A Guide to Qualifying for Home Health Care in California
Navigating the first steps toward getting medical care at home can feel overwhelming, but it all boils down to a few core requirements. Knowing what they are ahead of time makes the entire process much smoother for your family.
At Central Coast VNA & Hospice, we have guided families through this for over 74 years. Serving Monterey, San Benito, Santa Cruz, and South Santa Clara counties, our nonprofit mission is to help patients get the expert support they need in the comfort of their own homes.
The Foundational Requirements for Eligibility
To start, let’s get straight to the point. Qualifying for home health care, especially when using Medicare, hinges on a few specific, non-negotiable criteria. These rules are in place to ensure services go to the people who truly need them most.
You generally need to meet these three conditions:
- A Doctor's Order: A physician must formally certify that you need medical care at home. This is not just a suggestion; it’s a requirement that kicks off a formal plan of care.
- Need for Skilled Care: The care you need must be something that requires a licensed professional, like a Registered Nurse or a Physical Therapist. This is different from needing help with daily chores; it’s about medical treatment.
- Being Homebound: This is a big one. It means that leaving your home takes a considerable and taxing effort, making outpatient care a significant challenge.
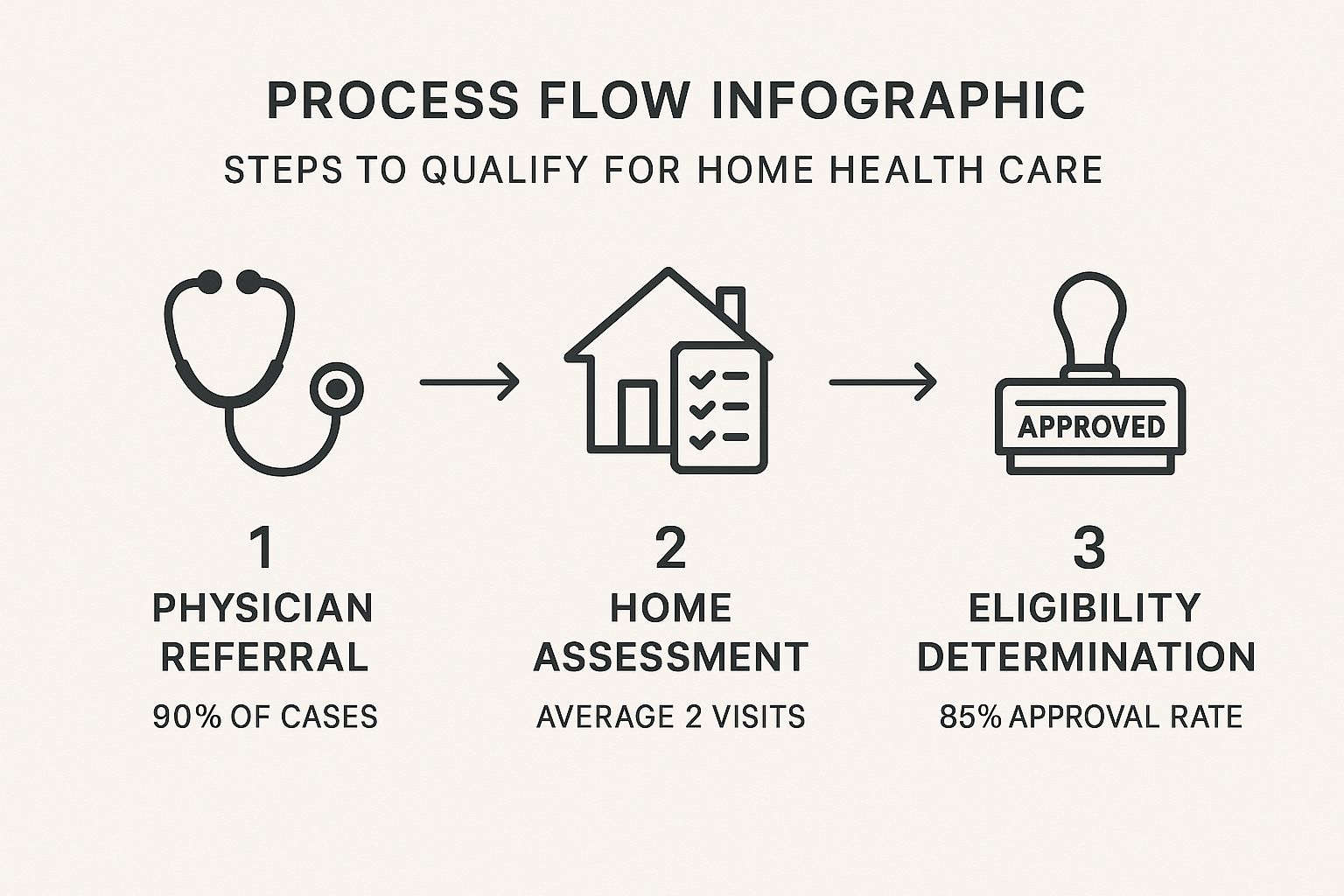
As you can see, it almost always starts with a doctor's referral. From there, a home health agency like Central Coast VNA & Hospice conducts an in-home assessment to confirm that home health is the right fit.
Core Eligibility Requirements at a Glance
To make this even clearer, here’s a simple breakdown of what these requirements mean in the real world. Our team helps families in Monterey County and surrounding areas understand these rules every day.
| Requirement | What It Means for Your Family | A Real-World Example |
|---|---|---|
| Doctor's Order | Your loved one's primary physician must create and sign a plan of care that outlines the necessary medical services. | After a hospital stay for a broken hip, a doctor orders physical therapy and skilled nursing at home to manage wound care and monitor recovery. |
| Homebound Status | Leaving home requires significant effort (e.g., using a walker, wheelchair, or needing help from others) and is infrequent. | A person with severe COPD who becomes short of breath after walking a few feet would be considered homebound, even if they can leave for doctor's visits. |
| Skilled Care Need | The patient needs intermittent services from a licensed professional, not just custodial or personal care. | A Registered Nurse is needed to administer IV antibiotics, or a speech therapist is required to help a stroke survivor regain their ability to swallow safely. |
Understanding these distinctions is key. They separate patients who qualify for these specialized medical services from those who might need other types of in-home assistance.
Medicare’s Role in Home Health Services
For millions of Americans, Medicare is the primary way to pay for home health care. In fact, in 2020, about 3.4 million Medicare beneficiaries relied on these services to recover at home. Because of this, Medicare's rules have become the gold standard that many private insurance plans follow.
At its heart, qualifying for home health care is about matching a patient's medical needs with the right professional support. It's about bringing a clinical team's expertise directly to the patient's bedside to foster safety, healing, and independence.
Central Coast VNA & Hospice is a nonprofit dedicated to providing these vital home health care services. We specialize in creating a smooth transition from the hospital back to the home, supporting patients every step of the way on their recovery journey.
Your Doctor's Role in Creating a Plan of Care

Your journey into home health care almost always begins with your physician. A doctor's official order, which comes after a thorough medical assessment, is what truly opens the door to receiving specialized services in your own home.
This order kicks off the creation of a vital document: the plan of care. You can think of it as the personalized roadmap for your recovery. It’s a collaborative game plan developed by your doctor and the clinical team from the home health agency.
What the Plan of Care Includes
The plan of care is the central hub that guides every single aspect of your treatment. It’s what keeps everyone on the same page—from your doctor to you, your family, and the entire home health team.
A truly comprehensive plan of care will spell out:
- Specific Services Needed: It clearly states which types of skilled care are medically required, whether that’s skilled nursing, physical therapy, occupational therapy, or speech-language pathology.
- Frequency and Duration of Visits: The plan details exactly how often a Registered Nurse or therapist will visit and gives an idea of how long you’ll need the services.
- Primary Diagnoses: This section identifies the specific medical conditions that make home-based care necessary.
- Health and Recovery Goals: It sets clear, measurable objectives, such as improving your ability to walk safely or managing pain.
- Medication and Treatment Orders: All medications, treatments, and any necessary medical supplies are documented right here.
To make sure your doctor’s orders and the resulting plan meet the strict eligibility requirements, it helps to understand essential medical documentation guidelines. This is the paperwork that justifies why the services in the plan are needed.
A Real-World Example in Salinas
Let’s look at how this plays out in a real-life situation. Imagine Maria, a Salinas resident in Monterey County, who is home after a hip replacement. Her surgeon knows she needs professional medical support to heal safely and properly at home.
The surgeon sends a referral to Central Coast VNA & Hospice. A CCVNA Registered Nurse then visits Maria at her home to do an initial assessment. From there, Maria’s surgeon and the CCVNA nurse work together to build her detailed plan of care.
This collaborative approach ensures that the plan of care is not just a document, but a living guide tailored to the patient's unique home environment and recovery needs. It bridges the gap between hospital-level care and safe, independent living.
For Maria, this personalized plan includes:
- Skilled nursing visits twice a week for wound care and to watch for any signs of infection.
- Physical therapy sessions three times a week to help her get her strength and mobility back.
- Medication management to keep pain under control and prevent complications like blood clots.
This plan gives Maria, her family, and her entire care team a clear path forward. It’s this physician-led, team-based approach that makes qualifying for home health care so effective, bringing expert medical support directly into homes across the Central Coast. Central Coast VNA & Hospice offers a wide variety of these home care services designed to support recovery and independence.
What 'Homebound' and 'Skilled Care' Really Mean

When families start looking into their options, a couple of terms almost always cause some confusion: "homebound" and "skilled care." Getting a handle on what these words actually mean in a medical context is essential, as they are the cornerstones of qualifying for home health services.
Defining 'Homebound' in the Real World
Let's tackle "homebound" first. The word itself sounds pretty restrictive, but it doesn't mean your loved one has to be confined to a bed. Instead, it’s a term used to describe a situation where leaving home takes a considerable and taxing effort.
Someone is considered homebound if they need help from another person or a device like a walker to leave home safely. Occasional, short trips for things like doctor's appointments, religious services, or even a haircut are generally fine.
Think about a patient in Santa Cruz County who's recovering from heart surgery. The thought of walking to the car and going to an appointment would leave them exhausted. This person is a perfect example of someone who is homebound.
The Meaning of 'Skilled Care'
The other key term is "skilled care." This isn't just any kind of help; it refers specifically to medical services that can only be performed correctly and safely by a licensed health professional like a Registered Nurse.
Skilled care is different from personal or custodial care, which covers assistance with activities like bathing and dressing. While a Home Health Aide can certainly provide personal care, it's typically only covered by insurance when a patient also needs skilled services. You can get a deeper understanding of these differences by reading our article on home health vs. hospice.
What does skilled care look like in practice? Here are a few examples:
- Skilled Nursing: A Registered Nurse (RN) visits to manage a complex wound, administer IV medications, or teach a patient about their condition.
- Physical Therapy: A Physical Therapist (PT) guides someone through targeted exercises to rebuild strength and balance after a fall or a stroke.
- Speech-Language Pathology: A therapist works with a patient to help them regain the ability to speak clearly or swallow safely.
- Occupational Therapy: An Occupational Therapist (OT) retrains a patient on how to safely handle daily tasks like bathing or cooking.
"During our first visit, we do more than just check vital signs. We have a compassionate conversation to understand the whole picture—how a patient feels, what challenges they face at home, and what their personal goals are. This helps us ensure the plan of care truly supports their safety and well-being." - Central Coast VNA & Hospice Clinician
This focus on skilled, professional care delivered right in the home is particularly critical for older adults. In fact, about 86% of all home health care patients in the United States are age 65 or older. For a broader look at the data, you can discover more home health insights and statistics.
Navigating Medicare and Other Insurance Coverage
Figuring out the financial side of home health care is often the biggest source of relief for families we work with. Once a doctor has certified that home-based medical care is necessary, the next logical question is always, "How are we going to pay for this?"
For most of our patients in Monterey, San Benito, Santa Cruz, and South Santa Clara counties, Medicare is the primary payer. It’s a huge weight off their shoulders to learn that when all criteria are met, Medicare Part A and Part B typically cover 100% of the cost for home health services.
What Medicare Typically Covers
When you qualify, Medicare coverage is quite specific. It's designed to pay for the intermittent, medically necessary services that help you recover from an illness, injury, or surgery.
Here's what that usually includes:
- Skilled Nursing Care: Provided on a part-time or intermittent basis by a Registered Nurse.
- Physical Therapy: To help restore mobility, balance, and strength.
- Occupational Therapy: To help you regain the ability to safely perform daily activities.
- Speech-Language Pathology Services: To address issues with communication or swallowing.
- Home Health Aide Services: For assistance with personal care, but only if you're also receiving skilled nursing or therapy.
It's just as important to know what Medicare doesn't cover. For example, it won't pay for 24-hour care at home, meal delivery, or "custodial care" if that's the only assistance you need. For anyone looking to bridge the gaps in Original Medicare, finding the best Medicare Supplement Plan is often a critical piece of the puzzle.
The goal of insurance coverage for home health is to provide the precise medical support needed for recovery, not to replace the non-medical help a family might provide. It’s about clinical care delivered in the home environment.
Private Insurance, Medi-Cal, and Other Payers
While many private insurance plans and Medi-Cal (California's Medicaid program) often follow Medicare's lead, their rules can vary. It's always best practice to contact your insurance provider directly to confirm your specific benefits.
At Central Coast VNA & Hospice, our team is here to help families make sense of their coverage options. As a local nonprofit provider with over 74 years of experience, we do everything we can to minimize financial surprises so you can focus on healing.
The Growing Shift Towards Home-Based Medical Care

Home health care isn't just about convenience anymore. It represents a real, positive change in how modern medicine works, and both patients and doctors are realizing that the best place to heal is often right at home.
This isn't just a fleeting trend. It’s a movement driven by our country's aging population and clear clinical proof that home-based treatment is highly effective. This evolution in healthcare aligns perfectly with our 74-year mission here at Central Coast VNA & Hospice.
Why Home Is Becoming the Preferred Place for Care
The desire to receive care at home goes beyond simple comfort—it's about getting better results. Thanks to incredible advances in technology, like telehealth and remote monitoring, sophisticated medical supervision is no longer confined to a hospital room.
This shift is making waves economically, too. The global home healthcare industry, which was valued at around USD 416.4 billion in 2024, is expected to keep growing as more people need ongoing medical support in their own homes.
Qualifying for home health care is more than just a procedural step. It’s an opportunity to embrace a better, more patient-centered model of care that prioritizes dignity, independence, and healing in the place you feel most secure.
This model lets people recover on their own terms, with the people and things they love close by. You can see this firsthand in stories about how people like veteran Nolan Chandler are impacting lives through home care.
Embracing a Better Model of Healing
For families living in Monterey County, San Benito County, Santa Cruz County, and South Santa Clara County, this shift means you have access to a higher standard of personalized medicine. It means less time in institutional settings and more time focusing on what really matters: getting better.
When you partner with a provider like CCVNA, you're choosing a team that is completely dedicated to this modern, compassionate philosophy. Families get incredible peace of mind knowing their loved one is receiving expert, one-on-one attention. If you're starting to explore your options, you might find our guide on the 9 ways home health care will benefit your loved one helpful.
Frequently Asked Questions About Home Health Eligibility
It is completely normal to have questions when first exploring home health care. Getting clear, straightforward answers is the best way to feel confident you are making the right choice for a loved one. With over 74 years of experience, our team at Central Coast VNA & Hospice is here to help you navigate the process.
We have gathered some of the most frequent questions we hear from families across Monterey, San Benito, Santa Cruz, and South Santa Clara counties. Let's tackle them one by one.
1. How do I start the process with Central Coast VNA & Hospice?
Getting started is simple. It all begins with a conversation with your doctor. Ask them if a referral for home health care might be a good fit for you. Your doctor can then send a referral directly to our team. You or your family members are always welcome to call us directly to ask questions and learn more.
2. Can I qualify if I live in an assisted living facility?
Yes, you absolutely can. A person's "home" can be a private house, an assisted living facility, or a group home. The key is meeting the other core eligibility criteria: you need a doctor’s order, must be considered homebound, and require intermittent skilled care.
3. How long can someone receive home health care services?
The length of care is based entirely on your specific medical needs and the goals in your physician-approved plan of care. Home health care is typically approved in 60-day periods. If you still need skilled support after 60 days, your doctor can "recertify" your care for another period.
4. What if my condition improves and I’m no longer homebound?
This is fantastic news and the goal of our services. The purpose of home health care is to help you recover to the point where you can manage safely on your own. If you are no longer homebound or no longer require skilled medical care, you would no longer meet the Medicare criteria for our services, and your care team would plan a safe discharge.
5. Are personal care services like bathing covered?
This is a very common question. Personal care from a Home Health Aide—like help with bathing or dressing—can be covered by Medicare, but with one critical rule. These services are only covered if they are part of a larger plan of care that also includes skilled services, like skilled nursing or physical therapy. For a deeper look, we've explained home health eligibility in detail in another guide.
At Central Coast VNA & Hospice, our mission as a nonprofit organization is to provide compassionate, high-quality care that helps you heal in the comfort of your own home. If you have more questions about qualifying for home health care or want to explore our continuum of care, from home health to palliative and hospice services, please reach out to us.
Learn more about how we can help by visiting https://ccvna.com or calling us today. We are here to serve the communities of Monterey County, San Benito County, Santa Cruz County, and South Santa Clara County.
7 Fulfilling Non-Profit Healthcare Jobs to Start in 2025
Are you searching for a career that offers more than just a paycheck? A role rooted in mission and community impact can provide profound personal and professional satisfaction.
For those drawn to serving others, non-profit healthcare jobs present a unique opportunity to align your skills with a meaningful purpose. These positions go beyond traditional clinical settings, focusing on compassionate, patient-centered care that addresses the whole person.
This guide illuminates a path for individuals seeking fulfilling work on the California Central Coast. We will explore key roles within a non-profit healthcare framework, from community-facing positions to vital administrative functions. You will gain a clear understanding of the responsibilities these professionals bring to patients and families across Monterey County, San Benito County, Santa Cruz County, and South Santa Clara County.
1. Program Manager - Global Health Initiatives
One of the most dynamic non-profit healthcare jobs is the Program Manager for Global Health Initiatives. These professionals are the architects of complex health programs, often addressing critical issues like disease prevention and access to essential medicines.
A Program Manager orchestrates everything from initial strategy to on-the-ground implementation. This role is pivotal in ensuring resources are used effectively to achieve life-saving goals.
They lead multi-disciplinary teams, manage substantial budgets, and navigate intricate political and social landscapes. The work is demanding but offers the profound reward of shaping health outcomes for entire communities.
Core Responsibilities and Required Skills
A Program Manager's duties are multifaceted, requiring a unique blend of leadership, technical knowledge, and strategic acumen. Their primary responsibilities include designing program frameworks, securing funding, and monitoring progress.
Success in this role hinges on a robust skill set that combines project management with a deep understanding of public health.
This infographic illustrates the hierarchical nature of a Program Manager's core functions, from high-level strategy to team and financial oversight.
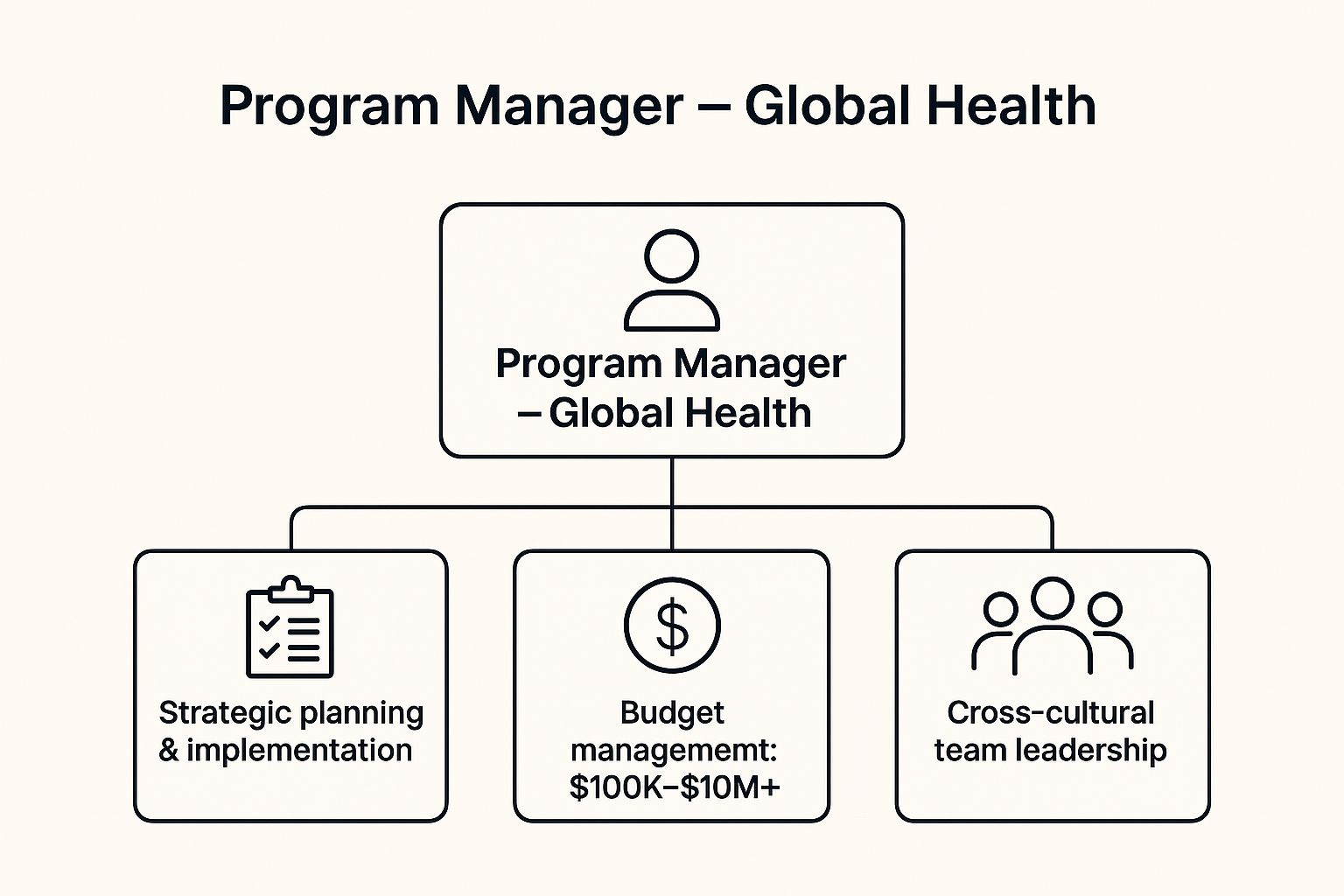
As visualized, strategic planning forms the foundation. This directly influences the management of budgets and the leadership of diverse, cross-cultural teams.
How to Pursue This Career Path
To become a Program Manager in global health, a strategic approach to building your expertise is essential.
- Gain Certifications: A Project Management Professional (PMP) certification is highly valued and demonstrates your ability to manage complex projects.
- Acquire International Experience: Volunteer with organizations like the Peace Corps or Doctors Without Borders to gain firsthand field experience.
- Develop Language Skills: Fluency in French, Spanish, or Portuguese can be a significant advantage, opening doors to programs in Latin America and Africa.
- Specialize Your Knowledge: Build deep expertise in a specific area, such as maternal-child health or infectious diseases, to become a more competitive candidate.
2. Grant Writer and Development Specialist
One of the most vital non-profit healthcare jobs is the Grant Writer and Development Specialist. These professionals are the financial lifeline, securing the necessary funding that allows mission-driven organizations to deliver essential medical services.
They are storytellers and strategists, translating an organization's impact into compelling narratives that resonate with funders. A Grant Writer ensures a non-profit has the resources to not just operate, but to innovate and expand its reach.
This role is fundamental for local health centers applying for funding to serve vulnerable populations. The work is detail-oriented, but it provides the satisfaction of knowing your efforts directly enable patient care and community wellness programs.
Core Responsibilities and Required Skills
A Grant Writer's duties demand a unique combination of exceptional writing, meticulous research, and strategic relationship management. Their core responsibilities include identifying grant prospects, drafting high-quality proposals, and tracking outcomes.
This position is a blend of art and science. It requires creative storytelling to articulate the organization's mission and analytical precision to manage budgets and data.
Their work ensures every dollar is accounted for and supports program goals. This includes everything from providing in-home nursing to funding supportive community services.
How to Pursue This Career Path
To become a successful Grant Writer, you must strategically build a foundation of specialized skills and a proven track record.
- Build a Strong Portfolio: Assemble a collection of successful grant applications, including narratives and budgets, to showcase your abilities.
- Develop Funding Expertise: Specialize in specific funding streams, such as grants from the Centers for Disease Control and Prevention (CDC) or local community foundations.
- Master Key Tools: Become proficient in using donor databases like Salesforce or Blackbaud Raiser's Edge to manage relationships and track progress.
- Join Professional Associations: Network and gain credentials through organizations like the Association of Fundraising Professionals (AFP).
- Collaborate with Program Staff: Develop strong internal relationships to gather powerful patient stories and accurate data for grant proposals.
3. Community Health Worker Coordinator
For those dedicated to grassroots healthcare, the Community Health Worker (CHW) Coordinator is one of the most vital non-profit healthcare jobs. These professionals lead teams of frontline public health workers who bridge the gap between residents and the healthcare system.
A CHW Coordinator ensures their team provides health education, connects individuals to services, and advocates for underserved populations.

