A Guide to Healing with Hospice Bereavement Services
When a loved one's journey ends, a new one begins for those left behind. Hospice bereavement services are a core component of end-of-life care, created to support families as they navigate the grieving process. It’s a bridge, extending the same compassionate support from hospice into the difficult period that follows a loss.
A Bridge of Support When a Journey Ends

The care a hospice team provides doesn't stop the moment a patient passes away. For mission-driven organizations like Central Coast VNA & Hospice, our commitment extends to the entire family. This continuing support is what we call hospice bereavement services—a specialized program designed to guide individuals and families through the complex emotions of loss.
This support isn't just a reaction after a death occurs. It often starts before the loss happens with what's known as anticipatory grief counseling. This proactive approach helps families begin to process the challenging emotions that naturally arise during a loved one's final months and weeks.
What Does Bereavement Care Involve?
Bereavement support offers a steady hand and a safe space for healing. It starts with the understanding that grief is a natural, yet incredibly challenging, experience. A comprehensive program offers a variety of resources to meet people wherever they are in their personal journey.
This often includes:
- One-on-One Counseling: Private sessions with a trained Bereavement Coordinator or Chaplain to talk through feelings.
- Support Groups: Professionally led groups that connect people with others who understand what they're going through.
- Educational Materials: Resources that explain the grieving process and provide practical coping strategies.
- Supportive Communication: Gentle check-in calls and mailings that remind families they haven't been forgotten.
At its heart, bereavement care is about honoring the whole family's experience. It validates the pain of loss while providing the tools needed to navigate a path toward healing and remembrance.
Support for Our Central Coast Community
As a nonprofit with over 74 years of local service, Central Coast VNA & Hospice provides these services as a fundamental part of our care. Our programs are available to the families we've served across Monterey County, San Benito County, Santa Cruz County, and South Santa Clara County.
We truly believe no one should have to walk through grief alone. Our dedicated team is here to offer comfort, understanding, and professional guidance. You can learn more about our bereavement and grief support groups, which build a community for those who need it most.
Why Professional Grief Support Is Essential

Losing a loved one can feel like trying to navigate a vast, unpredictable ocean. Professional bereavement support acts as a lighthouse, offering a safe harbor where you can process your emotions without judgment. While support from friends and family is invaluable, the guidance of a trained professional provides an essential layer of care.
Unaddressed grief can take a serious toll on both physical and emotional well-being. Without a healthy outlet, the stress and sorrow can manifest in surprising ways, from sleep problems to a weakened immune system. It can also lead to more serious challenges, like complicated grief or depression.
The Dangers of Navigating Grief Alone
Trying to manage a profound loss without guidance can be an incredibly isolating experience. The journey is rarely a straight line, as emotions like anger, denial, and deep sadness can appear unexpectedly. Without professional support, individuals may struggle with a range of issues.
- Emotional Overwhelm: It's easy to feel lost in a sea of intense emotions without the tools to understand or manage them.
- Physical Health Decline: The chronic stress of grieving can lead to real health problems, including increased inflammation and digestive distress.
- Prolonged Grief: Some people find themselves "stuck" in their grief, unable to find a path forward. This is an indication that more specialized support is needed.
- Strained Relationships: The intensity of grief can sometimes strain relationships with others who may not understand the depth of your pain.
Professional hospice bereavement services create a space where your feelings are validated. An experienced Bereavement Coordinator understands the complexities of loss and can affirm that your experience is a normal part of the grieving process.
The Growing Need for Structured Support
The importance of this kind of care is being recognized on a larger scale. As our population ages and awareness of holistic care grows, the demand for comprehensive hospice services—including bereavement support—is on the rise.
For over 74 years, Central Coast VNA & Hospice has seen firsthand how guided support helps people find their footing again. Our experience across Monterey, San Benito, and Santa Cruz counties shows that professional guidance can transform a journey of sorrow into one of meaningful healing. It provides a structured, compassionate framework for processing loss.
Engaging with hospice early on can also give families more time to access these vital support systems. You can explore more about the reasons to consider hospice for a loved one in our related article.
What a Comprehensive Bereavement Program Includes
A high-quality bereavement program is like a well-stocked toolkit, offering different tools to help families navigate the path of grief. There’s no one-size-fits-all approach. Instead, a truly supportive program provides a menu of services that can be tailored to each person's needs.
At Central Coast VNA & Hospice, our hospice bereavement services are built on this philosophy. We provide compassionate, flexible support for families throughout Monterey, San Benito, Santa Cruz, and South Santa Clara counties.

Personalized Counseling and Emotional Guidance
One of the most essential parts of any bereavement program is one-on-one counseling. It offers a private, non-judgmental space where you can explore your feelings with a trained professional, like a Bereavement Coordinator or a Chaplain.
These sessions are shaped entirely by your needs. The goal isn't to "fix" your grief but to walk alongside you, helping you find healthy ways to cope. It's a confidential space to speak honestly without worrying about burdening others.
Connection Through Support Groups
While individual counseling is vital, there's immense healing power in shared experience. Professionally led support groups are a cornerstone of effective bereavement care. They connect people who are facing similar losses, which can reduce the profound isolation of grief.
These groups are often organized around specific types of loss to create a stronger sense of kinship. Common examples include:
- Spousal or Partner Loss Groups: For those grieving the death of their life partner.
- Parental Loss Groups: For adults who have lost a mother or father.
- General Grief Groups: Open to anyone navigating the loss of a close loved one.
These gatherings provide a safe environment to share stories and build a new support network. This sense of community is often a critical piece of healing, much like the holistic support found in our continuum of care. You can learn more about the benefits of palliative care and how it also supports family well-being.
Educational Resources and Ongoing Outreach
Understanding the mechanics of grief can be incredibly empowering. Comprehensive programs offer educational materials that explain the common stages and symptoms of grief. This knowledge helps normalize the wide range of emotions people feel.
To help families understand the different ways support is offered, here is a breakdown of typical services:
Types of Bereavement Support Offered
| Type of Support | Description | Best For |
|---|---|---|
| Individual Counseling | Private, one-on-one sessions with a trained grief professional. | Individuals needing a confidential space to process personal feelings and experiences at their own pace. |
| Support Groups | Professionally facilitated group meetings with others who have experienced a similar loss. | People seeking connection, validation, and a sense of community with others who understand their journey. |
| Educational Materials | Newsletters, articles, and workshops explaining the grief process. | Anyone wanting to better understand their emotions and learn practical coping strategies. |
| Memorial Events | Community gatherings and services to honor and remember loved ones. | Families and individuals looking for a formal way to celebrate a loved one's life and find shared comfort. |
| Ongoing Outreach | Supportive phone calls and mailings sent periodically after the loss. | Those who appreciate knowing they are not forgotten and that support is still available long-term. |
These varied services ensure that support is available in the form that feels most helpful to each person. A core belief of nonprofit, mission-driven care is that support shouldn't stop after a few weeks. This sustained connection is a hallmark of our 74+ year commitment to our community.
Finally, memorial events and services of remembrance offer a beautiful way to honor the lives of those we've lost. These gatherings create a formal opportunity for reflection and community, helping families pay tribute in a deeply meaningful way.
How Central Coast VNA & Hospice Guides Families
At Central Coast VNA & Hospice, our commitment to families is woven into the fabric of who we are. As a nonprofit rooted on the Central Coast, our approach has always been mission-driven. This value shapes our hospice bereavement services across Monterey, San Benito, Santa Cruz, and South Santa Clara counties.
Our support often feels less like a clinical program and more like a neighbor helping a neighbor. With over 74 years of local experience, our dedicated team of Chaplains and Bereavement Coordinators offers deeply personal guidance that honors each family's unique path. We don't just provide services; we build relationships grounded in trust.
A Story of Compassionate Support
To see how this works, consider the story of the Garcia family. When their father entered our hospice program, our team focused not just on his comfort but on the well-being of his wife and their adult children. Our Bereavement Coordinator met with them early on to offer anticipatory grief support.
This gave them a safe space to ask tough questions before the loss even happened. After he passed, that support continued seamlessly. His wife found comfort in one-on-one sessions with our Chaplain, while his son joined a support group for adults grieving a parent.
This continuum of care is the heart of our nonprofit mission. It’s how we ensure families feel seen, heard, and supported from the moment they enter our care, cementing our role as a trusted partner in healing.
The Value of Nonprofit, Community-Focused Care
Because Central Coast VNA & Hospice is a nonprofit, our entire focus stays on the families we serve. We aren’t accountable to shareholders; we're accountable to our community. This freedom allows us to put resources into programs that provide genuine comfort.
- Truly Personal Support: We fit our services to the person, not the other way around. Our team is flexible and ready to help.
- Local Expertise: Our Chaplains and Bereavement Coordinators live and work on the Central Coast. They have a deep understanding of our local culture and resources.
- A Long-Term Commitment: Our help doesn’t stop after a few weeks. We remain a resource for families for as long as they need us.
The Growing Importance of Grief Support
The need for structured, compassionate grief support is gaining the recognition it deserves. The global grief counseling market—which includes many services offered by hospice—was valued at approximately USD 3.34 billion in 2024 and is expected to grow. This trend highlights a shift toward acknowledging the emotional needs that come with loss. You can read more about these developments in grief counseling.
For families on the Central Coast, this means having access to a team that is experienced and deeply embedded in the community. The support we provide is a core part of our hospice care philosophy. Our goal is to offer a steady hand and a compassionate heart to guide you through one of life’s most difficult transitions.
Who Can Receive Bereavement Support
After a loved one passes, it's common to hesitate before asking for help. Many people wonder if they are "allowed" to seek support. If your loved one was under the care of Central Coast VNA & Hospice, our hospice bereavement services are here for you.
This support isn't just for immediate family. We welcome close friends, partners, and anyone who played a significant role in the patient's life and is now grieving. Loss ripples outward, and we believe our support should too.
A Mandated and Cost-Free Service
It’s critical for families to know that our bereavement support is provided at no cost. This isn't an optional add-on; it's a required component of care under the Medicare Hospice Benefit. The goal is to ensure every family has access to professional grief support without worrying about a bill.
This gets to the heart of the hospice philosophy: caring for the family is as essential as caring for the patient. As a nonprofit, our focus is squarely on this mission. We ensure our programs are professional, compassionate, and completely free for the families we serve.
Our support is available for up to 13 months after a loved one's passing. Grief isn’t over in a few weeks or months. That extended timeframe allows our team to be there as you navigate the first year of anniversaries, holidays, and other milestones.
Support for the Entire Central Coast Community
With a history spanning more than 74 years on the Central Coast, our commitment to this community runs deep. While our program is designed for the families of our hospice patients, we are also a resource for anyone in Monterey County, San Benito County, Santa Cruz County, and South Santa Clara County who is grieving.
We help connect people with community resources to find the support they need. Being a community-based healthcare provider means fostering a supportive environment for everyone. You can learn more about how we provide trusted bereavement support in Monterey, CA and the surrounding areas.
This commitment includes:
- Access to Information: We guide community members toward publicly available support groups and other grief resources.
- Community Education: We work to raise awareness about healthy grieving and why reaching out for support is important.
- A Compassionate Point of Contact: Even if your loved one wasn't in our care, our team can offer guidance and point you in the right direction.
Our goal is to ensure no one on the Central Coast has to walk through grief alone. We strive to live up to our long-standing mission of caring for our community with empathy and integrity.
Taking the First Step Toward Healing
Grief is a heavy burden, and reaching out for support can feel like a monumental task. Asking for help is an act of strength. At Central Coast VNA & Hospice, we make that first step as simple and reassuring as possible.
This is your practical guide to our hospice bereavement services. It’s designed to clear up any confusion and remove hesitation. When you first connect with us, you'll speak with a compassionate team member whose only job is to listen and help.
How to Access Our Bereavement Support
Taking that first step is straightforward. Our Bereavement Coordinators are ready to talk, listen, and help you find the resources that feel right for you. We want you to feel empowered, not overwhelmed.
Connecting with us is easy:
- A Simple Phone Call: You can call our team directly to ask questions or set up a time to talk.
- An Email Inquiry: If writing is easier, send us a message, and a member of our team will get back to you.
- A Warm Introduction: Your hospice Registered Nurse or Chaplain can make a personal introduction to our bereavement staff.
We promise to meet you exactly where you are. Your journey through grief is your own, and our support is designed to honor your individual needs with empathy and respect.
A Community Commitment to Healing
Family-centered support is thankfully becoming recognized as a non-negotiable part of good healthcare. Hospice care has become a critical pillar for families across the country. According to the Centers for Medicare & Medicaid Services (CMS), over 1.72 million Medicare beneficiaries received hospice care in 2020. You can discover more about these hospice utilization trends in the latest CMS report.
This isn't just a number—it highlights the vital role hospice plays, not just in managing a loved one's final days, but in providing emotional and spiritual support for the entire family long after. As a nonprofit with over 74 years of service, our promise is to be a steadfast partner for families across Monterey, San Benito, Santa Cruz, and South Santa Clara counties. We are here for you and your family today, tomorrow, and for as long as you need us.
Contact us today to learn more about our bereavement programs and take the first step toward healing.
Your Questions About Bereavement Services Answered
Navigating the end-of-life journey with a loved one brings many questions about what comes next. The period after a loss can feel overwhelming, but you don't have to go through it alone. Here are answers to the questions we hear most often about hospice bereavement services.
What is the difference between grief and bereavement?
While often used interchangeably, these terms describe different parts of the same experience. Bereavement is the period of time after you’ve lost someone important; it is the state of having experienced a loss.
Grief, on the other hand, is the internal journey of emotions that come with loss, like sadness and anger. Bereavement is the event; grief is your response to it.
How long do hospice bereavement services last?
Grief doesn’t work on a schedule, which is why hospice bereavement support is designed for the long haul. At Central Coast VNA & Hospice, our support is available to family members for up to 13 months after a patient has passed away.
This 13-month timeframe is intentional. It ensures our team can walk alongside you through the difficult first year, which is often filled with painful firsts like anniversaries or holidays.
Is there a cost for bereavement support?
This is one of the most important things for families to know: hospice bereavement support is offered at no cost. These services are a core part of hospice care, required by the Medicare Hospice Benefit.
As a nonprofit organization that has served the Central Coast for over 74 years, this is a principle we stand behind completely. You will never receive a bill from us for bereavement counseling, support groups, or other grief resources.
Can children and teenagers receive support?
Absolutely. Losing someone is painful at any age, but for children and teens, the grieving process can look very different from an adult's. They might show their feelings through changes at school or in their behavior.
Specialized hospice bereavement services for young people use age-appropriate tools like art or play therapy to help them work through emotions safely. At Central Coast VNA & Hospice, we help families connect with the right resources to ensure every family member gets the support they need.
Do I have to join a support group?
No, you are never required to join a support group. A good bereavement program understands that everyone's needs are different. While many people find comfort in sharing their experiences, it's not the right path for everyone.
Our program at Central Coast VNA & Hospice is flexible. You choose what feels most helpful, whether it's one-on-one counseling, supportive phone calls, or educational materials. The choice is always yours.
What if my loved one wasn't a hospice patient?
While our formal 13-month bereavement program is designed for the families of our hospice patients, our commitment to the community doesn't stop there. As a local nonprofit, Central Coast VNA & Hospice serves as a compassionate resource for all our neighbors.
Our team can help connect any community member in Monterey County, San Benito County, Santa Cruz County, and South Santa Clara County with local grief support resources. Our goal is to ensure no one on the Central Coast has to navigate loss alone.
At Central Coast VNA & Hospice, we are committed to being a supportive partner for you and your family, today and tomorrow. Learn more about our services or contact us to find out how we can help.
Grief Counseling for Families: Healing Together
When a family loses someone they love, figuring out how to move forward can feel overwhelming and isolating. Grief counseling for families is a specific kind of support created to help everyone navigate this incredibly difficult time together. It provides a safe, guided space where each person can share what they're feeling, understand how others are grieving, and start to piece back together a sense of family connection.
How Family Grief Counseling Creates a Path for Healing
Losing a loved one impacts the entire family unit, but every single person experiences that loss differently. A young child’s confusion is different from a teenager's withdrawal, which is different from an adult’s heavy sense of responsibility. These different reactions can create silent gaps between family members right when they need each other the most.
You can think of a family as a ship caught in a storm. Grief counseling, led by professionals like our Chaplains and Medical Social Workers, acts like a skilled navigator, helping everyone on board work together to keep the ship from breaking apart.
This process isn't about making the sadness disappear. It’s about learning how to carry the weight of the loss in a healthy way, as a team. A professional bereavement counselor is a neutral guide who can help open up lines of communication that may have been shut down by pain or confusion.
Building a Foundation for Shared Support
The main goal here is to build mutual understanding and empathy. In a counseling session, families learn to see and respect that there's no “right” or “wrong” way to grieve.
A counselor might lead the family in activities designed to help them:
- Share memories of the person they lost in a way that feels healing, not just painful.
- Put words to difficult emotions without fear of judgment.
- Understand how grief looks different depending on a child's or teen's age and developmental stage.
- Create new family traditions or rituals that honor their loved one’s memory and place in the family.
The illustration below highlights the key goals of this supportive journey.
To make it clearer, here’s a quick summary of what family grief counseling focuses on.
Key Aspects of Family Grief Counseling
| Aspect | Description |
|---|---|
| Shared Healing Space | Creates a safe, neutral environment where all family members feel comfortable expressing themselves. |
| Guided Communication | A professional counselor facilitates open and honest conversations, helping to bridge emotional gaps. |
| Understanding Differences | Helps family members recognize and validate each other’s unique grieving styles and timelines. |
| Honoring Memory | Focuses on developing healthy ways to remember the loved one and integrate their memory into the family's future. |
| Developing Coping Skills | Equips the family with practical tools to manage grief triggers and support one another long-term. |
By working on these core areas, a family can begin to find a new sense of balance and support. Central Coast VNA & Hospice, a nonprofit with over 74 years of service to the Central Coast, knows how vital this journey is. We offer resources like our monthly grief support group for South Monterey County residents to help our community find its way through loss.
Why Shared Grief Support Is So Important
When a family loses someone they love, the experience can test their very foundation. Sometimes, a shared loss brings people closer together. Other times, it creates painful, silent distances that can be hard to bridge.
This is where professional grief counseling for families becomes so vital. It steps into that delicate space to address the entire web of relationships shaken by grief. Without a shared place to heal, unspoken expectations and clashing coping styles can strain even the strongest family bonds, leading to misunderstandings and deep feelings of isolation.

Think of a family as the crew of a ship caught in a terrible storm. A grief counselor is like a skilled navigator, one who can steady the ship and guide the crew to work together, facing the overwhelming waves as a single, unified team. This professional guidance ensures that every person’s voice is heard and valued—from a grieving child to an older adult—helping the family find its way back to solid ground, together.
Navigating Different Grieving Styles
There’s no right or wrong way to grieve. Every single person experiences loss on their own timeline and in their own way. One family member might need to talk things out constantly, while another might retreat into silence to process their feelings. Both are completely normal responses.
The trouble starts when these different styles are misinterpreted. One person’s silence can look like they don’t care, while another’s openness can seem overly emotional. This friction is the last thing a family needs when connection is what matters most.
A counselor helps the family understand and make room for these unique grieving styles by:
- Creating a safe space where everyone can express their true feelings without fear of judgment.
- Teaching family members how to communicate what they need from each other in a clear, healthy way.
- Validating each person's unique experience of the loss, reminding them that their feelings are legitimate.
This process helps stop resentment from building up and ensures every member of the family feels seen, heard, and supported by the people who mean the most to them.
Preventing Long-Term Complications
When grief isn't processed in a healthy way, it can fester and lead to lasting emotional problems. Family grief counseling is a powerful therapeutic tool designed to help families manage this intense distress and adjust to their new reality.
The importance of this is highlighted by the formal recognition of Prolonged Grief Disorder (PGD). This condition occurs when grief remains so intense and debilitating that it interferes with daily life. According to the American Psychiatric Association (APA), about 1 in 10 bereaved adults are at risk for developing PGD (APA, 2022).
By facing grief as a unit, families build a foundation of mutual support that can prevent these more severe outcomes from taking hold. It’s a proactive step toward protecting the long-term well-being of every single family member.
At Central Coast VNA & Hospice, our mission-driven services recognize just how important this shared journey is. Our professional team provides the guidance families in Monterey County, San Benito County, Santa Cruz County, and South Santa Clara County need to navigate loss together. You can learn more about our bereavement and grief support groups and see how we help families find their way back to healing.
The Unique Benefits of Grieving as a Family Unit
While grief is a deeply personal journey, there are powerful advantages to navigating it alongside your family. Thinking about grief counseling for families isn't just about "getting help"; it's a proactive step that can strengthen the very core of your family for years to come.
When a family heals together, they learn to speak the same emotional language. This creates a supportive home where vulnerability is met with compassion, not confusion or judgment.

