those who have given so much, ensuring their final journey is one of comfort, dignity, and peace.
Begin the Conversation Today
Thinking about end-of-life care can feel overwhelming, but you don’t have to walk this path alone. Our compassionate team is here to answer your questions, offer guidance, and support you every step of the way.
We can help you understand all the options and coordinate a care plan that honors your loved one’s wishes. If you believe your family could benefit from our veteran-focused hospice services, please reach out.
Contact us today to learn how our dedicated team at Central Coast VNA & Hospice can support you.
Frequently Asked Questions About Hospice Care for Veterans
1. Can a veteran receive hospice care at home?
Yes, absolutely. The VA Hospice Benefit is designed to provide care wherever a veteran calls home. This can be their private residence, an assisted living community, or a skilled nursing facility. At Central Coast VNA & Hospice, our teams bring expert medical care and support directly to veterans across Monterey, San Benito, Santa Cruz, and South Santa Clara counties.
2. Does using the VA Hospice Benefit affect other VA benefits?
No, it does not. Accepting the VA Hospice Benefit will not impact a veteran's other earned benefits, such as their disability compensation or pension. Hospice is an additional layer of support designed to provide comfort and improve quality of life.
3. What if a veteran is not currently enrolled in VA healthcare?
Even if a veteran isn't enrolled in the VA healthcare system, they may still be eligible for the hospice benefit. The first step is to apply for VA healthcare enrollment as soon as possible. A VA social worker or a team member here at Central Coast VNA & Hospice can walk you through the process and help determine eligibility.
4. What kind of support is available for the veteran's family?
Hospice is designed to support the entire family. Our support for families includes bereavement counseling for up to 13 months after a loved one has passed, spiritual support from our Chaplains, and education to help you feel more prepared and less anxious. Our goal is to be a steady presence, supporting you and your loved one through every step of this journey.
5. Why should I choose a local, nonprofit hospice provider?
Choosing a local, nonprofit provider like Central Coast VNA & Hospice means you are partnering with an organization that is mission-driven and deeply invested in the community. With over 74 years of service to the Central Coast, our focus is on patient well-being, not profits. We have strong relationships with the local VA and understand how to provide seamless, compassionate care close to home.
The team at Central Coast VNA & Hospice is deeply committed to honoring our nation's heroes with the compassionate care they have earned. If you have more questions or you feel ready to start the conversation, please contact us today to learn how we can help.
Find Hospice Volunteer Opportunities Near Me in 2025
Finding the right place to volunteer your time and compassion is a deeply personal decision. This guide is designed to simplify your search for meaningful hospice volunteer opportunities near me by providing a resource list of dedicated hospice organizations. Prospective volunteers, from family members of former patients to community members, need clear information to make an informed choice.
This article offers detailed profiles of various hospice programs, including local leaders like Central Coast VNA & Hospice. For each organization, you will find a breakdown of their volunteer roles, training, and the unique benefits of serving with them. Understanding an organization's mission and the significance of workplace culture can greatly influence your experience. Our goal is to equip you with the practical details needed to find a volunteer match that fits your skills and your heart.
1. VNA & Hospice Volunteer Program
For those searching for comprehensive hospice volunteer opportunities near me, the VNA & Hospice Volunteer Program at Central Coast VNA & Hospice (CCVNA) stands out. This program offers a structured and deeply meaningful way to contribute. It is backed by a respected nonprofit with a 74+ year legacy of compassionate healthcare in California.
It provides an exceptional framework for volunteers to make a direct, positive impact on patients and families. The service area covers Monterey County, San Benito County, Santa Cruz County, and South Santa Clara County.
What truly distinguishes the CCVNA program is its diversity of roles. Unlike other programs with limited engagement, CCVNA allows you to align your skills with specific needs. You can provide companionship through direct patient visiting, support essential functions in an office setting, or participate in specialized initiatives like the Veteran-to-Veteran program.
Key Program Features & Benefits
Volunteers are integrated into a professional, interdisciplinary care team, including Registered Nurses, Chaplains, and Hospice Aides. They receive comprehensive training and ongoing support. This ensures you are fully prepared and confident in your role.
- Diverse & Specialized Roles: Find a perfect fit, from patient companionship and respite for families to specialized support for veterans.
- Structured Training: Receive thorough preparation to confidently and compassionately engage with patients and families.