They are responsible for the training, supervision, and ongoing support of Community Health Workers. This role is crucial in local health departments and non-profits focused on community outreach.
By managing these programs, CHW Coordinators directly address social determinants of health. They empower community members to take control of their well-being.
Core Responsibilities and Required Skills
A Community Health Worker Coordinator's duties require a deep understanding of community dynamics combined with strong leadership. Key responsibilities include recruiting and training CHWs and developing outreach strategies.
Success depends on a diverse skill set that blends social advocacy with programmatic oversight. The CHW Coordinator role is pivotal in translating public health strategy into tangible, community-level action.
These professionals must be adept at program management, fostering trust and communication. This involves strong interpersonal skills and a genuine commitment to community empowerment, central to the mission of organizations like Central Coast VNA & Hospice.
How to Pursue This Career Path
Becoming a Community Health Worker Coordinator involves building a foundation in public health and hands-on community engagement.
- Gain Field Experience: Start by working or volunteering in roles related to community organizing or social work to understand community needs.
- Develop Multicultural Competencies: Becoming bilingual (e.g., in Spanish for communities in Monterey or Santa Cruz County) is essential for serving diverse populations.
- Understand Social Determinants of Health: Pursue education focused on how factors like housing and food security impact health outcomes.
- Obtain Certifications: Many states offer certifications for Community Health Workers, which can be a prerequisite for leadership roles.
4. Clinical Research Coordinator
One of the most vital non-profit healthcare jobs is the Clinical Research Coordinator. These detail-oriented professionals are the operational backbone of clinical trials and research studies designed to improve patient outcomes.
A Clinical Research Coordinator manages the day-to-day activities of a study. They recruit and enroll participants and ensure every piece of data is meticulously collected and recorded.
They work at the intersection of patient care and scientific inquiry. The work is precise but offers the immense satisfaction of contributing directly to evidence-based practices that shape the future of healthcare.
Core Responsibilities and Required Skills
A Clinical Research Coordinator's duties are diverse, demanding a unique combination of organizational prowess and interpersonal skills. Key responsibilities include screening patients, managing study documentation, and ensuring compliance with Good Clinical Practice (GCP) guidelines.
They must navigate complex regulatory requirements and communicate effectively with patients, investigators, and sponsors. The coordinator's work ensures the integrity of research, which is critical for developing new treatments.
This is especially true in fields like palliative care, where new approaches to symptom management are constantly being explored. Research informs CCVNA’s approach to palliative care.
How to Pursue This Career Path
To become a Clinical Research Coordinator and excel in this essential non-profit role, a focused approach to building your qualifications is key.
- Obtain Key Certifications: Earning a certification like the Certified Clinical Research Coordinator (CCRC) from the Association of Clinical Research Professionals (ACRP) validates your expertise.
- Learn Good Clinical Practice (GCP): A deep understanding of GCP guidelines is non-negotiable, as it forms the ethical and scientific quality standard for all clinical trials.
- Develop Technical Proficiency: Gain hands-on experience with electronic data capture (EDC) systems and other clinical trial management software.
- Strengthen Communication Skills: Your ability to clearly explain complex trial procedures to patients is fundamental to successful participant retention.
5. Public Health Data Analyst
For those driven by data, one of the most vital non-profit healthcare jobs is the Public Health Data Analyst. These professionals are the investigators and storytellers of healthcare, transforming raw numbers into actionable intelligence.
They collect, clean, and interpret complex health data to uncover trends and guide evidence-based decisions. Their work is designed to improve public well-being on a community-wide scale.

A Public Health Data Analyst is central to the mission of organizations focused on population health. They might work to analyze hospital readmission rates or monitor disease outbreaks for a local health department.
The insights they generate are critical. Their work ensures healthcare interventions are not just well-intentioned but are also measurably effective.
Core Responsibilities and Required Skills
A Public Health Data Analyst's role is a blend of technical prowess and strategic thinking. Their primary duties include managing large datasets, applying statistical methods, and creating compelling reports for stakeholders.
Key responsibilities involve identifying health disparities and evaluating the impact of public health interventions. Mastering these tasks is essential for driving meaningful improvements in community health.
This ensures organizations like CCVNA can tailor services, such as home health or palliative care, to the needs of populations in Monterey and San Benito Counties.
How to Pursue This Career Path
Building a career as a Public Health Data Analyst involves a deliberate focus on acquiring specialized technical skills.
- Master Statistical Software: Proficiency in statistical packages like R, SAS, or Python is highly valued in the field.
- Develop Data Visualization Skills: Gain expertise in tools like Tableau or Power BI to create interactive dashboards that tell a compelling story.
- Learn SQL and Database Management: Strong SQL skills are fundamental for retrieving and manipulating data from the relational databases common in healthcare.
- Understand Healthcare Data Standards: Familiarity with standards like HL7 and FHIR is essential for working with electronic health records.
6. Patient Navigator
For patients and families navigating healthcare complexities, a Patient Navigator is a compassionate guide and indispensable advocate. This role is one of the most hands-on and impactful non-profit healthcare jobs, focused on helping individuals overcome barriers to care.
Navigators coordinate the entire patient journey. They handle everything from scheduling appointments to accessing financial aid and community resources.
They serve as the central point of contact, ensuring seamless communication between patients, physicians, and other providers. The work is deeply personal, offering the reward of directly improving a patient's ability to receive timely and appropriate care.
Core Responsibilities and Required Skills
A Patient Navigator's responsibilities require a unique combination of empathy, organizational skill, and system-level knowledge. Their primary duties involve assessing patient needs, creating care plans, and educating families on treatment options.
Key skills include exceptional interpersonal communication, as navigators must build trust with patients from various backgrounds. Strong problem-solving abilities are essential for untangling insurance issues or finding solutions to logistical challenges.
A deep understanding of the healthcare landscape, from clinical processes to billing, is also vital for success in this role.
How to Pursue This Career Path
To become a Patient Navigator and effectively guide patients through their healthcare journey, a focused approach to skill development is key.
- Develop Strong Empathy and Communication: Master active listening and culturally competent communication to advocate for diverse patient populations.
- Learn Health Systems and Insurance: Gain a thorough understanding of Medicare, Medicaid, and private insurance to help patients manage costs.
- Acquire Case Management Experience: Work or volunteer in social work or case management to develop skills in coordinating complex care.
- Obtain Certification: Pursue a Patient Navigator certification from an organization like the Harold P. Freeman Patient Navigation Institute to validate your expertise.
- Build a Community Resource Network: Proactively build relationships with local support organizations, from food banks to mental health clinics.
7. Medical Social Worker
The Medical Social Worker is one of the most vital non-profit healthcare jobs. These professionals provide essential psychosocial support, counseling, and case management to patients and families facing difficult health challenges.
A Medical Social Worker goes beyond physical symptoms to address the social determinants of health. This includes factors like housing, financial stability, and emotional well-being that impact quality of life.
They are crucial members of the care team, connecting patients with resources and coordinating smooth care transitions from hospital to home. Their work ensures that no patient falls through the cracks, providing a safety net of support and advocacy.
Core Responsibilities and Required Skills
A Medical Social Worker’s role is deeply person-centered, blending clinical skills with resource management and advocacy. Key responsibilities include conducting psychosocial assessments, providing crisis intervention, and developing comprehensive care plans.
These professionals must have a strong grasp of how social, emotional, and financial factors intersect with health. For instance, at CCVNA, our Medical Social Workers collaborate closely with our Registered Nurses and other clinicians.
This synergy is essential for successful recovery and is a cornerstone of our home health services. Learn more about our collaborative home healthcare nursing.
How to Pursue This Career Path
Becoming a Medical Social Worker in a non-profit setting requires a dedicated educational and professional journey.
- Obtain a Master of Social Work (MSW): An MSW degree with a specialization in healthcare is the standard educational requirement.
- Gain Supervised Clinical Experience: Seek internships or entry-level positions in medical settings like hospitals or clinics to build hands-on experience.
- Develop Population-Specific Expertise: Focus on a particular area, such as geriatrics or palliative care, to become an invaluable specialist.
- Pursue Clinical Licensure: Earning a Licensed Clinical Social Worker (LCSW) credential significantly enhances your professional standing.
Build Your Career with Central Coast VNA & Hospice
Choosing a career in the nonprofit sector is a commitment to serve and uplift your community. The roles we've explored illustrate the diverse opportunities available within mission-driven healthcare.
Each position offers a unique way to apply your skills toward a greater good. You can directly impact the well-being of individuals and families across the Central Coast.
These non-profit healthcare jobs are built on a foundation of compassion and purpose. The focus is on patient outcomes and community health, not shareholder returns. This environment fosters professional satisfaction and a powerful sense of connection to the people you help every day.
Working at an organization like Central Coast VNA & Hospice means joining a legacy of care. We have proudly served Monterey, San Benito, Santa Cruz, and South Santa Clara counties for over 74 years.
Key Takeaways for Your Career Search
As you consider your next steps, remember these core insights:
- Mission Drives Everything: Your work will directly contribute to providing essential care to those in need, including seniors, veterans, and underserved populations.
- Diverse Skill Sets Are Valued: Whether your expertise is in data analysis, community outreach, or clinical care, there is a vital role for you.
- Professional Growth and Personal Fulfillment: These careers offer a blend of challenging, meaningful work and the opportunity to grow with a dedicated team.
Taking the Next Step in Your Journey
Embarking on a career in nonprofit healthcare requires preparation and passion. As you refine your resume to highlight your commitment to community-focused work, prepare for the modern hiring process.
Many organizations now use virtual platforms to connect with candidates. Learn more about how to prepare for a video interview to ensure you present your best self.
Ultimately, a career in this field is an investment in both your future and your community’s health. It is a chance to build a legacy of compassion, one patient at a time. The demand for dedicated professionals in non-profit healthcare jobs continues to grow.
Frequently Asked Questions (FAQs)
1. What is the main difference between a non-profit and a for-profit healthcare job?
The primary difference is the organization's mission. Non-profits, like Central Coast VNA & Hospice, reinvest revenue into their patient care programs and community services rather than distributing profits to shareholders. This creates a work environment focused on patient outcomes and community well-being.
2. Do non-profit healthcare organizations offer competitive salaries and benefits?
Yes. To attract and retain qualified professionals, reputable non-profits offer competitive compensation packages. These often include comprehensive benefits, retirement plans, and opportunities for professional development, such as our employee wellness program.
3. What kind of non-clinical jobs are available in non-profit healthcare?
Beyond direct patient care roles like Registered Nurses and Hospice Aides, there are many essential non-clinical positions. These include Grant Writers, Community Health Worker Coordinators, Data Analysts, and administrative staff who support the organization’s mission.
4. How does working for a local non-profit like CCVNA benefit the community?
Working for a local, mission-driven provider ensures that care is tailored to the specific needs of the Central Coast community. With over 74 years of service in Monterey, San Benito, Santa Cruz, and South Santa Clara counties, our focus remains on providing compassionate, high-quality home health, palliative, and hospice care to our neighbors.
5. Are there opportunities for career advancement within non-profit healthcare?
Absolutely. Non-profit organizations value retaining dedicated staff and often provide clear pathways for professional growth. Employees can advance into leadership roles, specialize in areas like palliative or hospice care, or transition between different departments to broaden their skills.
Are you ready to build a career with purpose at a trusted, local nonprofit? Explore current openings and discover how you can make a difference with Central Coast VNA & Hospice. Join our team and help us continue our legacy of providing compassionate care.
Finding the Best Hospice Care Near Me: A Guide for the Central Coast
When a loved one faces a life-limiting illness, the search for the "best hospice care near me" becomes a critical and deeply personal journey. This decision is about more than just medical services. It's about finding an organization that provides dignity, comfort, and comprehensive support for both the patient and their family.
The right hospice partner understands the unique needs of your community and delivers care with unwavering compassion. For families across California’s Central Coast, including Monterey County, San Benito County, Santa Cruz County, and South Santa Clara County, this choice is paramount. The goal is to ensure your loved one's final chapter is lived with peace and respect, supported by a dedicated team.
This guide is designed to simplify your search by providing a clear comparison of top-rated hospice providers. We will evaluate each organization based on key differentiators, service highlights, and their unique approach to end-of-life care. This will help you make an informed decision during a profoundly challenging time.
1. VITAS Healthcare: The National Leader in Hospice Services
As a pioneer of the American hospice movement, VITAS Healthcare has established itself as the largest provider of end-of-life care in the United States. Since its founding in 1978, VITAS has built a national model centered on an interdisciplinary team approach. This ensures that every aspect of a patient's physical, emotional, and spiritual well-being is addressed.
Their comprehensive service offerings range from standard in-home medical support to specialized pediatric programs. They also have dedicated inpatient hospice units designed for acute symptom management. For families on the Central Coast seeking a provider with standardized protocols and a vast network, VITAS presents a well-established choice.
Why VITAS Stands Out
VITAS's primary strength lies in its scale and experience. Having served millions of patients, the organization has refined its care delivery processes to maintain consistent quality across numerous locations. This is particularly beneficial for patients with complex medical needs.
The corporate structure of VITAS ensures access to extensive resources, including advanced telehealth services and specialized care programs. This makes them a strong contender for patients with highly specific or acute end-of-life care requirements. However, some families may find a large, national organization feels less personal than a local provider with deep community roots.
These figures underscore their long-standing presence and significant operational capacity in the national hospice landscape. Many of their services, such as managing complex symptoms, align with the goals of palliative care; you can learn more about the benefits of palliative care to see how it complements the hospice philosophy.
Actionable Tips for Families
If you are considering VITAS, it is important to engage proactively to ensure a personalized experience.
- Ask About Specialized Programs: Inquire about their specific programs for conditions like cardiac disease, respiratory illness, or dementia.
- Meet Your Care Team: Request an introductory meeting with the Registered Nurse, Hospice Aide, and Social Worker assigned to your family.
- Confirm Local Response Times: Ask about the location of their nearest office and their standard response times for after-hours needs.
2. Hospice of the Valley: A Nonprofit Community Pillar
As Arizona's largest and one of its most respected nonprofit hospice organizations, Hospice of the Valley has been a community pillar since 1977. They have built their reputation on a deeply patient-centered approach. This ensures every individual's journey is met with dignity, comfort, and comprehensive support.
While primarily serving the Phoenix area, their model provides an excellent benchmark for families on the Central Coast evaluating what makes for the best hospice care near me. Their services extend beyond traditional in-home care, encompassing dedicated inpatient hospice homes and innovative programs tailored to unique patient needs.

Why Hospice of the Valley Stands Out
Hospice of the Valley’s primary strength is its nonprofit, mission-driven philosophy combined with its extensive scale. This unique combination allows them to reinvest resources into pioneering new programs, such as specialized dementia care and extensive grief support services. A nonprofit status often translates into a deeper community focus.
Their commitment to serving the community is evident in their wide array of supportive services, which are often provided regardless of a patient's ability to pay. For those exploring their options, understanding the breadth of services offered can be incredibly beneficial. You can discover more about their approach to hospice care to see how it aligns with your family's needs.
Actionable Tips for Families
If you are inspired by the Hospice of the Valley model, use these tips to find a provider with similar values:
- Inquire About Volunteer Programs: Ask how volunteers are integrated into care for additional family support and companionship.
- Ask About Pet Therapy: If pets are an important part of your family’s life, inquire if the agency offers pet therapy or has protocols to support animals in the home.
- Evaluate Grief Support: Look into the grief counseling services offered. Ask if they have specialized programs for children or unique support groups.
- Consider Inpatient Options: For potential crisis care needs, confirm if they operate their own inpatient facilities or have strong partnerships with local ones.
3. Seasons Hospice & Palliative Care
Seasons Hospice & Palliative Care is a nationally recognized provider known for its strong focus on integrating palliative and hospice services. Operating across multiple states, their model emphasizes early, comprehensive support for patients with serious illnesses. This dual approach makes them a significant choice for families looking for the best hospice care near me.
Their care philosophy is built on personalized plans and strong partnerships with local hospitals and referring physicians. Seasons has a proven track record of successfully transitioning patients from palliative to hospice care. By focusing on expert pain and symptom management protocols, they help maintain high patient satisfaction.
Why Seasons Stands Out
Seasons' key advantage is its expertise in the continuum between palliative care and hospice. Many families are not ready for a hospice diagnosis, and Seasons provides a valuable bridge with its robust palliative programs. This allows patients to receive specialized symptom management and support earlier in their illness.
Seasons excels at managing the often-complex transition from palliative support to end-of-life care. Their integrated teams are trained to guide families through this emotional and clinical shift. This makes them an excellent option for patients who may benefit from an extended period of supportive care before hospice becomes appropriate.
Actionable Tips for Families
When considering Seasons, focus on understanding how their dual-service model can benefit your specific circumstances.
- Discuss Palliative Options: If your loved one is not yet eligible or ready for hospice, ask specifically about their palliative care programs.
- Inquire About Transition Protocols: Ask how the team manages the shift from palliative to hospice care.
- Verify Local Team and Response Times: Confirm the location of their nearest Central Coast office and their typical response times for routine and urgent needs.
- Review Family Communication: Discuss their standard procedures for keeping family members informed, especially those who may live out of the area.
4. Compassus: A Personalized Approach with National Support
Compassus operates on a model that blends national resources with local, community-based care. As one of the largest hospice providers in the U.S., they strive to deliver a personalized experience that respects patient dignity. Their philosophy focuses on providing care that is close to home, managed by local teams who understand the community.
This structure allows them to offer a high degree of personalization while maintaining rigorous quality standards. For families looking for the best hospice care near me that combines reliability with individual focus, Compassus presents a compelling option. Their integration with major health systems ensures a high level of clinical excellence.