Fostering Lifelong Communication Skills
One of the most profound benefits of grieving as a unit is the way it improves family-wide communication. A skilled counselor helps each person find the words for their needs and teaches everyone how to listen with genuine empathy.
These are not temporary fixes for getting through the immediate loss. They are tools that will help you resolve future conflicts and deepen your relationships for a lifetime.
Like the Japanese art of kintsugi, where broken pottery is mended with gold, counseling doesn’t hide the cracks. Instead, it highlights them, making the piece stronger and more beautiful. Family grief counseling helps mend the fractures caused by loss, reinforcing your family’s bonds with a newfound strength and understanding.
This focus on open communication is something we see in our other supportive care models as well. In fact, many families discover that learning to discuss difficult topics is also one of the key benefits of palliative care, as it improves everyone's quality of life by getting them on the same page.
Grieving together teaches a family that every emotion is valid and that every person’s experience matters. This shared validation reduces feelings of isolation and creates a powerful sense of unity.
Creating New Rituals and Continuing Bonds
A central part of family grief counseling is finding healthy, meaningful ways to honor the person you’ve lost. This often means creating new family rituals that keep their memory alive in a positive and comforting way.
These rituals can be simple or elaborate, but their purpose is profound. They provide a structured way for the family to connect with their loved one’s memory and with each other.
Some examples we’ve seen work beautifully include:
- Planting a memorial garden where each family member can contribute something special.
- Holding a yearly "memory night" on their birthday to share favorite stories or look through photos.
- Creating a "memory box" filled with items that represent the person and adding to it over time.
- Cooking their favorite meal together and sharing what made that dish so special to everyone.
Activities like these can transform a source of deep pain into a foundation for collective strength. They ensure the person you lost remains an integral part of your family’s ongoing story. By participating in grief counseling for families, you give your family the chance to grow stronger and more connected through the process of healing together.
What to Expect in a Family Counseling Session
Taking that first step toward grief counseling for families can feel huge, and frankly, a little scary. Knowing what a session actually looks like can take away a lot of that uncertainty. The whole point is to create a safe, supportive space with a compassionate professional who truly gets the tangled mess of shared loss.
It’s a judgment-free zone where every single voice matters. Think of your counselor as a neutral guide, not a referee. One of the first things they'll do is work with your family to set some simple ground rules for your conversations. This is key to building the trust you need for honest talk, even when things get emotional.
A Gentle and Guided Process
Once everyone feels safe, the real work of exploring your family's unique needs can begin. There’s no rigid script or one-size-fits-all agenda. The process is flexible and moves at your family's own pace, because healing can only be gently guided.
So, what might you actually do in a session? It could involve a few different things:
- Guided Discussions: The counselor might ask gentle questions to get people talking about their loved one and what this loss has been like for them personally.
- Memory-Sharing Exercises: Sometimes, activities are focused on remembering the good times, helping families celebrate the life that was lived.
- Collaborative Problem-Solving: Your counselor will help the family pinpoint specific struggles—like communication breakdowns or clashing coping styles—and then work together to find healthier ways forward.
The entire process is built around your family. The goal is to move forward together, making sure that even the quietest person in the room is heard and that everyone's grief is seen as valid and important.
A Growing Recognition of Support
We're seeing a much greater understanding of just how vital this kind of specialized support is. The global grief counseling market was recently valued at around $4.0 billion and is expected to grow significantly by 2032.
That kind of growth shows a real shift in public awareness about mental health and the need for accessible support when families are grieving. You can explore more about these trends and the expanding accessibility of grief support.
At Central Coast VNA & Hospice, our professional team, including our Chaplains and Medical Social Workers, is specifically trained to lead families through this process with skill and genuine empathy. We're here to provide this support for families across Monterey County, San Benito County, and our other service areas. You should never have to walk this path alone.
How Central Coast VNA & Hospice Supports Families
For more than 74 years, Central Coast VNA & Hospice has been more than just a healthcare provider. We are a mission-driven nonprofit woven right into the fabric of our communities. With deep roots in Monterey County, San Benito County, Santa Cruz County, and South Santa Clara County, our commitment is to provide compassionate care that goes far beyond the purely medical.
When a family is healing after a loss, we firmly believe they should never have to walk that path alone. This is exactly why we offer dedicated bereavement services as a core part of our continuum of care. Our support for families continues long after their loved one has passed, because we know that grief is a long journey, not a single event.

Comprehensive Bereavement Support for Your Family
At Central Coast VNA & Hospice, our professional Chaplains and Medical Social Workers are specially trained to guide families through the tough, tangled emotions of grief. They lead individual, group, and family counseling sessions that create a safe, supportive space for healing and honest communication. This professional support is a vital piece of how we care for the whole family.
We understand that the need for a helping hand doesn't just stop when hospice services do.
As a testament to our long-term commitment, Central Coast VNA & Hospice provides bereavement support services to the families of our hospice patients for up to 13 months after a loved one's passing. This ensures your family has a consistent, compassionate resource to lean on as you navigate the difficult months ahead.
This kind of long-term support is becoming more essential than ever as a society. We're finally starting to truly recognize the importance of mental health during the grieving process, helping families find the compassionate care they deserve.
How to Access Our Grief Support Services
Getting help from our grief counseling for families is a straightforward and gentle process. If your loved one received care from our team, our bereavement coordinators will proactively reach out to you and offer support. Of course, you are always welcome to contact us directly at any time to connect with our compassionate team.
Our goal is simple: to remove any barriers and make it easy for families to get the help they need, right here in the communities we've been serving for decades. This integrated approach to healing is central to our philosophy. To see how this fits into our broader services, you can learn more about our complete approach to hospice care.
We are here to support your family every step of the way.
Frequently Asked Questions About Family Grief Counseling
Deciding to look for support is a big step, and it's completely normal to have questions. We've put together some straightforward, reassuring answers to the things families ask us about most when considering grief counseling. Our hope is to give you the clarity you need to feel confident as you move toward healing.
Every family's path through grief is different. Let's walk through some of the practical and emotional parts of starting counseling, so you can get a better feel for what to expect.
1. Is grief counseling only for a crisis?
No, not at all. While counseling is a lifeline during a crisis, it’s just as powerful as a proactive tool to improve communication and build resilience. The right time to seek support is simply when you feel your family needs it.
2. How can we get our teenager to participate?
Getting a teenager on board can be a challenge. Our counselors know how to create a non-judgmental space where teens feel heard, not forced to talk. Framing it as a way for the family to get stronger together often helps.
3. What if some family members are resistant to counseling?
It’s incredibly common for some family members to be hesitant. Suggesting one introductory session, with no pressure to commit, can make a difference. Our team has experience navigating these delicate family dynamics with patience and compassion.
4. How long does family grief counseling last?
There’s no set timeline. The length of counseling depends entirely on your family’s unique needs and healing process. As part of our deep commitment to the community, Central Coast VNA & Hospice makes bereavement services available for up to 13 months after a loved one on our hospice service passes away.
5. Is this type of counseling affordable?
As a nonprofit organization, Central Coast VNA & Hospice provides bereavement support to the families of our hospice patients as a core part of our mission-driven care. We are committed to making sure compassionate, professional support is accessible to those who need it in Monterey County, San Benito County, Santa Cruz County, and South Santa Clara County. We encourage families to contact us today to learn about the support available.
6. What kind of professionals provide this counseling?
At Central Coast VNA & Hospice, grief counseling and bereavement support are provided by our specially trained Chaplains and Medical Social Workers. These compassionate professionals are skilled in guiding families through the complexities of loss and helping them find a path toward healing together.
Walking through grief is one of the hardest things a family can do, but you don’t have to do it by yourselves. The compassionate team at Central Coast VNA & Hospice is here to offer professional guidance and a supportive presence every step of the way. To learn more about our comprehensive continuum of care, from home health to hospice care, please contact us today.
Finding Grief Support Groups Near Me: A Guide to Local and Online Resources
Navigating loss is a deeply personal journey, and finding the right support can make a significant difference. The path through grief is unique for everyone. However, connection with others who understand can provide comfort, validation, and a sense of community. This guide is designed to help you find the best grief support groups near me, whether you prefer in-person meetings, online communities, or specialized programs.
This resource simplifies the search by compiling a comprehensive list of reputable organizations. We will explore each option in detail, providing practical information to help you make an informed choice. As a nonprofit healthcare provider with over 74 years of service to the Central Coast, Central Coast VNA & Hospice understands the importance of compassionate support during difficult times.
As part of navigating loss, many individuals also seek ways to commemorate their loved ones. If you are considering this, you can find meaningful memorial plaque wording examples for a lasting tribute. Our primary goal, however, is to connect you with immediate support systems that honor your unique journey toward healing.
1. Bereavement & Grief Counseling by Central Coast VNA & Hospice
Central Coast VNA & Hospice (CCVNA) offers Bereavement & Grief Counseling services that are deeply integrated and compassionate. This program is an exceptional starting point for anyone in Monterey County, San Benito County, Santa Cruz County, or South Santa Clara County searching for “grief support groups near me.” It stands out by embedding support within a trusted, nonprofit healthcare framework that has served the community for over 74 years.
The program’s core strength lies in its flexible and comprehensive approach. It recognizes that grief is a highly personal journey. CCVNA offers multiple avenues for support to meet individuals where they are.
Key Strengths and Features
CCVNA’s model provides a holistic support system delivered by a dedicated team. This team includes professionals like Registered Nurses, Chaplains, and Hospice Aides who care for the whole person.
- Hybrid Support Model: Participants can choose between in-person and virtual 'New Beginnings' support groups. This flexibility ensures accessibility for those with mobility or transportation challenges.
- Individualized Counseling: For those who prefer a one-on-one setting, personalized grief counseling is available. This allows for focused guidance tailored to unique circumstances.
- Integrated Healthcare Continuum: A key differentiator is its connection to CCVNA’s broader services. Support is seamlessly linked with our home health, palliative, and hospice care, providing continuous emotional and practical assistance.
- Trusted, Nonprofit Foundation: As a mission-driven organization, the focus is entirely on community well-being, not profit. This ensures a safe, respectful, and compassionate environment for all participants.
Practical Considerations
These services are primarily available to residents of California’s Central Coast. While virtual options offer flexibility, the in-person support and integrated care are geographically specific. To get started, visit the website for the most current meeting schedules and contact information. You can learn more about their available Bereavement and Grief Support Groups.
- Website: https://ccvna.com/bereavement-grief-counseling-monterey/
- Format: In-person and virtual groups, plus individual counseling.
- Access: Services are localized to the Central Coast of California (Monterey, San Benito, Santa Cruz, and South Santa Clara Counties).
2. GriefShare
GriefShare offers a distinctly structured approach to bereavement support. It is an excellent choice for individuals who benefit from a clear, curriculum-based path. Its nationwide network hosts groups that follow a consistent 13-week program, often in local churches.
The program is designed to be comprehensive. It integrates video seminars with grief experts, supportive group discussions, and personal workbook exercises for reflection.

What to Expect and How to Use It
GriefShare combines expert-led content with peer support. Each session focuses on a specific topic relevant to the grief journey. To find a group, use the "Find a Group" tool on their website by entering your city or zip code. Most groups charge a small one-time fee, typically around $20, which covers the cost of a personal workbook.
Pros and Cons
- Pros: The structured 13-week curriculum provides a clear roadmap. Its nationwide availability makes it one of the most accessible in-person options.
- Cons: The faith-based, Christian-oriented perspective may not be suitable for everyone. The 13-week commitment can be a challenge for some schedules.
Website: https://www.griefshare.org/
3. The Compassionate Friends
The Compassionate Friends provides highly specialized support for a uniquely painful type of loss: the death of a child. This focus makes it an invaluable resource for parents, grandparents, and siblings. The organization offers a robust nationwide network of local chapters.
This network extends beyond in-person meetings. It includes a strong online presence with private Facebook groups and virtual support communities, ensuring accessibility for everyone.
What to Expect and How to Use It
The Compassionate Friends is a peer-led organization, meaning meetings are facilitated by bereaved parents. To locate support, the website’s "Find Support" tool allows you to search for grief support groups near me by state or zip code. All meetings and online resources are offered free of charge.
Pros and Cons
- Pros: The specific focus on child loss creates a uniquely safe space. Support is available for the entire family, including siblings and grandparents.
- Cons: Its specialization means it is not a resource for other types of losses. The peer-led model may not be ideal for those seeking professional, therapist-led counseling.
Website: https://www.compassionatefriends.org/
4. Hospice Foundation of America
The Hospice Foundation of America (HFA) serves as a vital educational resource and directory. It is a powerful starting point for anyone seeking grief support. HFA provides a broad, comprehensive look at bereavement care, connecting individuals with various local resources.
HFA’s strength lies in its dual focus on direct support and grief education. The organization offers an extensive library of articles, books, and webinars that help individuals understand loss.
What to Expect and How to Use It
The HFA website is like a well-curated library of grief resources. To find help, you can navigate to their "Grief & Loss" section, which features a directory for finding grief support groups near me. Because the groups listed are independent, their formats and costs vary. The site is completely free to use.
Pros and Cons
- Pros: The comprehensive directory provides access to a wide variety of local groups. Its extensive educational materials are excellent for learning about the grieving process.
- Cons: The platform acts as a directory, so you must research and contact individual groups yourself. The quality of support can vary between listed organizations.
For those in Monterey County and surrounding areas, local providers like Central Coast VNA & Hospice can offer more direct, hands-on support to complement the resources found through HFA.
Website: https://hospicefoundation.org/Grief-%281%29/Support-Groups
5. HealGrief
HealGrief functions as a comprehensive digital hub connecting individuals with a wide array of grief support resources. It excels by offering an interactive and user-friendly directory. This includes everything from virtual support groups to educational articles.
This approach ensures that whether you need immediate virtual connection or local in-person meetings, you can find it in one place. Its modern interface simplifies the search for help during an often overwhelming time.
What to Expect and How to Use It
HealGrief stands out with its interactive map, a key feature for those searching for grief support groups near me. By entering your location, you can visually explore local resources. The platform also hosts its own virtual support groups, providing immediate connection. Access to the directory and most resources is completely free.
Pros and Cons
- Pros: The user-friendly interface and interactive map make finding local help straightforward. It offers a diverse mix of support, from virtual groups to articles.
- Cons: The availability of hyper-local resources can vary by region. The sheer volume of options might feel overwhelming to some users initially.
For those on the Central Coast, organizations like Central Coast VNA & Hospice provide dedicated local support that complements the broad resources found on platforms like HealGrief.
Website: https://healgrief.org/grief-support-resources/
6. The Dinner Party
The Dinner Party redefines grief support for a younger generation. It is designed specifically for 20-, 30-, and 40-somethings who have experienced the death of a close loved one. This unique model fosters candid conversations about loss among peers navigating similar life stages.
The platform’s core philosophy is that healing can happen through peer connection in a comfortable, informal environment. The emphasis is on lived experience rather than expert guidance.
What to Expect and How to Use It
Joining The Dinner Party involves filling out an application on their website to be matched with a local or virtual table. Tables are self-organized and peer-led, gathering for potluck-style dinners. To find grief support groups near me through their platform, you sign up and wait to be connected with a host in your area.
Pros and Cons
- Pros: The peer-to-peer model is highly relatable for young adults. Its informal, dinner-party format creates a relaxed atmosphere.
- Cons: It is specifically for young adults, so it is not a fit for all age groups. Availability can be limited in certain geographic areas.
Website: https://www.thedinnerparty.org/
7. Tragedy Assistance Program for Survivors (TAPS)
TAPS provides essential, specialized support for those grieving a military service member. The organization offers peer-based emotional support and dedicated programs tailored to the challenges faced by military families. This focus creates a deeply understanding and safe environment for healing.
The program's strength lies in its multi-layered approach. This includes a 24/7 National Military Survivor Helpline, a peer mentor program, and national seminars.
What to Expect and How to Use It
TAPS is entirely free for military survivors. The first step is often calling the 24/7 helpline or visiting the website to request a peer mentor. For in-person connections, you can search for TAPS Care Groups and events held across the country.
Pros and Cons
- Pros: Highly specialized support for the unique grief of military families. The 24/7 helpline offers immediate assistance. All services are offered at no cost.
- Cons: Services are exclusively for those grieving a military-related death. It is not a suitable resource for the general public.
For veterans and their families on the Central Coast, organizations like Central Coast VNA & Hospice provide compassionate care that honors military service. Discover more on the community services page.
Website: https://www.taps.org/
8. Emotions Anonymous
Emotions Anonymous (EA) offers a familiar and effective 12-step program. It is designed to help individuals achieve better emotional health, including coping with grief. This fellowship provides a safe space where members can share experiences.
The program's strength lies in its focus on emotional well-being as a whole. This can be helpful for individuals whose bereavement triggers a wide range of emotions.
What to Expect and How to Use It
Emotions Anonymous meetings are built on anonymity and mutual respect. To find a group, visit their website and use the "Find a Meeting" feature. There are no fees or dues required for membership.
Pros and Cons
- Pros: The structured 12-step program offers a proven system for emotional management. Meetings are widely available, and there are no fees.
- Cons: The 12-step model includes a spiritual component that may not align with everyone's beliefs. It is a peer-led support system, not a substitute for professional therapy.
Website: https://emotionsanonymous.org/
9. Lifestance Health
Lifestance Health offers a clinical, therapy-based framework for grief support. It is ideal for individuals seeking guidance from licensed mental health professionals. Lifestance provides access to credentialed counselors and therapists who specialize in bereavement.
This model is particularly beneficial for those experiencing complex or prolonged grief. The ability to choose between individual sessions and group settings allows for a personalized care plan.
What to Expect and How to Use It
Lifestance Health operates like a traditional healthcare provider. After an initial consultation, you will be matched with a therapist who fits your specific needs. To get started, use their website's provider search tool. Lifestance accepts most major insurance plans.
Pros and Cons
- Pros: Sessions are led by licensed mental health professionals. They offer flexible formats, including in-person and virtual therapy. Accepting insurance makes counseling more financially accessible.
- Cons: The availability of specific grief groups can vary by location. For those without adequate insurance, the cost can be a barrier.
Website: https://lifestance.com/services/grief-counseling/
10. Wellabe Grief Support Lookup
Wellabe Grief Support Lookup acts as a powerful and user-friendly directory. It connects individuals to bereavement services across the United States. It simplifies the initial search process for those navigating loss.
The platform's strength lies in its extensive listings and filtering capabilities. It allows you to quickly find both in-person and virtual groups, counseling, and other resources.
What to Expect and How to Use It
Using Wellabe is straightforward. Visit the website and use the search tool to enter your location, which pulls up a list of local resources. Its filters help you narrow your search for grief support groups near me. Since it is a directory, the platform is completely free to use.
Pros and Cons
- Pros: The platform is free, easy to navigate, and offers diverse support options. Its regularly updated listings ensure the information is reliable.
- Cons: As a directory, it requires you to do the follow-up work of contacting organizations. The quality of listed services can vary by location.
Website: https://www.wellabe.com/grief-support-lookup
11. Grouport Therapy
Grouport Therapy modernizes grief support by moving professionally-led group therapy online. It provides access to licensed therapists who guide each session. This model is ideal for those who want professional guidance combined with the shared experience of a support group.
This platform offers a vital service for individuals who face barriers to in-person meetings. It blends the convenience of telehealth with the connection that comes from sharing a journey.
What to Expect and How to Use It
Grouport Therapy delivers a clinical approach. To begin, you complete a brief online questionnaire and get matched with a suitable group. This makes finding professional grief support groups near me an immediate possibility, regardless of location. The service is fee-based but may be covered by some insurance plans.
Pros and Cons
- Pros: Sessions are led by licensed therapists. The online format provides excellent accessibility and convenience.
- Cons: Services are only available in select states. As a therapeutic service, it involves fees, and insurance coverage can vary.
For those seeking comprehensive support, organizations like Central Coast VNA & Hospice provide a continuum of services that can work alongside therapeutic options.
Website: https://www.grouporttherapy.com/
12. Carson's Village
Carson's Village acts as a compassionate and practical starting point for families. It functions as a resource hub, helping you find and vet the right support for your needs. Its user-friendly design simplifies what can be an overwhelming process.
The platform's strength lies in its educational approach. It offers clear guidance on what to look for in a support group.
What to Expect and How to Use It
Carson's Village excels as an informational aggregator. To begin, navigate to their "Finding a Grief Support Group" page and use the interactive map. Clicking on your state reveals a curated list of organizations. All resources on the site are provided completely free of charge.
Pros and Cons
- Pros: The interactive map is an intuitive tool for finding local options. It provides excellent educational content on how to choose a group. Access is completely free.
- Cons: It is a directory, not a direct provider. You will need to do additional research and contact the listed organizations yourself.
Website: https://carsonsvillage.org/resource/finding-a-grief-support-group/
Choosing the Right Grief Support For You
Finding the right support is a crucial and empowering step toward healing. Your search for "grief support groups near me" is often the first, most courageous act, and it's one you do not have to take alone. As you review the options, think about what kind of environment would feel most comforting.
Consider these factors when making your choice:
- Type of Loss: Are you grieving a spouse, parent, or child? Specialized groups like The Compassionate Friends offer a level of understanding that can be deeply validating.
- Format: Do you prefer in-person meetings in Monterey County? Or does the flexibility of an online group like Grouport Therapy better suit your needs?
- Structure: Do you thrive with a structured program like GriefShare? Or do you prefer an informal, peer-led discussion like The Dinner Party?
There is no "one-size-fits-all" solution. The best resource is the one that aligns with your emotional needs and provides a safe space for you to express your feelings without judgment.
Your Path Forward with Local, Compassionate Care
As a cornerstone of the Central Coast for over 74 years, Central Coast VNA & Hospice understands that comprehensive care extends beyond medical treatment. Our mission-driven, nonprofit approach ensures that support continues for families even after a patient has passed. Our bereavement programs are a vital part of our continuum of care, offering a gentle landing place for those navigating the complexities of loss.
We are here not just for our patients, but for the entire community we serve across Monterey, San Benito, Santa Cruz, and South Santa Clara Counties. At Central Coast VNA & Hospice, our professional team—including Registered Nurses, Chaplains, and Hospice Aides—is dedicated to supporting you with expertise and compassion.
If you or someone you know is coping with loss, our compassionate team is here to help. Contact us today to learn more about our local grief support services and how we can support you.
Frequently Asked Questions (FAQs)
1. What is the difference between grief counseling and a support group?
Grief counseling is typically one-on-one therapy led by a licensed mental health professional. A support group is a gathering of peers with shared experiences, often facilitated by a trained peer or professional, to offer mutual comfort and validation. Central Coast VNA & Hospice offers both individual counseling and group support.
2. How do I know if I'm ready for a grief support group?
There is no "right" time, but if you feel isolated in your grief and wish to connect with others who understand, it may be a good time to explore a group. Many people find comfort in sharing their story and hearing from others who are navigating a similar path.
3. Are there free grief support groups available near me?
Yes, many nonprofit and community-based organizations offer free grief support groups. Resources like The Compassionate Friends, TAPS, and many groups listed on directories like HealGrief and Wellabe are available at no cost.
4. Can I join a virtual grief support group if I don't live on the Central Coast?
Absolutely. Many organizations, such as Grouport Therapy and The Dinner Party, offer virtual groups that allow you to connect with others from anywhere. While CCVNA's services are focused on the Central Coast, these national platforms provide excellent online alternatives.
5. How does CCVNA’s nonprofit status benefit its grief support services?
As a mission-driven nonprofit, Central Coast VNA & Hospice reinvests all resources back into patient care and community programs. This means our primary focus is on providing high-quality, compassionate support to families in Monterey County and surrounding areas, rather than on generating profit.
6. How long does grief last, and how long should I attend a support group?
Grief is a highly individual process with no set timeline. Some people attend a support group for a specific period, like a 13-week program, while others find comfort in ongoing monthly meetings. The goal is to use the support for as long as it feels helpful to you. According to the National Hospice and Palliative Care Organization (NHPCO), providing bereavement support is a core component of hospice care, recognizing that grief is a long-term journey (NHPCO, 2021).
7. How can Central Coast VNA & Hospice help my family?
Central Coast VNA & Hospice provides a full continuum of care, from home health and palliative services to hospice care. Our support extends to the entire family, offering bereavement counseling and support groups to help loved ones navigate loss in our service areas of Monterey, San Benito, Santa Cruz, and South Santa Clara Counties.
Respite Care for Family Caregivers: A Guide to Support & Relief
When you are a family caregiver, your role is built on profound love and dedication. It is also one of the most demanding jobs anyone can have. That is where respite care for family caregivers comes in; it is a professional, short-term break designed to give you a chance to breathe.
Think of it as a strategic timeout in a marathon. It’s not about quitting; it’s about resting, recharging, and returning to your loved one with renewed energy and focus.
Why Respite Care Is Essential for Family Caregivers