- Reputable Organization: Contribute to a mission-driven nonprofit with deep community roots and a 74+ year history of excellence.
- Team Integration: Become an essential part of a professional care team, fostering personal growth and a strong sense of community.
The program requires a commitment to schedules and adherence to professional boundaries. Specialized roles like pet therapy may have extra screening requirements. For more details, explore the FAQs for the VNA & Hospice Volunteer Program on ccvna.com.
Visit the VNA & Hospice Volunteer Program Website
2. Allina Health Hospice Volunteer Opportunities
Allina Health offers a structured and diverse hospice volunteer program in the Minnesota region. Their program serves patients across 33 counties. Their website provides a clear pathway for individuals looking to find meaningful hospice volunteer opportunities near me.
The platform details a wide array of roles. This ensures that potential volunteers can find a position that aligns with their unique skills and interests.
What Makes It Stand Out
The key strength of Allina Health's program is its variety and comprehensive preparation. Volunteers can choose roles beyond basic companionship, including specialized services. Understanding the nuances between different types of end-of-life care is crucial, and you can learn more about the differences between palliative and hospice care to prepare for your role.
Practical Considerations
- Volunteer Roles: Options include patient companionship, family respite, bereavement support, massage therapy, and pet therapy.
- Training: Allina provides comprehensive training to ensure every volunteer feels prepared and confident.
- Geographic Reach: The program supports patients in private residences and hospice facilities throughout 33 Minnesota counties.
- Application Process: Be prepared for a thorough process that can take up to four weeks, reflecting their commitment to patient safety.
3. Providence Hospice of Seattle Volunteer Program
Providence Hospice of Seattle provides a compassionate framework for those searching for hospice volunteer opportunities near me in the Puget Sound region. Their program is well-regarded for its emphasis on specialized care. It serves patients in both King and Pierce Counties.
The program offers a thoughtful blend of direct patient support, pediatric care, bereavement services, and even complementary therapies. This ensures that individuals from all walks of life can find a fulfilling position.
What Makes It Stand Out
Providence distinguishes itself through its specialized volunteer tracks, particularly for pediatric patients and veterans. These tailored programs address the unique emotional and practical needs of specific patient populations. The comprehensive, role-specific training ensures every volunteer is prepared to handle the sensitivities of their assigned duties.
Practical Considerations
- Volunteer Roles: Opportunities include direct patient companionship, pediatric palliative care support (Safe Crossings program), veteran-to-veteran companionship, and administrative assistance.
- Training: Providence provides extensive, role-specific training to all volunteers before they begin their service.
- Geographic Reach: The program serves patients and families across King and Pierce Counties in Washington.
- Application Process: Be prepared for a detailed application, interview, and training process to ensure a good fit.
4. St. Luke's Hospice Services Volunteer Program
Based in Chesterfield, Missouri, St. Luke's Hospice Services provides a focused volunteer program for individuals looking to offer comfort. Their approach emphasizes direct patient interaction and administrative assistance. They create a variety of hospice volunteer opportunities near me for those in the St. Louis area.
The program is designed to integrate volunteers directly into the care team. They provide essential companionship and operational support that enhances the patient experience.
What Makes It Stand Out
St. Luke's stands out by offering flexible roles that cater to different personalities and skill sets. This flexibility allows volunteers to contribute in a way that feels most natural to them. Prospective volunteers should be prepared to contact the volunteer coordinator directly to learn more about the specifics of hospice care.
Practical Considerations
- Volunteer Roles: Core opportunities include direct patient companionship, providing respite for families, and assisting with administrative tasks.
- Training: St. Luke's provides the necessary training to ensure volunteers are prepared to offer compassionate support.
- Geographic Reach: The program primarily serves patients within the greater St. Louis, Missouri area.
- Application Process: The process requires reaching out to the volunteer coordinator via phone or email for an application.
5. The Hospice of East Texas Volunteer Program
Serving a 23-county region, The Hospice of East Texas offers a community-focused volunteer program. It appeals to a wide range of individuals searching for hospice volunteer opportunities near me. Its website clearly outlines diverse roles that extend beyond patient homes and into the broader community.
These roles include administrative work, event support, and even assisting in their resale shops. This variety ensures that every volunteer can contribute in a meaningful and comfortable way.