Why Compassus Stands Out
The key strength of Compassus is its "local-first" approach within a national framework. While they have extensive resources, care decisions are driven by local clinical teams who are familiar with the communities they serve. This can lead to a more personalized and responsive care experience.
Compassus emphasizes maintaining high quality scores through Medicare reporting and invests heavily in comprehensive staff training. Their model aims to give families the best of both worlds. This includes the assurance of a nationally recognized provider and the comfort of care from local professionals.
Actionable Tips for Families
When evaluating Compassus, focus on understanding their local team and care planning process to ensure it aligns with your family’s values.
- Ask About Local Staff Tenure: Inquire about the experience and longevity of the local Registered Nurses, Hospice Aides, and Social Workers to gauge team stability.
- Discuss Physician Collaboration: Ask how they will coordinate with your loved one's current doctors to create a seamless care plan.
- Request Quality Metrics: Ask for their specific quality and family satisfaction scores for the local branch.
- Explore Care Personalization: Discuss their process for developing a personalized care plan that reflects the patient’s unique wishes and goals.
5. Kindred Hospice: A Focus on Integrated Care
As a significant part of the Kindred Healthcare network, Kindred Hospice provides comprehensive end-of-life care services across the nation. Their model is built upon delivering comfort and enhancing the quality of life for patients. This connection offers a potential continuum of care that many families find reassuring.
Kindred’s services are designed to support both patients and their families through a difficult journey. By developing partnerships with local hospitals and medical communities on the Central Coast, they aim to facilitate smooth transitions. This helps patients move from curative treatment to compassionate hospice care at home or in a facility.
Why Kindred Stands Out
Kindred's main advantage is its connection to a broader healthcare ecosystem. For patients who may have already received care from other Kindred services, the transition to hospice can feel more seamless. This established relationship helps ensure continuity and a deeper understanding of the patient's medical history.
Kindred’s integration within a larger network allows for well-defined care protocols and effective coordination. Their structured approach is beneficial for families who value consistency and established processes. The organization's emphasis on pain management and symptom control is a cornerstone of their philosophy.
Actionable Tips for Families
If you are considering Kindred Hospice, taking these steps can help you make an informed decision.
- Discuss Care Transitions: Ask how they coordinate the transition from a hospital or another care facility to their hospice service.
- Inquire About Staffing: Request information about their local staff, including the medical director's involvement and standard after-hours response times.
- Understand Family Support: Inquire about the resources and support they provide for loved ones. These tips for family caregivers can offer additional valuable guidance.
6. Brookdale Hospice: Integrated Care for Senior Living Communities
Brookdale Hospice operates as a specialized branch of Brookdale Senior Living, one of the nation’s largest senior living providers. Their model is uniquely designed to deliver end-of-life care within assisted living, memory care, and independent living communities. This integration provides a seamless transition for residents who need hospice services.
For families seeking the best hospice care near me for a loved one already in a senior community, Brookdale offers a highly convenient option. Their services are built on a deep understanding of geriatric care. While their primary focus is on serving Brookdale residents, their hospice services are often available to the wider community.
Why Brookdale Stands Out
Brookdale's key advantage is its expertise in delivering hospice care within a senior living setting. Their clinical teams are adept at coordinating with facility staff, ensuring care plans are harmonized. This eliminates many logistical challenges families face when bringing an outside agency into a residential community.
The integrated nature of Brookdale Hospice means care is delivered by a team that understands the daily routines of a senior living environment. This can lead to a more comfortable and less disruptive experience for the patient. You can learn more about our continuum of care to see how different levels of support work together.
Actionable Tips for Families
If you are considering Brookdale Hospice, especially for a loved one in a senior living facility, here are some practical steps to take.
- Inquire About Geriatric Specialization: Ask about the specific training their Registered Nurses, Hospice Aides, and Social Workers have in geriatric and dementia care.
- Discuss Coordination with Facility Staff: Clarify how their hospice team will communicate and coordinate with the assisted living or memory care staff.
- Check Availability for Non-Residents: If your loved one does not live in a Brookdale community, confirm if they provide services in private homes in your area.
- Understand Family Involvement: Ask how they facilitate family participation and communication, particularly if you are managing care from a distance.
7. Central Coast VNA & Hospice: Your Local, Nonprofit Partner
For over 74 years, Central Coast VNA & Hospice (CCVNA) has been deeply embedded within the communities it serves. As the region's trusted nonprofit provider, CCVNA offers a uniquely personalized and community-centric approach to care. This makes them a premier choice for families looking for the best hospice care near me.
Their model is built on strong local connections and long-standing relationships with regional hospitals, physicians, and community resources. For families in Monterey County, San Benito County, Santa Cruz County, and South Santa Clara County, CCVNA offers the assurance of care from a team that understands the local landscape and is invested in the community's well-being. This local focus translates into highly responsive and adaptable care.
Why Central Coast VNA & Hospice Stands Out
The primary strength of CCVNA lies in its nonprofit, mission-driven philosophy and deep community integration. Unlike national for-profit chains, CCVNA reinvests its resources directly into patient care, staff training, and community-benefit programs. This structure fosters a culture of compassion and allows for a more personalized patient experience.
CCVNA also has robust and dedicated volunteer programs that enhance patient quality of life. These volunteers provide companionship, respite for family members, and specialized support, adding a layer of care that is a hallmark of a true community-based provider. To better understand the criteria for different levels of care, you can explore the eligibility requirements for home health and hospice to see how these services align.
Actionable Tips for Families
When considering Central Coast VNA & Hospice for your loved one, it is beneficial to explore its community-specific advantages.
- Research Their Local History: Ask about their 74+ year history in the area and their long-term community involvement.
- Inquire About Volunteer Support: Learn about their volunteer programs and how they integrate volunteers into the care team.
- Ask About Local Partnerships: Request information on their relationships with local hospitals, clinics, and other healthcare providers.
- Confirm Service Area: Ensure your location is well within their primary service areas of Monterey, San Benito, Santa Cruz, or South Santa Clara Counties.
Making the Right Choice for Your Family on the Central Coast
Choosing a hospice provider is a deeply personal decision, one that requires careful thought and a clear understanding of what matters most to your family. This guide has reviewed several well-known hospice organizations, but the search for the "best hospice care near me" often leads families back to one essential truth: local, community-focused care makes all the difference.
Navigating this journey with a provider that is woven into the fabric of the Central Coast means you receive more than just medical support. It means partnering with a team that understands the local healthcare landscape and community spirit of Monterey County, San Benito County, Santa Cruz County, and South Santa Clara County.
Key Takeaways for Your Hospice Search
As you reflect on the options, keep these critical factors at the forefront of your decision-making process:
- Nonprofit Mission vs. For-Profit Model: A nonprofit agency, like Central Coast VNA & Hospice, reinvests its resources directly into patient care and community programs. This mission-driven focus ensures patient well-being is the ultimate priority.
- A True Continuum of Care: A provider offering a seamless continuum from home health nursing to palliative care and finally to hospice ensures consistency and trust. This means a familiar team can support your family every step of the way.
- Deep Community Roots: An organization with a long-standing history, like CCVNA’s 74+ years of service, has built lasting relationships with local physicians and hospitals. This deep integration translates to better-coordinated, more responsive care.
- Comprehensive Support Services: Superior hospice care includes a holistic team of professionals: Registered Nurses for expert symptom management, Chaplains for spiritual support, Social Workers for emotional guidance, and dedicated Hospice Aides for personal care.
Actionable Next Steps for Your Family
Making the right choice starts with asking the right questions. Here is a practical checklist to guide your conversations with potential providers:
- Inquire About the Care Team: Ask specifically about the roles on their team. Who will be visiting the home? How often?
- Understand Their Service Area: Confirm they serve your specific town and ask about their staff's familiarity with local resources.
- Discuss After-Hours Support: How does the agency handle calls and visits on nights and weekends? Is a Registered Nurse available 24/7?
- Ask About Their Nonprofit Status: Inquire about their mission and how their organizational structure benefits patients and families.
Choosing hospice care is not about giving up; it is about embracing a philosophy of care that prioritizes comfort, dignity, and quality of life. By selecting a provider that aligns with your family’s values and has a proven legacy of compassionate, local service, you are making a powerful choice to ensure your loved one’s final chapter is lived with peace and respect.
Frequently Asked Questions (FAQs)
1. What is the difference between hospice and palliative care?
Palliative care can be provided at any stage of a serious illness, often alongside curative treatments, to manage symptoms and improve quality of life. Hospice care is a specific type of palliative care for individuals with a life expectancy of six months or less who are no longer seeking curative treatment.
2. Who is on the hospice care team at Central Coast VNA & Hospice?
Our team includes a Registered Nurse, Medical Social Worker, Hospice Aide, Chaplain, and trained volunteers. This interdisciplinary group works together under the supervision of our Medical Director to provide comprehensive physical, emotional, and spiritual support.
3. Does Central Coast VNA & Hospice provide care in facilities?
Yes, our compassionate hospice services can be provided wherever a patient calls home. This includes private residences, assisted living communities, and skilled nursing facilities throughout Monterey County, San Benito County, Santa Cruz County, and South Santa Clara County.
4. How is hospice care paid for?
Hospice care is covered by Medicare, Medi-Cal, the Veteran’s Administration (VA), and most private insurance plans. As a nonprofit organization, Central Coast VNA & Hospice is committed to providing care to all eligible patients, regardless of their ability to pay.
5. How do I know when it’s the right time to start hospice care?
It may be time to consider hospice when curative treatments are no longer effective or desired, and the focus shifts to comfort and quality of life. A conversation with your physician and a hospice provider like Central Coast VNA & Hospice can help determine if it is the right time for your family.
When searching for the best hospice care near you, turn to the trusted, nonprofit leader on the Central Coast. For over 74 years, Central Coast VNA & Hospice has provided unparalleled, compassionate care to local families. To learn how our dedicated team can support you, visit Central Coast VNA & Hospice or contact us today to start the conversation.
Top 7 Best Home Health Agency for Seniors in the Central Coast (2025)
Choosing a home health agency is one of the most important decisions a family can make. The right partner ensures your loved one receives skilled, compassionate, and reliable care in the comfort of their home, bringing peace of mind and enhancing their quality of life.
However, navigating the options on California's Central Coast can feel overwhelming. How do you identify the best home health agency for seniors that aligns with your family’s specific medical requirements and values? It is about finding a trusted team that becomes an extension of your support system.
This guide simplifies your search by comparing the top home health agencies serving Monterey, San Benito, Santa Cruz, and South Santa Clara Counties. We will explore what makes each organization unique, from their clinical expertise to their care philosophy. Our goal is to empower you with the clear, actionable information needed to make a confident choice for your loved one’s well-being.
1. Central Coast VNA & Hospice: A Legacy of Nonprofit, Comprehensive Care
For seniors and families on the Central Coast, navigating changing healthcare needs can be a significant source of stress. Central Coast VNA & Hospice (CCVNA) stands out as a definitive solution, earning its place as the top choice for its unparalleled, fully integrated continuum of care. For over 74 years, this mission-driven nonprofit has been a cornerstone of community health, offering a seamless transition between home health, palliative care, and hospice services.
This integrated model is what truly sets CCVNA apart as the best home health agency for seniors in the region. A patient recovering from surgery can start with home health nursing, transition to palliative care for ongoing symptom management, and later receive compassionate end-of-life support from the same familiar team. This continuity eliminates the disruption and anxiety of finding new providers, ensuring consistent, high-quality care.
Key Insight: CCVNA is the only organization on the Central Coast providing a full continuum of home health, palliative, and hospice care. This integrated approach ensures patients receive consistent, expert support from a single, trusted team as their healthcare needs change.
Why It Stands Out: The Integrated Care Advantage
CCVNA’s model is built on delivering whole-person care that addresses not just physical symptoms but also the emotional, social, and spiritual well-being of patients and their families. This is achieved through a dedicated, interdisciplinary team that collaborates on every care plan.
- Comprehensive Clinical Team: Care is delivered by a team of experts including Registered Nurses, Physical Therapists, Medical Social Workers, Chaplains, and Hospice Aides.
- Personalized Care Planning: Every patient receives a customized plan tailored to their unique medical needs, personal goals, and family dynamics.
- 24/7 Clinical Support: Patients and families have round-the-clock access to clinical support, providing peace of mind and immediate assistance when needed.
This holistic approach is especially beneficial for seniors managing complex or chronic conditions. The team works in concert, ensuring all aspects of the patient's well-being are addressed with compassion and professionalism.
Coverage Area and Accessibility
As a nonprofit, CCVNA is deeply committed to serving its community. Its services are available to all eligible residents across a wide swath of the Central Coast, including:
- Monterey County
- San Benito County
- Santa Cruz County
- South Santa Clara County
CCVNA accepts Medicare, Medi-Cal, and most private insurance plans, and its nonprofit status allows them to provide care to those in need. For families exploring options, a helpful first step can be to learn more about the benefits of palliative care on ccvna.com to understand this extra layer of support.
Website: https://ccvna.com
2. Amedisys Home Health Care
Amedisys is a national leader in home health, offering a robust framework of skilled medical care for seniors recovering from surgery or managing chronic conditions. With a strong emphasis on evidence-based practices, Amedisys aims to reduce hospital readmissions and improve patient outcomes. Its services are beneficial for older adults on the Central Coast who require specialized, in-home clinical support.
The Amedisys website is a comprehensive resource for patients and their families to understand available care options. This makes it one of the best home health agency for seniors looking for clear, actionable information. A guide to home health care services can provide further context on what to expect from these types of clinical programs.
Key Offerings and User Experience
Amedisys stands out for its structured, clinically focused approach to home health. It provides a level of specialized care that goes beyond basic assistance.
- Chronic Disease Management: Amedisys offers specialized programs for heart failure, COPD, and diabetes that include patient education and symptom management.
- Post-Surgical Recovery: The platform details its rehabilitation services, including physical, occupational, and speech therapy, helping patients regain independence.
- Technology Integration: They utilize remote patient monitoring to ensure continuous oversight and prompt intervention when a patient's condition changes.
Insurance and Availability
Amedisys accepts Medicare, Medicaid, veterans benefits, and many private insurance plans. Since it is a large national provider, service availability can vary by location. It is crucial for families on the Central Coast to confirm services in Monterey, San Benito, Santa Cruz, or Santa Clara counties.
Website: https://www.amedisys.com/
3. Visiting Angels
Visiting Angels is a well-established leader in non-medical home care, focusing on helping seniors maintain their independence and quality of life at home. Their services provide companionship, personal care, and respite support, making them an ideal choice for families on the Central Coast needing reliable, non-clinical assistance. The agency operates on a franchise model, ensuring a strong local presence.
The Visiting Angels website is straightforward and user-friendly, offering clear descriptions of their companion and personal care services. It is an excellent starting point for families exploring non-medical options. This type of assistance can be a lifeline; you can find more tips for family caregivers to help manage the journey.
Key Offerings and User Experience
Visiting Angels stands out for its highly personalized and flexible approach to care. Their commitment is to compassionate, one-on-one support.
- Personalized Care Plans: Each client receives a custom care plan tailored to their unique requirements, from light housekeeping to assistance with bathing and dressing.
- Flexible Scheduling: The agency offers adaptable scheduling options, including hourly, overnight, and 24/7 care, to fit the family's needs.
- Professional Matching: Families are involved in the process of selecting a compatible professional team member, ensuring a good fit based on personality and client preferences.
Insurance and Availability
While Visiting Angels is primarily private pay, many local franchises accept long-term care insurance and some government assistance programs. As they do not provide skilled medical services, traditional Medicare and Medicaid typically do not cover their care. Families in Monterey, San Benito, Santa Cruz, or Santa Clara counties should contact their local office directly to confirm offerings.
Website: https://www.visitingangels.com/
4. Home Instead
Home Instead is a globally recognized leader in non-medical in-home care, focusing on enhancing the quality of life for seniors. It has built a reputation for providing personalized, relationship-based support that allows older adults to age comfortably at home. Their approach is valuable for Central Coast families seeking reliable companionship and personal assistance.
The Home Instead website is a warm and inviting resource for families exploring care options. It clearly outlines the services available, from companionship to personal and memory care. This focus on non-medical, supportive services makes it one of the best home health agency for seniors who need help with daily living activities.
Key Offerings and User Experience
Home Instead excels at creating a supportive environment through carefully selected and trained staff who build genuine connections with clients. Their services are designed to address the holistic needs of seniors.
- Personalized Care Plans: Home Instead collaborates directly with seniors and their families to develop a customized care plan that fits the individual's needs and routine.
- Comprehensive Staff Training: Their professional staff receive extensive training, including specialized instruction for managing conditions like Alzheimer's and other dementias.
- Wide Range of Services: Offerings include personal care, companionship, meal preparation, medication reminders, light housekeeping, and transportation.
Insurance and Availability
While it is primarily a private-pay service, some locations may accept long-term care insurance, veterans benefits, and occasionally Medicaid waiver programs. It is essential for families on the Central Coast to contact their local branch. They should confirm availability and payment options in Monterey, Santa Cruz, or the surrounding areas.
Website: https://www.homeinstead.com/
5. Right at Home
Right at Home provides a flexible blend of non-medical and skilled nursing in-home care services designed to help seniors maintain independence. With an extensive network, it offers customized care plans that adapt to the evolving needs of older adults. This makes it a strong contender for the best home health agency for seniors who need a tailored approach.
The Right at Home website is user-friendly, allowing families to explore different levels of care. It clearly outlines its services, from basic companion care to complex dementia support and skilled nursing. Understanding the 5 essential benefits of hiring an outside agency can highlight the value of a professional service like Right at Home.
Key Offerings and User Experience
Right at Home excels by offering a spectrum of care that can be mixed and matched to create a truly personalized plan. This flexibility is a significant advantage for seniors.
- Customized Care Plans: The agency starts with a free in-home consultation to create a care plan tailored to the individual’s health, personality, and daily routines.
- Specialized Support: Right at Home provides targeted care programs for conditions like dementia and Alzheimer's, as well as post-operative assistance and skilled nursing.
- Professional Reliability: They use advanced tracking technology to ensure professional staff members are punctual and accountable, giving families peace of mind.
Insurance and Availability
Right at Home accepts various payment options, including long-term care insurance, veterans benefits, and private pay. While some locations may accept Medicare or Medicaid for skilled nursing services, this varies by franchise. Families on the Central Coast should connect with the local office serving Monterey, San Benito, Santa Cruz, or South Santa Clara counties to confirm service availability.
Website: https://www.rightathome.net/
6. BrightStar Care
BrightStar Care offers a unique, hybrid model of care, providing both non-medical and skilled nursing services under the supervision of a Registered Nurse. This integrated approach ensures that every client receives a personalized care plan tailored to their specific needs. For seniors on the Central Coast, this means access to a higher standard of care that adapts as their health needs evolve.
The BrightStar Care website is a clear and reassuring resource for families navigating care options. It communicates its commitment to clinical excellence, detailing its rigorous screening process and specialized programs. The platform's emphasis on nurse-led care makes it one of the best home health agency for seniors who need reliable, high-quality clinical oversight.
Key Offerings and User Experience
BrightStar Care distinguishes itself through its "A Higher Standard of Care" promise, which is backed by Joint Commission Accreditation. This clinical rigor is applied to both medical and non-medical services.
- Nurse-Supervised Care Plans: A Registered Nurse develops and oversees every client's plan of care, a feature not always standard with other agencies.
- Thorough Professional Screening: The platform highlights its stringent screening process, which includes background checks, drug screening, and verification of skills and licenses.
- Specialized Programs: BrightStar Care offers focused care for conditions like Alzheimer's and dementia, as well as dedicated support for post-hospital recovery.
Insurance and Availability
BrightStar Care accepts Medicare, Medicaid, and most long-term care insurance plans, as well as private pay. Since it operates as a franchise model, service availability can differ. Families on the Central Coast should connect with their nearest office in Monterey, Santa Cruz, or surrounding counties to confirm services and coverage.
Website: https://www.brightstarcare.com/
7. Enhabit Home Health & Hospice
Enhabit Home Health & Hospice operates as a dedicated provider of skilled medical care, bringing compassionate and clinically robust services directly to seniors' homes. With a strong presence across 34 states, Enhabit focuses on patient-centered outcomes. Its model integrates technology and personalized care plans to support independence.
The Enhabit website is a clear, user-friendly portal for patients and their families. It simplifies finding and understanding complex care options, offering detailed descriptions of skilled nursing, therapy, and hospice care. Families can learn more about what to expect from these types of Monterey senior care services to better prepare for in-home support.
Key Offerings and User Experience
Enhabit is recognized for its commitment to high-quality care and positive patient outcomes. Its services are structured to address specific medical needs with a compassionate approach.
- Comprehensive Clinical Services: Enhabit provides a full spectrum of skilled nursing, physical therapy, occupational therapy, and speech-language pathology.
- Specialized Care Programs: The agency offers targeted programs for chronic conditions like heart failure and COPD, as well as post-operative rehabilitation.
- Technology-Enhanced Care: By integrating modern technology, Enhabit ensures that clinical teams can respond quickly to a patient's changing health status.
Insurance and Availability
Enhabit accepts Medicare along with a wide range of other insurance plans. However, its availability is limited to the 34 states it serves. Families on the Central Coast should use the website’s location finder to confirm that services are available in Monterey, San Benito, Santa Cruz, or Santa Clara counties.
Website: https://www.ehab.com/
Making the Right Choice for Your Family on the Central Coast
Choosing the right in-home support for a loved one is a significant decision. This process requires careful thought, research, and an understanding of your family member’s specific medical needs and personal preferences. The Central Coast is home to a diverse array of providers, each with its own strengths.
As we have explored, national franchises like Amedisys and Enhabit offer structured, clinical programs. Agencies such as Visiting Angels, Home Instead, and Right at Home excel in providing essential non-medical and companion care. Meanwhile, providers like BrightStar Care stand out by ensuring nurse-led oversight for every client.
Actionable Steps for Selecting the Best Home Health Agency for Seniors
Making an informed choice involves more than just reading reviews. It requires a proactive, structured approach to ensure the agency you select is a perfect fit.
Here are the critical next steps to take:
- Assess Your Loved One's Needs: Create a detailed list of requirements. Does your loved one need skilled nursing, physical therapy, or assistance with daily activities like bathing and meal preparation?
- Verify Insurance and Coverage: Before scheduling consultations, contact your insurance provider to confirm which local agencies are in-network. This simple step can prevent unexpected out-of-pocket costs.
- Conduct Interviews: Prepare a list of questions for your top choices. Inquire about their staff screening process, training requirements, and how they handle emergencies.
- Check References: Do not hesitate to ask for references from current clients or healthcare professionals who have worked with the agency. Hearing firsthand experiences provides invaluable insight.
Why a Continuum of Care Matters
For families on the Central Coast, one factor stands above the rest: the ability to provide consistent, uninterrupted care as health needs change. This is where Central Coast VNA & Hospice offers a unique advantage. As the region’s only local, nonprofit provider offering a full continuum of home health, palliative care, and hospice, CCVNA ensures seamless transitions.
This integrated model means your loved one can move from home health nursing to palliative care, and eventually to hospice, all within the same trusted organization. This eliminates the stress of finding new providers and ensures the care team knows your family’s history. With over 74 years of mission-driven service to Monterey, San Benito, Santa Cruz, and South Santa Clara counties, CCVNA’s deep community roots provide unparalleled peace of mind.
Frequently Asked Questions (FAQs)
1. What is the main difference between home health care and non-medical home care?
Home health care provides skilled clinical services ordered by a physician, such as nursing care or physical therapy. Non-medical home care helps with daily activities like meal preparation, companionship, and personal hygiene but does not include medical services.
2. How does CCVNA’s continuum of care benefit patients?
CCVNA’s continuum of care allows patients to transition smoothly between home health, palliative, and hospice services without changing providers. This ensures consistent, coordinated care from a familiar team that understands the patient's history and goals.
3. What counties does Central Coast VNA & Hospice serve?
Central Coast VNA & Hospice proudly serves Monterey County, San Benito County, Santa Cruz County, and South Santa Clara County. As a local nonprofit, its mission is focused entirely on this community.
4. How is home health care typically paid for?
Skilled home health care is often covered by Medicare, Medi-Cal, and private insurance plans when deemed medically necessary by a doctor. Non-medical care is usually paid for privately or through long-term care insurance.
5. Why is being a nonprofit important for a home health agency?
As a mission-driven nonprofit, Central Coast VNA & Hospice prioritizes patient well-being over profits. Supported by community donations, it focuses on delivering compassionate, high-quality care to all eligible individuals, regardless of their ability to pay.
Ready to find a partner who can provide seamless, expert care through every stage of your loved one's health journey? Explore how Central Coast VNA & Hospice delivers an integrated continuum of home health, palliative, and hospice services right here on the Central Coast. Visit ccvna.com to learn more about our 74-year legacy of compassionate, nonprofit care.
Your Hospice After Death Checklist: Key Steps for Families
The moments following the death of a loved one in hospice care are tender and often overwhelming. While your hospice team provides immediate support, you are also faced with a series of necessary tasks. Having a clear plan can bring a sense of order during a disorienting time, allowing you to focus on grieving and honoring your loved one.
This hospice after death checklist is designed to guide you through the crucial steps with clarity and compassion. At Central Coast VNA & Hospice, we have supported families across Monterey County, San Benito County, Santa Cruz County, and South Santa Clara County through this process for over 74 years. Our experienced team, from Registered Nurses to Chaplains and Bereavement Specialists, is here to provide the continuity of care you need.
This guide breaks down the process into seven manageable steps, offering practical advice to help you navigate administrative, legal, and emotional responsibilities. It addresses everything from contacting the hospice team and securing documents to handling initial financial tasks and planning a memorial service.
By following this checklist, you can ensure that important obligations are met without feeling lost or overburdened. You will learn how to methodically manage each task, giving you the space to process your loss. Each step is an important part of a journey no one should walk alone.
1. Contact the Hospice Team and Physician
The very first action to take after a loved one passes away under hospice care is to contact their hospice provider. This step is a cornerstone of the entire hospice after death checklist because it initiates the formal process and ensures everything proceeds according to the established plan of care.
Unlike an unexpected death where calling 911 is the standard protocol, a hospice death is an anticipated event. The hospice team is prepared to guide you.
Why This Is Your First Call
Making the hospice team your first call ensures a peaceful and dignified transition. The team, including Registered Nurses and other dedicated staff, is trained to handle the moments after death with compassion and professionalism.
This prevents an unnecessary 911 call, which could trigger a full emergency response that is not required. The hospice Registered Nurse will coordinate the next steps, from the official pronouncement of death to contacting the pre-selected funeral home.
Practical Tips for Making the Call
To make this process as smooth as possible, follow these practical steps:
- Keep the Number Accessible: Post the hospice agency’s 24-hour hotline number in a visible place, such as on the refrigerator or near the patient's bedside.
- Designate a Caller: Decide in advance which family member will be the designated point of contact. This prevents confusion and ensures one person communicates with the medical team.
- Have Information Ready: When you call, have the patient's full name, date of birth, and address ready to provide to the on-call Registered Nurse.
- Ask About Timing: Inquire about the expected arrival time for the hospice Registered Nurse.
The following visual guide outlines the immediate notification process.
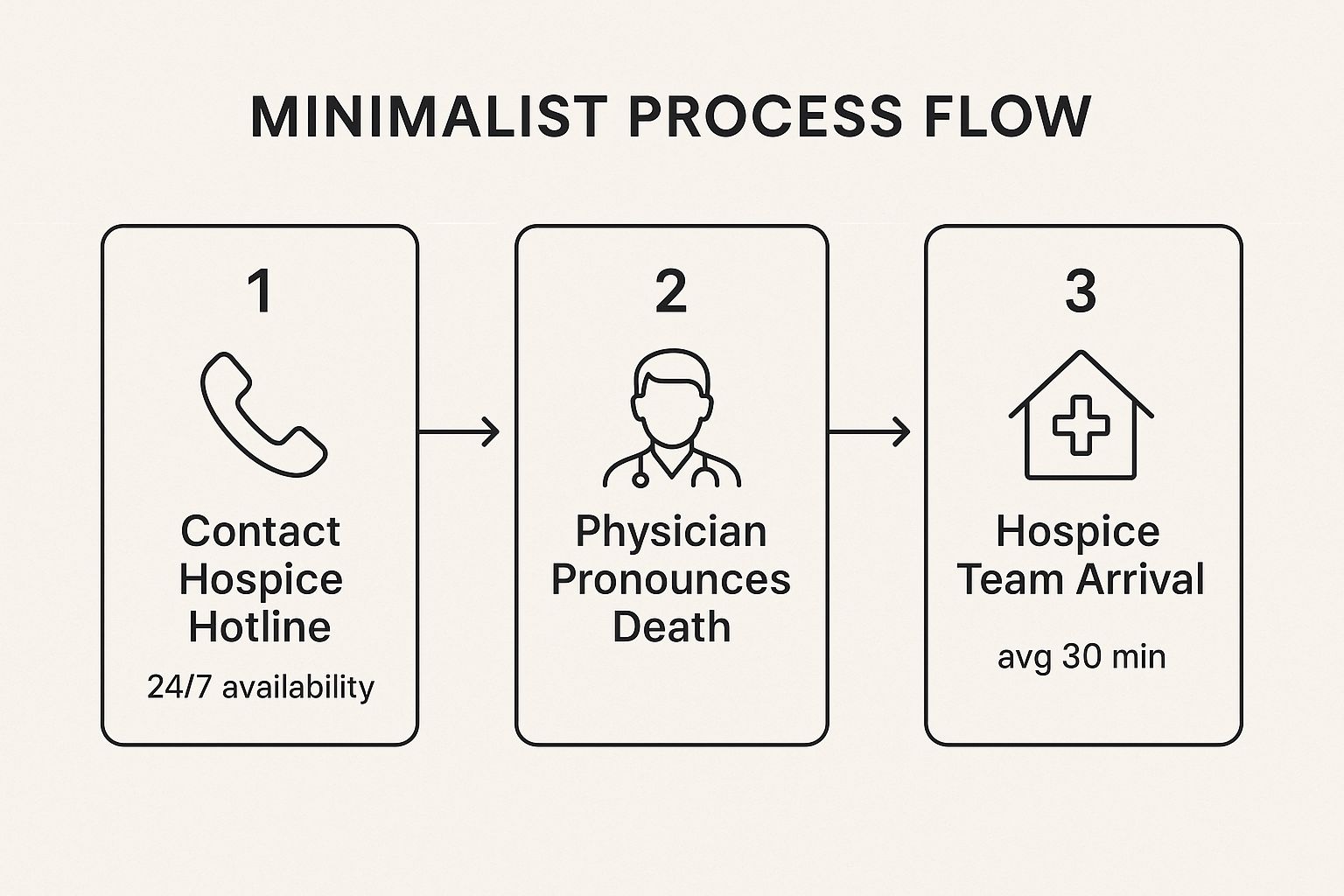
This simple flow illustrates that your first action directly leads to the official pronouncement and on-site support, bypassing emergency services entirely. For more information on creating a comprehensive care strategy, you can learn more about advance care planning.
2. Arrange for Body Preparation and Removal
After the hospice Registered Nurse has officially pronounced the death, the next critical step in the hospice after death checklist is arranging for the dignified preparation and transport of your loved one’s body. This process involves coordinating with a pre-selected or newly chosen funeral home or crematory service.
The hospice team remains a vital resource during this time, often assisting with the logistics to ensure a seamless and respectful transition. This step is deeply personal and can be emotionally challenging, but having a clear plan helps alleviate stress.