Taking on the responsibility of caring for a loved one is a deeply meaningful commitment. The constant physical and emotional demands can lead to exhaustion and burnout, which ultimately affects your own health and well-being. This is why respite care is not a luxury; it’s a vital part of any sustainable, long-term care plan.
Respite care is a partnership. It ensures your loved one continues to receive excellent support from a qualified professional while you take much-needed time for yourself. This could mean finally getting to a doctor's appointment, running errands without watching the clock, or simply resting.
To help clarify what respite care entails, here is a quick look at its core components.
Understanding Respite Care at a Glance
| Concept | Description |
|---|---|
| Purpose | To provide a planned, short-term break for family caregivers. |
| Primary Benefit | Prevents caregiver burnout, reduces stress, and improves the well-being of both the caregiver and the care recipient. |
| For the Loved One | Ensures continuous, professional care in a safe and supportive environment from skilled clinicians. |
| Providers | Typically offered by home health agencies, adult day centers, or residential facilities. |
Ultimately, respite care is about creating a healthier, more balanced caregiving dynamic for everyone involved.
The Growing Need for Caregiver Support
The role of the family caregiver is more common than ever. Recent data reveals there are now 63 million adults serving as unpaid caregivers in the United States, a significant increase from a decade ago. Despite this, many do not seek the professional help they need.
While 39% of caregivers believe respite care would be helpful, only 13% actually use these services, often due to concerns about trust or cost. Learn more about the challenges facing modern caregivers on homehealthcarenews.com.
This gap highlights a critical need. Prioritizing your own well-being through respite is not selfish; it’s essential for preventing burnout and allows you to continue providing the best possible care for your loved one.
A Partner You Can Trust on the Central Coast
Choosing a respite provider you can trust is the most important step. For over 74 years, Central Coast VNA & Hospice has been a steadfast, nonprofit partner for families across Monterey County, San Benito County, Santa Cruz County, and South Santa Clara County. Our mission is rooted in providing compassionate, expert care that supports both patients and their families.
As a mission-driven organization, we understand the immense pressures family caregivers face. Our team of skilled professionals, including Registered Nurses and Hospice Aides, delivers care with the same dignity and respect you provide. We work with you to create a respite plan that brings peace of mind, knowing your loved one is in capable and caring hands.
Ready to find support? Contact us today to learn how our respite services can help you and your family.
Recognizing the Signs You Need a Break

It’s surprisingly easy to become so wrapped up in your loved one’s needs that you miss the warning signs in yourself. Seeing the subtle signals of burnout is the first, most crucial step toward preventing it from taking over. Think of these signs not as failures, but as your body’s way of asking for help.
Taking care of someone is a massive responsibility, and it's a role more people are stepping into every year. According to the Population Reference Bureau, the number of family caregivers helping older adults with daily life jumped by 32% in just a decade—from 18.2 million in 2011 to 24.1 million in 2022 (PRB, 2023). You can read more about trends in family caregiving on prb.org.
These feelings are incredibly common, but they're also clear indicators that you need to make your own well-being a priority. Acknowledging them is not weakness; it’s a sign of real strength.
Physical and Emotional Indicators of Burnout
Caregiver stress has a way of creeping up on you. The changes are often gradual, so you might not even notice them at first, but they can build until they feel overwhelming.
One of the most common signs is a deep, persistent exhaustion—both emotional and physical. This isn't just feeling tired after a long day. It is a bone-deep weariness that a full night's sleep cannot seem to touch.
Another tell-tale sign is finding yourself more irritable or impatient than usual. This shift in mood is often a direct result of chronic stress.
Changes in Social Behavior and Personal Health
When burnout sets in, you might find yourself pulling away from the people and activities you used to love. Withdrawing from your social life is a common coping mechanism, but it often leads to isolation and loneliness.
Keep an eye out for these shifts in your behavior:
- Declining social invitations more often than you accept them.
- Losing interest in hobbies or passions that used to bring you joy.
- Feeling disconnected from friends and family, even when you’re together.
Perhaps the most telling sign is when you start neglecting your own health. This can look like skipping your own doctor's appointments, eating poorly, or letting your exercise routine slide. When your focus is entirely on someone else, it is all too easy for your own needs to fall to the bottom of the list.
If any of this sounds familiar, it is a clear signal that you need a break. Looking into respite care for family caregivers is a proactive step you can take to protect your health so you can continue providing the best possible support. For more guidance, you might find these tips for family caregivers from our team helpful.
Exploring Different Types of Respite Care