What Makes It Stand Out
The program’s standout feature is its integration of community engagement with traditional hospice support. Volunteers can choose roles that directly impact patient care or support the organization’s mission through other avenues. This model allows people with different skill sets and comfort levels to participate.
Practical Considerations
- Volunteer Roles: Opportunities include direct patient companionship, administrative assistance, special event support, and working in the organization’s resale shops.
- Training: Comprehensive training is provided to all volunteers, ensuring they are well-prepared for their roles.
- Geographic Reach: The program serves patients and families across 23 counties in East Texas.
- Application Process: Prospective volunteers must be at least 18 years old and complete a detailed application and training process.
6. Providence Portland Medical Center Hospice Volunteering
Providence offers a well-established program for those searching for hospice volunteer opportunities near me in the Portland, Oregon area. Their platform clearly outlines the path to becoming a volunteer. It emphasizes roles that support patients and families directly or assist with administrative tasks.
The program is designed to match an individual’s unique skills with the specific needs of their hospice patients.
What Makes It Stand Out
The standout feature of Providence's hospice program is its focus on creating a supportive and well-prepared volunteer community. They provide comprehensive, multi-session training to ensure volunteers feel confident. This commitment to preparation fosters a strong, capable team dedicated to compassionate end-of-life care.
Practical Considerations
- Volunteer Roles: Opportunities include direct patient and family support, administrative office help, and bereavement program assistance.
- Training: A comprehensive training program is mandatory, preparing volunteers for the emotional and practical aspects of hospice work.
- Geographic Reach: The program primarily serves patients within the Providence Portland Medical Center's service area.
- Application Process: Expect a thorough screening and application process. You can learn more on their website.
7. Elara Caring Hospice Volunteer Program
Elara Caring offers a robust and geographically diverse program for those searching for hospice volunteer opportunities near me. With operations spanning multiple states, their platform provides an accessible entry point for individuals. The program emphasizes flexibility, allowing volunteers to find roles that align with their interests.
What Makes It Stand Out
The primary strength of Elara Caring's program is its widespread reach and structured training. This ensures a consistent and high-quality experience for both volunteers and patients. You can discover more about the benefits of palliative care to see how volunteers contribute to patient comfort.
Practical Considerations
- Volunteer Roles: Flexible options include patient companionship, family respite, bereavement support calls, and office administrative assistance.
- Training: Comprehensive training is provided to prepare volunteers for their duties and ensure they feel confident and supported.
- Geographic Reach: Opportunities are available across the multiple states where Elara Caring provides hospice services.
- Application Process: The online application is straightforward, though some specialized roles might require additional certifications.
8. The Denver Hospice Volunteer Program
The Denver Hospice provides a robust and compassionate volunteer program for those in the Denver metropolitan area. Their website clearly outlines the journey for anyone searching for hospice volunteer opportunities near me. The program is distinguished by its inclusion of integrative therapies.
What Makes It Stand Out
The standout feature of The Denver Hospice is its commitment to holistic and integrative care. Volunteers with specific certifications can provide services like Reiki or pet therapy. Understanding what to expect during this time can help volunteers feel prepared; you can learn what happens in the last days of life to gain valuable insight.
Practical Considerations
- Volunteer Roles: Opportunities range from direct patient companionship and family relief to administrative office support.
- Specialized Therapies: The program actively seeks volunteers certified in Reiki and pet therapy to provide integrative support.
- Training: Comprehensive training is mandatory, ensuring all volunteers are equipped with the skills and confidence needed.
- Application Process: Be aware that some specialized roles, such as Reiki, will require proof of certification during the application process.
9. Hospice of Southern Maine Volunteer Program
Hospice of Southern Maine provides a well-defined and supportive framework for individuals looking for hospice volunteer opportunities near me. Their program is designed to welcome volunteers from all walks of life. Roles range from direct patient companionship to specialized services like music and pet therapy.
The organization emphasizes creating a strong, supportive community for its volunteers through comprehensive training and ongoing guidance.
What Makes It Stand Out
The standout feature of this program is its deep commitment to volunteer support and training. Hospice of Southern Maine ensures every volunteer feels equipped and valued. You can explore more about the value of giving back to organizations like VNA to understand the mutual benefits of such programs.
Practical Considerations
- Volunteer Roles: Opportunities include direct patient care, companionship, administrative assistance, music support, and pet therapy.
- Training: Comprehensive training is mandatory to prepare volunteers for the emotional and practical aspects of their roles.