Why This Is Your Next Step
Coordinating body removal promptly but without rush ensures the process is handled with dignity and respect. The hospice Registered Nurse will typically assist in contacting the funeral home once the family is ready.
This managed approach prevents the feeling of being rushed. It provides a structured, compassionate transition from the home environment to the care of the funeral service provider.
Practical Tips for Arranging Transport
To navigate this sensitive task, consider these practical steps to ensure everything is handled respectfully and efficiently:
- Pre-Arrange When Possible: If funeral or cremation services were pre-arranged, locate the "pre-need" contract. This document contains all the necessary contact information and details.
- Discuss Final Wishes: Clearly communicate any specific cultural, religious, or personal wishes for body preparation with both the hospice Registered Nurse and the funeral home staff.
- Take Your Time: You do not need to have your loved one removed immediately. Take the time you need to say your final goodbyes in the comfort of the home setting before the transport team arrives.
- Gather Important Documents: Keep the deceased's personal identification, Social Security number, and any pre-arrangement paperwork in an accessible folder to provide to the funeral director.
- Designate a Support Person: Ask a close friend, family member, or your hospice Chaplain to be present when the transport team arrives. Their presence can provide emotional support.
3. Notify Close Family Members and Friends
Once the hospice team has been contacted, the next step on the hospice after death checklist is to begin notifying close family members and friends. This is a deeply personal and emotional task, requiring sensitivity and careful thought.
Handling these conversations with compassion ensures that loved ones receive the news in a supportive and respectful manner.

This process is more than just sharing information; it is the beginning of a collective grieving process. Having a plan can reduce the immense stress of deciding who to call and what to say in the raw moments after a loss.
Why This Is Your Next Step
Prioritizing close family and friends ensures your immediate support network is aware and can begin to process the loss alongside you. It prevents them from hearing the news through less personal means, like social media, which can be hurtful.
Hospice Medical Social Workers are often available to help families navigate these difficult conversations. Many families also create a "phone tree" or communication plan in advance to distribute the responsibility.
Practical Tips for Making the Calls
To handle this sensitive task effectively, consider these practical recommendations:
- Create a Contact List in Advance: During the hospice care period, compile a list of immediate family, extended family, and close friends with their phone numbers and relationships.
- Designate Callers: Assign specific people to notify certain groups. For instance, an adult child can call aunts and uncles, while a close friend can inform the social circle.
- Prepare Key Information: Write down a few simple sentences to share. This ensures the message is clear, consistent, and you don’t forget important details during an emotional call.
- Consider the Timing: Be mindful of time zones and the recipient’s circumstances. It is generally best to call, as a text message can feel impersonal for such significant news.
- Ask for Help: Lean on your support system. Ask a sibling, spouse, or close friend to sit with you or help make some of the calls.
Navigating the grief that follows is a long-term process. For those needing additional emotional support, Central Coast VNA & Hospice offers bereavement and grief support.
4. Secure and Organize Important Documents
After addressing the immediate medical and emotional needs, the next critical task is locating and organizing your loved one’s important documents. This step is a foundational part of the hospice after death checklist.
These papers are essential for handling legal, financial, and administrative responsibilities. Gathering everything in one central place will significantly streamline the estate settlement process.
Why This Is a Critical Step
Securing important documents early on prevents potential legal hurdles and financial complications. It empowers you to manage the estate confidently, making informed decisions based on the deceased's expressed wishes.
Many of these documents have time-sensitive requirements, so locating them quickly is crucial. For instance, a will must be filed with the probate court, and life insurance companies have specific claim deadlines.
Practical Tips for Organizing Documents
To manage this task effectively, consider the following practical steps:
- Create a Master Inventory: Start by creating a comprehensive list of all essential documents and their locations. This inventory will serve as your guide.
- Locate Key Legal Papers: Prioritize finding the will or trust, birth and death certificates, marriage certificates, and Social Security information.
- Gather Financial Records: Collect bank and investment account statements, tax returns from the last few years, credit card statements, and information on any outstanding loans or mortgages.
- Check for a Safe Deposit Box: Look for a safe deposit box key or related paperwork. You may need to check with the family's attorney or financial advisor for its location.
- Make Copies: Before distributing any original documents, make multiple copies for your records and for submission to various agencies.
- Secure Valuables: Store all original documents, keys, and other small valuables in a secure, fireproof location until the estate is settled. As you work to secure and organize important documents, especially those containing sensitive personal and financial information, considering how to maintain confidentiality during their transmission can be important, and some might find it useful to review confidential cover sheet templates.
Advance directives, which outline medical care preferences, are also a key part of this collection. To understand their role more deeply, you can discover more about the three common types of advance directives.
5. Contact Insurance Companies and Begin Claims Process
Initiating contact with insurance providers is a crucial financial step in any hospice after death checklist. This task involves locating the deceased’s life insurance policies and submitting the necessary paperwork in a timely manner.
Prompt action ensures that beneficiaries receive the funds intended to cover final expenses, outstanding debts, or provide long-term financial support.
Why This Is a Critical Financial Step
Filing life insurance claims promptly helps secure the financial stability of the surviving family members. The benefits from these policies are often essential for covering immediate costs like funeral services or medical bills.
Delaying this process can create unnecessary financial strain during an already difficult emotional period. It is a key step in settling the deceased's estate and honoring their financial planning.
Practical Tips for Managing Insurance Claims
To navigate the insurance claims process efficiently, consider the following practical steps:
- Locate All Policies: Search the deceased’s personal files, safe deposit box, and digital records for all life insurance policies, including individual, group, and employer-sponsored plans.
- Order Multiple Death Certificates: Most insurance companies require a certified copy of the death certificate, not a photocopy. Order 5-10 copies from the funeral home or vital records office.
- Gather Key Information: Before calling, collect the policy number, the deceased's full name, date of birth, Social Security number, and cause of death.
- Document Everything: Keep a detailed log of every conversation. Note the date, the representative’s name, the claim number, and a summary of the discussion.
- Understand Payout Options: Ask about the available payout options, such as a lump-sum payment or an annuity, and discuss any potential tax implications with a financial advisor.
6. Handle Immediate Financial and Legal Obligations
Once the initial logistical arrangements are underway, addressing immediate financial and legal tasks becomes a critical part of the hospice after death checklist. This step involves securing the deceased’s assets, managing urgent bills, and notifying key financial institutions.
Acting quickly can prevent financial complications, protect against identity theft, and ensure a smoother transition for managing the estate’s long-term affairs.
Why This Is a Priority
Promptly managing financial matters protects the estate from liability and loss. Neglecting these duties can lead to significant problems, including identity theft or financial penalties if important bills are missed.
This step lays the groundwork for the executor or administrator to fulfill their duties. It establishes an orderly process, whether that involves a formal probate process or a simpler distribution of assets.
Practical Tips for Managing Finances
To navigate these responsibilities effectively, consider the following practical steps:
- Contact Banks Immediately: Notify all banks and financial institutions where the deceased held accounts. Request that the accounts be frozen or retitled to "Estate of [Deceased's Name]."
- Notify Credit Bureaus: Contact the three major credit bureaus (Equifax, Experian, TransUnion) to report the death. This places a "deceased alert" on the credit file to help prevent identity theft.
- Maintain Essential Payments: Continue paying the mortgage, utilities, homeowner’s insurance, and car insurance to protect the assets. Review bank statements for automatic payments and cancel any non-essential subscriptions.
- Gather Important Documents: Locate the will, trust documents, bank statements, deeds, life insurance policies, and tax returns. These will be essential for the estate settlement process.
- Consult an Attorney: If the estate is complex, involves significant assets, or if a will is contested, it is wise to consult with an estate or probate attorney.
Properly managing these initial financial steps is a foundational part of the estate administration process.
7. Begin Funeral or Memorial Service Planning
After addressing the immediate logistical and legal steps, the focus naturally shifts toward honoring your loved one. Planning a funeral or memorial service is a crucial part of this hospice after death checklist.
It provides a structured way for family and friends to grieve, share memories, and celebrate the life that was lived. This process involves numerous decisions, from the type of service to coordinating with a funeral home.
Why This Planning Is Essential
Organizing a memorial service provides a focal point for grief and remembrance. It helps formalize the passing and allows the community to pay their respects, which can be an important part of the healing process.
By carefully planning the event, you ensure it aligns with your loved one’s character. This provides a comforting experience for attendees, rather than adding stress during an already difficult time.
Practical Tips for Service Planning
To navigate the planning process effectively, consider these actionable steps:
- Review Pre-Arrangements: The first step is to locate and review any pre-planned funeral arrangements, wills, or written instructions your loved one may have left. This honors their wishes.
- Hold a Family Meeting: Gather key family members to discuss preferences, roles, and the budget. This ensures everyone feels involved and that financial constraints are respected.
- Delegate Responsibilities: You do not have to do everything yourself. Assign specific tasks, such as coordinating flowers or creating a slideshow, to willing family and friends.
- Plan for Guests: If friends or family will be traveling, provide them with information on local accommodations and transportation to ease their journey.
- Preserve Cherished Memories: As part of memorial planning, you might also consider preserving cherished memories by organizing and digitizing family photographs. Explore tips for preserving old photos effectively.
This stage is about creating a tribute that feels authentic and provides closure. To learn more about how compassionate support extends through every stage of end-of-life care, you can explore hospice care in Monterey County.
Compassionate Support for Every Step of the Journey
Navigating the days after a loved one passes is a journey no one should walk alone. This hospice after death checklist was designed to serve as a steady guide, breaking down tasks into manageable steps.
From the initial calls to the hospice team and family, to handling financial accounts and legal documents, each item is a critical piece of the puzzle. By addressing these responsibilities methodically, you create the space necessary to focus on what truly matters: grieving and healing.
Key Takeaways for Your Path Forward
As you move through this process, keep these core principles in mind. They are the emotional anchors that will support you through the practical demands.
- Lean on Your Support System: The hospice team’s role does not end at the moment of passing. Your Registered Nurse, Medical Social Worker, and Chaplain are invaluable resources.
- Organization is a Form of Self-Care: Gathering documents and making lists is a powerful tool that reduces stress and gives you a sense of control during a period that can feel anything but.
- Pace Yourself and Delegate: You do not have to do everything at once, nor do you have to do it all by yourself. Prioritize tasks and accept help from trusted relatives and friends.
Finding Meaning Amidst the Practicalities
While this checklist focuses heavily on the logistical side of loss, it is equally important to create space for remembrance and healing. These practical steps are a means to an end, freeing you to engage in the deeply personal work of grieving.
Finding ways to keep your loved one’s memory alive can take many forms. Some find solace in tangible keepsakes that serve as a constant, gentle reminder of their bond, such as personalized memorial jewelry.
As a nonprofit, mission-driven organization, Central Coast VNA & Hospice is committed to continuing our care long after a patient’s passing. Our bereavement services, which include support groups and individual counseling, are available to families for up to 13 months. According to the National Hospice and Palliative Care Organization (NHPCO), providing such bereavement support is a cornerstone of quality hospice care.
We understand that grieving is not a linear process, and our team of Medical Social Workers, Chaplains, and Bereavement Specialists is here to help you navigate it. If you are in Monterey County, San Benito County, Santa Cruz County, or South Santa Clara County and need guidance, please reach out. Let our 74+ years of compassionate care support you.
Frequently Asked Questions (FAQs)
1. What is the very first thing I should do when a loved one dies in hospice at home?
Your first call should be to the hospice agency's 24/7 on-call number, not 911. A hospice Registered Nurse will come to pronounce the death, provide support, and coordinate the next steps according to your loved one’s plan of care.
2. How long do I have before the funeral home needs to be called?
There is no immediate rush. The hospice team will wait until you and your family have had time to say your final goodbyes. The hospice Registered Nurse can help you contact the funeral home when you are ready.
3. Who at Central Coast VNA & Hospice can help me with the emotional stress?
CCVNA provides comprehensive bereavement support through our Medical Social Workers, Chaplains, and trained Bereavement Specialists. These services are available to families for up to 13 months after a loss and are a key part of our mission-driven care.
4. How many copies of the death certificate will I need?
It is generally recommended to order 5 to 10 certified copies. You will need them for life insurance claims, closing bank accounts, transferring titles, and notifying government agencies like the Social Security Administration.
5. How does Central Coast VNA & Hospice support families in the community?
As a local nonprofit with over 74 years of service, CCVNA provides a continuum of care that includes home health, palliative care, and hospice. We serve families across Monterey, San Benito, Santa Cruz, and South Santa Clara counties with a focus on compassionate, professional, and mission-driven healthcare.
At VNA and Hospice, we believe that compassionate care extends beyond a patient’s life to support the entire family through their grieving process. If you or someone you know in Monterey, San Benito, Santa Cruz, or South Santa Clara County needs guidance after a loss, our bereavement services are here for you. Contact us today to learn more about how our 74+ years of nonprofit service can support your family.
How Is Hospice Care Funded? A Compassionate Guide for Families
When you and your family are navigating end-of-life decisions, the cost of care should be the last thing on your minds. A question we often hear is: how is hospice care funded? The answer is that care is typically paid for by several sources, but for most individuals, the Medicare Hospice Benefit covers nearly all costs.
This comprehensive support ensures families can focus on what truly matters—comfort, dignity, and quality time together.
Understanding How Hospice Care Is Paid For
Hospice is not a physical place; it is a philosophy of care that prioritizes comfort and quality of life for individuals with a life-limiting illness. As a nonprofit provider with over 74 years of local service, Central Coast VNA & Hospice believes everyone in our community deserves this compassionate support.
Understanding how this specialized care is paid for can provide tremendous peace of mind. This guide will walk you through the funding process, step by step, so you can feel confident that comprehensive care is available for your family in Monterey County, San Benito County, Santa Cruz County, and South Santa Clara County.
Primary Funding Sources
Most hospice care in the United States is supported by a few key sources. This infographic gives a clear picture of the primary payers for hospice services.
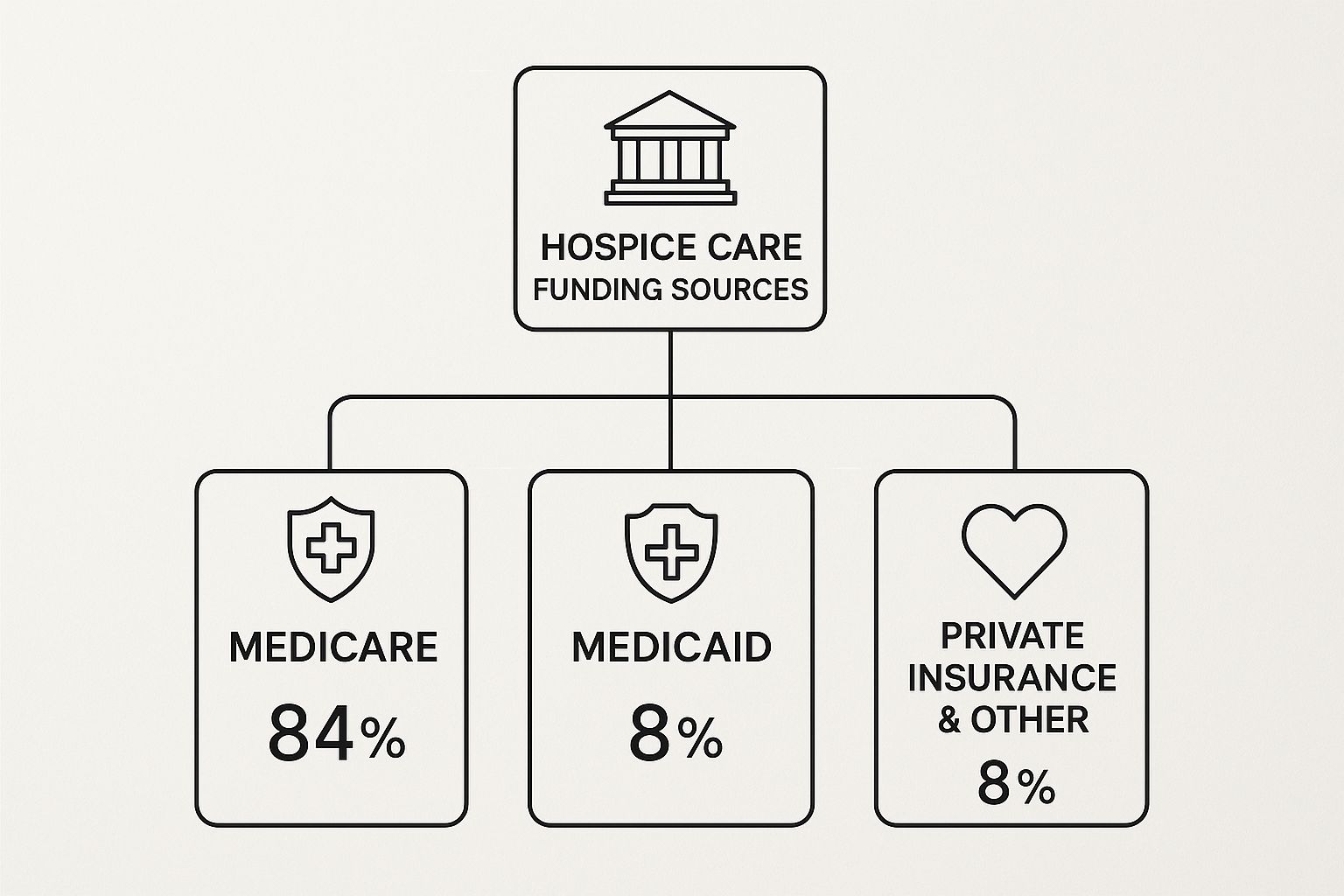
As you can see, Medicare is the largest payer for hospice services. This reflects a national commitment to supporting individuals and their families through the end-of-life journey.
To help you quickly see which options might apply to your family, here is a simple breakdown of the main funding sources.
Primary Hospice Funding Sources at a Glance
| Funding Source | Who It Covers | Primary Payer |
|---|---|---|
| Medicare Hospice Benefit | Individuals 65+ or those with qualifying disabilities | Federal Government |
| Medi-Cal / Medicaid | Low-income individuals and families | State/Federal Government |
| Private Insurance | Individuals with employer-sponsored or private health plans | Insurance Companies |
| Community Support & Grants | Uninsured or underinsured patients | Nonprofit Organizations |
| Out-of-Pocket | Individuals who do not qualify for other sources or prefer to pay directly | The Patient or Family |
This table provides a high-level overview. Let's explore the details of each so you can feel fully informed about your options.
Globally, the need for hospice is growing, with the market projected to reach $5.33 billion in 2025. This reflects a worldwide shift toward recognizing hospice as essential for managing chronic illnesses and supporting aging populations.
Beyond government programs and insurance, nonprofit hospices like Central Coast VNA & Hospice depend on community generosity to bridge care gaps. For those curious about how this works in the wider medical world, this is a complete guide to healthcare grants.
Exploring the Medicare Hospice Benefit