When you start looking into respite care for family caregivers, you’ll find that support is not a one-size-fits-all solution. It is more like a menu of options you can tailor to your family’s unique situation, your loved one's comfort, and the kind of break you truly need.
Knowing what’s available helps you make a choice that gives you real peace of mind. Whether you need a few hours to handle errands or a full week to genuinely unplug and recharge, there is a form of respite care that can fit the bill.
In-Home Respite Care
In-home respite care is easily one of the most popular and flexible choices. It’s exactly what it sounds like: a professional comes right to your home. This allows your loved one to stay in a familiar, comfortable space, which is incredibly reassuring.
A skilled professional, like a Hospice Aide from a trusted agency like Central Coast VNA & Hospice, can step in to help with a whole host of needs. The care is personalized, fitting right into your loved one’s existing routine.
This type of support often covers:
- Personal Care: Help with bathing, getting dressed, and grooming.
- Companionship: Simply being there for a chat, reading aloud, or doing light activities together.
- Meal Preparation: Making sure your loved one gets nutritious meals.
- Medication Reminders: Keeping them on track with their medication schedule.
This is a fantastic option for caregivers who need regular, scheduled breaks.
Out-of-Home Respite Options
For some families, a change of scenery is a welcome thing. Out-of-home respite care provides safe, supervised, and engaging environments that can offer new opportunities for social connection.
There are two main types of out-of-home respite:
- Adult Day Centers: Think of these as community-based group programs with a planned schedule. They offer a great chance for your loved one to socialize and receive necessary health services.
- Residential Facilities: When you need a longer break, you can arrange a short-term stay for your loved one at a place like an assisted living facility or a nursing home. This is often called "in-patient respite" and is a key part of the Medicare Hospice Benefit, covering up to five consecutive days of care.
Both of these give caregivers a more substantial break, all while knowing their loved one is in a professional and safe setting. For families navigating more complex health issues, learning about the benefits of palliative care can also show how these services all fit together.
Flexible Durations for Every Need
Respite care is built to be flexible. Breaks can last just a few hours or go on for several weeks—whatever you need. A couple of hours each week might be all it takes to make it to your own appointments or meet a friend for coffee.
An overnight stay can provide a full 24-hour period to catch up on much-needed sleep. Longer stretches, like a weekend or an entire week, open the door for a real vacation or dedicated time to focus on other family priorities. Here at Central Coast VNA & Hospice, we help families in Monterey County and San Benito County find the right type of care to restore balance.
How to Access and Fund Respite Care
Figuring out the logistics of respite care—how to find it, how to pay for it—can feel like taking on a second job. But with a clear roadmap, you can find the break you need without all the guesswork.
Thankfully, you have more options than you might think. From government programs to private insurance, there are several ways to cover the expense of respite care for family caregivers. The trick is figuring out which path makes the most sense for your family.
Navigating Funding and Eligibility
Talking about money and insurance can be draining, but breaking it down into smaller pieces makes it much more manageable. Each funding source has its own set of rules, so a little bit of homework upfront goes a long way.
Here are the most common ways families fund respite care:
- Medicare: If your loved one is already receiving hospice care, the Medicare Hospice Benefit can be a huge help. It covers temporary in-patient respite care in a Medicare-approved facility for up to five consecutive days.
- Medicaid (Medi-Cal in California): Many states offer Medicaid waivers designed to help low-income individuals access services like respite care. These waivers can often be used for in-home help or short-term stays in a care facility.
- Long-Term Care Insurance: Smart long-term care insurance planning is a game-changer for many families. If your loved one has a policy, many plans include a specific benefit for respite services.
- Private Pay: For families who are able, paying directly for services offers the most freedom. You can choose the exact type and amount of care you want without having to navigate strict eligibility rules.
Thinking about your options? This side-by-side look at in-home versus facility-based respite care can help you weigh the pros and cons.
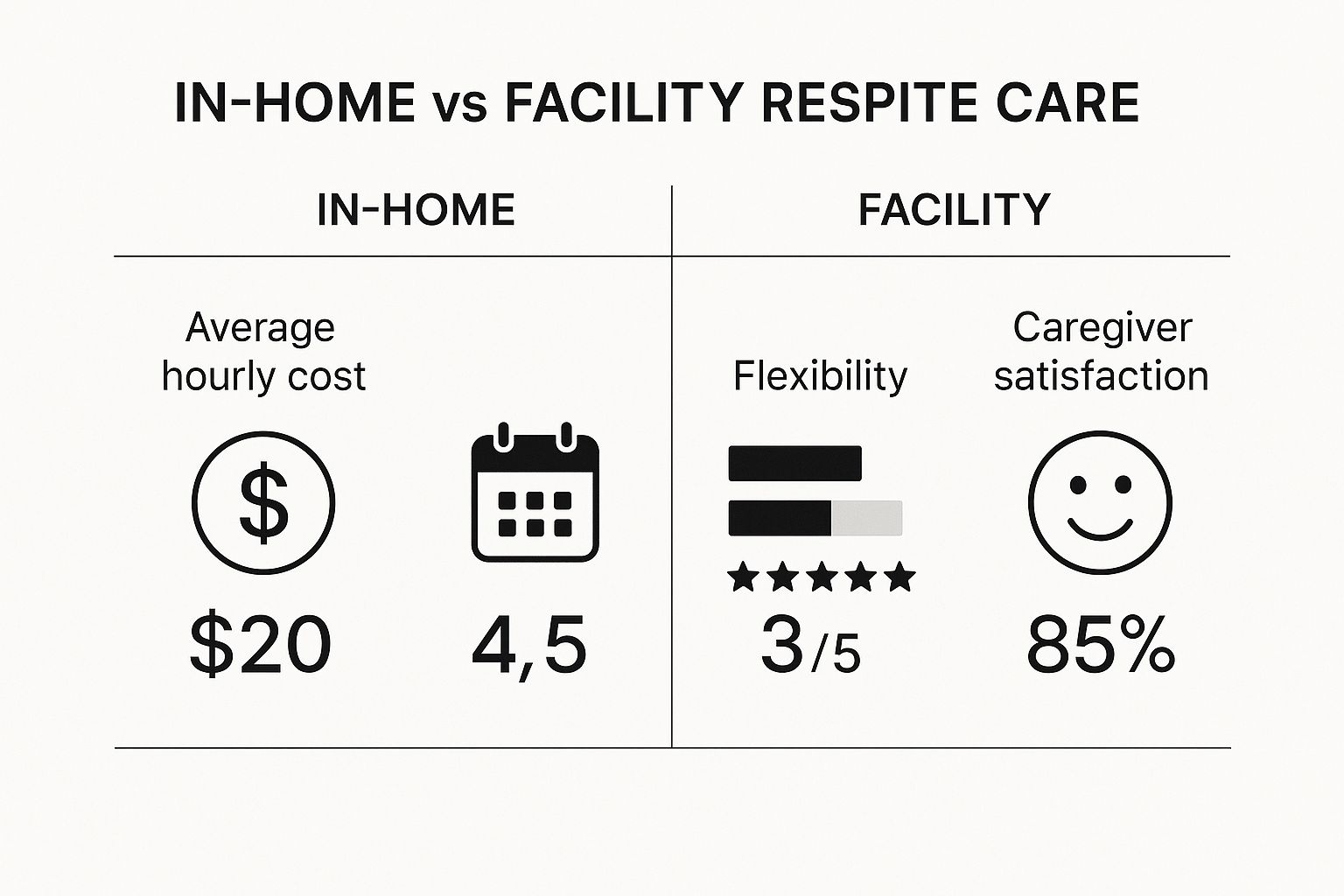
As you can see, both choices have unique strengths. In-home care might be more flexible and familiar, while a facility can offer a different level of support. It all comes down to what fits your family’s needs and budget.
Comparing Respite Care Funding Options
To make things even clearer, here’s a table breaking down the key funding sources.
| Funding Source | Who Might Be Eligible | Key Considerations |
|---|---|---|
| Medicare | Hospice patients needing a short-term break for their primary caregiver. | Limited to 5 consecutive days in an approved facility. |
| Medicaid (Medi-Cal) | Low-income seniors and individuals with disabilities, via state waivers. | Eligibility is state-specific and based on income/assets. |
| Long-Term Care Insurance | Individuals with an active long-term care policy. | Coverage and benefits vary widely by policy. |
| Private Pay | Anyone who chooses to pay for services out-of-pocket. | Offers maximum flexibility but requires personal financial resources. |
Each path has its own map, but knowing the landscape helps you choose the right direction for your family.
Finding a Reputable Local Provider
Once you have a handle on funding, the next big step is finding a provider you can truly trust. Especially when searching for respite care in Monterey County, look for an organization with deep roots in the community and a reputation built on compassionate, professional care.
When you work with a trusted, local nonprofit like Central Coast VNA & Hospice, you are not just hiring a service. You are partnering with a team that is accountable to the community it serves. A local provider understands the unique challenges and resources in the area and can connect you with a whole network of support.
For over 74 years, we have been a part of the Central Coast community, offering a full continuum of care that includes skilled home health care services, palliative care, and hospice. Our team of Registered Nurses, Chaplains, and Hospice Aides is here for families throughout Monterey, San Benito, Santa Cruz, and South Santa Clara counties.
If you’re ready to find a respite solution that works for you, please reach out. We are here to help you navigate the journey.
Preparing for a Successful Respite Experience
To really get the most out of respite care for family caregivers, a little bit of prep work can make all the difference. Taking a few simple steps beforehand ensures you get true peace of mind and your loved one has a smooth transition. It is all about setting everyone up for success so the experience feels comfortable and confident from the start.
The main goal is to make the handover feel seamless. When you provide clear information and talk to your loved one about what to expect, you build a foundation of trust with the professional care provider. This simple act of preparation can turn what might be an anxious time into a positive, reassuring experience.
Creating a Detailed Care Summary
Think of this as the "quick start guide" for your loved one. A simple, organized summary helps the respite provider—like a Hospice Aide from Central Coast VNA & Hospice—get up to speed on your loved one’s needs and preferences right away. You do not have to write a novel; just cover the essentials.
Make sure your summary includes:
- Medication Schedule: List every medication, the dosage, and the exact time it needs to be given. Be sure to note any special instructions, like whether a pill needs to be taken with food.
- Dietary Needs: Detail any food allergies, specific dietary restrictions (like low-sodium or soft foods), and even a few favorite snacks or drinks.
- Daily Routines: Outline their typical day. What time do they wake up? When are meals? Is there a regular nap time? Familiar routines provide a powerful sense of comfort.
- Emergency Contacts: Keep a clear list of key phone numbers. Include your own, another family member's, and the primary doctor's number.
This simple document is one of the most powerful tools you have for ensuring a great respite break. It gives the professional the information they need to provide truly personalized and compassionate support.
Emotionally Preparing Your Loved One
Change can be unsettling, especially for someone who finds comfort in a consistent routine. Talking with your loved one about the upcoming respite break ahead of time can make a world of difference. It helps to frame it positively—as a chance for them to have a nice visit with a new, friendly person while you take a little break.
If you can, try to arrange a brief meet-and-greet between your loved one and the respite professional before the first official session. This simple step can turn a stranger into a familiar face, which can do wonders to reduce any anxiety. Most importantly, reassure them that you are taking this time for yourself so you can come back as a better, more energized caregiver for them.
Making the Most of Your Break
Your time off is precious. The temptation to spend every free moment catching up on chores or running errands is strong, but try to resist. This is your chance to focus on your own well-being. A break is not really a break if you just switch from one to-do list to another.
Plan to do things that will actually restore you. Consider activities like:
- Connecting with friends over a long, unhurried lunch.
- Spending time in nature, whether it's a walk on the beach or just sitting in a local park.
- Picking up a hobby you’ve had to put on the back burner.
- Simply resting with a good book and a cup of tea, with zero interruptions.
Central Coast VNA & Hospice is here to help families across Monterey and San Benito counties get the support they need. Our continuum of care, including our specialized home care services, is designed to support the entire family. We want to make sure you have the resources to care for yourself, too.
How CCVNA Supports Families on the Central Coast
When you’re caring for a loved one, you know it’s a job that touches every part of your life. At Central Coast VNA & Hospice, we understand that. For over 74 years, our nonprofit team has been more than just a healthcare provider; we have become a trusted partner for families across Monterey, San Benito, Santa Cruz, and South Santa Clara Counties.
We see respite care for family caregivers as a core part of our mission. It’s not an add-on service—it’s a fundamental piece of our promise to deliver compassionate, holistic support that wraps around the entire family. Think of it as a built-in support system, designed to give you the strength and space you need at every step of your journey.
A Continuum of Compassionate Support
As your loved one's health needs change, the support you receive should change right along with them. Our model is built for that flexibility. We weave respite care into each of our core services, from home health to palliative care to hospice, so you can get the break you need, right when you need it most.
- Home Health: While our skilled Registered Nurses and therapists help your loved one recover from surgery or manage a new diagnosis through our skilled home health care services, we can provide respite to lift the weight of daily caregiving.
- Palliative Care: Our focus here is on improving quality of life and managing difficult symptoms. Respite gives you a chance to recharge, so you have the energy to be present and supportive.
- Hospice Care: Respite is a formal benefit included in hospice. Our dedicated team of Chaplains, Hospice Aides, and nurses provides expert, gentle care, giving you complete peace of mind to step away. You can learn more about our Medicare-certified hospice care services and how this vital support works for families.
Caring for the caregiver is just as important as caring for the patient. A rested, supported family caregiver is better equipped to handle the emotional and physical demands of their role, which leads to better outcomes for everyone.
Your Local, Nonprofit Partner in Care
Choosing a respite provider means placing your trust in someone else's hands—we understand how significant that is. As a community-based nonprofit, our only mission is to serve the families of the Central Coast with integrity and heart.
Our professional team lives here. We are your neighbors, and we are committed to providing the same dignified, expert care we would want for our own families.
If you’re a family caregiver feeling the strain of your responsibilities, you are not alone. Central Coast VNA & Hospice is here to help you find balance.
Frequently Asked Questions About Respite Care
Even after you understand what respite care is and how to find it, it's completely normal to have more questions. Making decisions about a loved one’s care is a huge responsibility. You want to feel confident you are making the right choice, and that comes from getting all the information you can.
To help with that, our team at Central Coast VNA & Hospice put together answers to the questions we hear most often from families just like yours. Our goal is to give you direct, compassionate answers that clear up any doubts and help you take the next step.
Will my loved one feel abandoned if I use respite care?
This is one of the most common worries we hear, and it comes straight from the heart. The best way to think about respite care is as something you are doing for both of you. It’s not about abandoning them; it’s about refueling so you can be a better, more patient, and more present caregiver for the long haul.
Gently explaining that a friendly, professional helper will be visiting can make a world of difference. An introductory meeting before the first real session also helps ease everyone into the new routine. Many families are pleasantly surprised to find their loved ones actually enjoy the new company and a change of pace.
How do I know I can trust the respite provider?
Trust is everything. The surest way to build that trust is by working with an established, reputable agency with deep roots in the community, like Central Coast VNA & Hospice. With over 74 years of service here on the Central Coast, our reputation is built on accountability and genuine compassion.
When you're vetting a potential provider, ask specific questions about their team. How do they screen professional team members like Hospice Aides? What kind of ongoing training do they receive? Choosing a licensed, insured, and nonprofit organization adds another layer of security and peace of mind.
What if my loved one has complex medical needs?
This is where a professional provider truly shines, especially one that is part of a comprehensive agency like CCVNA. Our respite services are an extension of our home health, palliative, and hospice programs. That means our clinical team is trained and comfortable managing a wide range of health challenges.
Before care starts, a Registered Nurse will typically conduct a thorough initial assessment. This visit allows us to create a very detailed and personalized care plan. This plan becomes the playbook for our Hospice Aides, ensuring they are fully prepared to manage medications, assist with mobility, and handle any other specific medical needs safely and competently.
Is respite care only for end-of-life situations?
Absolutely not. While respite is a formal benefit and a key part of hospice care, it’s a service available to any family caregiver who needs support. Your loved one's prognosis or life expectancy does not matter.
Think of it as a proactive tool you can use at any point during a long-term illness, a chronic condition, or even a tough recovery period. The real goal is to prevent caregiver burnout and support the health of the entire family. It is about making caregiving sustainable for the journey, whatever stage you are in.
How often can I use respite care services?
The simple answer is: as often as you need it. The frequency of respite care is incredibly flexible because every family’s situation is different. There is no one-size-fits-all schedule.
Some families just need a few hours a week to run errands or go to a doctor’s appointment. Others might arrange for care over several consecutive days to take a much-needed vacation. A care coordinator from an agency like Central Coast VNA & Hospice can help map out a schedule that works for your family in Monterey County or the surrounding areas.
At Central Coast VNA & Hospice, we are deeply committed to supporting the dedicated family caregivers in our community. If you’re feeling stretched thin, please remember you don’t have to carry this weight all by yourself.
Finding the Right Local Health Care Resources for Seriously Ill Family Members on the Central Coast
When a loved one is seriously ill, navigating the maze of healthcare options can feel overwhelming. Finding the right support is critical, but knowing where to start is often the biggest challenge.
This guide simplifies that process by compiling a detailed list of local health care resources for seriously ill family members on the Central Coast. We have gathered essential information on the most trusted providers in Monterey County, San Benito County, Santa Cruz County, and South Santa Clara County.
Our goal is to provide a clear, practical roadmap to help you make informed decisions with confidence. Whether you need skilled home health nursing, compassionate hospice services, or specialized palliative care, this resource list is designed for you.
1. Central Coast VNA & Hospice (CCVNA)
For families navigating the complexities of serious illness, Central Coast VNA & Hospice (CCVNA) stands out as the premier local health care resource on the Central Coast. For over 74 years, this nonprofit leader has provided an unparalleled continuum of in-home medical services.
This ensures patients receive seamless support as their needs evolve. Their integrated model means a person can transition from home health for recovery, to palliative care for symptom management, and finally to hospice care, all within one trusted organization.
Why CCVNA is Our Featured Choice
CCVNA’s strength lies in its holistic, team-based approach. Rather than just treating a condition, their interdisciplinary teams address the complete well-being of the patient and their family.
These teams include skilled professionals like Registered Nurses, Physical Therapists, Chaplains, and Medical Social Workers. This whole-person focus provides not just medical treatment but also essential emotional, spiritual, and bereavement support that families need.
As a mission-driven nonprofit, CCVNA’s care is always centered on patient need, not profit. They accept Medicare, Medi-Cal, and various private insurances to maximize accessibility for our communities.
Key Strengths & Use Cases
- Integrated Continuum of Care: A patient recovering from surgery can start with home health nursing. If their chronic condition worsens, they can transition to the palliative care team for specialized symptom relief without leaving the CCVNA system. This is a significant benefit, as detailed in their resources that explain the benefits of palliative care at home.
- Holistic Family Support: Beyond patient care, CCVNA offers robust support for loved ones, including counseling and bereavement services, recognizing that a serious illness impacts the entire family unit.
- Deep Community Roots: With a 74-year history serving Monterey, San Benito, Santa Cruz, and South Santa Clara counties, their reputation for compassionate, reliable care is well-established and trusted by local healthcare providers.
Access and Practical Considerations
Accessing services typically requires a physician referral, though the CCVNA team can help coordinate this. It's wise to initiate contact early to ensure timely support.
Their website, ccvna.com, offers clear pathways to learn about each service, understand insurance coverage, and make referrals.
2. Dignity Health – Central Coast Home Health, Hospice, and Infusion Services
Dignity Health offers a comprehensive suite of in-home services designed to support seriously ill family members across the Central Coast. Their website is a primary portal for families to explore skilled nursing, rehabilitative therapies, and hospice care.
The platform clearly outlines the different levels of support available. This helps users match their loved one's specific medical needs with the appropriate services.
Key Features and Use Cases
A standout offering is their in-home infusion service, which allows patients to receive intravenous treatments without visiting a hospital. This is a significant benefit for individuals with mobility challenges.
Families can use the website to find contact information for their specific area and initiate the referral process. This is typically coordinated through a physician.
Practical Considerations
While Dignity Health provides a robust network, service availability can differ between its locations in Arroyo Grande, Santa Maria, and San Luis Obispo. It is crucial to confirm that specific services are offered in your immediate area.
Understanding these distinctions is a key part of the care planning process. You can prepare by learning more about advance care planning on ccvna.com.
Website: Dignity Health Central Coast Home Health & Hospice Services
3. Central Coast Home Health and Hospice
Central Coast Home Health and Hospice provides physician-directed care across San Luis Obispo and Santa Barbara Counties. Their focus is on patients with serious illnesses.
Their website is a straightforward resource for families seeking skilled nursing, rehabilitation, or compassionate end-of-life hospice care at home. It details their scope of services and how their clinicians support a loved one's quality of life.

Key Features and Use Cases
A key strength is their team-based approach, which includes registered nurses, physical therapists, and medical social workers. Families navigating a new diagnosis can see how these roles coordinate a care plan.
The positive patient testimonials on the site offer valuable insight into the quality of care. This makes it a useful touchpoint for families evaluating local options.
Practical Considerations
This provider’s services are specifically limited to San Luis Obispo and Santa Barbara Counties. It's essential to confirm you are within their coverage area before proceeding.
The website serves as the primary contact point to initiate care. Families can prepare by reading a guide to home health care services on ccvna.com.
Website: Central Coast Home Health and Hospice
4. Central Coast VNA & Hospice
With over 74 years of dedicated service, Central Coast VNA & Hospice stands as a cornerstone nonprofit provider of in-home care. Their website is a crucial resource for families seeking skilled home health, palliative care, or hospice services.
It details a holistic care model that addresses not only medical needs but also the social and emotional well-being of seriously ill patients and their loved ones. CCVNA is deeply rooted in the communities of Monterey, San Benito, and Santa Cruz Counties.
Key Features and Use Cases
A defining feature is the integration of Medical Social Workers into their care teams. These professionals help families navigate complex challenges by connecting them to vital community resources.
Families can use the website to understand the scope of in-home therapies available. This includes physical, occupational, and speech therapy, which are essential for rehabilitation at home.
Practical Considerations
As a long-standing nonprofit, CCVNA has a deeply embedded reputation. Access to their services requires a physician’s order, a standard practice for Medicare-covered home health.
Families should note their services are focused on adults and do not include pediatric care. The first step is to consult with the patient's doctor to initiate a referral.
Website: Central Coast VNA & Hospice Home Health Care Services
5. Arosa – Central Coast In-Home Senior Care
Arosa offers personalized in-home care for seniors, focusing on creating compatible matches between clients and professional caregivers. With over two decades of experience, their website is a valuable resource for families seeking non-medical assistance.
The platform details their approach to creating customized care plans. It is a key starting point for those looking for dedicated, one-on-one support for an aging loved one.
Key Features and Use Cases
A standout feature is Arosa's emphasis on client-professional matching, which aims to align personalities, skills, and client needs. This creates a more harmonious care experience.
Families can use the website to understand this process and initiate a consultation. This is ideal when companionship and consistent, personalized support are top priorities.
Practical Considerations
While Arosa provides excellent non-medical support, their services are primarily focused on seniors. It is also important to note that this is private-pay care, not typically covered by Medicare.
Their website is best used for exploring supplementary care options. These can complement skilled medical services from other providers.
Website: Arosa Central Coast In-Home Senior Care
6. Accessible Home Health Care – Central Coast
Accessible Home Health Care offers specialized in-home support with a strong focus on creating customized care plans. Their website is a direct resource for families needing services like dementia care or companion support.
The platform emphasizes flexibility. This makes it a valuable option for those whose needs may change over time.
Key Features and Use Cases
A key advantage is their adaptable scheduling, offering both hourly and live-in care options without requiring long-term contracts. This is especially useful for families managing fluctuating conditions like Alzheimer's.
Users can browse the site to understand the scope of companion and personal care services. Then they can call to schedule a consultation and develop a tailored plan.
Practical Considerations
Accessible Home Health Care's service area may have limitations within the broader Central Coast region. Verifying coverage for your exact location is an important first step.
This agency focuses on non-medical companion care rather than skilled nursing or hospice. It is a complementary resource to other local healthcare providers.
Website: Accessible Home Health Care Central Coast
7. Home Matters Caregiving – Central Coast
Home Matters Caregiving provides specialized, non-medical in-home care. They focus on improving the quality of life for seniors across the Central Coast.
Their website helps families understand the different levels of support available. It is a valuable resource for those caring for a loved one with Alzheimer's, dementia, or other chronic conditions.
Key Features and Use Cases
A key feature is their highly flexible scheduling, which includes 24-hour, overnight, and live-in care options. This adaptability is critical for families whose care needs may change suddenly.
The site allows you to explore these services and request a complimentary assessment. An expert then helps develop a personalized care plan for your family member.
Practical Considerations
While Home Matters excels in providing robust support for seniors, their services are primarily non-medical. They do not extend to pediatric patients.
It is a strong choice for companionship and personal assistance. However, it may need to be supplemented with skilled nursing from other local health care providers.
Website: Home Matters Caregiving – Central Coast
8. Central Coast Senior Services, Inc.
Central Coast Senior Services, Inc. offers specialized in-home care and assisted living placement. They primarily serve families in the Monterey Peninsula and Salinas areas.
Their website is a direct portal for arranging non-medical support, focusing on helping seniors maintain independence at home. It details services like geriatric care management, assistance with daily activities, and companionship.
Key Features and Use Cases
A key feature is their 24-hour availability, ensuring continuous support for individuals with complex needs. This is particularly beneficial for families needing respite care or managing advanced Alzheimer's.
The website allows users to quickly understand the scope of in-home assistance available. They can initiate contact to schedule a consultation for a personalized care plan.
Practical Considerations
Their in-home services are geographically limited to the Monterey Peninsula and Salinas. Families outside this zone will need to seek other options.
Their model is centered on non-medical support, meaning they complement skilled nursing or hospice providers. Families can learn more about options for Monterey senior care services.
Website: Central Coast Senior Services, Inc.
9. Family Caregiver Alliance (FCA)
The Family Caregiver Alliance (FCA) is a national nonprofit that serves as a vital informational lifeline. It supports those caring for seriously ill relatives.
While headquartered in San Francisco, its website offers universally accessible resources. This makes it an essential platform for families on the Central Coast seeking guidance, education, and support.
Key Features and Use Cases
A core strength of the FCA website is its extensive library of educational materials. They cover topics from managing medications to legal and financial planning.
Families can access fact sheets, videos, and webinars at no cost, empowering them with knowledge. The "Family Consultants" feature offers personalized advice via phone or email, providing a direct connection to an expert.
Practical Considerations
The FCA is an informational hub, not a direct provider of in-home medical care. Its value lies in equipping you to manage care and advocate for your loved one.
To get the most from the site, start by exploring their publications relevant to your situation. You can build on this knowledge by exploring further tips for family caregivers at ccvna.com.
Website: Family Caregiver Alliance
10. Program of All-Inclusive Care for the Elderly (PACE)
The Program of All-Inclusive Care for the Elderly (PACE) offers a uniquely holistic medical and social care model. It is designed for frail seniors on the Central Coast.
The national website is an informational gateway for families to understand this comprehensive program. According to the National PACE Association (NPA), over 95% of PACE participants are able to successfully continue living in their community (NPA, n.d.).
Key Features and Use Cases
A core strength of the PACE model is its focus on preventive care to reduce hospitalizations. The interdisciplinary team addresses both the medical and social determinants of health.
For families seeking a single point of contact for nearly all care needs, PACE provides a simplified process. It integrates services from primary care to transportation and meals.
Practical Considerations
The primary limitation of PACE is its strict eligibility criteria. Participants must typically be 55 or older, live in a PACE service area, and be certified as needing nursing home-level care.
You must locate and contact the specific Central Coast PACE organization to verify service availability. The national website is a great starting point for research.
Website: National PACE Association
11. Natividad Medical Center
Natividad Medical Center serves as a critical healthcare anchor for the Central Coast. It operates as a 172-bed acute-care teaching hospital in Salinas.
For families navigating serious illness, its website is a key portal for understanding comprehensive inpatient and outpatient services. The site provides essential information on its specialty clinics and Level II Trauma Center.
Key Features and Use Cases
A defining feature is Natividad's role as a safety-net hospital, ensuring access to care regardless of a patient's ability to pay. Families can use the website to explore specialty clinics that address complex conditions.
Its affiliation with UCSF also signifies a commitment to high-quality medical education. This is a crucial consideration when seeking treatment for a seriously ill family member.
Practical Considerations
As a major trauma center and public hospital, Natividad can experience high patient volumes. This may lead to longer wait times for certain services.
Families should use the website to find direct contact numbers for specific departments to streamline inquiries. This hospital often serves as the starting point for a diagnosis before a transition to home-based care.
Website: Natividad Medical Center
12. SCAN Health Plan
SCAN Health Plan is a Medicare Advantage plan specifically designed for seniors. Services are available in select Central Coast counties.
The website is a crucial resource for families exploring insurance options that go beyond standard Medicare. It provides detailed information on plans that bundle medical, dental, and vision coverage.
Key Features and Use Cases
A significant feature is SCAN's focus on preventive care and chronic disease management through its programs. This in-home support helps seniors maintain independence and can reduce hospitalizations.
Families can use the website to check eligibility, compare plan benefits, and find local providers. This makes it a key tool for long-term care planning.
Practical Considerations
SCAN's primary limitation is its geographic availability. Before investing time, families must use the website’s "Check Availability" tool to confirm eligibility.
Understanding the specific benefits and provider networks for each plan is vital. This makes the website an essential first step in determining if SCAN is a viable resource for your family.
Website: SCAN Health Plan
Local Health Care Resources Comparison: Central Coast
| Provider | Core Services/Features | User Experience / Quality ★ | Target Audience 👥 | Unique Selling Points ✨ | Price / Value 💰 |
|---|---|---|---|---|---|
| 🏆 Central Coast VNA & Hospice (CCVNA) | Skilled home health, palliative, hospice care under one roof | ★★★★★ Trusted 74+ years, holistic interdisciplinary team | Seniors, chronically ill, terminal patients | Full continuum care; nonprofit; emotional/spiritual support | 💰 Accessible; Medicare & private insurances accepted |
| Dignity Health – Central Coast Home Health | Home health, hospice, in-home infusion services | ★★★★ Focus on comfort & dignity | Seriously ill patients on Central Coast | Unique infusion services; multiple locations | 💰 Varies by location |
| Central Coast Home Health and Hospice | Nursing, rehab, hospice, specialty programs | ★★★★ Certified, positive patient feedback | Seriously ill in San Luis Obispo & Santa Barbara | Physician-directed, quality of life emphasis | 💰 Not publicly disclosed |
| Arosa – Central Coast In-Home Senior Care | Personalized senior care, care management | ★★★★ Flexible scheduling, caregiver matching | Seniors needing home care | Personalized plans; strong local partnerships | 💰 Flexible; private pay likely |
| Accessible Home Health Care – Central Coast | Alzheimer's/dementia care, companion, therapy | ★★★ Flexible scheduling, no long-term contracts | Seriously ill, elderly, dementia patients | Customized care plans; hourly or live-in care | 💰 Competitive; flexible options |
| Home Matters Caregiving – Central Coast | 24-hr, overnight, live-in care for seniors | ★★★★ Expert care, flexible scheduling | Seniors with chronic/Alzheimer’s care | Holistic, personalized, no long-term agreements | 💰 Not specified |
| Central Coast Senior Services, Inc. | In-home care, assisted living, respite, Alzheimer's support | ★★★★ 24/7 support, focus on independence | Seniors in Monterey Peninsula & Salinas | Comprehensive senior services | 💰 Not publicly disclosed |
| Family Caregiver Alliance (FCA) | Education, support, webinars, consulting | ★★★★ Renowned authority on caregiver support | Family caregivers nationwide | Extensive resources, personalized advice | 💰 Free and nonprofit |
| Program of All-Inclusive Care for the Elderly | Interdisciplinary primary, home, social services | ★★★★ Holistic care, preventive focus | Frail elderly 55+ | Coordination of medical/social care | 💰 Medicare/eligibility-based |
| Natividad Medical Center | Acute care hospital, trauma center, specialty clinics | ★★★★ Safety-net hospital, UCSF affiliation | General & seriously ill Central Coast patients | Level II trauma, comprehensive medical education | 💰 Covered by insurance; potentially long waits |
| SCAN Health Plan | Medicare Advantage plan: medical, dental, vision, community | ★★★★ Tailored senior plans, preventive focus | Seniors in select Central Coast counties | Community-based programs; chronic disease management | 💰 Medicare plan; varies by county |
Final Thoughts
Navigating the healthcare system when a loved one is seriously ill can be a heavy burden for any family to carry. Our goal with this guide was to simplify that journey.
We compiled a list of the most vital local health care resources for seriously ill family members central coast residents can rely on. From in-home skilled nursing to compassionate end-of-life care, the Central Coast has a robust network of dedicated providers.
Key Takeaways and Actionable Next Steps
Choosing the right support system is a deeply personal decision, but it doesn't have to be a solitary one. Keep these crucial points in mind:
- Start the Conversation Early: Discussing advance care planning and preferences for care empowers your loved one and ensures their voice is heard.
- Assess the Level of Need: Is the need for post-hospitalization recovery (home health), symptom management (palliative care), or end-of-life comfort (hospice)? A clear assessment points you to the right provider.
- Verify Insurance and Eligibility: Always confirm coverage with your insurance provider. Ask providers directly about their accepted plans and any potential out-of-pocket costs.
- Involve Your Physician: Your family member's physician is a key partner. They provide referrals and collaborate with home health or hospice teams to ensure seamless medical oversight.
- Don't Forget Family Support: Caring for a seriously ill family member is a demanding role. Utilize resources like the Family Caregiver Alliance to protect your own well-being.
By taking a proactive, informed approach, you can build a circle of support that honors your loved one's dignity and provides peace of mind. The right combination of local resources can transform a challenging time into a period of connection and compassionate care.
Frequently Asked Questions (FAQs)
1. What is the difference between home health, palliative, and hospice care?
Home health care provides skilled nursing and therapy to help patients recover from an illness or injury at home. Palliative care focuses on symptom relief for a serious illness at any stage. Hospice care provides comfort and support for patients with a life-limiting illness, typically in the final months of life.
2. How do I know if my family member is eligible for services from Central Coast VNA & Hospice?
Eligibility for CCVNA's services, such as home health or hospice care in Monterey County, typically requires a physician's referral and meeting specific criteria defined by Medicare or other insurers. You can contact CCVNA directly to discuss your family member's situation and they can help coordinate with the physician.
3. Are these services covered by Medicare?
Most services like home health and hospice care are covered under Medicare Part A, provided the patient meets eligibility requirements and the agency is Medicare-certified. Palliative care is often covered under Medicare Part B. Non-medical home care is typically paid for privately.
4. What areas does Central Coast VNA & Hospice serve?
As a local, nonprofit provider, CCVNA has served the community for over 74 years. Their service area includes Monterey County, San Benito County, Santa Cruz County, and South Santa Clara County.
5. How do I start the process of getting in-home care for my loved one?
The best first step is to speak with your loved one’s doctor about their needs. The physician can provide a referral to an agency like CCVNA, which will then conduct an assessment to create a personalized plan of care.
When navigating the continuum of care, having a trusted, local partner makes all the difference. For over 74 years, Central Coast VNA & Hospice has provided expert home health, palliative care, and hospice services rooted in our nonprofit mission to serve the Central Coast community. To learn how our dedicated clinical teams can support your family's unique journey, visit us at VNA and Hospice or contact us today to start the conversation.
Where to Turn When a Loved One Is Seriously Ill: Central Coast VNA & Hospice
When a loved one is diagnosed with a serious illness, it feels like the world stops. The path forward is suddenly uncertain, and the questions can be overwhelming.
For families on California’s Central Coast, there's a trusted hand to hold through this journey: Central Coast VNA & Hospice. For more than 74 years, our nonprofit has been a steady presence, offering seamless in-home support that adapts as your needs change—from recovery to end-of-life care.
Your Compassionate Guide for a Serious Illness
Receiving a serious diagnosis is isolating. The immediate need isn’t just for medical answers, but for compassionate guidance to help you make sense of it all.
That's exactly the role we fill for families across Monterey, San Benito, Santa Cruz, and South Santa Clara counties. Our entire approach is built on a “Continuum of Care.”
Think of it as a single, unbroken thread of support that follows your loved one wherever their health journey leads. This ensures that as your family’s situation evolves, the team you trust remains right by your side, delivering care in the one place they want to be most: home. We're not just another healthcare provider; we're a community partner with a 74-year legacy of putting people before profit.
Understanding Your Options at a Glance
Navigating healthcare can feel like learning a new language. To make it simpler, we’ve organized our core services to align with the different stages of a serious illness. This helps you pinpoint the right level of support at the right time.
- Home Health Care: This is for recovery. After a hospital stay, surgery, or major health event, our team brings skilled nursing and therapy right to the home to help your loved one get back on their feet.
- Palliative Care: Think of this as an extra layer of support. It focuses on relieving the symptoms and stress of a chronic condition and can be provided right alongside curative treatments.
- Hospice Care: When a cure is no longer the goal, the focus shifts to comfort, dignity, and peace. Hospice wraps the entire family in comprehensive support, managing pain while providing emotional and spiritual care.
This visual helps show how hospice is about more than just medical needs—it’s a holistic philosophy of care.
As you can see, every element is designed to improve quality of life for both the patient and the family. To help you see the differences more clearly, here is a quick comparison of our primary services.
CCVNA's Continuum of Care at a Glance
| Service Type | Primary Goal | Patient Eligibility | Typical Services Provided |
|---|---|---|---|
| Home Health Care | Recovery and rehabilitation | Needs skilled care after hospitalization, surgery, or illness. Must be homebound. | Skilled nursing, physical/occupational/speech therapy, medical social work. |
| Palliative Care | Symptom and stress relief | Living with a chronic or serious illness, at any stage. Can receive curative treatment. | Pain management, advance care planning, coordination with doctors, emotional support. |
| Hospice Care | Comfort and quality of life | Terminal diagnosis with a life expectancy of 6 months or less. Not seeking a cure. | Pain and symptom management, nursing care, spiritual and emotional counseling, bereavement support for family. |
This table shows how each service is tailored to meet specific needs, ensuring your loved one receives the most appropriate care. At its core, our work is a partnership built on trust.
We are here to honor your loved one’s wishes and ensure they receive the best care possible in the familiar comfort of their own home.
Part of this journey involves having difficult but necessary conversations. You can find helpful tips for talking with a loved one that's terminally ill to navigate these moments with grace and compassion. In the sections that follow, we'll dive deeper into each of these services to help you feel confident in choosing the right path for your family.
Restoring Independence with Home Health Care

