One of the most difficult questions families face is: how do you know when hospice is needed? The answer often becomes clear when the focus of care shifts. Hospice is the right path when the goal is no longer to cure an illness, but to maximize comfort, dignity, and quality of life.
Defining the Shift to Comfort-Focused Care

Choosing to begin hospice care is a deeply personal and often challenging decision for everyone involved. It marks a significant transition away from aggressive, curative treatments toward a philosophy centered on comfort and peace.
This change is not about giving up. It is about making a proactive choice for compassionate support that honors a person’s final wishes.
For over 74 years, Central Coast VNA & Hospice has been a trusted, nonprofit partner for families navigating this journey. Our mission is to provide expert, mission-driven care that respects the values and goals of each individual we serve across Monterey County, San Benito County, Santa Cruz County, and South Santa Clara County.
Understanding the Goal of Hospice
The primary goal of hospice is to improve the quality of a person's remaining life. Instead of focusing on endless medical tests and treatments aimed at a cure, the team concentrates on managing symptoms. This means tackling issues like pain, anxiety, and shortness of breath so the person can live as fully and comfortably as possible.
This compassionate approach is carried out by an experienced, interdisciplinary team that includes:
- A primary or hospice physician
- A Registered Nurse to manage clinical care
- A Hospice Aide to assist with personal care like bathing and dressing
- A Chaplain for spiritual support
- A Medical Social Worker for emotional and practical support
When Is the Right Time to Consider Hospice?
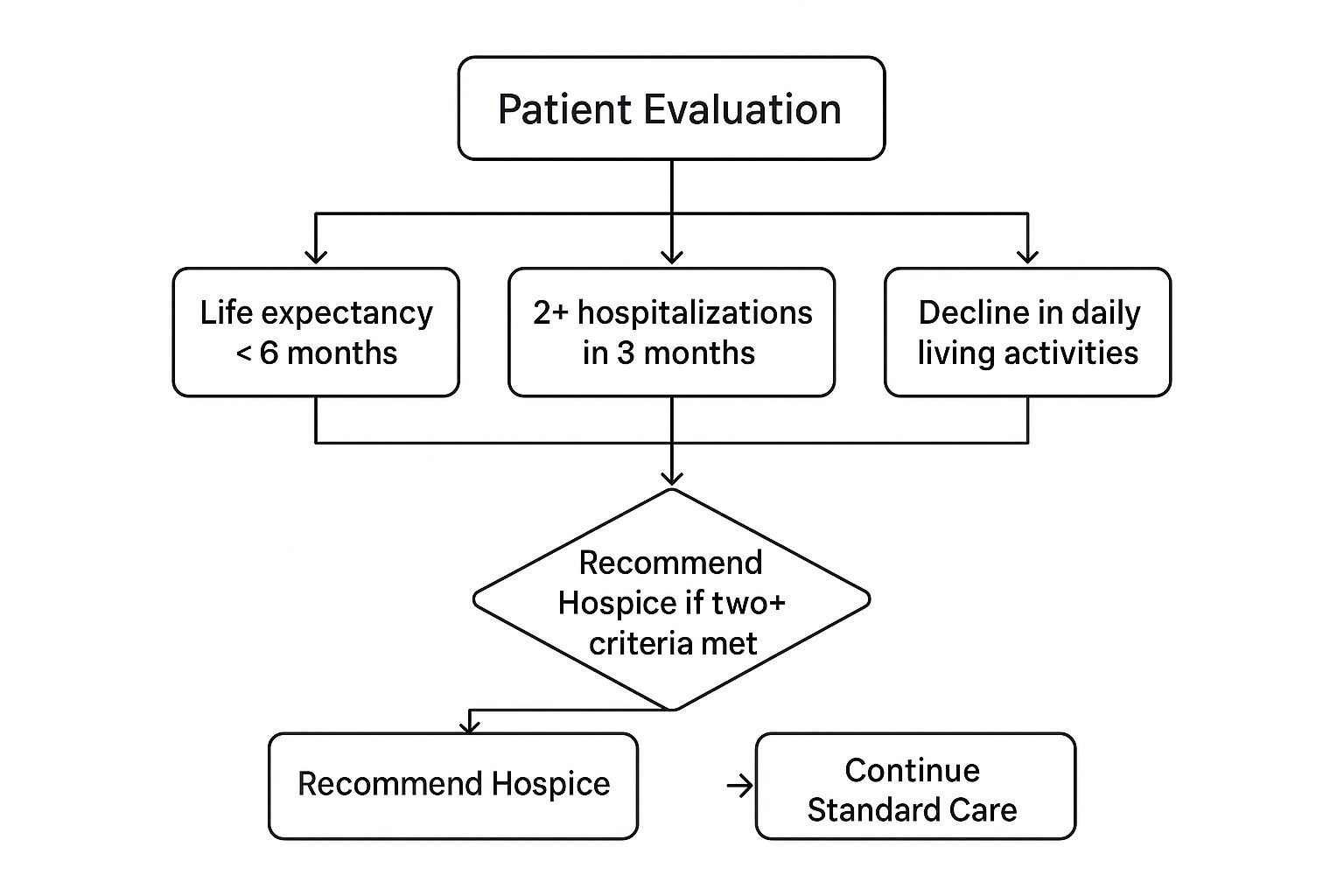
Determining the right moment requires open and honest conversations between the patient, their family, and their doctor. Generally, hospice is appropriate for someone with a life-limiting illness who has a prognosis of six months or less, if the disease runs its natural course.