For most American families, the conversation about how hospice care is funded begins with the Medicare Hospice Benefit. This program is the bedrock of end-of-life care in our country, designed with a powerful goal: to lift the financial burden so patients and families can focus on comfort and quality of life.
The purpose of this benefit is to cover everything related to a person’s terminal diagnosis. This marks a shift away from treatments aimed at a cure and toward managing symptoms and providing whole-person support. For over 74 years, our team at Central Coast VNA & Hospice has guided countless families through this process.
Who Is Eligible for the Medicare Benefit?
Eligibility for the Medicare Hospice Benefit is refreshingly straightforward. It is designed to ensure people who need this specialized care can access it without navigating complex requirements.
To qualify, a person must meet a few conditions:
- Be enrolled in Medicare Part A (the part that covers hospital stays).
- Have two physicians certify a terminal illness. This means their physician and the hospice medical director agree that, if the illness runs its natural course, life expectancy is six months or less.
- Formally choose comfort care over curative treatment by signing an election statement.
It is important to understand that choosing hospice is not "giving up." It is an empowered decision to prioritize dignity and comfort, putting the goals of what is advance care planning into action.
What Comprehensive Services Are Covered?
The Medicare Hospice Benefit is truly all-inclusive for the terminal diagnosis. It covers a wide range of services to meet a patient’s physical, emotional, and spiritual needs, all delivered by a dedicated, interdisciplinary team.
This benefit is about more than just medical care; it’s about wrapping a complete system of support around the patient and their family. The goal is to manage symptoms, reduce stress, and allow for meaningful moments during a difficult time.
Here’s a look at what’s included:
- Expert Clinical Team: All visits from the hospice team are covered, including a Registered Nurse, Hospice Aide, Medical Social Worker, and Chaplain.
- Medical Equipment and Supplies: Any equipment needed for safe and comfortable care at home is included, such as a hospital bed, oxygen, walker, or wound care supplies.
- Medications: Prescription drugs for pain relief and symptom management related to the terminal illness are fully covered.
According to the National Hospice and Palliative Care Organization (NHPCO), over 1.72 million Medicare beneficiaries received hospice services in 2020 (NHPCO, 2021). This reliable funding ensures that organizations like Central Coast VNA & Hospice can provide exceptional care without passing the cost on to those we serve in Monterey and Santa Cruz counties.
How Are Medi-Cal and Private Insurance Used for Hospice?

While the Medicare Hospice Benefit is the most common path for funding, it is not the only one. Other vital resources are available, including Medi-Cal and private health insurance plans.
At Central Coast VNA & Hospice, our nonprofit mission is to ensure everyone in our community can access compassionate end-of-life care. We have decades of experience guiding families in San Benito County and South Santa Clara County through these different payment options.
Understanding the Medi-Cal Hospice Benefit
For many Californians, Medi-Cal (the state's Medicaid program) acts as an essential safety net. The Medi-Cal hospice benefit mirrors the comprehensive coverage offered by Medicare, ensuring people who qualify based on income can receive the same high-quality hospice care.
This benefit is designed to support both the patient and their family with a wide range of services, including:
- An Interdisciplinary Team: This core group includes care from a Registered Nurse, a Hospice Aide, a Medical Social Worker, and a Chaplain.
- All Medical Necessities: All medical equipment, supplies, and medications related to the terminal illness are fully covered.
- 24/7 On-Call Support: Patients and families have around-the-clock access to clinical support.
This ensures a person's income never stands in the way of receiving compassionate care. Our team helps families verify Medi-Cal eligibility and coordinates all details to make the process as smooth as possible.
Navigating Private Health Insurance
Most private health insurance plans offered through an employer or the marketplace include hospice coverage. However, the specifics can vary significantly from one provider to another.
While most private plans cover hospice, the details are in the fine print. Understanding your specific policy—including deductibles, copayments, and any pre-authorization rules—is key to avoiding surprises.
It is important to contact your insurance company to get a clear picture of your hospice benefits. The experienced team at Central Coast VNA & Hospice can help with this process. We regularly work with insurance companies to verify benefits and manage the necessary paperwork, allowing your family to focus on what matters most.
How Community Support Funds Nonprofit Hospice

While insurance programs create the foundation for how hospice care is funded, they don't tell the whole story. What sets a nonprofit hospice apart is its mission, driven by community care rather than profit margins. This is where philanthropy plays an essential role.
For organizations like Central Coast VNA & Hospice, our nonprofit status is a promise to our community. It means we are committed to providing care to everyone who needs it, regardless of their ability to pay. This has been our guiding principle for over 74 years of service on the Central Coast.
Bridging the Financial Gap
Generous donations, grants, and local fundraising are the lifeline that allows us to fulfill this promise. These funds bridge the financial gap when a patient's insurance is not enough or when they are uninsured altogether.
This community-funded model allows us to go beyond what standard insurance reimbursements cover. Sound nonprofit financial management is key to ensuring we can deliver on our mission for years to come.
Funding Care Beyond the Basics
The generosity of our community allows us to offer programs that enhance a patient's quality of life in profound ways. These services often fall outside the scope of what traditional insurance will pay for, but they are central to our philosophy of compassionate care.
A nonprofit’s mission is to serve the community’s needs first. Donations directly translate into more comprehensive support, allowing us to care for the entire family and honor each patient's unique wishes with dignity and respect.
This support allows us to provide:
- Specialized Grief Support: We offer bereavement services to families for up to 13 months after a loved one’s passing.
- Enhanced Therapies: Community funds can support services like music or art therapy that bring comfort and joy.
- Volunteer Programs: Donations support the extensive training and coordination of our dedicated volunteers, who provide priceless companionship and respite for families.
This deep connection reinforces our local roots in Monterey County and beyond, showing how neighbors can support neighbors. To better understand the different types of care available, you can explore our detailed comparison of palliative vs hospice.
What Services Hospice Funding Typically Covers
When a family begins hospice, understanding what is covered provides tremendous peace of mind. Whether funded by Medicare, Medi-Cal, or private insurance, the hospice benefit is designed to be all-inclusive for the terminal illness.
The goal is to create a complete support system that addresses a patient's physical, emotional, and spiritual well-being. This approach allows patients to remain comfortably and safely in the place they call home.
The Interdisciplinary Care Team
At the core of hospice is a dedicated team of professionals who work together to create a personalized care plan. This team effort ensures every need is met with expertise and compassion.
The core members of this team include:
- Registered Nurse (RN): The RN is the main point of contact, managing medical care with a focus on pain and symptom control.
- Hospice Aide: Aides provide hands-on personal care, such as assistance with bathing and dressing, with a constant focus on comfort and dignity.
- Medical Social Worker: The social worker provides emotional support and helps families navigate practical challenges, from financial questions to community resources.
- Chaplain: A chaplain offers non-denominational spiritual support that honors the patient's and family's beliefs.
- Trained Volunteers: These dedicated individuals offer companionship for the patient and provide respite for family members.
Medical Equipment, Supplies, and Medications
Beyond the care team, the hospice benefit also covers all physical items needed to keep a patient comfortable at home. For any item related to the terminal diagnosis, there should be no out-of-pocket costs.
This comprehensive coverage is a cornerstone of how hospice care is funded. The aim is to remove any financial barriers to receiving necessary medical equipment, supplies, or medications for symptom management.
This includes:
- Durable Medical Equipment (DME): This covers items like a hospital bed, oxygen concentrator, walker, or wheelchair, delivered directly to the home.
- Medical Supplies: All necessary day-to-day supplies are provided, such as bandages, catheters, or skin care products.
- Medications: All prescriptions for pain relief and managing symptoms related to the hospice diagnosis are fully covered.
Research shows a significant emphasis on nursing services within hospice, highlighting the demand for skilled, professional care at home. You can read the full research about hospice services to see more on this trend.
Sometimes, a patient's condition may stabilize. In those cases, it is helpful to learn more by understanding long-term hospice and how care can adapt.
Taking the First Steps to Arrange Hospice Care
If you and your family are considering hospice, getting started is often the most important part of the journey. The process is designed to be supportive and straightforward.
First, talk with your loved one’s doctor. A physician’s referral is the first step to confirm that hospice care is medically appropriate and is a crucial requirement for how hospice care is funded. You can review the specific hospice care eligibility guidelines to learn more.
Contacting Central Coast VNA & Hospice
Once you have a referral, or even if you are just exploring your options, the next step is to reach out to us. Our team at Central Coast VNA & Hospice offers a no-obligation consultation for families throughout Monterey County, San Benito County, and our other service areas.
We believe every family deserves clear, honest guidance. Our dedicated team is here to walk you through every step—from verifying insurance benefits to creating a personalized plan of care that honors your loved one’s wishes.
As your partners in care, we are here to help you make sense of insurance coverage, answer all your questions, and lift some of the weight from your shoulders.
Ready to learn more? Contact us today to start the conversation. Our team is ready to provide the compassionate support your family deserves.
Frequently Asked Questions About Hospice Funding
Navigating hospice care can bring up many questions for families. We have gathered some of the most common ones to provide clear, compassionate answers.
1. Is hospice care only for the last few days of life?
This is a common myth. A patient is eligible for the Medicare Hospice Benefit when a physician certifies a life expectancy of six months or less, if the illness runs its natural course. Starting care sooner allows patients and families to receive the full benefit of support, which dramatically improves quality of life.
2. Does choosing hospice mean we are giving up hope?
Choosing hospice is not about giving up; it is about shifting what you hope for. The focus turns toward living the rest of life as fully and comfortably as possible. Hope becomes about quality of life, peaceful days, and meaningful moments with family.
3. Will we have to pay anything for hospice care?
For most patients covered by the Medicare Hospice Benefit, there are no out-of-pocket costs for care related to the terminal illness. In rare cases, a small copayment of around $5 might apply for certain prescriptions. As a nonprofit, Central Coast VNA & Hospice is committed to caring for everyone in our community, regardless of ability to pay.
4. Can a patient receive hospice care in a nursing home?
Yes. Hospice care follows the patient wherever they call home, including a private residence, an assisted living community, or a nursing home. The hospice benefit covers all services provided by our team, while room and board at a facility is a separate expense.
5. What if a patient's health improves on hospice?
It happens! Sometimes, with focused comfort care, a patient’s condition stabilizes. If they no longer meet the six-month life expectancy criteria, they can be discharged from hospice and are free to return to curative treatments. They can re-enroll in hospice later if their health declines again.
The team at Central Coast VNA & Hospice is here to answer any other questions you may have about hospice care, eligibility, or the funding process. Contact us today to learn how we can support your family with compassionate, expert care.
Hospice Pain Management: A Compassionate Guide
When a loved one is nearing the end of their life, their comfort becomes the single most important thing. This is the heart of hospice pain management.
It’s a specialized philosophy of care that shifts the focus away from curing a disease and toward providing a compassionate shield from distress. The goal is simple: to allow them to spend their remaining time with dignity, surrounded by family, and as free from pain as possible. Hospice pain management is about treating the whole person, not just the illness.
Understanding Compassionate Pain Management in Hospice
At Central Coast VNA & Hospice, our approach is built on more than 74 years of local, nonprofit service. We know firsthand that pain isn’t just a physical sensation.
It's a complex experience that can deeply affect a person’s spirit, emotions, and relationships. Because of this, our mission as a mission-driven healthcare provider is to address every part of a person's well-being.
The core philosophy is simple: every person deserves to live their final chapter with grace and comfort. Our job is to make that a reality for families in Monterey County, San Benito County, Santa Cruz County, and South Santa Clara County.
A Focus on Quality of Life
The primary goal of hospice isn't to extend life, but to maximize the quality of the life that remains. This means we build a care plan centered entirely around the patient's personal wishes and goals.
For one person, that might mean being alert and present enough to share stories with grandchildren. For another, it could simply be resting peacefully and without anxiety in the familiar comfort of their own home.
Effective pain relief is a fundamental human need. According to the World Health Organization (WHO), an estimated 56.8 million people, including 25.7 million in their last year of life, need palliative care each year (WHO, 2020). This global reality underscores just how critical dedicated hospice services are.
It's also important to know that while both palliative care and hospice care focus on comfort, they serve different needs. We've put together a guide that walks you through the key differences between palliative and hospice care to help you make informed decisions.
Before we go deeper, it helps to understand the foundational principles that guide our work. This isn't just a checklist; it's a commitment to ensuring every patient feels seen, heard, and cared for with the utmost respect.
Core Principles of Hospice Pain Management
| Principle | Description |
|---|---|
| Patient-Centered Care | The patient's personal goals, values, and preferences are the driving force behind all decisions. |
| Holistic Approach | Pain is treated as a multidimensional experience, addressing physical, emotional, social, and spiritual needs. |
| Proactive Management | We anticipate and treat pain before it becomes severe, rather than just reacting to it. |
| Continuous Assessment | Pain is regularly monitored and the care plan is adjusted in real-time to ensure ongoing comfort. |
| Interdisciplinary Teamwork | A team of experts collaborates to provide comprehensive, layered support for the patient and their family. |
These principles aren't just words on a page—they are the pillars of the compassionate care we provide every single day. They ensure that our focus remains squarely on the patient's comfort and dignity.
Building a Personalized Comfort Plan
There is no one-size-fits-all solution in hospice. Every person’s journey with their illness is unique, and so is their experience of pain.
That’s why our dedicated teams work side-by-side with patients and their families to craft a comfort plan that is as individual as they are. This plan always involves:
- Listening Carefully: We start by truly hearing the patient. We want to understand their specific symptoms, their fears, and most importantly, their wishes.
- Continuous Assessment: Pain isn't static; it can change from day to day, or even hour to hour. Our Registered Nurses continually monitor comfort levels and adjust the care plan as needed.
- A Team Approach: We bring together a compassionate team of experts—including a physician, Registered Nurse, and Hospice Aide—to provide layered, comprehensive support.
For families across the Central Coast, from Santa Cruz County to South Santa Clara County, our promise is to deliver expert, compassionate care when it matters most. By focusing on total comfort, we help ensure your loved one's final days are defined by peace, not by pain. Contact us today to learn how our team can support your family through this journey.
Your Expert Hospice Care Team

Effective hospice pain management isn't a one-person job. It takes a dedicated group of professionals working in harmony, each bringing their unique skills to the table. This creates a complete, layered system of support for both the patient and their family.
Think of it as a specialized support system where every single member plays a crucial part in ensuring total comfort. This team approach is the bedrock of our philosophy at Central Coast VNA & Hospice, something we've been refining for over 74 years.
It’s our way of making sure no aspect of a person’s well-being is overlooked—from physical symptoms to their emotional and spiritual needs. When you choose our services, you aren’t just getting a provider; you’re gaining an entire team of compassionate experts.
The Core Members of Your Care Team
Each professional on your hospice team has a specific focus, but they all communicate constantly. They share insights and adjust their approach together to meet your loved one’s changing needs.
This tight-knit coordination is what provides consistent and reliable comfort right at home. Here’s who is on your side:
- The Registered Nurse (RN): The RN is usually the team coordinator. They are true experts in assessing pain and other symptoms, managing medications, and, just as importantly, teaching the family how to provide day-to-day care.
- The Hospice Aide: These are the compassionate professionals who provide gentle, hands-on personal care. Their work, like helping with bathing and dressing, is absolutely essential for maintaining comfort and dignity.
- The Medical Social Worker: A serious illness brings more than just physical challenges. The Medical Social Worker is there to provide emotional support and help families navigate practical stressors, like financial concerns or finding community resources.
- The Chaplain: For many people, spiritual comfort is a vital part of finding peace. Our chaplains offer non-denominational spiritual support that respects every family's unique beliefs and traditions, helping address deep questions of meaning and legacy.
This team works together seamlessly to wrap your loved one in a blanket of comprehensive care.
How Your Team Works Together
What does this collaboration look like in practice? Imagine the Registered Nurse notices that a patient seems more restless than yesterday.
The RN immediately shares this observation with the team. The Hospice Aide might then suggest a new, more comfortable position in bed, while the Medical Social Worker could check in with the family to see if any new emotional stressors are contributing.
This constant, fluid communication ensures the care plan is always responsive. To keep everyone connected securely, your hospice team uses HIPAA-compliant video conferencing platforms for virtual consultations, protecting your loved one’s sensitive health information.
At Central Coast VNA & Hospice, our interdisciplinary team meets regularly to discuss every single patient. This ensures everyone is aligned on the care goals, creating a unified and powerful support network for families across Monterey, San Benito, Santa Cruz, and South Santa Clara counties.
This collaborative spirit means you always have multiple advocates working on your family’s behalf. To learn more about how our teams provide comfort and dignity, you can explore our detailed guide to Central Coast VNA & Hospice care.
How We Understand and Measure Pain

