Choosing between hospital and hospice care is a deeply personal decision. The two paths have different goals. Hospital care aims to cure illness and prolong life with aggressive treatment.
Hospice care shifts the focus to maximizing comfort and quality of life. This happens when a cure is no longer the main goal. Choosing hospice is not giving up; it is a choice to live the final months with dignity and support.
Understanding Your End-of-Life Care Options
When a serious illness progresses, the path forward isn't always clear. The decision between hospital treatments and hospice can feel overwhelming. The first step is to understand the core philosophy behind each option.
This guide brings clarity to families in Monterey County, San Benito County, Santa Cruz County, and South Santa Clara County. Central Coast VNA & Hospice is a local, nonprofit provider with over 74 years of community service. We help you navigate these sensitive decisions with expert, compassionate care.
This chart helps show the different priorities of hospital care versus hospice care.
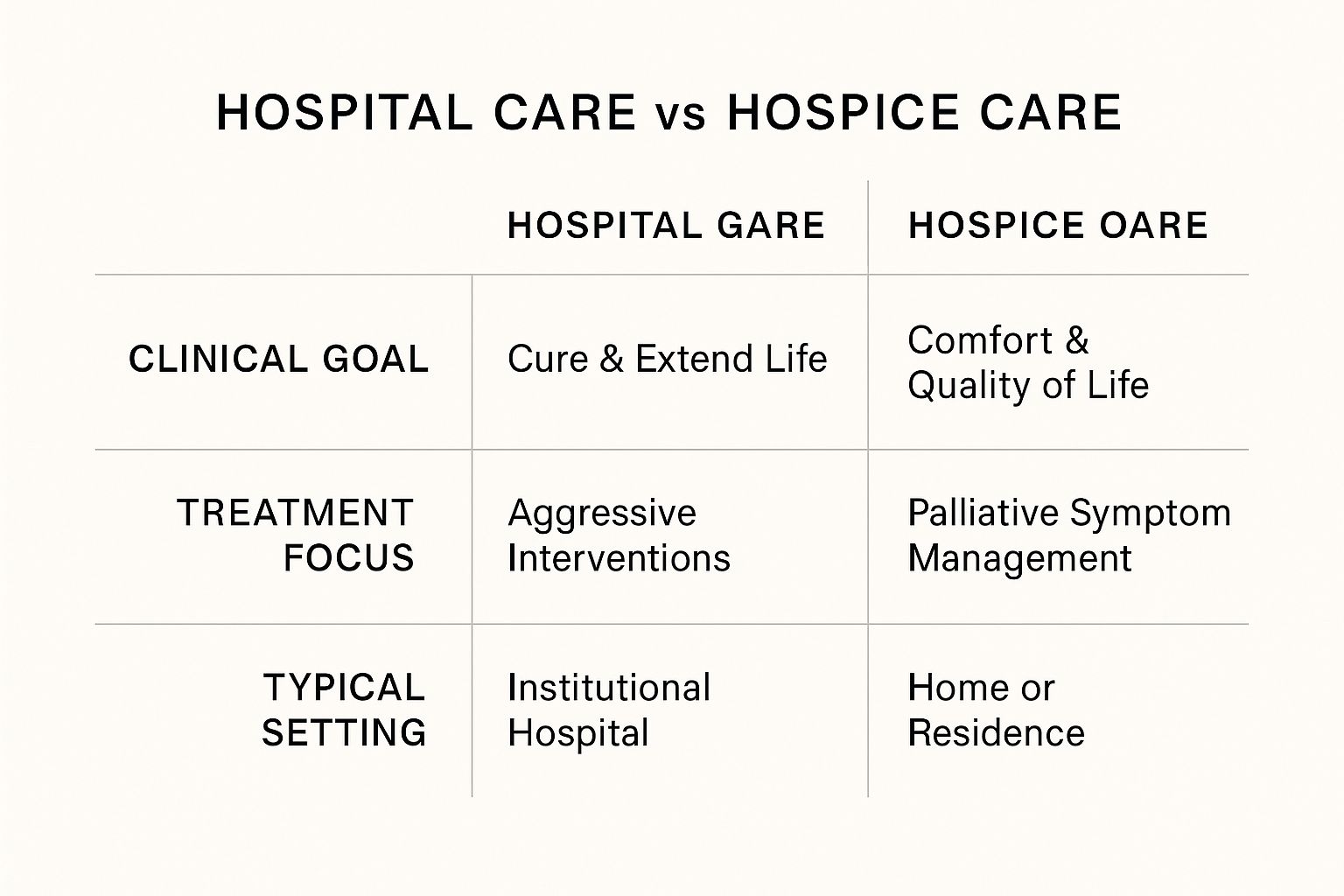
As you can see, the two approaches prioritize different outcomes. This directly impacts a person's daily experience and environment.