When a loved one comes home after a hospital stay, surgery, or another significant health event, the road to recovery can feel incredibly daunting. The goal is simple—to get back strength and independence—but getting there often requires skilled medical care that most families aren't prepared to provide on their own.
It's a critical time. You need to know where to turn for help, and that's where Central Coast VNA & Hospice offers a clear, supportive path forward.
Instead of dealing with the stress of constant trips to a clinic, our Home Health service brings expert care right to your loved one’s door. It’s a bridge between the hospital and self-sufficiency, built in the one place they feel most comfortable: home.
Who Benefits from Home Health Care?
Home Health is a vital lifeline for patients in a wide range of situations. Think of it as a proactive step to ensure recovery is smooth, safe, and effective, all while cutting down the risk of complications or another hospital stay.
This service might be the perfect fit if your loved one is:
- Recovering from surgery, like a joint replacement or heart procedure, and needs help with wound care and rehabilitation.
- Managing a new or complicated diagnosis, such as heart failure, COPD, or diabetes, which requires skilled monitoring and education.
- Healing from an injury after an accident or fall and needs therapy to safely get back on their feet.
- Experiencing frequent hospital visits; in-home nursing can help stabilize their condition and break that difficult cycle of readmissions.
Home Health Care is about more than just medical treatment. It's a partnership focused on empowerment. It transforms a period of vulnerability into a structured journey of healing, restoring not just physical strength but also confidence and hope.
A Team-Based Approach to In-Home Recovery
What truly makes Home Health so effective is the coordinated team that works together, all under the direction of your loved one’s doctor. This collaborative approach ensures the care plan is perfectly tailored to their specific medical needs and recovery goals.
At Central Coast VNA & Hospice, this team is made up of dedicated, licensed professionals. Depending on the personalized plan, your loved one might have visits from:
- Registered Nurses (RNs): They are the quarterbacks of care, managing medications, treating wounds, monitoring vital signs, and teaching you and your family how to manage the condition.
- Physical Therapists (PTs): These specialists focus on restoring strength, balance, and mobility through targeted exercises, helping your loved one walk safely and with confidence.
- Occupational Therapists (OTs): They are the experts in daily living. OTs help individuals regain the ability to do things like dress, bathe, and cook, often by teaching new techniques or suggesting adaptive tools.
- Speech-Language Pathologists (SLPs): For those recovering from a stroke or other neurological conditions, SLPs are essential for overcoming communication challenges and swallowing disorders.
- Medical Social Workers: These professionals provide crucial support, connecting families with community resources and helping everyone navigate the emotional weight of a serious illness.
This team-based model ensures a holistic recovery. It addresses the immediate medical issues, but just as importantly, it supports the practical and emotional sides of healing at home.
Our services are available across the Central Coast, including Monterey County, San Benito County, Santa Cruz County, and South Santa Clara County. If you think your loved one could benefit from this dedicated approach, we encourage you to learn more about our specific home health care services and how we can help.
Enhancing Quality of Life with Palliative Care
When a family is navigating a serious illness, the term "palliative care" often comes up. It's easy to confuse it with hospice, but they are two very different things.
Understanding this distinction is one of the most important first steps for families on the Central Coast trying to find the right support for a loved one.
Think of palliative care as a dedicated support system that works alongside your loved one's main medical treatments. It's not about giving up or stopping treatment. In fact, its sole purpose is to improve their quality of life by managing the pain, symptoms, and stress that so often come with conditions like cancer, heart failure, or COPD. It’s not about end-of-life care; it’s about making life better, right now.
More Good Days and Greater Strength
A serious illness is more than a physical battle. It can bring a wave of emotional distress, spiritual questions, and practical challenges that can feel overwhelming for both the patient and their family.
Palliative care is designed to address all of it. The goal is simple: to give your loved one more good days.
This is done by expertly managing symptoms that might otherwise force them into the emergency room or a hospital bed. When pain, nausea, or fatigue are controlled at home, patients feel stronger. They can engage more with their families and find the resilience they need to keep up with their medical treatments.
Palliative care is a philosophy of care that acknowledges the whole person. It empowers patients by giving them more control over their symptoms and more energy to focus on what truly matters to them—whether that’s attending a family wedding or simply enjoying a quiet afternoon at home.
How Palliative Care Works at Home
When you partner with Central Coast VNA & Hospice, our palliative care team works in close collaboration with your loved one’s existing doctors. We don’t replace their primary physician or specialists; we add another layer of specialized expertise in symptom management and supportive communication.
Our team, which can include Registered Nurses and Medical Social Workers, will create a personalized plan focused on:
- Symptom Control: Actively managing pain, shortness of breath, fatigue, and other distressing symptoms to maximize comfort.
- Stress Reduction: Providing emotional support and resources to help patients and families cope with the incredible strain of a serious illness.
- Clear Communication: Helping families have tough conversations about their goals and make complex medical decisions that align with their values.
- Care Coordination: Making sure all healthcare providers are on the same page, which creates a much smoother and less fragmented experience for the patient.
This support is brought directly into the comfort of your loved one's home, whether that's a private residence or an assisted living facility. Bringing care home helps avoid stressful trips and allows for a more peaceful, stable environment.
For families across Monterey, San Benito, Santa Cruz, and South Santa Clara counties, it's a vital service that puts an ally in your corner. To explore the specific ways this service can help your family, you can learn more about the benefits of palliative care in our detailed guide.
Choosing Dignity and Comfort with Hospice Care

Choosing hospice is one of the most profound acts of love a family can make. It’s a courageous decision to shift the focus away from aggressive, often draining treatments and toward what matters most: comfort, peace, and dignity.
For families on the Central Coast wondering where to turn when a loved one is seriously ill, Central Coast VNA & Hospice offers a clear and compassionate path forward.
We’ve always believed that hospice isn’t a place you go to—it’s a philosophy of care delivered wherever your loved one calls home. It’s about making a conscious choice to ensure their final months are lived as fully as possible, surrounded by the people and places they know and love.
A Philosophy of Comfort and Support
There’s a common misconception that choosing hospice means giving up. Nothing could be further from the truth. In reality, it’s about reclaiming control and aligning the goals of care with your loved one’s own wishes.
According to the National Hospice and Palliative Care Organization (NHPCO), over 1.72 million Medicare beneficiaries received hospice services in 2020 (NHPCO, 2021). This data reflects a growing movement toward embracing quality of life, comfort, and dignity in a person's final chapter.
Hospice is about adding life to days, not just days to life. It’s a dedicated service that honors a person’s final chapter by ensuring it is lived with as little pain and as much peace as possible.
When you choose Central Coast VNA & Hospice, you are choosing this philosophy. Our care is provided in private homes, assisted living communities, and nursing facilities all across Monterey, San Benito, Santa Cruz, and South Santa Clara counties.
The Interdisciplinary Team: A Circle of Care
One of the most powerful aspects of hospice is that it supports the entire family, not just the patient. At CCVNA, we achieve this through our interdisciplinary team—a group of dedicated professionals who work together to address every aspect of your loved one's well-being.
Your family’s dedicated team may include:
- Hospice Physician: Oversees the medical plan of care, working in close collaboration with your family's personal doctor.
- Registered Nurse: Makes regular home visits to manage pain and other symptoms while teaching the family how to provide confident, loving care.
- Hospice Aide: Helps with personal care like bathing and dressing, which goes a long way in maintaining comfort and a sense of dignity.
- Medical Social Worker: Provides vital emotional support and helps your family connect with practical community resources.
- Chaplain: Offers non-denominational spiritual support that honors the patient’s and family’s personal beliefs and values.
- Volunteers: Offer companionship for your loved one, much-needed respite for family members, and a friendly, supportive presence.
This comprehensive circle of support wraps around your family, helping to lift the burden so you can focus on what truly matters—spending meaningful time together.
Preparing for the Future with Peace of Mind
Beyond the immediate medical and comfort care, we know that peace of mind often involves addressing future planning. When a loved one is seriously ill, it’s natural to think about these practical matters to reduce stress on the family down the road.
You might find it helpful to look into resources for legal forms for estate planning related to things like wills and advance directives. Taking care of these details can be an empowering part of the process, ensuring your loved one’s wishes are clearly documented and honored.
Ultimately, choosing hospice is about choosing a path of dignity. If you’re exploring your options, our team can help you understand more about our hospice care services and how we can support your family during this important time.
Why a Local Nonprofit Partner Matters
When a loved one is seriously ill, you're faced with a flood of decisions. One of the most important is who to trust with their care.
In a landscape full of options, understanding the real difference between a for-profit agency and a local, mission-driven nonprofit like Central Coast VNA & Hospice is critical. The distinction really comes down to one thing: the mission. As a nonprofit, our primary commitment isn't to generating revenue for shareholders. It's to serving the well-being of our community.
A Mission Focused Entirely on Care
For more than 74 years, Central Coast VNA & Hospice has been woven into the fabric of this community. Our roots in Monterey County, San Benito County, Santa Cruz County, and South Santa Clara County run deep.
That deep connection means every resource we have and every decision we make is guided by one simple question: What is best for our patients and their families? This patient-first philosophy brings real, tangible benefits to your loved one.
- Reinvestment in Quality: Any financial surplus goes right back into our programs. This means better training for our clinical staff, state-of-the-art medical equipment, and the ability to offer specialized community programs that a for-profit agency might not find financially viable.
- Ethical Guidance: Our care plans are built on compassion and ethics, completely free from the pressure to hit financial targets. This ensures that every decision is based on medical necessity and your loved one's personal wishes.
- A Legacy of Trust: With such a long history here on the Central Coast, our reputation is built on generations of trust. Families know we'll be here for them, providing consistent, high-quality care today and for years to come.
Navigating a Growing Field with a Trusted Partner
The need for compassionate in-home care is growing fast. Over the last decade, the number of hospice providers has shot up, especially here in California. More choices can be a good thing, but it also makes it crucial to pick a provider with a demonstrated history of excellence and stability.
In such a crowded field, choosing a partner with a proven, long-term commitment to the community offers priceless peace of mind. A nonprofit’s mission ensures that the focus always stays on compassionate care, no matter how the industry changes.
Understanding the different types of providers is a huge part of that. To help, we’ve put together a guide covering the top 5 facts you need to know about hospices, which can clarify what to look for in a quality partner.
The Power of Local Roots and Community Focus
When you choose Central Coast VNA & Hospice, you're choosing a team of your neighbors. Our Registered Nurses, Hospice Aides, and Chaplains often live in the same towns they serve.
This local focus also means we're uniquely tuned into the specific resources and needs of the Central Coast. We have strong, established relationships with local physicians, hospitals, and community organizations, allowing us to provide care that is truly seamless and integrated. When your family needs support, you can be confident that our team not only has the medical expertise but also the local knowledge to connect you with the right help, right here at home.
How to Get Started with Our Care Services
Figuring out the next steps when a loved one is seriously ill can feel overwhelming. At Central Coast VNA & Hospice, our entire team is here to make this process as simple and supportive as possible. You don’t have to navigate this alone.
Anyone can start the conversation. It could be the patient, a concerned family member, a close friend, or a doctor. You don’t need an official referral just to call and learn about your options. The whole process begins with one phone call to our compassionate staff.
Your Initial Conversation with Our Team
When you first call us, our main job is to listen. We’ll take the time to understand what your family is going through, answer your most pressing questions, and gently explain which of our services might be the best fit.
If it feels right, we can then schedule a consultation to start creating a personalized plan of care.
You don’t have to wait for a crisis to explore your options. A proactive conversation today can provide immense relief and clarity for tomorrow, empowering your family with the knowledge to make confident decisions when the time is right.
Having these discussions early also gives your family a chance to prepare for what lies ahead. A crucial part of this is understanding how to make your loved one’s wishes official. You can learn more about this important step by exploring what is advance care planning in our detailed guide.
We encourage you to contact us today. Let us show you how our dedicated team can support your family through this challenging time. For families on the Central Coast wondering where to turn, Central Coast VNA & Hospice is here to help.