It's a vital service that helps many Americans. According to the National Hospice and Palliative Care Organization (NHPCO), about half of all Medicare beneficiaries who passed away in 2021 utilized hospice care (NHPCO, 2023). However, enrollment times vary widely, which often points to referrals happening too late.
The table below breaks down the fundamental differences between curative medical treatment and the comfort-focused philosophy of hospice care.
Comparing Curative Treatment vs. Hospice Care
| Focus Area | Curative Treatment | Hospice Care |
|---|---|---|
| Primary Goal | To cure the disease and prolong life | To enhance quality of life and provide comfort |
| Treatment Approach | Aggressive (surgery, chemotherapy, etc.) | Palliative (pain and symptom management) |
| Care Setting | Typically hospitals and clinics | Primarily in the patient's home or a facility |
| Team Focus | Medical specialists treating the disease | Interdisciplinary team addressing holistic needs |
| Emotional Support | Often secondary to medical treatment | A core component for patient and family |
| Family Involvement | Family provides support, but is not the focus | Family is central to the care plan |
As you can see, the shift to hospice represents a change in priorities, not an absence of care. It’s about choosing a different kind of care—one that puts the person, not the disease, at the center.
Hospice is not a place, but a philosophy of care. It focuses on bringing comfort, dignity, and peace to patients wherever they call home, ensuring their final chapter is lived on their own terms.
By choosing hospice, families can get back to what matters most: spending meaningful time together. At Central Coast VNA & Hospice, we are here to guide you through this process with compassion and expertise. Contact us today to learn more about our services.
Observing Key Physical and Clinical Indicators
When you're close to someone with a serious illness, you start to notice subtle shifts. It’s not just one thing, but a collection of changes that signal the body is weakening and could benefit from a different kind of care.
While every person's experience is unique, there are specific clinical signs that doctors look for when considering hospice. These are real-world changes that family members are often the first to see.
Recognizing these signs helps families understand when it might be time to shift the focus toward expert symptom management. Our Registered Nurses and Hospice Aides are specialists in managing these exact symptoms, all with the goal of enhancing comfort and preserving dignity.
Worsening Symptoms and Decline in Function
One of the most obvious signs is when a person’s ability to handle everyday tasks starts to slip. Medically, this is called a decline in Activities of Daily Living (ADLs).
You might see a loved one who was once independent now struggling with simple things. It often looks like this:
- Needing help to bathe or get dressed
- Struggling to get from the bed to a chair
- Losing control of their bladder or bowels
This physical decline usually comes with symptoms that are becoming harder to control. Think of persistent pain, constant shortness of breath, nausea that won't go away, or an overwhelming sense of fatigue. When usual treatments are no longer effective, it’s a strong sign that hospice care is needed.
Significant Weight Loss and Loss of Appetite
Another tell-tale clinical sign is noticeable, unintentional weight loss. This is often paired with a sharp drop in appetite. As the body grapples with a serious illness, it can lose its ability to use nutrients correctly, leading to cachexia, or wasting syndrome.
This is a profound metabolic change, not simply a matter of a person not feeling hungry. At this point, the goal of care naturally shifts from pushing food and fluids to honoring what the body is saying and focusing on comfort. A hospice team's role is to manage any discomfort and support the patient's choices.