Hospital vs. Hospice at a Glance
To quickly understand the core differences, this table breaks down the two approaches.
| Care Aspect | Hospital Care | Hospice Care |
|---|---|---|
| Primary Goal | Cure the illness and prolong life. | Manage symptoms and maximize comfort. |
| Typical Location | Clinical setting (hospital). | Patient's home or a home-like facility. |
| Treatment Approach | Aggressive and curative (e.g., surgery, chemo). | Palliative (comfort-focused) care. |
While both provide medical expertise, the philosophy guiding that expertise is what truly sets them apart.
Key Distinctions in Care Philosophy
The choice comes down to what matters most to the patient in their final chapter.
- Hospital care is centered on curative treatment. Medical teams use every tool available, from surgery to intensive care, to fight the disease. This path is ideal when a cure or significant recovery is still considered possible.
- Hospice care begins when the focus shifts from curing the illness to caring for the person. The priority becomes comfort, peace, and emotional well-being. Hospice allows the illness to take its natural course, free from aggressive medical interventions.
Defining Success Differently
In a hospital, success is measured by clinical outcomes like better lab results or stabilized vital signs. It’s an environment built for recovery.
Hospice defines success by the patient's quality of life. Is their pain managed? Are they receiving emotional support? You can learn more about preparing for these talks in our guide on end-of-life care planning.
Comparing Clinical Goals and Medical Treatment

The biggest difference between hospital and hospice care is their core mission. In a hospital, the entire team focuses on curing disease and extending life. This means pursuing aggressive treatments.
Hospice care redefines what "success" looks like. When a cure is no longer likely, the focus shifts to caring for the whole person. Hospice ensures a patient's final chapter is lived with comfort, dignity, and peace.
The Shift from Curative to Comfort Care
A hospital medical plan is built around curative treatments like surgery or chemotherapy. The goal is to buy the patient more time.
Hospice care follows a different philosophy. The hospice team, led by a physician and supported by a Registered Nurse and Hospice Aide, provides expert symptom management. This isn't giving up; it's changing the goal to quality of life.
“Our philosophy at Central Coast VNA & Hospice is that every individual deserves to live their final days with dignity and comfort. We craft personalized care plans with our hospice physicians to manage symptoms aggressively, so patients can focus on meaningful time with their loved ones, not on their pain.”
Crafting a Personalized Comfort Plan
Medical treatment in hospice is deeply personal. It centers on the patient's specific symptoms and wishes. The goal is to control pain, nausea, and other distressing symptoms.
The interdisciplinary hospice team creates a plan that may include:
- Pain Management: Using medications to keep the patient as comfortable as possible.
- Symptom Control: Addressing issues like fatigue and breathing difficulties.
- Medical Equipment: Providing a hospital bed or oxygen for use at home.
- Personal Care: Assisting with daily activities like bathing to maintain dignity.
This focus on comfort often allows patients to remain in their homes in places like Monterey County and Santa Cruz County. By providing 24/7 on-call support, hospice reduces the need for stressful emergency room visits. This breaks the cycle of hospital dependency. For more details, explore what palliative care and hospice are.
How Medical Roles Change
In a hospital, doctors and nurses focus on executing a treatment plan to combat disease.
In hospice, the team works with the patient and family to honor their wishes. A hospice physician from Central Coast VNA & Hospice oversees the care plan. A Registered Nurse makes regular visits to manage symptoms and educate the family.