Frequently Asked Questions (FAQs)
When a loved one is seriously ill, making decisions can feel overwhelming. It brings up a lot of questions. We’ve put together answers to some of the most common ones we hear from families right here on the Central Coast.
When Is the Right Time to Call Central Coast VNA & Hospice?
The best time to call is as soon as you feel you could use more support. You don't need to wait for a crisis. An early conversation allows our team to get the right care in place at the right time, whether your loved one needs Home Health, Palliative Care, or Hospice Care.
Is Palliative Care the Same as Hospice?
No, they are different. Palliative care is an extra layer of support focused on relieving symptoms of a serious illness and can be provided at any stage, even alongside curative treatments. Hospice care is for when curative treatment is no longer the goal, focusing entirely on comfort and quality of life.
How Is Care from a Nonprofit Like CCVNA Different?
As a nonprofit with over 74 years of history on the Central Coast, our mission is entirely focused on our patients and community. We reinvest all resources back into our care programs and staff. Our decisions are driven by what’s best for your family, not by profit margins.
Who Pays for These Services?
Home health, palliative care, and hospice are typically covered services. Medicare, Medi-Cal, the VA, and most private insurance plans include these benefits. Our team is here to help you verify your coverage and understand any potential costs upfront.
Does My Loved One Have to Leave Home for Hospice Care?
No, our primary goal is to provide hospice care wherever a person calls home. For most, that means their private residence, but it could also be an assisted living facility or a nursing home in Monterey, San Benito, Santa Cruz, or South Santa Clara County. We bring our entire team directly to the patient.
Navigating a serious illness is a journey no family should have to face alone. For compassionate guidance and expert in-home care, you can trust the local, nonprofit team that has served your community for over 74 years.
Contact Central Coast VNA & Hospice today to learn how we can support you. https://ccvna.com
Preventing Hospital Readmissions: A Guide to Safe Recovery at Home
When a patient goes home from the hospital, the real work of recovery begins. Preventing a return trip hinges on providing solid, coordinated care that supports them after discharge.
A seamless transition from hospital to home, guided by skilled professionals from Central Coast VNA & Hospice, is the most effective way to ensure recovery is safe and lasting. It’s all about addressing common post-discharge challenges before they become major problems.
Why Hospital Readmissions Happen and How to Prevent Them

For patients and their families, returning to the hospital shortly after coming home is incredibly frustrating and disruptive. These readmissions are often preventable and usually signal a breakdown in the continuity of care.
The first step to building a better path to recovery is understanding why they happen in the first place. Many readmissions are the result of gaps that appear once a patient is back home, feeling overwhelmed without professional support.
Common Causes of Hospital Readmissions
The shift from the structured, 24/7 environment of a hospital to the independence of home can be jarring. Patients suddenly face new medication routines, may not fully grasp their condition, or end up missing crucial follow-up appointments.
Some of the key factors we see contributing to readmissions include:
- Medication Confusion: Juggling multiple new prescriptions is tough. It’s easy to get confused about dosages, timing, and potential side effects.
- Lack of Follow-Up: Patients often fail to schedule or attend necessary appointments with their primary doctor or a specialist after they get home.
- Unrecognized Symptoms: Many people simply don't know which warning signs or "red flag" symptoms require immediate medical attention and which ones can wait.
- Inadequate Support at Home: Recovery can be derailed by a simple lack of help with daily activities, preparing meals, or personal care.
One of the biggest, and most frequently overlooked, factors is a patient's confidence. When individuals and their families feel unprepared to manage care on their own, anxiety shoots up. Small issues can quickly escalate, often leading to an unnecessary trip back to the emergency room.
The Role of a Coordinated Care Continuum
The best strategy for preventing hospital readmissions is creating a coordinated continuum of care that bridges the gap between the hospital and the home. This is where Central Coast VNA & Hospice excels, offering expert support across Monterey County, San Benito County, Santa Cruz County, and South Santa Clara County.
As a trusted nonprofit with over 74 years of service, we ensure patients get the right care at exactly the right time. Our compassionate, mission-driven approach weaves together several crucial services.
- Home Health Care: Our team of Registered Nurses and therapists brings skilled medical care right into the patient’s home. They perform safety assessments, reconcile medications to avoid dangerous errors, and provide hands-on education to ensure a stable recovery.
- Palliative Care: For patients managing serious or chronic illnesses, our palliative care at home focuses on managing symptoms and improving quality of life. This proactive approach helps prevent the kind of crises that frequently lead to re-hospitalization.
By creating a smooth transition and offering expert guidance, we empower both patients and their families. This compassionate, in-home support ensures that recovery continues safely and effectively, keeping our community members healthy and where they want to be—out of the hospital.
Contact us today to learn how our services can help you or a loved one.
Building A Strong Foundation Before Hospital Discharge
A successful recovery doesn’t start when a patient walks out the hospital doors. It begins long before that. The most effective strategies for preventing hospital readmissions are proactive, built on a strong foundation of thoughtful pre-discharge planning.
This is where hospital staff and home health agencies like Central Coast VNA & Hospice collaborate to set the stage for a safe, smooth transition home. This isn’t just about checking boxes; it’s a dynamic, hands-on process involving real conversations and clear communication.
Proactive Assessments And Personalized Care Plans
At Central Coast VNA & Hospice, our work often starts right inside the hospital. Our Registered Nurses conduct thorough pre-discharge assessments to get the full picture—not just the medical diagnosis, but the entire home environment and any potential roadblocks to healing.
We look closely at a few key areas:
- Medication Complexity: We review all prescriptions to spot potential conflicts, confusing schedules, or cost issues that might tempt someone to skip a dose.
- Mobility and Safety: We get a real sense of the patient’s physical abilities and scout for fall risks or other hazards in the home that need immediate attention.
- Support System: We talk with family members to understand what they can handle and give them the training they need to feel confident, not overwhelmed.
- Symptom Management: We create a clear, easy-to-follow plan for managing symptoms to stop a crisis before it starts. You can learn more about the benefits of palliative care for managing long-term illnesses.
From this deep dive, a truly personalized care plan is born. Think of it as a roadmap for those first critical days and weeks at home, outlining specific actions, goals, and "red flag" symptoms.
Key Focus Areas for Pre-Discharge Planning
| Focus Area | Objective | CCVNA Professional Involved |
|---|---|---|
| Medication Reconciliation | Ensure patient understands new medication schedule, purpose, and side effects. Address any cost or access concerns. | Registered Nurse (RN) |
| Home Safety Evaluation | Identify and mitigate fall risks and other hazards. Recommend necessary modifications or equipment. | Physical/Occupational Therapist, RN |
| Patient & Family Education | Empower the patient and family members with knowledge on symptom management, diet, and when to seek help. | RN, Dietitian, Medical Social Worker |
| Follow-up Coordination | Schedule the first home health visit and necessary physician appointments before the patient leaves the hospital. | RN, Care Coordinator |
| Emotional & Social Support | Assess the patient’s support system and connect them with community resources or counseling if needed. | Medical Social Worker (MSW) |
This structured approach ensures that our plan is not just comprehensive but also practical, addressing the real-world challenges patients face when they return home.
Real-World Scenarios In Pre-Discharge Planning
Let’s put this into practice. Imagine a patient in Monterey County recovering from heart surgery. Before they’re discharged, a CCVNA Registered Nurse meets with them and the hospital team. The nurse learns the patient lives alone in a two-story house and has five new medications to manage.
A proactive plan means addressing risks before they become emergencies. By identifying challenges early, we empower patients with the tools and support needed for a confident recovery journey.
Recognizing the high risk for both a fall and medication mix-ups, the nurse builds specific solutions right into the care plan. A Physical Therapist is scheduled for the very first day home to teach the patient how to safely navigate their stairs. The nurse also creates a simplified, large-print medication chart.
This infographic breaks down the core steps we follow to create a safe and effective plan for when a patient goes home.
As you can see, a solid discharge plan, quick follow-ups, and professional home health services are all connected. When we address each piece systematically, the risk of readmission drops significantly.
This early, coordinated effort provides incredible peace of mind. Patients and their families in our service areas—Monterey, San Benito, Santa Cruz, and South Santa Clara counties—leave with a dedicated partner and a clear, actionable plan.
How Patient and Family Education Empowers Recovery

When it comes to preventing hospital readmissions, knowledge is one of the most powerful tools we have. But real patient education isn’t about handing someone a stack of pamphlets.
It's about building confidence and turning anxious loved ones into capable partners in the healing journey. A patient who understands their condition and care plan is far more likely to have a smooth recovery.
Moving Beyond Instructions to Real Understanding
Just telling a patient what to do is never enough. Our Registered Nurses are trained to make sure both patients and their families understand the why behind every instruction.
One of the most effective tools we use is the “teach-back” method. After a nurse explains a medication schedule, they'll ask the patient or family member to explain it back in their own words. This isn't a quiz; it's a conversation that immediately shows us if there are any gaps in understanding.
This method helps confirm everyone is on the same page about crucial details, such as:
- The purpose of each medication and what side effects to look out for.
- How to properly care for a wound to prevent infection.
- What dietary or activity changes are essential for recovery.
Spotting Early Warning Signs
One of the biggest reasons patients end up back in the hospital is because a small, manageable issue isn't caught in time. A minor symptom can quickly escalate into a crisis if it's ignored.
That’s why a huge part of our education process is teaching families exactly what to watch for. This proactive approach is a cornerstone of how our team—with over 74+ years of local experience—helps keep our community safe and comfortable at home.
Empowering patients and families to identify warning signs isn't about creating alarm. It's about providing a clear, calm plan of action that replaces uncertainty with confidence, ensuring they know exactly when and how to seek help.
For instance, with a patient recovering from heart failure, our nurse will create a personalized list of "red flag" symptoms. This isn’t vague advice. It’s concrete, measurable guidance like, "Call us if you gain more than three pounds in one day," or "Contact your doctor if you feel short of breath and resting doesn't help."
Building Confidence and Setting Realistic Expectations
Recovery is a journey, not a destination. A critical part of education is setting realistic expectations for the healing process.
Our team, which includes Physical and Occupational Therapists and Medical Social Workers, helps patients and families understand the typical recovery timeline. We also focus on the emotional side of recovery.
Having open conversations about care preferences and future health decisions is vital. For a closer look at this important topic, you can explore our resources on how advance care planning is made simple. This complete approach ensures that families feel prepared not just for the medical tasks, but for the emotional journey, too.
Contact Central Coast VNA & Hospice today to learn more about how our home health and palliative care services can support your family.
Making the Transition to Home Health Care Seamless
The first 48 hours after a patient leaves the hospital are incredibly high-stakes. This is the window where a recovery can either take root or start to unravel, making it the most critical time for preventing hospital readmissions.
A smooth, professionally managed transition from the hospital back to home life acts as a crucial safety net. It’s all about catching potential problems before they escalate into full-blown emergencies.
At Central Coast VNA & Hospice, our home health care services are built to bridge this exact gap. We provide immediate, in-home support to make sure care continues safely and without interruption.
The Critical First Visit Home
The moment a patient gets home, our team is ready to go. A Central Coast VNA & Hospice Registered Nurse (RN) almost always makes the first visit, usually within 24 to 48 hours of discharge.
This isn't just a quick check-in. It’s a comprehensive clinical assessment designed to establish stability and map out a clear path forward.
During this vital first meeting, our RN zeroes in on a few key actions:
- Confirming the Medication Plan: The nurse meticulously reviews all hospital paperwork and compares it with the medications the patient has at home. They check for discrepancies and explain what each prescription is for.
- Performing a Hands-On Assessment: The nurse conducts a thorough physical assessment. This means checking vital signs, looking at how wounds are healing, and gauging pain levels to establish a baseline.
- Evaluating the Home Environment: Is the lighting dim? Are there loose rugs waiting to cause a fall? The nurse scans the home for these kinds of safety risks and gives immediate, practical advice to fix them.
This first visit builds a foundation of trust and safety. It’s our way of letting patients and their families know they aren't going through this alone.
Tailoring a Comprehensive Care Team
Every person's recovery is different, so a one-size-fits-all approach doesn't work. Based on that initial assessment, the RN works with the patient’s doctor to put together a personalized care team.
This team brings a whole range of expertise right into the home, focusing on exactly what the patient needs.
A tailored care team does more than just treat symptoms; it addresses the whole person. By integrating skilled nursing, therapy, and personal support, we build a robust circle of care that promotes physical healing and emotional well-being.
The professionals who might join a patient’s support system include:
- Registered Nurses to handle complex medical needs, from wound care to IV therapy.
- Physical and Occupational Therapists to help regain strength, mobility, and independence with daily tasks.
- Speech Therapists to help with swallowing or communication issues after a stroke or other illness.
- Medical Social Workers to connect families with helpful community resources and offer emotional support.
- Hospice Aides to give essential, dignified help with personal care like bathing and dressing.
This kind of teamwork makes sure every angle of the patient's recovery is covered. You can explore our full range of home health care services to see how we support patients across Monterey County, San Benito County, Santa Cruz County, and South Santa Clara County.
Managing Chronic Illness with Palliative Care at Home

When someone is living with a serious or chronic illness—like heart failure, COPD, or cancer—the focus shifts. It’s no longer just about recovering from a single hospital stay, but about preventing the next one.
Managing these long-term conditions at home demands a proactive strategy that puts comfort and quality of life first. This is where palliative care at home provides a powerful layer of support.
Palliative care, a core service at Central Coast VNA & Hospice, is specialized medical support that can begin at any stage of a serious illness. It is not the same as hospice and can be received alongside curative treatments.
A Team-Based Approach to Comfort and Quality of Life
One of the biggest strengths of palliative care is that it brings an entire interdisciplinary team right to the patient's home. This team works together to care for the "whole person," not just the disease.
At Central Coast VNA & Hospice, this compassionate team includes:
- Registered Nurses who are experts in managing pain and other difficult symptoms.
- Medical Social Workers who offer emotional support and connect families with essential community resources.
- Chaplains who provide spiritual guidance and support that respects the patient's personal beliefs.
- Hospice Aides who help with personal care, preserving both dignity and comfort.
This collaborative approach ensures every part of a patient's well-being is looked after, from physical pain to emotional distress. This level of comprehensive support can stabilize a patient’s condition and significantly reduce the likelihood of another hospital stay.
Proactively Managing Symptoms to Prevent Crises
For patients with chronic illnesses, uncontrolled symptoms are a primary driver of hospital readmissions. A sudden spike in pain or severe shortness of breath can quickly turn into an emergency.
Palliative care is all about getting ahead of these problems before they become unmanageable. This constant, in-home vigilance can prevent the kind of crisis that would otherwise land a patient back in the hospital.
The goal of palliative care is not just to manage illness, but to enhance life. By focusing on comfort, dignity, and personal goals, we empower patients to live more fully, even while facing serious health challenges.
This proactive stance helps patients feel more in control and less anxious. For those navigating their condition, having access to resources like a guide to living with cancer and thriving can offer more strategies for staying well at home.
Navigating Complex Decisions and Providing Emotional Support
Living with a serious illness often involves making tough decisions about treatments and personal care goals. The palliative care team is skilled at facilitating these important conversations, making sure the patient's voice is heard.
This complete support system strengthens a patient's ability to cope, reducing the kind of stress that can worsen physical symptoms. By understanding the different 4 stages of palliative care, families can better see how this support evolves to meet their changing needs.
For families across Monterey, San Benito, Santa Cruz, and South Santa Clara counties, palliative care from CCVNA offers a compassionate path forward. It provides the expert medical and emotional support needed to manage chronic illness effectively at home.
Navigating Healthcare Policies and Measuring Success
Preventing a trip back to the hospital isn't just a clinical goal; it's a national healthcare priority. Federal policies have put a spotlight on patient outcomes, holding entire health systems accountable.
For a mission-driven, nonprofit provider like Central Coast VNA & Hospice, this focus fits perfectly with what we’ve always done. Our commitment to exceptional care strengthens the healthcare ecosystem across Monterey County, San Benito County, Santa Cruz County, and South Santa Clara County.
The Bigger Picture of Readmission Prevention
Policies like the Centers for Medicare & Medicaid Services (CMS) Hospital Readmissions Reduction Program (HRRP) have fundamentally changed how hospitals think about care after discharge. The program uses financial penalties to motivate hospitals to lower preventable readmissions.
This encourages them to build stronger relationships with community-based providers like us. Our skilled teams provide the in-home support that bridges the gap between the hospital and a safe recovery at home.
Preventing a return to the hospital is a shared responsibility. It requires close collaboration between hospitals, physicians, and home health experts to create a safety net that supports patients long after they are discharged.
This national focus is starting to make a difference. According to Advisory Board, an estimated 2,247 hospitals will face readmission penalties in fiscal year 2025 (Advisory Board, 2024). This highlights the ongoing need for effective post-discharge care. You can dig into what these trends mean for providers in a report on readmission penalties.
How We Measure Our Impact
At Central Coast VNA & Hospice, our success is measured one person at a time. Of course, we track data like patient satisfaction and clinical outcomes.
But the real proof is seeing someone regain their independence and avoid the stress of another hospital stay. It’s the foundation of our more than 74 years of service to the Central Coast.
We keep a close eye on our performance to make sure we're living up to the highest standards. This involves:
- Tracking patient progress toward the specific recovery goals they set with their care team.
- Ensuring timely follow-up from our nurses and therapists to catch any issues early.
- Actively listening to feedback from patients and their families so we can keep getting better.
We also believe in helping families prepare for what lies ahead. Proactive conversations and planning are key to preventing future crises. You can learn more by reading our guide on what advance care planning is.
Frequently Asked Questions About Preventing Hospital Readmissions
When a loved one comes home from the hospital, it’s natural to have questions. Here are answers to some of the most common concerns we hear from families in Monterey County and surrounding areas.
1. What is the difference between home health care and palliative care?
Home health care is skilled medical care prescribed by a doctor to help you recover from a specific illness, injury, or surgery at home. Palliative care is an extra layer of support focused on relieving the symptoms and stress of a serious illness and can be received at the same time as curative treatment.
2. How do we arrange for CCVNA services after a hospital stay?
The easiest way is to ask the hospital's discharge planner or social worker for a referral to Central Coast VNA & Hospice. You or your family can also reach out to us directly to discuss your needs and how we can provide support in Monterey, San Benito, Santa Cruz, or South Santa Clara counties.
3. Who will be part of the care team coming to my home?
Your care team is built around your specific recovery needs as ordered by your physician. It may include a Registered Nurse, Physical or Occupational Therapist, Speech Therapist, Medical Social Worker, and a Hospice Aide, all working together to provide coordinated care.
4. Does Medicare cover services to prevent hospital readmissions?
Yes, in most cases. Medicare Part A and/or Part B generally cover home health nursing and therapy services if you meet the eligibility criteria. Palliative care is also often covered by Medicare and many other insurance plans.
5. What are the most important "red flag" symptoms to watch for at home?
While specific to each condition, common red flags include sudden shortness of breath, a fever over 101°F, increased pain that isn't relieved by medication, or signs of confusion. Our team will educate you on the exact symptoms to monitor for your specific situation.
Are you or a loved one in need of support after a hospital stay? Contact Central Coast VNA & Hospice to learn more about our home health, palliative, and hospice services at https://ccvna.com. Our nonprofit organization has proudly served the Central Coast for over 74 years.
A Guide to Home Medical Equipment Rental for In-Home Care
When managing a health condition or recovering at home, having the right support is essential. This is where home medical equipment rental comes in. It offers a practical and cost-effective way to get devices like hospital beds, wheelchairs, or oxygen concentrators exactly when you need them, without the commitment of buying.
This flexibility is a cornerstone of modern home healthcare. It helps patients stay independent and recover safely in a familiar, comfortable environment.