A common misconception is that hospice is only for cancer patients. While many hospice patients have cancer, data shows that a significant number have other conditions. Understanding the full range of indicators beyond a specific diagnosis is key. Discover more insights on hospice demographics and access patterns.
An Increase in Hospital or ER Visits
A revolving door of emergency room visits and hospital stays is often a clear indicator that an illness is progressing. If your loved one has been in the hospital two or more times in recent months for the same issue without lasting improvement, it is time to ask a tough question. Are these hospital visits truly helping them meet their goals for quality of life?
Each hospitalization can be incredibly draining, both physically and emotionally. Choosing hospice brings care directly into the home, whether in Monterey or San Benito County. This can prevent exhausting and stressful trips to the hospital. To get a better sense of the formal criteria, our guide on how doctors determine hospice eligibility is a great resource.
Listening to Emotional and Quality of Life Cues

Beyond the lab results and clinical charts, some of the most powerful signs come directly from your loved one. Their emotional state, words, and wishes are vital information. These cues are deeply personal and tell a story about their readiness to shift focus from fighting an illness to finding peace.
Paying close attention to these emotional and quality-of-life signals is a profound act of love. It’s about truly hearing them and acknowledging that they are the expert on their own journey.
Recognizing a Shift in Perspective
You might start to notice a significant change when someone begins pulling back from activities and people they once cherished. Maybe they no longer ask about their favorite sports team or gently decline visits from close friends.
This withdrawal isn't always a sign of depression. Often, it's a way of conserving precious energy and a natural turning inward as they prepare for what’s ahead.
Another unmistakable sign is when they express a clear desire to be at home instead of in a hospital. After an endless cycle of appointments and hospital stays, many people say, “I’ve had enough. I just want to be home.” That statement is a powerful declaration of their priorities.
Honoring this wish to be home is a cornerstone of hospice care. We know comfort isn't just about managing physical pain—it's about the deep, restorative peace that comes from being in a familiar, loving environment, surrounded by the people and memories that matter most.
The Emotional Toll of a Long Illness
Living with a terminal illness is draining. The exhaustion runs deeper than the physical body; it takes a heavy emotional and spiritual toll. It’s not uncommon to hear someone say they feel "done fighting," which is an honest admission of exhaustion.
At Central Coast VNA & Hospice, our Chaplains and Medical Social Workers are here to support patients and families through these complex emotional roads. They create a safe, compassionate space to explore feelings, talk through fears, and find meaning. This type of whole-person care is central to our mission as a nonprofit provider on the Central Coast.
These emotional cues are just as important as any clinical symptom. They are the vital signs of a person’s inner world, helping guide families toward a decision that honors their loved one’s wishes.
Starting the Conversation About Hospice Care

Broaching the topic of hospice care is often the hardest step for families. It feels heavy, final, and many worry it’s like admitting defeat. But this conversation can be one of the most loving and powerful things you can do.
When you frame it as a way to honor their wishes and reclaim control, the entire dynamic shifts. It becomes a moment of connection, not a moment of giving up. The key is to approach it with empathy, gentleness, and a genuine desire to listen.
Finding the Right Time and Tone
Timing is everything. Look for a quiet, private moment when you can speak freely without being rushed. A calm afternoon at home often works best.
Lead with your heart, not a medical agenda. Start with open-ended questions that center on their feelings and goals to show you respect their autonomy.
You could try saying something like:
- “I’ve been thinking about what’s most important to you these days. Can you tell me what a good day looks like for you?”
- “We’ve been in and out of the hospital so much. I’m wondering how you’d feel about focusing more on being comfortable at home.”
- “What are you worried about most right now? I want to make sure we're doing everything we can to help with those fears.”
Questions like these open a door to a real dialogue about their priorities. It can also be helpful to understand the specifics yourself; you can read more about palliative vs. hospice care in our detailed guide.
Focusing on Empowerment and Control
One of the greatest gifts of hospice is how it hands control back to the patient and their family. Instead of constantly reacting to the disease, you get to be proactive about how you want to live the time that remains.
Discussing hospice is not about giving up. It is about shifting focus to ensure your loved one's final chapter is written on their terms, filled with as much peace and comfort as possible.
When you have the conversation, emphasize that hospice adds a layer of expert support. Explain that a dedicated team from Central Coast VNA & Hospice can come right to the home. They manage pain and control symptoms so everyone can focus on quality time together.