You can't manage pain effectively if you don't first understand what a person is truly feeling. This isn't about running through a simple checklist.
It's an ongoing, compassionate conversation between our team, the patient, and their family. At Central Coast VNA & Hospice, we believe every expression of discomfort—spoken or unspoken—deserves to be heard, validated, and addressed.
Our entire approach is built on continuous assessment. Pain isn't a static condition; it can shift in intensity, location, and nature. Our Registered Nurses and Hospice Aides are constantly observing, listening, and asking questions to stay ahead of it.
The Art and Science of Pain Assessment
Measuring something as subjective as pain takes a blend of proven clinical tools and deep empathy. We tailor our methods to each individual.
This ensures we can get an accurate picture of their comfort level, whether they can speak for themselves or not. Our assessment methods include:
- Verbal Pain Scales: For patients who can communicate, we often use a simple 0-10 scale. Zero means no pain, and 10 represents the worst pain imaginable. This gives us a clear baseline.
- Descriptive Language: We also encourage patients to use their own words. Is the pain "sharp," "dull," "aching," or "burning"? These details help our clinicians pinpoint the source and choose the most effective treatment.
- Observing Non-Verbal Cues: Many of our patients can't articulate their feelings. In these situations, our team is expertly trained to recognize the non-verbal signs of distress.
These subtle but critical cues are often the clearest language a patient has. Recognizing them is a true cornerstone of compassionate care.
Listening to What Is Not Being Said
For patients who can't verbalize their needs, our hospice professionals become detectives of discomfort. We carefully watch for physical and behavioral shifts that signal pain.
We operate on a core belief: a person's inability to speak does not mean they have nothing to say about their pain. Our job is to listen with our eyes and our hearts, translating subtle cues into meaningful relief.
This focus on observation is vital for anyone in hospice, especially those with advanced dementia or who are non-responsive. The signs we look for include:
- Facial Expressions: Subtle grimacing, a furrowed brow, or frequent wincing can all point to pain.
- Restlessness: Increased agitation, constant fidgeting, or an inability to get comfortable are common signs.
- Changes in Breathing: Holding one's breath, taking shallow breaths, or a sudden spike in respiratory rate can be an involuntary reaction to discomfort.
- Body Language: Guarding a specific part of the body or pulling away when touched often signals the source of pain.
Family members are invaluable partners in this process. You know your loved one better than anyone and can often spot subtle changes that might otherwise be missed.
Your insights help us build a complete picture of your loved one’s comfort. You can learn more by reading our guide on how doctors determine hospice eligibility.
This detailed, ongoing assessment is what allows us to provide truly effective hospice pain management across Monterey County, San Benito County, and our neighboring communities. It ensures our care plan is always aligned with one simple goal: total comfort.
Tailoring Treatments for Total Comfort
Once we have a clear picture of what a person is feeling, our focus shifts entirely to bringing them relief. Think of it like opening a comprehensive comfort toolkit.
This kit isn’t limited to just one or two options. It’s filled with a wide range of tools, from proven medications to gentle, hands-on therapies. This allows us to build a hospice pain management plan that’s a perfect fit for the individual.
At Central Coast VNA & Hospice, our care philosophy isn't about choosing one method over another. It's about blending different approaches to create a layered, supportive effect for patients across Monterey County and our neighboring communities.
Pharmacological Treatments: The Role of Medication
Medication is often a cornerstone of effective pain management in hospice. Our expert medical team, led by a physician and closely managed by a Registered Nurse, uses medications with incredible precision.
The absolute priority is always to maximize comfort while keeping any unwanted side effects to a minimum. One of the most common concerns we hear from families is about the use of strong pain relievers, especially opioids.
They understandably worry about the risk of addiction. In the context of end-of-life care, however, the clinical focus shifts completely. The goal is to relieve the very real, physical suffering caused by a terminal illness, which means addiction is no longer a primary medical concern. Our team's expertise is in finding the lowest possible dose that still keeps your loved one comfortable.
Research into serious health-related suffering (SHS) from 1990 to 2021 revealed a growing need for hospice pain management worldwide. This was due to chronic conditions like cancer and dementia. This analysis highlights that pain management gaps disproportionately impact women, children, and the elderly. You can read the full research findings on global palliative care needs.
This careful, proactive management is what truly sets hospice care apart. It’s an approach designed to stay ahead of the pain.
Non-Pharmacological Methods: Comfort Beyond Medication
While medications are vital, they are only one piece of the puzzle. We know that true comfort comes from a holistic approach that nurtures the body, mind, and spirit.
This is where non-pharmacological—or non-medication—therapies play a crucial role. These gentle, supportive methods can be incredibly powerful, both on their own and when used alongside medication.
These comfort-focused therapies often include:
- Therapeutic Repositioning: Sometimes, a simple change in position is all it takes to relieve pressure and reduce stiffness. Our Hospice Aides are skilled in gently repositioning patients.
- Massage and Touch Therapy: A gentle hand or foot massage can do wonders for easing muscle tension, improving circulation, and providing a deep sense of human connection and calm.
- Music Therapy: Listening to favorite songs can lower anxiety, bring back positive memories, and offer a powerful, welcome distraction from physical discomfort.
- Creating a Peaceful Environment: Lowering the lights, reducing noise, and adding a pleasant scent to the room can transform a space into a tranquil sanctuary.
These techniques work in harmony to soothe the nervous system and promote deep relaxation. This integrated model shares many core principles with palliative care, which also focuses on improving quality of life. You can learn more about the wide-ranging benefits of palliative care in our detailed guide.
Pharmacological vs. Non-Pharmacological Pain Treatments
| Treatment Category | Examples | Best Used For |
|---|---|---|
| Pharmacological | Opioids (morphine, fentanyl), NSAIDs (ibuprofen), Nerve pain medications (gabapentin), Anti-anxiety medications | Managing moderate to severe persistent or breakthrough pain from the illness itself. |
| Non-Pharmacological | Massage, Therapeutic Repositioning, Music Therapy, Aromatherapy, Creating a calm environment | Easing anxiety, reducing muscle tension, promoting relaxation, and providing emotional and spiritual comfort. Often used with medications. |
It's not a matter of "either/or." The best, most comprehensive pain management plans use both approaches to address all facets of a person's discomfort.
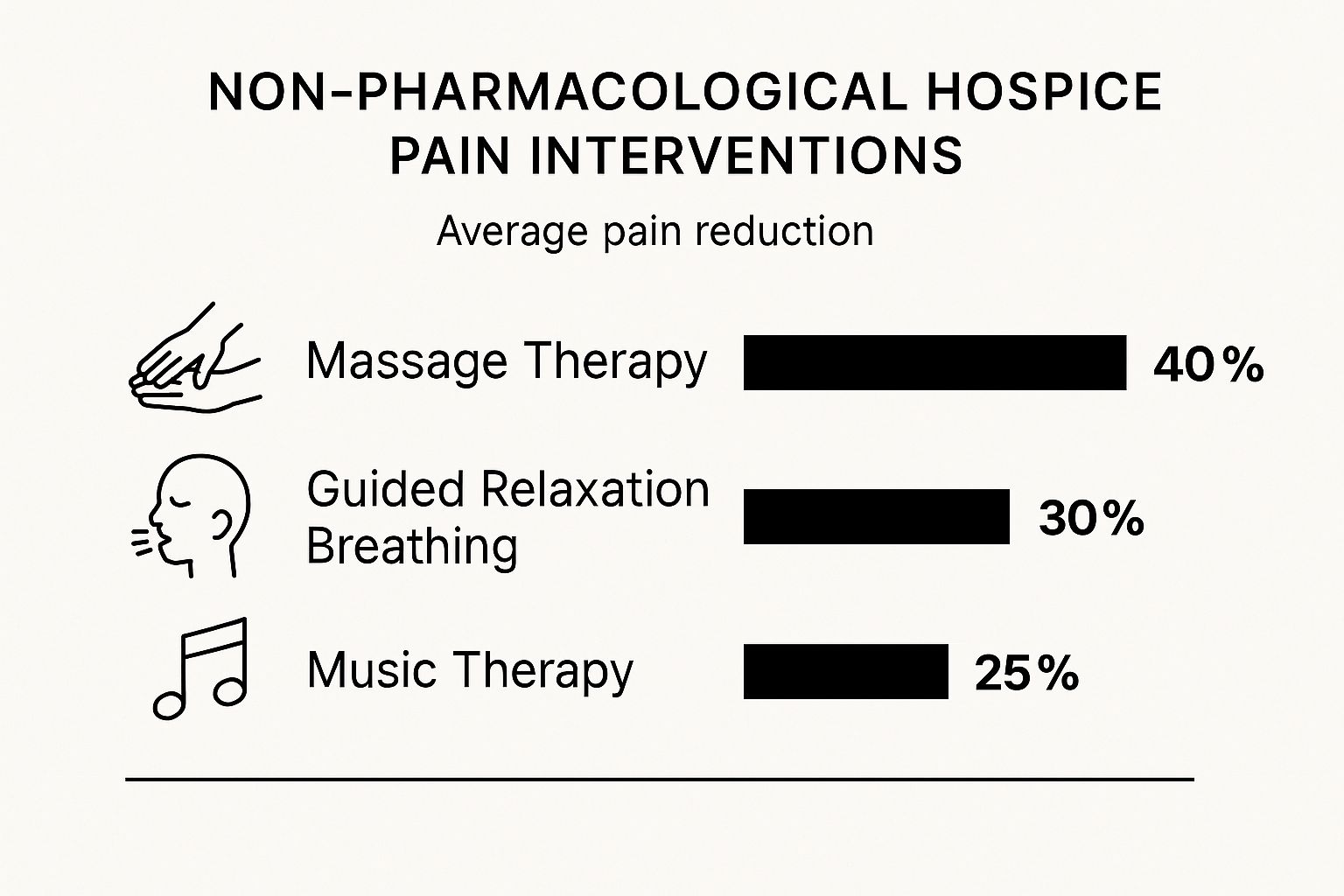
The data in this infographic really drives home the point. Gentle therapies like massage and guided relaxation can provide a significant reduction in pain, reinforcing the immense value of a multi-faceted comfort plan.
By blending the best of both worlds—expert medication management and compassionate comfort therapies—we create a truly personalized care experience. This is the promise of Central Coast VNA & Hospice.
How Families Can Partner in Providing Comfort
When a loved one receives hospice care at home, family members become essential partners in their comfort. You're not just a bystander; you're a vital part of the care team.
At Central Coast VNA & Hospice, our goal is to give families the knowledge and confidence to step into this active role. This partnership between our clinical team and your family is a cornerstone of effective hospice pain management.
Becoming an Effective Comfort Advocate
As a family member, your observations are invaluable. You know your loved one's normal moods, behaviors, and subtle cues better than anyone.
Being an effective advocate means knowing what to watch for and feeling confident when you communicate with your hospice team. Think of yourself as the team's eyes and ears between our visits.
Noticing small changes—and reporting them right away—allows our Registered Nurses to make timely adjustments to the care plan. Simple yet powerful ways you can be an advocate include:
- Observing and Reporting: Keep a simple log of when your loved one seems comfortable versus when they appear distressed. Note the time and the symptoms you see.
- Maintaining a Consistent Schedule: Giving pain medication on the schedule prescribed by the Registered Nurse is critical. This prevents the cycle of pain from returning.
- Communicating Openly: Never hesitate to call your hospice team with a question or concern. There's no such thing as an insignificant detail when it comes to your loved one’s comfort.
Creating a Soothing Home Environment
Beyond medication and direct care, the atmosphere of the home itself plays a huge role in providing comfort. You have the power to create a peaceful sanctuary.
Small, thoughtful actions can make a world of difference. These acts of care contribute directly to your loved one's sense of well-being and security.
Your presence and touch are powerful non-pharmacological tools. Simply holding a hand, reading aloud, or being quietly present can lower stress and provide a profound sense of connection and peace.
Consider these simple ways to foster tranquility:
- Reduce Sensory Overload: Dim the lights, lower the volume on the television, and minimize loud or sudden noises to create a calm space.
- Engage the Senses Gently: Play favorite, calming music from their past. Use a diffuser with a familiar, pleasant scent like lavender. Offer a soft blanket.
- Encourage Peaceful Moments: If you can, position their bed near a window with a pleasant view. Your own calm and reassuring presence is one of the most comforting things you can offer.
Partnering with Central Coast VNA & Hospice means you are never alone on this journey. We are here to support your entire family with education and reassurance across Monterey, San Benito, Santa Cruz, and South Santa Clara counties.
Taking the Next Steps With Confidence

We've walked through how hospice pain management really works. It’s a combination of a dedicated team, personalized assessments, and a mix of treatments all working together.
This isn't just a service; it's a fundamental right for every person as they near the end of life. The goal is to make sure your loved one feels peace, dignity, and comfort.
The road to end-of-life care can feel uncertain, but you don’t have to wait for a crisis to start getting answers. Looking into hospice is a positive, loving step you can take right now to honor your loved one's wishes.
A Legacy of Trusted, Nonprofit Care
For more than 74 years, Central Coast VNA & Hospice has been a steadfast, mission-driven partner for families in our community. As a local nonprofit, our focus is on people, not profits.
We've had the honor of serving generations of residents across Monterey, San Benito, Santa Cruz, and South Santa Clara Counties. The need for this kind of dedicated support has never been greater.
Starting the conversation about hospice early is one of the most empowering things you can do for your family. It puts the focus back on quality of life. If you're wondering how to begin, we offer guidance on how to prepare your loved one for hospice care.
Choosing hospice isn't about giving up. It's about choosing comfort, embracing peace, and giving your loved one the gentle, dignified care they deserve in the familiar surroundings of home.
Our team is here to walk alongside you on this journey. You are not alone, and we have the expertise to help you navigate this path with confidence.
Take the First Step Toward Peace of Mind
If you think a loved one could benefit from our compassionate hospice services, please reach out. Our team is ready to provide a consultation, answer your questions, and help you understand all of your options.
Contact Central Coast VNA & Hospice today to learn more about how we can bring comfort and dignity to your family when it matters most.
Frequently Asked Questions About Hospice Pain Management
Of all the topics surrounding hospice, pain management is often the one families have the most questions about. It’s completely understandable.
At Central Coast VNA & Hospice, we believe in being open and honest, giving you clear answers so you can feel confident. Here are some of the most common questions we hear.
Will my loved one become addicted to pain medication?
This is a worry we hear all the time, and it comes from a place of deep care. But in hospice, our goals shift completely.
Our primary mission is to provide comfort and ensure the best possible quality of life. The clinical definitions of addiction simply do not apply when treating pain from a terminal illness. Our expert team, led by a physician and a Registered Nurse, manages medications to relieve suffering so your loved one can be comfortable.
What if my family member cannot say they are in pain?
This is where the expertise of a hospice team shines. Our Registered Nurses and Hospice Aides are specially trained to recognize the non-verbal signs of discomfort.
We look for subtle cues like new restlessness, a slight grimace, or a change in breathing patterns. We also see you—the family—as our most essential partners. Your insights help us create a pain management plan that truly meets their needs.
One of our core beliefs is that every person has a right to be free from pain. An inability to speak doesn't change that right one bit. Our team is committed to listening with our eyes and our expertise to provide comfort.
Does pain medication in hospice speed up the end of life?
This is a persistent myth that causes unnecessary fear. The truth is, the goal of pain medication in hospice is to improve the quality of life, not shorten it.
When a person's body is no longer fighting against constant, exhausting pain, they can finally rest more peacefully. The medications prescribed are carefully dosed to provide relief and comfort, not to hasten death.
Are there non-medication options for pain relief?
Yes, absolutely. We believe in a holistic approach because pain isn't just physical. That's why we combine medication with other powerful, comfort-focused therapies.
Some of these non-medication options include:
- Gentle massage to ease tense muscles.
- Therapeutic repositioning to relieve pressure.
- Music therapy to soothe anxiety.
- Emotional and spiritual support from our Medical Social Workers and Chaplains.
Who pays for hospice pain management and medications?
For the vast majority of families, there is no out-of-pocket cost. Hospice care, which includes all team visits, medical equipment, supplies, and medications related to the terminal diagnosis, is covered 100% by the Medicare Hospice Benefit.
This coverage is also provided by Medi-Cal and most private insurance plans. As a nonprofit provider serving the Central Coast for over 74 years, Central Coast VNA & Hospice is committed to ensuring everyone can access this care.
Understanding your options is the first step toward finding peace of mind. To learn more about how our expert team can support your family with compassionate, personalized care, contact Central Coast VNA & Hospice today. Visit us at https://ccvna.com to start the conversation.
Your Guide to a Hospice Care Plan
When you hear the term "hospice care plan," you might picture a dry, clinical document. But it is so much more than that. Think of it as a personalized roadmap—one created not just by a medical team, but with the patient and their family at the very center of the conversation.
This plan is all about honoring a person's complete well-being—physical, emotional, and spiritual. It ensures their final chapter truly reflects their wishes for comfort and dignity.
A Roadmap for Comfort and Dignity

When a family chooses hospice, they embrace a philosophy of care that prioritizes quality of life. The hospice care plan is the tool that puts that philosophy into action. It translates deeply personal conversations about hopes, fears, and values into a practical, actionable guide for the entire team.
At its core, this plan ensures every single decision—from adjusting medication to scheduling visits from a Hospice Aide—is perfectly aligned with what the patient wants. It’s a process that removes the guesswork and anxiety, giving both the patient and their family a sense of control during a difficult time.
For over 74 years, Central Coast VNA & Hospice has been dedicated to this patient-first model. We bring compassionate care to families rooted right here in the communities we serve, including Monterey County and San Benito County.
What Does the Plan Actually Include?
A hospice care plan is a comprehensive document that coordinates every facet of a patient's journey. It’s not a "set it and forget it" document. Our interdisciplinary team constantly reviews and updates it to meet the patient's changing needs.
A great care plan is built on several key pillars:
- Pain and Symptom Management: This details the specific medications, therapies, and other interventions needed to manage physical symptoms like pain, nausea, or shortness of breath.
- Emotional and Psychosocial Support: A Medical Social Worker helps patients and their families navigate the immense emotional stress that comes with a terminal illness.
- Spiritual and Existential Needs: Our Chaplains offer support for a patient's beliefs, values, and search for meaning, no matter their spiritual background or affiliation.
- Family and Respite Support: This outlines services designed to support family members, including vital bereavement counseling and respite care to help prevent burnout.
A hospice care plan isn't about giving up. It's about shifting the focus to a different kind of hope—the hope for comfort, for peace, and for spending truly meaningful time with the people you love. It’s designed to honor a life fully lived, not just manage its end.
To give you a clearer picture, here’s a breakdown of the essential components that form a complete hospice care plan.
Key Elements of a Hospice Care Plan
This table outlines the core components that come together to create a patient-centered hospice care plan.
| Component | Description | Focus Area |
|---|---|---|
| Medical Assessment | Detailed evaluation of the patient's diagnosis, prognosis, and physical symptoms. | Clinical Needs |
| Symptom Management | Specific plan for medications, therapies, and medical equipment to ensure comfort. | Physical Comfort |
| Emotional Support | Counseling and resources for the patient and family to cope with anxiety, depression, and grief. | Psychosocial Well-being |
| Spiritual Care | Support from a chaplain to address spiritual or existential concerns, aligned with patient beliefs. | Spiritual & Existential |
| Family Support | Services like respite care and training for family members to help them provide care confidently. | Family & Health |
| Patient Goals & Wishes | Documentation of the patient's personal preferences for care, location, and end-of-life decisions. | Patient Autonomy & Dignity |
| Bereavement Plan | Support services planned for the family for up to 13 months following the patient's passing. | Grief & Family Continuation |
Each of these elements is woven together, creating a seamless and supportive experience for everyone involved.
A Foundation for Trust and Compassion
Ultimately, the care plan serves as the foundation for the trusted relationship between the hospice team, the patient, and their family. As a nonprofit, mission-driven provider, Central Coast VNA & Hospice makes sure every plan reflects our deep commitment to the communities we serve in Monterey County, San Benito County, Santa Cruz County, and South Santa Clara County.
By clearly documenting a patient's wishes, the plan provides clarity and invaluable peace of mind for everyone. To learn more about how our expert teams develop these personalized roadmaps, take a closer look at our approach to hospice care.
The Four Pillars of Compassionate Care

A truly effective hospice care plan is built on four interconnected pillars. Think of them like the legs of a sturdy table—each one is absolutely essential for providing balanced and complete support. At Central Coast VNA & Hospice, our teams work together to ensure every pillar is strong, creating a plan that cares for the whole person, not just their diagnosis.
We understand that a serious illness touches every part of a person's life. By focusing on these four key areas, we build a circle of support around the patient and their loved ones. This approach ensures comfort, preserves dignity, and honors the individual’s journey with deep compassion.
Pillar 1: Expert Pain and Symptom Management
The first and most important pillar is managing physical symptoms. It’s hard to find peace or connect with family when you’re in pain or uncomfortable. That’s why our primary goal is to provide expert relief from pain, shortness of breath, fatigue, and other symptoms that come with a life-limiting illness.
Our skilled Registered Nurses collaborate closely with the patient, their family, and our Medical Director to find the right mix of medications and therapies. This might involve:
- Medication Adjustments: Carefully fine-tuning doses to maximize relief while keeping side effects to a minimum.
- Non-Pharmacological Therapies: Using gentle positioning, breathing exercises, or calming music to complement medical treatments.
- Durable Medical Equipment: Arranging for a hospital bed, oxygen, or other equipment to make the home safer and more comfortable.
This proactive approach helps the patient stay as alert and comfortable as possible, so they can focus on what matters most. While some of these comfort measures overlap with other types of care, it's important to understand the distinctions. You can learn more in our detailed guide on palliative vs. hospice care.
Pillar 2: Emotional and Psychosocial Support
A serious illness often brings a wave of complex emotions for everyone involved. The second pillar of our care plans directly addresses these emotional and psychosocial needs. It’s about creating a safe space to process feelings of fear, sadness, anxiety, and even anger.
Our Medical Social Workers are trained professionals who provide critical support in this area. They help families navigate difficult conversations, work through unresolved issues, and find healthy ways to cope.
A hospice care plan recognizes that emotional health is just as important as physical comfort. It provides a dedicated support system to help families find strength and resilience during one of life's most challenging times.
This pillar is all about connection and understanding. The social worker becomes a trusted guide, helping to ease the emotional burden so families can focus on their precious time together.
Pillar 3: Spiritual Care and Support
The third pillar acknowledges the deeply human need for meaning, connection, and peace at the end of life. Spiritual care is a very personal part of the hospice plan that honors each person’s beliefs, values, and traditions—whether they are religious or not.
Our Chaplains are skilled at providing non-denominational support. They meet patients and families right where they are, offering a compassionate ear and gentle guidance. This could look like:
- Helping a patient reflect on their life and legacy.
- Facilitating religious rituals or connecting the family with their preferred spiritual leader.
- Simply being a quiet, reassuring presence when words aren't needed.
This support is designed to nourish the inner self, helping patients and their families find a sense of peace and closure.
Pillar 4: Practical Support for Families
Finally, the fourth pillar focuses on the practical, everyday needs of the family. A hospice care plan extends beyond the patient to support those providing love and care around the clock. Our team steps in to help lift some of the burdens that can lead to exhaustion and burnout.
Services like respite care offer family members a much-needed break. A Hospice Aide can step in for a few hours, allowing someone to rest and recharge.
This pillar also includes comprehensive bereavement support, providing counseling and resources for up to 13 months after a loved one has passed. This long-term commitment is a core part of our nonprofit mission, ensuring families in Monterey County and the surrounding areas are never alone in their grief.
How Your Hospice Care Plan Is Created
Creating a hospice care plan isn’t a clinical transaction where a doctor hands you a prescription. It's a thoughtful, collaborative process that unfolds through a series of conversations. The process always places the patient and family at the very center of every decision.
This careful approach ensures the final plan is a true reflection of the patient's values, goals, and wishes. Here at Central Coast VNA & Hospice, our process always begins with listening. We know that a meaningful plan can only be built on a deep understanding of your unique situation, your hopes, and your concerns.
Step 1: Initial Consultation and Assessment
The journey starts with an initial consultation and a comprehensive assessment. A Registered Nurse will meet with the patient and family, usually in the comfort of their own home, whether that's in Monterey, Santa Cruz, or a neighboring community. This first meeting is about so much more than just reviewing a medical history; it's a dedicated time for our team to simply listen.
During this assessment, the nurse evaluates physical symptoms and discusses the current medical situation. More importantly, they create a safe space for the family to ask tough questions and share what truly matters most to them. This foundational conversation sets a compassionate, respectful tone for all the care that follows.
Step 2: Setting Goals and Defining Wishes
Once we have a clear understanding of the situation, the next step is to define the goals of care. This is a critical conversation where the patient’s voice is the most important one in the room. What does a "good day" look like for them?
Our team, which includes a Medical Social Worker, helps facilitate these deeply personal discussions. The goals might be things like:
- Remaining at home, surrounded by familiar comforts and the people they love.
- Achieving enough pain control to be able to enjoy visits with family.
- Having spiritual support to find a sense of peace and closure.
These personal goals become the North Star for the hospice care plan. For families wondering how to even start these sensitive conversations, we offer guidance on how to prepare your loved one for hospice care.
Step 3: Assembling the Interdisciplinary Team
With the goals clearly defined, we assemble the interdisciplinary care team. This team is handpicked to meet the specific needs identified during the assessment and goal-setting talks. While a Medical Director oversees every plan, the specific team members involved will vary from person to person.
For example, a patient wrestling with spiritual questions will have a Chaplain as an active part of their team. A family feeling overwhelmed might receive extra support from a Medical Social Worker and trained Volunteers. This customized approach ensures the right experts are there to provide support across Monterey, San Benito, Santa Cruz, and South Santa Clara counties.
Step 4: Documenting and Implementing the Plan
With the team in place, we document the formal Plan of Care. This written guide translates the patient's wishes into concrete actions for the entire team. It details everything from medication schedules to emotional support strategies and bereavement plans for the family.
This infographic shows how we structure ongoing communication, which is vital to bringing the plan to life.
This structured flow ensures communication stays consistent. It also helps families feel continuously supported by their care team.
Step 5: Regular Meetings and Plan Updates
A care plan isn't a static document set in stone; it's a living guide. The interdisciplinary team meets at least every 15 days to review the patient's progress, discuss any changes, and make sure the plan is still meeting their needs.
This ensures the plan remains responsive and effective, adapting as the situation evolves. A patient's needs can change, and the care plan must be flexible enough to change right along with them. This constant fine-tuning is what keeps the focus squarely on comfort and dignity.
Meet Your Dedicated Hospice Care Team