- Geographic Reach: The program serves communities throughout Southern Maine.
- Application Process: Prospective volunteers must be at least 18 years old and should expect a detailed application and screening process.
10. Chicago Hope and Palliative Healthcare Volunteer Program
Chicago Hope and Palliative Healthcare offers a community-focused program for those searching for hospice volunteer opportunities near me in the Chicago area. Their approach is centered on matching a volunteer's unique skills with the specific needs of patients. Roles extend beyond traditional companionship, encompassing a holistic volunteer ecosystem.
What Makes It Stand Out
The primary strength of the Chicago Hope program is its flexibility and commitment to personalized role placement. The emphasis is on direct conversation to find the perfect fit for each volunteer. This ensures that every individual can contribute in a meaningful way.
Practical Considerations
- Volunteer Roles: Opportunities include direct patient care, grief and bereavement support, community outreach, and various administrative tasks.
- Training: All volunteers receive thorough training to prepare them for their roles and are provided with continuous support.
- Geographic Reach: The program is focused on serving patients and families within the greater Chicago metropolitan area.
- Application Process: The website encourages direct contact to learn more about specific roles and the application process.
11. Hospice Atlanta Volunteer Program
Hospice Atlanta provides a deeply community-focused program for those searching for hospice volunteer opportunities near me in the Atlanta area. Their website outlines how volunteers can contribute. The program is designed to be flexible, supporting patients in various settings.
What Makes It Stand Out
The strength of Hospice Atlanta's program lies in its flexibility and comprehensive support. It stands out by offering unique roles like pet care assistance, recognizing that support extends to beloved companions. This holistic approach ensures volunteers can find a niche where their passions can make a difference.
Practical Considerations
- Volunteer Roles: Opportunities include direct patient companionship, family respite, bereavement support, helping with special events, and pet care assistance.
- Training: Comprehensive training is mandatory, equipping volunteers with the necessary skills and emotional preparedness.
- Geographic Reach: The program serves patients and families throughout the greater Atlanta area.
- Application Process: Expect a detailed application and screening process, as some roles may require additional background checks.
12. Connecticut Hospice Volunteer Program
As a pioneering organization, the Connecticut Hospice Volunteer Program offers a deeply established framework for those searching for hospice volunteer opportunities near me. The program serves patients statewide. It provides a supportive entry point for individuals aged 18 and older.

What Makes It Stand Out
The key strength of this program is its rich history and integration of specialized volunteer roles. By offering opportunities in music and pet therapy, Connecticut Hospice acknowledges the diverse ways volunteers bring comfort. Their comprehensive training ensures every volunteer feels prepared and valued.
Practical Considerations
- Volunteer Roles: Opportunities include direct patient companionship, administrative assistance, music support, and certified pet therapy visits.
- Training: All volunteers receive comprehensive, mandatory training to prepare them for their roles and responsibilities.
- Geographic Reach: The program supports patients in their homes and at the main hospice facility, serving communities across Connecticut.
- Application Process: Prospective volunteers must complete an application and interview, with an age requirement of 18 or older.