This reframes the entire concept. Hospice becomes a new beginning, one focused on living as well as possible, for as long as possible.
Arranging Hospice Care on the Central Coast
Once your family feels that hospice might be the right path, the next steps can feel overwhelming. But the process is designed to be supportive and clear, taking the stress off your shoulders. It all starts with a simple conversation and an evaluation.
The first official step is usually a physician’s referral, which confirms a life-limiting prognosis. You can also contact Central Coast VNA & Hospice directly to request a hospice evaluation. We’ll then coordinate with your loved one’s doctor to get the necessary orders.
The Informational Visit and Assessment
After you make that initial contact, a Registered Nurse can schedule an informational visit. This is a no-pressure, no-obligation meeting that can happen wherever your loved one calls home in Monterey, Santa Cruz, or South Santa Clara County. The nurse will assess your loved one's specific needs, answer every question, and explain how our team provides support.
During this visit, you'll get a clear picture of:
- How a personalized care plan is created.
- The roles of each team member, from the Hospice Aide to the Chaplain.
- How we handle getting all necessary medical equipment and supplies delivered to the home.
- The 24/7 on-call support that's always available for urgent needs.
Understanding Financial Coverage
Worrying about cost should never stand in the way of getting excellent care. Hospice is a fully covered benefit under Medicare Part A, Medi-Cal, and most private insurance plans. This comprehensive coverage removes the financial burden by paying for the hospice team's services, medications, and equipment.
As a nonprofit organization with 74 years of local history on the Central Coast, we are committed to providing care to everyone who is eligible. For a complete overview of what our hospice care entails, take a look at A Compassionate Guide to Hospice Care on the Central Coast.
Choosing hospice is a significant decision. With the right information and support, it can bring peace and comfort to your entire family.
Frequently Asked Questions About Hospice Care
When you're faced with the decision to start hospice care, a million questions can run through your mind. It’s an emotional and often confusing time. Getting clear, straightforward answers is one of the most reassuring things a family can experience.
Here are some of the most frequent questions we hear from families across Monterey County and the surrounding areas. We want to clear up the confusion and give you the peace of mind you need.
Does choosing hospice mean we are giving up hope?
Absolutely not. Choosing hospice isn’t about giving up hope; it’s about changing what you hope for. The focus shifts from hoping for a cure to hoping for comfort, peace, and quality time with loved ones.
It’s an active decision to ensure the time someone has left is lived with dignity and without pain. Hope becomes about good days, meaningful moments, and a peaceful environment.
Can a patient leave hospice care if their condition improves?
Yes, they can. A patient always has the right to stop hospice care at any time, for any reason. If their condition stabilizes or they decide to try a new curative treatment, they can be discharged from the hospice program.
The care plan must always reflect the patient's current needs and wishes. If their health declines again later, they can easily re-enroll in hospice when the time is right.
Who pays for hospice care?
Hospice care is covered by Medicare Part A, Medi-Cal, the Department of Veterans Affairs, and most private insurance plans. This comprehensive coverage includes everything from the hospice team's services to the medical equipment, supplies, and medications related to the terminal illness.
As a nonprofit organization that's been serving the Central Coast for over 74 years, Central Coast VNA & Hospice is dedicated to caring for all eligible patients. Our mission is to ensure everyone in our community can access compassionate end-of-life support.
What is the difference between palliative care and hospice care?
This is a great question, as the two are related but serve different purposes. Palliative care can start at any point during a serious illness, even while someone is still receiving curative treatments. The main goal is to relieve symptoms and stress to improve quality of life.
Hospice care is a specific kind of palliative care for people with a life-limiting illness and a prognosis of six months or less who are no longer seeking a cure. At Central Coast VNA & Hospice, we are proud to offer a full continuum of care, allowing for a smooth transition from home health to palliative care to hospice if and when a patient's needs evolve.
Where is hospice care provided?
Hospice care is provided wherever the patient calls home. This is most often their private residence, but it can also be a skilled nursing facility, an assisted living community, or a board and care home.
Our team at Central Coast VNA & Hospice brings expert medical, emotional, and spiritual support directly to patients across Monterey County, San Benito County, Santa Cruz County, and South Santa Clara County. The goal is to provide comfort in a familiar setting.
The team at Central Coast VNA & Hospice is here to answer any other questions you may have. We provide compassionate guidance to families across the Central Coast. Contact us today to learn more.