Why Renting Medical Equipment Is a Smart Choice
Deciding whether to rent or buy medical equipment can feel like a big decision. For many families, renting is the most logical and supportive path. It gives you access to high-quality, professionally maintained devices without the steep upfront cost.
This is especially true if the need is temporary, such as for recovery after surgery or an injury. Renting also provides incredible flexibility. As a patient's condition changes, so do their equipment needs, making it easy to adapt.
A rental agreement lets you swap a wheelchair for a walker or return a hospital bed once it's no longer necessary. This ensures the support at home always matches the current stage of recovery.
Commonly Rented Home Medical Equipment
To help you get a better sense of what's available, here’s a quick look at some commonly rented items and how they’re used.
| Equipment Category | Examples | Common Use Cases |
|---|---|---|
| Mobility Aids | Wheelchairs, walkers, crutches, scooters | Assisting with movement, improving stability, and preventing falls. |
| Bedroom Equipment | Hospital beds, patient lifts, overbed tables | Enhancing comfort, promoting proper positioning, and making caregiving easier. |
| Respiratory Support | Oxygen concentrators, nebulizers, CPAP/BiPAP machines | Managing breathing conditions like COPD, asthma, or sleep apnea. |
| Bathroom Safety | Shower chairs, toilet risers, grab bars | Reducing the risk of slips and falls in the bathroom. |
The right equipment is always tied to an individual's specific health needs. These needs should be determined in partnership with a healthcare professional.
Supporting Safety and Independence at Home
The right equipment does more than just help with recovery—it empowers people to live more safely and independently. This philosophy is at the heart of what we do at Central Coast VNA & Hospice. As a nonprofit organization, we have been proudly serving our communities for over 74 years.
By integrating durable medical equipment (DME) into a holistic care plan, we help create a secure environment that reduces the risk of falls and other complications. This is a key component of successful in-home care.
For families in Monterey County, San Benito County, Santa Cruz County, and South Santa Clara County, renting home medical equipment is an accessible solution. It fits seamlessly into a broader care plan. It works hand-in-hand with services like our skilled home health care services and our palliative and hospice programs, ensuring every aspect of a person’s well-being is addressed.
The demand for these rental solutions is growing. According to one report, the global medical equipment rental market was valued at about USD 56.25 billion in 2024 and is expected to keep climbing (Cognitive Market Research, 2024). This trend shows a clear shift toward cost-effective, home-based healthcare.
Matching the Right Equipment to Your Needs
Figuring out the right home medical equipment is a critical step for a safe and comfortable recovery at home. This process should always start with a professional assessment. Relying on a clinical expert helps you avoid the frustration of getting equipment that doesn't fit your home or your health needs.
A Registered Nurse or a Physical Therapist, like those on our team at Central Coast VNA & Hospice, can perform a detailed evaluation. They assess mobility, strength, home layout, and daily routines to pinpoint exactly what kind of support is needed.
Navigating Insurance for Medical Equipment
Once you know what's needed, the next step is understanding how insurance covers the home medical equipment rental. This part often feels like a maze, but it's manageable. Medicare, Medi-Cal, and most private insurance plans have specific rules for durable medical equipment (DME).
The most important term you'll hear is "medical necessity." For insurance to cover a rental, a physician must document that the equipment is essential for treating an illness or injury. For instance, a hospital bed is medically necessary if a patient requires specific positioning to relieve pain, not simply for comfort.
This visual breaks down the core steps to getting it right.
As the infographic shows, it’s a clear path. A professional assessment leads to the right equipment match, which is then adjusted as needed. This structured approach prevents mistakes and keeps patients safe.
Actionable Steps for Verifying Coverage
To make the approval process smoother, it pays to be proactive. A few organized steps can make a huge difference and prevent delays.
- Get a Detailed Prescription: Your physician needs to provide a prescription that clearly states your diagnosis, the exact type of equipment required, and an estimate of how long you'll need it.
- Contact Your Insurance Provider: Call the member services number on your insurance card. Ask directly about your plan’s specific coverage for DME rentals and any copayments or deductibles.
- Work with an Approved Supplier: Insurance companies have a network of approved DME suppliers. You must rent from one of these in-network providers for your claim to be covered.
At Central Coast VNA & Hospice, our team helps patients and their families navigate these exact steps. As a nonprofit that has served Monterey, San Benito, Santa Cruz, and South Santa Clara counties for over 74 years, we have deep experience in coordinating with physicians and suppliers to ensure everything goes smoothly.
Keeping good records is vital. Hold on to copies of all prescriptions, letters of medical necessity, and any communication with your insurance company. This helps you stay organized and provides a paper trail if you need it.
You can learn more about how our home health care team provides this kind of support throughout the recovery journey.
Finding a Trusted Rental Partner on the Central Coast

Choosing a company for a home medical equipment rental is a big decision. It directly impacts a patient's safety and comfort. Not all providers are the same, so it’s critical to look for specific signs of quality and reliability.
A truly trusted partner does more than just drop off equipment. They become an extension of your care team, providing compassionate and reliable service.
When you're vetting potential providers, accreditation is a powerful shortcut to identifying excellence. Look for companies accredited by respected organizations like The Joint Commission. This certification signals that the provider meets tough national standards for safety and equipment maintenance.
What to Look for in a Provider
Beyond formal accreditation, a few practical things will define your experience. A reliable rental partner needs to deliver in these key areas.
- Equipment Quality and Cleanliness: The equipment should be well-maintained and spotless. Ask about their sanitization process, which should follow strict protocols between each patient.
- Responsive Customer Support: What happens if equipment malfunctions? A reputable company will offer 24/7 support to handle emergencies and walk you through problems when they happen.
- Knowledgeable Staff: The technicians who deliver and set up the equipment should be experts. They need to provide clear, patient training on how to operate everything safely and confidently.
Let’s walk through a real-world scenario. Imagine an oxygen concentrator alarms in the middle of the night. A quick call to a responsive provider should connect you with a technician who can calmly walk you through the fix, restoring your peace of mind.
The Value of Coordinated Care
The best results happen when your equipment provider works closely with your healthcare team. When a provider has an established relationship with an organization like Central Coast VNA & Hospice, it creates a much smoother care experience. This collaboration ensures that everyone—from your Registered Nurse to the equipment technician—is on the same page.
As a nonprofit organization with a 74-year legacy on the Central Coast, we’ve seen firsthand how important these partnerships are. Coordinating with trusted local suppliers is a core part of our commitment to delivering comprehensive care. This approach simplifies communication and guarantees that any issues are handled quickly.
Our focus is always on creating a safe, supportive home environment. You can learn more about how our home health care services in Monterey, CA integrate this model. The same principles of vetting a partner apply to finding trusted disability services, where choosing the right organization is key.
Your Guide to Equipment Delivery and Setup

When your home medical equipment rental arrives, it should not be a quick drop-off. A quality rental provider knows this moment is crucial. It’s a comprehensive service designed to ensure you and your family can use the device safely and with total confidence.
The technician who delivers the equipment plays a huge role. Their job goes beyond plugging something in; they are your personal, hands-on trainer. A proper setup session is essential for preventing accidents and ensuring the equipment helps, rather than hinders, your independence.
What to Expect During the Setup Session
A professional setup process should never feel rushed. The technician should patiently walk you through every feature and function. This is your time to learn, so feel comfortable asking them to slow down or repeat something.
A complete training session should cover a few key areas:
- Daily Operation: This includes how to turn it on and off, adjust settings, and understand its main functions. For a hospital bed, they should show you how to raise and lower all parts of the frame.
- Safety Features: The technician must demonstrate every safety mechanism. This includes locking the wheels on a walker, operating bed side rails, and knowing what alarms mean.
- Basic Cleaning and Maintenance: Keeping equipment clean is vital. The technician should explain how to clean the device, how often, and which cleaning products are safe to use.
- Emergency Protocols: You need to know what to do if the equipment stops working. This includes recognizing specific alarm sounds and knowing who to call for 24/7 support.
The point of the setup session is to empower you. By the time the technician leaves, you should feel completely comfortable managing the equipment. This hands-on guidance reflects a provider’s commitment to patient safety.
Asking the Right Questions
This is not the moment to be shy. Before the technician leaves, make sure all your questions have been answered. Getting clear on everything from the start can prevent stress down the road.
Consider asking these questions to make sure you’re fully prepared:
- "Can you watch me do it?" After they demonstrate a function, ask them to watch while you do it. This is the best way to confirm you’ve understood correctly.
- "What are the most common problems people have with this?" This gives you a heads-up on potential hiccups and how to handle them before they become an issue.
- "Who is my direct contact if I have a non-emergency question?" Try to get a specific contact for those "just in case" questions.
At Central Coast VNA & Hospice, we see how proper equipment training is a critical piece of a patient’s overall care plan. It fits perfectly with our mission to provide compassionate care across Monterey, San Benito, and Santa Cruz counties. You can explore our comprehensive guide to understanding home health care.
Living with Your Equipment and Planning for Its Return
Bringing medical equipment into your home can feel overwhelming at first. The key is making a few simple changes to ensure safety and comfort. You’ll want to create clear, wide pathways for getting around with a walker or wheelchair.
This is often as easy as shifting a coffee table or securing a rug to prevent trips. You also need to think about power cords for devices like a hospital bed. Tucking them along baseboards or using cord covers removes a common tripping hazard.
These small adjustments make a huge difference. They help your loved one maintain independence and give everyone peace of mind. The trend toward home-based care is a global movement, with Europe representing over 30% of the worldwide market for medical equipment rentals (Cognitive Market Research, 2024).
When Your Needs Change
A person's healthcare journey is rarely a straight line. As needs change, the equipment that was once essential might no longer be necessary. This is often a good sign—it's a mark of progress in recovery.
As a patient's condition improves, Central Coast VNA & Hospice clinicians continually assess their needs. This ensures you always have the right support at the right time, whether you are receiving home health, palliative, or hospice care.
Our experienced team, including Registered Nurses and Physical Therapists, knows what to look for. They are trained to spot when a piece of equipment has done its job. They will work with you, your family, and the physician to update the care plan and arrange for the return of unneeded items.
Scheduling an Equipment Return
When the time comes, the return process is straightforward. Your only job is to call the rental provider to schedule a pickup. They will confirm the appointment and explain everything you need to know.
On pickup day, the company's technician will handle everything. Here’s what you can expect:
- Inspection: The technician will give the equipment a quick check to ensure it's in good working condition.
- Disassembly: For larger items like a hospital bed, they will handle disassembly carefully and efficiently.
- Removal: The technician will remove the equipment from your home, making sure not to cause any disruption.
- Paperwork: You’ll likely sign a form to confirm the return, which officially closes your rental agreement.
This simple return process is a major benefit of renting. It frees families in Monterey, San Benito, Santa Cruz, and South Santa Clara counties from worrying about what to do with equipment they no longer need.
Frequently Asked Questions About Home Medical Equipment Rental
It's completely normal for patients and their families to have questions about renting medical equipment. Getting clear, straightforward answers is the first step toward feeling confident and secure. Central Coast VNA & Hospice is here to provide the compassionate, professional guidance you need.
1. What happens if the rental equipment breaks down?
Reputable rental providers offer 24/7 support for maintenance and emergency repairs. Before signing an agreement, always ask about their service policy. If your care is coordinated by an agency like Central Coast VNA & Hospice, our clinical team will advocate for you to get any issues resolved quickly.
2. Can I rent equipment for just a few weeks?
Yes. Short-term rentals are a practical solution for temporary situations, like recovering from surgery. This flexibility means you can get a hospital bed or walker for only the time you need it, avoiding the high cost of buying.
3. How do I know the rental equipment is sanitary?
Accredited rental companies must follow strict federal and state guidelines for infection control. Every piece of equipment is thoroughly cleaned, sanitized with medical-grade disinfectants, and inspected for safety before it is delivered to a new patient.
4. Who decides which equipment I need?
The decision is a clinical one made by a healthcare professional. Your physician, Physical Therapist, or Occupational Therapist will determine medical necessity and write a prescription based on an assessment of your condition and home environment. Central Coast VNA & Hospice clinicians conduct these assessments and coordinate with your physician to ensure you get the right equipment.
5. Will my insurance cover a home medical equipment rental?
Most insurance plans, including Medicare and Medi-Cal, cover DME rentals if they are deemed "medically necessary" by a physician. Coverage varies, so it's important to contact your insurance provider to understand your specific benefits, copayments, and any pre-authorization requirements. Our team can help you navigate this process.
At Central Coast VNA & Hospice, our 74-year mission as a local, nonprofit organization is to provide compassionate, high-quality care that supports every aspect of your well-being. From our home health nursing to palliative and hospice care, we serve communities across Monterey County, San Benito County, Santa Cruz County, and South Santa Clara County. If you have more questions or need guidance, our team is here to help.
Learn more about our continuum of care at https://ccvna.com.
A Guide to Preventing Falls in the Home
Preventing falls at home isn't just about avoiding a scraped knee. It's about taking proactive steps to safeguard independence and ensure a loved one can continue living safely and confidently in their own space.
This starts with simple but powerful changes to the home environment and daily habits, like improving lighting, securing loose rugs, and installing safety aids such as grab bars.
Why Preventing Falls at Home Matters So Much

Before we get into the how, it's essential to understand the why. Making a home safer is about so much more than preventing an accident. It’s about preserving a person's independence, their confidence, and their overall quality of life.
A fall can have consequences that linger long after the physical injury has healed. It often creates a deep-seated fear of everyday activities, which can lead to a person moving less and becoming socially isolated. That emotional toll is exactly why taking proactive steps is one of the most loving things a family can do.
Preserving Independence and Well-being
Creating a secure home environment is an achievable goal. A few thoughtful adjustments can make a significant difference.
These changes aren't about limiting freedom—they're about enabling it. They empower your loved one to move around their home with greater assurance.
A safe home fosters confidence, allowing individuals to continue engaging in the daily routines and activities that bring them joy and fulfillment. It is a cornerstone of maintaining dignity and autonomy.
The statistics are sobering. According to the World Health Organization, falls are a major public health issue, with an estimated 37.3 million falls annually that are serious enough to require medical attention (WHO, 2021). These incidents often lead to significant long-term disability and steep healthcare costs.
For over 74 years, our team at Central Coast VNA & Hospice has been committed to supporting families across Monterey County, San Benito County, Santa Cruz County, and South Santa Clara County. As a local, nonprofit organization, we have a deep understanding of how important it is to feel safe at home.
Our compassionate teams, which include Registered Nurses and Occupational Therapists, provide expert guidance that’s tailored to each person's unique situation. Through our home health care services, we help families pinpoint hazards and put effective, practical strategies in place. Our mission is to ensure every person we serve can live safely and comfortably, supported by a continuum of care that adapts as their needs change.
Your Room-by-Room Home Safety Walkthrough
The best way to create a safer home is to walk through it with fresh eyes. This isn’t a sterile inspection, but a practical tour to spot hazards that are easy to overlook.
By tackling the risks room by room, making a home safer becomes a much more manageable and empowering process. This walkthrough is about understanding how you or your loved one actually moves through and uses a space. We'll start with the areas where falls happen most often, pointing out specific issues and offering real-world, compassionate advice.
Navigating Hallways and Stairways
Hallways and stairs are the main highways of a home, but they’re also prime spots for trips and falls. The first thing to check is lighting.
Are light switches easy to find at both the top and bottom of the stairs? Good lighting is non-negotiable, and it might be worth considering installing motion sensor lights so the path is always illuminated.
Next, take a hard look at the pathways themselves.
- Clear the way: Get rid of anything on the floor that doesn't need to be there—shoes, books, stray decorative items.
- Secure the rugs: Any throw rugs or runners need a solid non-slip backing. If they still slide, use rug tape to secure them firmly to the floor.
- Check the handrails: Are there sturdy handrails on both sides of the staircase? Give them a good shake to make sure they can support a person's full weight.
Creating a Safer Bathroom
With its mix of hard surfaces and water, the bathroom is one of the most common places for a fall to happen. Thankfully, a few small changes here can make a world of difference in safety.
For starters, installing grab bars inside the shower and next to the toilet provides a stable handhold exactly where it's needed most. This isn't a minor tweak; it's a game-changer for stability.

As the image shows, professionally installed grab bars are a straightforward way to add security. Don't forget to place non-slip mats both inside the tub or shower and on the bathroom floor to give feet better traction on wet surfaces.
Optimizing Bedrooms and Living Areas
The bedroom and living room should be spaces for rest and relaxation, not sources of worry. Look at the furniture layout.
Are the paths clear and wide enough to walk through easily, even in the dark? Cords and cables from lamps, TVs, or medical equipment are major tripping hazards and should be tucked away or secured along the walls.
A critical detail that often gets missed is the height of chairs and beds. Seating should be high enough that a person can sit down and stand up while keeping their feet flat on the floor for leverage and support.
This isn't just a local issue. A 2022 meta-analysis found that around 26.5% of older adults across the globe experience a fall each year, with that number climbing to 27.9% in the Americas. These aren't just statistics; they represent millions of preventable injuries.
For families here on the Central Coast, from Monterey to Santa Cruz County, getting help is easy. The professional team at Central Coast VNA & Hospice can provide expert guidance during a home care visit, offering personalized advice to make your home as safe as it can possibly be.
Making High-Impact Home Modifications