Emotional and Spiritual Support for the Whole Family

The end-of-life journey is an emotional and spiritual experience for the patient and their loved ones. A hospital's focus is medical intervention, which can feel impersonal.
Hospice care provides holistic support, placing emotional and spiritual well-being at the center of its mission. Central Coast VNA & Hospice operates on the philosophy that the family is part of the unit of care.
A Team Dedicated to the Whole Family
A hospital patient might have a brief visit from a social worker or chaplain. Hospice offers an entire interdisciplinary team to support the patient and their loved ones.
This team includes:
- Medical Social Workers: Professionals who help families manage stress and find resources.
- Chaplains: Spiritual guides who honor each family’s unique beliefs and traditions.
- Bereavement Specialists: Counselors who provide grief support for up to a year.
Our nonprofit mission is to create a peaceful, supportive atmosphere. We believe this is best achieved in the familiar comfort of home.
Honoring Patient Wishes and Providing Peace of Mind
Studies show that most patients prefer to die at home. Yet, hospitals remain a common place of death. Hospice bridges this gap.
By bringing expert care into the home, we make it a safe option. This allows a patient's final wishes to be honored. For some, this support is supplemented by the non-medical end-of-life care provided by death doulas.
Spiritual Care Tailored to Individual Beliefs
Spiritual distress can show up as fear or a loss of meaning.
"Our role is to listen deeply and walk alongside families, providing a compassionate presence without judgment. We help them find sources of comfort and meaning, whether that comes from faith, nature, music, or simply sharing stories."
Spiritual support in hospice is not about pushing religion. Chaplains from Central Coast VNA & Hospice are trained to meet people where they are. Learn more about our approach to spiritual care in hospice.
Navigating the Financial Costs of Care
The financial side of end-of-life care is a major source of stress. A long hospital stay can lead to a mountain of medical bills. Every test and procedure adds up.
This financial pressure comes at the worst possible time. Understanding the financial differences between hospital and hospice care is important.
The Comprehensive Hospice Benefit
Hospice provides great financial relief. For patients who qualify, hospice care is typically covered 100% by Medicare. This benefit is also mirrored by Medicaid and most private insurance plans.
This all-inclusive coverage is designed to remove money as a barrier. Families can focus on spending meaningful time together.
The Medicare hospice benefit is comprehensive, covering:
- The entire hospice team: All visits from the Registered Nurse, Hospice Aide, Social Worker, and Chaplain.
- Medical equipment: A hospital bed, oxygen, or wheelchair delivered at no cost.
- Medications: All prescriptions for managing pain and symptoms.
- Medical supplies: Items like bandages and catheters.
At Central Coast VNA & Hospice, our nonprofit mission is to ensure that financial stress never stands in the way of high-quality, compassionate care. Our team helps families in Monterey County and surrounding areas access these benefits so they can focus on their loved one.
Comparing Hospital and Hospice Costs
Hospital care operates on a fee-for-service model. Every blood test and scan is a separate line item on the bill. Out-of-pocket costs can be staggering.
Hospice is usually paid through a per diem rate. This single daily rate covers all services, equipment, and medications. For those planning ahead, policies like critical illness insurance can also offer support.
As a local nonprofit serving the Central Coast for over 74 years, we are committed to making care accessible. We walk families through the insurance process. You can find out more in our guide on how to pay for hospice care.
How Environment Shapes the End-of-Life Experience

Where a person spends their final days shapes their sense of peace. A hospital is an institutional environment built for medical intervention. It can lack personal space.
Hospice care operates on a different philosophy: comfort is best found in familiar surroundings. Our services are brought to wherever a patient calls home. This could be a private home in Monterey or an assisted living facility in Santa Cruz County.
The Power of Familiarity and Autonomy
Being at home gives a person a sense of control. They can be surrounded by memories and welcome loved ones without visiting hours. This can reduce anxiety for the patient and family.
At Central Coast VNA & Hospice, this principle is the bedrock of our care. We empower patients to remain where they feel most secure.
“A person’s home is their sanctuary. Our goal is to bring expert medical care into that sanctuary, adapting to their needs rather than forcing them to adapt to an unfamiliar clinical setting. It’s about honoring their life, right where they lived it.”