A hospice care plan is a promise of support delivered by a team of committed professionals. We call this group the interdisciplinary team, and they work together to make sure every aspect of your care plan is carried out with skill and genuine compassion. Each person brings a unique expertise, forming a complete circle of care around you and your family.
At Central Coast VNA & Hospice, our entire nonprofit, mission-driven approach is built on this very idea. For over 74 years, we’ve seen firsthand that the best care comes from a group of experts working hand-in-hand. Let's introduce the core members of the team who will walk alongside you on this journey.
Your Clinical and Medical Support
At the heart of your team are the clinical experts who oversee the medical side of your hospice care plan. Their focus is on ensuring your physical comfort and managing complex symptoms with precision and kindness.
The Medical Director is a physician with specialized training in palliative and hospice medicine. They provide overall medical leadership for every patient, working closely with the patient's own doctor and the rest of the hospice team.
Your main point of contact will be the Registered Nurse (RN). The RN makes regular home visits to assess your condition, manage medications, and handle pain and other symptoms directly. They are also an incredible source of education and support for the family.
Hands-On Personal and Practical Care
Beyond the medical side, your team provides the essential hands-on support that makes a world of difference in daily quality of life. These team members focus on comfort, dignity, and helping you navigate any practical hurdles that come up.
The Hospice Aide is there to provide gentle, personal care. This might include helping with bathing, dressing, and other daily activities that have become challenging. Their warm presence and respectful approach are key to maintaining a patient’s dignity and comfort.
A Medical Social Worker is your go-to resource for navigating emotional and practical challenges. They offer counseling, connect you with community resources, and assist with complex things like advance directives. They're there to ease the non-medical burdens that can add so much stress.
A hospice care team is like a symphony orchestra. Each musician plays a different instrument, but together, they create a beautiful, cohesive piece of music that soothes and supports the listener.
This collaborative approach ensures that every need—from medical to emotional—is met. Here's a quick look at how each team member contributes to your well-being.
Your Hospice Interdisciplinary Team Roles
The strength of hospice care lies in its team-based model, where professionals from different fields collaborate to provide holistic support. The table below outlines the key members of your team and what they do.
| Team Member | Primary Role |
|---|---|
| Medical Director | Oversees all medical care and collaborates with the team on symptom management. |
| Registered Nurse | Manages pain and symptoms, provides clinical care, and educates the family. |
| Hospice Aide | Offers hands-on personal care, including bathing, dressing, and daily assistance. |
| Medical Social Worker | Provides emotional support and connects families with practical resources. |
| Chaplain | Offers spiritual support that respects all beliefs, values, and backgrounds. |
| Volunteer | Provides companionship for the patient and respite breaks for the family. |
Each role is distinct, yet they all work in unison to wrap a complete layer of support around you and your loved ones.
Spiritual and Companionship Support
Finally, some members of the team focus on the spiritual and social needs that are so integral to a person's sense of self and peace. Their goal is to provide connection, comfort, and a sense of calm.
The Chaplain offers spiritual support that is completely inclusive and respects all beliefs, traditions, and backgrounds. They are skilled listeners who can help patients and families explore questions of meaning, find peace, and reflect on a life's legacy.
Last but not least, our highly trained Volunteers are the heart of our community-based care. They might read to a patient, offer simple companionship, or just provide a comforting presence that can dramatically reduce feelings of isolation. They also give family members a chance to take a much-needed break.
The True Value of a Formalized Care Plan
A structured hospice care plan is so much more than a clinical checklist. It is a roadmap for comfort, clarity, and communication. It ensures that a patient’s wishes are not just heard, but turned into compassionate actions every single day.
For the person at the center of care, having a formal plan provides a sense of control and dignity when so much feels uncertain. There's real peace of mind in knowing your preferences are clearly documented and respected. It’s about ensuring your final chapter is written on your own terms.
Easing the Burden on Families
For families, a well-defined hospice care plan is a huge relief. It helps lift the heavy weight of second-guessing decisions or worrying if they're doing the "right" thing. The plan lays out a clear path that everyone can follow, clarifying roles and setting up straightforward communication with the hospice team.
This allows family members to step back from managing logistics and focus on what truly matters: spending meaningful time together. It creates a framework of support that helps prevent burnout and lets the family feel guided. For anyone navigating this journey, understanding the 5 reasons to consider hospice for a loved one can offer even more clarity and confidence.
Enhancing Quality of Life Through Organized Care
One of the greatest gifts of a formal hospice care plan is how much it improves a patient's quality of life. By proactively managing symptoms, the plan helps keep pain and discomfort under control. This allows the patient to stay as alert and engaged as they want to be.
This organized approach coordinates the entire spectrum of care, from visits by a Hospice Aide to counseling from a Medical Social Worker. It’s about nurturing the whole person—body, mind, and spirit. At Central Coast VNA & Hospice, our nonprofit mission is rooted in this philosophy, ensuring a smoother journey for everyone involved across Monterey and our neighboring counties.
A formalized hospice care plan is the bridge between a patient's wishes and the compassionate care they receive. It ensures that every action taken by the care team is a direct reflection of what is most important to the person at the center of it all.
The preference for this kind of organized, comfort-focused care is clear. According to the National Hospice and Palliative Care Organization (NHPCO), over 1.72 million Medicare beneficiaries received hospice services in 2020 (NHPCO, 2021). The overwhelming majority of this care was provided as Routine Home Care, highlighting the desire for supportive services at home. You can explore more hospice care trends in this federal report.
Care That Adapts to Every Person and Place
A hospice care plan is anything but a standard document. It's a deeply personal roadmap that is flexible enough to honor a person’s unique life, their specific situation, and where they feel most comfortable. Truly compassionate care is all about meeting people exactly where they are—both physically and emotionally.
The real sign of an excellent hospice care plan is its ability to adapt. At Central Coast VNA & Hospice, our teams have spent over 74 years mastering this. We specialize in tailoring support to fit the individual needs of every patient and family we serve across Monterey County, San Benito County, Santa Cruz County, and South Santa Clara County.
Care Wherever Someone Calls Home
While most people think of hospice care happening in a person’s own home—and it often does—our support follows the patient wherever they reside. A well-designed hospice care plan works just as effectively and compassionately in any setting. The priorities of comfort and dignity never change.
We are experienced in creating specialized plans for individuals in:
- Skilled Nursing Facilities: We work closely with the facility's staff, adding another layer of expert symptom management and emotional support.
- Assisted Living Communities: Our team integrates into the community, supplementing the care already in place and focusing on the specific needs that come with end-of-life journeys.
- Board and Care Homes: In these smaller homes, our plan ensures patients get the full benefit of our entire team, from nursing and medical oversight to spiritual and emotional support.
This flexibility guarantees that every patient gets consistent, high-quality hospice care, no matter what they call home.
Adapting Plans for Different Health Conditions
Just as every home is different, so is every patient's diagnosis. A hospice care plan has to be precisely tuned to manage the specific symptoms and challenges that come with different terminal illnesses.
For example, a plan for someone with advanced cancer might focus on sophisticated pain management strategies. But for a patient with end-stage heart failure, the focus would shift to managing shortness of breath and fatigue.
A hospice care plan for a person with dementia requires a special kind of understanding. It must anticipate non-verbal cues for discomfort and focus on creating a calm, soothing environment to minimize confusion and agitation.
For conditions like advanced dementia or ALS, the plan will often emphasize non-verbal communication and gentle personal care from a Hospice Aide. It will also include significant emotional support for the family as they navigate what can be a long and heart-wrenching journey. This detailed, person-centered care is part of our commitment to serving the entire Central Coast community.
Frequently Asked Questions About Hospice Care Plans
Navigating end-of-life care brings many questions, and getting clear, straightforward answers can provide comfort and control. At Central Coast VNA & Hospice, we believe open communication is the heart of compassionate care. Below, we've answered some of the questions we hear most often.
Who creates the hospice care plan?
A hospice care plan is developed by an interdisciplinary hospice team in collaboration with the patient and their family. The team includes a Medical Director, Registered Nurse, Medical Social Worker, and Chaplain. However, the patient's personal wishes and goals are the most important factor guiding every decision in the plan.
How often is the care plan reviewed?
By regulation, the interdisciplinary team formally reviews the care plan at least every 15 days. In reality, it can and should be updated any time there’s a noticeable change in the patient's condition, symptoms, or personal preferences. This flexibility ensures care remains perfectly aligned with the patient's current needs.
Can a patient or family request changes to the plan?
Yes, absolutely. Patients and their families are essential partners in this process. If you notice a new symptom, have a concern, or feel a part of the plan isn't working, you should speak up right away. Your hospice Registered Nurse is your primary contact for discussing adjustments to the hospice care plan.
What happens if a patient's condition improves?
It is possible for a patient's health to stabilize or improve while receiving the comprehensive comfort of hospice care. If their prognosis improves to the point where they no longer meet medical requirements, they can be discharged from hospice services. Our team at Central Coast VNA & Hospice would then help coordinate a safe and seamless transition back to curative treatment or another level of care. You can learn more by reading our guide on hospice care eligibility.
Does the care plan include support for the family after death?
Yes, it does. Comprehensive support for the family, known as bereavement care, is a core part of the hospice philosophy and is included in the care plan from the beginning. Our commitment to families in Monterey, San Benito, Santa Cruz, and South Santa Clara counties continues for up to 13 months after their loss, providing counseling, support groups, and other resources.
The end-of-life journey is deeply personal, and having a compassionate, expert team by your side makes all the difference. At Central Coast VNA & Hospice, we are here to answer your questions and guide you with care and respect. Contact us today to learn more about our nonprofit hospice services.
How Do You Know When Hospice Is Needed? A Guide for Families
One of the most difficult questions families face is: how do you know when hospice is needed? The answer often becomes clear when the focus of care shifts. Hospice is the right path when the goal is no longer to cure an illness, but to maximize comfort, dignity, and quality of life.
Defining the Shift to Comfort-Focused Care

Choosing to begin hospice care is a deeply personal and often challenging decision for everyone involved. It marks a significant transition away from aggressive, curative treatments toward a philosophy centered on comfort and peace.
This change is not about giving up. It is about making a proactive choice for compassionate support that honors a person’s final wishes.
For over 74 years, Central Coast VNA & Hospice has been a trusted, nonprofit partner for families navigating this journey. Our mission is to provide expert, mission-driven care that respects the values and goals of each individual we serve across Monterey County, San Benito County, Santa Cruz County, and South Santa Clara County.
Understanding the Goal of Hospice
The primary goal of hospice is to improve the quality of a person's remaining life. Instead of focusing on endless medical tests and treatments aimed at a cure, the team concentrates on managing symptoms. This means tackling issues like pain, anxiety, and shortness of breath so the person can live as fully and comfortably as possible.
This compassionate approach is carried out by an experienced, interdisciplinary team that includes:
- A primary or hospice physician
- A Registered Nurse to manage clinical care
- A Hospice Aide to assist with personal care like bathing and dressing
- A Chaplain for spiritual support
- A Medical Social Worker for emotional and practical support
When Is the Right Time to Consider Hospice?
Determining the right moment requires open and honest conversations between the patient, their family, and their doctor. Generally, hospice is appropriate for someone with a life-limiting illness who has a prognosis of six months or less, if the disease runs its natural course.
It's a vital service that helps many Americans. According to the National Hospice and Palliative Care Organization (NHPCO), about half of all Medicare beneficiaries who passed away in 2021 utilized hospice care (NHPCO, 2023). However, enrollment times vary widely, which often points to referrals happening too late.
The table below breaks down the fundamental differences between curative medical treatment and the comfort-focused philosophy of hospice care.
Comparing Curative Treatment vs. Hospice Care
| Focus Area | Curative Treatment | Hospice Care |
|---|---|---|
| Primary Goal | To cure the disease and prolong life | To enhance quality of life and provide comfort |
| Treatment Approach | Aggressive (surgery, chemotherapy, etc.) | Palliative (pain and symptom management) |
| Care Setting | Typically hospitals and clinics | Primarily in the patient's home or a facility |
| Team Focus | Medical specialists treating the disease | Interdisciplinary team addressing holistic needs |
| Emotional Support | Often secondary to medical treatment | A core component for patient and family |
| Family Involvement | Family provides support, but is not the focus | Family is central to the care plan |
As you can see, the shift to hospice represents a change in priorities, not an absence of care. It’s about choosing a different kind of care—one that puts the person, not the disease, at the center.
Hospice is not a place, but a philosophy of care. It focuses on bringing comfort, dignity, and peace to patients wherever they call home, ensuring their final chapter is lived on their own terms.
By choosing hospice, families can get back to what matters most: spending meaningful time together. At Central Coast VNA & Hospice, we are here to guide you through this process with compassion and expertise. Contact us today to learn more about our services.
Observing Key Physical and Clinical Indicators
When you're close to someone with a serious illness, you start to notice subtle shifts. It’s not just one thing, but a collection of changes that signal the body is weakening and could benefit from a different kind of care.
While every person's experience is unique, there are specific clinical signs that doctors look for when considering hospice. These are real-world changes that family members are often the first to see.
Recognizing these signs helps families understand when it might be time to shift the focus toward expert symptom management. Our Registered Nurses and Hospice Aides are specialists in managing these exact symptoms, all with the goal of enhancing comfort and preserving dignity.
Worsening Symptoms and Decline in Function
One of the most obvious signs is when a person’s ability to handle everyday tasks starts to slip. Medically, this is called a decline in Activities of Daily Living (ADLs).
You might see a loved one who was once independent now struggling with simple things. It often looks like this:
- Needing help to bathe or get dressed
- Struggling to get from the bed to a chair
- Losing control of their bladder or bowels
This physical decline usually comes with symptoms that are becoming harder to control. Think of persistent pain, constant shortness of breath, nausea that won't go away, or an overwhelming sense of fatigue. When usual treatments are no longer effective, it’s a strong sign that hospice care is needed.
Significant Weight Loss and Loss of Appetite
Another tell-tale clinical sign is noticeable, unintentional weight loss. This is often paired with a sharp drop in appetite. As the body grapples with a serious illness, it can lose its ability to use nutrients correctly, leading to cachexia, or wasting syndrome.
This is a profound metabolic change, not simply a matter of a person not feeling hungry. At this point, the goal of care naturally shifts from pushing food and fluids to honoring what the body is saying and focusing on comfort. A hospice team's role is to manage any discomfort and support the patient's choices.
A common misconception is that hospice is only for cancer patients. While many hospice patients have cancer, data shows that a significant number have other conditions. Understanding the full range of indicators beyond a specific diagnosis is key. Discover more insights on hospice demographics and access patterns.
An Increase in Hospital or ER Visits
A revolving door of emergency room visits and hospital stays is often a clear indicator that an illness is progressing. If your loved one has been in the hospital two or more times in recent months for the same issue without lasting improvement, it is time to ask a tough question. Are these hospital visits truly helping them meet their goals for quality of life?
Each hospitalization can be incredibly draining, both physically and emotionally. Choosing hospice brings care directly into the home, whether in Monterey or San Benito County. This can prevent exhausting and stressful trips to the hospital. To get a better sense of the formal criteria, our guide on how doctors determine hospice eligibility is a great resource.
Listening to Emotional and Quality of Life Cues

Beyond the lab results and clinical charts, some of the most powerful signs come directly from your loved one. Their emotional state, words, and wishes are vital information. These cues are deeply personal and tell a story about their readiness to shift focus from fighting an illness to finding peace.
Paying close attention to these emotional and quality-of-life signals is a profound act of love. It’s about truly hearing them and acknowledging that they are the expert on their own journey.
Recognizing a Shift in Perspective
You might start to notice a significant change when someone begins pulling back from activities and people they once cherished. Maybe they no longer ask about their favorite sports team or gently decline visits from close friends.
This withdrawal isn't always a sign of depression. Often, it's a way of conserving precious energy and a natural turning inward as they prepare for what’s ahead.
Another unmistakable sign is when they express a clear desire to be at home instead of in a hospital. After an endless cycle of appointments and hospital stays, many people say, “I’ve had enough. I just want to be home.” That statement is a powerful declaration of their priorities.
Honoring this wish to be home is a cornerstone of hospice care. We know comfort isn't just about managing physical pain—it's about the deep, restorative peace that comes from being in a familiar, loving environment, surrounded by the people and memories that matter most.
The Emotional Toll of a Long Illness
Living with a terminal illness is draining. The exhaustion runs deeper than the physical body; it takes a heavy emotional and spiritual toll. It’s not uncommon to hear someone say they feel "done fighting," which is an honest admission of exhaustion.
At Central Coast VNA & Hospice, our Chaplains and Medical Social Workers are here to support patients and families through these complex emotional roads. They create a safe, compassionate space to explore feelings, talk through fears, and find meaning. This type of whole-person care is central to our mission as a nonprofit provider on the Central Coast.
These emotional cues are just as important as any clinical symptom. They are the vital signs of a person’s inner world, helping guide families toward a decision that honors their loved one’s wishes.
Starting the Conversation About Hospice Care