Volunteer Program Comparison of 12 Hospice Providers
| Volunteer Program | Core Features/Roles | Training & Support | Target Audience 👥 | Unique Selling Points ✨ | Accessibility & Commitment 💰 |
|---|---|---|---|---|---|
| VNA & Hospice Volunteer Program (CCVNA) | Diverse roles: patient visits, pet therapy, office support | Comprehensive training & ongoing support | Community members across CA Central Coast | 74-year legacy 🏆, veteran & pet therapy, interdisciplinary team | Schedule commitment; some roles need qualifications |
| Allina Health Hospice Volunteer | Companion, bereavement, massage, pet therapy | Structured comprehensive training | Volunteers in 33 MN counties | Broad geographic coverage ✨ | 4-week application process |
| Providence Hospice of Seattle | Patient support, pediatric care, bereavement, therapies | Role-specific comprehensive training | King & Pierce Counties volunteers | Specialized pediatric & veteran programs 🏆 | Some roles require certifications |
| St. Luke's Hospice Services | Patient interaction, administrative support | Basic training implied | Chesterfield, MO community | Flexible roles | Limited online info; contact needed |
| The Hospice of East Texas | Patient care, admin, resale shop, events | Comprehensive training & support | Volunteers in 23 TX counties | Resale shop & event support ✨ | Must be 18+ years |
| Providence Portland Medical Center | Patient, bereavement, admin roles | Comprehensive training & support | Portland, OR area volunteers | Supportive environment, diverse roles | Some roles require certifications |
| Elara Caring Hospice | Companionship, bereavement, admin | Comprehensive training & volunteer support | Multi-state volunteers | Flexible multi-location roles ✨ | Some require certifications |
| The Denver Hospice | Patient care, Reiki, pet therapy, admin | Comprehensive training programs | Denver area volunteers | Integrative therapies like Reiki & pet therapy | Certain roles require certifications |
| Hospice of Southern Maine | Patient care, pet therapy, music, admin | Comprehensive training & support | Southern Maine community volunteers | Emphasis on complementary therapies | Volunteers must be 18+ |
| Chicago Hope and Palliative Health | Patient care, grief support, outreach, admin | Comprehensive training & support | Chicago area volunteers | Community outreach roles ✨ | Limited online info; contact needed |
| Hospice Atlanta | Patient companionship, bereavement, pet care, events | Comprehensive training programs | Atlanta area volunteers | Pet care & event support | Some roles require certifications |
| Connecticut Hospice | Patient care, admin, pet therapy, music | Comprehensive training & support | Statewide volunteers 18+ | Music and pet therapy specialization | Volunteers must be 18+ |
Final Thoughts
Finding the right way to give back can feel like a significant undertaking. However, there are numerous paths to making a profound impact. Your search for "hospice volunteer opportunities near me" is the first step toward a rewarding journey.
This journey offers comfort, dignity, and companionship to individuals and families during a critical time. We've explored a variety of programs, each with its own unique structure and community focus. The key takeaway is that no single volunteer role fits everyone.
Making Your Decision: Key Considerations
As you evaluate opportunities, it’s crucial to look beyond basic role descriptions. Consider the following factors to ensure a fulfilling and sustainable commitment:
- Training and Support: Does the organization offer comprehensive training? A strong support system for volunteers is essential for preventing burnout.
- Time Commitment: Be realistic about the time you can dedicate. Some programs require a weekly commitment, while others are more flexible.
- Alignment with Your Values: Reflect on what matters most to you. Finding an organization whose mission resonates with your values will make your service more meaningful.
Ultimately, volunteering in hospice care is a powerful act of compassion. It is a commitment that gives back in immeasurable ways. The perfect role for you is out there, waiting for someone with your unique compassion and willingness to serve.
Frequently Asked Questions (FAQs)
1. What do hospice volunteers typically do?
Hospice volunteers perform a variety of tasks based on their skills and the patient's needs. Common roles include providing companionship, reading to patients, offering respite for family members, helping with light errands, or providing administrative support at the hospice office. Specialized roles like pet or music therapy are also available at organizations like Central Coast VNA & Hospice.
2. Do I need a medical background to volunteer for hospice care?
No, a medical background is not required for most hospice volunteer roles. Organizations like Central Coast VNA & Hospice provide comprehensive training to prepare you for patient and family interactions. The most important qualifications are compassion, empathy, and a willingness to offer comfort and support.
3. What is the time commitment for a hospice volunteer?
The time commitment varies by organization. Most programs ask for a commitment of a few hours per week to ensure consistency for patients. However, many programs, including CCVNA's, offer flexible roles that can accommodate different schedules, such as helping with events or administrative tasks.
4. Can I volunteer if I have recently experienced a loss?
Most hospice organizations recommend waiting for a period of time, typically one year, after a significant personal loss before volunteering. This allows you time to grieve properly, ensuring that your volunteer experience is healthy and positive for both you and the patients you serve.
5. How do I get started as a hospice volunteer in Monterey County or surrounding areas?
To volunteer on the Central Coast of California, you can start by visiting the Central Coast VNA & Hospice website. The application process typically involves an application form, an interview, a background check, and a comprehensive training program to prepare you for your role. Contacting the volunteer coordinator is a great first step.
If you are located in Monterey County, San Benito County, Santa Cruz County, or South Santa Clara County and feel inspired to make a difference, we invite you to explore opportunities at VNA and Hospice. With over 74 years of nonprofit service to the Central Coast community, our volunteer program is a cornerstone of our compassionate continuum of care. Learn more about how you can join our dedicated team by visiting VNA and Hospice today.