Reducing Hospital Dependency with 24/7 Support
One of the biggest fears for families is a medical crisis at night. This anxiety often drives people to the emergency room.
Hospice care is designed to eliminate that fear. Central Coast VNA & Hospice provides 24/7 on-call nursing support. This gives families a direct line to a Registered Nurse at any time. This immediate access helps manage symptoms at home and prevents most ER visits.
The Global Need for Home-Based Care
While we have robust hospice services on the Central Coast, this is not a global reality. According to the World Health Organization, only about 14% of people who need palliative care currently receive it. You can learn more about these global care disparities.
This data underscores the importance of organizations like ours. We are dedicated to ensuring everyone in our community has access to comfort and dignity.
Our philosophy is simple: end-of-life care should revolve around the patient’s life. By enabling them to stay in their cherished surroundings, we help preserve their identity.
Deciding When It Is Time for Hospice
Knowing when to shift from curative treatments to hospice care is a profound decision. It is a choice rooted in love.
The technical requirement for hospice is simple. A doctor must certify that a patient has a life-limiting illness with a prognosis of six months or less. But that is only one part of a bigger picture.
Recognizing the Signs
You may see signs that the burdens of treatment outweigh the benefits. These shifts can indicate it is time to talk about comfort care.
Look for these key changes:
- Frequent Hospitalizations: A revolving door of ER visits can be exhausting.
- Declining Function: A drop in the ability to handle daily activities like walking or eating.
- Increasing Symptoms: Pain, shortness of breath, or fatigue become harder to manage.
The Value of Early Conversations
Waiting for a crisis makes these decisions harder. Advance care planning is very important. Talking openly about end-of-life wishes gives everyone clarity.
These conversations are about values, not just medical directives. Exploring when to call hospice sooner allows you to take full advantage of the support hospice provides.
It is also important to remember that end-of-life needs are not just for cancer. The National Hospice and Palliative Care Organization (NHPCO) notes that many people receive hospice for heart disease, dementia, and lung disease (NHPCO, 2021).
Palliative Care as a Bridge
Sometimes, a person needs help with symptoms but is not ready for hospice. This is where palliative care acts as a vital bridge. It can be provided alongside curative treatments.
At Central Coast VNA & Hospice, we see palliative care as an extra layer of support. It helps manage the physical and emotional burdens of a serious illness, giving patients and families in Monterey County and San Benito County the strength to navigate their healthcare journey.
This service can ease the transition long before hospice becomes the right path. Our goal is to empower you with the right information and support.
FAQs: Your Questions About Hospice and Hospital Care
Navigating end-of-life decisions brings up many questions. Here are answers to some common questions we hear from families in Monterey County.
1. Can a patient still see their primary doctor in hospice?
Yes. A patient’s relationship with their primary care physician is important. We honor that connection. Central Coast VNA & Hospice works in partnership with a patient's chosen doctor. Our hospice physician complements their care, not replaces it.
2. Who is the primary carer in hospice at home?
A family member or close friend usually steps into the role of primary carer. This person handles the patient's day-to-day needs. Our job at Central Coast VNA & Hospice is to empower that individual with training, resources, and 24/7 on-call support.
3. What happens if a patient’s condition improves?
If a patient's health stabilizes, they can be discharged from hospice care. This is a wonderful outcome. The patient can go back to pursuing curative treatment. They can re-enroll in hospice later if needed.
4. Can you be in hospice and still go to the hospital?
The goal of hospice is to manage symptoms at home. Our 24/7 on-call support is designed to handle medical issues before they become emergencies. If a symptom becomes too severe, the hospice team might arrange a short hospital stay for symptom control, but the goal remains comfort, not cure.
5. Do I have to give up all medical treatments in hospice?
You agree to shift away from curative treatments for your terminal illness. You do not give up medical care. You continue to receive treatments focused on comfort, such as medications for pain and therapies to improve quality of life.
Making the right choice for end-of-life care is a profound act of love. If you have more questions or want to understand how our continuum of care can support your family, the compassionate team at Central Coast VNA & Hospice is here to help. Contact us today to learn more about our services in Monterey County, San Benito County, Santa Cruz County, and South Santa Clara County. https://ccvna.com