Broaching the topic of hospice care is often the hardest step for families. It feels heavy, final, and many worry it’s like admitting defeat. But this conversation can be one of the most loving and powerful things you can do.
When you frame it as a way to honor their wishes and reclaim control, the entire dynamic shifts. It becomes a moment of connection, not a moment of giving up. The key is to approach it with empathy, gentleness, and a genuine desire to listen.
Finding the Right Time and Tone
Timing is everything. Look for a quiet, private moment when you can speak freely without being rushed. A calm afternoon at home often works best.
Lead with your heart, not a medical agenda. Start with open-ended questions that center on their feelings and goals to show you respect their autonomy.
You could try saying something like:
- “I’ve been thinking about what’s most important to you these days. Can you tell me what a good day looks like for you?”
- “We’ve been in and out of the hospital so much. I’m wondering how you’d feel about focusing more on being comfortable at home.”
- “What are you worried about most right now? I want to make sure we're doing everything we can to help with those fears.”
Questions like these open a door to a real dialogue about their priorities. It can also be helpful to understand the specifics yourself; you can read more about palliative vs. hospice care in our detailed guide.
Focusing on Empowerment and Control
One of the greatest gifts of hospice is how it hands control back to the patient and their family. Instead of constantly reacting to the disease, you get to be proactive about how you want to live the time that remains.
Discussing hospice is not about giving up. It is about shifting focus to ensure your loved one's final chapter is written on their terms, filled with as much peace and comfort as possible.
When you have the conversation, emphasize that hospice adds a layer of expert support. Explain that a dedicated team from Central Coast VNA & Hospice can come right to the home. They manage pain and control symptoms so everyone can focus on quality time together.
This reframes the entire concept. Hospice becomes a new beginning, one focused on living as well as possible, for as long as possible.
Arranging Hospice Care on the Central Coast
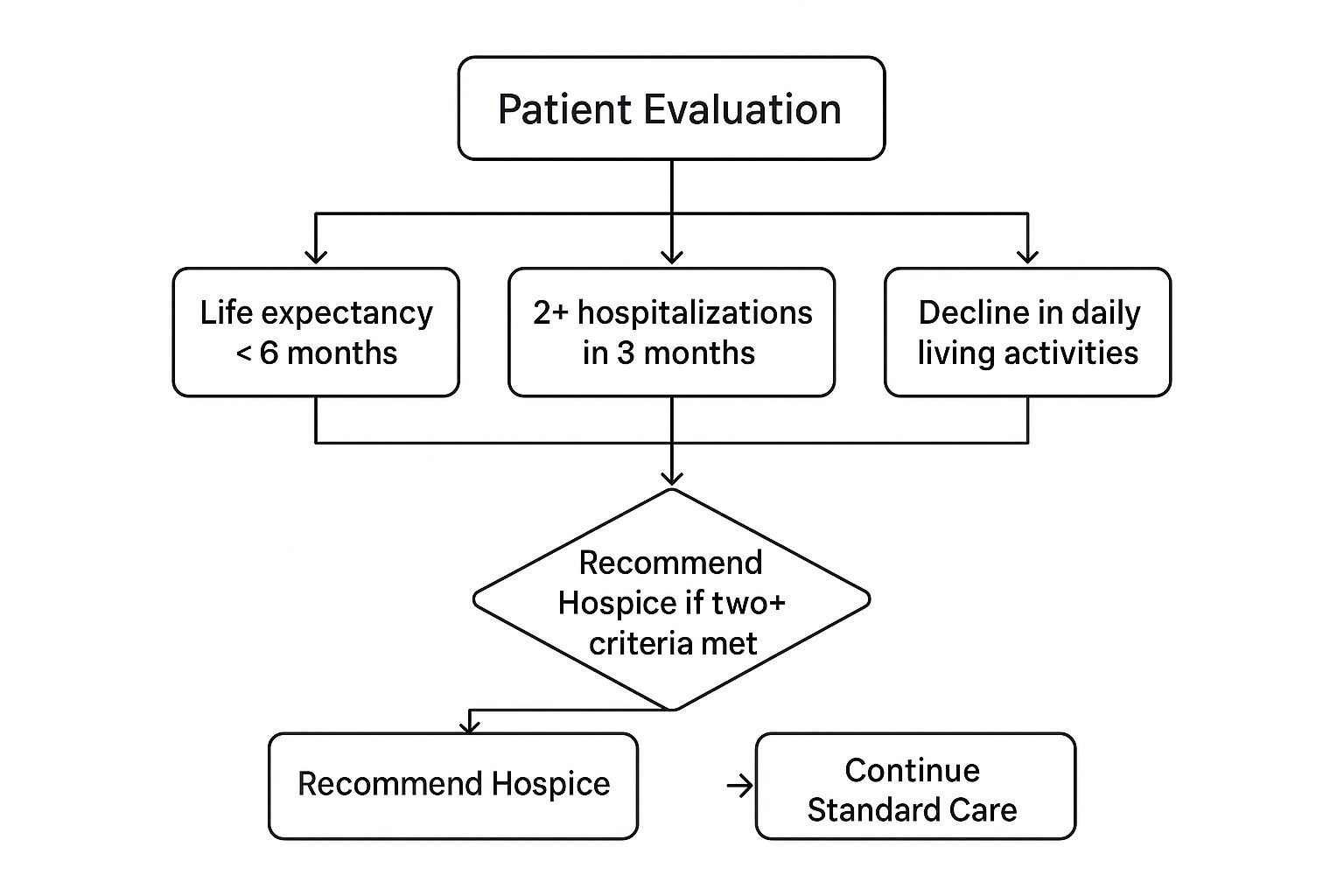
Once your family feels that hospice might be the right path, the next steps can feel overwhelming. But the process is designed to be supportive and clear, taking the stress off your shoulders. It all starts with a simple conversation and an evaluation.
The first official step is usually a physician’s referral, which confirms a life-limiting prognosis. You can also contact Central Coast VNA & Hospice directly to request a hospice evaluation. We’ll then coordinate with your loved one’s doctor to get the necessary orders.
The Informational Visit and Assessment
After you make that initial contact, a Registered Nurse can schedule an informational visit. This is a no-pressure, no-obligation meeting that can happen wherever your loved one calls home in Monterey, Santa Cruz, or South Santa Clara County. The nurse will assess your loved one's specific needs, answer every question, and explain how our team provides support.
During this visit, you'll get a clear picture of:
- How a personalized care plan is created.
- The roles of each team member, from the Hospice Aide to the Chaplain.
- How we handle getting all necessary medical equipment and supplies delivered to the home.
- The 24/7 on-call support that's always available for urgent needs.
Understanding Financial Coverage
Worrying about cost should never stand in the way of getting excellent care. Hospice is a fully covered benefit under Medicare Part A, Medi-Cal, and most private insurance plans. This comprehensive coverage removes the financial burden by paying for the hospice team's services, medications, and equipment.
As a nonprofit organization with 74 years of local history on the Central Coast, we are committed to providing care to everyone who is eligible. For a complete overview of what our hospice care entails, take a look at A Compassionate Guide to Hospice Care on the Central Coast.
Choosing hospice is a significant decision. With the right information and support, it can bring peace and comfort to your entire family.
Frequently Asked Questions About Hospice Care
When you're faced with the decision to start hospice care, a million questions can run through your mind. It’s an emotional and often confusing time. Getting clear, straightforward answers is one of the most reassuring things a family can experience.
Here are some of the most frequent questions we hear from families across Monterey County and the surrounding areas. We want to clear up the confusion and give you the peace of mind you need.
Does choosing hospice mean we are giving up hope?
Absolutely not. Choosing hospice isn’t about giving up hope; it’s about changing what you hope for. The focus shifts from hoping for a cure to hoping for comfort, peace, and quality time with loved ones.
It’s an active decision to ensure the time someone has left is lived with dignity and without pain. Hope becomes about good days, meaningful moments, and a peaceful environment.
Can a patient leave hospice care if their condition improves?
Yes, they can. A patient always has the right to stop hospice care at any time, for any reason. If their condition stabilizes or they decide to try a new curative treatment, they can be discharged from the hospice program.
The care plan must always reflect the patient's current needs and wishes. If their health declines again later, they can easily re-enroll in hospice when the time is right.
Who pays for hospice care?
Hospice care is covered by Medicare Part A, Medi-Cal, the Department of Veterans Affairs, and most private insurance plans. This comprehensive coverage includes everything from the hospice team's services to the medical equipment, supplies, and medications related to the terminal illness.
As a nonprofit organization that's been serving the Central Coast for over 74 years, Central Coast VNA & Hospice is dedicated to caring for all eligible patients. Our mission is to ensure everyone in our community can access compassionate end-of-life support.
What is the difference between palliative care and hospice care?
This is a great question, as the two are related but serve different purposes. Palliative care can start at any point during a serious illness, even while someone is still receiving curative treatments. The main goal is to relieve symptoms and stress to improve quality of life.
Hospice care is a specific kind of palliative care for people with a life-limiting illness and a prognosis of six months or less who are no longer seeking a cure. At Central Coast VNA & Hospice, we are proud to offer a full continuum of care, allowing for a smooth transition from home health to palliative care to hospice if and when a patient's needs evolve.
Where is hospice care provided?
Hospice care is provided wherever the patient calls home. This is most often their private residence, but it can also be a skilled nursing facility, an assisted living community, or a board and care home.
Our team at Central Coast VNA & Hospice brings expert medical, emotional, and spiritual support directly to patients across Monterey County, San Benito County, Santa Cruz County, and South Santa Clara County. The goal is to provide comfort in a familiar setting.
The team at Central Coast VNA & Hospice is here to answer any other questions you may have. We provide compassionate guidance to families across the Central Coast. Contact us today to learn more.
A Guide to Hospice Eligibility Requirements
Thinking about hospice care brings up many emotions and questions. The first step toward understanding it is quite straightforward.
At its core, hospice eligibility comes down to a doctor’s professional judgment. They must determine that a patient has a terminal illness and a life expectancy of six months or less, assuming the illness takes its natural course. This marks a fundamental shift in focus—away from treatments meant to cure and toward care centered on comfort, dignity, and peace.
When Is It Time to Consider Hospice Care?

Knowing when to explore hospice is a deeply personal process. While the medical prognosis is the official starting point, the decision is really about changing the philosophy of care. It’s about choosing to prioritize quality of life when aggressive treatments may no longer be working or wanted.
This is a conversation, not a command. A patient’s own doctor and a dedicated hospice medical director work together to make the clinical determination. At Central Coast VNA & Hospice, our team is committed to supporting families through this process with warm, compassionate guidance.
We ensure everyone in Monterey County, San Benito County, Santa Cruz County, and South Santa Clara County feels heard, informed, and respected. Our local roots and 74+ years of service mean we understand our community's needs.
The Focus on Quality of Life
Hospice isn't about giving up. It’s about adding life to a patient's days, not just more days to their life. The eligibility process is designed to recognize that point when the burdens of treatment start to outweigh the potential benefits.
This opens the door to a kind of care that addresses the whole person. Of course, that includes managing physical pain, but it also means providing emotional and spiritual support for both the patient and their family. Our interdisciplinary team—which includes Registered Nurses, Chaplains, and Medical Social Workers—works together to create a plan that honors the patient’s wishes.
Understanding the Prognostic Guideline
The "six-month" timeline is a key part of the hospice eligibility requirements first established by Medicare. This has become the standard for most private insurance as well. According to the National Hospice and Palliative Care Organization (NHPCO), over 1.72 million Medicare beneficiaries received hospice services in 2020 (NHPCO, 2021).
It's critical to understand that this is a guideline, not an expiration date. It's a medical estimation of what the future may hold. Taking a moment to explore the distinctions between palliative and hospice care can help clarify how each one supports patients at different stages of a serious illness along our continuum of care.
At Central Coast VNA & Hospice, with over 74 years of nonprofit service, we believe that understanding these requirements is the first step toward accessing profound support. Our local roots and mission-driven approach ensure that every family receives the guidance they need to make the best decision for their unique situation.
If you believe a loved one might benefit from this specialized care, starting the conversation is a courageous and loving act. Contact us today to learn more about how we can help.
Understanding the Core Medical Criteria
While the official starting point for hospice is a six-month prognosis, what does that really look like day-to-day? The clinical side of hospice eligibility requirements goes much deeper than just a timeline. It’s about observing specific, tangible changes in a person’s health and well-being that tell us an illness is entering its final stage.
This is where a concept called functional decline comes into play. It’s simply a term for a noticeable and progressive loss of ability to perform daily activities. Recognizing these signs is often the first step for families in understanding that it might be time to have a meaningful conversation about comfort care.
What Is Functional Decline?
Think of functional decline not as one single event, but as a slow, steady tide going out. It reveals new challenges that weren't there before. For families, these shifts are often the most visible evidence that a loved one’s condition is advancing beyond what curative treatments can manage.
The presence of functional decline helps doctors paint a much clearer picture of a patient’s overall health. It gives them concrete evidence to support a terminal prognosis, which makes the whole eligibility determination more accurate. It's why our team at Central Coast VNA & Hospice pays such close attention to these details during an assessment.
Our expert Registered Nurses, with their deep experience in home-based care across Monterey County and the surrounding areas, are trained to see these subtle but significant changes. They work side-by-side with a patient’s primary doctor to ensure the evaluation is both thorough and compassionate.
Common Signs of Functional Decline
It can be tough to watch these changes happen, but knowing what to look for can empower you. Some of the most common indicators that may point toward hospice eligibility include:
- Progressive Weight Loss: This is unintentional weight loss, especially when someone is eating normally. It can be a sign the body is no longer able to process nutrients effectively because of the advanced illness.
- Increased Assistance with Daily Activities: A growing need for help with simple tasks like bathing, getting dressed, eating, or even just moving from a bed to a chair often shows declining strength and energy.
- Worsening Symptoms: This could be pain, shortness of breath, or nausea that becomes more frequent, more intense, or stops responding to the usual treatments.
- More Frequent Hospitalizations: If trips to the ER or hospital stays are becoming more common, it can signal that an illness is getting harder to manage outside of a supportive care setting.
- Decreased Alertness: Spending more time sleeping, being less engaged in conversations, or showing new signs of confusion can all point to a significant physical decline.
These markers aren't just a checklist; they're pieces of a larger story. Every person’s journey is unique, and our nonprofit, mission-driven approach ensures we always see the individual, not just the symptoms. For a deeper look, you can learn more about how doctors determine hospice eligibility in our related guide.
The Role of a Professional Assessment
While families are often the first to notice these changes, a formal evaluation by a professional is a necessary step. A patient’s personal physician, working with a hospice medical director, must certify that the medical criteria have been met.
At Central Coast VNA & Hospice, this process always begins with a compassionate conversation. One of our Registered Nurses will conduct an in-home assessment, respectfully observing the patient’s condition and talking with the family. This visit provides the clinical information the physician needs to make a final determination.
Our role, built on 74 years of serving the Central Coast, is to bring clarity and support. We help translate complex medical information into terms everyone can understand, making sure families in Monterey, San Benito, Santa Cruz, and South Santa Clara counties feel confident in their decisions. If you've noticed signs of decline, contacting us is a proactive step toward getting the answers and support your family needs.
Navigating Medicare and Insurance for Hospice

Worrying about how to pay for hospice care is a burden no family should have to carry. When a loved one needs comfort and dignity, cost should never be a barrier. Thankfully, the financial side of hospice is often much more straightforward than people think.
The key is the Medicare Hospice Benefit, which falls under Medicare Part A. It sets a comprehensive standard of care that most other payers—including private insurance, Medi-Cal, and VA benefits—tend to follow. It’s designed to be an all-inclusive benefit, covering nearly everything a patient needs related to their terminal diagnosis.
As a local nonprofit serving Monterey County, San Benito County, Santa Cruz County, and South Santa Clara County, our team at Central Coast VNA & Hospice has spent decades helping families make sense of their coverage. Our only goal is to make this process clear and stress-free.
What the Medicare Hospice Benefit Covers
Once a patient meets the hospice eligibility requirements and chooses to begin care, Medicare Part A steps in to cover a surprisingly wide range of services. This support is built to manage the illness, control symptoms, and lift up the entire family, all while minimizing out-of-pocket costs.
All services are organized through a single, interdisciplinary plan of care. This just means your hospice team coordinates everything to provide seamless support. After 74 years of refining this approach, we know it's the best way to ensure every aspect of a patient's well-being is addressed.
Core services covered typically include:
- Nursing Care: Regular visits from a Registered Nurse to manage symptoms, adjust medications, and provide skilled care right where the patient lives.
- Medical Equipment: Hospital beds, wheelchairs, oxygen, and any other necessary equipment delivered directly to the home.
- Medical Supplies: Items like wound care dressings, catheters, and incontinence products are fully covered.
- Medications: All prescriptions for pain relief and symptom management tied to the hospice diagnosis.
- Support Services: Visits from a Medical Social Worker, Chaplain, and Hospice Aide for personal, emotional, and spiritual support.
This comprehensive coverage frees families to focus on what truly matters: the patient’s comfort and quality of life.
Understanding the Four Levels of Hospice Care
The Medicare Hospice Benefit isn't one-size-fits-all. It defines four distinct levels of care to meet a patient’s needs as they change over time. The overwhelming majority of this care happens wherever the patient calls home.
- Routine Home Care: This is the most common level of hospice care. All the services listed above are delivered directly to the patient in their own home, an assisted living facility, or a nursing home.
- General Inpatient Care: If pain or other symptoms become too difficult to manage at home, a patient can be temporarily moved to an inpatient facility. This allows for more intensive, round-the-clock medical attention to get symptoms back under control, after which the patient can return home.
- Continuous Home Care: For brief periods of medical crisis, this level brings more intensive, "round-the-clock" nursing care into the home. It’s designed to manage severe symptoms without having to go to a hospital.
- Inpatient Respite Care: This service gives family members a much-needed break by allowing a patient to be temporarily placed in a Medicare-approved facility for up to five days.
The numbers show just how central home-based care is. In a recent fiscal year, Medicare recorded approximately 147.7 million hospice days of care. Of those, about 146 million were for routine home care. You can read more on hospice utilization in this CMS report.
At Central Coast VNA & Hospice, our mission as a community-based nonprofit is to ensure care is always accessible. We help families navigate their Medicare, Medi-Cal, VA, or private insurance benefits to ensure they receive all the support they are entitled to.
If you have questions about your coverage or how to access hospice care in Monterey County and our neighboring communities, we're here to give you clear answers. Contact us today to see how our team can help you and your family.
Eligibility Signs for Common Conditions
The "six-month prognosis" is a good starting point for hospice care eligibility, but it can feel abstract when you're dealing with a specific illness. Every condition follows its own path. Knowing what to look for can help families and doctors recognize when a shift toward comfort care makes sense.
It’s about understanding the specific clinical markers that signal a disease has entered its final, most challenging phase. For each of these, our team at Central Coast VNA & Hospice looks for clear signs that an illness has advanced to its terminal stage.
While many people still think of hospice as being primarily for cancer, you can see that conditions like end-stage heart failure and advanced dementia are major reasons people seek this specialized support. To give you a clearer picture, this table shows some of the key clinical signs that often point toward hospice eligibility for several common conditions.
Hospice Eligibility Indicators by Common Condition
This table outlines common medical conditions and associated clinical signs that may indicate a patient meets hospice eligibility requirements. This is for informational purposes and not a substitute for a physician's evaluation.
| Condition | Common Clinical Indicators for Eligibility |
|---|---|
| Dementia/Alzheimer's | Reaching Stage 7 on the FAST scale; limited speech; inability to walk or sit up without help; significant weight loss; recurrent infections (e.g., pneumonia, UTIs); difficulty swallowing (dysphagia). |
| Heart Disease | Persistent congestive heart failure symptoms (e.g., shortness of breath) at rest despite maximum medical therapy; documented ejection fraction of 20% or less; frequent hospitalizations for cardiac issues; significant functional decline. |
| Lung Disease (COPD) | Severe, disabling shortness of breath (dyspnea) at rest or with minimal activity, unresponsive to bronchodilators; need for continuous oxygen; right-sided heart failure (Cor pulmonale); unintentional weight loss of more than 10% in six months. |
| Cancer | Stage IV disease with widespread metastasis; a notable decline in functional ability (e.g., low Palliative Performance Scale score); decision to stop curative treatments like chemotherapy or radiation; worsening, uncontrolled symptoms like pain or nausea. |
Of course, these are just reference points. A full, compassionate assessment by a clinical team is the only way to formally determine if a patient qualifies for hospice. Let’s break down what these indicators look like in more detail.
Advanced Dementia and Alzheimer’s Disease
Dementia is a slow-moving disease that chips away at a person's memory, thinking, and ability to manage daily life. In the advanced stages, the need for round-the-clock support becomes undeniable, which is often when a person becomes eligible for hospice.
Doctors often use a tool called the Functional Assessment Staging Tool (FAST) to see how far the disease has progressed. Patients who reach stage 7 are generally considered eligible for hospice. At this point, they typically have very few words left, can no longer walk without help, and eventually lose the ability to sit up on their own.
Other signs we look for in dementia patients include:
- Significant, unexplained weight loss over the past six months.
- Recurring infections, like pneumonia or urinary tract infections.
- Trouble swallowing (dysphagia), which can lead to aspiration.
- The presence of other serious health issues, such as heart or lung disease.
End-Stage Heart Disease
For someone with severe heart disease, there comes a time when treatments just don't bring lasting relief anymore. The patient might feel constant, exhausting symptoms even when they're just sitting in a chair, which is a clear sign their condition has hit an advanced stage.
Our Registered Nurses and physicians—serving communities from Monterey to South Santa Clara County—look for evidence that the heart simply can't keep up. This is a critical factor in determining hospice eligibility.
Key clinical signs include:
- Constant symptoms of congestive heart failure, like chest pain or shortness of breath, that are tough to manage.
- Frequent trips to the emergency room or hospital for heart problems.
- A documented ejection fraction of 20% or less, which is a measure of how effectively the heart is pumping blood.
- A major decline in function, leaving the person mostly confined to a bed or chair.
Advanced Lung Disease (COPD)
Chronic Obstructive Pulmonary Disease (COPD) and other advanced lung conditions can turn every breath into a battle. As the disease worsens, patients often need continuous oxygen and experience severe shortness of breath (dyspnea) with even the slightest movement.
Hospice eligibility here often hinges on how severe the lung damage is and how much it impacts daily life. The Central Coast VNA & Hospice team looks at how the disease is preventing the body from getting enough oxygen and the functional decline that results.
Common markers for hospice eligibility include:
- Severe, chronic lung disease that is documented by medical tests.
- Disabling shortness of breath that doesn't get better with treatments like bronchodilators.
- An increase in respiratory infections or hospital visits for breathing issues.
- Cor pulmonale, a type of right-sided heart failure caused by high blood pressure in the lungs.
- Losing more than 10% of body weight over six months without trying.
Stage IV Cancer
When cancer reaches Stage IV, it means the disease has metastasized, or spread, to other parts of the body. While every cancer behaves differently, this advanced stage often signals that curative treatments are no longer working or are no longer what the patient wants.
Hospice eligibility for cancer patients rests on two things: the clinical proof that the disease is progressing and the patient's personal choice to shift their focus to quality of life. This is a deeply personal decision, one our team has supported with compassionate care for 74 years.
Factors that often point toward hospice readiness include:
- Widespread, metastatic disease that has been confirmed by a doctor.
- A significant drop in functional ability, measured by tools like the Palliative Performance Scale (PPS).
- A decision to stop aggressive treatments like chemotherapy or radiation.
- The presence of worsening, uncontrolled symptoms like pain, nausea, or profound fatigue.
FAQs About Hospice Eligibility
When you’re exploring hospice care, it’s natural to have a lot of questions. We've gathered some of the most common concerns we hear about hospice eligibility requirements to give you straightforward, compassionate answers. As a trusted nonprofit that has served the Central Coast for over 74 years, we believe in empowering families with information.
What happens if a patient on hospice lives longer than six months?
This is one of the first questions many families ask. If a patient lives beyond the initial six-month prognosis, they can absolutely continue receiving hospice care. The Medicare Hospice Benefit is designed with flexibility in mind.
Care is structured in "benefit periods." As long as the hospice medical director or attending physician re-certifies that the illness is still life-limiting, services continue without interruption. Our team at Central Coast VNA & Hospice regularly re-evaluates each person's condition to ensure they still qualify.
Can a patient stop hospice care if they change their mind?
Yes, absolutely. A person has the right to stop hospice care at any time for any reason. This is called "revoking" the benefit, and it ensures the patient is always in control of their healthcare choices.
Sometimes, a person's condition might unexpectedly improve, or they may decide to try a new curative treatment. If they decide to return to hospice later, our Central Coast VNA & Hospice team is ready to help restart the process quickly and smoothly.
Is a DNR order required to be eligible for hospice?
No, a patient does not need a "Do Not Resuscitate" (DNR) order to qualify for hospice care. This is a common myth that can unfortunately keep families from getting the support they need sooner.
While we encourage gentle conversations about advance directives, it is never a requirement for admission. Our Medical Social Workers and Chaplains are fantastic at helping patients and families explore these topics, but the final decision always belongs to the patient.
How do we start the conversation about hospice with our doctor?
Bringing up hospice with a physician can feel intimidating. We’ve found that a direct, honest, and caring approach works best. You could try saying, "We want to make sure we understand all our options, including hospice. Could we talk about whether it might be the right choice?"
Another option is to call Central Coast VNA & Hospice directly. Our team can speak with you first. Then, with your permission, we can coordinate with your doctor to explore eligibility together across Monterey, San Benito, Santa Cruz, and South Santa Clara counties.
Is hospice care only for the last few days of life?
This is probably the biggest myth about hospice. While some people are referred very late in their illness, the benefit is actually designed to provide meaningful support for months, not just days. To get a better feel for this, you can explore our resources on receiving hospice care for comfort and dignity.
Studies show that patients and families get the most out of hospice when it begins earlier. That extra time allows for better symptom management and lets a real, trusting relationship build with the care team. We always encourage families to ask about hospice sooner to improve a loved one's quality of life.
How is hospice eligibility different from palliative care eligibility?
Palliative care can be started at any stage of a serious illness, even at the same time as curative treatments. Hospice eligibility, on the other hand, requires a physician's certification that the patient has a life expectancy of six months or less and has chosen to stop curative treatments. Central Coast VNA & Hospice offers both services as part of our continuum of care.
How soon does hospice care start after eligibility is confirmed?
Once eligibility is confirmed and the necessary consent forms are signed, care can often begin within 24 to 48 hours. Our mission at Central Coast VNA & Hospice is to provide support as quickly as possible. The admission process is designed to be smooth and stress-free for families throughout our service areas.
The journey through a serious illness is full of questions. If you're exploring options for yourself or someone you love, the compassionate team at Central Coast VNA & Hospice is here with clear answers and unwavering support. Contact us today to learn more about our home health, palliative, and hospice services.