Once you've pinpointed the potential fall hazards in a home, it's time to take decisive action. Making a few targeted modifications can transform a high-risk environment into a safe, empowering space.
These aren't just about tidying up; they are strategic adjustments that support independence and bring peace of mind to families across the Central Coast. Many of these changes are surprisingly straightforward, but their impact on day-to-day safety is massive.
Prioritizing Bathroom and Stairway Safety
Bathrooms and stairways are hotspots for serious falls. In the bathroom, you have a dangerous combination of wet surfaces, hard flooring, and the need to step in and out of a tub.
Simply installing properly anchored grab bars inside the shower and next to the toilet is one of the most effective changes you can make. They provide a sturdy, reliable handhold right when balance is most precarious.
Here are a few other essential updates to consider:
- Non-slip mats are a must. Place them inside the tub or shower and on the main bathroom floor to add crucial traction.
- A shower seat or bench makes bathing safer by allowing someone to sit, which reduces fatigue and the risk of slipping.
- Make sure sturdy handrails are installed on both sides of every staircase to offer continuous support.
These modifications do more than just add hardware; they build confidence back into daily routines. For more comprehensive ideas, guides on home modifications for elderly safety and comfort offer a wealth of valuable insights.
Enhancing Lighting and Securing Pathways
Poor visibility is a major culprit behind trips and stumbles, especially at night. One of the simplest yet most powerful ways to boost safety is by improving the lighting throughout the home.
A good first step is to swap out dim bulbs for brighter ones, paying special attention to hallways, stairwells, and entryways. Placing nightlights in bedrooms, bathrooms, and connecting hallways creates a safe path for anyone who gets up during the night.
Key Takeaway: Good lighting removes the guesswork from navigating a home. This is especially critical for anyone with vision challenges or those who need to get up frequently during the night.
This isn't just common sense—the evidence backs it up. One community-based study showed that personalized home modifications, guided by occupational therapists, can slash in-home falls by nearly 40%. The most effective fixes were installing grab bars, improving lighting, and adding handrails.
The team here at Central Coast VNA & Hospice, including our skilled Registered Nurses and therapists, helps families apply these principles. Our professionals serve both Monterey and San Benito Counties, assessing homes and recommending effective modifications. For more advice, be sure to check out our home health care tips for fall prevention.
Boosting Stability Through Health and Activity
A fall-proof home is only half of the equation. True, lasting stability comes from within—from maintaining your own health, strength, and daily activity levels.
We all lose some muscle and balance as we get older. But with gentle, targeted physical activity, you can slow that decline and even build back strength. You don't need a fancy gym membership; some of the most effective exercises can be done right in your living room.
Building Strength and Balance at Home
Even small movements can make a huge difference in your stability. The key is to focus on exercises that strengthen your core and leg muscles.
Here are a few safe and simple ideas to get you started:
- Chair-Based Strength Training: While seated, try doing simple leg lifts or marching in place. You can also do bicep curls with light hand weights or a can of soup.
- Gentle Tai Chi: This ancient practice is highly recommended for older adults. Its slow, graceful movements are incredible for improving balance, flexibility, and body awareness.
- Standing Balance Exercises: Hold onto a sturdy countertop and practice standing on one foot for a few seconds. Or, try walking heel-to-toe, like you're on a balance beam.
These activities aren't just about physical strength; they're about building confidence. You can find more ideas and motivation by exploring the importance of staying active and how it fits into a healthy life.
The Role of Medication, Nutrition, and Vision
Beyond exercise, your overall health has a direct line to your risk of falling. Things like dizziness, weakness, or feeling disoriented can dramatically increase your chances of an accident.
Proactive health management isn't just about treating sickness. It's about building a strong foundation for physical stability and stopping accidents before they happen.
First, review all medications. Some prescriptions—or a combination of several—can have side effects like drowsiness or dizziness. It is crucial to have a doctor or pharmacist review everything you take at least once a year.
Don't overlook the basics, either. Proper nutrition and hydration are non-negotiable. Finally, you can't navigate your home safely if you can't see it clearly. This essential guide to eye tests for the elderly explains why regular check-ups are so important.
For families in Monterey County and the surrounding areas, the expert team at Central Coast VNA & Hospice can bring this support right to your door. Our home health Registered Nurses and therapists work with patients to manage medications, create safe exercise routines, and address every aspect of health that keeps you stable and independent at home.
Knowing When to Ask for Professional Help
Sometimes you need to call in an expert. Recognizing that you might need a professional’s eye is one of the smartest things you can do to prevent falls.
A professional brings a new level of expertise to the table. They can create a personalized plan that matches your loved one’s specific health needs and home layout.
This is especially critical if your loved one has complex health conditions or has already experienced a fall. A professional assessment can uncover hidden risks and give you a clear, actionable plan. It’s about more than a checklist; it’s about getting an expert who understands the dance between health, mobility, and the home environment.
The Experts Who Can Help
When it comes to fall prevention, a few key professionals can make a world of difference. Each one brings a unique and vital skill set to the team.
- Occupational Therapists (OTs): Think of an OT as a specialist in daily living. They are experts at helping people perform everyday activities safely and independently. An OT will conduct a thorough home safety assessment and recommend practical solutions.
- Physical Therapists (PTs): A PT is all about improving physical function. They focus on building strength, fine-tuning balance, and improving how a person walks. If a walker or cane is needed, a PT ensures it's the right type and fitted perfectly.
A professional assessment isn't just a list of things to buy. It's a tailored roadmap to safety, built around an individual's unique movements, habits, and health challenges.
How Central Coast VNA & Hospice Supports You
As a nonprofit organization with over 74 years of service here on the Central Coast, we bring this professional support right into your home. Our home health services provide a complete range of care designed to maximize safety for residents in Monterey County, San Benito County, Santa Cruz County, and South Santa Clara County.
Our skilled team, including experienced Registered Nurses and therapists, is ready to provide thorough assessments and hands-on support. A Registered Nurse can help manage medications to reduce side effects like dizziness, while our therapy team can implement the very strength and balance programs we've discussed. We work side-by-side with patients and their families, ensuring the care plan aligns with their goals.
If you're seeing changes in a loved one's stability or mobility, it might be time to take action. You can learn more by reviewing these 5 warning signs that elderly parents may need home health care.
If you feel that professional guidance could benefit your family, our compassionate team is here to listen. Contact us today to learn more about how our nonprofit mission can support your fall prevention goals.
FAQs: Your Fall Prevention Questions Answered
When you're trying to make a loved one's home safer, questions often come up. Our teams at Central Coast VNA & Hospice have put together answers to some of the most common questions we hear from families.
What is the single most important change to prevent falls?
Improving lighting and bathroom safety are the two most impactful changes. Adding bright nightlights in hallways and bathrooms prevents falls in the dark. In the bathroom, installing sturdy grab bars and non-slip mats addresses the highest-risk area in the home.
How can I encourage a parent to use a walker or cane?
Approach the conversation with empathy, framing the device as a tool for independence, not a sign of weakness. Focus on how it enables them to continue activities they love, like walking in the park. A recommendation from a professional, like a Physical Therapist from CCVNA, can also be very persuasive.
What are the best exercises to improve balance?
Gentle exercises that strengthen core and leg muscles are highly effective. We often recommend heel-to-toe walking (with a hand near a wall for support), single-leg stands while holding a sturdy chair, and tai chi for its focus on slow, controlled movements. A Physical Therapist can create a personalized and safe routine.
How often should medications be reviewed for fall risk?
Medications should be reviewed with a doctor or pharmacist at least once a year and anytime a new drug is added or a dose changes. This includes all prescriptions, over-the-counter medicines, and supplements, as some combinations can cause dizziness or drowsiness that increase fall risk.
Can CCVNA help check a home for fall risks?
Yes. A professional home safety assessment is a fundamental part of our home health care services. Our Registered Nurses and Occupational Therapists are trained to spot potential hazards and provide practical, personalized recommendations to families throughout Monterey, San Benito, Santa Cruz, and South Santa Clara counties.
At Central Coast VNA & Hospice, we are dedicated to helping families on the Central Coast live safely and with dignity at home. If you have more questions about preventing falls or our continuum of care from home health to hospice, please contact us. Learn more about our nonprofit mission and how we can support you by visiting our website.
Your Guide to Home Wound Care
When you take on wound care for a loved one at home, you're doing something truly incredible. It can feel like a lot to handle at first, but with the right guidance, you absolutely have what it takes. Getting home wound care right is the key to preventing infections, speeding up the healing process, and keeping your family member comfortable and safe where they want to be—at home.
Your Role in Successful Home Wound Care
Think of this guide as a partner in your corner, here to break down the essentials of cleaning, dressing, and watching over a wound. We want to turn what feels like a clinical, intimidating task into a routine you can handle with confidence. It’s all about giving you the practical skills to be an amazing partner in their healing journey.
For over 74 years, our team at Central Coast VNA & Hospice has focused on one thing: bringing expert clinical care into homes across the Central Coast. We’ve been a part of families' lives throughout Monterey County, San Benito County, Santa Cruz County, and South Santa Clara County, because we know that real healing happens at home.
The Foundation of Effective Care
At its core, effective wound care boils down to three simple things: keeping the area clean, dry, and covered. This straightforward approach is your best defense against complications and creates the perfect environment for the body to do its healing work.
You do not need a medical degree to provide great care, but you do need to be consistent and pay close attention to the details. Your main job is to follow the specific instructions from our clinical team and act as their eyes and ears, as your observations are incredibly valuable.
Central Coast VNA & Hospice was founded on the belief that compassionate, skilled care belongs in the home. Our Registered Nurses and clinical teams provide families with personalized training and ongoing support, ensuring you never feel alone in this journey.
This guide is meant to back up the hands-on training our clinicians provide. It’s a resource you can come back to for a quick reminder or a bit of reassurance as you get more comfortable with the process.
What You Will Learn
We’ve designed this guide to be as clear and actionable as possible, without confusing medical jargon. We will walk you through just the straightforward, step-by-step instructions to give you the tools for success.
We will cover:
- Setting Up Your Space: How to create a dedicated, clean, and organized spot for wound care.
- Cleaning Techniques: The right way to gently clean a wound without causing more pain or introducing germs.
- Applying Dressings: How to apply the specific dressing your nurse recommended to keep the wound protected.
- Monitoring for Issues: How to spot the early warning signs of an infection or other problems.
A Partnership in Healing
Remember, you aren't doing this alone; you are a critical part of the care team. The information you share and the care you provide are essential to the success of the clinical plan our home health professionals have put together.
Central Coast VNA & Hospice is the only local nonprofit that offers a full continuum of care, from home health to palliative and hospice services. This means that if your loved one's needs evolve, our team is right there to ensure the transition is smooth and the care is consistent. We are committed to supporting you and your family every step of the way. Contact us today to learn more about our home health nursing services.
Setting Up Your Wound Care Station
Before you even touch a dressing, the very first step toward safe and stress-free home wound care is creating an organized space. Having a dedicated, clean station is about more than just being tidy—it's your front line of defense against contamination. It also makes the entire process calmer for both you and your loved one.
Think of this as your mission control for healing. Find a spot with good lighting and a hard, non-porous surface you can easily wipe down, like a kitchen counter away from food prep or a small utility cart. The key is to choose a location that's out of the way of daily household hustle to keep things as sterile as possible.
When you're in the middle of a dressing change, the last thing you want is to be scrambling for a roll of tape or a pair of gloves. Having everything you need laid out and within arm's reach is critical to providing the best care without interruption.
Assembling Your Essential Supplies
Your Central Coast VNA & Hospice Registered Nurse will always give you a list of supplies tailored to the specific wound you're caring for. Still, it’s a good idea to have a basic kit on hand and understand what each item is for.
These supplies are essential, and their impact is felt on a global scale. The market for wound and skin care products is projected to hit USD 14,141.47 million by 2035, which really underscores how vital quality supplies are for successful healing at home. You can explore more market trends and the data behind them on Future Market Insights.
Here’s a quick checklist to help you create a foundational wound care kit.
Essential Home Wound Care Supplies Checklist
This table breaks down the basic supplies you'll want to have ready at your station.
| Supply Item | Purpose and Key Considerations |
|---|---|
| Disposable Gloves | A must-have. Always wear a fresh pair to protect both yourself and the person you're caring for from infection. |
| Sterile Saline Solution | This is the go-to for gently cleaning most wounds without harming the delicate, healing tissue. |
| Sterile Gauze Pads | Use these for cleaning the wound itself and for carefully patting the surrounding skin dry. |
| Prescribed Dressings | Your nurse will tell you exactly what you need. This could be anything from simple pads to advanced hydrocolloid or foam dressings. |
| Medical Tape or Wraps | Secures the dressing. Hypoallergenic tape is a great choice, especially for sensitive or fragile skin. |
| Scissors | Keep a clean pair of scissors dedicated only to cutting tape and dressings to avoid cross-contamination. |
| Small Trash Bag | Have a bag ready to immediately toss soiled dressings and used gloves. This simple step is huge for infection control. |
Having these items organized and ready to go makes the entire process smoother and safer for everyone involved.
Key Insight: Consistency is your most powerful tool. By using the same clean, organized space for every dressing change, you create a reliable routine that promotes safety and reduces the chance of errors. This predictability can also be very reassuring for the person receiving care.
Organizing for Safety and Efficiency
Once you've gathered your supplies, the next step is organizing them. A clean plastic bin or a small set of drawers works wonders for keeping everything together and labeled.
Before you begin a dressing change, take a moment to lay out everything you'll need on your clean surface in the order you'll use it. This simple act of preparation transforms the task into a calm, controlled procedure.
This level of preparation and attention to detail is a hallmark of the professional support we provide through our home health care services. Our clinical teams empower families in Monterey County, San Benito County, and the surrounding communities with the practical skills needed for excellent home wound care. By setting up a proper station, you're laying the groundwork for successful healing.
A Practical Guide to Cleaning a Wound
This is where your hands-on care truly begins. It might seem intimidating, but with the right approach, cleaning a wound is a straightforward process. The single most important first step, always, is to wash your hands thoroughly with soap and water before putting on a pair of disposable gloves.
Begin by gently removing the old dressing, being mindful of the skin. Take this moment to look closely at the wound and the skin around it—are there any changes? This initial check is a key part of effective home wound care.
The Cleaning Process Step-by-Step
When it comes to cleaning, gentleness is the guiding principle. Your goal is simply to clear away debris and bacteria without disturbing the delicate new tissue that’s forming. Your CCVNA Registered Nurse will give you the exact cleaning solution needed.
Using sterile gauze moistened with that solution, you’ll clean the wound using a very specific motion:
- Start right at the center of the wound.
- Gently wipe in a single motion from the center toward the outer edge.
- Get a fresh piece of gauze for each and every wipe. This is critical for preventing cross-contamination.
- Keep going with this method until you've cleaned the entire wound bed.
This “center-out” technique actively pulls potential contaminants away from the wound, rather than accidentally pushing them in.
A Note on Cleaning Products: Unless a clinician specifically tells you otherwise, you should avoid using harsh products like hydrogen peroxide or rubbing alcohol. These can actually damage the fragile new cells your body is creating to heal.
After the wound itself is clean, take a fresh piece of sterile gauze and gently pat the healthy skin around the wound until it's completely dry. Getting the skin dry is essential for making sure the new dressing sticks properly.
Handling Soiled Materials Safely
Properly disposing of used supplies is a critical part of infection control. As you work, place all soiled items—your used gloves, the old dressing, and dirty gauze—directly into the small trash bag you set up at your station.
Once you’re all done, seal the bag tightly and toss it in your regular household trash. It’s a simple professional practice that helps contain any bacteria, protecting everyone in the household.
The commitment to these small but vital steps is what defines excellent care. It’s a calling many of our team members feel deeply, and you can learn more about how to make a difference in our community through the work we do.
Building Your Confidence
Remember, this guide is here to back up the personalized, hands-on training your Central Coast VNA & Hospice clinician provides. Every wound is unique, and the care plan we create is tailored to meet those specific needs, whether you're in Monterey, San Benito, Santa Cruz, or South Santa Clara County.
Your role is to follow that plan with care and attention. With each dressing change you complete, you'll feel your confidence grow, knowing our nonprofit team is right here to support you.
How to Apply a New Wound Dressing
Okay, you've cleaned the wound and the skin around it is nice and dry. Now comes the most important part of home wound care: protecting it with a fresh dressing. This isn't just about covering the wound; the specific dressing your CCVNA clinical team chose is designed to create the perfect moisture balance for proper healing.
The first rule? Keep everything sterile. Once you open the new dressing package, only touch the very edges to prevent germs from getting onto the sterile pad that will sit right on the wound.
Positioning and Securing the Dressing
Gently place the dressing directly over the wound. You're aiming for the sterile pad to cover the entire wound bed, with about an inch of overlap onto the healthy skin around it to create a good seal.
With the dressing in position, it's time to secure it. Use the medical tape your nurse recommended to tape down the edges so it's snug, but never so tight that it causes discomfort or cuts off blood flow.
Here’s a quick rundown of what to do:
- Handle by the Edges: Never touch the middle of the sterile dressing pad.
- Center and Cover: Make sure the pad covers the whole wound plus a small margin of healthy skin.
- Secure Firmly: Tape all sides of the dressing down. It should be snug, not tight.
This visual breaks down the core cycle of home wound care, from cleaning all the way to monitoring.
As you can see, these three steps—Clean, Protect, and Monitor—are part of a continuous loop that gives the body the support it needs to heal itself.
Tips for Tricky Areas and Tracking
Some spots are just harder to bandage than others, like a heel, elbow, or any other joint that’s always moving. For these tricky areas, your CCVNA Registered Nurse can show you specific taping techniques that create a more flexible, secure dressing.
Pro Tip: Get into the habit of writing the date and time of the dressing change on a piece of medical tape and sticking it on the dressing. This tiny step is incredibly helpful for tracking how the wound is healing and keeping you on a consistent schedule.
A consistent schedule and clear documentation are huge parts of a successful care plan. In fact, clear communication about these details is a cornerstone of good advance care planning, making sure everyone involved knows how things are progressing.
When to Call for Professional Help
When you're managing wound care at home, you are the first and most important line of defense. Following the steps for cleaning and dressing is vital, but your role as an observer is just as critical.
Trust your intuition. After a few days of handling the care routine, you’ll get a feel for what “normal” healing looks like. If something seems different or feels off, don't ever dismiss that feeling.
Knowing exactly what to look for empowers you to act quickly. Catching the earliest signs of a complication is key to stopping a minor issue from turning into a serious problem.
Red Flags That Require a Phone Call
Think of your Central Coast VNA & Hospice Registered Nurse as your partner in this. They count on your updates to make sure the care plan is working as it should, and a quick phone call might give you peace of mind or confirm a visit is needed.
Never feel like you’re bothering the clinical team. They're available to families across Monterey County, San Benito County, Santa Cruz County, and South Santa Clara County for this very reason.
Here are the most common red flags that mean it's time to pick up the phone:
- New or Worsening Pain: If the pain suddenly gets worse or doesn't respond to prescribed medication.
- Spreading Redness: Redness spreading outward from the wound is a classic sign of infection.
- Increased Warmth: The skin around the wound feels hot to the touch compared to the surrounding skin.
- Unusual Drainage: Any drainage that is thick, cloudy, green, yellow, or has a foul smell.
- Fever or Chills: A body temperature of 101°F (38.3°C) or higher, especially when paired with chills.
Key Takeaway: You aren't expected to diagnose the problem. Your job is simply to report what you see. Describing these signs over the phone gives your CCVNA nurse the information they need to guide you on the next steps.
For families caring for an older adult, recognizing these changes is especially important. If wound care is becoming one of several growing concerns, it might be helpful to review these 5 warning signs that your elderly parents need home health care.
When to Call a Clinician Red Flag Chart
When you're in the thick of it, it helps to have a quick reference. This chart breaks down the most common warning signs and what to do when you see them.
| Symptom or Sign | What It Might Mean | Action to Take Immediately |
|---|---|---|
| Spreading redness | Infection (Cellulitis) | Call your CCVNA nurse or clinician. |
| New or worse pain | Deep infection or complication | Call your CCVNA nurse or clinician. |
| Thick, smelly drainage | Bacterial infection | Call your CCVNA nurse or clinician. |
| Fever over 101°F (38.3°C) | Systemic infection | Call your CCVNA nurse or clinician. |
| Hot to the touch | Inflammation from infection | Call your CCVNA nurse or clinician. |
| Uncontrolled bleeding | Severe vessel injury | Call 911 immediately. Apply pressure. |
| Wound opens up | Dehiscence (surgical wound separation) | Call 911 immediately. Cover with a clean, moist dressing. |
Think of this table not as a diagnostic tool, but as a guide to empower you to make a confident, timely call. Your quick action can make all the difference.
When to Seek Immediate Emergency Help
Some situations are a clear step above a routine call to your nurse. These require immediate emergency medical attention.
Call 911 without delay if you observe:
- Uncontrolled Bleeding: The wound is soaking through a dressing quickly and won't stop even after 10 minutes of direct, firm pressure.
- Signs of Shock: This includes symptoms like confusion, dizziness, pale or clammy skin, and a rapid pulse.
- A Wound Reopening: The edges of a surgical incision have pulled apart, exposing deeper tissues.
In a worst-case scenario involving severe bleeding, knowing how to apply a tourniquet can be a crucial, life-saving skill while you wait for help. Your vigilance is the bridge between routine care and necessary clinical intervention.
Frequently Asked Questions About Home Wound Care
It's completely normal to have questions when helping someone heal at home. Families across Monterey County, San Benito County, Santa Cruz County, and South Santa Clara County often ask us about the practical realities of wound care.
For over 74 years, our nonprofit has been built on providing this kind of compassionate, expert support. We believe that giving you the right knowledge is a powerful part of the healing journey itself.
How often should I change the wound dressing?
This completely depends on the type of wound and the specific dressing being used. Your CCVNA Registered Nurse will give you a clear, personalized schedule to follow. Changing a dressing too often can disrupt healing, while waiting too long can increase infection risk, so sticking to the prescribed schedule is critical.
Is it okay for the person I'm caring for to shower?
Whether showering is safe hinges on the wound's location, its healing stage, and the type of dressing. In many cases, a special waterproof dressing can be used to protect the wound completely. Always check with your home health nurse first, as they will provide specific instructions to keep the area dry and safe.
What if I accidentally touch the sterile part of the dressing?
Don't panic—it happens. If you even think you might have contaminated the sterile part of the dressing, the safest thing to do is to discard it and start over with a fresh one. Protecting that sterility is non-negotiable for preventing infection, which is why having a few extra supplies on hand is always a good idea.
Can diet really affect how a wound heals?
Absolutely. Nutrition is a cornerstone of healing, as the body needs specific raw materials to build new tissue and fight infection. Key nutrients include protein for tissue creation, Vitamin C for collagen production, and zinc for cell repair. Staying well-hydrated by drinking plenty of water is also crucial for transporting these nutrients to the wound site.
What if the person's condition changes and they need more help?
This is a valid concern and precisely why CCVNA's continuum of care is so valuable. If your loved one's needs evolve beyond what home health can manage, our team coordinates seamlessly with our palliative and hospice care specialists. This ensures a smooth transition to the right level of care, managed by a team you already know and trust. We are committed to providing continuous, compassionate support every step of the way. To learn more, you can read about the benefits of home health care in Monterey, CA.










